Abstract
Blood products are indicated for a plethora of conditions in several settings, with a variety of products available for transfusion, from highly processed specific components to whole blood. Matching the donor product to the recipient is crucial in avoiding serious transfusion reactions, with the extent of matching depending on the physiological need, setting, and product. There are important factors related to sex and gender differences in donated blood products, adverse reactions to those products, interplay with underlying pathology, as well as sociocultural differences in the collection. This article will review key sex- and gender-specific research related to the use of blood products with an emphasis on the acute care setting.
Introduction
Blood products are indicated for a variety of conditions in several settings, and there are a growing number of products available for transfusion. We will focus primarily on the products given in the setting of trauma: red blood cells (RBCs), platelets, plasma (fresh frozen plasma [FFP]), and whole blood (Figure 1).
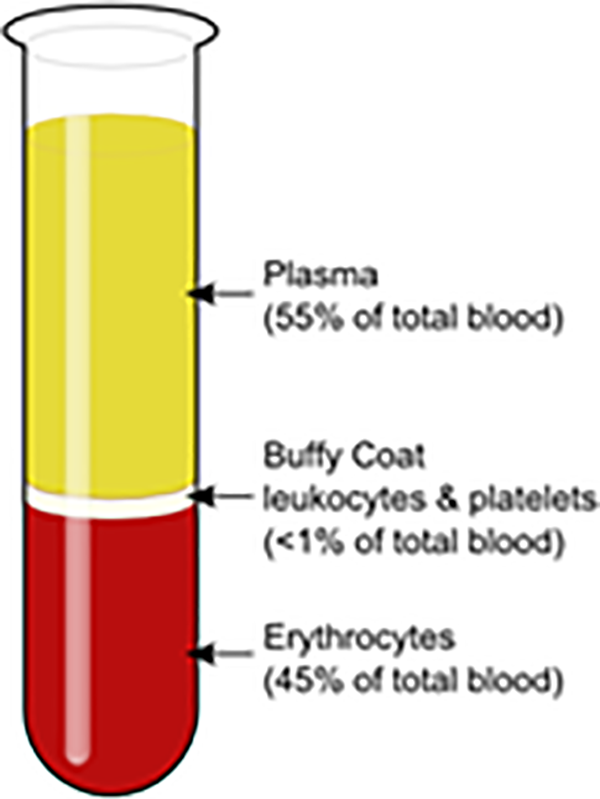
This figure depicts centrifuged blood with the relative amounts of each component in the donor whole blood. Plasma contains the majority of clotting factors and proteins found in blood, including HNA and HLA antibodies. Platelets are a primary agent in hemostasis and are either pooled (taken from multiple donors and combined into a bag for donation to a recipient) or apheresis (taken from a single donor and given to a recipient). Apheresis platelets contain significant amounts of plasma and therefore also contain pertinent antibodies. Red blood cells are used clinically to increase hematocrit and replenish volume and they also contain a small amount of plasma. KnuteKnudsen at English Wikipedia. Link to license: https://creativecommons.org/licenses/by/3.0/deed.en.
Donor sex and parturition status are recorded at the time of collection but their use in guiding transfusion practices varies based on the product and has changed over time. 1,2 What follows is a review of key sex- and gender-specific research related to the use of blood products with an emphasis on the acute care setting.
Donor Sex-Related Factors in TRALI
Transfusion-related acute lung injury (TRALI), a leading cause of transfusion-related morbidity and mortality, is primarily the result of donor HLA and HNA antibodies activating recipient neutrophils. 3 Although any donor can have HLA antibodies, most do not, and there is a dose–response curve between HLA antibodies and the number of pregnancies a woman has undergone. 4 As described in Figure 1, all 4 blood products described contain some of these proteins, but to varying degrees, and therefore TRALI can occur in recipients of plasma, apheresis platelets, or very high volume transfusions of RBCs. 3 Plasma is most prone to inducing TRALI, and in particular, plasma from females exposed to fetal blood. American multicenter retrospective study by Vossoughi et al found female donated plasma resulted in 20 times the TRALI rate (33.85 vs 1.59), whereas the risk in donated female RBCs was much lower (1.97 vs 1.15). 1 And TRALI is not the only pulmonary pathology that has been correlated with female plasma; 1 small study of 82 patients found male donated FFP had an odds ratio (OR) of 0.219 for all-cause pulmonary distress (19 patients) in recipients (5 of 19 were TRALI). 5 The increased risk of TRALI consistently found in many studies led the AABB (an international nonprofit and the accrediting body to virtually all US blood banks and most US hospital transfusion centers) to instate guidelines requiring plasma come from male donors or never-pregnant females, and that never-pregnant female platelet donors be HLA tested. These restrictions also generally apply to all other blood products where these antibodies are present (eg, apheresis platelets and whole blood). 6 The sex-specific research on transfusions described in the paragraph above led to an 80% reduction in TRALI after plasma transfusion and a 64% decrease after platelet transfusion. 4,7
Donor–Recipient Sex Concordance in RBCs
Donor–recipient sex concordance may affect recipient mortality after RBC transfusion according to 6 retrospective observational studies designed to explore this relationship. 2,8 In a 2019 meta-analysis reviewing 5 of the 6 studies, Zeller et al concluded that there was a pooled hazard ratio (HR) of 1.13 (CI: 1.02-1.24) for mortality in sex discordant transfusions, although due to confounding, selection, and reporting bias, the quality of evidence was deemed low. 8 The sixth study, published after the meta-analysis by Zeller et al, found no mortality difference in 2 of their 3 data sets. 2 The third (and smallest) data set had an HR of 1.08 for patients having received 1 or 2 discordant transfusions and HR 1.14 for those receiving 5 or 6. Unfortunately, we are unaware of any prospective studies performed on this important topic.
Whether or not a mortality difference exists, we know based on the study of tens of thousands of donor blood samples that female and male RBCs tend to have different characteristics (Table 1). These differences are proposed to have an impact on oxygen delivery, hemodynamics, coagulation, and extracellular vesicles, which together could explain the mortality difference found in most studies of sex-discordant transfusions. 9
Differences Between Male and Female RBCs.a
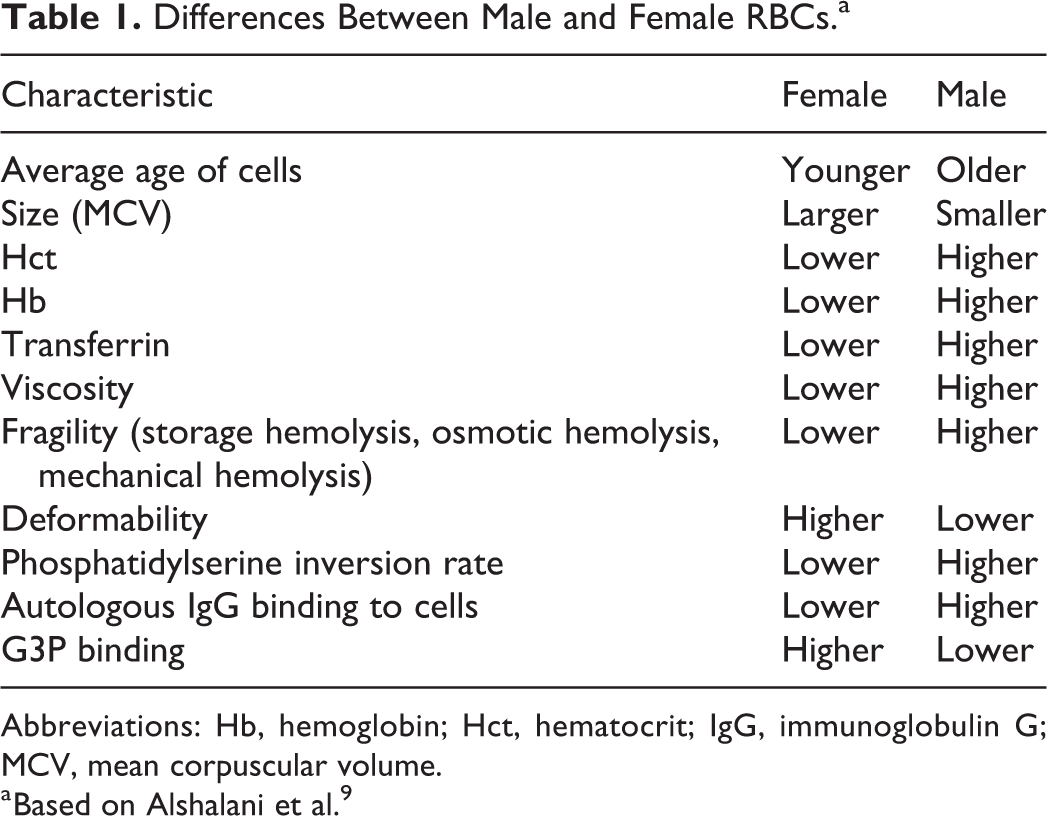

Abbreviations: Hb, hemoglobin; Hct, hematocrit; IgG, immunoglobulin G; MCV, mean corpuscular volume.
a Based on Alshalani et al.9
It is clear that donated RBCs differ between sexes, and despite most studies finding a slight mortality increase in sex-mismatched blood, blood banks have not moved to update RBC transfusion protocols. There is clearly a need to further elucidate underlying mechanisms that could inform best practices and explain a potential mortality difference. 9
Recipient Sex-Related Factors in Transfusion Reactions
Not surprisingly, sex of the recipient is also a risk factor that can influence mortality rates. As with the donor product, sex appears to modify transfusion reaction rates from the recipient side. Most research has focused on TRALI and Transfusion Associated Circulatory Overload (TACO), which contribute the most mortality and occur somewhat frequently (1.63% of all transfusions in 1 sample). 10 Transfusion reactions can range from annoying (eg, urticaria, rigors) to fatal (eg, TRALI, TACO). Regarding recipient sex and TRALI, a US study among older inpatients found an OR of 1.26 among female recipients and also discovered a unique sex-specific risk factor (smoking). 3 Regarding TACO risk, one American case–control study looking at 83 TACO events found female sex conferred over twice the risk (OR 2.1). 11 Another study found transfusion reactions in general were twice as likely in pregnant women, citing their elevated levels of leukocyte antibodies. 12 Higher rates of reactions in women, especially pregnant women, have been found with certain other potentially fatal transfusion reactions like the rare post-transfusion purpura, which involves immune-mediated destruction of platelets. 13 Some less fatal transfusion reactions, like febrile nonhemolytic transfusion reaction, have also been found to be slightly more common in females generally (OR 1.15). 14 Although most studies specifically investigating the link between transfusion reactions and sex have found a correlation, 1 study of over 200 nonhemolytic transfusion reactions found no link between donor or recipient sex and reaction type, severity, or frequency, but they did find increased anti-HLA antibody levels in females. 15 Given the sex-based differences found in most studies, some authors have called for sex-specific interventions to lower risk, including leukoreduction of the donated blood product, especially for recipients who have been pregnant. 3
Factors such as body weight could be modulating the sex-based effects found in the studies discussed above. Indeed, low body weight (<46 kg) confers 8 times the risk of TACO, and it seems a cautious volume-conscious approach to blood products may be a primary way to improve outcomes. 16 One case–control study found that among patients receiving over 4 units of any blood component, TACO rates were higher among females but not males when compared to their matched controls, but height or weight were not analyzed as specific variables by sex. 17 The fact that the quantity of blood products transfused affects people of different sizes and sexes differentially has important implications, as males and females tend to, and probably should receive different amounts of blood products in resuscitation. 18
Sex and Gender Differences in Transfusion Protocols
Looking beyond the donor and recipient effects of sex in transfusion reactions, there are also sex- and gender-specific factors relevant to how these products should be given. This is especially pertinent in trauma, a field in which women are particularly under-represented. 18 Regarding total volume given to trauma patients, the Pragmatic Randomized Optimal Platelet and Plasma Ratios (680 individuals, 20% female) found that establishing hemostasis in a patient with active hemorrhage usually occurred within 3 hours of admission and involved similar amounts of blood products being used between males and females. 18 However, an intriguing finding is that in the 24 hours after surgical hemostasis was achieved, women received 50% fewer blood products. 18 It is unclear whether this difference represents sex-informed treatment tailored to a patient’s actual requirement for fewer blood products, gender bias among the treatment team, or some other factor. Overwhelmingly, research shows significant differences in how males and females achieve and maintain hemostasis and coagulation.
For instance, sex differences in physiology as fundamental as the relative quantity of proteins comprising apheresis platelets have been observed, 19 and we know there are also clinically significant sex differences in hemostatic response to trauma, with females being more hypercoagulable. 20,21 The prevailing modern resuscitation strategy in traumatic hemorrhage, which was borne from military studies predominantly using young men, is called Damage Control Resuscitation (DCR) and involves giving blood products early and aggressively in high ratios (1:1:1 or 1:1:2 of plasma: platelets: RBC) while limiting crystalloid use. At least 2 studies have found mortality differences based on recipient sex, and the ratio of blood products they are resuscitated with. 18,21 Specifically, males have been shown to have lower mortality when given 1:1:1 versus 1:1:2, with 1 study finding a greater than 10% mortality improvement in 1:1:1. 21 In females, neither study found a mortality difference between the 2 ratios. 18,21
A noteworthy study by Coleman et al looked at sex as a specific variable and used thromboelastography (TEG), a fast, comprehensive, and accurate measure of coagulation profiles to guide resuscitations in nearly real time. 20 They analyzed the coagulation profiles of 464 patients who required trauma activations in 2 American emergency departments while noting the mortality and quantity of blood products given. Females had greater clot formation and clot strength, were less hyperfibrinolytic, less likely to have prolonged activating clotting time at presentation, and in the setting of reduced clot strength females were more likely to survive. Hyperfibrinolysis was more lethal in men. Of note, traditional coagulation assays did not find the difference that TEG was able to demonstrate. Thromboelastography performed on healthy individuals has demonstrated that females are more hypercoagulable at baseline, 22,23 and even more so during pregnancy, 22 although there is not enough data for a tailored transfusion protocol for use specifically in postpartum hemorrhage. 24 The study by Coleman et al demonstrated that the hypercoagulability females experience at baseline persists in trauma in a clinically significant way, but how do clinicians interpret that at the bedside?
Current transfusion protocols in trauma do not use sex-specific guidelines, and even the TEG based resuscitation protocols were established in a predominantly male population. 25 Therefore, it is somewhat unsurprising that despite using resuscitation protocols guided by nearly real-time data on coagulation profiles, there was no sex difference in the amount of blood product given in the study by Coleman et al. 20 Females may be overly resuscitated with certain blood products under current protocols, which can have significant consequences including thromboembolic events. Prior to modern DCR, a greater amount of crystalloids were given in massive hemorrhage, and aggressive volume resuscitation with crystalloids can lead to coagulopathy, for which females have twice the mortality. 26 We may have, seemingly unintentionally, improved mortality for female trauma patients in particular by shifting to DCR. This could be why, despite being more hypercoagulable, a less significant difference in trauma mortality between sexes has been found in some modern studies. 18 With the availability of technology like TEG in emergency settings, more individualized resuscitation protocols can begin to be developed and tested, but outcomes will be hampered if females are not equally represented in the design of those protocols.
Role of Gender in Donation Behavior
Increasingly, gender-specific factors are coming to light that relate to donor health and behavior, beyond the safety of the samples they provide. Understanding the role of gender will help maximize this vital resource and allow donors to more feel respected. Men and women initially present to donate at approximately similar rates, with some studies showing women presenting at higher rates. 27,28 However, most studies find women are less likely to become repeat, stable donors, despite some conflicting evidence to the contrary. 27 -29 The apparent disconnect between initial donation and repetitive donation behavior could be due to differential experiences while donating, as well as sex- and gender-specific deterrents. Women are more likely to report adverse physical reactions even after controlling for weight and age, 28 possibly due to the fact that they donate a larger percentage of their blood volume per donation. 27 Compounding this difference, adverse events are also more likely to deter them from returning. 28 Therefore, most of the deterrent to returning seems to stem from an increased psychological aversion to higher rates of unpleasant physical experiences. Some of these experiences include “medical reasons, feeling sick, and difficult veins” and observational data confirm their subjective reports, showing women have more vasovagal responses and more difficult venous access. 27,30 Premenopausal females may be particularly vulnerable to iron deficiency anemia which is a reason donors can be turned away, after which they may not return. 6 Women’s motivations to donate are also different, more often citing altruistic motives than men. 28 Because sex and gender influence the deterrents and motivations around this behavior, specific best practices should be put in place to reduce the push away from donation while tailored recruitment campaigns increase the pull toward donation. 28,29,31
Individual Sex and Gender Discordance
The percentage of individuals who identify as transgender (TG) comprise a quickly growing section of our population, recently estimated to be over 0.5% of US adults. 32 Notably, approximately one-third of the TG community does not identify with a gender binary, and some people do not identify with any gender terminology. 33 Although the accurate categorization of blood products by biological sex is critical to reducing harm from transfusions, in many cases blood is collected based on a self-reported gender binary. The Food and Drug Administration mandates either a male or female “self-identified or self-reported” gender be correlated with every unit of blood. 34 Collection practices vary by center, and some have employees and software ready to handle nonbinary donations. 33 Red blood cells are always tested for the group, Rh type, atypical cells, and certain diseases, but not for donor sex. 34 The AABB reported that among 3 separate samples of TG donors, the percentage of TG males stating they had been pregnant prior to donation (and therefore raising the risk of HLA antibodies in their FFP and platelets which would have been otherwise categorized as male) ranged between 1.5% and 6%. 35 As the understanding of sex- and gender-based research evolves, so should our collection tools for documenting biological sex versus current gender identity.
Conclusion
Females are not only recipients of these lifesaving blood products but also represent an important donor pool. Some important sex-specific research has already been applied to make transfusions extraordinarily safer, 1,4 but the nuanced field of transfusion medicine deserves further high quality sex- and gender-specific research. Equal representation of males and females in every stage of research as well as analyzing and reporting their data separately will inform the creation of clinical guidelines based on the significant sex differences. This commentary has illustrated sex and gender differences are important to consider in many aspects of transfusion medicine from recruitment strategies to adverse reactions, where even a small mortality benefit could have meaningful implications. Remarkable progress has been made in the last 15 years, and with further attention to this topic, many more lives will be saved.
Footnotes
Acknowledgments
We would like to acknowledge the Division of Sex and Gender in Emergency Medicine at Alpert Medical School of Brown University.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
