Abstract
Background:
Up to two-thirds of pregnancies among young, unmarried women in the United States are unintended, despite increased access to highly effective contraceptive options.
Aim:
This study implemented and evaluated a social marketing campaign designed to increase access to a full range of contraceptive methods among women aged 18–24 years on a southeastern university campus.
Methods:
Researchers partnered with Choose Well and Student Health Services to design, implement, and evaluate You Have Options, a 10-week multi-media social marketing campaign. The campaign aimed to raise awareness, increase knowledge, and improve access to contraceptive options, including long-acting reversible contraception (LARC) methods among college women. A pretest-posttest web-based survey design measured campaign awareness and recognition, as well as attitudes, subjective norms, and behavior.
Results:
Participants demonstrated a significant increase in knowledge about intrauterine devices (IUDs) between pretest (M = 2.66, SD = 1.30) and posttest (M = 3.06; SD = 1.96); t(671) = −2.60, p < .01). Analysis revealed that frequent exposure to the campaign prompted participants to engage in discussions about LARC with friends (p < .05). In addition, 20- to 24-year-olds who reported seeing the campaign messages were more likely to seek out information (p < .01) and adopt a LARC method (p = .001) than 18- or 19-year-olds who saw the campaign messages.
Conclusion:
Findings from the study offer practical recommendations for implementing social marketing campaigns aimed at increasing access to LARC and reducing unintended pregnancy.
Introduction
Nearly half of all pregnancies in the United States—almost three million annually—are unintended. 1 Long-acting reversible contraception (LARC), including intrauterine devices (IUDs) and the implant, may offer one solution to the burden of unintended pregnancy. 2 College-aged women (aged 18–24 years) experience the highest incidence of unintended pregnancy compared to other age groups. 3 Women in this age group may be more likely to use less effective contraceptive methods 4 and are in need of more effective options. The purpose of this study was to design, implement, and evaluate a multi-media social marketing campaign to raise awareness, increase knowledge, and improve access to contraceptive methods among college women.
In 2012, the American College of Obstetricians and Gynecologists (ACOG) recommended LARC methods as first-line contraceptives for all women and adolescents (ACOG 5 ), a recommendation reinforced by the American Academy of Pediatrics in 2014. 6 In the United States, LARC use has increased from 2.4% of contraceptive users in 2002 7 to 14% in 2014. 8 LARC methods are the most effective contraceptive options available, with perfect and typical failure rates of less than 1%. 9 These methods offer increased effectiveness because they remove the risk of user error that often accompanies daily methods. 2 Studies confirm that LARC methods are safe 2 and have high continuation and satisfaction rates. 3 Further, these options address women’s concerns about convenience, specifically daily maintenance of the oral contraceptive pill (OCP). 10
Although the OCP is the most common reversible contraception option, 3 it has a 9% typical failure rate. 9 Some women reject LARC methods because they perceive them as unsafe and alien. 11
Social marketing
Social marketing uses commercial marketing techniques to achieve specific behavioral objectives for a social good. 12 Contraceptive access initiatives have utilized social marketing as a means to decrease unintended pregnancy. Social marketing has been used to increase condom uptake, current use, and consistent use among partners in developing nations. 13 In a systematic review of social marketing interventions in the United States, 9 of the 12 initiatives showed significant effects on at least one of the outcomes related to reducing teen pregnancy, 14 such as increasing awareness and improving contraceptive use. Findings suggested that successful family planning social marketing initiatives should focus on the marketing mix: price, place, product, and promotion.14,15
Theoretical frameworks
Social marketing is a multidisciplinary whole systems approach to behavior change that provides a framework to employ a range of theories to support effective campaigns. 12 This social marketing campaign was developed through rigorous systematic theory-based formative research based on the theory of planned behavior (TPB) and diffusion of innovations (DOI) theory.16,17
TPB
The TPB suggests that subjective norms, attitudes, and perceived behavioral control may predict behavioral intention and actual behavior. 18 Researchers note that TPB may predict whether an individual chooses to adopt or change a particular health behavior, 19 increasing the usefulness of this theory in social marketing interventions. TPB has been used to predict intention to use condoms 20 and contraception. 21 Further, exposure to health communication campaigns informed by perceived behavioral control may be effective in influencing health behaviors. 22 Thus, creating a successful social marketing intervention requires targeting the appropriate construct (i.e. attitude, subjective norm, and/or perceived behavioral control), to persuade individuals to modify or adopt a health behavior. 23 As a result, TPB may be useful in increasing access to LARC among college women.
DOI theory
DOI theory postulates that an innovation spreads among members of a social system, communicated through certain channels, over time. The process of innovation adoption includes innovators, early adopters, early majority, late majority, and laggards. 24 Studies examining the relationship between social communication and mass media found that contraceptive use was commonly associated with the belief that social network members were using contraception. 25 Specifically, women were more inclined to view IUDs positively if their social support systems also expressed similar opinions. 26 DOI may be helpful in understanding the uptake of LARC methods among college women where interpersonal communication between friends, family, and doctors becomes increasingly important in complex decision-making processes.
The present study utilized the TPB and DOI to implement and evaluate a social marketing campaign to raise awareness, increase knowledge, and improve uptake of LARC methods among young women at a mid-sized southeastern university campus. Researchers predicted the following:
H1. Women who recall a campaign message will engage in increased information-seeking behaviors about highly effective contraception compared with women who do not recall a message.
H2. Women who recall a campaign message will report increased uptake of highly effective contraception compared with women who do not recall a message.
H3. Increased exposure to the campaign will have a significantly positive impact on information-seeking behaviors and adoption.
Methods
You Have Options: a contraceptive choice campaign
Researchers partnered with Choose Well and Student Health Services to design, implement, and evaluate You Have Options, a 10-week multi-media social marketing campaign. You Have Options was designed to raise awareness, increase knowledge, and improve access to LARC methods among college women. The multi-media messages were developed through rigorous systematic theory-based formative research based on TPB and DOI.16,17 Female college students were the primary target audience for the campaign. Researchers segmented the audience and developed behavior change strategies based on a robust understanding of the target audience’s perceptions of benefits, barriers, and competition.
The YHO campaign aimed to reposition IUDs and the implant as “safe, easy, and most effective.” The campaign emphasized the marketing mix, including the four P’s (i.e. product, price, place, and promotion) (see Table 1). The core product included the target audience’s perceived benefits of LARC methods, including safety, ease of use, and effectiveness. For example, messages highlighted the increased effectiveness of LARC methods compared with the most commonly used contraceptive method among college women, the OCP. The actual product included the LARC methods, including IUDs and the implant, which were provided on campus by Student Health Services. The augmented product included empowerment to make an informed choice (i.e. You Have Options). The price included the costs to the target audience, such as the time for a doctor’s appointment and the pain of insertion. As a result of the Affordable Care Act, all Food and Drug Administration (FDA)-approved contraceptive methods should be available through health insurance without cost-sharing (i.e. free). The place included the campus and Student Health Services. Promotion included new and traditional media. Communication channels were strategically selected to target college women. New media, incorporating digital and social media channels, included Facebook, Twitter, Instagram, and emails. Traditional media included printed flyers/posters, brochures, buttons, media relations, and campus events (see Table 2).
The marketing mix for You Have Options.

FDA: Food and Drug Administration; LARC: long-acting reversible contraception; IUD: intrauterine device.
Definitions adapted from French et al. 12
Campaign messages and materials (N = 398).

IUD: intrauterine device.
Messages were developed and tested through formative audience research and a pilot campaign (see advertisements and messages in Sundstrom and colleagues16,17). The overall campaign message was, “You Have Options.” Supporting messages included “The IUD and implant are 99% effective in preventing pregnancy” and “Your birth control may not be working as hard as you. The pill is only 91% effective at preventing pregnancy” (see Table 2 for all campaign messages). Messages were printed on posters, flyers, banners, brochures, and buttons (see Figures 1 and 2 for sample materials). Buttons were distributed to students across campus to start a conversation about LARC through interpersonal communication. Messages were also disseminated on Facebook, Instagram, and Twitter, including Twitter Chats. The campaign utilized unique hashtags, such as #YouHaveOptions, #KnowYourOptions, and #LoveYourLARC, to create a conversation about these methods. Researchers developed a customizable presentation to share at events and with groups of students across campus. Undergraduate and graduate students on the Women’s Health Research Team were trained to conduct peer-to-peer presentations in classes, at events, and in residence halls. The Campus Health Education Office included an hour-long version of the presentation as part of its standard core of offerings. Through the Health Education Office, the campaign presentation was delivered to classes in a variety of disciplines, departments, clubs, and student organizations. A 15-min version of the presentation was developed for peer-to-peer facilitators to deliver during the year-long required course for all first-year students.
Study design
A pretest-posttest web-based survey design measured the impact of You Have Options, a 10-week multi-media social marketing campaign. The campaign intervention study was conducted at a mid-sized liberal arts university in a southeastern, urban city. The university’s Student Health Services began offering LARC options to female students 3 months prior to the start of the campaign. At pretest, Student Health Services was not conducting advertising and/or outreach to inform students about these options.
Participants
Female students, aged 18–24 years, participated in the study. Researchers recruited a random sample of female students who were seeking care at Student Health Services to complete the pretest survey (n = 275). Following the pretest, You Have Options, a 10-week multichannel social marketing campaign was implemented on campus. After the conclusion of the campaign, a random sample of female students seeking health care at Student Health Services completed the posttest survey (n = 398). The current population receiving services at Student Health Services includes 10,440 undergraduate students (18–21 years of age). Of this population, 62.8%, or 6554, are women and 37.2%, or 3886, are men. Approximately 82% of the population is White/Caucasian, 6.8% is Black/African American, and 4.4% is Latino/Hispanic, with 6.7% being of another race/ethnicity or multiple ethnicities. In the year immediately preceding this campaign, there were 12,218 appointments at Student Health Services among women aged 18–24 years.
Participants received identical surveys at pretest and posttest, except for questions specific to campaign exposure at posttest. This between-subjects design captured overall exposure to the campaign. This design was preferred to measure change in the campus community. The random sampling framework (e.g. approaching every other eligible student) allowed researchers to recruit a wider audience to understand campaign exposure and influence on campus. Recruitment occurred in the same manner at pretest and posttest using a predetermined number of recruitment days; however, increasing numbers of individuals seeking care at Student Health Services at different time periods during the study may explain the higher number of participants in the posttest (e.g. study abroad travel appointments, allergy appointments, colds/flus). The College of Charleston Institutional Review Board (IRB) reviewed and approved this study (IRB approval code: GMGM-10-24-2016).
Researchers completed face-to-face recruitment in the Student Health Services waiting room every day (Monday through Friday) from 8:30 a.m.–4:30 p.m. with a break for lunch. Although many participants agreed to participate in the study, we did not record the number of participants who declined participation. Participants were given an iPad with a self-administered electronic questionnaire developed in Qualtrics. Participants were informed that if they did not finish the survey, they could take the iPad into the exam room, complete the survey there, and return it to the research station following their appointment. All participants were electronically consented and informed that their participation was voluntary, would not impact the care they received at Student Health Services, and could be stopped at any time. Following completion of the survey, participants were invited to select a small gift (e.g. school logo t-shirt, school logo mug, and school logo socks) to thank them for their participation.
Measurement tool
The survey was designed based on a review of the extant literature, the research team’s prior work on contraception,16,17,25,27,28 the TPB, 29 and DOI theory. 30 This study incorporated measures from nationally validated questionnaires, including the National College Health Assessment (NCHA) and the National Survey of Family Growth (NSFG). The survey consisted of five sections: demographics and sexual history, contraceptive use, LARC knowledge, LARC communication channels, and campaign exposure (see survey instrument in Supplemental Material).
Demographics and sexual history
Survey items at pretest and posttest pertained to age, race/ethnicity, year at the university, residence (on/off campus), sexual orientation, and sexual history.
Contraceptive use
Pretest and posttest survey items included participants’ history of contraceptive use, including current contraceptive method, primary contraceptive method, and reasons for choosing a particular method.
LARC knowledge
Pretest and posttest survey items assessed participants’ knowledge of LARC methods. Content was derived from national sources of contraceptive information.4,9
LARC communication channels
Survey items assessed where participants had heard about LARC methods. These items were asked at both pretest and posttest.
Campaign exposure
Process evaluation
Process evaluation offers a valuable approach to evaluating social media in health promotion campaigns. 31 Researchers tracked key performance indicators (KPIs), including exposure, reach, and engagement. Social media metrics to assess campaign exposure included number of posts, impressions, likes, shares, reach, and followers. In addition, researchers measured the Klout score to track online social influence. Scholars recommend Klout to measure engagement because the score incorporates the influence of social networks by measuring the number of individuals influenced by the campaign, as well as how much those individuals influence others. 31
Outcome evaluation
Survey items assessed participants’ recall of the YHO contraceptive campaign on campus. Questions included whether they had seen campaign messages in the past 3 months and the communication channels where the messages appeared (e.g. flyers, brochures, buttons, presentations, social media). Participants also answered questions about how frequently they saw the messages.
In line with the goals of social marketing to promote behavior change, survey items assessed whether the LARC messages from the YHO campaign prompted participants to engage in action, such as talking to friends or family members about IUDs/implant, searching for additional information about these methods, asking a doctor about getting an IUD or implant, making an appointment for LARC insertion, or having a LARC method inserted. Survey items also assessed whether participants had made an appointment or had a LARC inserted at Student Health Services. A series of 7-point scales asked whether participants found the campaign information positive, helpful, and believable. Finally, participants were asked to provide information regarding the best way to communicate about LARC methods with students.
Data analysis
Researchers utilized descriptive statistics to analyze participant characteristics and item responses. Researchers utilized independent samples t tests to understand cohort differences between pretest and posttest in IUD and implant knowledge. To measure change in knowledge, knowledge questions were scored either correct or incorrect and an independent samples t test was performed on the means. To measure campaign exposure frequency effects on behavior items, chi-square analyses were used. In addition, age category (under 20; over 20) effects on LARC behavior items were measured via chi-square analyses. This age dichotomy was selected as lower and upper classmen may vary in their contraceptive needs and reproductive life planning, which may impact their interest in LARC methods.32,33 Unanswered survey items were treated as missing variables, but no observations were removed during analyses. All analyses were performed using IBM-SPSS 21.0.
Results
Sample
The You Have Options communication campaign was implemented between February and April, 2016. A total of 275 participants completed the pretest survey and a total of 398 women completed the posttest survey. Although standardized procedures resulted in more participants recruited at posttest than pretest, there were no statistically significant demographic differences between pretest and posttest. Participants’ age range was 18–24 years with a mean age of 19.8 ± 2.21 years at pretest and 20.1 ± 1.37 years at posttest. At posttest, participants self-identified as first-year students (27.9%, n = 111), sophomores (24.1%, n = 96), juniors (23.1%, n = 92), or seniors (24.9%, n = 99). The majority of the sample identified as White (83.7%, n = 333), with 10.3% (n = 41) identifying as Black, 3.3% (n = 13) as Hispanic/Latino, and 2.8% (n = 11) as another race. This sample is similar to the overall campus population, which includes 80.1% White students. Of the 398 participants, 183 (46.0%) lived on campus, while 215 (54.0%) lived off campus. Participants primarily identified as heterosexual/straight (92.0%, n = 366), while 2.8% (n = 11) self-identified as homosexual/gay/lesbian and 4.5% (n = 18) self-identified as bisexual. Three participants identified as asexual or queer. The majority of participants indicated a history of vaginal intercourse (84.7%, n = 337) with a mean age of initiation of 16.77 ± 1.69 years.
Contraceptive knowledge
Knowledge about IUDs was significantly higher among the posttest cohort (M = 3.06; SD = 1.96) compared to the pretest cohort (M = 2.66, SD = 1.30, t(671) = −2.60, p < .01). Although knowledge about the implant was higher among the posttest cohort compared to the pretest cohort, the change was not significant. For additional information on contraceptive knowledge and awareness at posttest, see Table 3.
Contraceptive knowledge and awareness statements.
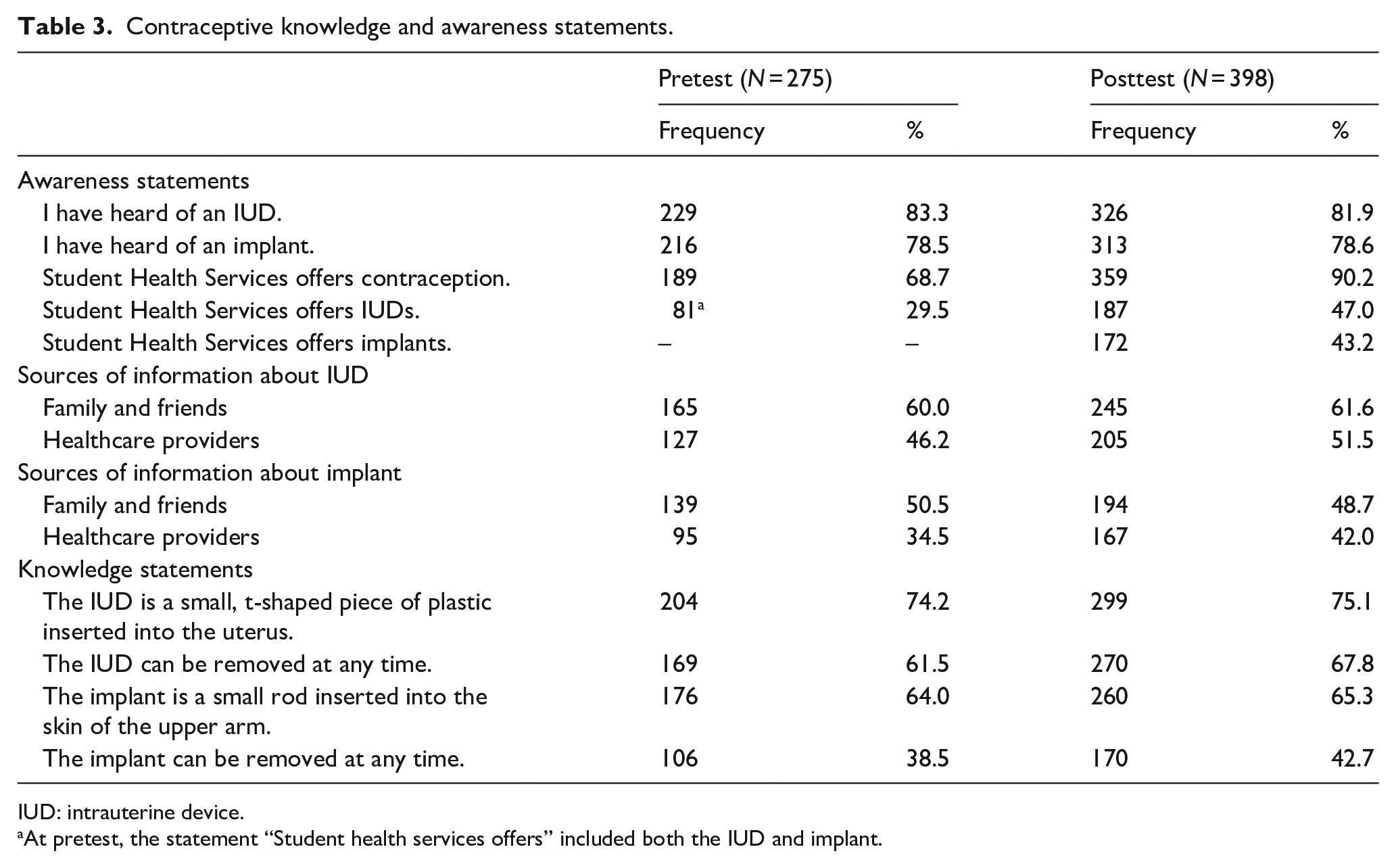
IUD: intrauterine device.
At pretest, the statement “Student health services offers” included both the IUD and implant.
Campaign exposure
Process evaluation
Social media metrics for Twitter, Facebook, and Instagram indicated significant exposure and saturation of the campaign messages. The Klout score, a number between 1 and 100 measuring online social influence, the highest form of engagement, increased by 34 points during the campaign indicating substantial reach and influence of the campaign messages. There were 24,478 tweet impressions, 605 total profile visits, and mentions were up by 100% on Twitter during the campaign. The highest total reach of the Facebook page during the campaign increased from 2000 to 10,000 impressions. The campaign peaked with over 1500 likes, comments, and shares in 1 week. Instagram followers grew by over 40% during the campaign.
Outcome evaluation
Overall, 69% (n = 275) of participants indicated exposure to the campaign messages, which included seeing or hearing one or more campaign messages on any communication channels. The majority of participants (62.8%, n = 250) indicated social media, including Facebook, Twitter, and Instagram, were the best method to educate students about the IUD and implant. The main modes of communication through which participants were exposed to campaign messages included printed flyers or posters around campus (41.7%, n = 166) and word of mouth (27.1%, n = 108) (Table 2). Most participants reported that the campaign was positive (52.8%) and believable (52.0%), while 46.9% found the campaign helpful. Place of residence (e.g. living on or off campus) did not have a significant effect (p > .05) on exposure to the campaign messages.
Campaign impact
Hypothesis 1 correctly predicted that individuals who indicated seeing the campaign reported that the messages prompted them to take action. Based on campaign messages, participants reported searching for additional information about the IUD (18.8%, n = 75)/implant (17.1%, n = 68), talking with friends about an IUD (26.6%, n = 106)/implant (21.6%, n = 86), considering adopting an IUD (15.6%, n = 60)/implant (14.3%, n = 57), and asking a doctor about getting an IUD (14.8%, n = 59)/implant (13.1%, n = 52). Only 7.5% (n = 30) and 10.3% (n = 41) of participants reported taking no action to obtain the IUD or implant, respectively.
Thirteen participants (3.3%) had an IUD inserted and six (1.5%) participants had an implant inserted as a result of seeing the campaign messages. Further, 11 participants indicated they had an appointment for an IUD insertion and 7 participants indicated they had an appointment for an implant insertion (Table 4). Of those who had a LARC appointment or insertion, eight participants had an IUD inserted and one participant had an implant inserted at Student Health Services. Ten participants made an appointment for an IUD insertion at Student Health Services and two participants made an appointment for an implant insertion at Student Health Services. This finding demonstrates support for Hypotheses 2 and 3, suggesting that recall of campaign messages prompted increased uptake of effective contraception.
Behavior prompt statements from campaign messages at posttest (N = 398).

IUD: intrauterine device.
Participants who reported increased exposure to campaign messages were prompted to discuss the IUD with friends. Participants who saw the campaign 2–3 or more times per month were significantly more likely to discuss the IUD with friends than those who were exposed to the campaign 1 time per month or less (p < .05), lending support for Hypothesis 3.
Age was significant in the campaign’s impact on behavior. Participants 20–24 years old were significantly more likely than 18- to 19-year-olds to ask a doctor about the IUD (p = .01), to search for additional information about the IUD (p < .01), to search for additional information about the implant (p < .05), and to talk with family members about the implant (p < .05) when exposed to the campaign messages. Notably, 20- to 24-year-olds were significantly more likely (p = .001) to have an IUD inserted because of the campaign messages than 18- and 19-year-olds (Table 5).
Behavior prompt statements from campaign messages at posttest by age (N = 398).

IUD: intrauterine device.
p < .05, **p ⩽ .01, ***p = .001.
Discussion
The You Have Options social marketing campaign aimed to raise awareness, increase knowledge, and improve uptake of LARC methods among college women. This study presents the implementation and evaluation of a theory-based multi-media social marketing campaign to increase access to LARC methods. Those who saw messages from the You Have Options campaign reported that the campaign prompted them to engage in information-seeking and adoption behaviors compared with those who did not report seeing the campaign. Following the 10-week campaign, 19 individuals reported adoption of a LARC method as a result of exposure to the campaign messages. Thirteen participants (3.3%) had an IUD inserted and six (1.5%) participants had an implant inserted as a result of seeing the campaign messages. In line with the goals of social marketing, this brief campaign influenced measurable behavior change.12,14 Although the adoption of LARC in our sample was low, it reflects the relatively low rates of LARC uptake in the United States. 8 Findings illustrate that the audience-centered nature of social marketing provides an effective framework for increasing LARC adoption on college campuses because it can address barriers, such as knowledge gaps, misinformation, and fear, by providing explicit, simple steps for changing behavior. These findings build on extant research in the field of contraceptive social marketing campaigns demonstrating that improving awareness and access increases contraceptive uptake. 13
Participants’ age impacted the likelihood of behavior change following exposure to campaign messages. Women aged 20–24 years were more likely to ask a doctor about the IUD, to search for additional information about the IUD and implant, and to talk with family members about the implant compared with those aged 18–19 years. In addition, participants aged 20–24 years were more likely to report having an IUD inserted because of the campaign messages. College students aged 20–24 years, typically juniors and seniors, may be more difficult to reach because there are fewer institutional opportunities to address a captive audience (e.g. orientation and first-year experience). This finding suggests that incorporating campaign materials and messages into resident advisor (RA) training, senior capstone courses and leadership development programs (e.g. student government leaders, student athlete captains), may increase the success of contraceptive access social marketing campaigns by targeting older students.
As ACOG continues to strengthen LARC recommendations urging obstetrician-gynecologists to educate and encourage LARC use among young women and adolescents, 34 health communication and social marketing campaigns should emphasize that LARC methods are safe and effective for all women and adolescents. Further, tailoring campaigns to address different audiences’ concerns can decrease barriers to choosing a LARC method.
Increased exposure to the campaign prompted participants to initiate discussions about LARC with friends. This finding builds on previous research indicating that as complexity of an innovation increases, individuals rely more closely on interpersonal communication as they consider behavior change. 35 Thus, participants in this study may be engaging in interpersonal communication about LARC methods prompted by the campaign messages as an initial step toward adopting an IUD or implant. This finding illustrates the subjective norm construct of TPB. Women who discuss these methods with important others may be influenced by their social system to adopt a LARC method. 26
Interestingly, place of residence (e.g. living on or off campus) had no effect on students’ recall of campaign messages. In terms of campaign exposure, this serves as a positive sign indicating that multichannel communication campaigns are effective in reaching students, regardless of time spent on campus. Perhaps including social media and Internet components exposed even commuting students to the LARC messages. From pretest to posttest, knowledge of the IUD increased significantly. Although there was an increase in knowledge about the implant between pretest and posttest, the change was not significant. These findings suggest that changing recommendations regarding the IUD continue to impact college women’s understanding of the method. The campaign improved college women’s knowledge of the IUD, extending prior research demonstrating women desire information but may not be informed about LARC methods.36,37 As a result, LARC campaigns on college campuses can significantly increase contraceptive knowledge in this important demographic.
Approximately 63% of participants indicated that social media was the best method of educating women about LARC. To reach college students, utilization of social media platforms is critical. Social media can be a cost-effective and appropriate way to increase the reach of social marketing campaigns, especially to this demographic. Beyond campaign reach and exposure, social media analytics indicated increased audience engagement with the campaign messages, illustrating that social media serves as an important channel for health information among college-aged women. This finding expands on previous research noting that the incorporation of social media into health campaigns may increase the influence of the campaign and potential for behavior change.16,38 Surprisingly, participants also indicated greatest exposure to the campaign messages through printed flyers, posters, and word of mouth. This provides further evidence that social marketing campaigns should include multiple communication channels to bridge traditional and social media and capitalize on the power of interpersonal communication to increase campaign impact. For example, integrating social and traditional media through QR codes on posters may link the target audience with interactive social media and prompt online dialogue. Incorporating a variety of communication channels may contribute to message saturation, while avoiding message fatigue.
Conclusion and limitations
The campaign only operated for 10 weeks due to budget and time constraints, limiting its overall reach and potential impact. Continuing the campaign for a longer period of time would provide greater opportunity to test the effectiveness of the campaign on LARC adoption. Because the study included only women in a southeastern university, the findings may not be generalizable to other, geographically dissimilar populations. In addition, the participants were primarily White; therefore, findings may not be generalizable to demographically diverse populations. Since participants were students at a university, they are more educated and likely maintain a higher socioeconomic position (SEP) compared to the general population.
Because the survey was conducted electronically in Student Health Services, there were repeat visitors in the health center who could not take the survey more than once, limiting recruitment. In addition, the survey items assessed various retrospective data about campaign messages and exposure. As a result, there could be limitations due to incorrect recall. Future research should further examine how age impacts college women’s LARC adoption behavior.
This study supports previous research indicating the importance of utilizing theory-based audience research in campaign implementation. Findings from this study provide evidence for a unique social marketing approach to increase adoption of LARC methods on college campuses. College women are an important population in reducing the burden of unintended pregnancy in the United States. This study provides the opportunity to normalize LARC methods among college women through multichannel social marketing campaigns that are cost-efficient and have high reach. This study may serve as a model for other universities to raise awareness, increase knowledge, and improve access to LARC methods among young women.
Supplemental Material
sj-pdf-1-map-10.1177_23992026211003499 – Supplemental material for You Have Options: Implementing and evaluating a contraceptive choice social marketing campaign
Supplemental material, sj-pdf-1-map-10.1177_23992026211003499 for You Have Options: Implementing and evaluating a contraceptive choice social marketing campaign by Beth Sundstrom, Andrea L DeMaria, Merissa Ferrara, Stephanie Meier, Kerri Vyge, Deborah Billings, Dee DiBona and Bridget M McLernon Sykes in Medicine Access @ Point of Care
Supplemental Material
sj-pdf-2-map-10.1177_23992026211003499 – Supplemental material for You Have Options: Implementing and evaluating a contraceptive choice social marketing campaign
Supplemental material, sj-pdf-2-map-10.1177_23992026211003499 for You Have Options: Implementing and evaluating a contraceptive choice social marketing campaign by Beth Sundstrom, Andrea L DeMaria, Merissa Ferrara, Stephanie Meier, Kerri Vyge, Deborah Billings, Dee DiBona and Bridget M McLernon Sykes in Medicine Access @ Point of Care
Supplemental Material
sj-pdf-3-map-10.1177_23992026211003499 – Supplemental material for You Have Options: Implementing and evaluating a contraceptive choice social marketing campaign
Supplemental material, sj-pdf-3-map-10.1177_23992026211003499 for You Have Options: Implementing and evaluating a contraceptive choice social marketing campaign by Beth Sundstrom, Andrea L DeMaria, Merissa Ferrara, Stephanie Meier, Kerri Vyge, Deborah Billings, Dee DiBona and Bridget M McLernon Sykes in Medicine Access @ Point of Care
Footnotes
Acknowledgements
The authors would like to acknowledge the support of the College of Charleston’s Student Health Services in the conduct of this research. The authors thank the members of the Women’s Health Research Team for their assistance.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported in part by the College of Charleston’s Office of Undergraduate Research and Creative Activities (URCA) and the Summer Undergraduate Research with Faculty (SURF) Program. This research was also supported in part by the College of Charleston’s Humanities and Social Sciences Dean’s discretionary funds.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
