Abstract
Chronic exposure to uncontrollable stress causes loss of spines and dendrites in the prefrontal cortex (PFC), a recently evolved brain region that provides top-down regulation of thought, action, and emotion. PFC neurons generate top-down goals through recurrent excitatory connections on spines. This persistent firing is the foundation for higher cognition, including working memory, and abstract thought. However, exposure to acute uncontrollable stress drives high levels of catecholamine release in the PFC, which activates feedforward calcium-cAMP signaling pathways to open nearby potassium channels, rapidly weakening synaptic connectivity to reduce persistent firing. Chronic stress exposures can further exacerbate these signaling events leading to loss of spines and resulting in marked cognitive impairment. In this review, we discuss how stress signaling mechanisms can lead to spine loss, including changes to BDNF-mTORC1 signaling, calcium homeostasis, actin dynamics, and mitochondrial actions that engage glial removal of spines through inflammatory signaling. Stress signaling events may be amplified in PFC spines due to cAMP magnification of internal calcium release. As PFC dendritic spine loss is a feature of many cognitive disorders, understanding how stress affects the structure and function of the PFC will help to inform strategies for treatment and prevention.
Introduction
The higher cognitive functions of the recently evolved prefrontal cortex (PFC) are weakened with exposure to stress, reducing top-down regulation and switching control of behavior to more primitive brain circuits. Impaired PFC function can be caused by either a physiological or psychological stress and can occur with even mild, acute psychological stress if the subject feels threatened or out of control. Given the importance of strong PFC function to modern society, these changes are important to understand at the neurobiological level to inform treatment and prevention.
Under optimal conditions, the PFC provides goal-directed regulation of our thoughts, actions, and emotions. 1 PFC circuits expand greatly over brain evolution, and have the special ability to generate and sustain mental representations in the absence of sensory stimulation, the foundation of abstract thought. 2 The PFC generates and sustains goals for top-down control, e.g. filtering out irrelevant operations and enhancing processing of relevant stimuli. These functions are often assessed in the laboratory using tests of working memory, attentional regulation, decision-making and extinction of conditioned fear in both animals and humans.3,4 Research has shown that these PFC operations can be impaired by exposure to either physiological stressors such as hypoxia,5,6 head trauma,7,8 or inflammation, 9 or by psychological stressors, where the subject feels little control over the stressful experience.10–18 The cellular bases for many of these changes are just beginning to be elucidated. However, there are hints that both physiological and psychological stressors may share underlying mechanisms that ultimately lead to the loss of synapses on dendritic spines and the weakening of higher cognitive abilities. Many of these changes are also seen in the aging PFC, 19 where recent data indicate that dysregulation of stress signaling pathways contributes to impaired neuronal firing, loss of synapses, and risk of degeneration with advancing age.20–22 The role of chronic physiological and psychological stressors on the long-term structure and function of the PFC is particularly important given our aging society and the increasing burdens of chronic diseases. The following article provides a review of this important and expanding area of neuroscientific research.
A few notes of caution: The research described in this review utilized a variety of experimental conditions, including different 1) species (mouse, rat, rhesus monkey, human), 2) PFC subregions, 3) layers (III vs. V), and 4) stress paradigms. The PFC expands greatly from rodent to monkey to human, 23 with dorsolateral PFC (dlPFC) and frontal pole regions expanding in primate that are not found in rodents. There are also differences in the organization of the medial PFC (mPFC) between rodents and primates that are particularly confusing to the field, 24 where circuit identification will be needed to clarify apparent discrepancies, e.g. whether a PFC neuron excites or inhibits stress actions in amygdala. There are also differences between in vivo vs. in vitro studies, where cell cultures emphasize developmental events that can differ from in vivo conditions. For example, thin spines are immature in cell cultures, but are mature (and predominate) in primate dlPFC. Studies using in vivo neuronal recordings or calcium imaging can be especially affected by laminar differences. For example, physiological recordings in monkey PFC often focus on layer III Delay cells, while recordings from PFC in rodents often capture layer V cells, as layer V is particularly large in rodent mPFC, while layer II/III is small. Calcium imaging in rodents often focuses on layer I, which contains the dendritic tuft of layer V pyramidal cells, while deeper dendrites are not visible. Much of the rodent research on glutamate actions with chronic stress, including interactions with amygdala and the effects of ketamine, have focused on layer V pyramidal cells and their dendritic tuft in layer I. In contrast, rodent research examining the effects of chronic stress on working memory and attention regulation, and the effects of stress-induced catecholamine release, have focused on spine loss from layer II/III pyramidal cells. As layer II/II mPFC is a replicated site of spine loss with chronic stress in rodents, and deep layer III dlPFC microcircuits are central to higher cognition and a focus of spine loss in schizophrenia and aging, layer III is a particular focus of the current review. However, additional research is needed to better bridge across species and circuits, as we are already learning that stress effects are circuit specific. 25 In humans, chronic stress exposure is associated with reduced gray matter volume in dlPFC, 26 and mPFC 27 and spine loss from the orbital PFC. 28 We have little knowledge of the neuromodulatory needs of mPFC neurons in primates, and how similar or different they may be to dlPFC or to rodent mPFC. This will be an important area for future research.
Although there may be multiple avenues by which stress initially impacts neuronal physiology, there appear to be final common pathways involved in synapse removal. Thus, the varied effects of chronic stress exposure may ultimately lead to shared mechanisms. This review will first describe the signaling events activated by acute stress exposure that likely lead to spine loss with sustained activation, followed by the mechanisms that may be initiated with chronic stress exposure that lead to actin collapse and phagocytosis by glia, creating the architectural changes seen in the chronically stressed brain.
Acute, Uncontrollable Stress Weakens PFC and Strengthens More Primitive Circuits
Exposure to even a mild, acute uncontrollable, psychological stressor can rapidly weaken PFC connectivity and cognitive functioning in rodents, monkeys, and humans. 14 A key factor is the subject experiencing themselves as having no control over the stressor, thus initiating monoamine release in the PFC. 13 For example, stressful levels of loud noise (>95dB) impair cognitive performance in rats, 29 monkeys, 30 and humans. 10 Decades of psychological studies in humans have found evidence that uncontrollable psychological stress impairs a variety of cognitive functions that we now know are reliant on the PFC, including performance of the Stroop interference task, 31 working memory, 32 decision-making, 33 and extinction of a conditioned fear response. 34 Functional brain imaging studies have confirmed reductions in dlPFC activity with stress exposure during working memory performance, 35 and suggest that the dlPFC can regulate the visceral stress response via projections to the ventromedial PFC Brodmann Area (BA),32,36 which has extensive connections with BA25, a region that becomes overactivated in depression, and mediates the visceromotor outputs from the PFC.37–39 Thus, uncontrollable stress has heterogeneous effects on PFC circuits, generally decreasing the activity of those that subserve higher cognition and provide top-down control of emotion, while increasing the activity of circuits inducing affective, visceral responses.
Studies in animals have revealed some of the neurobiological basis for these rapid changes in higher cognitive abilities. Many of these actions are likely circuit-specific, an arena of recent progress, e.g. with optogenetic identification. Studies in rodents have found increased glutamate release in mPFC during an acute stressor that depends on glucocorticoid stimulation.40,41 Stress-induced glutamate release may involve projections from the amygdala, as part of reciprocal circuits within the mPFC. 42 It is unclear if elevated glutamate leads to expanded or atrophied dendrites with chronic stress exposure, which may be circuit-specific.
There is also extensive evidence of stress-induced catecholamine release in PFC arising from brainstem catecholamine neurons that are especially sensitive to aversive experience.14,43–45 Catecholamine release in mPFC occurs rapidly with stress onset 46 and thus can have immediate effects on cognitive functioning. As reviewed below, high levels of the catecholamines, norepinephrine (NE) and dopamine (DA) in the PFC rapidly activate intracellular stress signaling pathways to weaken PFC synaptic connections and impair PFC cognitive function in primates, which will be the primary focus of this review. 47
Detailed studies of the layer III microcircuits in primate dlPFC that generate mental representations have provided an in-depth understanding of how chemical changes during stress can rapidly impair higher cognitive operations. Under non-stress conditions, extensive, recurrent excitatory connections on spines maintain the persistent firing needed for working memory via NMDAR glutamatergic synapses on spines, while lateral inhibition from interneurons refines the information held in “mind”.48,49
Layer III dlPFC spines also contain negative feedback mechanisms to prevent seizures in a recurrent excitatory circuit, where feedforward Ca2+-cyclic adenosine monophosphate (cAMP) signaling can increase the open state of nearby potassium (K+) channels to weaken connectivity and reduce firing. The feedback signal may involve Ca2+ entry through multiple sources, including the calcium conductance of N-methyl-D-aspartic acid (NMDAR) channels (specifically composed of GluN2B subunits) themselves as well as release from internal storage within the smooth endoplasmic reticulum (SER), called the spine apparatus when it extends into the spine.50–54 As illustrated in Figure 1, there is evidence for feedforward cAMP-Ca2+ signaling in dlPFC spines: Ca2+ is released through calcium channels on the SER – the inositol triphosphate receptors (IP3R) and ryanodine receptors (RyR) – which are both localized on the spine apparatus in layer III dlPFC spines.55–57 These spines also express the molecular machinery for cAMP-PKA signaling to magnify internal Ca2+ release from the SER spine apparatus through these channels, which in turn can drive more cAMP production, creating a vicious cycle. As shown in Figure 1(a), this molecular machinery is held in check by receptors that inhibit the production of cAMP, i.e. the alpha-2A adrenergic receptor (α2 A-AR) and the metabotropic glutamate receptor type 3 (mGluR3), as well as by phosphodiesterase type 4 (PDE4) enzymes, which catabolize cAMP once it is synthesized.21,58,59 Conversely, cAMP-Ca2+ signaling is driven by high levels of catecholamines acting through lower affinity NE alpha-1 adrenergic receptors (α1-AR) and DA-1 receptors (D1R) to drive Gq-IP3R-mediated calcium-protein kinase C (PKC) signaling and Gs-cAMP-PKA signaling, respectively (Figure 1(b)).
cAMP-Ca2+ signaling can markedly alter the efficacy of synaptic connections, with moderate levels strengthening connectivity by increasing calcium near the post-synaptic density, but higher levels weakening connectivity by opening nearby K+ channels. As shown in Figure 2, layer III dlPFC spines express K+ channels (HCN, KCNQ) whose open states are increased by cAMP-PKA signaling. Under non-stressed, alert conditions (Figure 2(a)), moderate levels of catecholamine release engage high affinity α2 A-AR and D1R to dynamically regulate synaptic strength needed for working memory. For example, administration of the α2-AR agonist, guanfacine, systemically or directly into rat or monkey PFC can enhance neuronal firing and improve working memory, attention regulation, and behavioral inhibition.60–66 However, during uncontrollable psychological stress (Figure 2(b)), high levels of catecholamine release engage α1-AR and large numbers of D1R to drive calcium-cAMP-PKA-K+ signaling, which rapidly decreases dlPFC neuronal firing and takes the dlPFC “off-line.” dlPFC network connectivity and function can return to normal if PDE4 enzymes catabolize cAMP and normalize intracellular signaling.

Regulation of cAMP-Ca2+ signaling in the dendritic spine. (a) Within the dendritic spine, cAMP- Ca2+ signaling is regulated by several key mechanisms to maintain the integrity of calcium homeostasis. Transmission through α2 A-AR (via norepinephrine (NE)) and mGluR3 (via NAAG), receptors that are positioned in postsynaptic compartments in dlPFC layer III, inhibits cAMP signaling and thus, reduces cAMP- PKA mediated calcium leak into the dendritic spine via phosphorylation of calcium channels (e.g. inositol triphosphate receptors (IP3R) and ryanodine receptors (RyR)) located on the smooth endoplasmic reticulum (SER). Inhibition of cAMP-PKA mediated calcium leak further reduces K+ channel opening (e.g. HCN and KCNQ), leading to maintenance of working memory. Based on our immunoEM data, we see a decrease in α2 A-AR localization on the dendritic spines in aged macaques, insinuating a likely loss in calcium regulation. Our immunoEM data has further revealed a constellation of cAMP-related proteins associated with SER within the thin dendritic spines in dlPFC layer III microcircuits. The scaffolding protein disrupted in schizophrenia 1 (DISC1) interacts with phosphodiesterase-4 isozymes (PDE4) to regulate cAMP degradation intracellularly, preventing exacerbated feedforward cAMP- Ca2+ signaling. (b) The dendritic spines also contain calcium regulatory machinery that can conversely drive cAMP- Ca2+ signaling. Higher levels of NE can signal through lower affinity α1-AR which can drive Gq-IP3R-mediated calcium-protein kinase C (PKC) signaling, leading to increased cAMP-PKA mediated calcium leak. Higher levels of dopamine (DA) can signal through Dopamine-1 receptor (D1R) on the spine, consequently driving greater calcium leak into the dendritic spine and decreasing dlPFC neuronal firing, impairing working memory.

Effects of stress on the synapse in the dlPFC. (a) At the non-stress synapse on the dendritic spine, there is regulated NMDAR transmission with Ca2+ and Na+ with low levels of K+ extrusion through the K+ channels (HCN, KCNQ) as well as low levels of feedforward Ca2+-cAMP signaling. Moderate to low levels of NE signaling through α2 A-AR, which inhibits cAMP signaling, allows for enhancement of network firing in the dlPFC by increasing synaptic efficacy for inputs from target neurons. Conversely, moderate to low levels of dopamine (DA) signaling through D1R allows for decreases in synaptic efficacy of the inappropriate neurons. (b) Acute stress drives Ca2+-PKC and cAMP-PKA feedforward signaling via increased dopamine (DA) activation of D1R and norepinephrine (NE) activation of α1-AR, respectively. This leads to increased calcium leakage from the SER through Protein Kinase A (PKA)-mediated phosphorylation of IP3R and RyR as well as Protein Kinase C (PKC) activation. Subsequent increases in feedforward calcium-cAMP signaling opens K+ channels and thus, weakens synaptic efficacy and working memory. The perturbation of calcium levels in the spine may promote architectural changes in the spine as well as mitochondrial dysfunction. C. Chronic stress further exacerbates the pathways observed in acute stress. Prolonged Ca2+-cAMP feedforward signaling leads to a decrease in neuronal firing required for higher-order cognition, resulting in working memory deficits, a core cognitive deficit observed in several neuropsychiatric and neurodegenerative diseases. The prolonged Ca2+-cAMP feedforward signaling causes sustained elevations of calcium could further cause perturbations in mitochondria morphology, resulting potentially in the “mitochondria-on-a-string” (MOAS) phenotype.
Toxic catecholamine actions in PFC also have been seen following traumatic brain injury67–69 and hypoxia, 6 suggesting this may be a universal stress response for both psychological and physical stressors. The detrimental effects of catecholamines in PFC are amplified by glucocorticoids, 70 which block catecholamine reuptake into glia. 71 In contrast to the PFC, high levels of catecholamines in the amygdala strengthen emotional responses. 72 This switches control of brain and behavior from the thoughtful PFC to the reactive amygdala. Similar mechanisms appear to occur in humans, where stress-induced dlPFC dysfunction in working memory is strongly related to a genetic variation in COMT, which increases catecholamine levels. 73
Chronic Stress Causes Loss of Spines
Chronic exposure to physiological or psychological stressors induces additional alterations, including initiating mechanisms to remove dendrites and spines from PFC neurons. As schematically illustrated in Figure 2(c), chronic stress weakens connectivity and reduces cell firing by amplifying NE signaling in rat PFC, and increasing KCNQ channel actions, greatly reducing neuronal firing. As reviewed below, sustained elevations in PKC and calcium signaling may lead to a number of additional actions that promote architectural changes in spine structure.
Although loss of spines has been most commonly studied with chronic psychological stressors,16,25,74–77 it has also been observed following hypoxia 6 and TBI. 8 Loss of dendritic spines and/or dendrites is accompanied by, and often correlates with, the loss of PFC cognitive functioning.15,16,75 For example, Figure 3(a) and (b) show how chronic stress induces spine loss from rat layer II/III mPFC neurons that correlates with loss of working memory abilities. Furthermore, the spine loss and working memory deficits were rescued with chelerythrine, a PKC inhibitor, emphasizing the important functional significance of these architectural changes and the key role of regulatory molecules. (Note that this research has been done in rodents for both practical and humane reasons).

Chronic stress correlates with spine loss and working memory deficits. Chronic stress exacerbates feedforward Ca2+-cAMP-K+ signaling through increased PKC and PKA activation. This leads to opening of K+ channels, decreasing persistent firing and ultimate loss of spine density and deficits in working memory. (a) Representative images from rodent layer II/III of prelimbic cortex of distal dendritic segments, showing that chronic stress reduces spine density, while daily pretreatment with the PKC inhibitor, chelerythrine (CHEL), prevented spine loss. (Nonstress and vehicle-treated, gray; nonstress and CHEL-treated, blue; stress and vehicle-treated, red; stress and CHEL-treated, green; scale bar = 25 µm). (b) Both working memory and spine loss caused by chronic stress were prevented by chronic administration of the PKC inhibitor, CHEL. Working memory performance on the last two days of stress significantly correlated with distal spine density (r = 0.636, P <0.001). Figures (a) and (b) from Hains et al., 2009 with permission.
The loss of spines and dendrites with chronic stress is region and circuit specific. Stress-induced dendritic retraction is found in mPFC, and with sufficient stress, in the hippocampus, 78 but not in orbital PFC. 76 In contrast to the PFC, dendrites actually expand with chronic stress in the amygdala, 78 further accentuating the switch from reflective to reflexive state. Even within the mPFC, stress-induced changes are circuit specific. An elegant study by Shansky and colleagues showed that stress reduces dendrites in mPFC neurons involved with cortical-cortical processing, but increases dendrites in the mPFC neurons that project to and excite amygdala actions. 25 Shansky also discovered sex differences in these circuits, where females with circulating estrogen had greater responses to stress,79,80 which may arise from their increased responsiveness to catecholamines. 81 The molecular mechanisms that lead to expanded vs. atrophied dendrites with chronic stress exposure will be an important area for future research.
Although most of this research has been done in animals, one can also see evidence of reduced connectivity in humans exposed to chronic stress. Analysis of a post-mortem cohort of psychiatric cases where subjects had experienced severe stressors at different stages of life revealed substantial reductions in mushroom spine density in layer II/III and V of the OFC. 28 This study also found negative correlations between glucocorticoid receptor mRNA/protein expression with total spine density. 28 Structural imaging studies have shown reduced PFC gray matter in humans that correlates with the number of aversive events they have experienced.27,82 Loss of gray matter was especially evident in the mPFC areas (BA32 and BA10m) that mediate interactions between cognitive and affective circuits. Functional imaging studies have also reported reduced functional connectivity with a mild chronic stressor in medical students studying for the medical boards, that recovered once the stress was over. 15 The reversal of spine and dendritic loss can also be seen in rodents after extended periods of non-stress,15,77,83 although this resilience decreases with age. 83
What causes dendritic spines and dendrites to be lost with extended stress exposure? As described below, there are a number of interacting factors that appear to contribute to dendritic spine removal with chronic stress. ImmunoEM evidence suggests that NE axons actually express more tyrosine hydroxylase with chronic psychological stress exposure, 84 and increased catecholamine release in PFC is also seen with hypoxia 6 and TBI. 67 Thus, a prolonged catecholamine response likely contributes to the pathophysiology of these psychological and physiological stressors. Chronic stress also activates inflammatory signaling that likely contributes to weaker synaptic connections. For example, chronic stress and inflammation increase the production and release of kynurenic acid from astrocytes,85,86 an endogenous metabolite that blocks NMDAR,87,88 and impairs PFC working memory function. 89 Stress and inflammation also increase the astroglial release of the enzyme GCPII (glutamate carboxypeptidase II).90,91 GCPII hydrolyzes N-acetylaspartylglutamate (NAAG) to glutamate and N-acetylaspartate (NAA), and thus increases glutamate concentration at the synapse. Importantly, GCPII prevents NAAG mediated activation of mGluR3, which is located post-synaptically in layer III dlPFC microcircuits, leading to an increase in cAMP concentrations within the spine. 59 Both of these chemical changes would weaken the efficacy of NMDAR synaptic transmission in the primate dlPFC, and may lead to additional loss of trophic factors, as described below.
It is possible that a variety of molecular events initiated by stress exposure ultimately lead to similar toxic Ca2+ actions and neuroinflammatory synapse removal. Ca2+ dysregulation has traditionally been considered in terms of glutamate excitotoxicity, with high levels of glutamate stimulation of NMDAR (especially those with GluN2B subunits) causing excessive Ca2+ entry into the cytosol and the initiation of apoptosis to kill the neuron. A lower, nonapoptotic level of Ca2+ entry through NMDAR may be an important initiating event for some PFC neurons that are excited under conditions of stress exposure. However, other PFC pyramidal cells likely show reduced firing and thus reduced glutamate release during stress, e.g. due to increased D1R and α1-AR activation of Ca2+-cAMP-K+ signaling. In these important microcircuits, the elevated Ca2+ would arise from catecholamine activation of feedforward Ca2+-cAMP signaling in spines, driving both internal Ca2+ release and Ca2+ entry through voltage-gated channels. Thus, it is possible that the initiating stress signaling events that lead to elevated cytosolic Ca2+ differ between neurons, but that they ultimately engage common final pathways. Furthermore, there may be interactions between seemingly disparate signaling pathways, e.g. where REDD1 (Regulated in Development and DNA Damage responses-1) inhibition of mTOR signaling and subsequent spine loss can be initiated by glucocorticoids, 92 but may also be driven by PKA activation of REDD1 following high levels of catecholamine release. 47 Altogether, the evidence suggests multiple interacting pathways that lead to a similar phenotype of spine loss in the neural circuits that normally provide top-down regulation of emotion, thus disinhibiting the brain’s stress response.
The following sections below summarize current literature and proposed hypotheses on how sustained high levels of feedforward, Ca2+-PKC-cAMP-PKA signaling and weakened synaptic transmission, or sustained Ca2+ entry through NMDAR, may lead to loss of trophic factors, actin depolymerization, mitochondrial changes and the induction of inflammatory mechanisms to remove PFC connections during chronic stress exposure.
Potential Mechanisms Involved With Spine Removal
Weaker Synaptic Transmission Leading to Loss of BDNF
Brain-derived neurotrophic factor (BDNF) is a versatile neurotrophin contributing to brain development, neuronal survival, and maintenance of dendritic arborization and plasticity in the CNS.93–95 It is expressed across all regions in the brain, but it is highly expressed within the hippocampus and the cerebral cortex.96–102 BDNF exists in numerous functional isoforms, each with variable levels of expression across brain regions.99,100 Pro-BDNF consists of both the pro-domain and a mature domain that can either be cleaved to form mature BDNF (mBDNF) and BDNF pro-peptide or secreted as its own functional protein.100–102 Pro-BDNF and mBDNF have unique targets: the p75 neurotrophin receptor (p75NTR) and tropomyosin-related kinase B (TrkB) receptor, respectively. Generally, the functions of pro-BDNF and mBDNF are often seen at odds with one another.103–105 For instance, pro-BDNF can elicit long term depression (LTD) in the hippocampus, 106 while mBDNF primarily elicits long term potentiation (LTP) in the hippocampus.94,106–117 These interactions lead to a diverse host of downstream signaling cascades that can regulate transcription factors and ultimately, synaptic activity.
How does BDNF affect the synapse at the structural level? BDNF is thought to play a role in both spinogenesis as well as maintenance of mature spines.118–123 For instance, several studies have shown that the long-term administration of BDNF in primary rodent pyramidal hippocampal neurons or cerebellar purkinje neurons leads to increased dendritic spine density.124–127 Studies have found this to be directly mediated through TrkB signaling, as Trk receptor antagonists can directly prevent the BDNF-induced increase in spine density.128,129 At the same time, in vivo and in vitro studies have demonstrated the ability for BDNF to alter the morphology of spines, altering post-synaptic densities and neurotransmitter receptor distributions. For example, gradual BDNF administration to primary hippocampal neurons led to spine neck elongation. 129 It is noteworthy, however, to mention that increase in spine density secondary to exogenous application of BDNF is not appreciated in all the various culture and slice studies, which highlights the complexity of how BDNF’s effects are modulated (for comprehensive reviews on BDNF, see Kowiański et al. 93 and Kellner et al. 130 ) Notably, the majority of the literature has focused on the effects of exogenous BDNF. It is a challenge to understand the specific roles of endogenous BDNF, since homozygous BDNF KO mutations are lethal. 131 However, studies using heterozygous BDNF KO mice and inhibitors of TrkB, for example, have begun to elucidate the nature of endogenous BDNF. Nevertheless, it is evident that BDNF seems to be critical in supporting the development and maintenance of dendritic spines at the synapse.
Yet another important consideration regarding BDNF is the various pools of BDNF acting at the synapse, e.g. from presynaptic terminals, 108 postsynaptic dendrites,101,132 astrocytes, 133 and microglia.134,135 For instance, in addition to BDNF release from the presynaptic terminal onto post-synaptic TrkB receptors, BDNF may also be released by glia and by the post-synaptic compartment (Figure 4) at low but physiologically important levels for maintaining synaptic integrity. 136 Recognizing that BDNF can come from several local sources at the synapse has profound clinical implications for treatments as they converge on BDNF modulation.
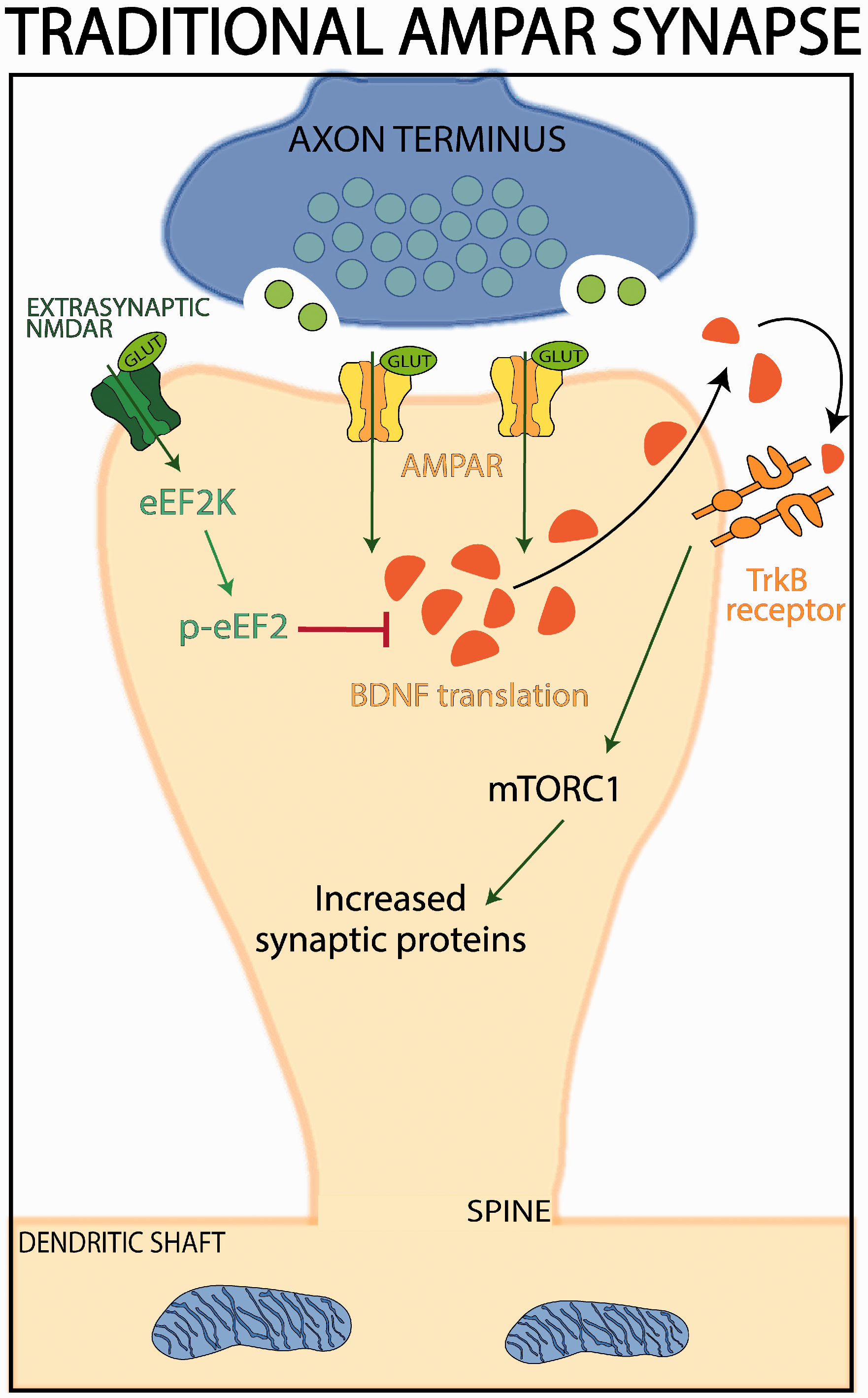
BDNF-mTORC1 signaling in a traditional AMPAR synapse. This figure is adapted from a review by Ron Duman and colleagues, Hare et al., 2017. In a traditional AMPAR synapse, NMDAR are extrasynaptic and respond to overflow of glutamate from the synapse. AMPAR stimulation activates BDNF translation in the spine. Subsequent BDNF release activates post-synaptic TrkB receptors that activate mTORC1 signaling to enhance the synthesis of synaptic proteins. In contrast, extrasynaptic NMDAR activate eEF2K which phosphorylates eEF2 to inhibit the translation of BDNF. This is likely different in the recently evolved circuits in primate dlPFC, where NMDAR are synaptic, and there is a more limited role of AMPAR neurotransmission.
What are the mechanisms that mediate BDNF expression? There is a large body of literature demonstrating a strong correlation between neuronal activity and BDNF transcription and secretion. 128 Various paradigms simulating increased neuronal activity have demonstrated upregulation of BDNF transcription. For instance, BDNF transcription is seen during kindling, 137 LTP induction,138–140 in vivo associative learning,141–144 and membrane depolarization.145–148 Furthermore, animal and in vitro studies have revealed that neuronal activity also regulates secretion of BDNF.94,114–117,149–152 While there is experimental support for the activity-dependent modulation of BDNF, this work has primarily been in the hippocampus and the cortex. Thus, there remains much work to be done to expand the scope of examined regions in order to understand how region-specific activity can regulate BDNF.
Accumulating data suggest that reductions in BDNF with chronic stress may contribute to loss of dendritic spines. These studies have utilized a variety of chronic stress paradigms (e.g., foot shock, swim stress, restraint stress, social isolation, etc.) over a wide temporal scale (ranging from 7 to 21 days) and have largely observed decreased levels of BDNF.153–155 For example, daily restraint of rats for 3 weeks resulted in decreased BNDF mRNA in the hippocampus and the subsequent atrophy of hippocampal pyramidal neuron dendrites. 156 However, an important limitation of these studies is the scope of regions and cell types examined. This is critical, since the role of BDNF is circuit-specific. For instance, chronic stress in rodents leads to a decrease in BDNF and TrkB mRNA in the hippocampus, but leads to an increase in BDNF mRNA expression in the amygdala and nucleus accumbens.156,157 This difference harkens back to our brain’s ability to rapidly switch from a reflective to a reflexive state, which necessitates different underlying circuitry for the regions involved. BDNF signaling may be altered by catecholamine mechanisms, where mechanisms that promote connectivity also amplify BDNF. For example, a study investigating PFC neurodegeneration in the setting of hypobaric hypoxia in layer II of rat mPFC found that administering guanfacine increased the anti-apoptotic Bcl2 and BDNF and decreased pro-apoptotic Bax and caspase.5,158,159 Thus, catecholamine actions may have widespread influences on dendritic spine health through regulation of BDNF signaling.
BDNF may also influence synaptic health via mTOR (Mammalian Target of Rapamycin) signaling, which regulates local protein synthesis to facilitate synaptic plasticity.160–165 mTOR is strongly activated by BDNF/TrkB signaling and thus, likely links BDNF and synaptic plasticity.162,165 Conversely, chronic stress upregulates REDD1, which inhibits mTOR via the mTORC1 subunit. 92 The work of Duman and colleagues have summarized how AMPAR signaling can increase the translation of BDNF in spines, leading to BDNF release and engagement of TrkB receptors that activate mTORC1 signaling to increase the production of synaptic proteins (Figure 4). 166 This model depicts a traditional synapse, where NMDAR are extrasynaptic, and inhibit BDNF translation (Figure 4). Thus, ketamine blockade of NMDAR in these circuits would promote synaptic growth, e.g. in mPFC neurons that express DA D1R and project to the amygdala and are needed for ketamine’s beneficial actions in mice. 167 However, the reader is cautioned that recently evolved circuits in primate layer III dlPFC are very different, with NMDAR exclusively in the synapse, and having little reliance on AMPAR53. As a result, it is likely that NMDAR would enhance rather than impede BDNF actions in these circuits. Thus, molecular mechanisms may differ substantially in recently evolved primate circuits.
Human studies echo the findings from research in animals. For example, postmortem PFC of human subjects with Major Depressive Disorder (MDD), similar to stressed rodents, have reduced levels of BDNF,168–173 elevated levels of REDD1, 92 and decreased levels of mTOR.92,169 Conversely, the antidepressant treatment response paralleled an increase in BDNF mRNA levels in the hippocampus and PFC169,174 There are also relationships to aging, as a cohort study following over 500 aged participants until death revealed that a higher level of brain BDNF expression was associated with a slower rate of cognitive decline. 175
Altogether, BDNF signaling is complex and the extent of its capabilities not fully understood, but it is vital to the synapse. And while reduced BDNF appears to contribute to synaptic loss under chronic stress, the specific pathways facilitating this loss have yet to be elucidated.
Changes in the Actin Cytoskeleton
Actin is a critical component of the dendritic spine’s ability to alter its structure in response to synaptic signaling and mediate synapse stability. Dendritic spines are built on a complex network of branched and linear filamentous (F)-actin that form the basis of the spine shape, including stable vs. dynamic changes in spine morphology. 176 As a result, alterations in actin may contribute to loss of dendritic spines during chronic stress. Molecular regulation of the actin cytoskeleton is complex, but can be linked to signaling cascades known to be activated by chronic stress exposure.
One mechanism that likely impacts actin is the increase in PKC signaling during stress exposure, which has been found in both rodent and macaque PFC. 177 Inhibition of PKC signaling prevents spine loss with chronic stress, highlighting its importance. 16 PKC phosphorylates several substrates that directly affect the morphology of actin cytoskeleton. 178 One substrate is myristoylated alanine-rich C kinase substrate (MARCKS).179,180 As illustrated in Figure 5, MARCKS directly stabilizes F-actin by connecting the cytoskeleton to the spine membrane, but this stabilizing function is lost when MARCKS is phosphorylated by PKC. In in vitro rat hippocampal cultures, depletion of MARCKS resulted in loss of spine density, width and length of the dendritic spines. 179 Adducin is yet another known substrate of PKC and is critical in assembling the spectrin-actin network, providing physical support, as well as capping the fast-growing ends of actin filaments.181,182 Importantly, it is enriched in dendritic spines and has been found to be important in synapse formation and stabilization,183–185 while PKC phosphorylation of adducin causes spine disassembly. 165 Thus, increased levels of PKC during chronic stress may disrupt a number of regulators of the actin skeleton leading to architectural collapse of the dendritic spine.
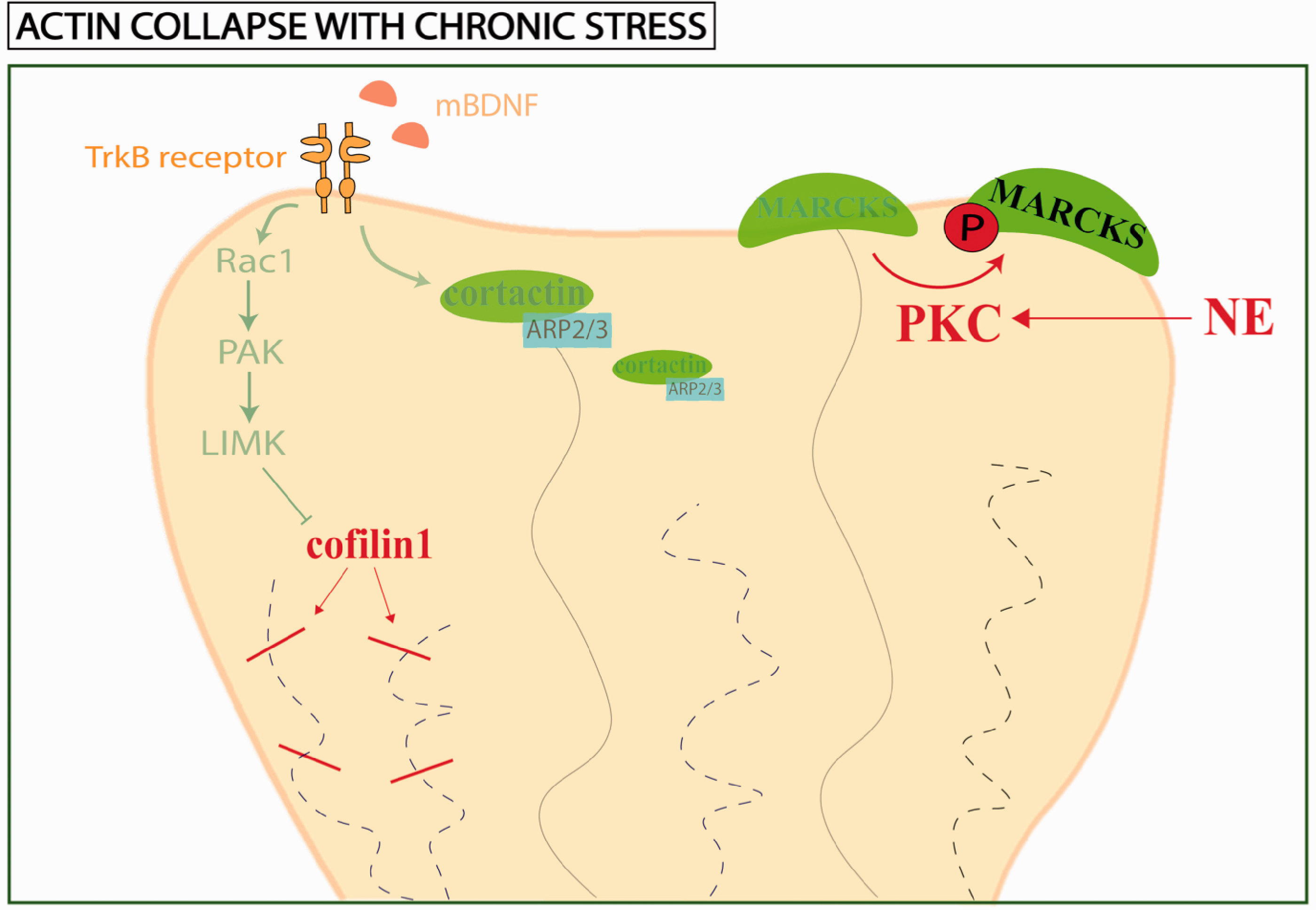
Roles of PKC and BDNF on maintenance of the actin cytoskeleton in the dendritic spine. Protein Kinase C (PKC) and Brain-derived neurotrophic factor (BDNF) regulate and maintain the actin cytoskeleton in the dendritic spine. PKC can interact directly with actin regulating proteins by phosphorylating them. Myristoylated alanine-rich C kinase substrate (MARCKS) is a F-actin cross-linking protein acting as a bridge connecting the actin cytoskeleton directly to the dendritic spine membrane. Furthermore, it can promote actin polymerization. Upon phosphorylation by PKC, MARCKS is redistributed from the plasma membrane to the cytoplasm and unable to bind to F-actin. PKC can also alter actin indirectly, e.g. through phosphatidylinositol 4,5-biphosphate (PIP2) actions. In the setting of increased stress, high levels of catecholamines, including norepinephrine (NE), can act through lower affinity alpha-1 adrenergic receptors (α1-AR) to drive Gq-IP3R-mediated calcium-protein kinase C (PKC) signaling. In both stressed rodent and macaque models, PKC expression is increased in PFC. The increased PKC signaling could lead to actin cytoskeletal disruption resulting in dendritic spine instability. BDNF is a versatile molecule that can influence actin cytoskeleton through TrkB receptor signaling. Downstream of TrkB receptor signaling leads to recruitment of RHO-family GTPase (RAC1), leading to activation of serine/threonine-protein kinase (PAK) and LIM domain kinase 1 (LIMK1) which can phosphorylate and inhibit cofilin1, thus blocking its ability to sever actin filaments. Another pathway downstream of BDNF-TrkB signaling is the recruitment of cortactin, an F-actin binding protein. Cortactin activates and stabilizes actin-related protein 2/3 (ARP2/3) complex for nucleation of actin filaments, which is necessary for formation of new actin filament branches. In the setting of increased, persistent stress, we see alterations of BDNF expression, notably decreases in BDNF expression. This could have significant downstream consequences for the actin cytoskeleton structure of dendritic spines.
As shown in Figure 5, BDNF is also known to influence actin stability through TrkB receptor signaling. BDNF can stimulate the recruitment of RHO-family GTPase (RAC1), leading to activation of serine/threonine-protein kinase (PAK) and LIM domain kinase 1 (LIMK1) which can phosphorylate and inhibit cofilin1, thus blocking its ability to sever actin filaments. 165 This cascade of events was tested in rat primary neuron cultures, which demonstrated that LIMK1 translation was dependent on BDNF and directly led to phosphorylation of cofilin1 at Ser-3, locally in the dendrites, which increased spine size and stability. 186 Thus, chronic stress mediated spine loss could be mediated through loss of BDNF, as described above. Alternatively, BDNF-TrkB signaling can cause increased recruitment of cortactin, an F-actin binding protein, especially at the postsynaptic density in association with NMDAR. Cortactin interacts with actin-related protein 2/3 (ARP2/3) to stabilize the formation of a new actin filament branch within the dendritic spine.187–189 Notably, there is conflicting data surrounding activation states of these actin-binding proteins in disease states. This is likely because actin cytoskeleton is dynamically modulated and thus, at different stages of disease, requires preferential activated or inactivated forms.
There are changes in actin regulatory molecules in brains of patients with mental disorders, such as schizophrenia.190–192 For instance, transcription levels of ARP2/3 complex subunits and nucleation promotion factors were significantly decreased in layer III pyramidal cells of the dlPFC from patients with schizophrenia. 193 Schizophrenia is also associated with alterations in CDC42 (cell division cycle 42), which organizes the actin cytoskeleton and has been implicated in genetic studies of schizophrenia.194–196 Thus, these changes in actin mechanisms are perhaps key in understanding the dendritic spine loss that is seen in schizophrenia and bipolar disorder among other mental disorders.197,198
Calcium Dysregulation Leading to MOAS and Inflammation
In addition to the direct effects of PKC signaling on actin dynamics, elevated cytosolic calcium levels can induce a series of events to activate inflammatory signaling and the removal of afflicted synapses. Very high levels of cytosolic calcium can induce apoptotic cell death, e.g. caused by excitotoxicity in neuronal cultures. However, most cognitive disorders do not involve apoptotic cell death, but demonstrate early dendritic atrophy. This may arise from more subtle, sustained increases in cytosolic calcium, e.g. from chronic stress or aging. Calcium dysregulation can arise from numerous sources, including reductions in calcium binding proteins, reduced regulation of cAMP-drive on internal calcium release, and increased flux through calcium channels. For example, stress or age can increase calcium efflux from the SER through RyR and IP3R, and lead to elevated cytosolic calcium.21,199–205
Elevated calcium can lead to calcium overload of mitochondria. Mitochondria are essential organelles that support neurons by directing energy metabolism, cellular respiration, reactive oxygen species (ROS) generation and dissipation, and calcium homeostasis.206,207 They are highly dynamic organelles, undergoing fission and fusion depending on energetic demands of the cell. These functions ultimately can determine the fate of the neuron, leading the neuron to apoptosis or synaptic loss when they are perturbed.207–209 Given the versatile nature of mitochondria, they can serve as an important indicator of the health of the cell.
Calcium is a critical substrate for mitochondria that can disrupt oxidative phosphorylation leading to release of ROS and nitric oxide. Calcium crosses the outer mitochondrial membrane (OMM) through the voltage-dependent anion channel (VDAC) and across the inner mitochondrial membrane (IMM) through the mitochondrial Ca2+ uniporter (MCU). 209 Calcium enters the mitochondrion through ER-coupling sites called mitochondria-associated-membranes (MAMs).210–212 MAMs are critical sites for lipid, phospholipid, and Ca2+ exchange from the ER to the mitochondria which can support neurotransmission, bioenergetics, and apoptosis initiation.210–214 Mitochondria are also ideally positioned near regions of high Ca2+ levels, allowing calcium concentrations to reach concentrations 5- to 10-fold higher than that of calcium in the cytosol.215–218 This, however, is a point of debate as some studies have suggested that high Ca2+ levels in fact draw mitochondria to those regions. 219 Nevertheless, the general consensus is that mitochondria play a critical role in regulating calcium levels, and that calcium in turn can alter mitochondrial function.
Synapses are especially dependent on mitochondria for the necessary large amounts of ATP and thus, synapses may be particularly susceptible to disruptions in calcium regulation. For instance, when mitochondria sense an excess of Ca2+, this can lead to increased formation of mitochondrial permeability transition pores (mPTP) which can trigger a loss in mitochondrial membrane potential, reduced ATP formation, and a cascade of inflammatory events. 220 Abnormal mitochondria can also take on dysmorphic morphologies.221–224 The Zhang group has identified one abnormal mitochondrial phenotype as “Mitochondria-on-a-string” (MOAS).221,225,226 MOAS are defined as long mitochondrion with bulbous segments of the organelle and connected by highly constricted segments, e.g. as schematically illustrated in Figure 2(c). As proposed in Figure 6, MOAS may arise from disruptions in calcium flux and bioenergetic stress leading to an interruption of fission.221,227–229 Consistent with this hypothesis, we have observed MOAS within the dendritic shafts of glutamatergic-like pyramidal neurons within layer III of the dlPFC of aged rhesus macaques, with pinched “string” regions next to calcium-containing SER. 225 Especially relevant to the loss of spines, calcium overload of mitochondria can elevate the release of ROS, which can initiate production of pro-inflammatory cytokines, such as activation of the NOD-, LRR- and pyrin domain-containing protein 3 (NLRP3) inflammasome.230–233 Further investigation is necessary, however, on how these prolonged pro-inflammatory signals can ultimately lead to the removal of the synapse. We explore this in the next section.

Proposed model for MOAS and complement signaling with microglia. A consequence and subsequent driver of the exacerbated cAMP-PKA signaling is high levels of cytosolic Ca2+ within the dendritic spine. Calcium levels rise through multiple sources, including the calcium conductance of N-methyl-D-aspartic acid (NMDAR) channels (specifically composed of NR2B subunits) as well as release from internal storage within the smooth endoplasmic reticulum (SER), called the spine apparatus once it extends into the spine. Calcium leaves the SER through calcium channels, specifically IP3R and RyR. Mitochondria have the ability to modulate calcium overload in the dendritic spine. Calcium regulation can be achieved through mitochondrial uptake of Ca2+ as well as direct calcium exchange through mitochondria associated membranes (MAMs) which are regions that connect the SER and the mitochondria. We hypothesize that as mitochondria become calcium overloaded, this leads to mitochondrial dysfunction (e.g. interruption to fission), resulting in a phenotype called “Mitochondria on a string” (MOAS). Within the dendritic shafts of glutamatergic-like pyramidal neurons of layer III of the dlPFC of aged rhesus macaques, we have observed MOAS with pinched “string” regions next to calcium-containing SER. We further propose that MOAS can generate inflammatory signaling molecules, e.g. C1q, that can recruit nearby microglia to phagocytose the ailing spine. It is known that dysfunctional mitochondria can result in elevated reactive oxygen species (ROS) production and generation of inflammatory molecules, such as complement proteins. C1q is a component of the classical pathway of complement signaling. It initiates activation of downstream complement proteins, which can signal to microglia through their receptors. Microglia are equipped with complement receptors (CR1, C1qRp, CR3, CD93, MEGF10), which can recognize complement proteins and initiate phagocytosis of these spines. Consistent with this hypothesis, we have seen the presence of C1q in the aged macaque dlPFC in three separate neuronal compartments (spine head, presynaptic axon terminus, and in the dendritic shaft next to dysmorphic mitochondria-on-a-string “MOAS”). It is important to note that while this model focuses on complement as a downstream signaling molecule to local glia, there are other potential downstream signaling molecules, e.g. phosphatidylserine, caspase 3, that can also lead to pruning by glia.
MOAS and Inflammation Engaging Phagocytosis by Glia
Glia account for approximately 50% of the cells present in the brain, and include oligodendrocytes, ependymal cells, microglia, and astrocytes.58,234–236 They provide fundamental support for neuronal health and function, including elimination of inappropriate synapses by astrocytes 237 and by microglia. 238 While synaptic elimination and glial participation have been best characterized at the neuromuscular junction (NMJ) in the PNS, there is growing evidence for glial involvement during synaptic elimination in the CNS.239–245 Synaptic elimination has been studied in the developing CNS and in CNS disorders. For example, glial phagocytosis of synapses has been documented in various pathological conditions, e.g., Alzheimer’s Disease (AD), Huntington’s Disease (HD), Parkinson’s Disease (PD), and schizophrenia, all of which have underlying synaptic dysfunction.246–251 Many studies have begun to identify the molecules that facilitate glial phagocytosis, but chief among them are complement proteins.250–255 Genetic association studies suggest that complement signaling may be a key factor in the activation of microglia and astrocytes to remove synapses. For example, in schizophrenia there is a strong genetic association with complement C4a (a gene encoding a complement component),57,256–261 while Complement Receptor 1 (CR1) is associated with increased risk of AD.262–265
Complement signaling is one of the key arms of the innate immune system, allowing our immune system to quickly identify and remove foreign antigens. The classical pathway of complement activation is initiated by C1q, which leads to activation of downstream complement components, importantly C3 and C4, which can then signal to microglia through their receptors.250,266,267 It is also possible that C1q engages other immune pathway receptors, such as major histocompatibility complex I (MHC I) on neurons.268–271
The role of complement signaling in the brain has been largely studied in developmental models where inappropriate synapses are pruned by glia. For instance, Stevens et al. first noted the production of complement C1q in Retinal Ganglion Cells during the critical period in visual development in mice. 272 The Stevens group also determined the role of microglial C3 in activity-dependent synaptic pruning in the developing retinogeniculate system and found that the upregulation in neuronal C1q was regulated by astrocytic release of TGF-ß (a growth factor), thus implicating both glial subsets in coordinating synaptic removal. 273 C1q and C4 have been found to increase with age, especially in AD vulnerable regions like the hippocampus, while C3 has been shown to decrease with age.274–276 Additionally, the mRNA for complement proteins is appreciably increased in early and late stage AD brains.276,277 Furthermore, the genetic depletion of C1q in AD mouse models (APP and APP/PS1) has been found to decrease neuronal injury and reduce the numbers of activated microglia surrounding the Aß plaques.246,278,279 However, there is also some evidence that C3 and C5 can be neuroprotective in AD, since C1q can enhance phagocytosis and clear apoptotic and cellular debris. 280 As a result, these studies seem to suggest the importance of complement proteins and the complement cascade in AD pathology, and more specifically synaptic health. It is also likely playing a dual – neuroprotective and neuropathological role, e.g. by removing both injured and functional synapses.
We have seen the presence of C1q in the aged macaque dlPFC in glial profiles, as expected, but also in three separate neuronal compartments (spine head, presynaptic axon terminus, and in the dendritic shaft next to dysmorphic mitochondria-on-a-string “MOAS”). 22 These data suggest that calcium overload in pyramidal cell spines can lead to dysmorphic mitochondria in neighboring dendrites, which then induce the expression of C1q to label nearby synapses for removal by glia. This hypothesis is depicted in Figure 5 and indicates an important area for further research.
Relevance to Mental Disorders and Their Treatment
Understanding the molecular mechanisms underlying spine removal may provide treatment strategies for those exposed to psychological or physiological trauma. For example, inhibiting cAMP-PKA signaling with α2-AR agonists prevents PFC spine loss in rats, 63 and these agents are useful in treating traumatized children,78,81 patients with TBI,281,282 or with emergence delirium from anesthesia. 103 Similarly, inhibition of PKC signaling protects spines and cognition in rats, 16 and treatments for bipolar disorder such as lithium that reduce PKC signaling protect PFC gray matter in patients. 283 Finally, both typical antidepressants and ketamine can restore spine numbers in stressed rodents, the latter via mTOR signaling.77,284 Taken together, these data suggest that understanding how stress alters PFC circuits has relevance to human disorders.
Concluding Remarks
The PFC provides top-down regulation of thought, action and emotion, allowing us to adapt and function in our increasingly information-driven, inter-connected society. In recent years, we have begun to identify the components of the underlying molecular machinery that provide strong dlPFC function, as well as the active mechanisms for weakening neuronal firing and removing synaptic connections during stress. Significant advances have been made in understanding how stress can change the circuitry, synaptic density, signal transmission, and cell-to-cell interactions in the PFC. We highlight a few questions that require further illumination in Table 1. Understanding the role of stress signaling pathways in the recently evolved PFC can shed light on why these circuits are especially vulnerable across numerous neurological disorders and provide strategies for therapeutic interventions.
Outstanding questions.

Footnotes
Acknowledgments
The authors would like to dedicate this work to the memory of Ronald Duman, who made groundbreaking studies on the mechanisms underlying stress-related spine loss and their recovery with antidepressant medications.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Yale University and AFTA receive royalties from Shire/Takeda from the USA sales of extended release guanfacine (Intuniv). They do not receive royalties from international nor generic sales of Intuniv.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: EW has been supported by training grant 1T32GM136651-01; AFTA is supported by R01 AG061190-01 and NSF 20,15,276; LHS is supported by NIH R01NS097728, R01NS095993, U01NS113445 and AHA EIA34770133; DD is supported by Alzheimer’s Association Research Fellowship AARF-17-533294, and an American Federation for Aging Research/Diamond Postdoctoral Fellowship.
