Abstract
Background
It is not entirely understood how medical students make their future career decisions or what influences them. Furthermore, the factors that affect the perception of pathology as a future career are diverse and related to the exposure of medical students to pathology education in their first 3 years in medical school.
Aim of the study
We aim to assess how medical students in Jordanian Universities perceive pathology as a potential job and the variables influencing their decisions. To identify the preferred medical specialties among medical students in Jordan.
Materials and methods
An observational cross-sectional study was conducted on a randomly selected sample of students from the faculties of medicine at Jordanian universities, including those in the second to sixth year and recently graduated students. Data was collected via a web-based self-administered questionnaire. Descriptive statistics were employed to summarize the responses. Pearson's Chi-squared test and Fisher's exact test were utilized for variable assessment. Statistical significance was defined as a
Results
When comparing students based on their perceived adequacy of pathology training in the first 3 years of medical school, several significant differences emerged across key characteristics: the understanding of the pathologist's job, case-based learning led by pathologists, ratings for a separate pathology course, and the perception of pathologists as introverts. On the other hand, no statistically significant differences were found in age, gender, secondary school background, or whether students considered pathology as a future specialty across the different training exposure groups.
Introduction and Literature Review
The field of medical education is changing, and numerous changes have been made in medical colleges worldwide. Students’ opinions and comments greatly affect academic development.
Pathology is a medical discipline that is often labeled as a paramedical field that establishes the scientific basis for all medical practices. The pathologist collaborates with all other medical specialties, using laboratory medicine methods to provide knowledge important for clinical problem-solving. 1 Pathologists’ scope of practice encompasses a broad range of activities, including the interpretation of tissue biopsies, surgical specimens, cytological samples, and autopsies, as well as oversight of clinical laboratory testing. Through histopathological, immunohistochemical, and molecular analyses, pathologists provide definitive diagnoses that guide therapeutic decision-making, disease prognostication, and personalized treatment strategies. 2
Moreover, they contribute to multidisciplinary team discussions, participate in quality assurance programs, and are integral to cancer screening and monitoring programs. By integrating morphological findings with advanced molecular diagnostics, pathologists ensure accurate, timely, and clinically relevant information that directly impacts patient outcomes. 3
Although a pathologist's role is crucial in diagnosing and managing diseases, medical students often remain unaware of both the pathologist's contributions and the career of pathology. In an article published in the College of American Pathologists, CAP Today newspaper, “What influences med students to choose pathology,” many pathologists believe that changes in the medical student curriculum are leading to decreased interest and that there is insufficient visibility of pathologists in the diagnostic process. These curricular changes are mainly the subject-based curriculum, the standalone pathology course identified pathologists as a separate profession and knowledge base; with a recommendation to shift toward a more integrated system-based learning. The lack of a clinical rotation in the pathology department in the students fourth to sixth years also contributed to the pathologist role invisibility among medical students. The authors emphasized a need to focus less on first- and second-year curriculum course structures and shift pathologists thinking to teaching students about pathology profession. 4
The concern about the knowledge of pathology and the perception of pathology in undergraduate medical students is there in different parts of the world. In a study conducted on medical students at a university in Saudi Arabia showed that only 8.7% of the students considered pathology as a possible future career and only 2 students (0.7%) selected pathology as first option. 5
In a qualitative study conducted in India, personal interviews with 15 participants (13 undergraduates and 2 postgraduates) in pathology showed that the interviewed medical students perceived that pathologists have minimal patient contact and a limited role in treating patients. The students thought that undergraduate courses and curricula in pathology were inadequate and did not provide enough exposure to the actual practice of pathology. 6
In a national survey of fourth-year US allopathic medical students conducted to assess experiences, knowledge, and attitudes of pathology and factors that impact specialty choice. Most participating students believed they were not exposed to pathology enough to consider it a future specialty. There was a lack of understanding of the pathologist's activities and work. 7
These findings highlight a consistent theme: limited exposure and insufficient curricular integration of pathology contribute to lack of understanding and misconceptions about the specialty.
In Jordanian medical schools, the curriculum is standardized across the surveyed universities, consisting of a 6-year program. The first 3 years are dedicated to basic medical sciences, distributed across 3 semesters, followed by 3 years of bedside clinical teaching in hospital settings. Pathology is introduced early in the curriculum, beginning in the first semester of the second year through a 16-week general pathology course covering fundamental topics such as cellular injury, inflammation, hemodynamic disorders, and neoplasia. Subsequently, pathology instruction continues through integrated lectures within system-based modules, complemented by practical sessions that familiarize students with tissue processing and glass slide preparation. However, dedicated pathology neither mandatory nor elective rotations are not incorporated into the clinical years, limiting students’ opportunities to directly observe pathologists’ roles and responsibilities in real-world hospital practice.
The process through which medical students make career decisions and the factors that influence these decisions are not fully understood. Some studies have addressed this complex decision-making process.
Querido et al, suggested that there are 5 primary categories related to a career choice or specialty preference: (1) characteristics of medical school, (2) characteristics of medical students, (3) personal preference of medical students, (4) factors of career needs to be met mainly the income expected and the work-life balance; and (5) perception of specialty characteristics. Medical career decision making is frequently linked to perceptions of specialized characteristics and career needs in particular. 8
In Jordan, a cross-sectional questionnaire-based survey was carried out among second, fourth, and sixth-year medical students at the Jordan University of Science and Technology, which showed that surgery, internal medicine, pediatrics, and obstetrics and gynecology were the most preferred specialties of medical students. 9
A study performed on medical students at Al-Balqa Applied University proposed the integration of pathology curriculum with histology, concluded that case discussions proved to be successful, and the microscope remains an effective and preferred tool for teaching microscopic morphology. They concluded that much effort is needed to increase students’ affinity for surgical pathology.
Aim of the Study
To assess medical students’ knowledge and perceptions of pathology, as well as their decisions to select pathology as a prospective career. To identify factors influencing medical students’ choices of medical specialties. To provide recommendations regarding the implementation of a 2-week elective clinical rotation in pathology.
Materials and Methods
Study Design and Setting
This study was conducted cross-sectionally across 4 medical schools in Jordan. Data were collected using a structured, self-administered questionnaire designed to assess medical students’ perceptions of pathology and factors influencing their specialty preferences.
Study Population and Sample Size
The target population consisted of undergraduate medical students enrolled in the participating Jordanian medical schools (N ≈ 10,000). Using a 95% confidence level and a 5% margin of error, the minimum recommended sample size was calculated to be approximately 370 students. To ensure adequate representation and account for potential non-response, a final sample size of 395 participants was selected.
Inclusion and Exclusion Criteria
The inclusion criteria comprised undergraduate medical students enrolled at 1 of the 4 participating medical schools in Jordan (Yarmouk University, Hashemite University, Jordan University of Science and Technology, and the University of Jordan), from all academic years including interns and recent graduates within the study period, who provided informed consent to participate.
The exclusion criteria included students who declined to provide consent at the beginning of the questionnaire, those not enrolled in the medical programs of the participating universities during the data collection period, and questionnaires that were incomplete or missing essential demographic or study-related information.
Data Collection
The survey was conducted over a 3-month period, from January 1, 2025 to March 31, 2025. The questionnaire was disseminated electronically via institutional email lists and student social media platforms to maximize accessibility and participation. Participation was voluntary, and informed consent was obtained electronically through an introductory question at the beginning of the survey.
Questionnaire Structure
The questionnaire consisted of 4 sections: (1) consent to participate, (2) demographic data, (3) decisions regarding future specialty choice, and (4) perceptions of pathology as a specialty. The pathology section explored 3 key areas: (a) perceptions of pathology exposure, (b) the role of pathology within the medical school curriculum, and (c) resources used to learn more about pathology.
Pilot Testing
A pilot study involving 58 medical students was conducted from October 2 to 8, 2023 to evaluate completion time, question interpretation, and survey flow. The average completion time was 5.15 min, and no significant issues were reported. Final adjustments were made based on this feedback. For the full dataset (excluding extreme outliers over 30 min):
Average completion time: 5.15 min; Median: 5 min; Range: 1 to 11 min; and Valid responses considered: 54.
This indicates that most respondents completed the questionnaire in about 5 min, which is ideal for this type of survey.
Statistical Method
Descriptive statistics were employed to summarize the sociodemographic characteristics of participants, their preferred medical specialties, and their perceptions regarding pathology exposure and the discipline as a future career. Categorical variables were presented as frequencies and corresponding percentages. Comparative analyses were conducted to assess associations between students’ perceptions and their self-reported adequacy of pathology training during the first 3 years of medical education. Pearson's Chi-squared test was utilized for variables with expected cell counts ≥5, while Fisher's exact test was applied when this assumption was not met. Statistical significance was defined as a
Ethical Approval
This study received ethical approval from the Research Ethics Committee on Human Subjects at Yarmouk University, Institutional Review Board, under reference number IRB/2024/078, and all procedures were conducted by the relevant guidelines and regulations.
Participation was anonymous, voluntary, and based on informed consent, which was obtained electronically at the beginning of the questionnaire. No identifiable personal information was collected, and responses were used solely for research purposes.
Patient and Public Involvement
Patients and members of the public were not involved in the design, conduct, reporting, or dissemination plans of this research.
Reporting Standards
This study was conducted following the STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) guidelines for cross-sectional observational studies, as recommended by the EQUATOR Network.
Results
A total of 395 participants were included in the study. Most were aged 20 to 24 years (91.14%). More than half were female (53.16%), while males made up 46.33%, and 0.51% preferred not to disclose their gender. Participants were primarily from Yarmouk University (42.03%), followed by Hashemite University (25.06%), Jordan University of Science and Technology (24.30%), and the University of Jordan (8.61%). Regarding academic year, the most represented were third-year (25.82%), fifth-year (22.03%), and fourth-year students (21.77%). A smaller proportion were in sixth year (13.67%), internship (10.63%), or had recently graduated (4.05%). Notably, 8.86% of participants had a parent who was a physician, and 37.72% had a sibling studying or who had studied medicine (Table 1).
Demographic Characteristics of Medical Student Participants.
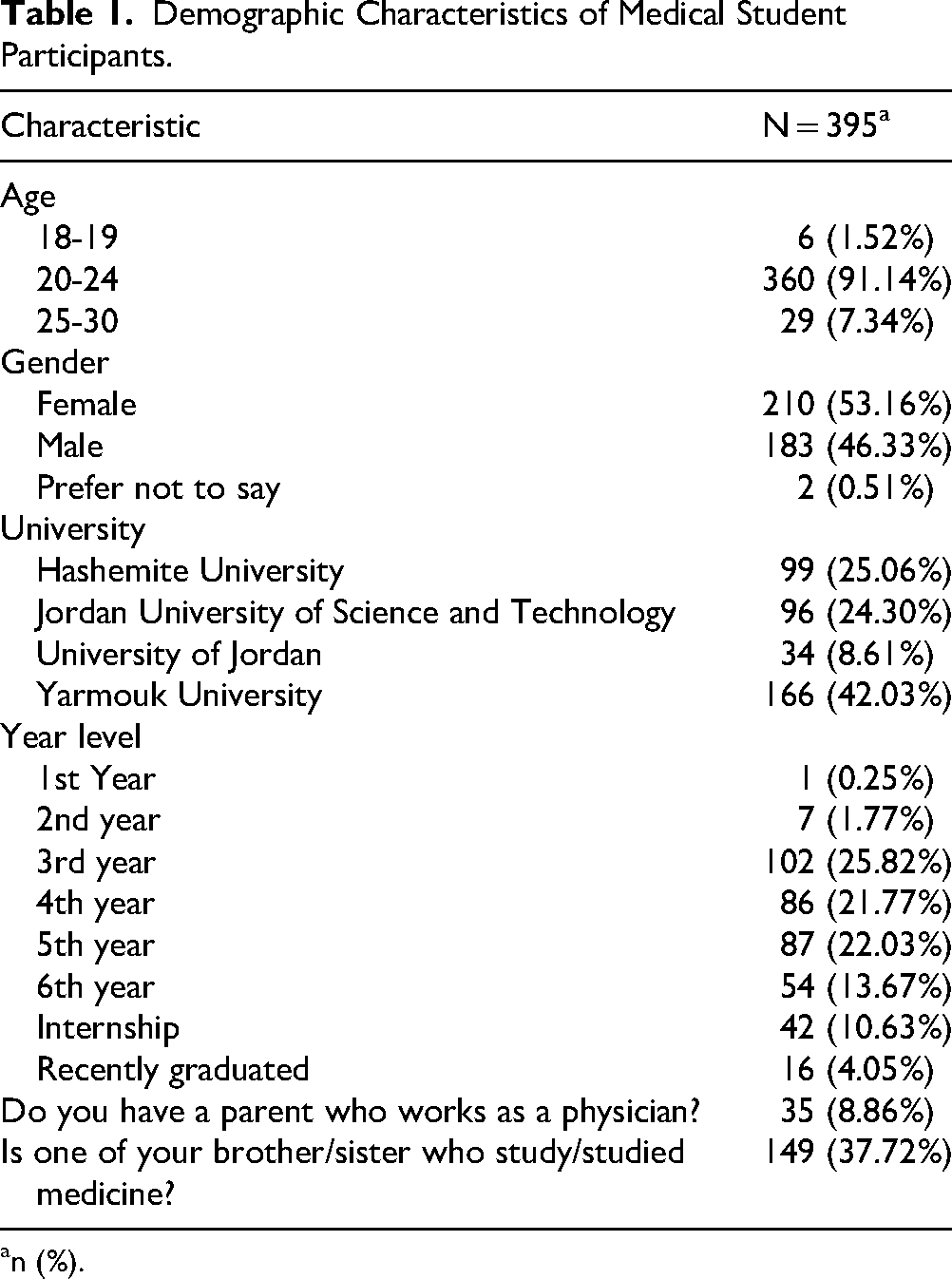
n (%).
The most commonly preferred specialties among participants were internal medicine (46.84%), dermatology (31.14%), ophthalmology (30.13%), and general surgery (34.43%). Other specialties such as pediatrics (23.54%), neurosurgery (22.53%), and neurology (21.77%) were also favored, while pathology was selected by 10.13% of respondents. Regarding when students decided on their preferred specialty, 21.77% had not yet decided, while others made their choice mostly during the fourth year (20.00%), fifth year (17.97%), and third year (15.44%). When asked if they had considered pathology as a possible future specialty, 60.00% responded “No,” 24.05% said “Maybe,” and only 15.95% answered “Yes.” Among those who did not consider pathology, the most common reasons were a preference for another specialty (59.83%), a lack of knowledge about pathology as a career (23.70%), and indecision regarding a future specialty (16.47%) (Table 2).
Preferred Medical Specialties and Interest in Pathology Among Participants.

n (%).
Regarding perceptions of pathology exposure, only a third of participants (33.92%) agreed they received adequate pathology training during their first 3 years, while 33.67% were neutral, and 17.47% disagreed. Understanding of the pathologist's job was moderate, with 31.39% agreeing and 33.42% remaining neutral, while nearly one-third either disagreed (24.56%) or strongly disagreed (5.32%). When asked whether they were sufficiently exposed to pathology to consider it as a career, only 17.22% agreed and 2.28% strongly agreed, while a notable 33.67% disagreed and 10.89% strongly disagreed. Social media's role in shaping perceptions was limited, with only 16.20% agreeing that the information was encouraging and 42.28% expressing neutrality.
As for curriculum exposure, most students rated lectures by pathologists during the first 2 years as moderately helpful, with 34.18% giving a score of 3 of 5 and 27.34% scoring 4 of 5. Microscope use and gross specimen demonstrations were generally rated low, with 50.63% and 46.58% giving a 1 of 5 score, respectively. Case-based learning led by pathologists showed slightly more engagement, but still, 31.39% rated it just 2 of 5. Pathology exposure during other clinical rotations was also minimal, with 35.70% scoring it 1 of 5. Regarding a separate, graded pathology course, responses were more evenly distributed, but still leaned lower, with 24.81% rating it 1 of 5 and only 13.16% giving it the highest score of 5 of 5 (Table 3).
Perceptions of Pathology Exposure and Curriculum Structure in Medical School.

n (%).
Participants generally held a favorable view of pathology as a medical specialty. A combined 56.2% agreed or strongly agreed that pathology offers adequate scholarly and research opportunities, while only 8.61% disagreed or strongly disagreed. Similarly, 63.04% believed that pathologists have a good work–life balance. Nearly three-quarters (72.41%) agreed that pathology has limited opportunities for direct patient contact, reflecting a common perception of the specialty. Half of the participants (50.38%) agreed that pathology offers opportunities to utilize new technologies, while only 18.98% disagreed. In terms of income potential, responses were more neutral, with 54.94% selecting “Neutral” and only 31.9% expressing agreement or strong agreement. When asked whether pathologists are introverts, 26.33% agreed, 17.22% disagreed, and a large portion (43.80%) remained neutral. Regarding intellectual challenge, 47.6% agreed or strongly agreed that pathology offers a satisfying level, while 41.27% were neutral.
As for resources used to learn more about pathology, the most common source was the pathology faculty at students’ medical schools (66.84%), followed by the internet or social media (47.34%). Other notable sources included pathologists outside the medical school (21.01%), the student affairs office (18.99%), professional organization websites (18.99%), and friends (18.73%). Fewer students cited family (6.84%) or other sources (9.37%) as their primary resources (Table 4; Figure 1).
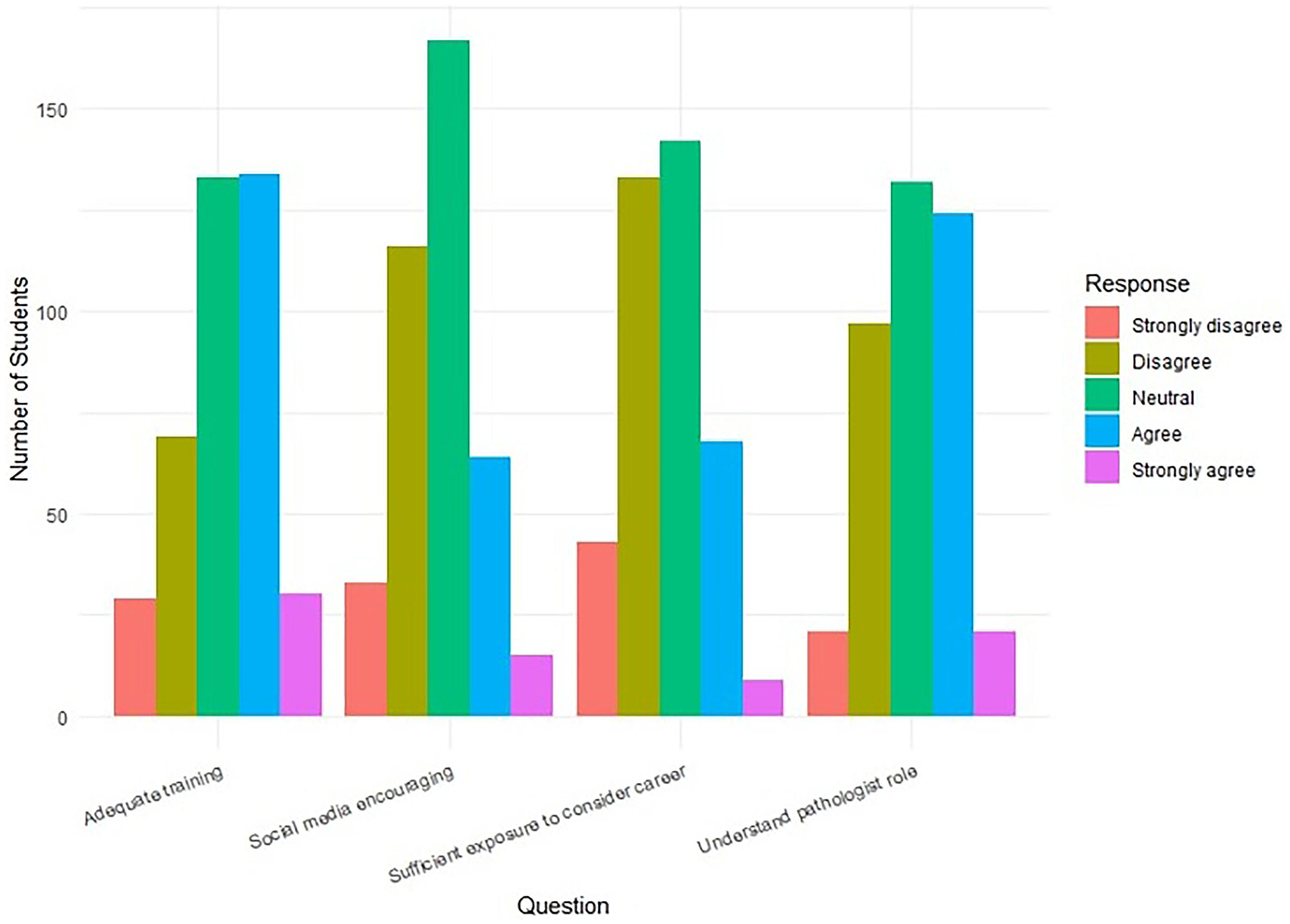
Perceptions of Pathology Exposure and Curriculum.
Students’ Perceptions of Pathology as a Medical Specialty and Sources of Information.

n (%).
When comparing students based on their perceived adequacy of pathology training in the first 3 years of medical school, several significant differences emerged across key characteristics. The understanding of the pathologist's job varied notably (

Understanding of Pathologists’ Role by Pathology Training Level (
Similarly, case-based learning led by pathologists showed variation (
On the other hand, no statistically significant differences were found in age (
Comparison of Student Characteristics and Perceptions Based on Quality of Pathology Training in the First 3 Years.

n (%).
Fisher's exact test.
Pearson's Chi-squared test.
HU: Hashemite University; JUST: Jordan University of Science and Technology; UJ: University of Jordan; YU: Yarmouk University.
Discussion
Pathology is a fundamental medical specialty. Pathologists play a crucial role in diagnosing and managing diseases. Pathology provides vital insights into the structural and functional changes in tissues during disease processes and acts as a bridge between basic science and clinical medicine. Through microscopic examination, molecular testing, and laboratory analyses, pathologists identify disease mechanisms and are key to cancer diagnosis, staging, and treatment assessment. Pathology remains vital in modern healthcare as medicine moves toward personalized approaches and adopts new technologies like digital pathology and genomics. In medical education, pathology serves as the essential link between basic science and clinical practice. Understanding disease mechanisms at cellular and molecular levels helps medical students grasp the pathophysiology of diseases. Comprehending pathology is crucial for future physicians to correctly interpret lab results and effectively incorporate them into patient management and diagnosis.
The findings of this study show medical students’ specialty preferences, with internal medicine, general surgery, dermatology, and ophthalmology being the most commonly selected fields. Pathology was considerably less favored, chosen by only 10.13% of respondents. This highlights a potential gap in exposure, understanding, and interest in pathology as a career option. While many students reported deciding on their preferred specialty during clinical years, a substantial number had not yet made a decision, suggesting a critical period during which targeted exposure to underrepresented specialties like pathology could influence career considerations.
One of the most notable barriers to students considering pathology was a lack of adequate exposure and understanding of the specialty. Only a third of participants agreed they received sufficient pathology training during the preclinical years, and less than one-fifth (17%) felt adequately exposed to consider it as a career. These findings align with previous literature that underscores the role of early comprehensive specialty exposure in affecting student interest. In a study performed to assess student interest and understanding of pathology careers, before and after the Pre-clerkship Residency Exploration Program (PREP) elective at Dalhousie University in Canada, 40 second-year medical students participated in PREP showed that a brief clinical experience in pathology through PREP can improve students’ understanding of pathology careers. 10 In this study, traditional pathology teaching methods—such as microscope work and gross specimen demonstrations—were poorly rated, while case-based learning received slightly more favorable ratings. This suggests a need for clinically integrated educational strategies.
Despite limited consideration of pathology as a career, participants generally recognized that this specialty has the advantages of providing research potential, work-life balance, and intellectual challenge. However, most agreed that pathology involves limited patient contact and is perceived as a career of introverts.
Interestingly, the study identified significant differences in students’ understanding of the pathologist's role, level of engagement with pathology content, and perceptions based on the adequacy of their early training. Students who rated their pathology training as “good” reported significantly better understanding and more positive learning experiences across multiple domains. This association reinforces the importance of preclinical pathology education in shaping students’ preferences of specialties
Conversely, demographic factors such as age, gender, and school background did not significantly influence these outcomes. This suggests that institutional and curricular factors, rather than student characteristics, are more influential in determining perceptions and interest in pathology.
Strengths and Limitations
This study has several strengths, including its relatively good and diverse sample, which covered multiple medical schools across Jordan, thereby enhancing the representativeness of the findings. The use of a well-structured, comprehensive questionnaire enabled the exploration of multiple dimensions of students’ perceptions of pathology (demographics, specialty preferences, perceptions of pathology exposure, curriculum structure, and career considerations), allowing for a multidimensional analysis. The application of appropriate statistical methods increased the robustness of the analyses. Additionally, adherence to STROBE guidelines and obtaining ethical approval strengthened the credibility of the study.
However, certain limitations should be acknowledged. The cross-sectional design precludes establishing causal relationships between exposure to pathology education and career preferences. The self-administered nature of the questionnaire may have introduced response and recall biases, and voluntary participation may have resulted in sampling bias. Furthermore, the absence of qualitative data limits our ability to gain deeper insights into students’ perceptions. Although the target sample size was reached, data saturation was not achieved, which should be acknowledged as a limitation.
Conclusion
This study highlights a concerning lack of interest in pathology among medical students, mainly attributed to inadequate exposure and limited understanding of the specialty. Despite recognizing its intellectual and lifestyle benefits, students rarely consider pathology as a career, often due to teaching methods and a lack of career guidance. Importantly, improved educational experiences were associated with more favorable perceptions and better understanding, indicating that curriculum enhancements, particularly during the early years of medical school, positively influence interest in pathology. Integrated clinical-pathological teaching, increased visibility of pathologists, and mentorship opportunities may help bridge this gap. Ultimately, a concerted effort to modernize and promote pathology education is essential in addressing workforce shortages and ensuring a balanced distribution of future medical specialists.
Footnotes
Authors’ Contribution
NB led the conceptualization and overall coordination of the study. MAA contributed to the design of the methodology and supervised the data analysis process. AR was responsible for the development and validation of the questionnaire, as well as overseeing data collection. MA participated in the data entry, preliminary analysis, and contributed to the literature review. MO assisted in interpreting the results and played a key role in drafting and revising the manuscript. All authors reviewed and approved the final version of the manuscript and agreed to be accountable for all aspects of the work.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
