Abstract
Rationale and Objectives
Teleradiology and artificial intelligence (AI) have emerged as important tools for facilitating healthcare workers in diagnosing, treating, and preventing diseases. They can also be used in the analysis of X-ray images, magnetic resonance imaging, and computed tomography scans. This study delves into the perceptions of medical students at Imam Abdulrahman University (IAU) regarding the role of AI and teleradiology. The findings also shed light on the opinions of medical students at the IAU regarding the potential augmentation and replacement of radiologists with AI.
Materials and Methods
A cross-sectional study was conducted in August 2023 among 292 medical students and interns at Imam Abdulrahman bin Faisal University (IAU), Eastern region, Saudi Arabia, with a response rate of 65.2%. Data were collected using an online self-administered questionnaire. The Chi-square test was applied to evaluate the association between demographic factors and perceptions of AI and teleradiology. Since the study was conducted at a single institution, the findings may not be generalizable to all medical students in Saudi Arabia. Students from other universities with different curricula and exposure to AI/teleradiology may have different perceptions. Future multicenter studies are recommended to provide a broader perspective. Additionally, self-reported data are susceptible to response bias, as participants may provide answers they perceive as socially desirable rather than their true opinions. To minimize this, the questionnaire was anonymous, and students were encouraged to answer honestly. However, the possibility of bias cannot be eliminated.
Results
The study concluded that 65.2% believed that radiologists should embrace AI. Moreover, 56.1% agreed that the AI would augment the radiologist's capability and efficiency. However, 46.2% believed that teleradiology could replace radiologists working at the hospital, and 42.5% agreed that the impact of AI alone would reduce the number of radiologists needed in the field.
Conclusion
Medical students expressed different opinions on the role of AI in augmenting or replacing radiologists. As for teleradiology, the results were promising as students showed interest and optimistic views. Understanding and addressing these perceptions from our future physicians is crucial for developing a strong radiology workforce capable of navigating the transformative journey of a more technological healthcare environment.
Introduction
The field of radiology is undergoing a significant transformation driven by artificial intelligence (AI) and teleradiology. AI tools are now capable of detecting abnormalities in X-ray, computed tomography, and magnetic resonance imaging scans with high accuracy, while teleradiology platforms are expanding access to imaging services in remote areas. These innovations are reshaping diagnostic workflow, improving efficiency, and enhancing patient care, marking a pivotal shift in modern radiology.
As technology continues to revolutionize healthcare, AI and teleradiology have become indispensable in radiology. For instance, teleradiology, the use of technology and electronic communication improves access to remote healthcare services such as diagnosis, examination and medical consultaions. 1
Understanding medical students’ perceptions of these technologies is crucial, as their attitude and knowledge will directly influence their adaptability to integrate them into future clinical practice. Without adequate awareness and training, future radiologists may struggle to adapt to an increasingly AI-driven and teleradiology.
Despite the growing role of AI in radiology, concerns persist regarding its potential to replace radiologists and alter job availability. Similarly, while telemedicine and teleradiology offer improved accessibility and efficiency, their long-term implications for radiology practice remain a topic of debate. Addressing these concerns early in medical education can help ensure that future radiologists are not only aware of technological advancements but also equipped with the skills and confidence to utilize them effectively.
AI has emerged as a critical component in modern medicine, particularly in radiology. AI can predict patient outcomes based on historical data, aiding in patient management and personalized treatment planning. Beyond diagnostics, AI contributes to administrative efficiency by automating tasks such as sorting images based on urgency, ultimately improving workflow and patient care. 2 Similarly, teleradiology has revolutionized healthcare accessibility by enabling faster delivery of imaging results, leading to quicker diagnoses and timely interventions. 3
Despite these advantages, the integration of AI and teleradiology into clinical practice presents several challenges. One major hurdle is the significant financial investment required for infrastructure and training. The high cost of implementing AI-driven radiology solutions may make it difficult for numerous healthcare organizations, especially those with limited resources. Large datasets are also needed for the development and verification of AI algorithms, which raises difficulties within data security, privacy, and the potential for biases in diagnostic accuracy. Furthermore, effective interoperability with current medical systems, which might be technically challenging, is necessary for the incorporation of AI into workflow procedures. A further barrier to widespread utilization is healthcare professionals’ resistance, which stems from concerns regarding losing their jobs and their lack of trust in AI-generated diagnoses.
The utilization of AI in radiology presents a number of ethical and professional difficulties in addition to practical difficulties. The responsibility is an important concern: Who is ethically and legally responsible if an AI system misdiagnoses a patient? Concerns in transparency are also raised by the “black box” aspect of many AI algorithms, which makes it difficult for physicians to completely understand how an AI system makes a certain diagnosis. A heavy reliance on AI may also result in unemployment, which would limit radiologists’ independence in interpreting and validating medical images. Furthermore, since AI systems need huge amounts of patient data, which must be managed with strict privacy protections, patient permission and data security are both important.
The perspective that medical students see AI and teleradiology greatly influences how well-prepared they are for a highly technological healthcare industry. Students may be less likely to adopt new technologies if they believe AI could threaten their job security rather than be a tool to increase performance. Future radiologists are able to understand AI's role as a supporting instrument rather than an alternative for human expertise with the right instruction and training on AI applications in radiology. Medical schools can ensure that graduates are able to use technology effectively in their future jobs by incorporating AI-related courses and practical experience with AI-driven diagnostic tools into their educational programs.
While several studies have explored the impact of AI on radiology, research on medical students’ perceptions remains limited. Most existing literature focuses on the perspectives of practicing radiologists’ and radiology trainees’ attitudes toward AI and teleradiology, with limited emphasis on how medical students who represent the future health workers perceive these technological advancements. Additionally, while AI's technical capabilities in image interpretation are well-documented, fewer studies have examined its impact on medical education and professional training and career decision making. Barriers such as insufficient AI training, doubt about AI-driven diagnoses, and concerns over professional autonomy further complicate its integration into clinical practice. The evolving integration of AI and teleradiology into radiology raises critical questions about how these advancements shape students’ career choices and perceptions of job security. This study aims to bridge this gap by analyzing the perspectives of medical students at Imam Abdulrahman University (IAU), shedding light on their understanding, concerns, and expectations regarding AI and teleradiology in radiology.
Materials and Methods
Study Design and Study Setting
This cross-sectional study aimed to assess medical students’ awareness and attitudes toward teleradiology and the application of AI in radiology. The study was conducted at the College of Medicine in IAU, located in the Eastern Province of Saudi Arabia. The college is affiliated with King Fahad Hospital, a renowned tertiary care teaching hospital equipped with advanced radiology facilities, providing students with exposure to modern imaging technologies.
Participants
A total of 292 medical students from the second to sixth academic years and interns at IAU, both male and female, participated in the study. Inclusion criteria were current enrollment in the medical program and willingness to participate. Students from other health-related disciplines and those who did not provide consent were excluded.
To ensure a comprehensive and representative sample, factors such as gender, academic years, marital status, and total family income were considered. An online recruitment strategy was implemented, where trained data collectors disseminated study details by social media platform and direct communication. This remote, self-administered questionnaire approach ensured accessibility and flexibility for participants.
Questionnaire Development
The questionnaire was designed based on a literature review of AI and teleradiology studies, ensuring relevance to students’ knowledge, attitudes, and concerns. It consisted of a brief introduction to the research topic and the objectives of the study, explaining the aim of the study and assuring confidentiality. It included 4 sections: demographic information, knowledge of AI/teleradiology, attitude toward AI in radiology, and perceived career impact. The questionnaire included both Likert-scale and multiple-choice questions.
Data Collection
The data collection phase lasted for 6 weeks, starting from August 1 to September 13, 2023. Throughout this period, participants were invited to complete the questionnaire online. Data collectors were available during university hours in designated study areas to assist participants, answer any questions or concerns, and ensure the smooth progress of data collection. The extended duration of 6 weeks allowed for an adequate sample size and accommodated the availability and schedules of the participants.
Ethical Considerations
The study received ethical approval from the Institutional Review Board (IRB) of Imam Abdulrahman University (IRB-2023-01-303). All participants provided informed consent and were made aware of the voluntary nature of their participation, as well as the purpose of the study. We prioritized the maintenance of confidentiality and anonymity throughout the research process, and we took great care to prioritize the wellbeing of the participants.
Data Analysis
The data were collected, reviewed, and then entered into the Statistical Package for Social Sciences version 21 (SPSS: An IBM Company). All statistical methods used were 2-tailed with an alpha level of 0.05 considered significant if the P-value was ≤ .05.
Descriptive statistics were used to summarize the participants’ demographic data and their perceptions of AI and teleradiology in radiology, including frequency distributions and percentages. The Chi-square test was used to assess the associations between categorical variables, such as gender, academic year, and opinions on AI and teleradiology. Missing data were handled using listwise deletion to ensure data integrity.
This study adheres to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines for cross-sectional studies. The STROBE checklist has been completed to ensure comprehensive reporting. 4
Sample Size
The sample size was determined based on previous studies assessing AI/teleradiology awareness among medical students. Given the student population at IAU and a desired confidence level of 95%, a sample size of 292 was sufficient for significant statistical analysis.
Results
The participants expressed a range of opinions regarding the role of AI and teleradiology in radiology. Figure 1 illustrates the selection process of study participants. Out of 448 eligible medical students, all were invited to participate. A total of 292 students completed the survey, resulting in a response rate of 65.2%. Nonparticipation (34.8%) was attributed to factors such as lack of interest, academic workload, or technical barriers. A significant proportion, 56.1%, believed that AI would enhance radiologists’ capabilities and improve their efficiency. In contrast, 23.4% felt that AI could completely replace radiologists in the current era, while 42.5% thought AI alone could reduce the number of radiologists needed. Despite these concerns, 65.3% of the students agreed that radiologists should embrace AI and collaborate with the IT industry to facilitate its implementation, as shown in Figure 2.
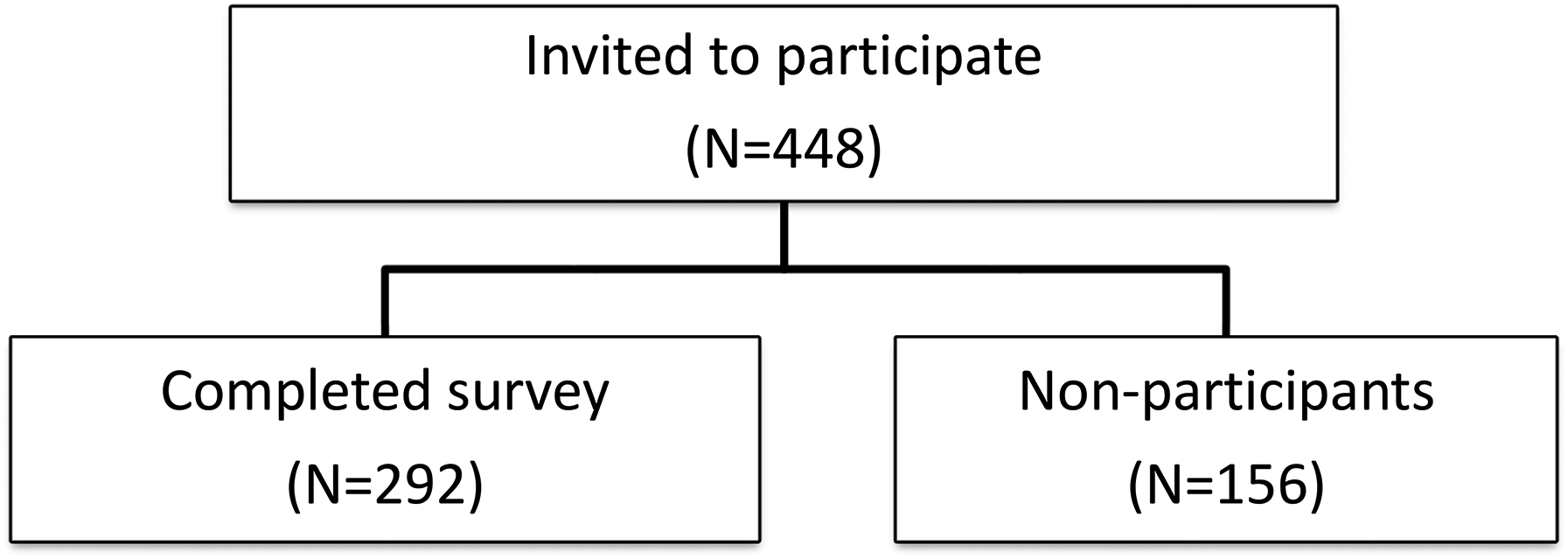
Flowchart of Participant Selection and Response Rate.
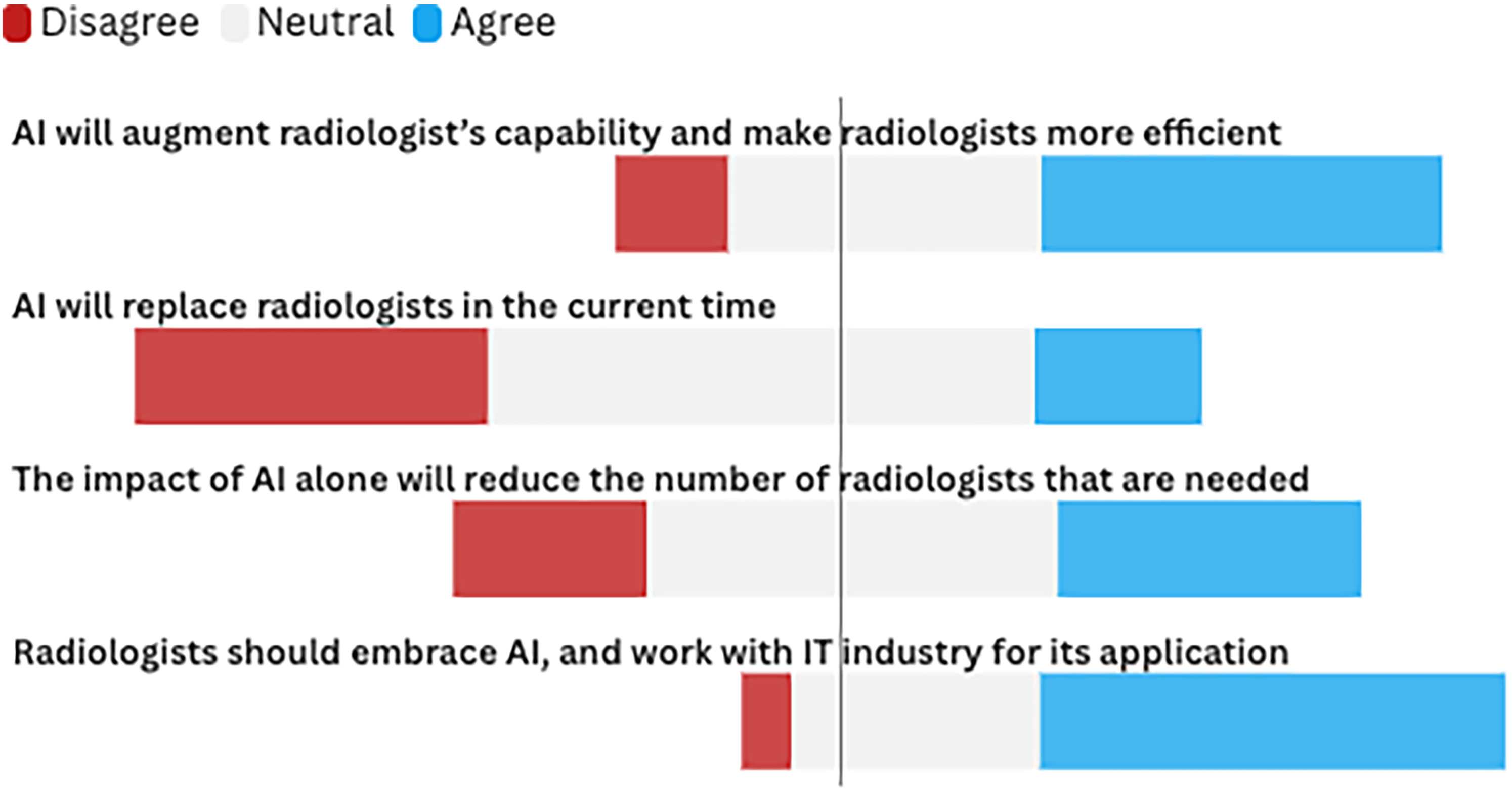
Medical Students’ Perceptions of AI in Radiology.
Regarding telemedicine and teleradiology, 15.5% expressed a personal interest in these technologies, yet 45.5% mentioned that the introduction of telemedicine/teleradiology influenced their decision to pursue radiology as a specialty. Furthermore, 84.9% believed that telemedicine/teleradiology could improve patient care. When asked about the potential impact on the workplace, 46.2% agreed that teleradiology could replace hospital-based work, while a larger proportion, 62.2%, indicated they planned to integrate telemedicine/teleradiology into their future careers, as shown in Figure 3.
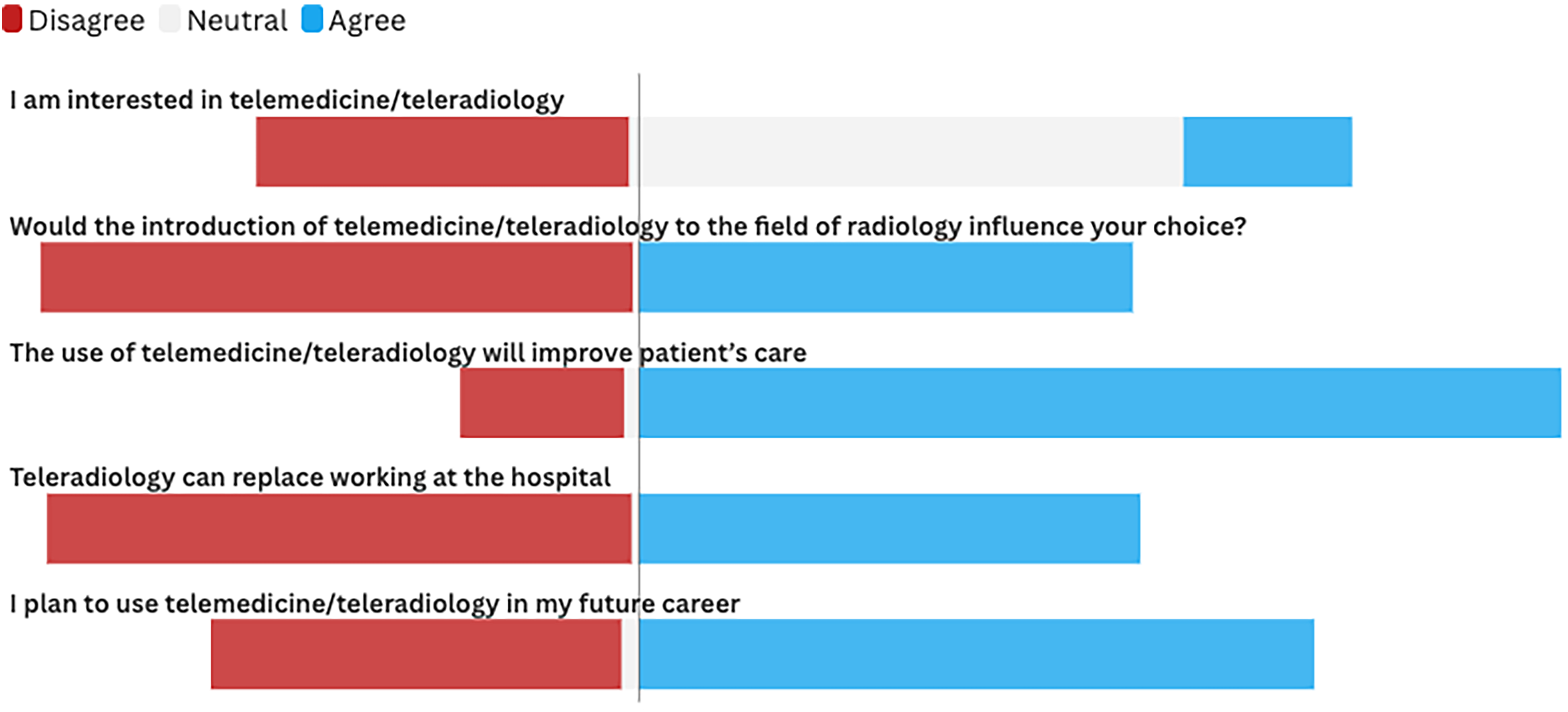
Medical Students’ Perception of Telemedicine and Teleradiology.
Although efforts were made to recruit participants using social media and direct communication, approximately 34% of eligible students did not complete the survey. While the response rate was acceptable, the perceptions of nonrespondents may differ from those who participated, which could influence the results.
A total of 292 responses were analyzed. Missing data were minimal, with listwise deletion applied to maintain data integrity. The proportion of missing responses for individual questions did not exceed 5%, ensuring no significant impact on statistical conclusions. Table 1 presents a summary of participants’ responses regarding AI and teleradiology.
Role of Artificial Intelligence and Teleradiology in Radiology as Reported by Medical Students.

This flow illustrates the selection process of study participants. Out of 448 eligible medical students, all were invited to participate. A total of 292 students completed the survey, resulting in a response rate of 65.2%. Nonparticipation (34.8%) was attributed to factors such as lack of interest, academic workload, or technical barriers. No responses were excluded from the final analysis.
This figure illustrates the distribution of medical students’ opinions on the role of AI in radiology. The responses are categorized into 3 groups: disagree (strongly disagree/disagree) in red, neutral in gray, and agree (somewhat agree/agree/strongly agree) in blue.
The figure demonstrates medical students’ perspectives on telemedicine and teleradiology. The majority agree (blue) that teleradiology can enhance patient care and plan to incorporate it into their future careers.
However, opinions are divided on whether it can fully replace in-hospital work. While many acknowledge its potential influence on career choices, a notable portion remains neutral or disagrees (red) with embracing telemedicine in their practice.
Discussion
In our study, 56.1% of medical students agreed that AI will augment radiologists’ capabilities and improve efficiency. This aligns with a meta-analysis by Hassankhani et al, which reported that 79.48% of respondents, including medical students, radiology trainees, and radiologists, believed AI will revolutionize radiology in the future. 5 Similarly, Klenam et al found that 76.9% of students were influenced to consider radiology as a future career due to the application of technology and AI in the field. 6
Conversely, 42.5% of medical students in our study believed that AI would reduce the number of radiologists needed, and 23.4% felt that AI would replace radiologists. This is consistent with findings from Bin Dahmash et al, where 44.8% of medical students believed AI would minimize the need for radiologists in the future, and 31% believed AI would replace radiologists within their lifetime. 7 Cherry sit also concluded that medical students saw AI as a potential “threat,” making them less inclined to specialize in radiology. 8 Reeder and Lee reinforced these concerns, finding that approximately one-third of medical students thought AI would fully replace radiologists, and about half of aspiring radiologists expressed anxiety toward AI. 9
Moreover, Hassankhani et al noted that medical students had a higher rate of belief (42.66%) that AI poses a threat to the radiology job market compared to radiology trainees and radiologists (6.25%). 5 As the field shifts toward teleradiology, our study found that 45.5% of medical students’ choice of radiology as a specialty was influenced by the introduction of telemedicine/teleradiology. This trend may impact the level of interest in diagnostic radiology, as medical students often prefer specialties with more direct patient contact, as noted by Hammond et al. 10
A systematic review by Santomartino found that medical students were almost evenly divided in their belief that AI poses a threat to the radiologist's role, with 36.6% agreeing, 25.7% neutral, and 37.6% disagreeing. This division highlights the uncertainty among medical students regarding the future impact of AI on radiology. 11
Furthermore, a study by Grayev revealed that approximately one-third of Canadian medical students thought AI would fully replace radiologists, and about half of aspiring radiologists expressed anxiety toward AI. 12 This anxiety may deter some students from pursuing radiology as a specialty.
These studies collectively indicate that while many medical students recognize the potential benefits of AI in enhancing radiological practice, there is also significant concern about job displacement and the future role of radiologists. This ambivalence underscores the need for educational initiatives to address misconceptions about AI and to prepare future radiologists for a landscape increasingly influenced by technological advancements.
Our study, conducted at a single institution focusing on medical students at IAU in Saudi Arabia's Eastern region, has limitations that should be acknowledged. While these findings provide valuable insights, they may not be generalizable to other institutions or regions. Future research should include multicenter studies to capture a more comprehensive perspective. Additionally, the study's participant diversity was somewhat limited, and despite efforts to include a broad sample, the perspectives of underrepresented groups may not be fully reflected. Furthermore, a formal power analysis was not conducted, which limits the ability to determine whether the sample size was sufficient to detect meaningful statistical differences. This should be considered in the interpretation of the results, and future studies should conduct power analyses to ensure adequate statistical power.
The cross-sectional design offers only a snapshot of participants’ perceptions at a specific point in time. Future studies should incorporate a longitudinal approach to track changes in attitudes over time, providing deeper insights into evolving perceptions regarding AI and teleradiology. Moreover, the absence of a comparison group, such as practicing radiologists or other healthcare professionals, restricts the broader context of these findings. Including such groups in future research could offer valuable comparative insights.
To strengthen future research, studies should employ more rigorous designs, expand sample diversity, and integrate advanced statistical analyses. Such approaches would enhance the understanding of medical students’ attitudes toward AI and teleradiology.
Conclusion
Medical students at IAU had mixed views on AI in radiology; some saw it as a tool for improving accuracy and efficiency, while others worried about job displacement. Similarly, many viewed teleradiology as a way to enhance patient care, but concerns persisted about its ability to fully replace hospital-based radiology.
These findings emphasize the need for targeted education to help future radiologists navigate AI and telemedicine advancements. Integrating these topics into medical training will ensure a workforce that embraces innovation while maintaining patient-centered care.
Supplemental Material
sj-docx-1-mde-10.1177_23821205251358005 - Supplemental material for Attitudes and Awareness of Medical Students Toward Teleradiology and the Application of Artificial Intelligence in Diagnostic Radiology: A Cross-Sectional Study
Supplemental material, sj-docx-1-mde-10.1177_23821205251358005 for Attitudes and Awareness of Medical Students Toward Teleradiology and the Application of Artificial Intelligence in Diagnostic Radiology: A Cross-Sectional Study by Afnan Almuhanna, Danyah Almohsen, Deem AlSultan, Deemah Alhuraish, Farah AlRatrout, Rabab Alzanadi and Rana Abbas in Journal of Medical Education and Curricular Development
Footnotes
Ethical Considerations and Consent to Participate
This study obtained approval from the Institutional Review Board (IRB) at Imam Abdulrahman Bin Faisal University on July 31, 2023.
IRB number: IRB-2023-01-303
Consent for Publication
All participants provide consent for publication of the research manuscript. We confirm that we have reviewed and approved the final version of the manuscript for publication.
Author Contributions
AA supervised the project. FAR contributed to the introduction. DHA wrote the results. DA wrote the discussion. DAS served as the project administrator and wrote the abstract and results section. RAZ contributed to data analysis and prepared the table. RA wrote the limitations, added the charts, figures, and contributed to the submission. All authors reviewed the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets used or analyzed during the current study are available from the corresponding author on reasonable request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
