Abstract
Acute-onset heart failure in a young, otherwise healthy patient can be due to either acquired or congenital etiologies. While some diagnoses carry specific histologic hallmarks, many causes of myocardial injury culminate in the relatively nonspecific morphologic pattern of dilated cardiomyopathy. In such cases, a broad differential diagnosis and close clinicopathologic correlation are essential. Here we describe the acute and chronic histologic features of heart failure arising in the context of long-standing abuse of cocaine, alcohol, and marijuana. The mechanisms of cardiotoxicity are discussed for each drug, with particular emphasis on the amplified cardiac injury caused by concomitant cocaine and alcohol use. Although its histologic features are themselves nonspecific, correlation with clinical history, targeted studies to exclude alternative diagnoses, and careful morphologic examination permit confident diagnosis of cardiomyopathy secondary to polysubstance abuse.
Keywords
Introduction
Acute-onset heart failure in a young, previously healthy patient is a rare occurrence. A broad differential diagnosis and a thorough workup are required, in order to provide the proper diagnosis and management. Key clinical and pathological considerations include genetically determined cardiomyopathies, viral or other infections, nutritional or endocrine deficiencies, infiltrative myocardial disease, and drug-induced cardiac toxicity. In such cases, the pathologist plays a critical role, both as a diagnostic consultant and in confirming the final tissue diagnosis, whether at biopsy, explant, or autopsy.
Here we discuss an instructive case of acute-onset heart failure in an otherwise healthy 24-year-old man with a history of polysubstance abuse. We review the histological differential diagnosis and discuss the interrelated mechanisms of cardiac injury related to cocaine, alcohol, and marijuana use, with particular emphasis on cocaethylene-mediated cardiotoxicity.
Case report
A 24-year-old man presented to his primary care provider, complaining of 1 month of chest pain with exertion and shortness of breath, which was worse when lying flat. He reported that he drank 4–5 alcoholic beverages daily on weekdays and 12–16 alcoholic beverages daily on weekends. He had also smoked marijuana 10–15 times weekly for multiple years and had used intranasal cocaine 2–3 times weekly for at least 1 year. He worked in an accounting office and did not smoke cigarettes. He denied any recent fever or upper respiratory symptoms, and he had no family history of heart failure or sudden cardiac death. Echocardiography revealed a left ventricular ejection fraction of 10%, with severe mitral regurgitation and four-chamber dilatation. Cardiac catheterization showed unobstructed coronary arteries, but pulmonary artery pressures were 89/42. Abdominal and thoracic imaging revealed no tumor. The clinical differential diagnosis included viral myocarditis, infiltrative disease involving the myocardium, and heart failure secondary to polysubstance abuse. Genetic causes of dilated cardiomyopathy were considered a diagnosis of exclusion.
The patient remained hospitalized and inotrope-dependent for 6 weeks. Laboratory tests for coxsackievirus, adenovirus, cytomegalovirus, Epstein–Barr virus, human immunodeficiency virus, toxoplasmosis, and Lyme disease were negative. Thyroid studies, vitamin B12, folate, thiamine, prealbumin, and albumin were normal, and body mass index was within the normal range. After 5 weeks, the ejection fraction remained at 25% with inotrope support, and a left ventricular assist device (LVAD) was placed. The patient was discharged 1 week later. Microscopic evaluation of the ventricular core obtained at LVAD placement revealed myocyte hypertrophy and cytoplasmic vacuolation, interstitial edema with patchy myocardial fibrosis, and focal acute and chronic interstitial inflammatory infiltrates (Figure 1). No contraction bands were identified.
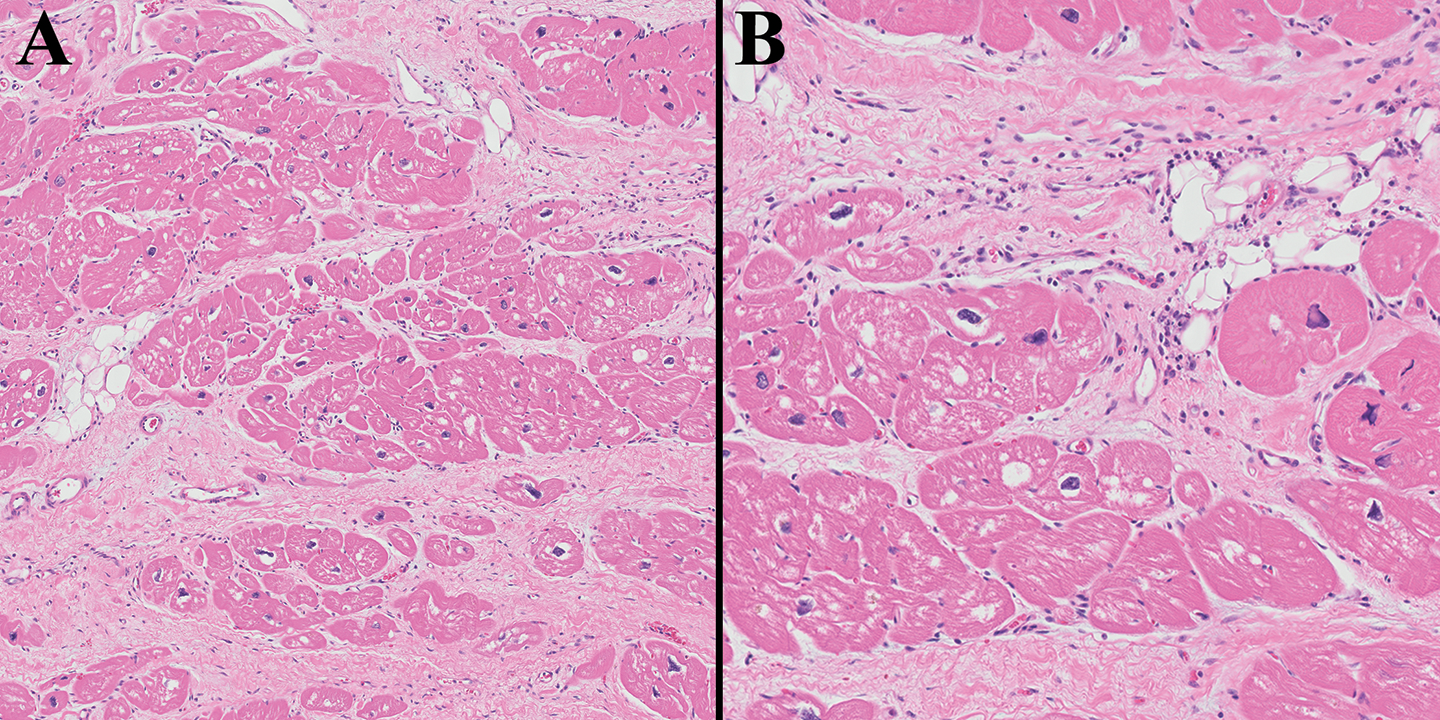
(A) and (B) The left ventricular core (sampled at LVAD placement) exhibits both acute and chronic cocaine-induced injury, including interstitial inflammation, cytoplasmic vacuolization, myocyte dropout with hypertrophy of remaining myocytes, and loose interstitial fibrosis (H&E, 200× (A) and 400× (B)). LVAD: left ventricular assist device.
Over the following months, the ejection fraction remained at 20–25%, and the patient remained symptomatic. He reported total abstinence from alcohol, marijuana, and cocaine, which was confirmed by laboratory testing at regular intervals. Sixteen months after initial presentation, the patient underwent orthotopic heart transplantation.
The heart weighed 275 g following LVAD removal. Gross examination revealed mild dilatation of the ventricles, although the apex could not be assessed due to distortion from the removal of LVAD (Figure 2). Septal hypertrophy was not appreciated, and discrete areas of fibrosis were absent.
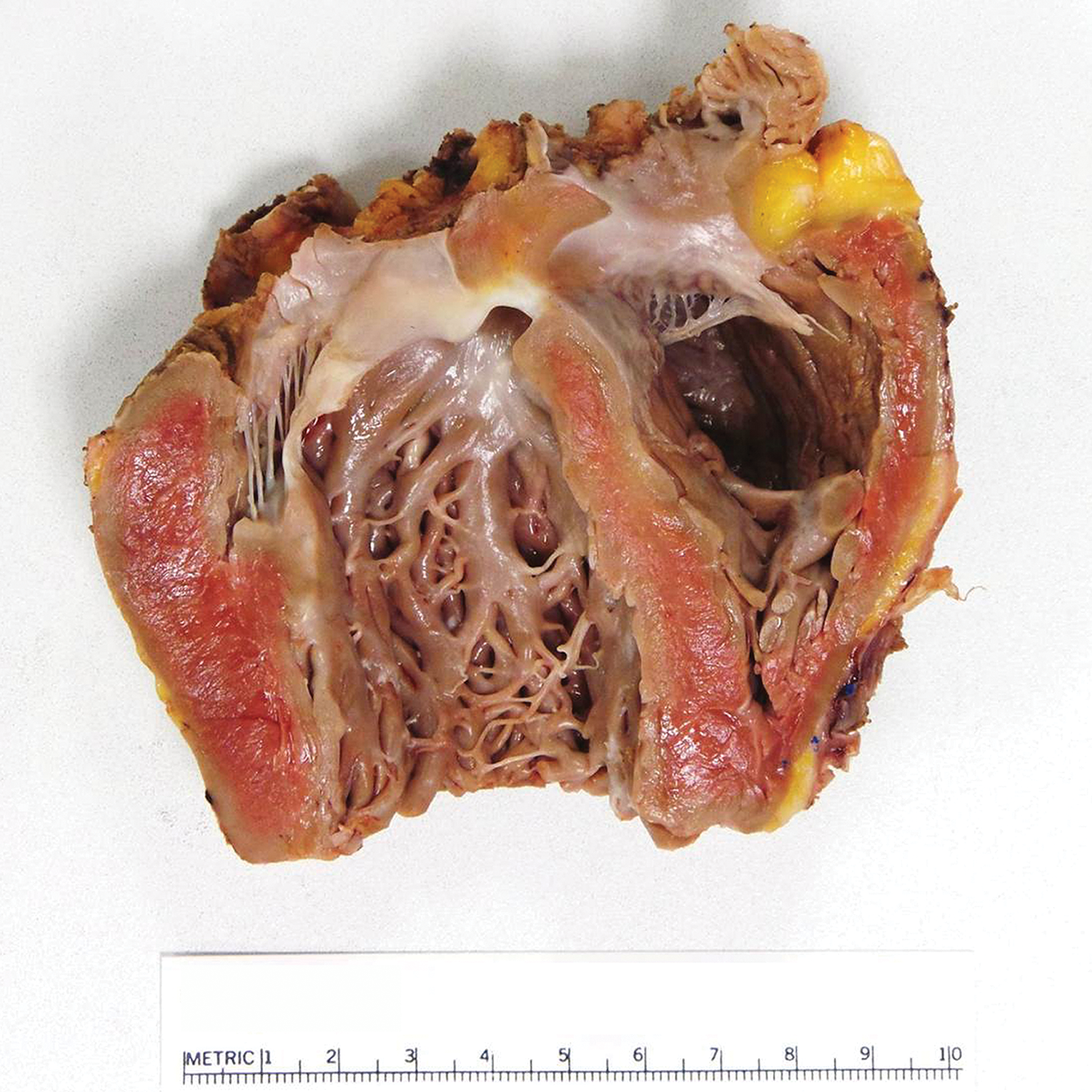
The explanted heart demonstrates mild left ventricular dilatation, without septal hypertrophy or gross fibrosis. Both the atria and the cardiac apex are surgically absent.
Microscopic examination revealed diffuse moderate to marked interstitial fibrosis, equally affecting the full myocardial thickness (Figure 3(a) and (b)). The myocytes were hypertrophic, with prominent nuclear enlargement and pleomorphism. Focal vacuolization of the myocyte cytoplasm was also present (Figure 3(c) and (d)). Myocyte disarray was not prominent, and the coronary arteries exhibited no more than 10% atherosclerotic occlusion.
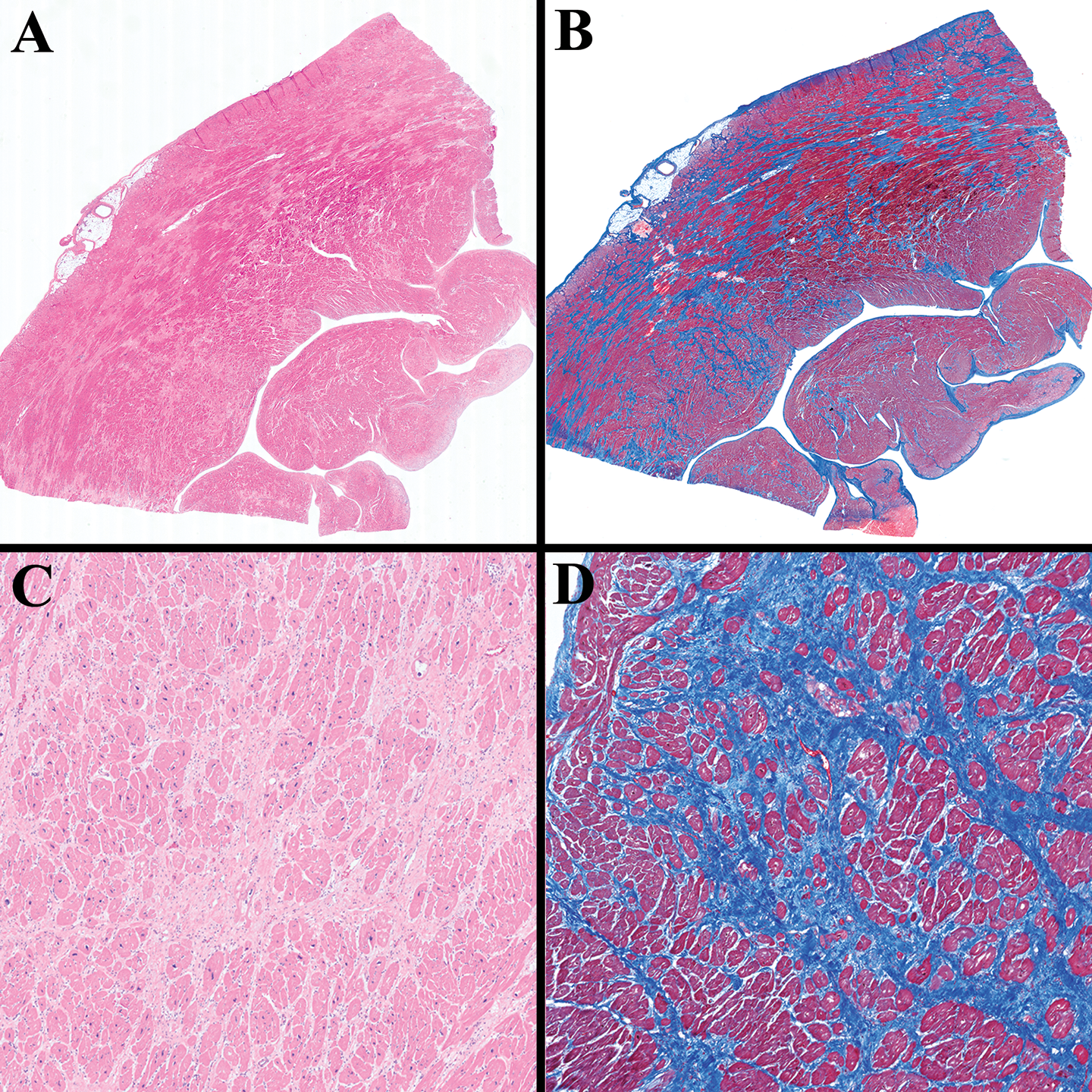
(A) and (B) A full-thickness section of the left ventricle (sampled at explant) demonstrates moderate to marked interstitial fibrosis, equally affecting the full myocardial thickness. (C) and (D) At intermediate magnification, myocyte dropout and marked interstitial fibrosis are evident, with hypertrophy of remaining myocytes (H&E, 20× (A) and 100× (C); trichrome, 20× (B) and 100× (D)).
Discussion
Differential diagnosis
The histologic differential diagnosis in this case included ischemic heart disease (IHD), myocardial involvement by a systemic or focal infiltrative process, genetically determined dilated cardiomyopathy, and dilated cardiomyopathy secondary to toxic exposure, particularly due to polysubstance abuse.
Although atherosclerotic disease was ruled out by examination of the coronary arteries, IHD secondary to vasospasm or global hypoperfusion remained under consideration. However, there was no history of an angina or significant hypotension. Furthermore, equal fibrosis of the inner and outer myocardium is not typical for IHD; accordingly, the histopathologic findings suggested predominantly nonischemic injury.
Infiltrative processes under consideration included principally amyloidosis, disorders of lipid metabolism, and glycogen storage disorders. A negative Congo red stain argued strongly against amyloidosis. Focal myocyte vacuolization raised the possibility of a disorder of glycogen or lipid metabolism. Such metabolic storage disorders classically present before adulthood, with multi-organ involvement, but presentation in adulthood is described, particularly in Fabry disease. However, Fabry disease presents with diffuse myocyte vacuolization and minimal interstitial fibrosis, in contrast to the current case. A toluidine blue stain, which highlights sphingolipid accumulation, was also negative. Glycogen storage disease type 2 (Pompe disease) characteristically presents with heart failure, but presentation is almost universally in young children, and cytoplasmic vacuolization is diffuse. In this case, a negative periodic acid–Schiff stain ruled out a glycogen storage disorder.
Idiopathic dilated cardiomyopathy may result from mutation in a number of both sarcomeric and non-sarcomeric proteins, complicating interpretation of genetic studies performed on a case-by-case basis. Genetic causes were considered a diagnosis of exclusion, with genetic testing to be pursued only in the absence of an identified cause of the patient’s heart failure.
Environmental or workplace exposures to toxins were not evident in the patient’s history. Conversely, the most striking feature of this patient’s clinical history was his polysubstance abuse, including daily use of alcohol and marijuana, and frequent use of intranasal cocaine. Diagnosis of cardiomyopathy secondary to polysubstance abuse relies heavily on clinicopathologic correlation, and histomorphologic evaluation plays a critical confirmatory role.
Numerous distinct pathophysiologic processes share dilated cardiomyopathy as their endpoint, with common histologic features including myocyte dropout with interstitial fibrosis and hypertrophy of residual myocytes. These were the principal histologic findings in the current case and are consistent with both cocaine- and alcohol-induced cardiomyopathy. The myocardial effects of long-term high-dose marijuana use are less well described, but frequent use may accentuate the vasospastic and catecholaminergic mechanisms of cocaine-induced cardiac injury.
With correlation of the clinical history and pathologic findings, a diagnosis of “dilated cardiomyopathy secondary to polysubstance abuse” was rendered.
Pathophysiology of cocaine-, alcohol-, and marijuana-related cardiac injury
Cocaine-induced cardiac injury
Virtually all reports on the histology of cocaine-induced cardiac injury examine either patients dying of cocaine overdose or individuals entering rehabilitation in the context of acute heavy cocaine use. 1,2 As a result, these reports emphasize acute histologic changes, including myocyte necrosis, contraction band formation, and interstitial edema and inflammation. 3 –5 In contrast, given our patient’s 16-month abstinence from substance abuse between initial presentation and heart transplant, this case represents a rare report of the persistent, chronic histologic effects of cocaine-induced cardiac injury. Not surprisingly, while features of acute injury were present in the LVAD core (see Figure 1), these have resolved by the time of explant, with only reparative fibrosis remaining (see Figure 3).
Cocaine causes cardiac injury through both ischemic and toxic pathways. Cocaine inhibits catecholamine reuptake by the presynaptic nerve, increasing the synaptic catecholamine concentration and producing coronary vasoconstriction. With sustained cocaine use, the resulting ischemia produces myocyte death and myocardial fibrosis. 6 Additionally, ultrastructural evidence indicates that direct myocardial toxicity plays a major role in cocaine-induced cardiac injury. 2 Direct cardiotoxicity results from intracellular calcium overload, and from oxidative stress exerted by reactive oxygen species and catecholamine oxidation products, termed aminochromes. Together, calcium overload and oxidative agents derange electron transport, precipitating mitochondrial permeabilization and myocyte death, which may present with either acute (takotsubo-like) or chronic heart failure. 7,8
Alcohol-induced cardiac injury
Like cocaine, excessive alcohol consumption results in potent oxidative injury to the mitochondria—resulting from fatty acid ethyl esters and acetaldehyde produced by alcohol metabolism in the heart. 9,10 And, like cocaine-induced cardiomyopathy, alcoholic cardiomyopathy exhibits the generally nonspecific histologic findings of dilated cardiomyopathy. 11 Because of frequent concurrent malnutrition, heart failure secondary to nutritional deficiency (as in wet beriberi) must also be excluded in alcoholic patients.
Cocaethylene in cardiac injury
Cocaethylene is a cocaine metabolite, produced in the liver only in the presence of ethanol. Given this patient’s frequent overlapping use of cocaine and alcohol, he very likely experienced high cocaethylene levels at least weekly. While the specific cardiotoxic effects of cocaethylene have not been well elucidated in humans, several animal models have shown potent cardiac depression and a high incidence of arrhythmia following direct infusion of cocaethylene or simultaneous infusion of cocaine and ethanol, with resulting cardiac impairment greater than the use of either cocaine or ethanol alone. 8,12,13
Interestingly, while animal studies have demonstrated potent cardiotoxicity associated with hepatic cocaethylene production, and while this toxicity has been assumed to apply to humans as well, 8 there are very few reports or studies documenting this effect. In this case, however, given the patient’s young age, relatively short duration of drug abuse, frequent co-use of cocaine and alcohol, and lack of evidence for alternate diagnoses, we find it likely that cocaethylene toxicity was a key contributor to this patient’s dramatic heart failure presentation.
Marijuana and cardiac injury
While alcohol- and cocaine-induced cardiac injury is well-documented, the association between marijuana and cardiovascular disease is poorly defined. Marijuana intoxication does enhance catecholamine production, which could mimic (albeit to a lesser degree) the catecholaminergic injury caused by cocaine. 14 Additionally, marijuana-induced coronary vasospasm and tachycardia may contribute to an increased risk of myocardial infarction (particularly in concert with cocaine use), 15 and rare case reports do describe acute-onset cardiomyopathy in the setting of high-dose marijuana use. 16 While current evidence does not provide a compelling link between marijuana use alone and significant cardiotoxicity, marijuana use may potentiate the toxic effects of cocaine and alcohol, whether through increased catecholamine production, coronary vasospasm, or both.
Conclusion
Thorough clinicopathologic correlation is essential in the diagnosis of cardiomyopathy secondary to cocaine or alcohol toxicity, as these may histologically show only with nonspecific findings of dilated cardiomyopathy. In the present case, multiple years of heavy alcohol and cocaine consumption likely produced a multiplicative effect, with damage caused by each substance individually and by their co-metabolite cocaethylene, culminating in severe myocardial damage earlier than would have been seen with abuse of alcohol or cocaine alone. The additive toxic effect of daily marijuana use is unclear; however, given the increased catecholamine release and coronary vasospasm associated with marijuana use, it seems possible that marijuana may have further potentiated this patient’s myocardial injury.
This case highlights individuals’ apparently variable predisposition to toxin-related injury. That is, while the patient in the current case developed severe, potentially fatal cardiomyopathy after few years of combined cocaine and alcohol abuse, clinical experience can provide ample instances of patients who sustained polysubstance abuse for far longer, without ever developing clinically significant myocardial injury. The exact factors that mediate this predisposition are currently unknown, but detailed metabolic and genetic study of patients with dilated cardiomyopathy secondary to polysubstance abuse could help to elucidate this complex problem.
Unfortunately, patients with cardiomyopathy secondary to polysubstance abuse have limited clinical options, with heart transplant as the therapeutic mainstay. Furthermore, the current case suggests that the myocardial damage in such cases is effectively irreversible, even with long-term abstinence. This point further emphasizes the need to better understand the main predisposing factors in polysubstance abuse-related cardiac injury. Rigorous early interventions in those at particular risk may be able to forestall the development of irreversible damage and ultimately heart failure.
Finally, this report highlights the work that remains to be done in defining the specific health risks of regular marijuana use, particularly in light of the increasing social and legal availability of cannabis, largely without product standardization or safety data. Dedicated work in this realm could play an important role in avoiding or at least tempering a significant threat to public health.
Diagnosis of cardiomyopathy associated with drug abuse is complicated by both nonspecific histology and relative rarity in daily pathology practice, increasing the risk of a missed diagnosis. A high index of suspicion, a complete clinical history, and attention to histologic detail are all necessary for proper diagnosis, whether in the biopsy, explant, or autopsy setting.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
