Abstract
Background
Escape Rooms in medical education have been shown to improve learner satisfaction and reinforce knowledge in pulmonary and critical care medicine, yet virtual escape rooms (VER) as instructional strategies have remained understudied.
Objective
We aimed to evaluate participants’ perception and knowledge acquisition after completing a VER as part of a national fellows’ course.
Methods
We designed a prospective study conducted during the 2022 CHEST Pulmonary and Critical Care Medicine Fellow's Virtual course. This was a 2-day back-to-back national course targeting pulmonary and critical care fellows. The course had 5 virtual and 1 VER session, each lasting 50 min. A pre- and post-course knowledge assessment included 9 clinical questions (1 for each of the 5 virtual sessions and 4 for the VER session). A summative score and an individual session score were obtained. Participant's VER perceptions were analyzed using a 5-point Likert scale (1 = strongly disagree and 5 = strongly agree).
Results
Fifty-nine (34.5%) of the 165-course participants completed the pre-test, and 29 (17.8%) completed the post-course test. Higher clinical knowledge assessment total score and VER scores were seen in the post-test compared to the pre-test (77.8 ± 14.9 vs 59.6 ± 23.1 P < .001) and (77.3 ± 26.6 vs 62.5 ± 32.5, P < .05) respectively. VER perceptions in the course were positive across participants and sustained after deployment.
Conclusions
Implementing an educational VER in a national pulmonary and critical care fellows’ virtual course may promote knowledge acquisition and could potentially lead to a positive perception among participants. Longitudinal studies in various contexts are required to further elucidate direct causality between gamification and learner centric outcomes.
Keywords
Background
Escape rooms are a type of interactive, and typically theme-based activity, where players work collaboratively with each other to “escape” from a “locked situation” by solving a variety of puzzles. Escape rooms have gained popularity and prominence as innovative instructional strategies reinforcing knowledge and skills across many disciplines in medicine.1–6 The setting of delivery of these escape rooms is variable, however, literature supports that medical education escape rooms are associated with high learner satisfaction and are feasible for delivery at an in-person national scientific conference or a national course. 6 This aspect of delivery is important as national conferences bring learners from across the country, different institutions, and often multiple disciplines together.
Although feasible and highly engaging when delivered in-person, delivery of education in an escape room format virtually allows for overcoming the limitations of geography, traveling, costs, and disciplinary silos. The COVID-19 pandemic hastened the move of traditional educational offerings into the virtual space. We pivoted the process of adapting to learners’ needs during the pandemic by deploying virtual escape rooms (VER). 6 The impact of VER on educational outcomes, including knowledge retention and learners’ perceptions is in early stages of being explored. A study including Emergency Medicine trainees found conflicting results in terms of efficacy of VER compared to traditional education; however, other studies exploring VERs for nursing, pharmacy, pre-clinical, and clinical settings have found VERs effective and engaging. 7 There is no study evaluating efficacy of delivery of VER at a national level educational activity.
Our pilot study aimed to explore learner's knowledge acquisition and perceptions of a VER when deployed at a national level pulmonary and critical care medicine fellow's course.
Methods
Study Design and Participants
We conducted a prospective pilot study embedded in the 2022 Pulmonary and Critical Care Medicine (PCCM) Fellows Virtual Course, sponsored by the American College of Chest Physicians (CHEST). The course was delivered via Zoom to pulmonary, critical care and PCCM fellows across the United States and promoted via CHEST member communications and social media. Program directors nominated second- or third-year fellows through an online nomination portal at their discretion. To ensure broad representation, at least 1 fellow per training program was accepted. The reporting of this study conforms to the “DoCTRINE” guideline (Supplemental File 1). 8
Course Structure and Intervention
The virtual course included five 50-min didactic lectures delivered virtually (3 on day one and 2 on day two). A subject-matter expert and a content-delivery expert co-chaired sessions on the following topics: Chest Radiology, Mechanical Ventilation, Pulmonary Hypertension, Sleep Medicine, Veno-venous Extracorporeal Membrane Oxygenation (ECMO). These lectures used traditional slide presentations that incorporated case-based discussions and an audience response system. The course concluded with the 50-min VER session. The design and delivery of this VER, titled “First Contact,” has been previously published. 6 The game was designed to immerse players in a narrative where they are passengers on a space shuttle in the year 2120 headed to a scientific meeting on Jupiter Station. A potential catastrophe ensues, and players must work together to solve complex lung radiology, pathology, and physiology puzzles to resolve the crisis. For example, a puzzle might require players to match several exposure histories with their corresponding lung CT scans and biopsy results to complete a “circuit” and restore power to the ship. A teaser trailer was created to build anticipation for the players and can be viewed at: https://youtu.be/ZgzyAM69sQg?si=x6sFpQ1WZ_qzBlye.
The VER was delivered to teams in Zoom breakout rooms using a custom-built, hyperlinked PowerPoint presentation. Faculty moderators, all of whom were pulmonary/critical care medicine physicians, controlled the slides and facilitated the sessions while role-playing as non-medical shuttle pilots. A detailed script, including puzzle answers, anticipated player responses, and technical contingency plans, was provided during a training session required for all moderators (Supplemental File 2).
From a feasibility standpoint, the VER required a minimal technology footprint. There was no physical infrastructure. The intervention relied solely on the Zoom platform and hyperlinked PowerPoint presentation and video components created by one faculty member (WK) using free iMovie software and less than $200 in stock images purchased online. Faculty moderator training was about 30 min and involved experiencing the room as a player and then as a moderator. The initial development of the puzzles and script was time-intensive for core faculty. A moderator-to-player ratio may ideally be 1:8 but was flexible and could be scaled based on need.
Outcomes and Data Collection
The primary outcome was the change in participants’ clinical knowledge from pre-course to post-course. The secondary outcome was participants’ perceptions and attitudes toward the VER session.
We asked all accepted fellows to complete a pre-course demographic survey through the CHEST's learning management system and a pre-and-post course knowledge assessment through SurveyMonkey (Supplemental File 3-4). The knowledge assessment contained 9 questions: 1 for each of the 5 virtual sessions and 4 for the VER session (2 on lung pathology and 2 on critical care ultrasound). The assessment was developed through a standardized process. For each of the 5 virtual sessions, the 2 session co-chairs—a subject-matter expert and a content-delivery expert—jointly identified one single-best-answer question or multiple-choice question to align with that session's objectives. In addition, the VER chairs selected 4 questions to assess overall knowledge acquisition for the VER session. These questions were previously piloted with PCCM fellows and faculty during an in-person VER session. The author team edited all items for clarity and formatting, and the co-chairs provided final approval. The knowledge assessment contained 9 questions: 1 for each of the 5 virtual sessions and 4 for the VER session (2 on lung pathology and 2 on critical care ultrasound). The items were then uploaded to the online survey platform and administered to participants. Learners did not receive real-time feedback on pre-test performance to avoid a co-intervention between pre- and post-tests. Because the pre- and post-assessments used identical items and structure, content and difficulty were comparable. The knowledge survey also included a question on prior escape room experience, and the post-course survey included 2 questions on VER perceptions using a 5-point Likert scale (strongly disagree to strongly agree). We calculated total scores and session-specific scores.
Statistical Analysis
Categorical variables are reported as frequencies and percentages, and continuous variables are reported as mean and standard deviation (SD). We used the Wilcoxon signed-rank sum test to compare paired pre- and post-test scores due to the non-parametric nature of the data. We considered a 2-sided P-value of less than .05 to indicate statistical significance. All analyses were performed using Stata version 17.
Results
The 2-day course used 165 unique logins. Demographics were obtained for 85 participants (46.4%), 18 (30.5%) with prior escape room experience, and 4 (6.9%) with experience with VER (Table 1). A total of 59 (35.5%) and 29 (17.8%) participants completed the pre- and post-course tests, respectively.
Participant Demographics.
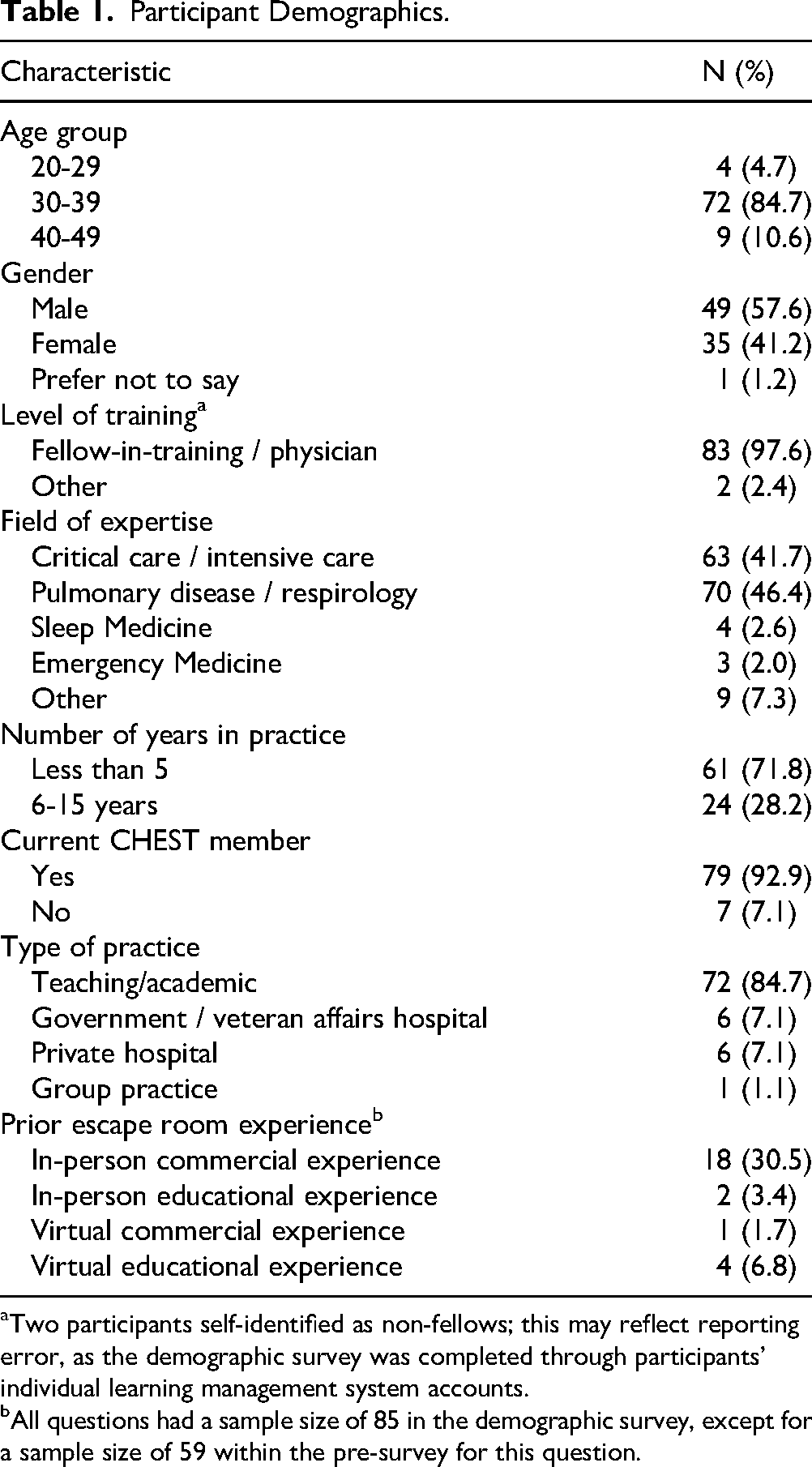
Two participants self-identified as non-fellows; this may reflect reporting error, as the demographic survey was completed through participants’ individual learning management system accounts.
All questions had a sample size of 85 in the demographic survey, except for a sample size of 59 within the pre-survey for this question.
The mean clinical knowledge assessment total score and VER scores were significantly higher in the post-test compared to the pre-test (77.8 ± 14.9 vs 59.6 ± 23.1, P < .001) and (77.3 ± 26.6 vs 62.5 ± 32.5, P < .05), respectively (Figure 1). The percentage of correct answers for each of the 5 virtual sessions was significantly higher in the post-test compared to the pre-test for Chest Radiology (100% vs 84.7%, P < .05), Mechanical Ventilation (75.9% vs 8.5%, P < .001), Veno-venous ECMO (96% vs 72.9%, P < .05), with no difference in the Pulmonary Hypertension and Sleep Medicine sessions (Figure 2).

Pre- and Post-Course Clinical Knowledge Assessment Scores. The First Plot Indicates the Total Score That is Cumulative of the Virtual Sessions and Virtual Escape Room Score, the Second Plot Demonstrates the Scores After Delivery of the Virtual Didactic Session (Virtual Sessions Score), and the Third Plot Indicates the Scores After Attendees Completed the Virtual Escape Room (Virtual Escape Room Score).

Clinical Knowledge Assessment Questions Individual Performance.
Escape rooms as a “fun activity” and “its recognition as a session that provides new learning” were positively perceived before and after the VER without significant differences. When providing feedback after attending the VER, participants strongly agree that interactive experiences like the VER should be available for future scientific society events (4.11 ± 1.16).
Discussion
Implementing a VER into a national PCCM fellows’ course demonstrated both knowledge acquisition and sustained positive perceptions of this instructional modality. To our knowledge, this represents the first integration of a VER into a national PCCM course.
In-person escape rooms have been found to be effective for improving various learner outcomes in a variety of settings and in various disciplines. A systematic review and meta-analysis by He et al reported that compared to traditional learning, escape rooms had a more significant effect on various domains of learning, including knowledge, teamwork, learner satisfaction, and interprofessional study. 9 VER provides a low-cost, innovative approach to virtual learning in graduate medical education. 10 Studies, as described earlier in this manuscript demonstrate that VERs have shown to be efficacious and engaging but in limited contexts. We sought to explore if VER can be an effective learning modality at a national or potentially inter-institutional educational activity. In our study, it proved feasible and effective in fostering clinical knowledge, as reflected by improved test performance across most sessions, including those delivered via the VER. Absent gains in the pulmonary-hypertension and sleep sessions may reflect variability in pulmonary-hypertension exposure (particularly among early second-year fellows), inclusion of critical care-only fellows without a traditional sleep-medicine curriculum, and the advanced, short-answer format of the sleep-session item.
The VER created a supportive, engaging learning environment, achieving high participant satisfaction—an often-challenging goal in virtual education. This approach aligns with the evolving needs of medical education, promoting adaptability to new technologies and teaching modalities.
Despite the growing familiarity with escape room gamification, its application in virtual medical education remains underutilized as evidenced by the fact that only one-third of participants reporting having prior in-person escape room experience and fewer than 7% reported familiarity with VERs. The VER's design, incorporating interactive tasks, individual breakout rooms, and structured collaboration, offers a personalized and empowering educational experience.11–13 Additionally, this platform may contribute to trainees’ well-being by encouraging interactions, potentially mitigating burnout and depressive symptoms commonly observed in this cohort. 14 Notably, the high engagement and satisfaction persisted even after 10 h of Zoom-based instruction over 2 days, underscoring the VER's appeal and effectiveness.
Challenges included motivating participants to enable video during gameplay and orienting first-time users to the rules. However, peer engagement often encouraged broader participation. These considerations emphasize the need for clear pre-session instructions and strategies to foster early involvement.
The primary limitation of our study was the low survey response rate, a common challenge in research involving physicians. 15 Multiple solicitations might have improved participation. Secondly, our study's design assessed immediate post-session knowledge gains, precluding insights into long-term retention. Additionally, since we did not have a control group, both in terms of learners and a different educational modality, we cannot draw inferences on the effectiveness of VERs compared to other active educational modalities. Future research should explore these aspects and further validate the use of VERs in diverse educational contexts.
Conclusion
The VER represents an innovative and potentially effective instructional strategy for virtual graduate medical education, with indication of improved clinical knowledge acquisition and high learner satisfaction in a national PCCM fellows’ course. Its engaging, low-cost design addresses key challenges in virtual learning and holds promise for broader applications in medical education, however, further studies with larger sample sizes, diverse settings, and ideally comparing VER to other active learning modalities are necessary to validate its long-term educational impact and generalizability.
Supplemental Material
sj-docx-1-mde-10.1177_23821205251388211 - Supplemental material for Implementation of a Virtual Escape Room Into a Pulmonary and Critical Care Fellows National Course: A Pilot Study
Supplemental material, sj-docx-1-mde-10.1177_23821205251388211 for Implementation of a Virtual Escape Room Into a Pulmonary and Critical Care Fellows National Course: A Pilot Study by Yerandy Gil, Michele Iguina, Roger Wong, Viren Kaul, William F. Kelly and Mauricio Danckers in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205251388211 - Supplemental material for Implementation of a Virtual Escape Room Into a Pulmonary and Critical Care Fellows National Course: A Pilot Study
Supplemental material, sj-docx-2-mde-10.1177_23821205251388211 for Implementation of a Virtual Escape Room Into a Pulmonary and Critical Care Fellows National Course: A Pilot Study by Yerandy Gil, Michele Iguina, Roger Wong, Viren Kaul, William F. Kelly and Mauricio Danckers in Journal of Medical Education and Curricular Development
Footnotes
Acknowledgments
The authors would like to acknowledge the American College of Chest Physicians for their generosity in sponsoring the fellows'' virtual course and the statistical analysis of the project data. We would also like to thank HCA Healthcare for their support with publication fees.
Ethics
This study was conducted in accordance with the ethical standards of the Declaration of Helsinki and relevant national regulations. Review by the Centralized Algorithms for Research Rules on IRB Exemption (C.A.R.R.I.E) determined the project to be exempt from Institutional Review Board oversight. No identifiable personal data were collected, and participant confidentiality was maintained throughout the study.
Consent
This study received an Institutional Review Board (IRB) exemption through the Centralized Algorithms for Research Rules on IRB Exemption (C.A.R.R.I.E). It was approved to be conducted without explicit consent from the participants.
Author's Contribution
Yerandy Gil, Michele Iguina, Viren Kaul, William Kelly and Mauricio Danckers contributed the drafting of the entire document. Roger Wong contributed to the creation of graphs/tables and statistical analysis, as well as review of the document. The author's disclose that an abstract of this work was presented in a national scientific meeting and published in the journal abstract issue (CHEST 2022;162(4):A1467).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: CHEST provided funding for statistical analysis and the HCA Healthcare for publication fees.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr Kaul, Dr Kelly and Dr Danckers have held or hold voluntary non-profit committee leadership position within the American College of CHEST Physicians (CHEST). The authors certify that they have no affiliations with any organization or entity with any financial interest in the subject matter or materials discussed in this manuscript. CHEST sponsored the pulmonary and critical care fellows’ virtual course and provided funding for the statistical analysis. This research was supported (in whole or in part) by HCA Healthcare and/or an HCA Healthcare affiliated entity. The views expressed in this publication represent those of the authors and do not necessarily represent the official views of HCA Healthcare or any of its affiliated entities.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
