Abstract
Background:
Oral epignathus teratoma is an extremely rare neoplasm that occurs exclusively in neonates. The tumor can grow to a large size obstructing airways and it may prevent fusion of the nasal septum with the palatine processes, which may result in cleft palate formation. The rare tumor may also co-exist with other congenital malformations such as hamartoma and choristoma causing airway obstruction and death.
Case report:
We present a case of a one-day-old male neonate who presented with oral mass associated with difficulty in breathing and inability to suck breast milk. Computed Tomography (CT) scan revealed multiple masses involving the alveolar, palate, and tongue along with cleft palate. Emergency surgery was done to relieve the airway and histology confirmed epignathi teratoma with tongue choristoma.
Conclusion:
Epignathus teratoma is a rare condition that requires prenatal prompt diagnosis. However, in countries with underprivileged hospital facilities, early surgical intervention during the neonatal period is what is required to save the patient from airway obstruction. Association of the tumor with midline anomalies is mostly the norms, however, 5% of cases with malignant transformation have been reported and the tumor is commonly associated with endodermal sinus tumor. Therefore long term follow-up of patients with serum tumor markers is highly recommended.
Introduction
Teratomas are neoplasm composed of tissue driven from 3 germ cell layers. The overall incident of the neoplasm is 1: 40,000 live births. 1,2 Congenital teratoma is a rare neoplasm that occurs in the head and neck region in only 2% to 9% of all cases of teratoma with 5% chances of malignant transformation. 1 A choristoma is a mass of normal tissue in an abnormal location, when it occurs in the tongue it may obstruct the airway or digestive tract. 3 The co-existence of multiple congenital teratoma of the head and neck region with choristoma and cleft palate in a neonate is a rare presentation that prompted the need for this case report to re-emphasize on its complexity and management.
Case Report
A day old, term, male neonate weighing 2.7 kg was referred to oral and maxillofacial surgery department for evaluation and management of “multiple large oral masses” noticed at birth obstructing adequate breathing, feeding, and preventing mouth closure with no other medical problems. The child was born to a 30 year old Kanuri woman P3+0 A3, the father is 53 years old, both parents were of sound health with no similar presentation or ill health in other siblings. No antenatal visits or Ultrasound scan was done during pregnancy. No maternal febrile, ingestion of traditional concoction, exposure to radiation, or use of cytotoxics drugs during pregnancy. The mother does not smoke or take alcohol. The delivery method was by spontaneous vertex, uneventful, at home supervised by a traditional birth attendant, and was immediately taken to a peripheral hospital for evaluation before referral to our center where the airway was maintained by nasal cannula and face mask oxygen, lateral positioning and regular oral suction. No attempt at feeding was done, the patient was placed on intravenous fluids.
On examination, the patient was found to have severe respiratory distress with SPO2 of 42%. Occipito-frontal circumference of 34 cm and length of 48 cm. He was fully conscious, alert with good cortical activity. The heart sounds were S1, S2 no added sounds. The liver and spleen were not enlarged, the kidneys were not ballotable. A round firm swelling was located on the palate with a separate swelling on the lower anterior gum pad attached and continuous with the anterior tongue, with associated bluish discoloration of the lips and inability to suck breast milk. There were no other swellings in other parts of the body. A patent airway was maintained with lateral positioning and supplemental nasal oxygen.
The patient was then reviewed by Anesthesiologist and immediately taken for emergency airway control, examination under anesthesia, and tumor excision. Intra-operatively there was a midline intraoral mass measuring 3 × 2 cm attached inferiorly to the lower anterior gingiva/floor of the mouth and the superior margin was continuous with the tongue pushing it posteriorly toward the nasopharynx (Figure 1A). The surface of the mass appeared multinodular with a hard cartilaginous stalk attached firmly to the gum pad of the mandibular symphysial region. Cleft palate deformity with another palatal mass measuring 4 × 3 cm was seen projecting from the region of the vomer, obliterating the soft palate. Computed tomography scan revealed a mass obliterating the left nasopharynx with no intracranial extension (Figure 1B and C). An assessment of congenital teratoma was made. The patient had excision of the palatal mass and the lower anterior oral masses (Figures 1D to I and 2A and B). Consultant Anesthetist experienced in neonatal intubation successfully intubated the patient using a paraglossal approach with a Miller blade size 0 passed from the right corner of the mouth. Special considerations for intubation include the use of a straight blade instead of the Macintosh blade. This overcomes the problem of interference curvature into the line of sight. Also, improved glottis view by head extension is achieved with the straight blade and not with a curved blade.
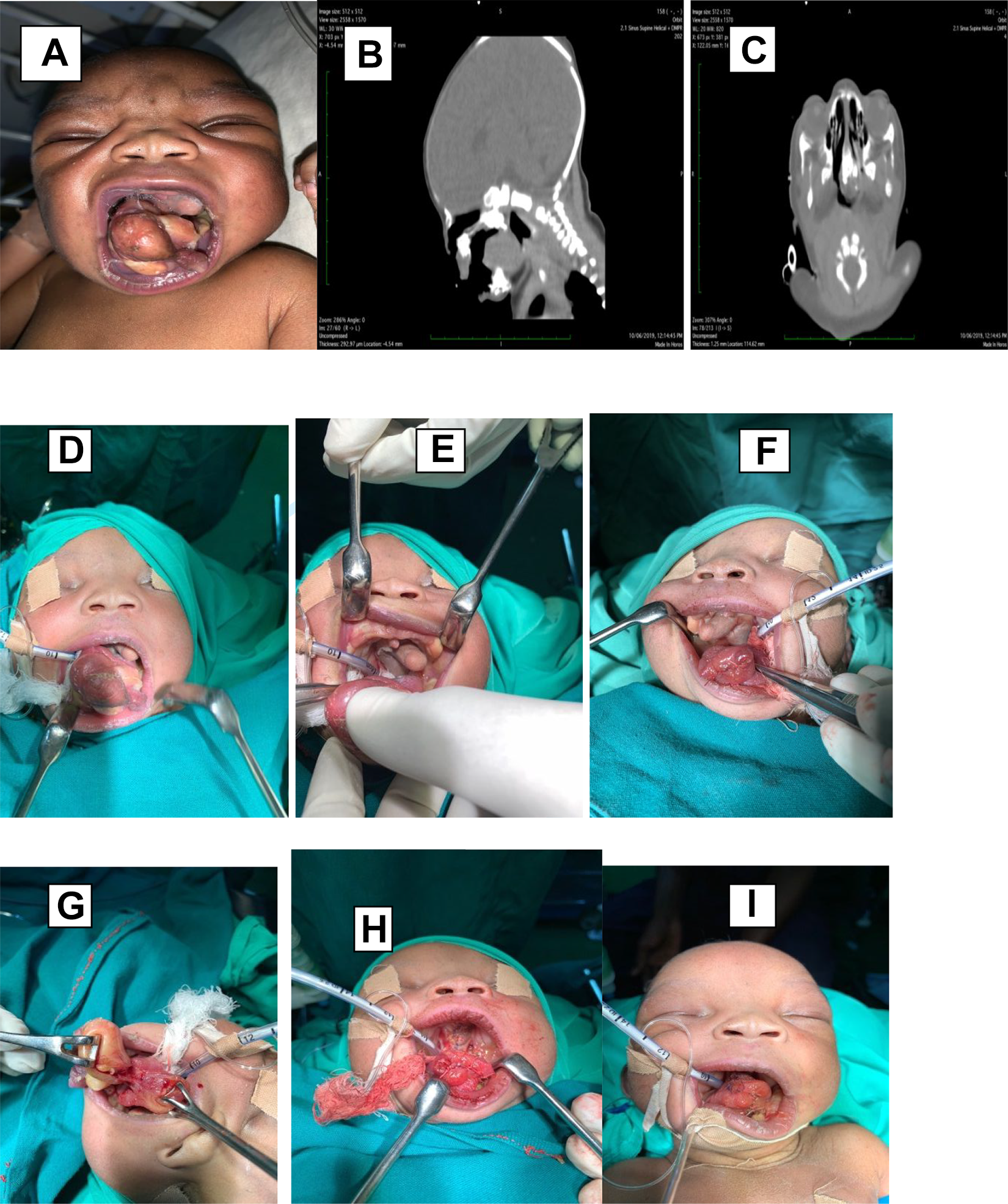
A-show oral mass before surgery. B, C-show CT scan showing hyperdense areas of alveolar, palatal and tongue mass. D, E, F, G, H, I-show surgical steps taken in removing alveolar, palatal and tongue masses.
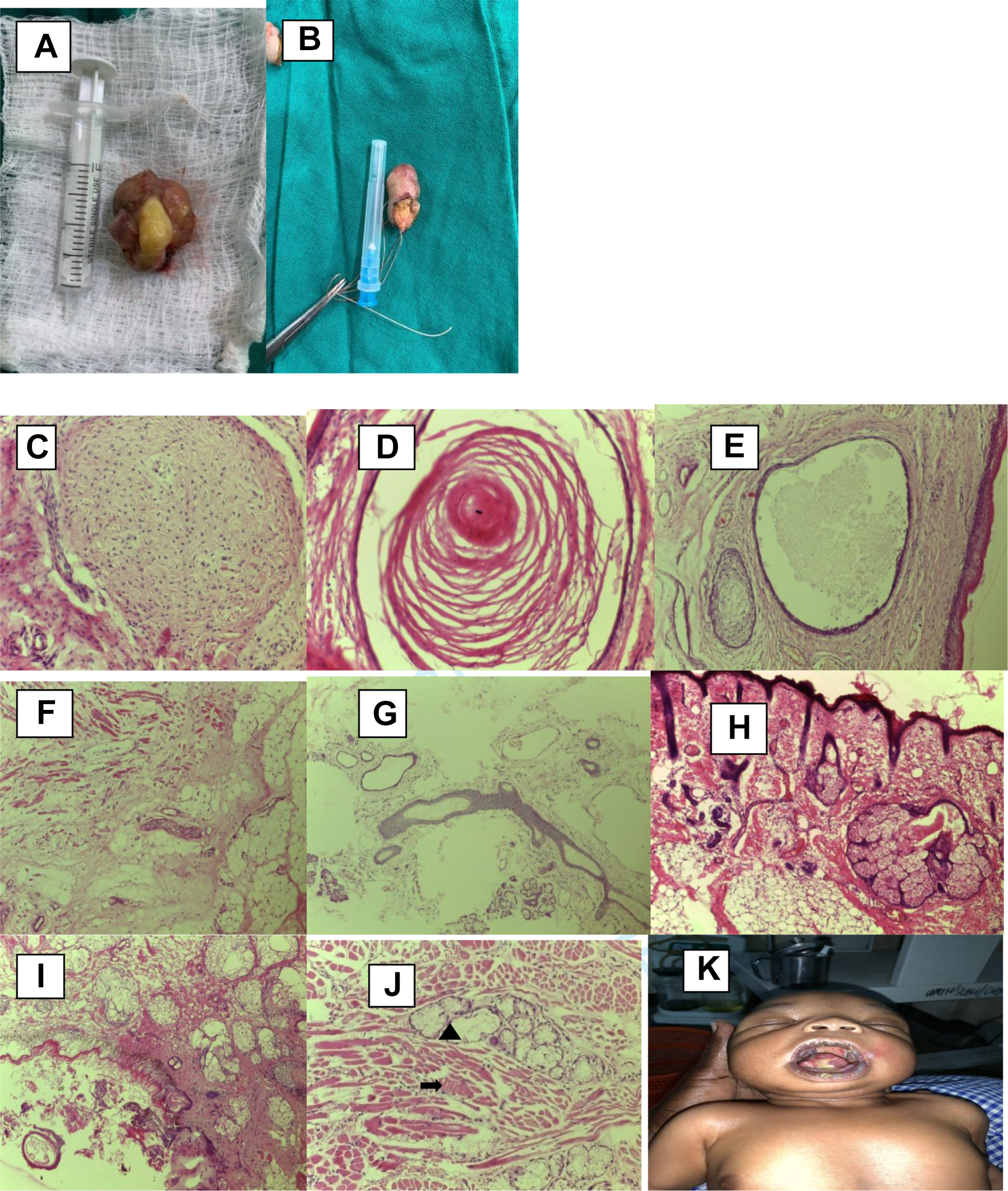
A, B shows an excised tumor from the tongue-alveolar and palatal masses respectively. C, D, E, F, G and H shows mature teratoma composed of neural elements, keratinous cyst, skin with skin adnexal glands, adipose tissue and smooth muscle bundles from the alveolar and palatal masses. I and J from the tongue mass show choristoma composed of skeletal muscle bundles (arrow) and entrapped mucous glands (triangle). (H and E X 100). K shows the patient 2weeks postoperatively.
The mass was excised. After postoperative recovery, the patient was moved to the special care baby unit for monitoring, neonatal intensive care unit is not available in our center. Postoperative care included regular wound care, oral toileting, suctioning, and antibiotics. The baby was initially fed with expressed breast milk using a cup and spoon and gradually introduced to latching. The patient showed satisfactory postoperative healing and excellent health. Recovery was evidenced by improved respiration, latching, and weight gain. The discharge was delayed for 3weeks because of the long processing time of histology in our center and parents requested to stay due to long distance from their domain. The patient was followed up for 6weeks before defaulting. At each visit, the tumor bed was inspected for any recurrence in the clinic under direct vision. Postoperative wound healing of the resection site and tongue movements were also assessed. The cleft palate is planned for closure when the patient is 18 months old with no tumor recurrence. The histology report confirmed Epignathi teratoma with tongue choristoma (Figure 2C to J).
Discussion
The term teratoma is derived from the Greek word “teraton” meaning monster. 2 It is composed of various cellular elements from the 3 germ layers ectoderm, mesoderm, and endoderm. 1 The tumor commonly developed from the midline structures of the body with an incidence of 1 in 35,000-200,000 live births, 1,4 and it is 3 times more common in females than males. 5 The presence of teratoma in the head and neck region is uncommon and accounted for only 1-10% of cases 1,2,6,7 while oropharyngeal teratomas are extremely rare accounting for only 2% of all teratomas. 1,2 In our case the patient is a male and he presented with both palatal and alveolar mature solid and cystic teratoma, (epignathi teratoma) composed of mainly ectodermal and mesodermal elements and tongue choristoma comprising skeletal muscle bundles and mucous glands. The term epignathus is reserved for teratomas that arise specifically from the alveolar of the mandible, 1 however, teratoma arising from the soft or hard palate, cheek, buccal mucosa, and tongue are also regarded as epignathus. 6 Generally epignathus teratoma occurs at the rate of 1:35,000 to 1:200,000 live births with slight female predominance. 2 Majority of the tumors are benign and most of the patients present with airway obstruction or feeding problems 6 as in the index case. Epignathus teratoma associating with other midline anomalies such as harmatoma, choristoma, and encephalocele have been observed and reported in many studies, 8 however, the presence of choristoma in the oral region are rare and often misdiagnosed as benign tumors rather than tumor-like lesions. 9 –11 In a literature review of reported cases of choristoma over a decade (2000 to 2012) there were 96 cases with the age of patients at presentation ranging from birth to 85 years. In the majority of the cases (53.2%) the lesion was located on the tongue as in our case, this is followed by the floor of the mouth (27%). 10 The mass was also mostly single elements in 59.4% of cases study and 40.6% of the cases showed mixed elements. 10 Respiratory, gastric and cartilage tissues were the most prevalent single tissue patterns seen in choristoma while respiratory/gastric and epidermal/follicular were the most prevalent mixed tissue. 10 In our case, the tissue elements are predominantly skeletal muscle and follicular tissue in the form of mucous glands (Figure 2I and J). Cleft palate occurs as a result of the tumor mass preventing the fusion of palatal shelves during the eigth to twelve weeks of intrauterine life 2,12 a feature that is similar to our case. Epignathus has been reported to be associated with other malformations, most commonly, cleft palate and rarely, maxillary dublication. 4,13 Co-existence of epignathus teratoma with tongue choristoma is very rare, 10 based on our English PubMed literature searched we found only 2 cases. 14,15 There are only 13 cases of isolated oral epignathus teratoma reported in the literature from the first case report in 1930 to 2004. 7 The ages of the patients at diagnosis were within the prenatal period which ranges from birth to 5 months and majority of the cases reported were females (8 out of 13 cases). 7 The largest excised mass from that study measure 10 × 12 cm. 7 Similarly, 2 cases of epignathus teratoma from the sphenoid bone causing a sphenoidal cleft without intracranial extension has been reported. 16 The co-existence of epignathus teratoma with malignant germ cell tumors is uncommon 10 but malignant transformation from preexisting benign oral teratoma has been reported in less than 5% of cases. 2 That is why congenital teratoma should always alert the surgeon to the possibilities of york sac tumors, which is usually detected by high serum level of alpha foeto protein (AFP) produced by the tumor. 2 AFP has not been done for our patient because of financial constraints. A case of partial facial duplication with confirmed mandibular, maxillary, and tooth elements has been reported. 13 Although the etiology of fetal duplication is uncertain, however, proposed theories such as fusion, fission, and ischemic atrophy have been described. 4,13 The most accepted theory is the failure of fusion of the palate because of the attached parasitic fetus on the tongue. 13 Even though the distinction between twin and mature teratoma is controversial. 13 Teratoma developing during intrauterine life may result in polyhydramnious 2 therefore, prenatal care such as ex-utero intrapartum treatment or tumor resection at the time of caesarian section and before cutting of umbilical cord is usually done to save the patient’s life. 2 In our case the patient presented within 24 hours after birth, thereafter the tumor was resected to relieve the airway obstruction.
Conclusion
Epignathus teratoma co-existing with tongue choristoma and cleft palate is a rare presentation. The present case report highlights the pathology of the tumor co-existing with tongue choristoma and its relationship with other midline anomalies and the possibilities of the presence of malignant germ cell tumor. Although serum AFP was not done in our patient because of financial constraints, it is, however, necessary to rule out the possibility of malignant germ cell tumors. This case report shows how this case was diagnosed and managed within our limited facilities despite the complexity of the condition.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
