Abstract
Metastasis to the mandibular condyle and cervical spine in oncologic patients is rare, and clinicians should therefore be alert if patients present with such suspicious lesions for further clinical and pathological examinations. A 58-year old female patient with uterine cervical cancer initially presented with mild left condylar dysfunction. CT-imaging revealed a progressive osteolytic lesion of the left condyle and at the same time CT-scans revealed an osteolytic lesion of the cervical spine. Further metastatic bone lesions were ruled out. An incisional biopsy of the left condyle revealed metachronous metastasis from the uterine cervical carcinoma. Based on clinical and radiological examinations the patient underwent surgery with total alloplastic replacement of the temporomandibular joint (TMJ) and in a second surgical approach stabilization of the cervical spine. Suspicious symptoms with TMJ dysfunction in conjunction with osteolytic lesions of the maxillofacial skeleton in oncologic patients should be addressed quickly to prevent further diagnostic delay. Surgical resection of metastatic lesions should be considered as a palliative treatment option in selected patients.
Introduction
Metastatic lesions to the oral cavity and maxillofacial skeleton are rare comprising about 1% of all oral malignancies. 1 –4 Such metastatic lesions usually develop at the end stage of cancer and may complicate the further clinical course of the malignancy. 5
The diagnosis of a condylar metastasis can be rather difficult because of unspecific clinical and radiological findings. Symptoms such as pain, trismus, swelling, and occlusal dysfunction are often reported although not conclusive. 6 Therefore, such symptoms need adequate attention in particular in patients with a known history of a malignant tumor. 7
Early detection and treatment of metastatic lesions to the jaw bones may improve the quality of life (QoL) of patients and prolong survival. Dentists and maxillofacial surgeons have an important role in the diagnosis and management of cancer patients, in particular in patients with undiscovered malignancy. 1
We report an unusual rare case of metastatic uterine cervix cancer with simultaneous metastatic bone lesions of the mandibular condyle and cervical spine. Based on imaging and pathological findings, both metastatic lesions were surgically removed successfully. Functional reconstruction of the condyle was achieved using an alloplastic temporomandibular joint (TMJ) stock prosthesis. Our case report highlights the importance and need for close interdisciplinary management of cancer patients within the multidisciplinary tumor board.
Case Report
In February 2019, a 58-year-old female was referred to the Department of Oral and Maxillofacial Surgery of the Academic Teaching Hospital Bremerhaven, Germany, complaining of slowly progressive swelling and pain in the left TMJ. Her clinical history revealed uterine cervix cancer diagnosed in February 2018. The cancer stage was IVB according to the International Federation of Gynecology and Obstetrics. The patient underwent surgical removal of the tumor, including hysterectomy, paraaortal and pelvine lymphadenectomy, and total peritonectomy. The histological diagnosis was gastric-type endocervical mucinous adenocarcinoma. Postoperatively, the patient received 4 cycles of adjuvant chemotherapy with carboplatin and paclitaxel. In May 2018, a recurrent adenocarcinoma with infiltration of the bladder wall was diagnosed and treated with radiation therapy up to 66.4 Gy and simultaneous cisplatin. After treatment completion, the patient was followed up with regular visits with her oncologist.
On physical examination during her first presentation at the Department of Oral and Maxillofacial Surgery, she complained of local pain in her left TMJ. The patient had no facial asymmetry or mandibular deviation. However, she demonstrated light trismus with an interincisal mouth opening of 28 mm. Panoramic radiography and computed tomography (CT) revealed an osteolytic lesion of the left mandibular condyle (Figures 1 and 2). Furthermore an osteolytic lesion of the cervical spine (C5) was diagnosed (Figure 3). Both lesions were highly suspicious of bone metastasis of a uterine cervix carcinoma. Subsequently, a 99mTc-scintigraphy was performed and ruled out further osseous lesions. In March 2019, an open biopsy of the left mandibular condyle was performed and confirmed that the lesion as metastasis originating from the uterine cervix cancer. Subsequently, a partial mandibular resection and condylectomy with immediate alloplastic reconstruction of the condyle and fossa using an alloplastic TMJ stock prosthesis (Zimmer Biomet Microfixation, Warsaw, IN, USA) was performed in April 2019 using a combined retromandibular and preauricular approach. The postoperative course was uneventful, and the patient was referred to the Department of Orthopedic and Trauma Surgery for further treatment of the metastatic C5 lesion. Due to progressive osteolysis of the cervical spine, a lateral cervical surgical approach with corporectomy C5, cervical discectomy, and replacement of C5 with titanium mesh cage reconstruction (VBR-S, Trabecular Metal Material, Zimmer Biomet, Warsaw, IN, USA) and ventral fusion of C4/C6 was performed in May 2019. Postoperative panoramic radiograph and CT scan of the cervical spine showed adequate reconstruction of both the left condyle and C5 (Figures 4 and 5). The total treatment was well tolerated with no mandibular dysfunction. Following hospital discharge, the patient continues her regular oncological follow-up during which abdominal CT revealed progressive retroperitoneal lymphnode metastasis. Following further discussion within the multidisciplinary tumor board (MDT), the patient underwent palliative radiotherapy of the left condyle as well as cervical spine C4/C6 up to 38 Gy, followed by chemoradiation of paraaortal lymphoma with gemcitabine/oxaliplatin and radiation up to 50 Gy. In the further clinical course, there was no evidence of further osseous metastases, but there was further retroperitoneal tumor progression, in which the patient died in December 2019.
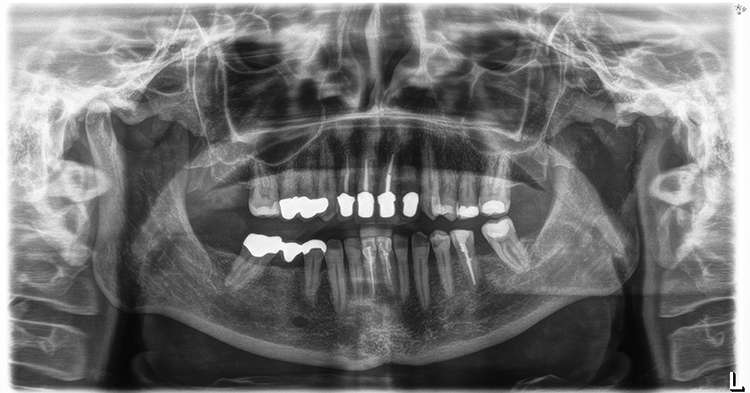
Panoramic radiograph shows osteolytic lesion of the left condyle and coronoid.
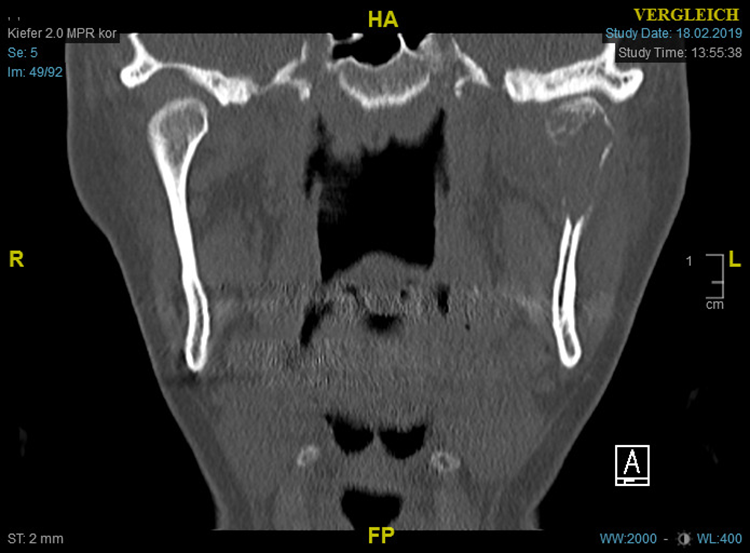
Coronal CT scan shows large osteolytic lesion of the left condylar head process.
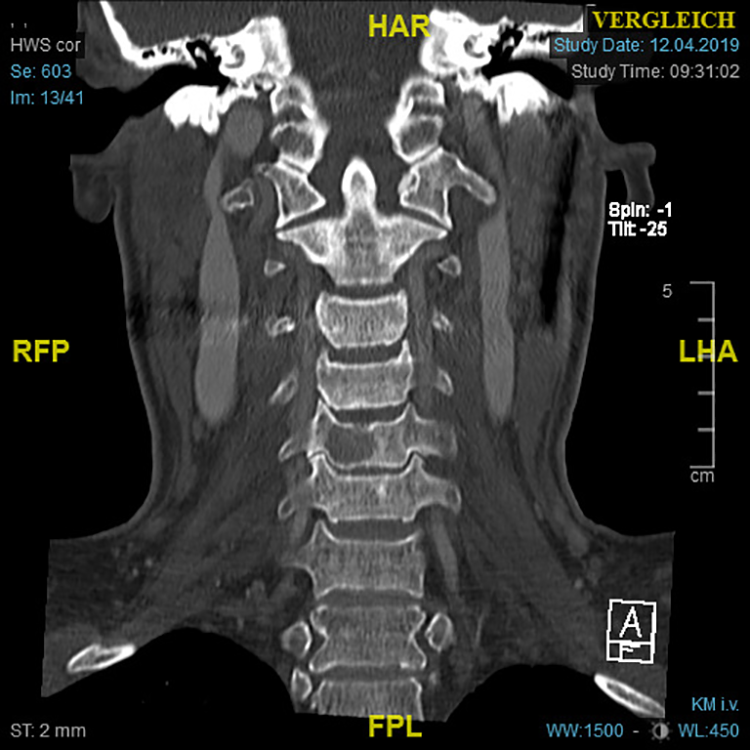
Coronal CT scan of the cervical spine shows an osteolytic lesion of C5.
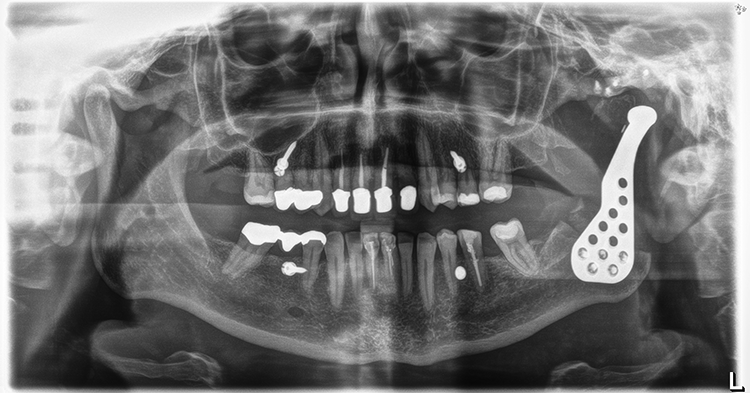
Postoperative panoramic radiograph with alloplastic reconstruction of left temporomandibular joint and glenoid fossa.
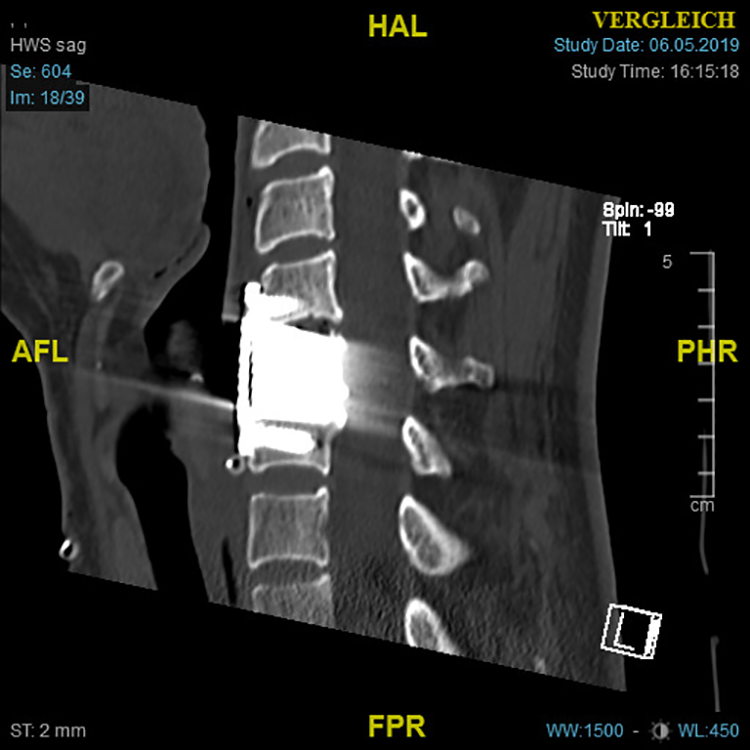
Postoperative sagittal CT scan of the cervical spine with fusion between C4/C5 and vertebral body replacement (VBR-S, Trabecular MetalTM Material, Zimmer Biomet) of C5.
Histological Examination
All surgical specimens were subjected to hematoxylin and eosin staining as well as selected immunostaining for CK-7 and CK-5/6.
The histopathological investigation of both lesions revealed differently differentiated tumor infiltrates of both adenocarcinoma and squamous cell carcinoma (Figure 6).
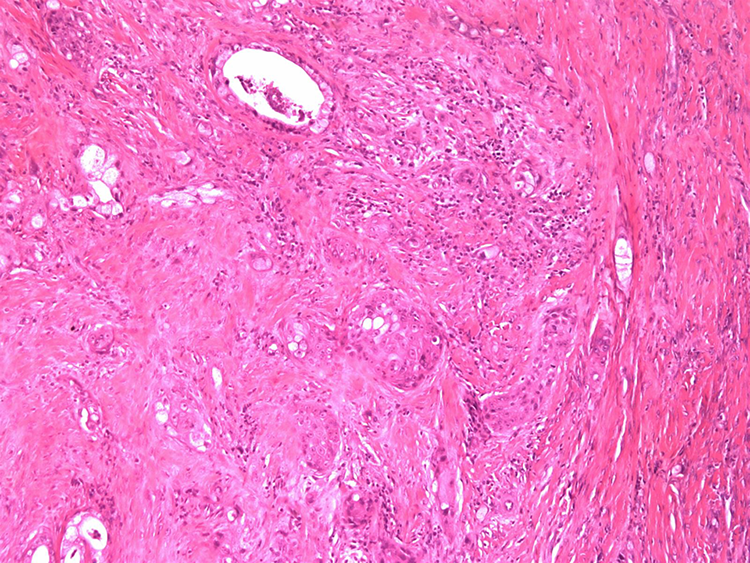
Soft tissue taken from the left mandibular condyle with differently differentiated tumor infiltrates (hematoxylin–eosin 100×): Adenocarcinoma in upper, squamous cell carcinoma in lower half of the image.
Further immunohistochemical double staining (CK-7 and CK5/6) of tumor tissue confirmed adenocarcinoma and squamous cell carcinoma (Figure 7).
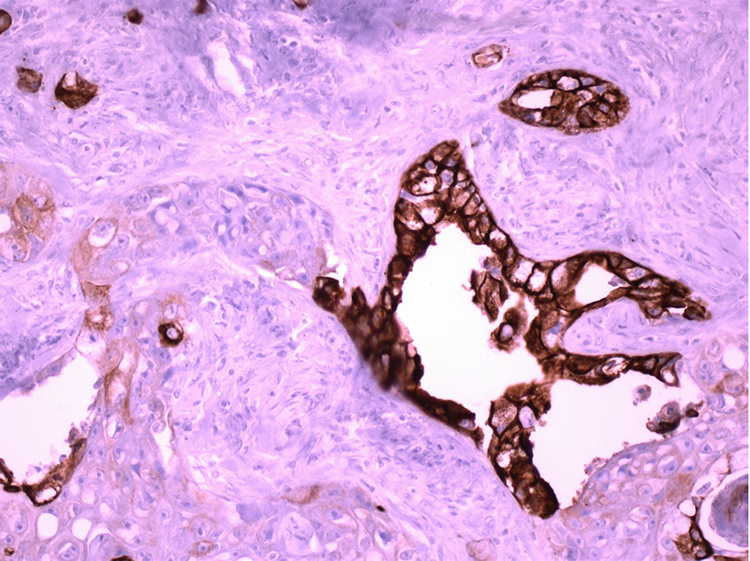
Tumor tissue (immunohistochemical double staining, 200×) with adenocarcinoma (cytokeratin 7-positive, brown color reaction) and squamous cell carcinoma (cytokeratin 5/6-positive, red color reaction.
Similar histological features were demonstrated in the specimen from the cervical spine.
Discussion
Metastatic tumors of the oral and maxillofacial region and in particular of the temporomandibular joint are rare. 8 –10 Nearly 1% of all oral and maxillofacial malignant tumors involve metastatic lesions from solid tumors of other parts of the body. 3
In a recent comprehensive review of 453 patients with metastatic lesion in the jaw bones, the majority of metastatic lesions were found in the mandible (73.7%), and the temporomandibular joint and condyle were affected in 8.1%. 3 Interestingly enough the diagnosis of a metastatic lesion was the first sign of malignancy in 125 cases (27.6%).
Metastasis to the condyle mostly originate from tumors of the breast, uterus, rectum, and melanoma. The exact mechanism of the low incidence of metastatic lesions in the condyle is not well understood, however it might be due to the deficiency of bone marrow and isolated blood supply from the maxillary/temporal artery.
The diagnosis of metastatic lesions of the TMJ can be rather difficult because clinical and radiological signs are often unspecific. Trismus, pain, soft tissue swelling, and occlusal disturbances may occur, therefore such symptoms are frequently misdiagnosed as TMJ myoarthropathy. In cases of simultaneous TMJ complaints and presence of malignant disease, the clinician should consider a differential diagnosis of TMJ metastasis. 8 –10
Overall, bone metastasis to the maxillofacial skeleton is a rare but complicating condition during the clinical course of the cancer disease. Breast and prostate cancer are often reported and less frequently cancer of the lungs, liver, and kidneys. The uterine cervix as the primary site is rarely reported in the literature. 11
Such unusual sites of distant metastatic involvement are clavicle, scapula, fibula, tarsal and metatarsal bones, and extremely rarely to the jaw bone and cervical spine. 12 The bony spine is overall the third most common site for distant cancer metastases, with the cervical spine involved in approximately 8% to 20% of metastatic spine disease. 13 Management of patients with cervical spine metastases is controversial due to limited information and inconclusive results. In a recent review article, 24 patients with cervical spine metastasis underwent palliative surgical treatment. 14 Overall, 21 patients experienced complete or almost complete pain relief. The authors concluded that appropriate patient selection of the surgical technique is mandatory. 14 Metastatic lesions to the maxillofacial skeleton may be a therapeutic challenge for the clinician, since such lesions are often detected in an end stage of the disease. Primary tumor site and the extent of metastatic spread are the most important facts to predict prognosis and treatment planning. 15 According to most clinicians, the metastatic lesion should be treated by radiation, chemotherapy, surgical resection, or in a combined modality approach.
Therefore, it is of major importance to discuss available treatment options both with the patient and their family and within the MDT. In case of early detection of jaw metastasis, immediate treatment, including surgical approach, offers a chance to improve QoL of patients and prolong survival. Apart from oncological diagnosis of the patient, she was in a good general health condition, and therefore, the patient was offered palliative surgery for both metastatic lesions of the left condyle and cervical spine to be followed by adjuvant radiotherapy of the involved regions.
In summary, our case report emphasizes that palliative treatment can be effective and helpful in reducing pain and tumor size and allows to preserve oral/mandibular function for the remaining life span.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Patient Consent
Written informed consent was obtained from the family of the patient.
