Abstract
Introduction
Gallstone diseases, mainly cholelithiasis and choledocholithiasis, are common surgical conditions influenced by a variety of metabolic and hormonal factors. Recent research suggests a potential link between hypothyroidism and the pathogenesis of gallstones.
Aim and Objectives
To assess the correlation of hypothyroidism in patients diagnosed with cholelithiasis or choledocholithiasis by measuring the biochemical parameters and to determine the clinical significance of hypothyroidism as a potential risk factor in gallstone formation.
Methods and Methodology
This was a cross-sectional study conducted in the Department of Surgery at a medical college in Northern Karnataka between April 2023 and January 2025. A total of 110 patients diagnosed with gallstone disease of all age groups and both genders were included. Patients with known thyroid disorders under treatment or who underwent thyroid surgery were excluded. All patients underwent thorough evaluation. In addition, thyroid function tests (serum T3, T4 and thyroid stimulating hormone (TSH) levels) were performed. These patients underwent the necessary treatment according to standards.
Results
Among the 110 patients studied, 65 (59%) were women and 45 (41%) were men. Middle-aged patients were predominant. Hypothyroidism was detected in 15 patients (13.6%), of whom 11 were women, while the remaining 95 patients (86.4%) were euthyroid.
Conclusion
Subclinical hypothyroidism may be a potential contributing factor in the development of gallstone diseases. Routine screening for thyroid dysfunction in patients diagnosed with cholelithiasis or choledocholithiasis is recommended. Early identification and management of hypothyroidism may reduce the recurrence or progression of gallstone disease.
Keywords
Introduction
Gallstone disease represents one of the most common biliary pathologies with significant morbidity.
Within India, the prevalence shows striking regional variation. Populations in the North experience a two- to four-fold higher burden than those in the South. 1
Hypothyroidism is common, frequently remains subclinical and therefore goes undetected. A sizeable overlap exists between individuals who develop gallstones and those with diminished thyroid function, suggesting an endocrine contribution to cholelithiasis.2, 3
Thyroid hormones normally promote relaxation of the sphincter of Oddi via thyroxine receptors. When thyroid hormone levels fall, as in hypothyroidism, sphincter tone rises and biliary pressure increases, fostering stasis. These physiological alterations support the concept that hypothyroid states predispose to biliary stasis. Evaluating the frequency of hypothyroidism in patients with gallstones could thus clarify the strength of this association.4, 5 This study was conducted with the intent of finding a correlation between gallstone disease and thyroid disorders.
Methods and Methodology
This was a cross-sectional study conducted in the Department of Surgery at a medical college situated in Northern Karnataka from April 2023 to January 2025. The study included patients of any age or gender who were treated under the Department of Surgery with a diagnosis of cholelithiasis or choledocholithiasis. Patients with known thyroid disorders (either hypothyroidism or hyperthyroidism), those on thyroid medications or individuals who had undergone thyroid surgery were excluded. This prospective observational study received Institutional Ethical Committee (IEC) permission and patients were included after informed consent. The research was based on the hypothesis that there is a rise in the incidence of gallstone diseases (cholelithiasis or choledocholithiasis) in patients with hypothyroidism. Using the formula n = Z²pq/d², where Z is the standard normal deviation, p is the estimated proportion, q = 100 − p and d is the desired precision, the minimum sample size was determined to be 93, assuming an expected proportion of hypothyroidism in gallstone disease of 18.5% with a 95% confidence level and 8% absolute precision the sample size required was 110. 6 Microsoft Excel was used to enter the data, while SPSS software version 20 was used for analysis. Categorical variables were displayed as frequencies and percentages and continuous variables were represented as mean ± standard deviation (SD), median and interquartile range. The chi-square test was used to examine relationships between categorical variables and a P value of less than .05 was deemed statistically significant.
Results and Analysis
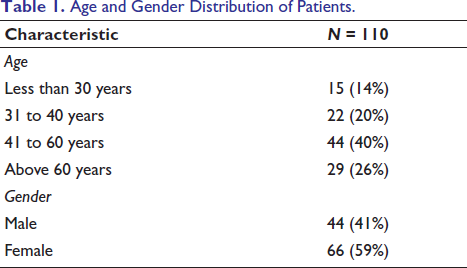
The study population consisted of 110 patients diagnosed with cholelithiasis or choledocholithiasis. Among them, the highest percentage of patients were in the 41-60 years age group (40%), followed by those above 60 years (26%). A smaller percentage of patients were in the 31-40 years category (20%), while the least were below 30 years (14%). Among the study participants, females accounted for a higher proportion (59%) compared to males (41%) (Table 1).
Age and Gender Distribution of Patients.
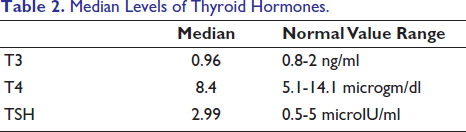
The median levels of thyroid hormones in the entire study population were as follows: T3, 0.96 ng/mL; T4, 8.4µg/dl; and TSH, 2.99µIU/mL. These values provide a baseline reference for evaluating thyroid function in gallstone patients. Hypothyroidism was detected in 15 patients (13.6%), of whom eleven were women, while the remaining 95 patients (86.4%) were euthyroid. While median TSH levels were within the normal range, the variability in TSH and thyroid hormone levels necessitated subgroup analysis (Table 2).
Median Levels of Thyroid Hormones.
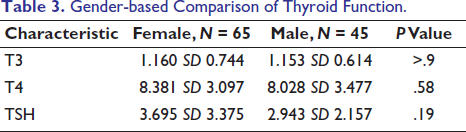
When comparing thyroid parameters between males and females, T3 levels were slightly higher in females, while T4 levels remained similar in both genders. TSH levels were marginally higher in females, though these values are not statistically significant (P > .05) (Table 3).
Gender-based Comparison of Thyroid Function.
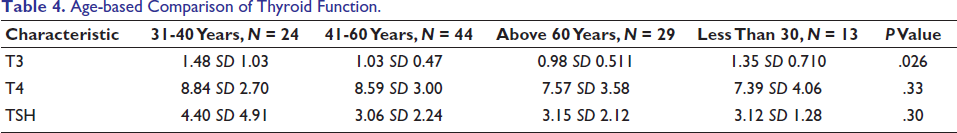
Upon analysing thyroid function across different age groups, younger patients (<30 years and 31-40 years) exhibited higher T3 levels compared to older patients. The highest mean T3 was seen in the 31-40 years group (1.48), while it was lowest in those above 60 years (0.98). T4 levels did not show significant variation across age groups. There was no significant gender-based difference in patients diagnosed with hypothyroidism. TSH levels were relatively high in younger patients, with a slight decline in the 41-60 age group before rising again in the elderly. However, none of these variations were statistically significant (P > .05), indicating that age alone does not significantly impact thyroid dysfunction in gallstone patients (Table 4).
Age-based Comparison of Thyroid Function.
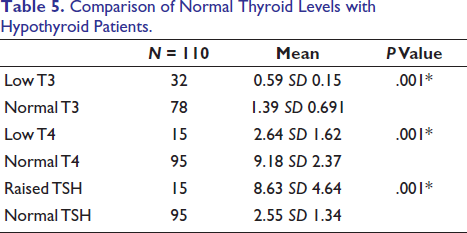
There was a significant difference in Serum T3, T4 and TSH Levels between normal and hypothyroid patients (Table 5).
Comparison of Normal Thyroid Levels with Hypothyroid Patients.
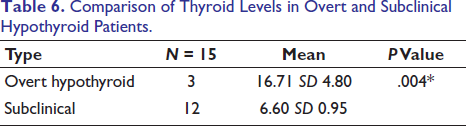
There was a significant difference in serum T3, T4 and TSH levels when overt and subclinical hypothyroid patient groups were compared (Table 6).
Comparison of Thyroid Levels in Overt and Subclinical Hypothyroid Patients.
Discussion
The interplay between reduced thyroid function and biliary stone disorders, including cholelithiasis and choledocholithiasis, has drawn considerable investigative attention. In our cohort, women accounted for 59% whereas men comprised 41%, mirroring published data that consistently report a female predominance. One representative series, for example, noted a 66% female versus 34% male distribution among patients with gallstone diseases. 5
With respect to the status of thyroid functions, 13% of individuals in our study were hypothyroid. This proportion closely parallels earlier findings. Ahmad et al. documented a 12% prevalence among biliary stone carriers. 7 Laukkarinen et al. reported 10.2% in persons with common bile-duct stones, 8 Inkinen et al. observed 10.6%, 9 and Völzke et al. in a large series of 1,500 subjects, described a 2.8% rate. 5
Several mechanisms plausibly connect hypothyroidism with lithogenesis. Thyroid hormone deficiency promotes dyslipidaemia, leading to cholesterol-supersaturated bile, it diminishes bile flow and weakens the pro-relaxation effect of thyroid hormones on the sphincter of Oddi, thereby increasing sphincter tone, raising intra-biliary pressure and favouring stasis. 10 These are key steps in gallstone formation.
Age-related patterns differ across other studies. Our data show peak gallstone prevalence between 41 and 60 years, whereas two studies recorded the highest rates in patients older than 60 years.8, 9 Ahmad et al. found that 66% of their gallstone hypothyroid cohort fell into the 51-60 year bracket. 7 Although Kulkarni et al. identified male predominance among hypothyroid patients with gallstones. 10 The majority of other reports, including ours, observed female preponderance.
Similarly, not every study demonstrated a statistically meaningful link between thyroid dysfunction and gallstone disease, with two of them reporting no significant association at all.11, 12 These disparities likely reflect variations in study design, demographic characteristics and sample size.
Limitations of the study were a single-centre experience and individuals with known hypothyroidism were not evaluated for gallstone disease.
Conclusion
Our findings suggest a possible connection between hypothyroidism and gallstone disorders, particularly in middle-aged women. Thyroid insufficiency may facilitate stone formation through dyslipidaemia, diminished bile flow and increased sphincter of Oddi tone. Routine thyroid function testing should therefore be contemplated in patients presenting with gallstones, especially those with coexistent risk factors such as obesity or lipid abnormalities.
Footnotes
Authors’ Contribution
Dr Venkata Challa is the primary researcher.
Dr Siddharoodha Sajjan performed the radiological investigations
Drs Girish Kullolli, Shruti Sheelin and Shivaraj Mangyal were part of the team during the collection of data, analysis and results.
Dr Tejaswini Vallabha is the guide of the research work and contributed to data collection, results analysis, drafting and correction of the article.
Declaration of Conflict of Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
The ethical clearance has been obtained from the Institutional Ethics Committee.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed Consent
The informed consent was obtained from the patients for the study.
