Abstract
Aims and Objectives:
The aim of this case series is to retrospectively analyze cases of masseter muscle hypertrophy and the surgical procedures carried out for their treatment in SDM craniofacial unit, Dharwad. The main objectives taken into account are the adjunctive procedures such as genioplasty and coronoidectomy, which help improve the esthetics and mouth opening of the patients postoperatively.
Materials and Methods:
This retrospective case series was conducted in the Department of Oral and Maxillofacial Surgery, SDM craniofacial unit, Dharwad, from 2010 to 2015. A total of 5 cases were operated on during this period. Orthopantomograms, computed tomography scans of the head and neck region, and lateral cephalograms of each patient were taken into account. Data were collected to study the treatment protocols and the adjunctive procedures, which helped improve the results of the surgery.
Results:
Of the 5 patients operated in the last 5 years, surgical debulking of the masseter muscle was the optimal treatment followed with genioplasty, which provided improved esthetics from the square-shaped jaw appearance. Coronoidectomy was helpful in increasing mouth opening in patients with trismus.
Conclusion:
The case series was not only carried out to enunciate causes of masseter muscle hypertrophy and its complications but also to discuss optimal treatment protocols along with adjunctive procedures to enhance the postoperative results and patient satisfaction.
Introduction
Masseter muscle hypertrophy (MMH) is an abnormal enlargement of the masseter muscle, either unilaterally or bilaterally characterized by an increase in the volume of the muscle mass. 1 It is a rare, benign, generally asymptomatic condition with no gender predilection and with a high incidence of occurrence in second and third decades of life. First described by Legg in 1880 as a concurrent idiopathic MMH case in a 10-year-old girl, 1,2 it has ever since been a subject of discussion as it has no known etiology except for a few contributing factors cited such as bruxism, malocclusion, clenching, temporomandibular joint (TMJ) disorders, emotional disorders (stress and nervousness), and so on. 1 –4
The masseter is a thick trilayered quadrilateral shaped muscle of mastication whose action is to elevate the mandible to bite; hence its hypertrophy leads to function impairment such as trismus, protrusion, and bruxism. 1,2 A clinician is majorly consulted for aesthetic reasons as it causes an alteration in facial lines, asymmetry of the face, and prominence of the angle of the mandible, 1 hence decisive surgeries like coronoidectomy and genioplasty can be considered along with surgical debulking of masseter muscle.
Its differentiation from other diagnoses such as oral submucous fibrosis, parotid inflammation and tumors, lipoma, benign or malignant muscle and mandibular tumors, and vascular tumors is based on clinical examination and the use of imaging modalities such as conventional radiographs, computed tomography (CT), and ultrasonography, which aid in the diagnosis of the condition. 4
Materials and Methods
The group of patients, who were considered for the surgical debulking of masseter muscle, consisted of 4 female patients and 1 male patient with an average age of 22.6 years. On an average, MMH was noticed 4.1 years prior to surgery.
In all the 5 patients, the reason for surgical correction was chronic pain, trismus, and esthetics in the form of facial asymmetry. The hypertrophy was bilateral in 4 patients and unilateral in 1 patient—on the left side. None of the patients had temporal headaches or tension sensation on opening his or her mouths. We could not find any etiological factors responsible for the hypertrophy in any of the patients.
All the patients who reported to our craniofacial unit from 2010 to 2015 came with a complaint of inability to open their mouths properly since 5 to 6 years. They elucidated being all right 5 years ago when they noticed gradual inability to open their mouths. None of them were able to recall any kind of injuries to the face at that time or any ear infection. Mild pain was present if they tried to open their mouths wide, associating it with bilateral pain in front of the ears. Patients were devoid of any medical histories in favor of systemic illnesses, drug allergies, or psychological disorders. Extraoral examination revealed bilateral enlargement over the lower one-third of their faces. The average preoperative mouth opening for all patients was 1.5 cm. There was reduced lower facial height with retruded mandibles. Mild hyperexostosis of the angles of the mandible bilaterally were evident. On palpation, TMJ movements were present bilaterally. Intraoral examination showed a full set of teeth present with palpable masseter bulk bilaterally, which was slightly tender on palpation. Class II division 1 malocclusion was present with increased overjet and overbite. No abnormality was detected in relation to the buccal mucosa, tongue, or lips of any of the patients.
Preoperative orthopantomograms and CT scans of the face were recommended to the patients along with ultrasonography of the masseter muscles as an adjunctive radiographic tool. Orthopantomograms revealed prominent angle of the mandible bilaterally with increase in the width of the ramus. Bony spurs were evident bilaterally. All the 5 patients presented with impacted wisdom teeth except for 1, who had got his maxillary third molars removed earlier. Computed tomography scan revealed hypertrophy of the masseter muscle along with mild symmetrical elongation of the coronoid processes of mandibles on both the sides. The lateral cephalograms also revealed mild deficiency of lower half of the face in the anteroposterior dimension.
Our treatment protocol included surgical debulking of the masseter muscle, bilateral angle osteoplasty, bilateral coronoidectomy, advancement genioplasty, surgical extraction of impacted third molars, and aggressive physiotherapy postoperatively.
Postoperative assessment of pain, facial symmetry, mouth opening, and chin projection was eventually carried out.
Technique
The surgery for MMH was done under general anesthesia with nasotracheal intubation. Local anesthesia with adrenaline (1:200 000) was infiltrated along the proposed incision line bilaterally. An intraoral incision was made extending from mid ramus level to the third molar and a vestibular incision to the premolars to expose the entire length of the masseter muscle. Careful subperiosteal dissection was carried out, followed by surgical extraction of impacted third molars. Attachment of temporalis muscle was stripped from anterior border of ramus, and sufficient retraction was achieved using coronoid retractor. Deep belly of masseter was identified and stripped from superficial belly. Care was taken to avoid damage to facial artery and vein. The lateral attachment was then identified and using a cautery, muscle belly was incised and separated from superficial belly. A similar procedure was carried out on the contralateral side along with extraction of impacted third molars.
Bilateral coronoidectomy was then carried out by holding the coronoids individually with Kocher’s forceps and making an osteotomy cut extending from sigmoid notch to anterior border of ramus which was followed by extraction of maxillary third molars. Flaring hyperostosis was noted along the mandibular angle, which was approached using the same incision. A channel retractor was used to expose the flare, and the spur was marked by a straight fissure bur. Using an angular oscillating saw, the prominence was then osteotomized followed by smoothening of sharp margins using Rossete bur. A similar procedure was performed on the contralateral side.
Advancement genioplasty was then performed using an intraoral vestibular incision. Subperiosteal stripping of soft tissue was carried out to identify the lower border of the mandible. After marking the midline with a number 701-fissure bur, genioplasty osteotomy was done using an oscillating saw. The osteotomy segment was advanced vertically and anteroposteriorly and stabilized with chin miniplates. The osteotomy gap was packed with the osteotomized coronoid process using bur holes to maintain bone-to-bone surface contact. Pressure bandage or dynaplast was placed over the angle regions bilaterally to prevent hematoma formation.
Results
Chronic pain was one of the major factors assessed postoperatively using the Visual Analog Scale (VAS). Of the 5 patients, 3 returned for their first follow-up after a month with a complaint of mild pain in the posterior tooth region. They were put on analgesics and asked to return after 6 months. They returned for a second follow-up with no fresh complaints and the wound healing was satisfactory.
Facial asymmetry was also one of the trivial complaints of the patients. Postoperatively, all the 5 patients were satisfied with the outcome of the surgery. Surgical debulking helped in regaining the initial symmetry of their faces, to which the patients were highly compliant. The long slender chin projection also added to the aesthetics due to genioplasty, which enhanced the results of the surgery (Figures 1 –3).
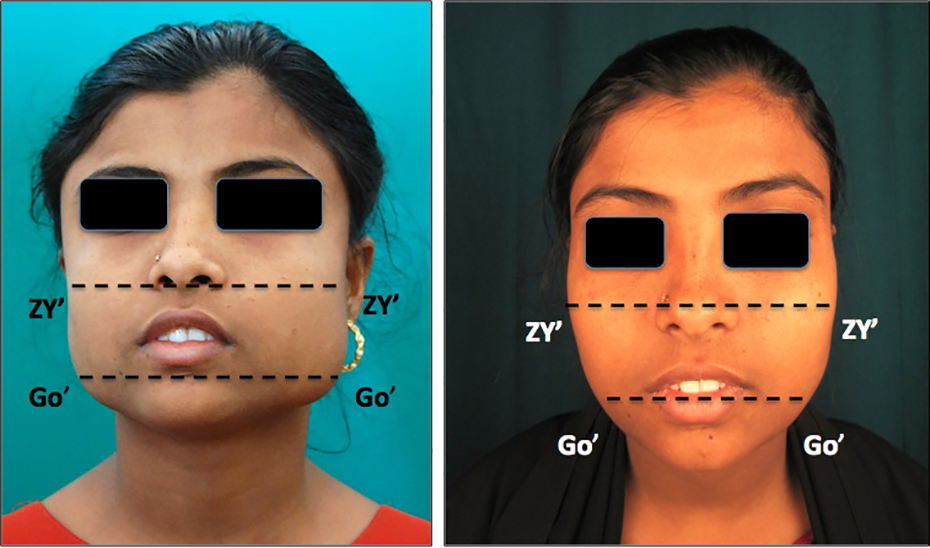
Preoperative and postoperative frontal profile of a patient.
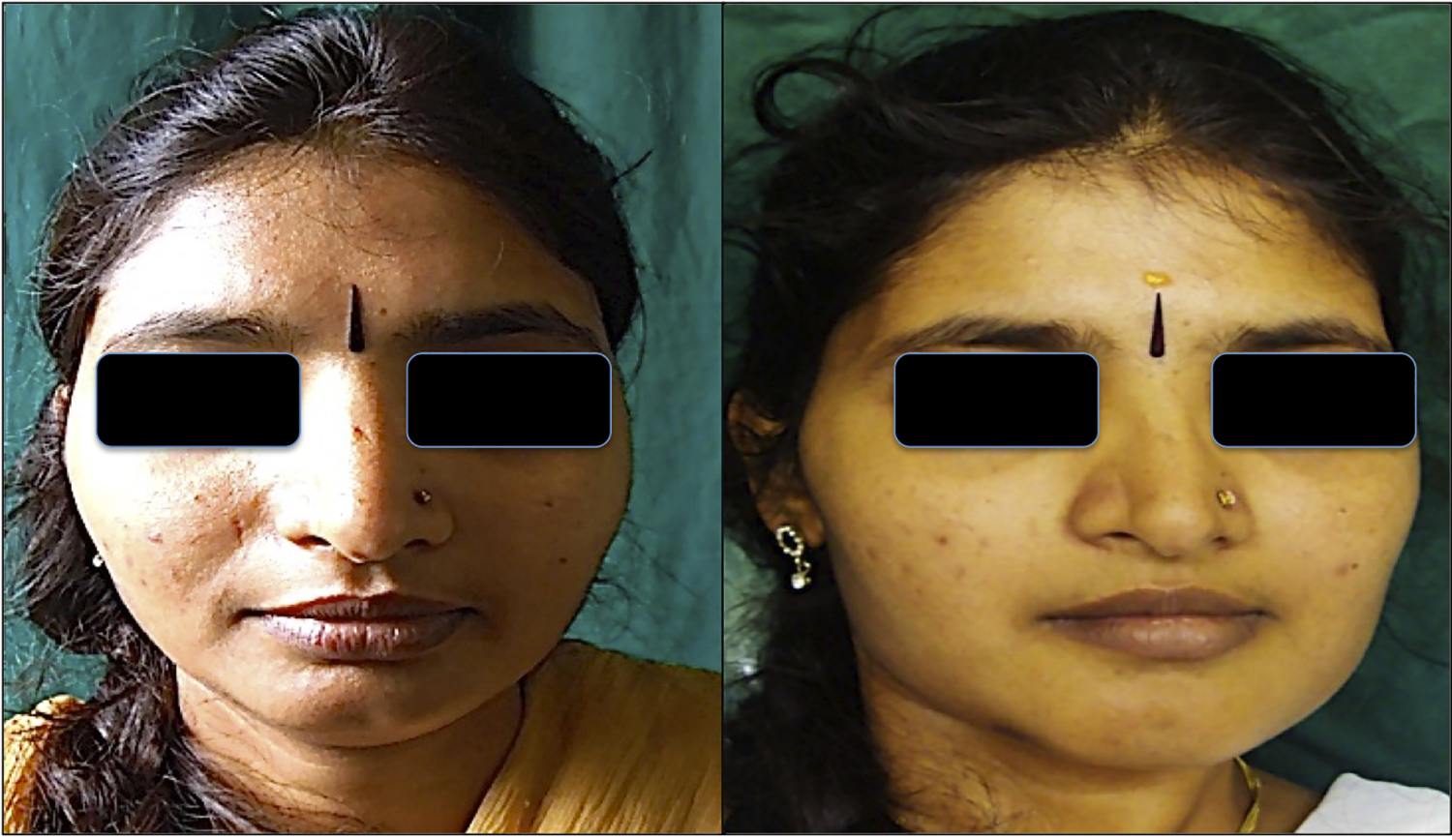
Preoperative and postoperative frontal profile of a patient.
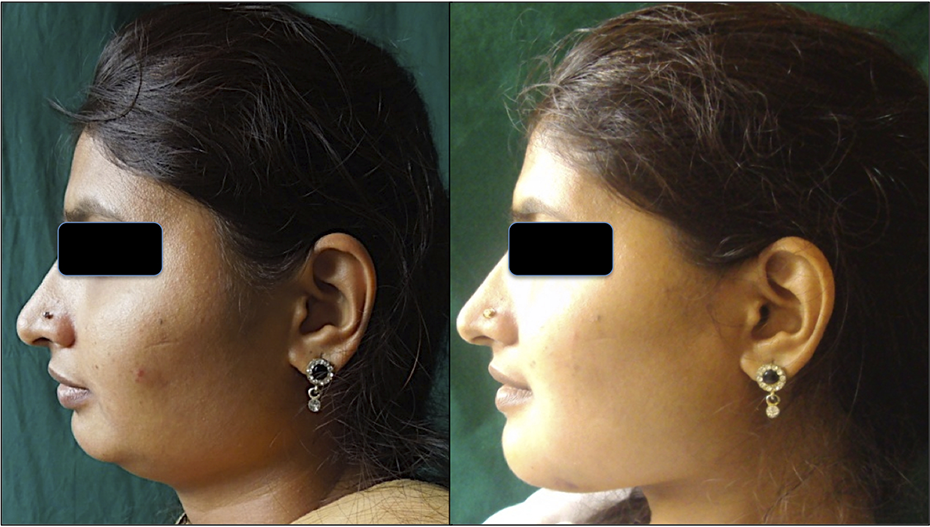
Preoperative and postoperative lateral profile of a patient.
Trismus was also considered postoperatively. The bilateral coronoidectomy helped us to achieve a satisfactory mouth opening from 1.5 to 4 cm. There were no incidences of trismus after surgery and the pressure bandages helped to prevent accumulation of hematoma, which is one of the etiological factors for trismus postoperatively. All our 5 patients were satisfied with the active and passive mouth opening and were put on physiotherapy regimen to maintain it adequately (Figure 4). None of our patients had any immediate significant postoperative complications or complaints.
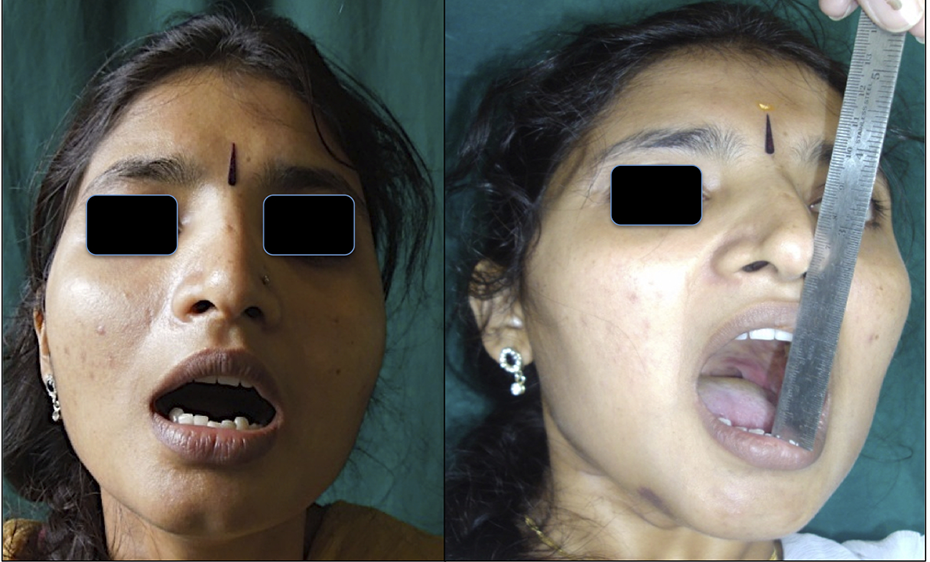
Preoperative and postoperative mouth opening.
Discussion
Masseter muscle hypertrophy is considered to be a rare phenomenon with an unknown cause. The factors most affected are aesthetics and functioning of the muscle resulting in patients presenting with trismus 5 and a poor cosmetic appearance of the face. The characteristic rectangular or square-shaped facial configuration results due to hypertrophy of the masseter muscle thickness, which lies along the inferior portion of the mandibular ramus, where the facial contour normally tapers. 1 –4,6 In our study, all the 4 patients complained of trismus and square-shaped configuration of the face. None of them had severe pain, temporal headache, or sensation of tension in jaws as was evident in several other studies also. 6 –9
The etiological association of this disorder with defective teeth, habit of chewing gum, TMJ disorders, congenital or functional hypertrophies, and psychological stresses is very common. According to Teixeira et al, there are 2 types of MMH: congenital or familial and acquired due to functional hypertrophy. 10 However, in our patients, none of them could recall any kind of injury, functional disparity, any psychological stresses, or any of the above-mentioned etiological factors, which could have been responsible for the hypertrophy. History given in general by all of them was a swelling in the angle of the mandible, which gradually grew in size over a period of 4 to 5 years leading to the impairment.
Orthopantomograms, anteroposterior views of the face, CT scans, magnetic resonance imaging (MRI), and digital palpation of the muscle are some of the ideal methods to diagnose MMH. According to Seltzer and Wang, CT and MRI scans produce excellent images for the diagnosis of various masseter muscle conditions. 11 Digital palpation can be carried out by asking the patient to clench his or her teeth to make the muscle more prominent and then palpating the hypertrophied portion of the muscle using fingers. 2,3 Orthopantomograms and anteroposterior views of the face are optimal in detecting bony spurs in the angles of the mandible. 12 Guggenheim and Cohen proposed that forces exerted on the mandible due to hyperactivity of the masseter muscle lead to periosteal irritation and irregular deposition of bone in the form of bony spurs (Figures 5 and 6).
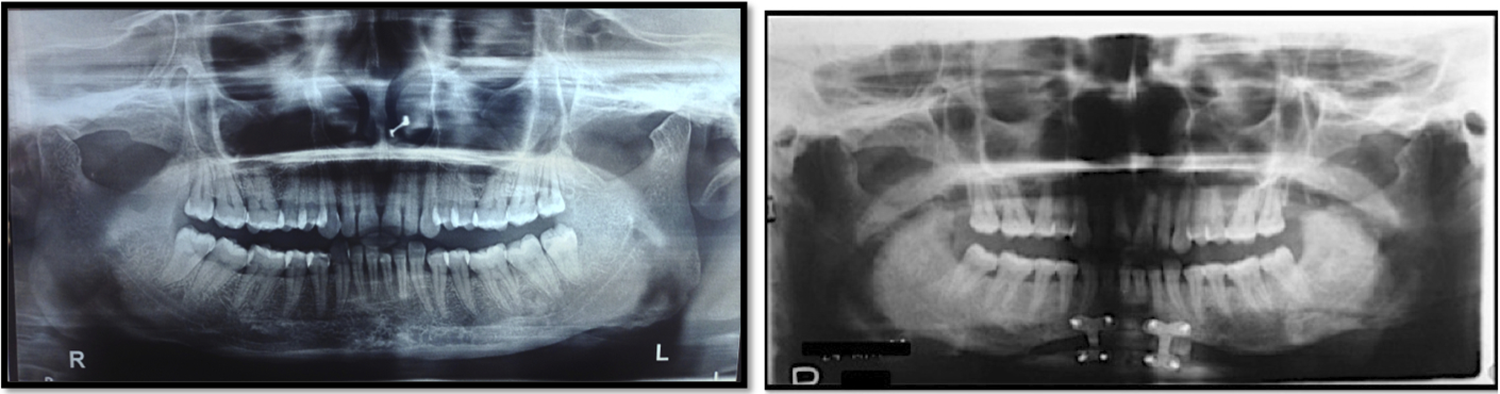
Preoperative and postoperative orthopantomogram.
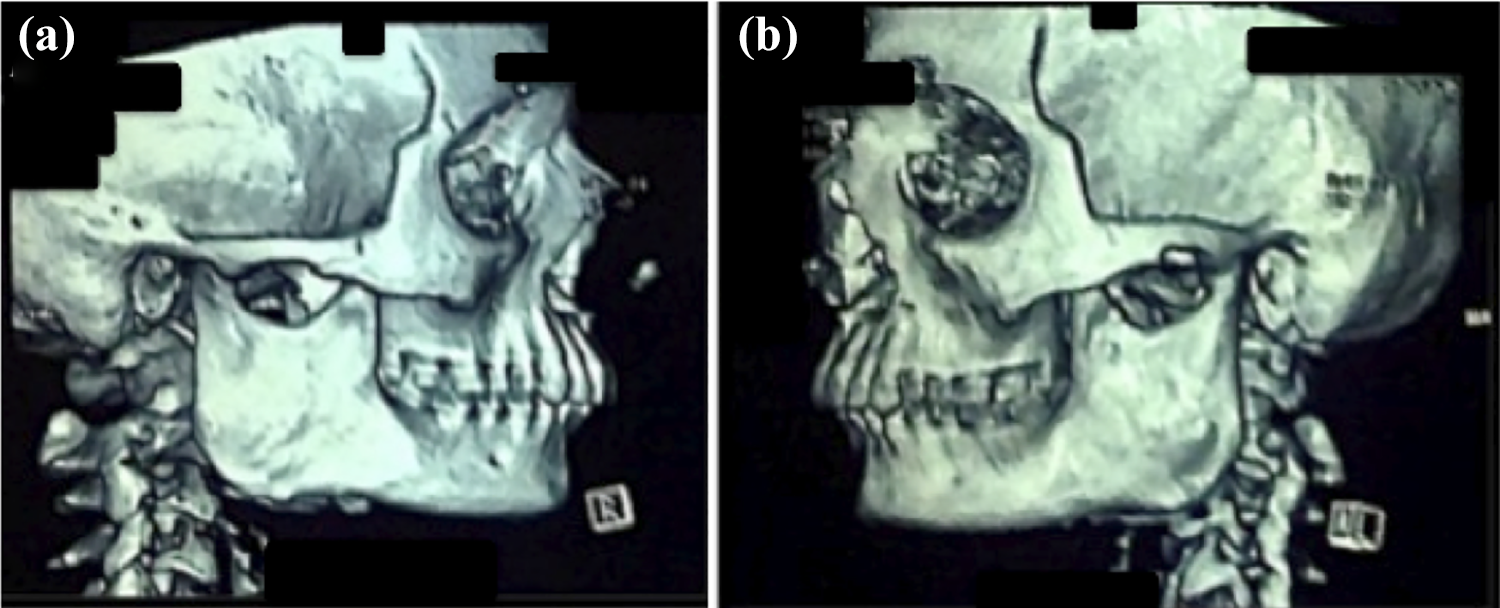
Preoperative CT scan of the face (3D reconstruction). CT indicates computed tomography; 3D, 3-dimensional.
The treatment approaches can be classified into nonsurgical and surgical methods. The nonsurgical methods broadly include psychological counseling, use of mouth guards, muscle relaxants, anxiolytic drugs, analgesics, physical therapy, dental restorations, and occlusal adjustments to correct premature contacts. 6,13 None of these methods were employed for our patients, as they did not have any conditions pertaining to the above-mentioned treatments and there is no reliable report on the literature on the success rates of isolated clinical therapy.
One of the alternative methods for treating maxillary muscle hypertrophy is injecting botulinum toxin type A into the hypertrophied muscle, as first suggested by Smyth 14 and Moore and Wood. 15 It is looked upon as a noninvasive method, which works upon the principle of inhibiting muscle contraction by hindering the release of acetylcholine. 16 This results in paralysis of the muscle leading to “disuse atrophy” and reduction in the muscle volume. However, the disadvantage of this method is the temporary effect of the toxin proceeding to reversion to the original state in about 6 months. 17 Also, botulinum is expensive and needs to be administered multiple times due to its reversible action.
Masseter hypertrophy reduction with radiofrequency coagulator is a safer, less invasive procedure compared to the surgical excision method and a much more long-lasting procedure than botulinum toxin therapy. 18 Introduced first by Powell et al, 19 this method uses radiofrequency energy, which creates resistance that turns to heat within the tissue. This results in heat ranging from 50 to 90°C, which coagulates muscle tissue and forms scar tissue that shrinks the overall volume of involved muscle. Such reduction in muscle volume begins 3 weeks after the operation and continues up to 6 to 8 weeks. However, more studies are needed for long-term efficacy of the procedure.
Various studies have advocated surgical debulking of the hypertrophied muscle along with the removal of hyperostotic areas of the mandibular angle (if necessary) as the primary procedure for the treatment. The debulking procedure is based upon extraoral and intraoral approaches. In our study, all the 5 patients were treated with intraoral approach as the incidence of facial nerve injury is high with the extraoral approach.
The first description of an intraoral approach was published by Ginestet et al. 20 Da Cruz et al believed that the intraoral approach offers lower risk of infection and better cosmetic results. 2 The inner part of the muscle is rich in fusiform muscle fibers so diminishing them will help change the efferent system followed by rearrangement of muscle control. This will also prevent relapse of the hypertrophy. However, unlike Ginestet, we preferred to round off and smoothen the bony spurs in all our patients to enhance esthetics. Surgical treatment by an extraoral approach was proposed for the first time by Gurney, where submandibular incisions were placed and removal of muscle mass was carried out. 21 Adam 22 introduced mandibular angle osteotomy in 1950 and also supported the extraoral approach along with Gelbke 23 and Ginwalla. 24 With the advent of new armamentaria like angular saws or retractors, it is possible to carry out angular osteotomy/osteoplasty intraorally and this would prevent or minimize injury to the marginal mandibular branch of facial nerve. In the 2 case reports presented by Kim and Kameyama, focus was placed more on mandibular angloplasty as a primary treatment protocol followed by supplemental myotomy. 25 However, complete resection of the bony angle increases the chances of damage to the inferior alveolar nerve bundle, which restricts the angloplasty only below the nerve canal. A similar technique was proposed by Wood, which involved resection of only the bony protuberance of mandibular angle without removing any parts of the masseter muscle. 26 Nevertheless, studies put forth by Rispoli et al, 2 Biruktawit Kebede et al, 1 and Shetty et al 27 had a more crucial approach to managing the hypertrophy. They believed in the surgical resection of excessive muscle fibers from the inner third of the masseter vertical muscle fibers and banked on reduction osteoplasty only if bony hyperplasia was present. Excision of the inner layer of the hypertrophied muscle bundle was considered to be a more essential approach as hyperactivity of the masseter muscle was considered to be the key etiology behind excessive bone deposition at the mandibular angle. So, muscular resection was acknowledged as prime followed by mandibular angloplasty, as and when required. Resecting the bone subperiosteally leaves the muscle sling intact, minimizing the possibility of nerve damage. Excessive retraction during the intraoral approach can also damage the nerve. However, we did not experience any nerve damage or any other complications in patients treated with the above-mentioned intraoral approach.
A condition similar to MMH is masticatory muscle tendon-aponeurosis hyperplasia, which presents itself with a hard cord-like structure along the overhang of the anterior border of the masseter muscle on intraoral palpation along with restricted mouth opening. 28 The other features are similar to hypertrophy of the muscle. The standard therapy considered for the management is bilateral coronoidectomy with anterior partial aponeurectomy of the masseter muscle. Coronoidectomy is helpful to relieve trismus as it removes the tendon arising from the posterior and superior aspects of the coronoid process.
Trismus was one of the distinctive clinical features of MMH in our case series; hence coronoidectomy was one of the adjunctive treatment modalities considered in our modus operandi. Impairment of the normal functioning of the muscle has serious health implications such as malnutrition due to impaired mastication, difficulty in speech, and compromised oral hygiene resulting in a functional deficiency of the stomatognathic system. 29 Trismus is a postoperative problem for both extraoral and intraoral surgical approaches as put forth by Adams, 22 Gelbke 23 and Masters et al. 30 Masters et al 30 suggested postoperative chewing exercises prevent the impairment and Beckers recommended expansion exercises. 6 However, the bilateral coronoidectomy carried out for all our patients helped us achieve a satisfactory mouth opening of 4 cm postoperatively from just 1.5 cm preoperatively with no incidences of trismus after the surgery. Mouth opening was maintained even during follow-up with the help of a strict regimen of physiotherapy.
Pain is considered to be the initial etiology for trismus but after 5 to 10 days the replacement of intramuscular hematoma by scar tissue leads to contraction of scar and trismus. 6 Of our 5 patients, 3 presented with mild pain postoperatively, which was evaluated using the VAS. After a follow-up of 6 months, all the patients were relieved of the chronic pain, which they had experienced initially.
Genioplasty can be looked upon as an essential surgery for the enhancement of the esthetics of the patient being treated for masseteric hypertrophy. 31,32 All of our 5 patients were concerned about facial asymmetry in the form of mild retrogenia. The mean value for the distance between Pogonion and Nasion perpendicular to horizontal plane was −7.6 mm and this can be attributed to hyperactivity of the muscle that causes mandible to grow in a horizontal direction rather in a vertical one leading to reduced lower facial height and a rectangular configuration of the face, which projects in the form of a retruded mandible or retrognathia, supporting the theory put forth by Bengt Ingervall and Birgit Thilander in 1974. 33 However, sliding and augmentation genioplasty enables to esthetically correct the deformity by giving a long slender chin and devoiding the necessity of a bilateral split sagittal osteotomy. In our study, all the 5 patients underwent advancement genioplasty in both vertical and anteroposterior direction, which was reviewed with satisfactory esthetics (Figure 7). Photographic evaluation was considered to assess the pre- and postoperative changes seen in the lower facial region of the patients. The intergonial width was evaluated to understand the reduction in the thickness of the masseter muscle from the square-shaped jaw to normal anatomy of the lower face, postsurgery. The preoperative bigonial width reduced from an average of 5.8 to 4 cm after surgical intervention in all our patients.
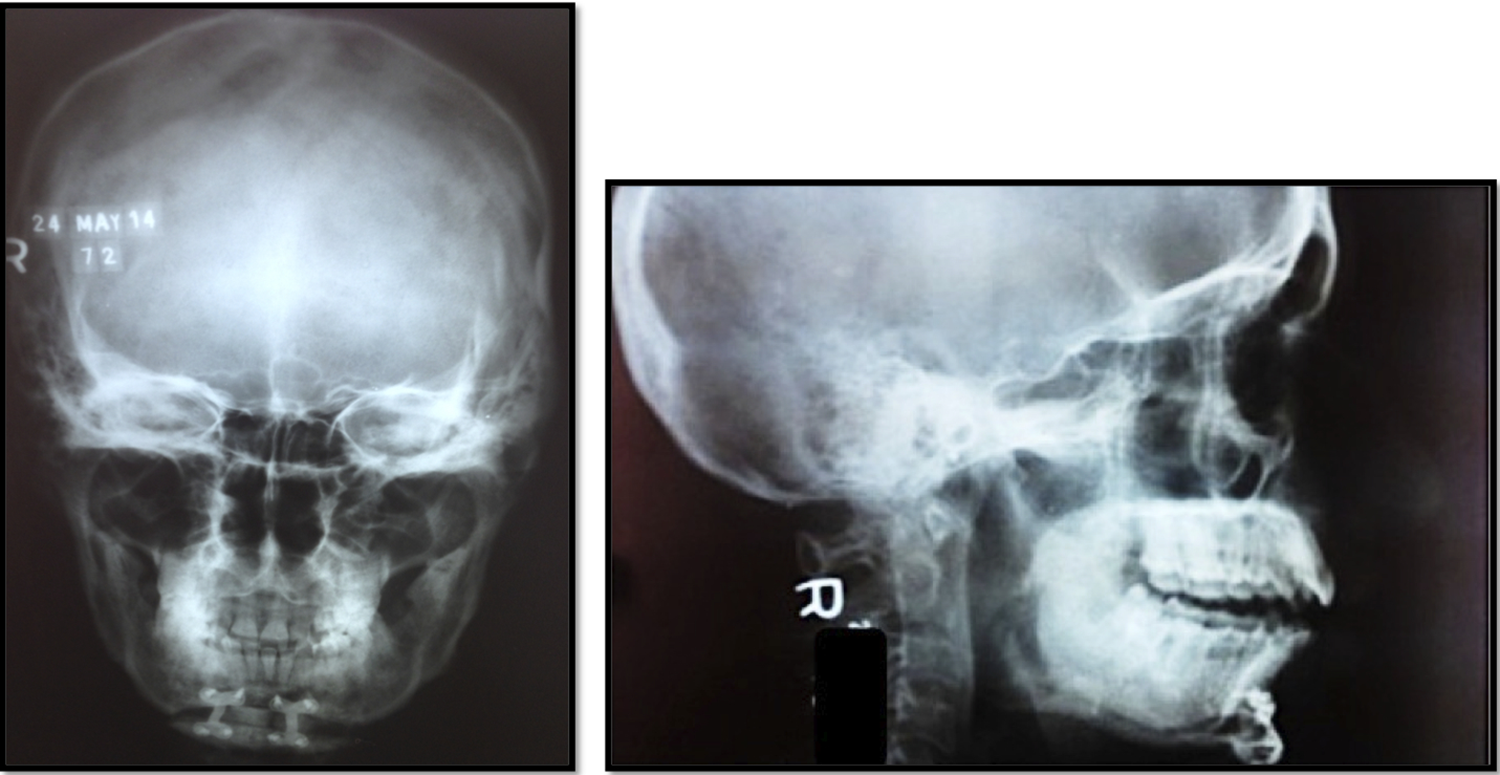
Postoperative AP view and lateral cephalogram. AP indicates anteroposterior.
In our case series, the adjunctive surgical procedures helped in addressing the patients’ complaints of facial asymmetry and functional rehabilitation satisfactorily.
Conclusion
The conclusion, which could be drawn from our study and case reports, is that the factors accountable for MMH are still obscure except for maybe a few contributing conditions. Two of the most trivial complaints of the patients are esthetics and functional impairment, which need to be given prime importance during the surgical intervention. Hence, adjunctive surgical methods such as genioplasty and coronoidectomy should also be taken into consideration along with intraoral approach for debulking of the masseter muscle, in order to augment the postoperative results and patient satisfaction.
Footnotes
Acknowledgements
The authors would like to thank Dr Srinath Thakur, Principal, SDM College of Dental Sciences and Hospital and Dr Niranjan Kumar, Director, SDM Craniofacial Centre for the encouragement and facilities provided.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Clearance
For this type of study, formal consent is not required. This article does not contain any studies with human participants or animals performed by any of the authors. The manuscript was reviewed by Institutional review Board for publication.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
