Abstract
Aliskiren (ALS) is a direct renin inhibitor with low bioavailability and high drug cost. The goal of this study was to increase the bioavailability of ALS through nanoformulation. The optimized formulation was then evaluated in spontaneously hypertensive rats (SHRs). We developed an ALS poly(lactic-
Introduction
One quarter of the world population lives with hypertension, a precursor of more severe cardiovascular disease; therefore, effective regulatory medications have risen in importance. 1 Blood pressure maintenance is typically controlled through the renin–angiotensin–aldosterone system, which prompts renin secretion in response to low plasma volume, decreased renal blood flow, or increased sympathetic central nervous system activity. 2 In this system, renin enzymatically cleaves angiotensinogen into the inactive peptide angiotensin I. Angiotensin converting enzymes (ACEs) then process angiotensin I into angiotensin II, which interacts with angiotensin II type 1 receptors inducing vasoconstriction and the release of catecholamines. Although ACE inhibitors block the formation of angiotensin II, angiotensin I production continues and may be converted to angiotensin II via other metabolic pathways. 3 While multiple inhibition checkpoints are available to prevent angiotensin II formation, inhibition of renin, as the first enzyme in the pathway, is a logical option. 4 Inhibition at this step may increase circulating renin; however, renin inhibitors block enzyme activity. 2
Aliskiren (ALS) is a non-peptide, orally active renin inhibitor discovered using X-ray crystallographic structure analysis and molecular modeling. 4 In March 2007, ALS became the first in class renin inhibitor to receive approval from the United States Food and Drug Administration (FDA) 5,6 and is effective as a monotherapy or in combination with other antihypertensive drugs, such as hydrochlorothiazide. 3,6 A half-life of approximately 23–36 h provides suitability for once daily ALS dosing, typically 150 or 300 mg in humans. Side effects have included headache, diarrhea, and dizziness, but these were reported in less than 3% of patients. 7
Although ALS has positive attributes in regard to blood pressure maintenance, such as rapid maximum plasma concentrations (
Particle size plays a role in NP surface property modifiability which may affect degradation time, elimination processes, and intracellular uptake. When the diameter of NPs are reduced below 100 nm, degradation in the mononuclear phagocytic system can be avoided, enabling extended circulation in plasma and increasing the probability of delivery to the site of action. 18 Particle charge also has a significant effect on NP distribution. 9,19 Adherence of cationic NPs to the negatively charged cell membrane essentially increases cellular uptake.
The FDA-approved, biodegradable, linear copolymer poly(lactic-
In an effort to reduce the amount of ALS per dose and thereby reduce associated drug costs, our laboratory employed nanoformulation using PLGA. Various parameters, including organic solvent choice and stabilizer concentration, were examined to determine an optimized formula. Pharmacokinetic parameters were assessed in rats to determine relative bioavailability. As ALS has been shown to exhibit renoprotective properties, 24,25 renal parameters were examined for both formulations. This study sought to develop an ALS-NP formulation which would exhibit enhanced bioavailability and comparable renal parameters.
Materials and methods
Chemicals
ALS hemifumarate and verapamil (VER) were purchased from ChemScene, LLC (Monmouth Junction, New Jersey, USA) and Selleck Chemicals (Houston, Texas, USA), respectively. Dichloromethane, didodecyldimethylammonium bromide (DMAB), and PLGA (50:50 copolymer compositions; molecular weight 30,000–60,000 Da) were obtained from Sigma-Aldrich (St. Louis, Missouri, USA). O-phosphoric acid (85%), ammonium hydroxide, acetone, ethyl acetate, high-performance liquid chromatography (HPLC) grade water, and acetonitrile were acquired from Fisher Scientific (Fair Lawn, New Jersey, USA). All solvents used for LC-mass spectrometry (MS)/MS analysis were of LC-MS grade from Honeywell-Burdick and Jackson (Muskegon, Michigan, USA).
Formulation of NPs
NP formulations were prepared based on a previously described method 26 with some modifications such as using a variety of solvents, stabilizer concentrations, or centrifugation speeds. 27
Effect of varying organic solvents
The emulsion–diffusion–evaporation method was employed with slight alterations in this study. In brief, 50 mg of PLGA was completely dissolved in 3 mL of dichloromethane, ethyl acetate, or ethyl acetate/acetone. To the organic solvent, 10 mg of ALS was added under moderate stirring. Simultaneously, 0.25% w/v of DMAB was placed in water (6 mL) and allowed to fully dissolve under moderate stirring. While the aqueous phase was under moderate stirring, organic phase was added dropwise. The suspension was sonicated for 5 min at 20 kHz and then the contents were stirred (30–40 min) under a chemical hood to facilitate solvent evaporation. Upon completion, each solution was centrifuged at 10,000 r/min using a Sorvall Biofuge Stratos centrifuge equipped with a Heraeus fixed angle rotor (#3335) made by Thermo Fisher Scientific Inc. (Waltham, Massachusetts, USA) for 5 min. The supernatant was collected to measure entrapment efficiency.
Effect of varying stabilizer concentration and centrifugation speed
The stabilizer concentrations of DMAB included 0.10%, 0.25%, 0.50%, and 1.00% w/v, while the centrifugation speeds were 10,000 or 12,000 r/min (15,554 or 18,665 g). As each parameter has shown the ability to alter NP characteristics in a previous study, 28 these variations allowed for the detection of an optimal NP formulation.
NP characteristics
Formulations were evaluated using various NP criteria: entrapment efficiency, particle size, zeta potential, and polydispersity index (PDI).
Entrapment efficiency
For all measurements of entrapment efficiency, a calibration curve was constructed using solutions of known ALS concentrations (10–1000 µg/mL) and the corresponding absorbance values detected using ultraviolet–visible spectroscopy (Eppendorf Biophotometer, Hauppauge, New York, USA) with a wavelength set at 260 nm.
A 1:2 ratio dilution of collected supernatant to HPLC-grade acetonitrile was performed, and the corresponding absorbance values were measured. These values were employed for the calculation of entrapment efficiency as previously described. 28
Particle size, zeta potential, and PDI
A NICOMP Particle Sizer (Particle Sizing Systems, Port Richey, Florida, USA) was used to evaluate particle size via dynamic light scattering, while zeta potential was approximated under an electrical field with a foundation of electrophoretic mobility. The PDI of each formulation, as an indication of particle size distribution, was also measured using the NICOMP Particle Sizer.
Animals and drug administration
In order to administer the NP formulation to the animals, a fresh batch of ALS-NP (40 mL, final volume of 35 mL) was prepared by dissolving 350 mg of PLGA polymer and 70 mg of ALS (ALS hemifumarate salt) in organic phase consisting of 21 mL of ethyl acetate. For the aqueous phase, 1% w/v DMAB stabilizer was added to 42 mL of water. Organic phase was added to aqueous phase in a dropwise manner and sonicated for 5 min at 20 kHz. After sonication, solutions were constantly stirred at 750 r/min to facilitate organic phase evaporation. Following evaporation, NP solution was centrifuged at 10,000 r/min for 5 min and supernatant was collected. The parameters of the formulation dosed are presented in Table 1.
Nanoformulation parameters of dosed ALS NPs.
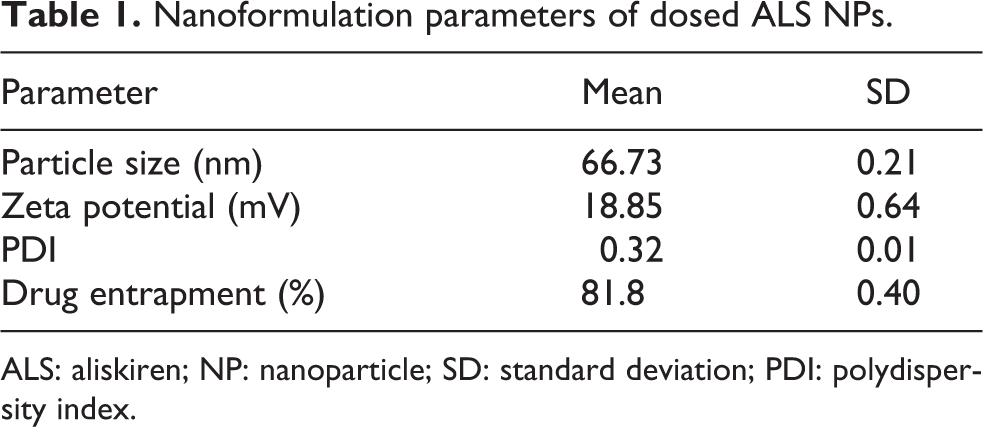
ALS: aliskiren; NP: nanoparticle; SD: standard deviation; PDI: polydispersity index.
Fourteen male spontaneously hypertensive rats (SHRs; 265.36 ± 8.04 g), approximately 7 weeks old, were randomly assigned to receive either orally gavaged ALS (30 mg/kg) or ALS-NP (equivalent to ALS dose) in accordance with an animal protocol approved by the East Tennessee State University Committee on Animal Care. On day 0, one blood sample (0.5 mL) was taken, via cannulation, for baseline biomarker assay as well as a pre-dose ALS time point along with a 12-h urine collection (baseline). On day 1, rats were administered ALS (
Sample preparation and LC-MS/MS conditions
The detection method used in this study was based upon a previous method by Burckhardt et al. 29 Sample preparation was achieved using 1 mL Isolute supported liquid extraction (SLE+) cartridges from Biotage (Charlotte, North Carolina, USA). The sample analysis occurred on a Shimadzu LCMS-IT-TOF (ion trap-time of flight) system from Shimadzu Scientific (Columbia, Maryland, USA). This system consisted of two LC-AD20 pumps, a SIL-20ACHT autosampler, an in-line degasser (DGU-20A3), and a CTO-20A column oven. Chromatographic separations were carried out using a C18 XBridge column (150 × 4.6 mm, 3.5 µm) from Waters (Milford, Massachusetts, USA).
SLE+ of ALS and the internal standard, VER, utilized a 0.5 M ammonium hydroxide buffer pretreatment and elution with methyl-
Real sample peak area ratios were compared against linear regression equations of daily calibration curves to calculate ALS concentrations in these samples (coefficient of variation of <5%).
Pharmacokinetic parameters
Pharmacokinetic sampling occurred at 0, 0.5, 1, 2, 4, 6, 8, 12, and 24 h post-dose. Pharmacokinetic parameters, including half-life (
Electrolyte analysis
An EasyLyte electrolyte analyzer (Medica Corporation, Bedford, Massachusetts, USA) was utilized to assay sodium (Na) and potassium (K) concentration in both plasma and urine. An equation incorporating ion concentration (
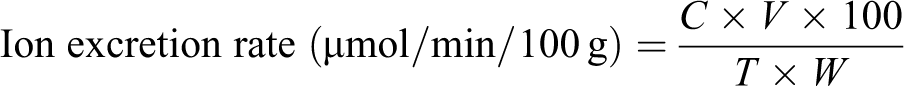
Kidney injury molecule-1 assay
Kidney injury molecule-1 (KIM-1) concentration was determined in urine using a Kamiya Biomedical Company enzyme-linked immunosorbent assay following manufacturer instructions (Seattle, Washington, USA). Briefly, urine samples were removed from −80°C, brought to room temperature, and diluted as 1:3 provided diluent prior to analysis. One hundred microliters of rat KIM-1 calibrator (0.1–10 ng/mL) or sample were added to respective wells in duplicate. The covered plate was then incubated at room temperature for 2 h on an orbital shaker. Following four washes with wash solution, detection antibody (100 µL) was added to each well and then shaken for 20 min protected from light. Then horseradish peroxidase-streptavidin (100 µL) was added following four more washes. After a subsequent shaking, light-protected incubation (20 min), the plates were washed four times. One hundred milliliters of tetramethylbenzidine substrate solution were added and then incubated for 10 min under the prior incubation conditions. Finally, 100 µL of stop solution was added and the plate was read at 450 nm. A four-parameter logistics curve fit was established using MyAssays software (Sussex, England).
Blood urea nitrogen assay
A blood urea nitrogen (BUN) enzymatic assay kit (Bioo Scientific Corporation, Austin, Texas, USA) was used to analyze baseline and post-dose plasma. Samples and kit reagents were brought to room temperature and then 5 µL of standard (0–200 ppm) or sample was added to respective wells in duplicate. One hundred and fifty microliters of urease mixture were transferred into the wells and gently mixed. Following a 15-min room temperature incubation, alkaline hypochlorite (150 µL) was added. The plate was read at 620 nm after a 10-min incubation. The slope and intercept of the standard curve data trend line was used to determine BUN concentration.
Creatinine assay
Plasma and urine samples were analyzed for creatinine concentration using a creatinine colorimetric/fluorometric assay kit (BioVision, Milpitas, California, USA). Fifty microliters of plasma, 5 µL dilute urine (prior to analysis urine was diluted 1 µL urine to 24 µL creatinine assay buffer), or 0–10 µL creatinine standard (1 nmol/µL) was added to the microplate wells. The urine and standard volumes were adjusted to 50 µL with creatinine assay buffer and then 50 µL reaction mix was added to each well. Following a 1-h incubation at 37°C, the plate was read at 570 nm. The respective concentrations were determined using a standard curve.
Data treatment and statistical analysis
In the formulation optimization stage, each experiment was carried out in triplicate. Variation in centrifugation speeds and pharmacokinetic parameters was compared with the use of a Student’s
Results
Effect of varying organic solvents
Different organic solvents were examined to optimize results in terms of drug entrapment efficiency.
Entrapment efficiency
For each known concentration of ALS formulation, the absorbance value was measured in triplicate, and the average value was plotted against the known concentration of ALS solution. With an
Effect of various organic solvents at 0.25% w/v DMAB and 10,000 r/min on ALS entrapment efficiency.
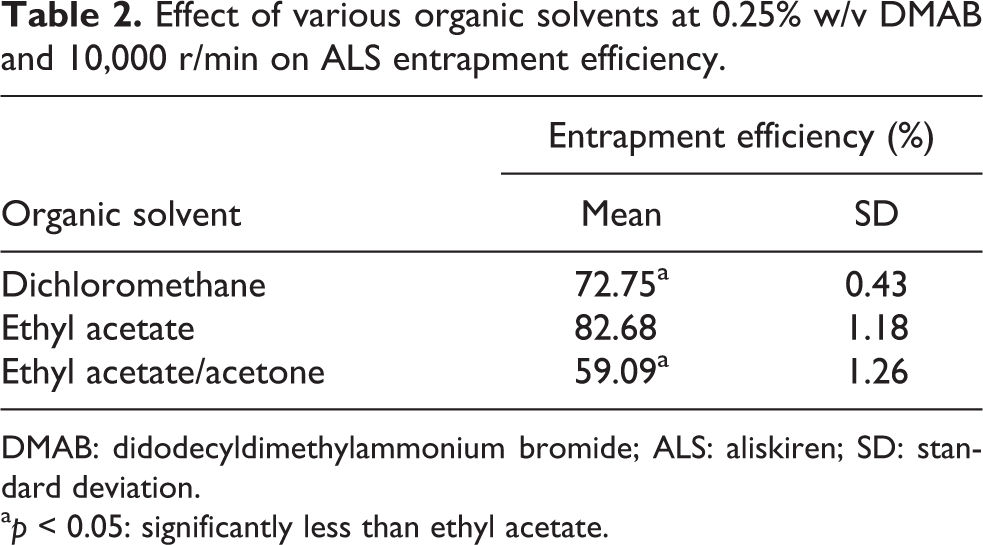
DMAB: didodecyldimethylammonium bromide; ALS: aliskiren; SD: standard deviation.
a
Effects of varying stabilizer concentration and centrifugation speed
The use of increasing concentrations of stabilizer along with variation in centrifugation speed allowed for the optimization of NP formulation.
Particle size
When DMAB stabilizer concentration or centrifugation speed was varied, the first characteristic analyzed was particle size (Figure 1). Centrifugation speed alteration produced significantly different particle sizes for the PLGA-NP formulations containing 0.10%, 0.50%, and 1.00% stabilizer concentrations. The smallest acquired particle size (67.27 ± 0.87 nm) was found with the use of 0.50% w/v DMAB stabilizer and a centrifugation speed of 12,000 r/min.
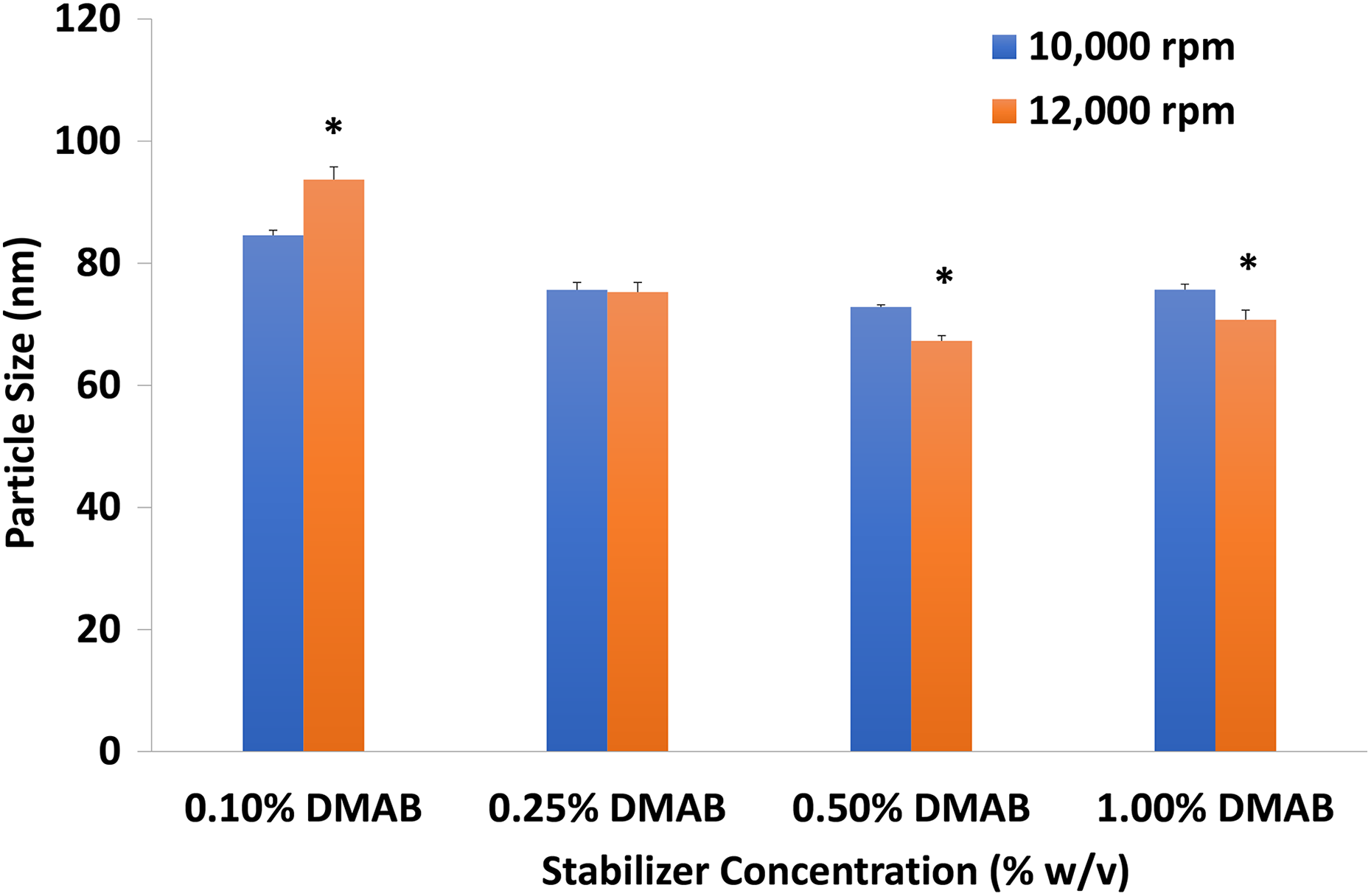
Effect of DMAB concentration at 10,000 or 12,000 r/min on NP particle size. DMAB: didodecyldimethylammonium bromide; NP: nanoparticle; p < 0.05: significantly different from 10,000 rpm.
Zeta potential
For zeta potential, variation in centrifugation speed produced a significant change within the formulations employing 0.50% and 1.00% stabilizer concentration (Figure 2). When analyzed, the highest zeta potential (18.73 ± 0.03 mV) was seen with 1.00% w/v DMAB stabilizer and 10,000 r/min centrifugation speed.
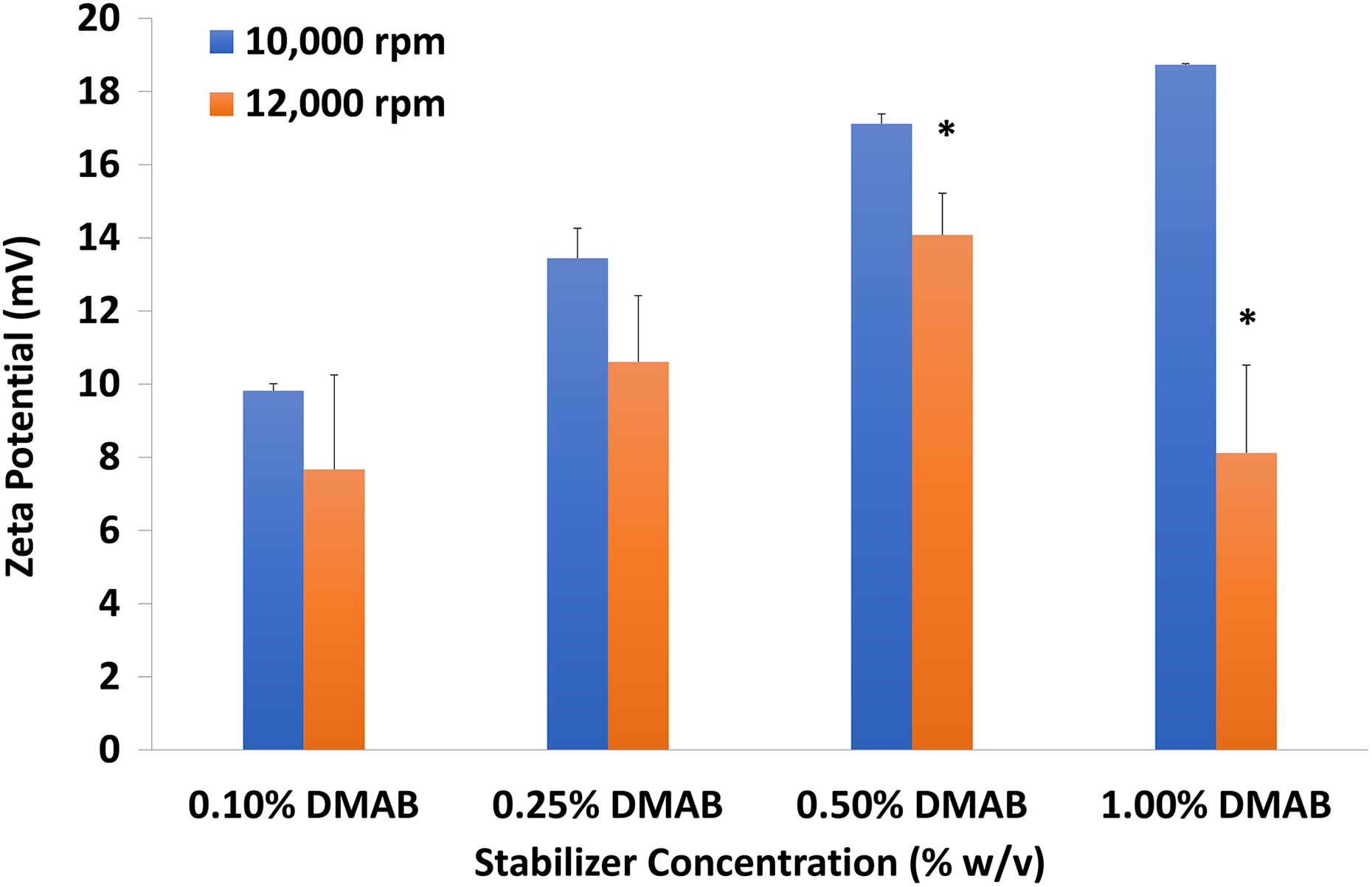
Effect of DMAB concentration at 10,000 or 12,000 r/min on NP zeta potential. DMAB: didodecyldimethylammonium bromide; NP: nanoparticle; p < 0.05: significantly different from 10,000 rpm.
Polydispersity index
In this study, the best PDI (0.15 ± 0.03) value was observed when employing 0.25% w/v DMAB stabilizer and 10,000 r/min centrifugation speed (Figure 3). However, the chosen formulation of 1.00% w/v DMAB stabilizer at 10,000 r/min centrifugation speed displayed a value of 0.32 ± 0.01 for PDI. Though a high value, the formulation demonstrated sufficiently consistent dispersion of PLGA-NPs in the final formulation. A significant change was observed in PDI only in the formulation using 0.50% stabilizer concentration.
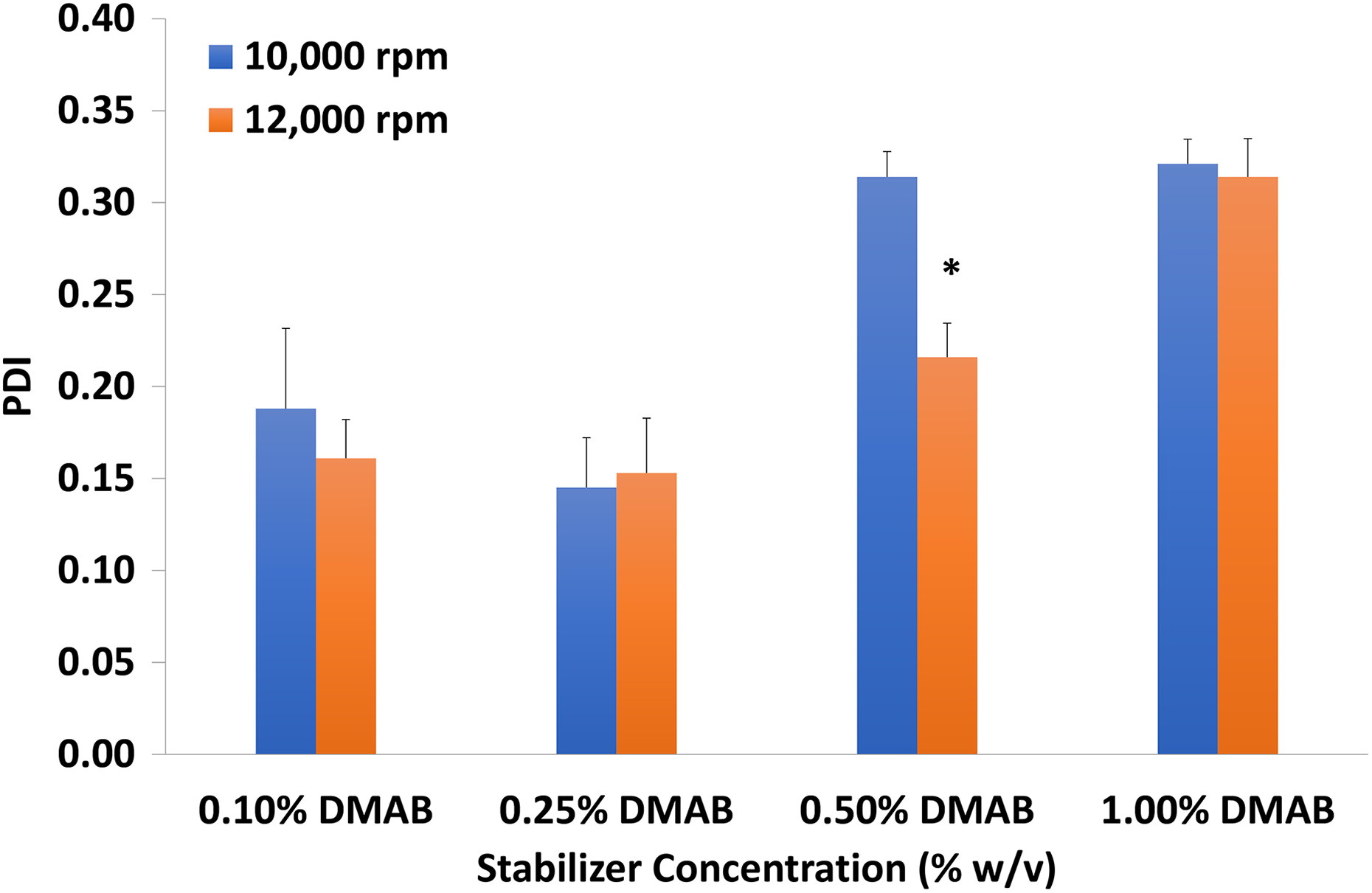
Effect of DMAB concentration at 10,000 or 12,000 r/min on NP PDI. DMAB: didodecyldimethylammonium bromide; NP: nanoparticle; PDI: polydispersity index; p < 0.05: significantly different from 10,000 rpm.
Entrapment efficiency
Entrapment efficiency was significantly different between centrifugation speed in all formulations using 0.10%, 0.25%, 0.50%, and 1.00% stabilizer concentrations. Although the highest entrapment efficiency (82.68 ± 1.18%) was achieved when 0.25% w/v DMAB stabilizer and 10,000 r/min centrifugation speed were used (Figure 4), we chose the formulation of 1.00% w/v DMAB stabilizer at 10,000 r/min centrifugation speed displaying 71.62 ± 0.11% for entrapment efficiency, due to sufficient encapsulation of ALS, optimized particle size, and zeta potential values.
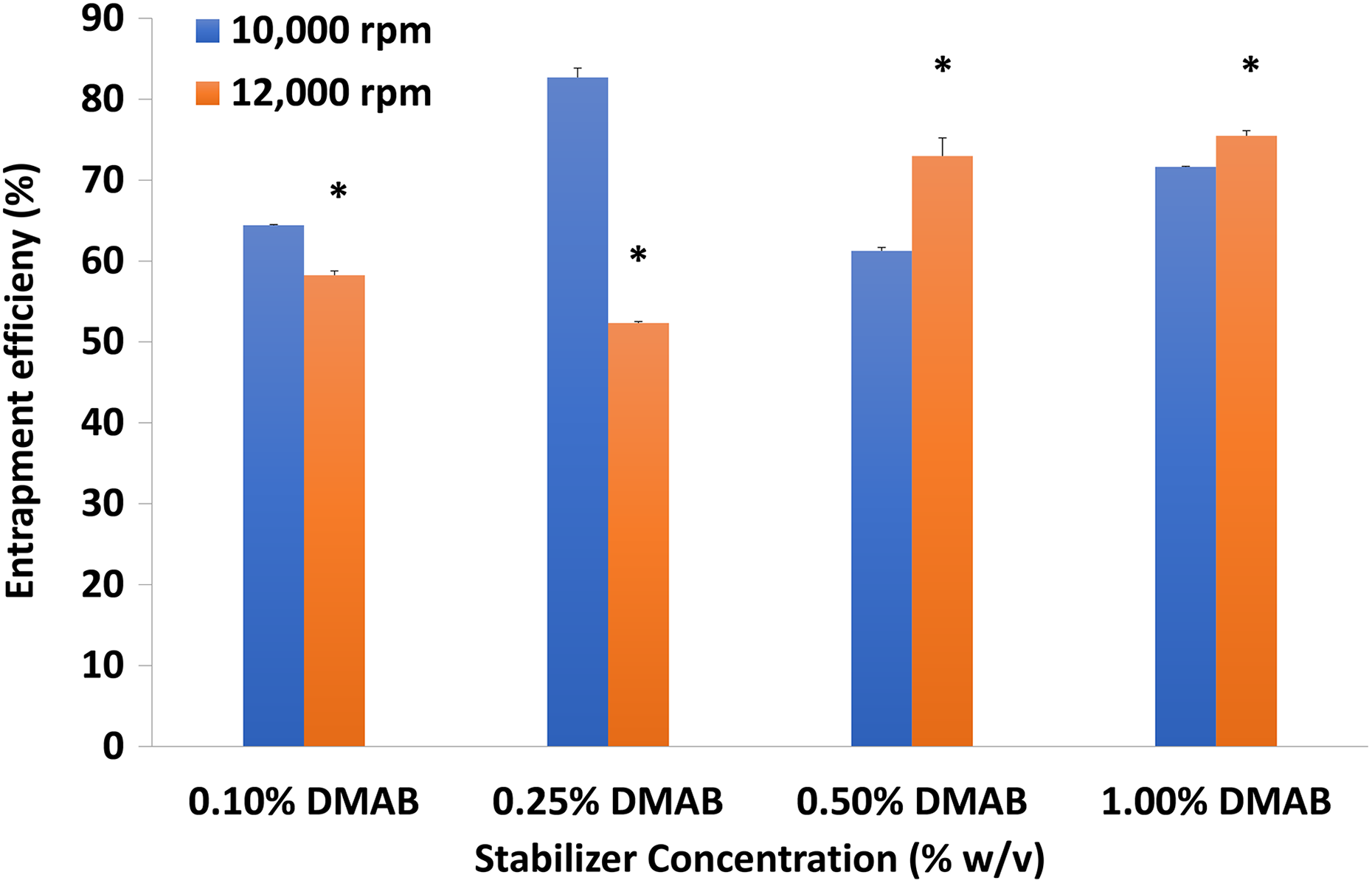
Effect of DMAB concentration at 10,000 or 12,000 r/min on NP entrapment efficiency. DMAB: didodecyldimethylammonium bromide; NP: nanoparticle; p < 0.05: significantly different from 10,000 rpm.
Pharmacokinetic parameters
Mass chromatograms (Figure 5) associated with the
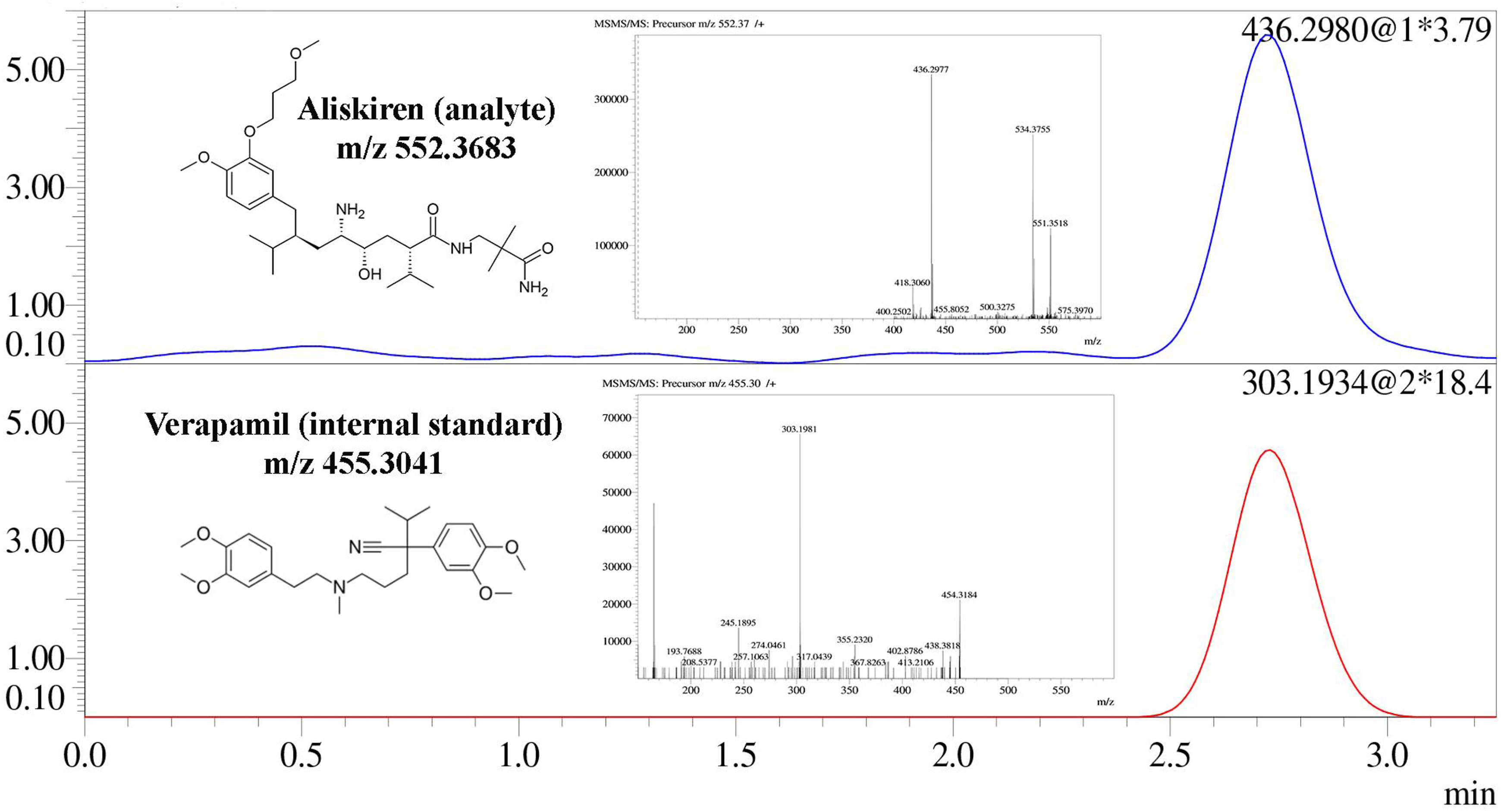
Mass chromatogram of ALS and VER. ALS: aliskiren; VER: verapamil.
Figure 6 shows the plasma concentration–time curve obtained from each formulation, while Table 3 denotes individual parameters. The
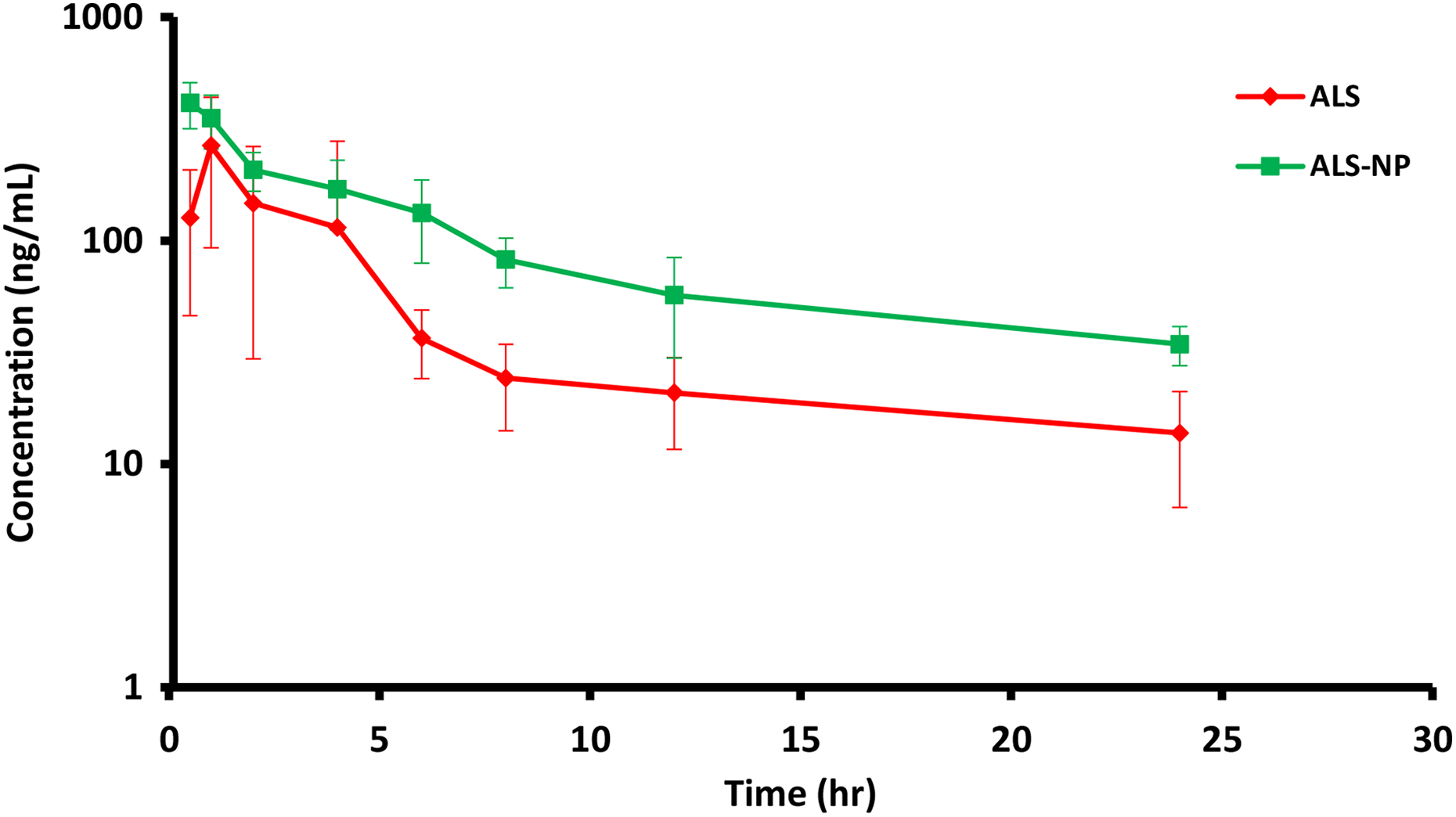
Plasma concentration–time curves following a single oral dose of ALS (30 mg/kg) and equivalent ALS-NP in rats. ALS: aliskiren; ALS-NP: aliskiren-loaded nanoparticle.
The pharmacokinetic parameters of ALS following a single oral dose of ALS (30 mg/kg) or a PLGA NP equivalent in rats.a
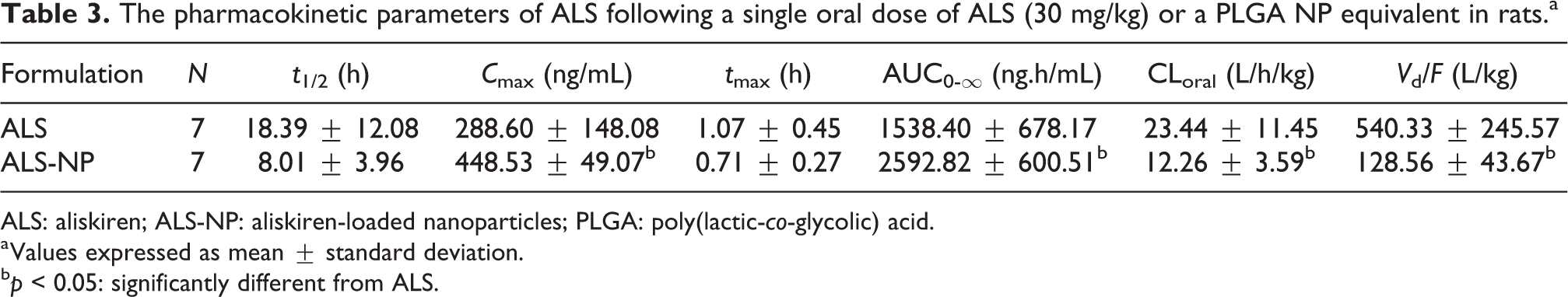
ALS: aliskiren; ALS-NP: aliskiren-loaded nanoparticles; PLGA: poly(lactic-
a Values expressed as mean ± standard deviation.
b
Electrolyte analysis
As ANOVA detected significance among the groups (
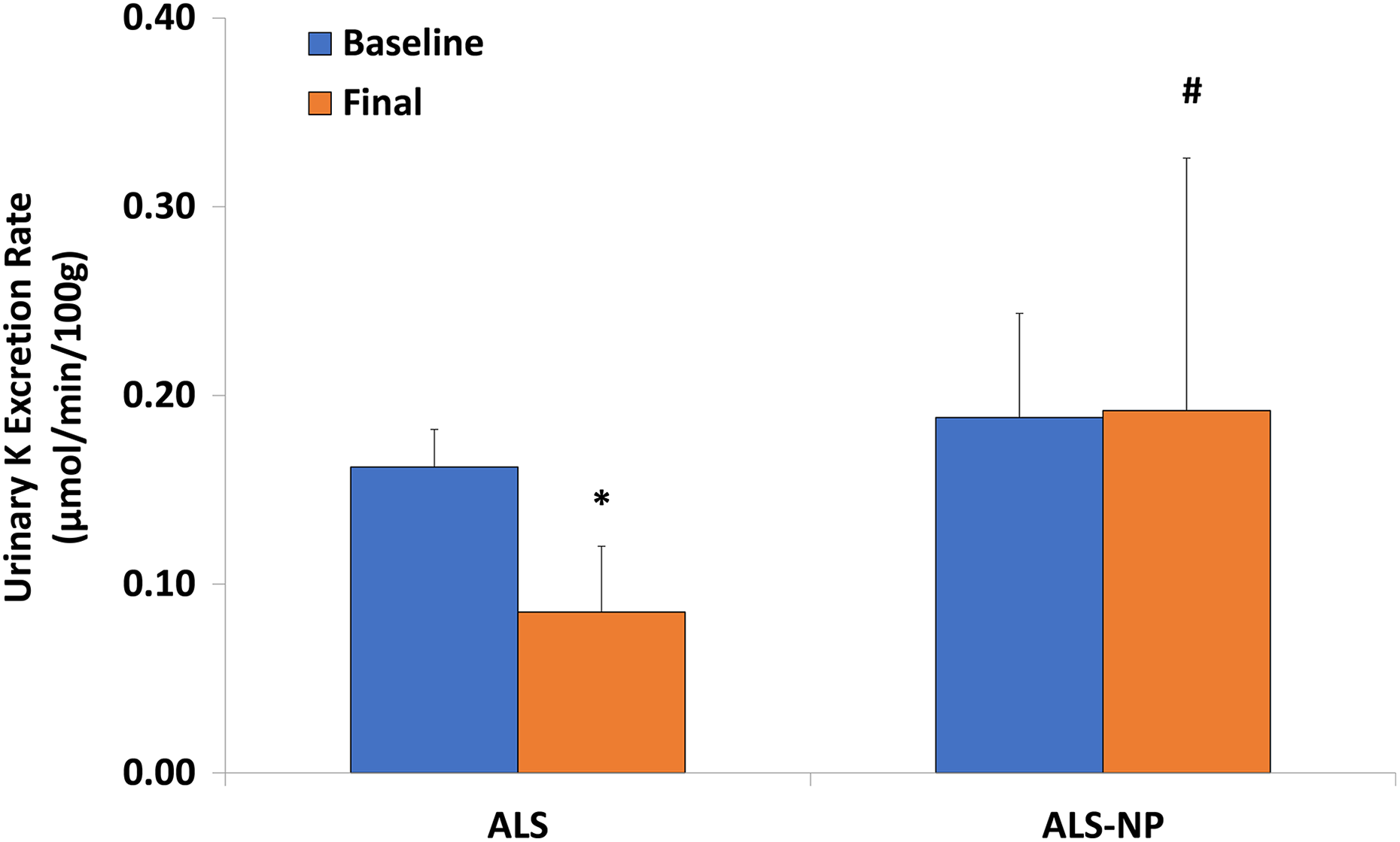
Effect of formulation on urinary K excretion rate in rats. K: potassium; ALS: aliskiren. *
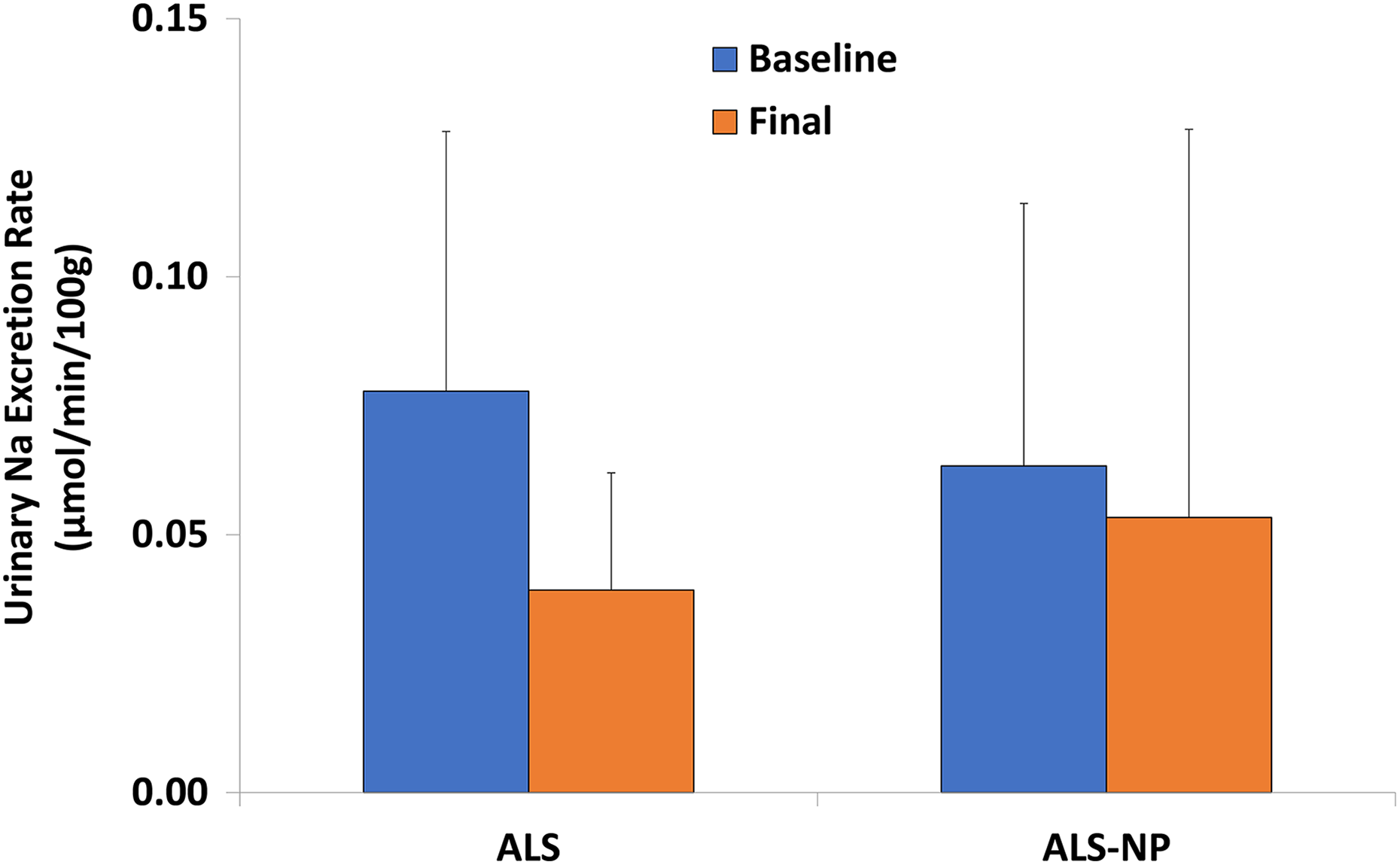
Effect of formulation on urinary Na excretion rate in rats. Na: sodium.
Plasma electrolyte concentrations on day 2.a
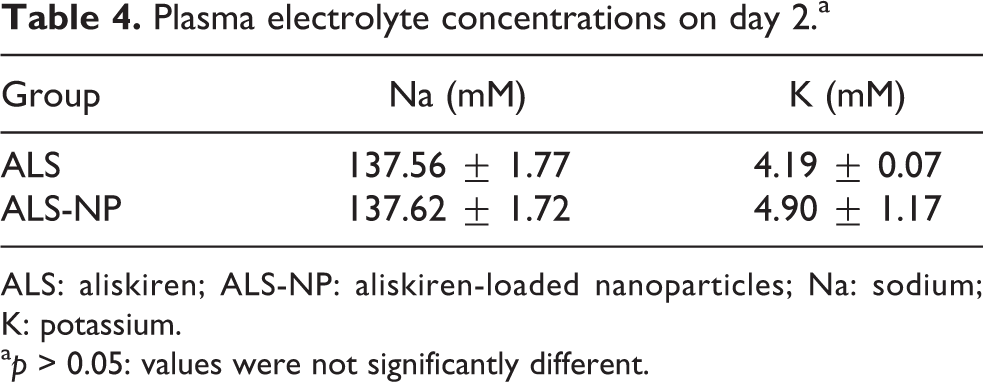
ALS: aliskiren; ALS-NP: aliskiren-loaded nanoparticles; Na: sodium; K: potassium.
a
Urinary KIM-1 assay
ANOVA testing showed a significant alternation between groups (
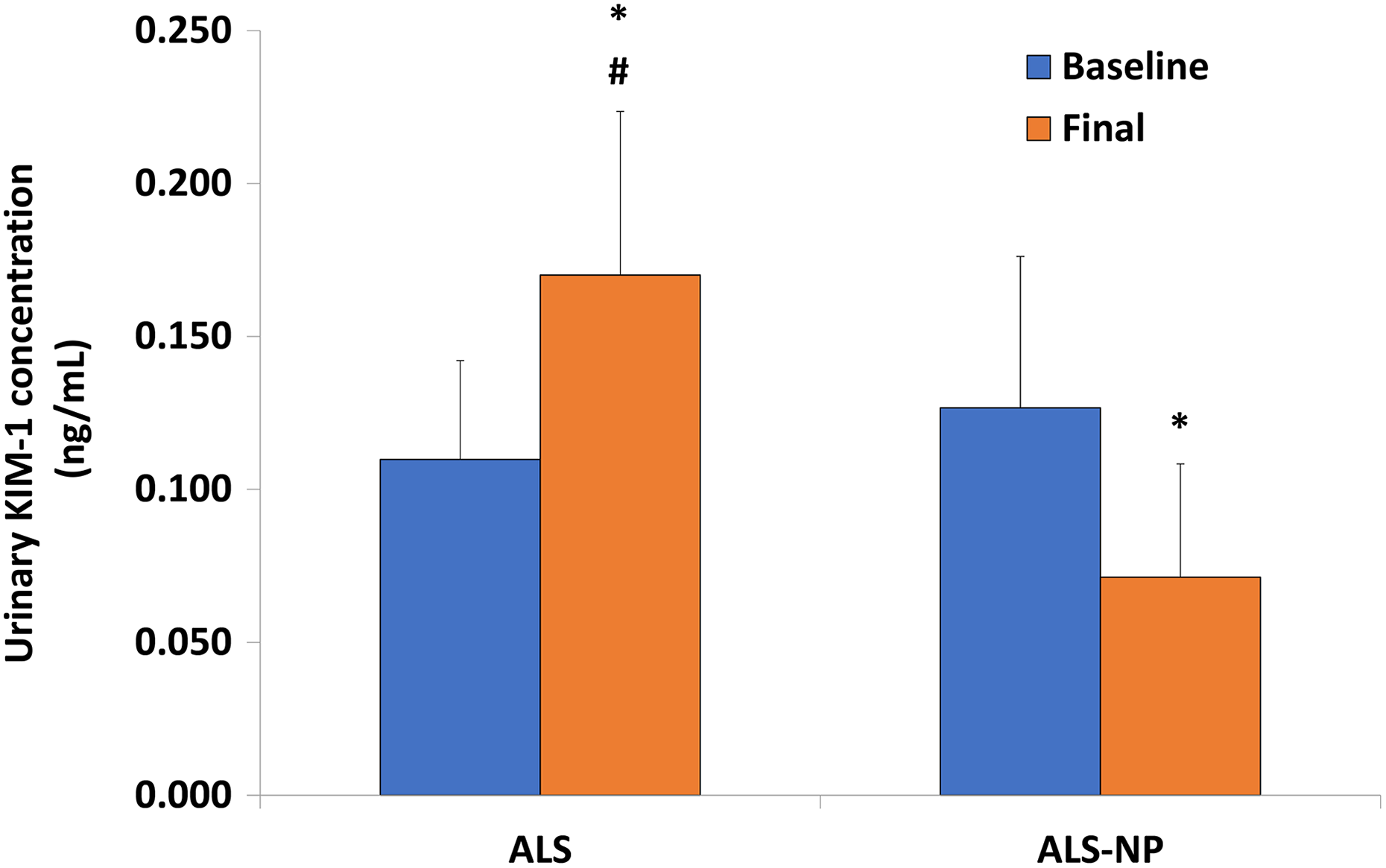
Effect of formulation on urinary KIM-1 in rats. KIM-1: kidney injury molecule-1; ALS: aliskiren; ALS-NP: aliskiren-loaded nanoparticle. *
BUN assay
Significant (ANOVA;
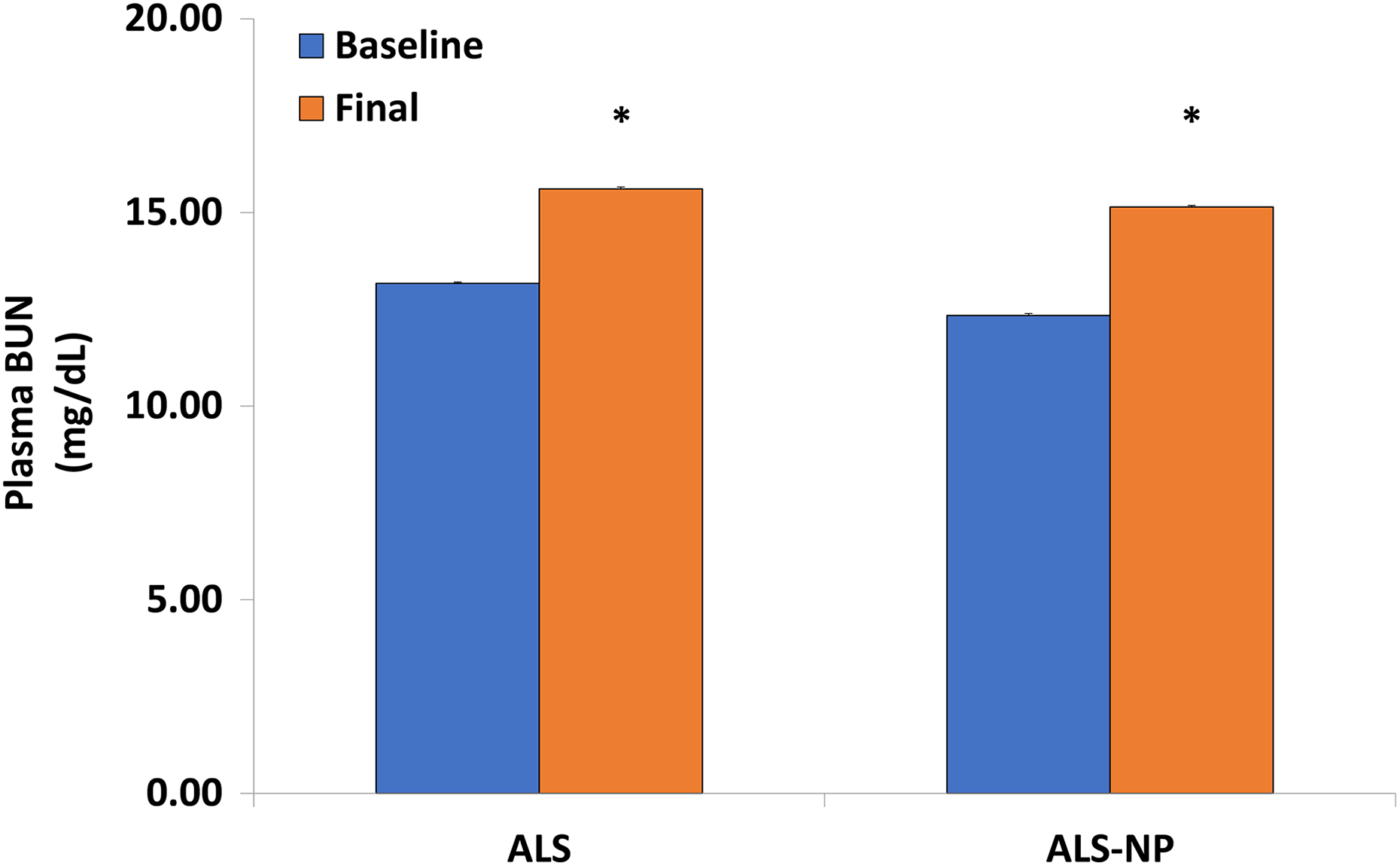
Effect of formulation on plasma BUN in rats. BUN: blood urea nitrogen. *
Creatinine assay
Following group testing via ANOVA, creatinine levels were found to be significantly (
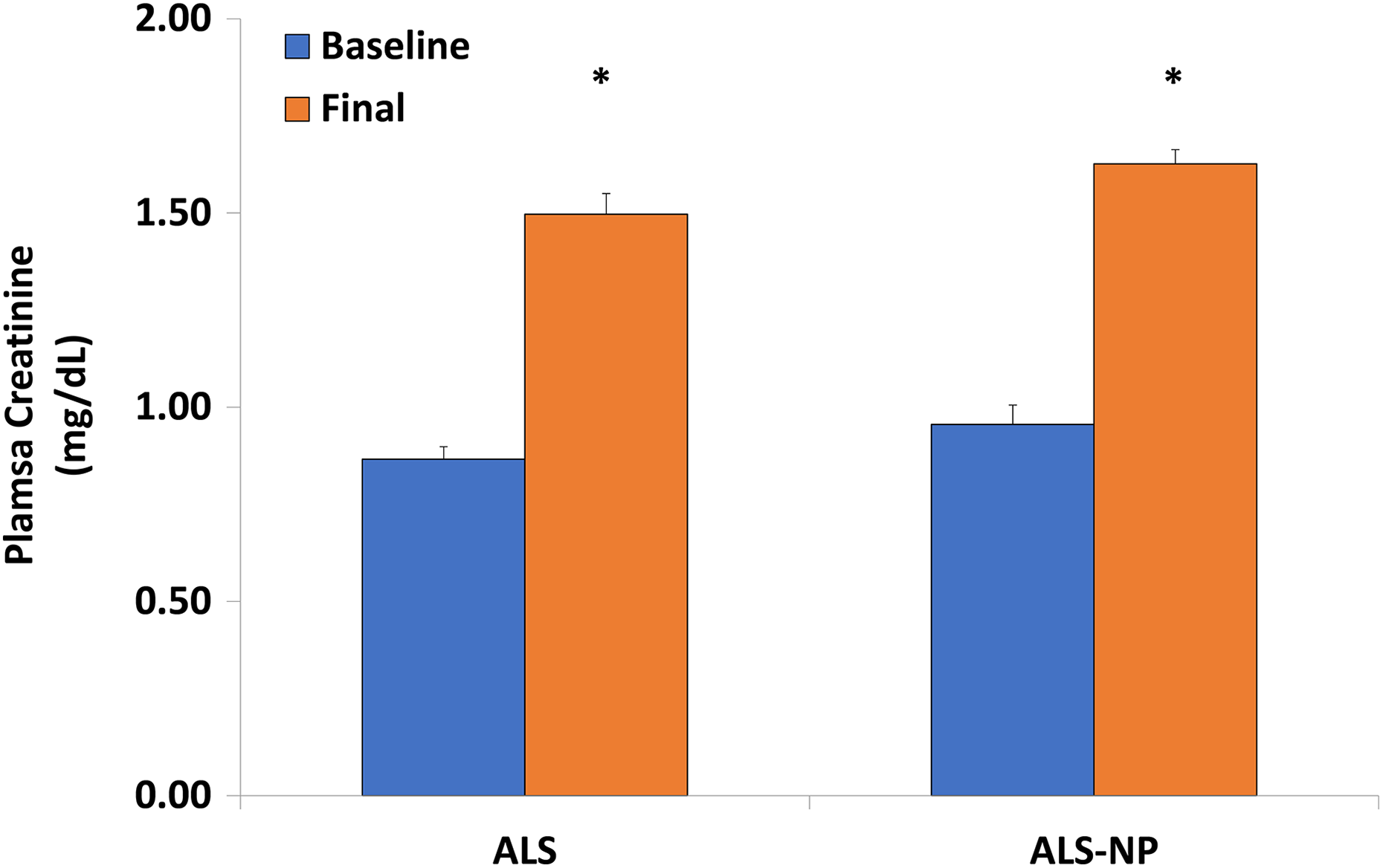
Effect of formulation on plasma creatinine in rats. *
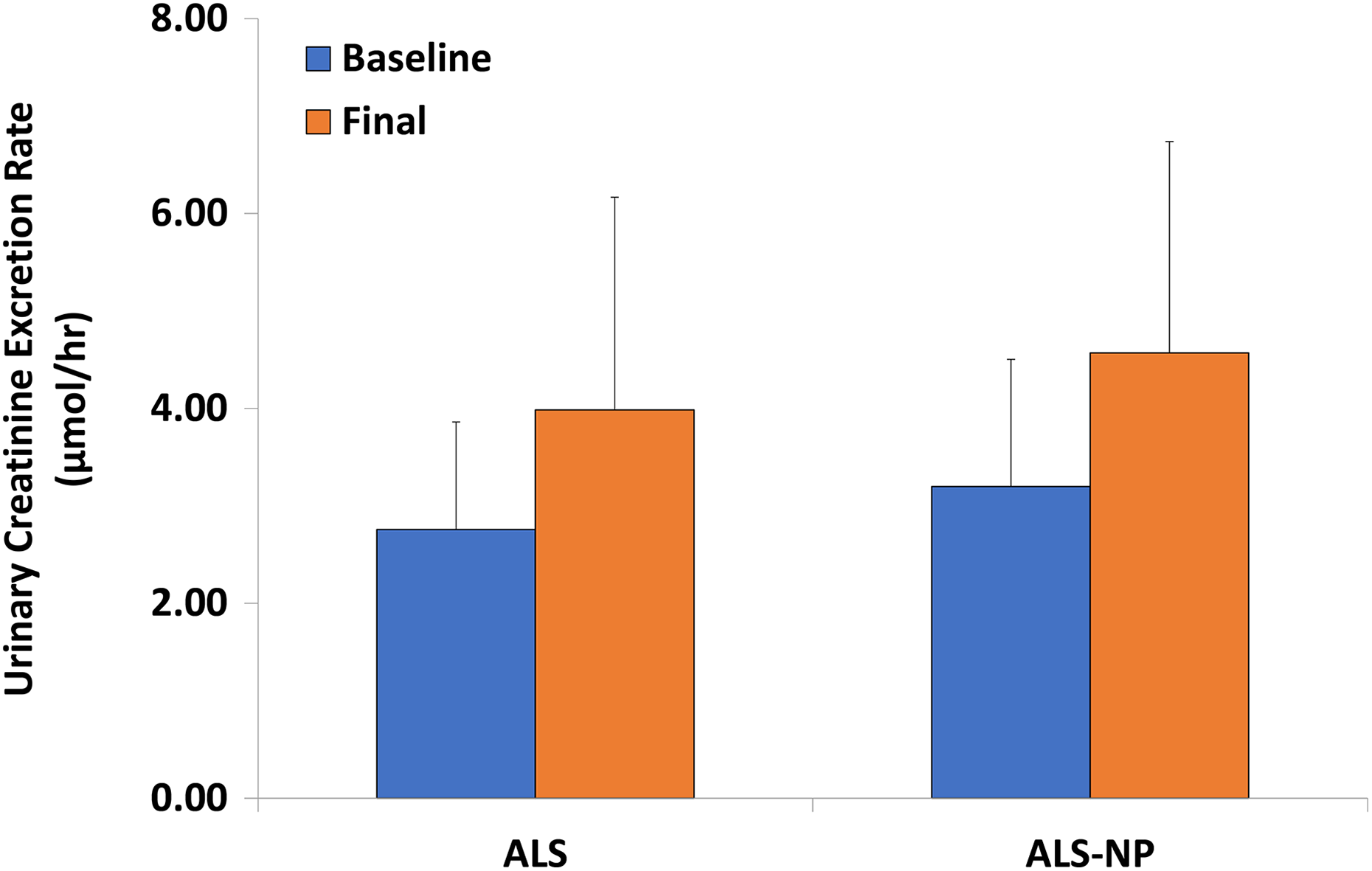
Effect of formulation on urinary creatinine excretion rate in rats.
Discussion
Different organic solvents were examined to optimize results in terms of drug entrapment efficiency. The role of the organic solvent is to provide adequate solubility for the drug, while ultimately promoting drug entrapment. Of the solvents considered (dichloromethane, ethyl acetate, and ethyl acetate/acetone), entrapment efficiency was highest (82.68 ± 1.18%) for PLGA-NPs that were formulated employing ethyl acetate as the organic solvent, 0.25% w/v DMAB, and 10,000 r/min centrifugation speed. Ethyl acetate is the most polar of the solvents considered, making it a suitable match for the ALS. As shown in Table 2, dichloromethane facilitated adequate entrapment (72.75 ± 0.43%). The ethyl acetate/acetone mixture produced the lowest overall entrapment (59.09 ± 1.26%). The ethyl acetate formulation exhibited the most ideal characteristics including small particle size and high entrapment efficiency. These conditions are more suited to the in vivo conditions of the vascular and lymphatic systems, therefore decreasing the chance of clearance from the circulatory system. 30 Particles that measure less than 100 nm are small enough to permeate submucosal membranes, whereas particles greater than 100 nm remain in the epithelial lining and do not reach the target delivery site. 14 In turn, cellular uptake is affected as the number of NPs which reach the cell are minimized. The decreased particle size is related to an increased surface area which allows for more interaction with the solvent. 27 The low entrapment efficiency with ethyl acetate/acetone and dichloromethane indicate that, of those organic solvents tested, ethyl acetate was the best choice for this PLGA-NP formulation in regard to adequate entrapment.
For a drug delivery system to be considered successful, a high loading capacity is essential to curtail the overall dosage requirement. The larger entrapment efficiency value indicated that there was a greater amount of ALS inside the NP per total amount of ALS used for NP production. Further, the amount of drug bound to the NP was greatly influenced by the copolymer PLGA and the chemical structure of ALS. 31 It is possible that entrapment efficency was overestimated as a result of free drug within the NP containing supernatant.
The use of increasing concentrations of stabilizer along with variation in centrifugation speed allowed for the optimization of NP formulation. Zeta potential and PDI are both parameters that guide NP formulation optimization. A more positive zeta potential value, around 20 mV, is desirable so that the NPs may adhere to the negatively charged cell membrane. 16 Higher bioavailability will be achieved if the PLGA-NP is capable of permeating the cell membrane and transported to the primary endosomes within the cell. 14 From there, the PLGA-NPs can be separated, and selected NPs are recycled to the cell exterior to maintain a required concentration gradient of NPs. Without this balance, exocytosis of the NPs will be activated. Inside the cell, the remaining encapsulated PLGA-NPs migrate to the cytoplasm where controlled release of ALS occurs. Charge was highly considered when choosing an optimal formulation due to the vital role this property plays in cellular uptake and drug release.
Once our ALS-NP formulation was optimized, and fresh NPs were prepared, we conducted a oral dose pharmacokinetic study using SHRs. In another study in which SHRs were dosed with a single oral administration of 30 mg/kg in 5% dextrose solution, pharmacokinetic sampling yielded an AUC0-∞ of 3.06 ± 1.8 h.µmol/L (approximately 1688.38 ± 993.17 h.ng/mL) which agrees with the ALS formulation in our study.
32
The mean
A reduction in electrolyte excretion is typically a negative effect as subsequent fluid retention will likely occur leading to high blood volume. In the case of K excretion, the NP formulation appears to show an improvement compared to the methylcellulose form; however, the plasma concentration of K did not show significant variation. When these findings are coupled with a high variation in urinary Na excretion and a nonsignificant plasma Na change, the changes observed may be attributable to an increase in food intake over the examined window.
The results of the urinary KIM-1 assay support the use of this ALS-NP through a reduction in this biomarker of kidney injury. However, the change seen with ALS may change over time. Following 28 days of BID 10 mg/kg ALS oral dosing in C57BL/6-(hREN)/(hAGT) double transgenic mice with concurrent coadministered subcutaneous cyclosporine A (20 mg/kg), urinary KIM-1 (approximately 3.25 ng/mL) was not significantly changed (
Our data show no effect on the plasma BUN response using the nanoformulation. This change may also be time-dependent as the Saraswat et al. study showed that BUN (22.33 ± 0.56 mg/dL) was not significantly changed (
In another study, Sprague-Dawley rats treated with daily intramusculuar gentamicin (100 mg/kg) and ALS (25 mg/kg) via osmotic pump for 14 days, plasma creatinine concentration was reduced compared to gentamicin alone.
34
Further, in five out of six nephrectomized rats treated with oral 10 mg/kg ALS over 4 weeks, plasma creatinine was significantly reduced (
Conclusion
Of the various parameters assayed, the optimum formulation of ALS-NPs was achieved using ethyl acetate as the organic solvent, 1.00% DMAB stabilizer, and a centrifugation speed of 10,000 r/min. For all possible alterations, these conditions offered the highest zeta potential, reasonable particle size below 100 nm, agreeable entrapment efficiency, and a uniform distribution of NPs in the solution. At the dosage tested, ALS-NP showed favorable kidney changes compared to ALS in regard to KIM-1 and K excretion rate. Additionally, the other parameters tested exhibited equivalent outcomes to the ALS formulation. As patient compliance may be more favorable due to an estimated reduction of cost for the antihypertensive drug, this ALS-NP formulation may be the starting point for improving ALS dosing.
Footnotes
Authors’ note
Portions of this article were published in thesis form in fulfillment of the requirements for the Undergraduate Honors Program for Student Jessica Coleman.
Acknowledgment
The authors would like to thank Gregory Hanley, Dustin L Cooper, Fessou Lawson-Hellu, Hannah V Oakes, Angela V Hanley, Kenny W Bullins, Brian G Evanshen, and Judy A Whitmore for their technical assistance.
Author contributions
Derek E Murrell and Jessica M Coleman contributed equally to this work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The funding for this project was made possible through an East Tennessee State University (ETSU) Research and Development Committee Small Grant and an ETSU Honors College Student-Faculty Collaborative Grant. Also, this research was supported in part by the National Institutes of Health grant (C06RR0306551).
