Abstract
Objective
Lumbar fractures are the most common spinal injuries, and surgery is required for severe fracture. This study aimed to investigate the variations in motion and stress in varying states of activity after minimally invasive and traditional open pedicle screw placement for L1 vertebral fracture stabilization.
Methods
We studied a male volunteer (26 years old) with no history of chronic back pain or lumbar spine trauma. We used the finite element method for this investigation. Using finite element software, we created a three-dimensional model of L1 vertebral compression fracture. We also constructed models for four percutaneous pedicle screws spanning the fractured vertebra and four screws traversing the damaged vertebra with transverse fixation.
Results
In all three-dimensional movement directions, the open pedicle fixation system experienced maximum stress higher than its percutaneous counterpart. With axial spinal rotation, von Mises stress on the traditional open pedicle screw was considerably lower than that with percutaneous pedicle fixation, but peak stress was elevated at the transverse connection. Traditional open pedicle fixation displayed less maximum displacement than percutaneous pedicle internal fixation.
Conclusions
During axial spinal movements, high peak stress is observed at the transverse connection. Patients should avoid excessive axial rotation of the spine during recovery.
Keywords
Introduction
Thoracolumbar fractures are prevalent types of spinal injuries, and approximately 90% of such injuries are located in the thoracolumbar section.1,2 Initiating an early intervention that involves reduction and internal fixation is critical, particularly because the fixation approach greatly affects the treatment outcome and prognosis. These fractures are often the result of high-energy trauma. 3 Surgical intervention can restore the spinal anatomy, rebuild the spinal biomechanical stability, shorten the bed rest duration, and facilitate quicker recovery, among other benefits. 4 Current surgical techniques for thoracolumbar fractures can be broadly categorized into traditional open internal fixation and percutaneous pedicle internal fixation. Traditional open internal fixation involves larger incisions and extensive paravertebral soft tissue dissection and traction, which can lead to ischemia, necrosis, and fibrosis of the paravertebral muscular tissues. Consequently, this approach can cause postoperative lumbar stiffness and chronic pain, greatly affecting the patient’s prognosis. 5 In recent years, minimally invasive technology advancements have led to the use of percutaneous pedicle screw fixation because of its advantages, such as smaller incisions, minimal blood loss, less back muscle damage, quicker postoperative recovery, and fewer complications than the traditional technique.6–8 The biomechanical properties and pedicle screw stress distribution vary depending upon the fixation method and the screw itself.
Posterior approach surgery is a traditional operation for thoracolumbar fractures, and it offers benefits such as minor trauma and a quick recovery. 9 In the posterior internal fixation system, the pedicle screw system is a popular choice in clinical practice because of its high mechanical strength and stability. The reduction principle primarily involves restoring spinal biomechanical stability through the screw system’s stretching effect and the ligament’s axial reduction. 10 Studies have shown that finite element analysis is a vital research method in orthopedic biomechanics, particularly in spinal internal fixation and implantation.11,12
The pedicle screw fixation method is widely used in clinical practice for the treatment of lumbar vertebral fractures owing to its simplicity and ease of operation. Finding a method that can simulate and evaluate the safety of posterior pedicle screw fixation for treating lumbar vertebral fractures before surgery has been a focus of research. Finite element analysis is currently a commonly used method for evaluating pedicle screw fixation models and analyzing their safety. However, previous researchers did not consider the absence of fiber reinforced structures when modeling hyperelastic material models. Additionally, small joints and ligaments have been simplified, making the real human body structure more complex. Furthermore, current research has not simulated muscle contraction. Muscle contraction may result in complex external forces that have a major effect on the biomechanical angle.
This study aimed to carefully examine the changes in motion and pressure under different activity states after minimally invasive and traditional open pedicle screw placement. We used the finite element method to conduct this study. Our findings will hopefully provide a more reliable theoretical basis for reducing the risk of secondary surgery caused by loosening or breaking of pedicle screws after surgery.13,14
Development of the three-dimensional lumbar spine model
Clinical data
We selected a young male volunteer with no history of chronic back pain or lumbar spine trauma. He was aged 26 years and had a body mass index of 21.5 kg/m2. He underwent a lumbar spine X-ray examination to rule out the presence of spinal diseases. The study protocol was approved by the ethics committee of the First Affiliated Hospital of Hebei North University (approval number: W2023036). The volunteer was a graduate student in the research team and provided written informed consent.
Validation of the lumbar spine finite element prototype
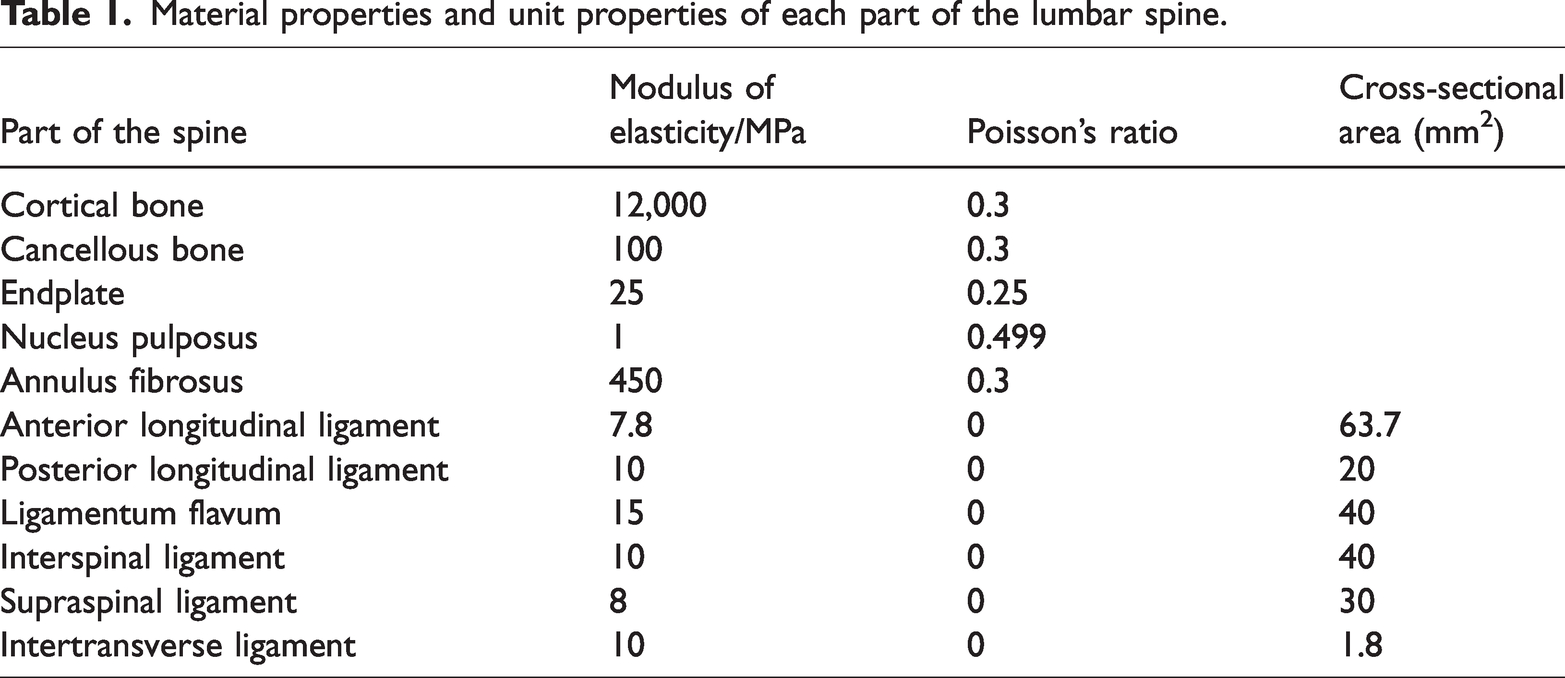
An L1 vertebral burst fracture finite element model was developed on the basis of an Angola classification A3 fracture with a thoracolumbar injury severity score of 4 to 5. The finite element model was created using software including Mimics 17.0 (Materialise, Inc., Leuven, Belgium), Geomagic studio 2013 (Geomagic, Inc., Research Triangle Park, NC, USA), and Hypermesh 13.0 (Altair Engineering, Inc., Executive Park, CA, USA).15,16 Material properties including elastic modulus and Poisson’s ratio were designated to components, such as bone tissue, soft tissue ligaments, pedicle screws, and rods, on the basis of previous studies (Table 1). 13 We used Mimics software to process DICOM format computed tomographic images and reconstruct T12–L2 segment models. We used Geomagic software to refine T12–L2 spinal models. SOLIDWORKS software version 2020 (SolidWorks Corp., Waltham, MA, USA) was used to reassemble cortical and trabecular bone of vertebrae, and to establish related spinal accessory anatomical structures, such as intervertebral discs, the nucleus pulposus, and ligaments. The finite element model of T12–L2 segments created as mentioned above was imported into Workbench software version 2021 R1 (ANSYS Inc., Canonsburg, PA, USA) in STEP format and material properties were set. The size of cortical bone, cancellous bone, intervertebral discs, and mesh division was 2 mm. The endplate and articular cartilage are weaker than the other components. Therefore, we divided them more precisely to obtain a more accurate calculation. Consequently, the mesh size was set to 0.5 mm.
Material properties and unit properties of each part of the lumbar spine.
We constrained all six degrees of freedom of the endplate under L2 conditions as boundary conditions. We applied a compression force of 500 N to the upper surface of the model to represent the upper body weight, and applied a torque of 10 Nm to simulate the six movement directions of the lumbar spine model: flexion and extension, left and right lateral bending, and left and right axial rotation. Six standard lumbar motions were simulated: forward flexion, backward extension, left lateral flexion, right lateral flexion, lateral bending, and rotation. The computed relative range of motion of the L1–L2 segment was compared with that in Natajaran et al.’s in vitro study 16 and Xiao et al.’s finite element analysis. 13
The range of motion results showed robust agreement between this model and previous data (Table 2), validating the T12–L2 segment finite element prototype.
Relative range of motion data of L1–L2 segments under different movements.

Generation of L1 fracture and dual pedicle screw fixation configurations
The pedicle screw designs were transferred to Workbench 17.0 in STEP format. The L2 vertebra base was fully immobilized to restrict six-directional movement. A 500-N load applied on T12 mimicked upper body mass. A reference point over the lumbar rotation center enabled proper load transmission. Additional 10-Nm torque loads simulated six lumbar motions. The distribution of von Mises stress and maximum pedicle screw displacements were assessed (Figures 1 and 2).

Distribution of von Mises stress of screws for percutaneous pedicle screw fixation. (a) Anterior flexion; (b) posterior extension; (c) left flexion; (d) right flexion; (e) left rotation and (f) right rotation.

Distribution of von Mises stress of screws in traditional open pedicle screw fixation. (a) Anterior flexion; (b) posterior extension; (c) left flexion; (d) right flexion; (e) left rotation and (f) right rotation.
Results
Investigation of von Mises stress distribution in two pedicle screw rod stabilization systems
We examined and compared von Mises stress dispersion in the pedicle screw between two distinct fixation techniques (Table 3). The fatigue threshold of the pedicle screw was 550 MPa, the yielding threshold was 869 MPa, and the breakage threshold was 924 MPa according to a previous study. 17
von Mises stress peak values of the two internal fixation methods.

The conventional open pedicle internal fixation prototype showed elevated peak stress across three-dimensional maneuvers compared with percutaneous pedicle internal fixation, which suggested superior structural rigidity in the former. In percutaneous pedicle screw stabilization, peak von Mises stress was high in the upper screw tail (292.09 MPa), while in open pedicle screw fixation, it was 195.35 MPa at the transverse connector. During flexion, the stress on the screw of open internal fixation surpassed that of percutaneous pedicle screw fixation. In contrast, the screw stress of open internal fixation was inferior to percutaneous pedicle screw fixation during extension, left/right bending, and left/right rotation motions. The maximum stress exerted on the transverse connector during axial rotation of open internal fixation was 880 to 950 MPa, which exceeded the yield strength of titanium alloy metal. This finding suggested that frequent lumbar axial rotation activities could heighten the stress on the transverse connector, escalating the risk of fatigue fracture at the transverse connection.
Examination of maximum displacement in two pedicle screw rod configurations
We examined the peak displacement of both pedicle internal fixation prototypes under mechanical loading (Table 4). We found that displacement of percutaneous pedicle fixation during flexion, extension, and left/right bending was approximately equivalent to that of standard open pedicle fixation in all six movement directions of the lumbar spine model. The maximum displacement of open pedicle internal fixation during left and right rotations was inferior to that of percutaneous pedicle internal fixation during these maneuvers. This finding suggests that owing to the transverse connector, open pedicle internal fixation effectively constrains the axial rotation displacement of the vertebral body, thereby enhancing torsional stability of the internal fixation construct.
Maximum displacement of the vertebral body after implantation with the two internal fixation methods.

Discussion
This study used the finite element method to examine variations in motion and stress in varying states of activity after minimally invasive and traditional open pedicle screw placement for L1 vertebral fracture stabilization. Finite element analysis is an effective way to simulate the intricate spinal mechanical system and provides a reference for clinical planning of pedicle screw placement strategies. In all three-dimensional movement directions, the open pedicle fixation system showed maximum stress that was higher than its percutaneous counterpart. With axial spinal rotation, von Mises stress on the traditional open pedicle screw was considerably lower than that with percutaneous pedicle fixation. However, peak stress was elevated at the transverse connection with traditional open pedicle fixation. Furthermore, traditional open pedicle fixation showed less maximum displacement than percutaneous pedicle internal fixation.
Numerous researchers have accomplished promising clinical outcomes through short segment internal fixation after posterior pedicle internal fixation for managing thoracolumbar fractures. This technique is effective in preserving typical spinal motion unit mobility, minimizing spinal motion segment loss, and enhancing spinal range of motion. Short segment internal fixation has advantages compared with long segment internal fixation. However, in burst fractures showing severe instability, long segment fixation is recommended because of inadequate structural rigidity in short segment fixation, rendering it unable to sustain spinal stability after major instability. 18
In recent years, advancements in minimally invasive spinal surgery have led to a comparable clinical effectiveness of percutaneous pedicle screw internal fixation versus open pedicle internal fixation for treating thoracolumbar fractures without nerve injury. Percutaneous pedicle screw fixation is being rapidly adopted by spine surgeons for its benefits, such as reduced surgery duration, bleeding, trauma, and hospitalization, and a faster return to daily living.19–22 In open pedicle screw systems, the transverse connector is a vital component. The role of the transverse connector in spinal internal fixation remains controversial. Dhawale et al. 23 suggested that clinically using transverse connectors does not provide anticipated advantages in biomechanical assessments. Limiting transverse connector use may not only reduce costs but also decrease postoperative infections. However, Viljoen et al. 24 showed that transverse connectors can enhance spinal axial rotation stability.
In this analysis, an L1 vertebral burst fracture finite element model was developed on the basis of an Angola classification A3 fracture with a thoracolumbar injury severity score of 4 to 5. After development of the model, two distinct internal fixation approaches were established. The finite element technique was used to load the model and evaluate the biomechanical effects of both pedicle arch root internal fixation systems. Comparison of the two fixation strategies showed approximately equal maximum displacement for anterior flexion, posterior extension, left curvature, and right curvature between conventional and percutaneous pedicle fixation. The maximum displacement from left and right rotations was lower in open pedicle fixation than in percutaneous pedicle fixation. These findings are in agreement with other researchers who consider that transverse connectors can improve axial rotation stability with a minimal effect on lateral flexion and flexion-extension. 24
In our study, open pedicle internal fixation with transverse connectors showed substantially larger maximum stress across three-dimensional movements than percutaneous fixation, which indicated stronger structural rigidity. Moreover, open surgery screw stress was lower than minimally invasive screws during movements, such as extension, left/right bending, and left/right rotation, especially axial rotation.
Some limitations should be considered in this study. Computational modeling is a useful tool for spinal biomechanics, and can be used to create the spinal finite element model. However, a lack of quantitative data available for building computational models is the primary limitation hindering model development because it is based on in vitro studies, which lack empirical data, and it does not account for the multitude of factors that may affect cellular activity. Furthermore, other factors, such as the viscoelastic behavior of disc fibers and ligaments, dynamic material properties, and complex muscle interactions, can also affect accuracy of the model. 25 Garay et al. showed that, across all levels of the cervical spine, sex can have an effect on bone density and volume. 26 Age and the position of the vertebral body itself, such as lateral–posterior regions of the vertebrae, surgical fixation of the posterior elements, and the posterior portion of the vertebral body, can affect bone density. All the above-mentioned factors can cause certain errors in the stress analysis after modeling.
Conclusions
Computational modeling is a powerful tool to study complex biological systems and is gaining in popularity in the scientific community. Computational modeling has the advantage of being able to predict changes in the in vivo environment of the spinal disc without the costly, time intensive, and extremely difficult, if not impossible, task of direct measuring. Furthermore, computational analysis allows for more precise control and testing of individual parameters, which can lead to a better understanding of the complex interplay of numerous factors in lumbar vertebral fractures.
The transverse connector binds the screws and rods bilaterally into an “H”-shaped structure, forming an effective three-dimensional fixation device. Consequently, forces from the upper spine can be evenly distributed through this H-shaped fixation, considerably reducing concentration of stress. This reduction may minimize the risks of pedicle screw and rod breakage. Open pedicle internal fixation also produces peak stresses of 891.7 MPa and 886.34 MPa at the transverse connector during left and right spinal rotation, respectively. The regulatory yield strength for Ti-6Al-7Nb alloy spinal implants is 880 to 950 MPa, indicating that the peak stresses generated during axial rotation are within the titanium alloy yield limits. 27 Therefore, frequent future lumbar axial rotation could increase stress at the transverse connector, elevating fatigue fracture risks at this location.
The main difference between the two modes of fixation used in this study is the presence of a transverse connection, and increasing the transverse connection may enhance the axial stability of the pedicle screw and the maximum pulling force of the screw. In the clinical setting, in patients with thoracolumbar compression fractures, strong internal fixation is required to promote fracture healing when the fracture is not healed, and patients are not recommended to remove this fixation early or reduce lumbar mobilization. During axial spinal movements, high peak stress is observed at the transverse connection. Therefore, patients should avoid excessive axial rotation of the spine during recovery. Although there was no broken pedicle screw in our experiment, the transverse connection will increase the stiffness of the whole internal fixation system, thus reducing its toughness, and there is a risk of a long-term broken screw. In clinical practice, when there is a thoracolumbar compression fracture, fracture healing takes 3 to 4 months. We recommend using a transverse connection as long as possible, and it should be avoided in the early postoperative period to prevent loosening of the internal fixation device.
Footnotes
Acknowledgements
We thank Chunbo Huang and Zepei Zhang for revising this work. We also thank Home for Researcher for language editing.
Author contributions
PPM was the principal investigator, conceived and designed the study, collected the data, analyzed the data, and wrote the manuscript. PPM participated in data analysis and discussion of results, and revised the manuscript. ZYL, JM, and XZ participated in discussion of results and revised the manuscript. TL supervised the work and revised the manuscript. All authors approved the final manuscript.
Data availability
The data are available from the corresponding author upon reasonable request.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was supported by a grant from the Science and Technology Bureau of Zhangjiakou, Hebei Province (2021061D).
