Abstract
Study Design:
Suprafascial free flaps have become common place in reconstructive surgery units. Nomenclature related to these flaps has not been uniform throughout the scientific literature, especially in regard to planes of dissection. This study is designed as a comprehensive review of the literature.
Objectives:
Our study highlights which flaps are used most frequently, their main indications, their survival rate, and how they have evolved in the last few decades as innovations have been introduced.
Methods:
A review of the literature was performed using keywords and Medical Subject Headings search terms. PubMed, Embase, and Cochrane Library were searched using the appropriate search terms. Data collected from each study included flap type, dissection plane, preoperative planning, area of reconstruction, as well as complications, donor-site morbidity and survival rate.
Results:
Seven hundred and fifty-five studies were found based on the search criteria. After full-text screening for inclusion and exclusion criteria 34 studies were included. A total of 1332 patients were comprised in these studies. The most common types of flaps used were superficial circumflex iliac perforator flap (SCIP), anterolateral thigh flap (ALT), and radial forearm flap. The most common areas of reconstruction were head & neck and limbs. There was no significant difference in survival rates between flaps that were raised in different planes of dissection.
Conclusions:
Based on the author’s review of the literature, suprafascial flaps are reliable, they have low donor site morbidity, and there is a wide selection available for harvest. The use of new technologies for preoperative planning, such as CT-Angiography and UHF ultrasound, have contributed to have more predictable results. We propose a standardized classification for these flaps, in order to create a uniform nomenclature for future reference.
Keywords
Introduction
The plane of dissection for soft tissue free flaps has changed significantly in the last few decades. The first type of free flaps was musculocutaneous flaps, 1 which included the underlying muscle and the skin paddle above it. These were very popular but presented significant donor site morbidity and bulk. In 1981, Pontén 2 described the fasciocutaneous flap which consisted of cutaneous and subcutaneous tissue and the deep muscle fascia, leaving behind the muscle. These flaps were raised in the subfascial plane, such as the radial forearm flap originally described by Yang et al 3 in 1981.
Perforator flaps, first described by Koshima and Soeda 4 in 1989, are an evolution of the fasciocutaneous flaps, because they rely on the perforating vessels going through the muscle or muscle septum and into the skin and subcutaneous tissue superficially, leaving behind the muscle and sometimes deep muscle fascia. Using supermicrosurgical techniques that allow anastomosis of vessels less than 0.8 mm in diameter, these flaps could be raised without the need to dissect a long pedicle, and thus avoid trauma to the muscle.
Recently, studies carried out by Hong et al 5,6 show that a flap can be raised safely in the plane of the superficial adipose fascia that separates the superficial and deep fat lobules of the subcutaneous adipose tissue. We refer to free flaps raised in this plane as thin flaps.
As we can see, the evolution shows that soft tissue free flaps have become thinner as they are raised in a more superficial plane of dissection. This has been possible due to new technologies such a Computed Tomographic Angiography (CTA) and high-frequency ultrasound 7 as well as a deeper knowledge in vascular anatomy such as the perforasome theory described by Saint-Cyr et al. 8
Narushima et al 9 proposed a classification of thin flaps based on the anatomical plane on which they are raised: thin flaps dissected in the plane of the superficial adipose fascia, super thin flaps going above the superficial fascia, full thickness skin flap or pure skin perforator (PSP) flaps that are only as thick as the dermis and its superficial plexus of vessels, and split thickness skin flaps.
The objective of this study is to do a review of the flaps raised above the deep muscle fascia and their different variations. Our goal is to identify which flaps are used most frequently, their main indications, their survival rate, and how they have evolved in the last few decades as innovations have been introduced. We also propose a standardized classification for these flaps, to create a uniform nomenclature for future reference.
Materials and Methods
Between January 2019 and September 2020, a comprehensive search and review of the PubMed, Embase and Cochrane databases was carried out. This study has been conducted in accordance to the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines. 10 Two independent reviewers (S.R. and S.H.) screened each study for relevance, conflicting studies were reviewed by a third reviewer (M.F). The following search terms were used: “suprafascial free flap,” “thin perforator flap,” “super thin perforator flap,” “ultra thin perforator flap,” and “pure skin perforator flap.” A complete list of keywords and medical subject headings is reported (Table 1).
Keywords, MeSH Terms and Search Syntax Used for Screening.

The inclusion criteria were: 5 or more clinical cases, only free flaps, dissection plane above the deep muscle fascia, and accessibility through the aforementioned databases. The exclusion criteria were: secondary thinning of the flaps, cadaveric or radiological studies. Only English language articles were reviewed. Studies from the same institution with verified, identical, duplicated data were excluded.
After a thorough review of the selected articles, we identified the following variables: flap type, plane of dissection, preoperative imaging and planning, area of reconstruction, number of patients, complications, donor-site morbidity, flap survival, final outcome and conclusions. Information from the included studies was recorded using Microsoft Excel 2019.
In the variable “plane of dissection” we will use the following classification: suprafascial flap refers to the plane above the deep muscle fascia, thin flaps refers to the plane of the superficial adipose fascia, super thin for flaps dissected above the superficial adipose fascia, and pure skin perforator flaps (PSP) that are only as thick as the dermis and the subdermal vessel plexus. Institutional ethics board approval was not required for this study, as it was a retrospective review of published literature.
Results
The initial literature search provided a total of 755 articles. We removed 203 duplicates from the selection, leaving 552 articles. After a first round of title and abstract screening, we removed 313 articles which were irrelevant to our study, leaving 239 articles. In the third round of screening, we completed full-text review and removed 205 articles based on our inclusion and exclusion criteria, leaving 34 articles for our final review (Figure 1).
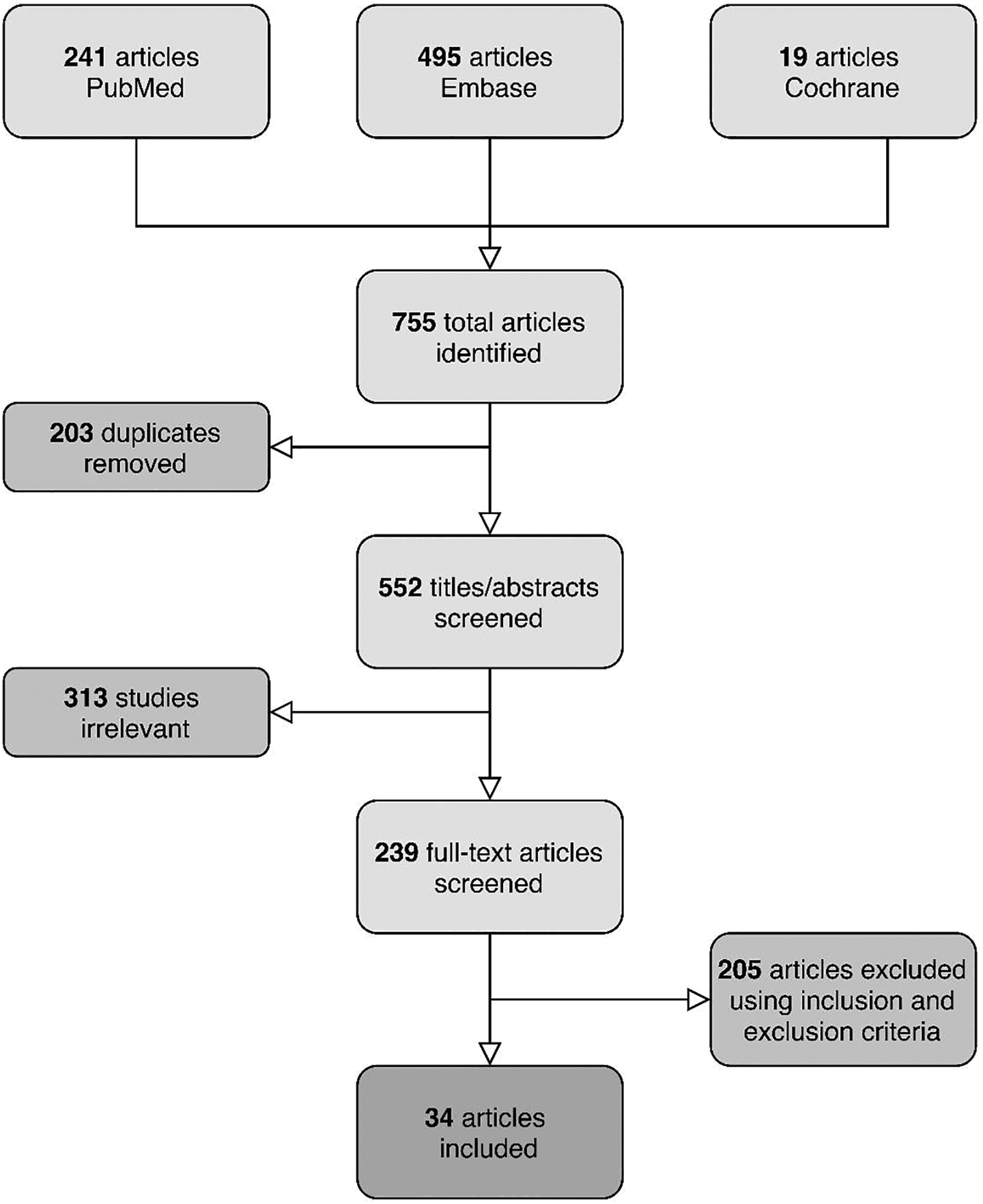
Systematic search scheme divided by screening.
We found a total of 34 articles that describe suprafascial free flaps and met all of our criteria. These studies are summarized in Table 2. There were 1332 patients included in these studies. The articles included were published between 1996 and 2020. Of these, 79% were published in the last 10 years. There were 14 articles that described flaps raised above the deep muscle fascia (suprafascial flaps), with 9 of them comparing suprafascial vs subfascial dissection planes. In 16 articles, the authors reported series of flaps raised on the superficial adipose fascia (thin flaps), with 1 of them comparing thin vs suprafascial dissection planes. There was 1 article that described ALT flaps raised above the superficial fascia (super thin), and compared them to the suprafascial dissection plane. In 3 articles Narushima presented clinical series of flaps dissected in a subdermal plane while preserving the subdermal vessel plexus (pure skin perforator flaps).
Main Characteristics of the Articles Included for Review.
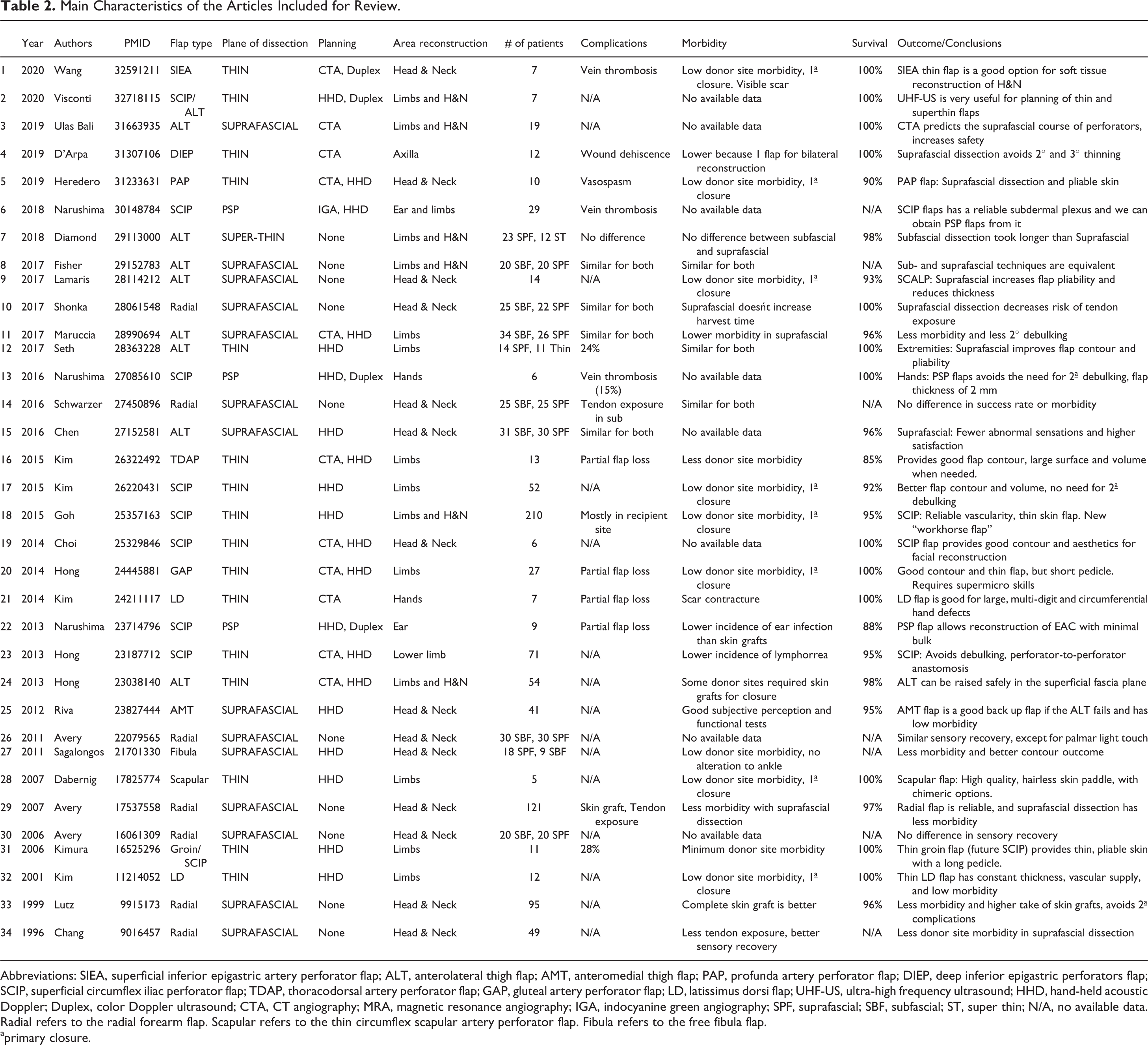
Abbreviations: SIEA, superficial inferior epigastric artery perforator flap; ALT, anterolateral thigh flap; AMT, anteromedial thigh flap; PAP, profunda artery perforator flap; DIEP, deep inferior epigastric perforators flap; SCIP, superficial circumflex iliac perforator flap; TDAP, thoracodorsal artery perforator flap; GAP, gluteal artery perforator flap; LD, latissimus dorsi flap; UHF-US, ultra-high frequency ultrasound; HHD, hand-held acoustic Doppler; Duplex, color Doppler ultrasound; CTA, CT angiography; MRA, magnetic resonance angiography; IGA, indocyanine green angiography; SPF, suprafascial; SBF, subfascial; ST, super thin; N/A, no available data. Radial refers to the radial forearm flap. Scapular refers to the thin circumflex scapular artery perforator flap. Fibula refers to the free fibula flap.
aprimary closure.
With regard to nomenclature, we found that the authors used different terms to describe the plane of dissection and the types of flap. If we consider Narushima’s classification of thin flaps, 94% of authors used this terminology. Those that did not use this nomenclature referred to thin flaps as super thin flaps. 11,12
There were 12 different types of flaps used in the articles reviewed. The frequency of the flaps that were used was as follows: superficial circumflex iliac perforator flap (SCIP) 8 articles (398 total patients), anterolateral thigh flap (ALT) 7 articles (309 total patients), radial forearm flap 7 articles (462 total patients), latissimus dorsi (LD) 2 articles (19 patients in total). The following had 1 article per flap type: scapular, fibula, superficial inferior epigastric artery perforator flap (SIEA), thoracodorsal artery perforator flap (TDAP), deep inferior epigastric perforator flap (DIEP), profunda artery femoris flap (PAP), gluteal artery perforator flap (GAP), anteromedial thigh flap (AMT).
A summary of indications and outcomes grouped by the different flap types is provided in Table 3. These indications and outcomes are solely based on the articles included in this review, and do not include the full range of indications for the flaps listed.
Indications and Outcomes Grouped by the Different Flap Types (Based on the Articles Included in This Review).
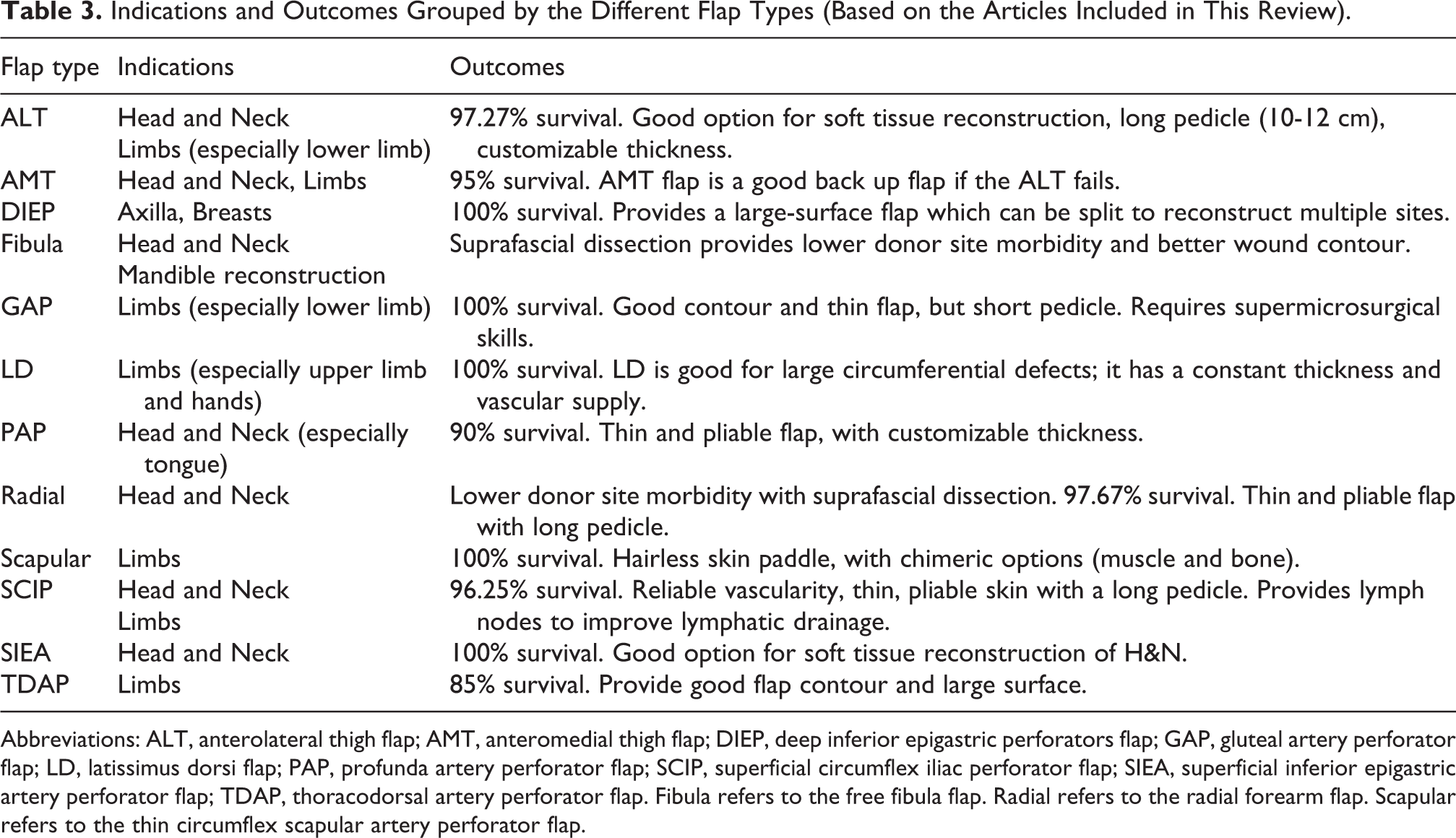
Abbreviations: ALT, anterolateral thigh flap; AMT, anteromedial thigh flap; DIEP, deep inferior epigastric perforators flap; GAP, gluteal artery perforator flap; LD, latissimus dorsi flap; PAP, profunda artery perforator flap; SCIP, superficial circumflex iliac perforator flap; SIEA, superficial inferior epigastric artery perforator flap; TDAP, thoracodorsal artery perforator flap. Fibula refers to the free fibula flap. Radial refers to the radial forearm flap. Scapular refers to the thin circumflex scapular artery perforator flap.
The most common area of reconstruction was head and neck (21 articles, 748 patients), followed by limbs (14 articles, 610 patients). Other areas of reconstruction included hands (2 articles, 13 patients) and axilla (1 article, 12 patients). The number of patients included ranged from 5 to 210 patients, with an average of 43 of patients per study.
Preoperative imaging planning to find dominant perforators was done in 67% of articles. The most common method of imaging was the hand-held acoustic Doppler (9 articles, 444 patients), followed by CT-Angiography (3 articles, 38 patients) or a combination of both (7 articles, 248 patients). Other forms of preoperative planning included ultra-high frequency ultrasound (UHF-US) (4 articles, 29 patients) and indocyanine green angiography (1 article, 29 patients). No preoperative planning was done with radial forearm flaps.
The complication rate was generally underreported, with many articles not making any mention of them (only 50% of studies made direct reports of complications). In general, they included partial flap loss (6%), wound dehiscence (8%), vein thrombosis (9%), seroma (2%) and tendon exposure in radial flaps (up to 20% in subfascial dissection). However, most authors did mention that the rate of complications was similar for both suprafascial and subfascial flaps (mentioned in 5 out of the 9 articles that made the comparison).
The donor site morbidity of the flaps was low in all cases, and allowed for primary closure in 85% of cases (except in radial flap). Most articles that reported donor site morbidity showed that it was similar in subfascial and suprafascial dissections (12 out of 34 articles). Suprafascial dissection showed less morbidity over the subfascial dissection in ALT flaps. 13 In radial flaps, suprafascial dissection has shown to decrease tendon exposure and improved healing of skin grafts. 14 –17 Fibula flaps dissected in the suprafascial plane have also shown lower donor site morbidity and better wound contour. 18 Thin flaps (dissected in the superficial adipose fascia) have also shown to improve donor site aesthetics due to a more uniform wound contour and higher primary closure rate. 6
All free flaps had survival rates of more than 85%. The flaps that presented the best survival rates based on more than 50 patients in the study were radial forearm (97.67%, 263 patients), ALT (97.29%, 258 patients), and superficial circumflex iliac perforator (SCIP) flap (96.25%, 369 patients). The following list shows the rest of the survival rate average based on the flap type: gluteal artery perforator (GAP) flap (100%, 27 patients), latissimus dorsi flap (100%, 19 patients), deep inferior epigastric artery perforator (DIEP) flap (100%, 12 patients), superficial inferior epigastric artery (SIEA) perforator flap (100%, 7 patients), scapular flap (100%, 5 patients), profunda artery perforator (PAP) flap (90%, 10 patients), anteromedial thigh (AMT) flap (95%, 41 patients), and thoracodorsal artery perforator (TDAP) flap (85%, 13 patients).
There was no significant difference in survival between flaps that were raised in different planes of dissection. Suprafascial flaps had a 96.14% survival rate, based on 498 flaps that were included. Thin flaps had a 96.78% survival rate, based on 529 flaps that were included. Super thin flaps had a 98% survival rate, based on 12 flaps that were included. PSP flaps had a 99% survival rate, based on 15 flaps. Using a one-way ANOVA test no significant statistical differences were found between these survival rates (P = 0.16).
Discussion
In this study we conducted a thorough review of the literature in regard to suprafascial free flaps. We presented the most useful techniques available for reconstruction that require thin, pliable and customizable flaps, and only included articles with clinical cases and significant caseloads, in order to show the reader feasible and reliable practices.
When looking at the chronological order and evolution, we see that initially soft tissue free flaps were dissected in a subfascial plane, therefore, when surgeons required a thin flap the one that was used the most was the radial forearm flap. Next there was a progressive surge in the use of perforator flaps, following studies carried out by Wei et al 19,20 describing a perforator-based ALT flap. Following this there have been different types of perforator flaps described, and the trend has been to leave behind the fasciocutaneous flaps for cutaneous perforator flaps in an ever-thinner plane of dissection. In our study we see that in the first 10 years radial flaps were primarily being used, then SCIP flaps, and in the last 10 years mostly ALT. Almost 80% of the articles included were published in the last decade, 21 –36 indicating that this a very contemporary subject in reconstructive surgery (Figure 2).
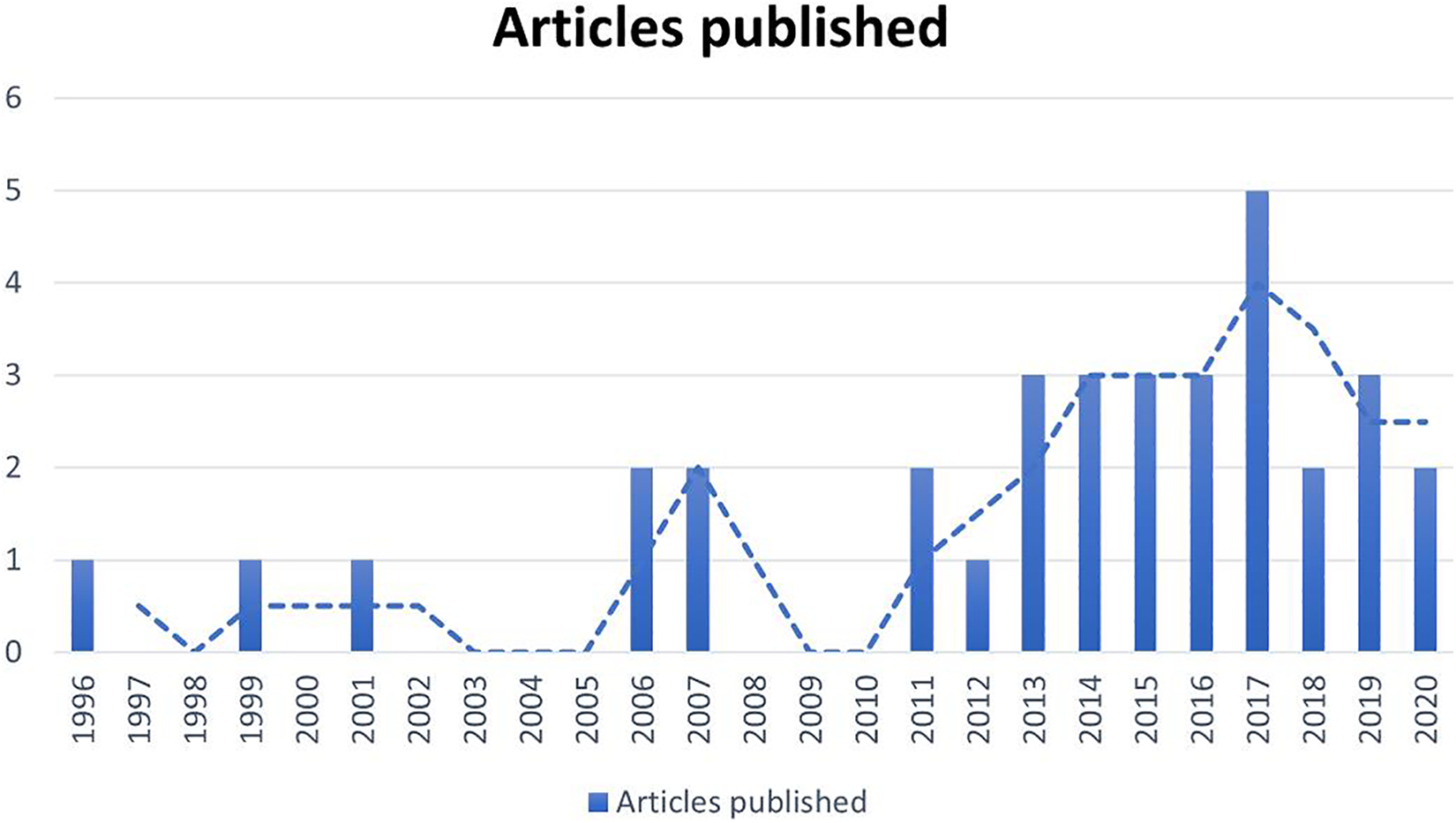
Chronological evolution of included studies.
In regard to the nomenclature, some authors used the term suprafascial indistinctively when mentioning the deep and superficial fascia. Also, some referred to thin flaps as super thin. 11,12 This was noted in the 34 articles that we reviewed in depth, but there was a lack of consensus in regard to the definition of these terms in the scientific literature. For this reason, we believe that adopting a common classification is necessary and we propose to use the following classification: Subfascial = below the deep muscle fascia, Suprafascial = above the deep muscle fascia but below the superficial adipose fascia, Thin flaps = dissected on the plane of the superficial adipose fascia, Super thin flaps = dissected above the superficial adipose fascia, Pure skin perforator (PSP) flaps = include only the skin and subdermal plexus vessels (Figure 3).
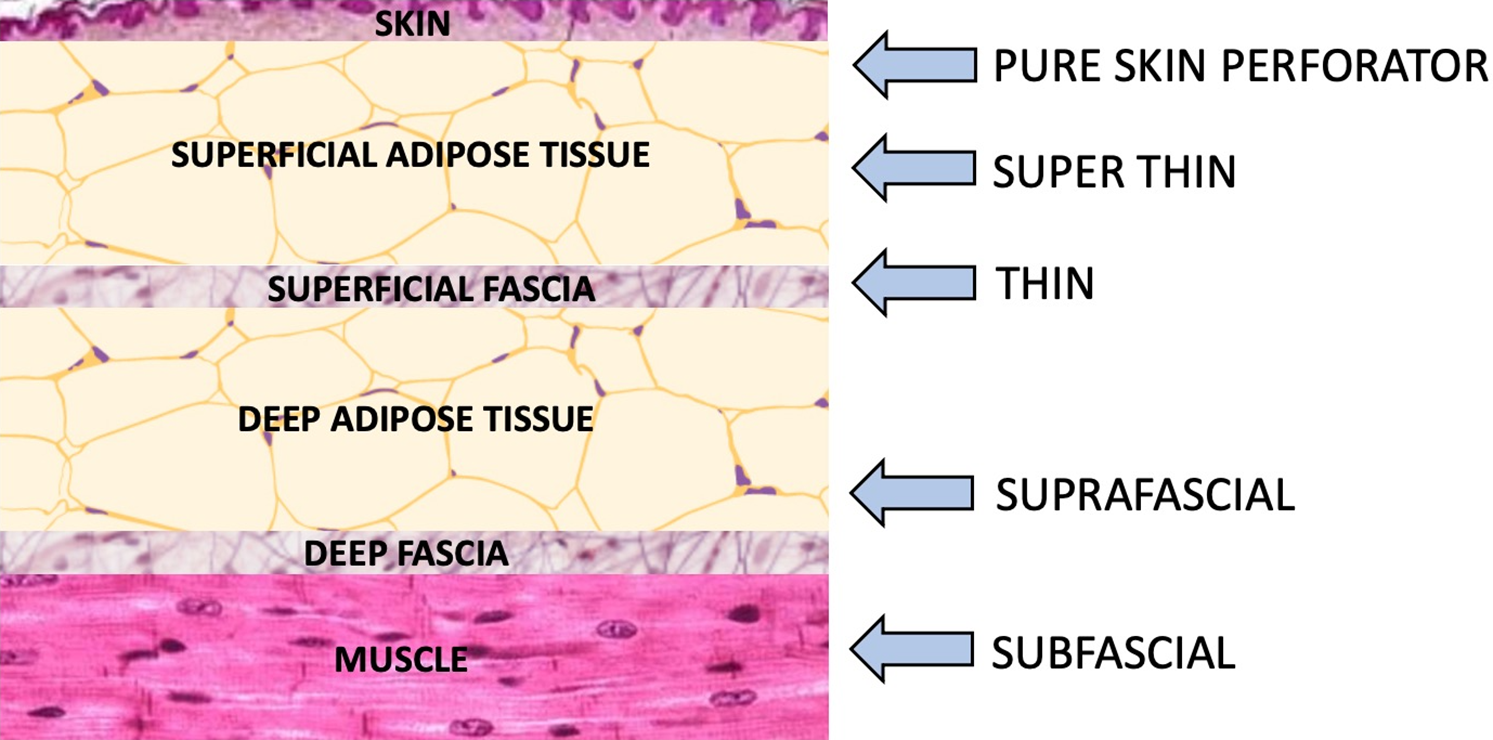
Dissection planes and nomenclature of flaps.
According to the literature, the main areas of reconstruction were head and neck, and limbs. This is because these areas normally require thin and pliable flaps, with long pedicles for anastomosis. For example, even though the radial forearm flap is the most commonly used flap for tongue reconstruction after hemiglosectomy, flaps like the PAP or ALT flap are preferable alternatives that provide thin and pliable tissue when they are dissected as thin flaps. Heredero et al 37 demonstrated that these thin flaps can be obtained even in obese patients when dissected above the superficial adipose fascia.
Most of the reviewed series of flaps dissected above the deep or the superficial fascia include preoperative imaging planning. Studies carried out by Heredero et al 37 with CT-angiography and Visconti et al 7,38 using ultra-high frequency ultrasound (UHF-US) allow us to map out the patterns of the perforating vessels in the suprafascial plane preoperatively. When we combine this knowledge with hand-held acoustic Doppler and/or duplex ultrasound, we have high confidence in the anatomical disposition of the vessels in our flaps. This improves flap survival and shortens operating time. 7,37,38 It also allows us to have thinner flaps, which are more suitable for extremity or head and neck reconstruction, and have lower donor site morbidity. These flaps combined with super-microsurgical techniques, 39 which allow us to anastomose ever smaller vessels (in general under 0.8 mm in diameter), improve our reconstructive options and lead to better outcomes.
Donor site morbidity has been improved with the advent of suprafascial flaps. Our series of articles show that donor site morbidity in suprafascial dissection is either similar or better than subfascial dissection, with no authors reporting inferior results. Suprafascial flaps also provide better wound contour and aesthetics, 6,18,40,41 decrease the risk of tendon exposure and improve the healing of skin grafts in the radial forearm flap donor site, 15,42 as well as allowing for a higher rate of primary closure in the ALT flap donor site. 6
One of the key aspects that has allowed for thin flaps to become mainstream today, is that the flap survival is independent to the plane of dissection. Studies carried out by Hong and Chung 6 and Narushima et al 43 showed that if the vascular network of vessels is preserved, we can dissect extremely thin flaps. These authors also described 3 key areas which are critical to flap survival and must be carefully manipulated, which are the subdermal plexus, the perforating vessels that go through the deep muscle fascia, and the microsurgical anastomosis. Some flaps require customized design to see the perforating vessel patterns, and this is where new technologies have had an important role. 7,37,38,43,44
Conclusions
Suprafascial free flaps are becoming the new workhorse for surgeons as their variety and reliability have improved. We have seen that these flaps are just as reliable as subfascial flaps, they have less donor site morbidity, and there is a wide selection available for harvest. The use of new technologies for preoperative planning, such as CT-Angiography and UH-F ultrasound, have contributed to have more predictable results and they are becoming common techniques for surgeons harvesting these flaps. We propose a standardized classification for these flaps, in order to create a uniform nomenclature for future reference.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
