Abstract
Temporomandibular joint (TMJ) arthroscopy is considered a safe, minimally invasive procedure for the treatment of certain TMJ derangements. However, as TMJ arthroscopy is being popularized, more complications are being reported. Though exceedingly rare, arteriovenous fistula (AVF) can occur. We describe a case of superficial temporal artery (STA) fistula formation successfully treated with coil embolization.
Keywords
Introduction
Temporomandibular joint (TMJ) arthroscopy is an important procedure that has been used for years in the treatment and management of TMJ dysfunction and pain. With a low rate of morbidity and published complication rates between 1% and 10.3%, the procedure is generally regarded as safe and relatively low-risk. 1 –6 However, as more TMJ arthroscopies are being performed, complications are being reported in greater numbers. Arteriovenous fistula (AVF) is an incredibly rare complication with a mere handful of well-documented cases of AVF secondary to TMJ arthroscopy reported in the English literature. 7 –10
Case Report
A 27-year-old woman presented with a 10-year-history of right TMJ pain, rated as 6 out of 10 at baseline, exacerbated to 10 out of 10 with chewing, smiling, or talking. Initially, non-surgical treatment was recommended which included soft diet, warm compresses, NSAIDs, muscle relaxants, physical therapy, splint therapy, and avoidance of wide opening. Though she had temporary relief with Botox injections, she ultimately failed conservative management and with the return of her symptoms was scheduled for and underwent a right TMJ arthroscopy without any intraoperative invasive procedures. Using a Storz all-in-one arthroscopy system, a sharp trochar was placed into the posterior superior joint space through which the arthroscope was placed. Ultimately, via level I arthroscopy utilizing a single portal, visualization of the TMJ was achieved. Lysis and saline lavage revealed extensive degenerative changes, erythema, fibrillations and adhesions, consistent with osteoarthritis and severe synovitis. 11 The disc was anteriorly displaced with no perforation or folding and had a normal osseous contour (Wilkes stage 3). After removal of the arthroscope, .5 ml of Kenalog steroid was injected into the joint and the incision was closed.
The following day, the patient complained of a right-sided throbbing pain and muffled sound in her right ear which developed into a persistent ringing sensation. She was prescribed Percocet which temporarily alleviated the pain and was told to follow-up in clinic 6 weeks later. A month after her initial procedure, the patient called to report no improvement in pain or function following the arthroscopy and the presence of a chronic throbbing sound in her right ear that seemed synchronous with her heartbeat. At this time, surgical options involving disc salvage and removal were discussed and planned. A few weeks thereafter, she arrived in the pre-op area reporting fullness and tenderness in her pre-auricular region. On physical examination, she had fullness of her right pre-auricular region with a palpable diffuse thrill. Digital pressure over the area of fullness partially improved the throbbing sound in her ear. Given the suspicion for a vascular abnormality, a computed tomography angiography (CTA) was performed which showed a prominent vessel anterior to the right external ear, raising the possibility of an arteriovenous fistula (Figure 1). A diagnostic angiogram was then performed under general anesthesia, which showed an AVF in the pre-auricular soft tissues, likely the source of the patient’s symptoms (Figure 2). The fistula was successfully abolished with coil embolization of the superficial temporal artery, and the patient’s right-sided tinnitus completely resolved upon emergence from anesthesia. Three days later, the patient underwent a right TMJ arthroplasty and successful repositioning of the disc for persistent pain, during which time the coils were removed (Figure 3).
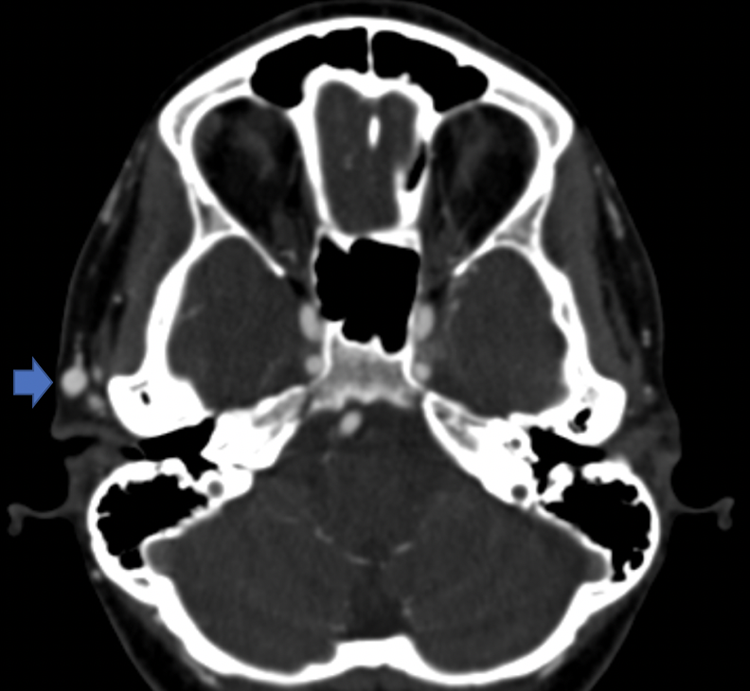
This figure is an axial CTA of the neck showing a dilated vessel in the right pre-auricular soft tissues, concerning for a vascular abnormality. No dilated vessels are seen in the contralateral pre-auricular soft tissues.
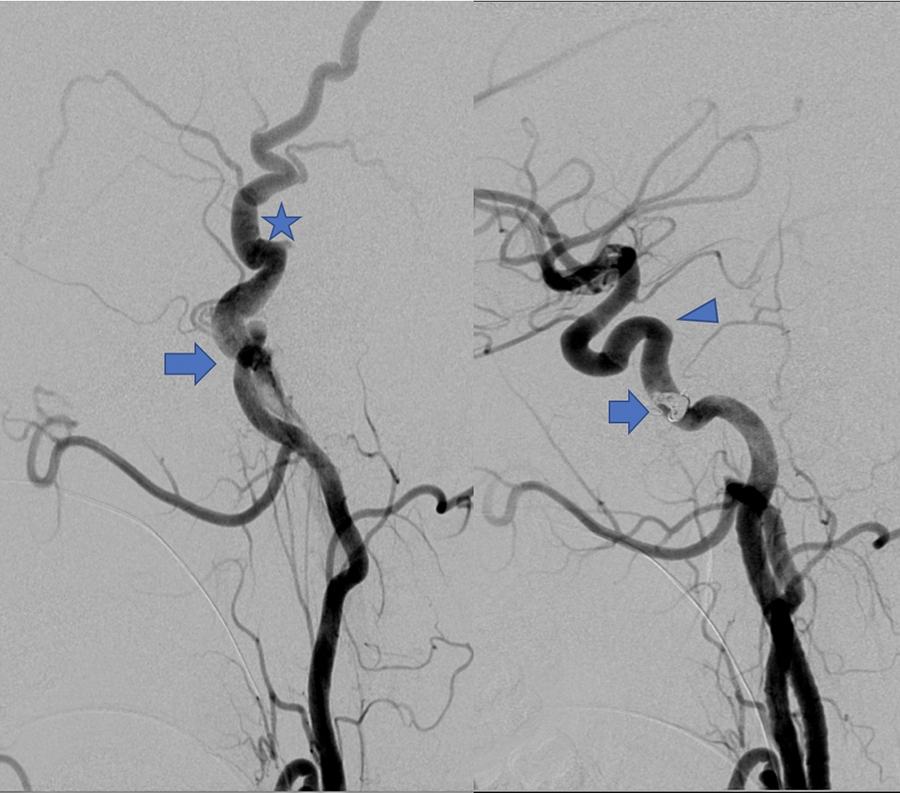
The first image in this figure is a lateral projection of a right external carotid artery angiogram, showing a direct arteriovenous fistula (arrow) between the right superficial temporal artery and adjacent dilated vein (star). The second image is a post-embolization lateral projection right common carotid artery angiogram showing coils at the site of the fistula, with no further filling of the fistula. The dilated vein is no longer visible. The right internal carotid artery is normal in appearance (arrowhead), visible on this injection due to the catheter tip position in the right common carotid artery.
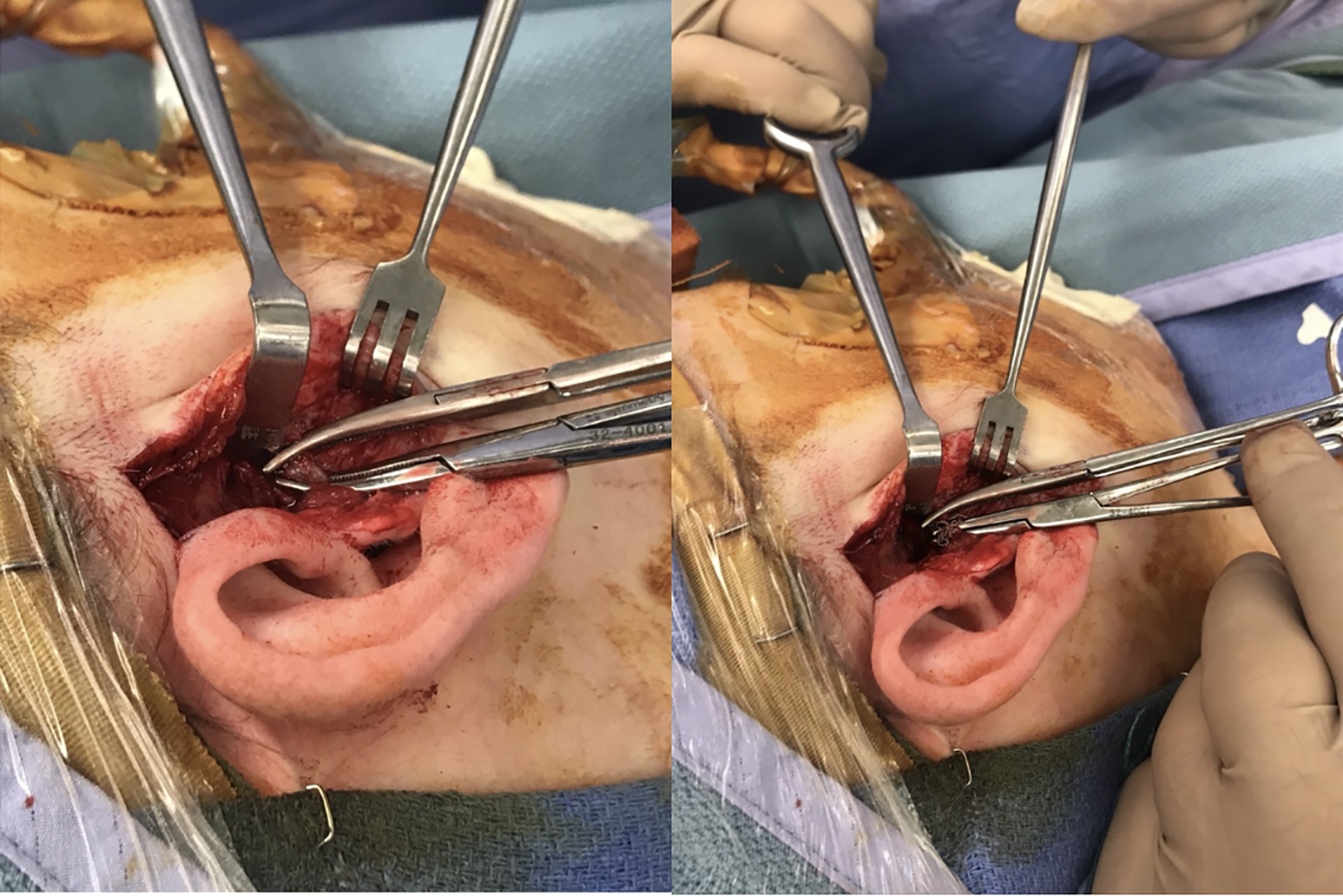
Intraoperative image showing extracted coils in the pre-auricular soft tissues during TMJ arthroplasty.
Discussion
In comparison to alternative surgical techniques or conservative measures, TMJ arthroscopy has been shown to provide for faster postoperative recovery, more effective treatment of pain, and less post-op morbidity, with evidence from cadaveric studies showing that collateral damage to surrounding structures is indeed rare. 3,5,8 At present, treatment options for temporomandibular disorders range from conservative approaches such as muscle exercises and splint therapy, physiotherapy, intraarticular injections of hyaluronic acid or corticosteroids, to arthrocentesis, arthroscopy, and open joint surgery. Despite the number or treatment options available, evidence supports that minimally invasive procedures are remarkably effective at reducing pain and improving mouth opening and may be used as first-line treatment without the need for exhausting conservative management options. 5 However, with the popularization of TMJ arthroscopy, certain complications are being reported in greater numbers due to the quantity of arthroscopies being done, however, the percentage of complications continues to remain low. While infection, otologic, vascular, neurologic injury, and perforation of the middle cranial fossa are often reported, 1 arteriovenous fistula (AVF) remains exceedingly rare with very few well-documented instances. 7 –10,12 In such cases, the superficial temporal artery is the most commonly affected vessel, however, there was one incident in which a fistula formed from the middle meningeal artery 9 and another from the pterygoid branch of the internal maxillary artery. 13
The pathogenesis of posttraumatic AVF formation has been proposed by various mechanisms, with the laceration and disruption theory being the 2 most often cited. 14 In the former, a concurrent laceration of both an artery and its accompanying vein results in a single fistula. In the latter, it is suggested that endothelial cell proliferation leads to the formation of numerous, small vascular channels through which blood can travel. 14 Our case is most consistent with the laceration mechanism wherein trauma leads to a connection between the high-pressure superficial temporal artery (STA) with the adjacent, low-pressure yet richly vascular venous pterygoid plexus. Upon fistula formation, a direct communication between high arterial flow and slow venous flow produces a high pressure differential leading to dilation of the weak walled venous vessel resulting in a mass with a palpable thrill and an audible bruit—findings which have been described in our case and all previous cases. 7
As for the diagnosis of AVFs, multiple imaging modalities have been used in the past, however, intra-arterial angiography—the modality used in our case report—remains the definitive method for both investigation and diagnosis. Ultimately, AVFs may be treated either by surgical ligation and excision under a local or general anesthetic or by endovascular techniques. 15 Regarding treatment of STA fistulas specifically, a review of the literature shows that although STA fistulas can indeed be treated with ligation via open surgery, several authors report great results through endovascular embolization. 8 In direct surgery, partial excision or ligation alone is frequently followed by recurrence, therefore complete resection of a lesion is essential. 15 Endovascular treatments, which include percutaneous coil embolization, embolization with liquid embolic agents such as isobutyl l-2-cyanoacrylate or Onyx, direct-puncture coil embolization, and injection of absolute alcohol all have the added benefit of avoiding cosmetically unacceptable scars. Moreover, coil embolization provides an optimal diagnostic and therapeutic modality that can be performed at the same time as angiography. 15,16 While surgical techniques have been the most common method of treating the lesion in the vast majority of reports, endovascular embolization appears not only to be suitable for treating this condition but is in fact believed by some to be the preferred treatment strategy over surgery. 15 Our case shows successful treatment of STA fistula with coil embolization. This technique has shown positive outcomes when compared to prior reports endorsing detachable balloons, which are no longer available in the United States. 17 Furthermore, coils are more controllable and delivered more accurately. 7 When compared to Onyx, which has shown favorable results compared to N-butyl cyanoacrylate 18 , coil embolization seems the superior option on account of the many disadvantages associated with Onyx. In addition to transiently causing patients to give off an unpleasant odor and permanent skin staining, Onyx also requires a learning curve in order to avoid unwanted reflux and to manipulate flow. Moreover, because it takes time to create a proximal plug, Onyx carries a risk of prolonged exposure to radiation during fluoroscopy, a scenario which has been associated with alopecia and radiation burns. Finally, when compared to NBCA, Onyx has the disadvantage of being more expensive, sticking to the microcatheter which can lead to breakage, and is associated with migration and pulmonary embolism formation. 18 Similarly, alcohol ablation—though effective—is not without its own list of complications and side-effects. Outside of bronchospasm and cardiovascular collapse which are the most common and potentially dangerous complications in these neurointerventional procedures, alcohol ablation can be quite painful. Other adverse reactions to ethanol, such as hemolysis, alterations in anesthetic agent activity, and skin necrosis, are more common with higher doses used in treatments outside the CNS. 19
Conclusion
In the end, although TMJ arthroscopy is relatively safe and associated with low morbidity, complications can occur. Though few cases have been previously described, STA fistula formation secondary to TMJ arthroscopy trauma should be suspected in the patient that presents with feelings of fullness in the pre-auricular region with a palpable diffuse thrill and aural throbbing. A careful arthroscopic technique is needed to avoid such complications. Ultimately, while surgery is a viable option to fix such a lesion, we add our case to the growing list of STA fistula cases that have been successfully treated with coil embolization.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
