Abstract
INTRODUCTION
Inpatient psychiatry faculty manage complex clinical, administrative, and legal issues amid increasing mental health service utilization rates, limiting time for (1) focusing on lifelong learning and (2) connecting. We examined the impact of a monthly journal club on inpatient psychiatry faculty's (1) confidence that their practice is evidence informed, (2) stress related to board recertification, and (3) sense of connectedness with peers.
METHODS
We employed a primarily qualitative approach using semi-structured interviews and brief survey questions to elicit input from inpatient psychiatry faculty at an academic medical center on their experience participating in a monthly journal club, including perceived changes in one's practice of evidence-based medicine, recertification stress, and connectedness with peers.
RESULTS
Thirteen faculty who participated in the journal club responded to at least one survey or interview. Many faculty reported feeling more confident that their clinical practice was evidence informed, less stressed about board recertification, and more connected to peers at 6 and 12 months following the commencement of the journal club. Following in-person attendance, video-based learning (an innovative method of participating in the journal club) was found to be the second most preferred method of participation among respondents. All respondents noted that the journal club was a valuable use of their time and enjoyable.
CONCLUSION
A monthly journal club has the potential to increase hospital psychiatry faculty confidence in evidence-based clinical practice, reduce board recertification stress, and improve sense of peer connectedness. Future research should examine the journal club experience and impact among a larger number of faculty and incorporate additional measures of learning outcomes.
Introduction
Psychiatrists working as faculty on inpatient psychiatric units within academic medical settings face many challenges, including managing high clinical acuity, overseeing multidisciplinary teams, effectively teaching and supervising medical learners, and addressing legal (eg, civil commitment) and administrative (eg, insurance authorization) issues. 1 Moreover, rates of mental health service utilization have increased since 1990,2,3 with an especially noticeable increase following the Covid-19 pandemic.4–6 Among those psychiatrically hospitalized, research has shown longer lengths of stay and increased suicidal ideation since the start of the Covid-19 pandemic. 7 All of these demands siphon the time for inpatient psychiatry faculty to (1) focus on lifelong learning and (2) connect with each other as a community.
Regarding lifelong learning, research has suggested that psychiatrists have generally found the American Board of Psychiatry and Neurology (ABPN)'s article-based continuing certification (ABCC) program to be meaningful, relevant, positively impacting patient care, and strongly preferable to the traditional every-10-year multiple choice examination format. 8 Research has not explored the extent to which the ABCC program contributes to stress and subsequent burnout. In our anecdotal experience, psychiatrists in a variety of settings commonly report some level of stress related to completing article-based requirements for board certification, given time constraints created by high clinical demands and obligations outside of work.
These same time constraints can limit opportunities for inpatient faculty to connect on a professional or personal level, further compounded by the lingering effect of restrictions on group gatherings imposed during the Covid-19 pandemic. 9 A lack of connection with peers can have an adverse impact on faculty morale, feelings of belongingness, and vulnerability to burnout. 10 Given the increasing attention to the outcome of provider burnout in the literature, recommendations have been made for organizational leaders to actively build a community of mutual support to counter burnout among health providers. 11
One vehicle with the potential to facilitate lifelong learning, reduce board recertification stress, and enhance connectedness among inpatient psychiatry faculty is the implementation of a journal club. Historically defined as “a group of individuals who meet regularly to discuss critically the clinical applicability of articles in the current medical journals,” 12 the first formally documented journal club was established by Sir William Osler in 1875 at McGill University in Canada, as a way of sharing limited educational resources. 12 Osler encouraged his journal club attendees to apply their recently acquired knowledge from this forum to the care of their patients, precedentially starting a journal club goal of fostering knowledge sharing and translation into evidence-based care. 13 Since then, identified evidence-based considerations to develop or enhance a journal club curriculum include focusing on one article at a time, having a weekly to monthly cadence, scheduling according to participant availability, using a duration of 60 min, including 5 to 15 participants, using collaborative learning to encourage diverse perspectives and develop interpersonal skills, using technology-enabled learning such as blogs, videoconferencing, or social media to increase accessibility and engagement, having faculty- or participant-driven leadership, offering incentives (eg, refreshments), summarizing key points, sharing an article and discussion summary for additional self-directed learning, and implementing iterative changes based on participant feedback.14–17
Research suggests journal clubs have accomplished the goals outlined by Osler, in addition to fostering collaboration, critical appraisal, and leadership skills in medical learners of all stages, particularly if utilizing mentored approaches (whereby a faculty member oversees residents engaging in peer teaching) and group discussions.18–22 While various formats of journal clubs have emerged over the years (ie, in-person, virtual, hybrid mixture of in-person and virtual, and social media-based),14,23 each with their advantages and drawbacks, most have maintained goals of keeping current with and critically appraising health literature. Less is known to date about the impact of journal clubs on stress related to board recertification and physician connectedness.
Informed by the literature and our investigative team's professional and scholarly experience, we undertook a primarily qualitative study to examine the impact of a monthly journal club on academic inpatient psychiatry faculty's (1) confidence in conforming to evidence-based medicine (EBM) in clinical practice, (2) level of stress related to board recertification requirements, and (3) sense of connectedness with peers. For brevity, these 3 parameters will be summarized throughout as EBM adherence, recertification stress, and peer connectedness. To our knowledge, this is the first study to explore whether a journal club could be helpful with these particular parameters among inpatient psychiatry faculty.
Methods
Place, period, and nature of study
Our study was conducted at the adult inpatient psychiatry program of Michigan Medicine, an academic tertiary medical center in Ann Arbor, Michigan, from July 2022 to June 2023. We employed a primarily qualitative approach using semi-structured interviews and brief survey questions to elicit information on inpatient psychiatry faculty members’ experiences participating in a monthly journal club. Details of the journal club design and implementation and study methods are presented below.
Inclusion and exclusion criteria
Inclusion criteria for the selection of subjects for our study included being a current faculty member in the University of Michigan Department of Psychiatry regularly working on the Michigan Medicine adult inpatient psychiatry unit. Exclusion criteria included being a current student, resident, or health professional other than a faculty member in psychiatry and not working regularly on the adult inpatient psychiatry unit at this medical center. For feasibility and availability of faculty, we determined that 13 participants would be sufficient for this primarily qualitative study and likely the maximum that could be recruited for the study.
Article presentation
The journal club entailed monthly 1-h presentations utilizing PowerPoint© 24 technology given by 3 of the study authors (DI, AB, and CR, presenting in turn) delivered in a hybrid format to include an in-person and co-occurring virtual format via a cloud-based video conferencing platform (Zoom).© 25 Each presentation reviewed a scientific article featured by the ABPN/ABCC program, addressing topics clinically relevant for an inpatient psychiatry service. The first author (DI) met with other presenting authors (AB and CR) prior to commencement of the first journal club session and on a twice-monthly basis thereafter to collaboratively establish a uniform approach to presenting articles, including highlighting key points in each article, assessing understanding and retention of material through periodic multiple choice questions (carefully crafted so as not to duplicate the quiz questions featured in the ABPN/ABCC portal), and fostering participant engagement through open dialogue for faculty to share related experiences. For in-person attendees, lunch was provided and there were creative incentives to actively participate (eg, treat or gift for faculty who first answered a multiple choice question correctly).
To accommodate faculty members unable to attend the presentations in person or via Zoom,© 25 a highlight document (4 to 5 PowerPoint© 24 slides summarizing key points) and 5-min video summary (5MVS, a video recording of the presenting author discussing the highlight document) were emailed to all hospital psychiatry faculty members following each monthly journal club presentation.
Interviews
Faculty were given the option (via a survey item) to voluntarily participate in a 15-min Zoom© 25 or phone interview with a research team member (AL or LS) regarding their experiences with the journal club. Interviews were semi-structured with a standard set of questions for interviewers to ask respondents and follow-up questions as appropriate based on responses to the standard questions. Interviews were recorded and responses transcribed using the Zoom© 25 transcript function (or by hand in cases of phone interviews) by the 2 research team member interviewers (AL and LS).
Surveys
Inpatient psychiatry faculty members at our academic medical center were sent a brief electronic survey developed specifically for this study, assessing their self-perception of EBM adherence, recertification stress, and peer connectedness. The few survey questions prompted a response from 5 options on a Likert-type scale using Qualtrics© 26 software as seen in Table 1. The questions were sent to faculty at the beginning of the study period (July 2022) and at 6- and 12-month time points following the commencement of the journal club. The initial survey questions (prior to journal club) also prompted respondents to indicate their gender and number of work years as a hospital psychiatry faculty member (<1, 1-5, 6-10, and >10). As seen in Table 1, the 6- and 12-month surveys were slightly modified by inquiring about respondents’ perceptions regarding the 3 parameters of interest relative to six months prior (eg, items would start with, “Compared to 6 months ago…,” and response options included, “Much less,” “Somewhat less,” “Equally,” “Somewhat more,” and “Much more”). The survey also included multiple choice questions assessing how often faculty members read the articles presented, perception of the journal club as valuable and/or enjoyable, and preferred method of participation. Finally, respondents were asked for suggestions to improve the journal club experience, prompting a free-text response where data were treated qualitatively as described below in relation to qualitative data analysis.
Survey items and response choices for main parameters of interest.

Qualitative interview and brief survey question data analysis
An open coding technique was used to generate themes across qualitative semi-structured interview and free-text survey questions. 27 Grounded theory methods 28 were used involving data collection and analysis from semi-structured interviews and free-text survey questions to allow for theories (ie, understandings of journal club experiences) to emerge and be grounded in the collected data. The themes that emerged across all qualitative data were subsequently organized through a deductive process into a final framework for interpreting journal club experiences. Univariate explorations were conducted in Excel 24 of responses from the brief survey questions for descriptive purposes (ie, frequency and percentage) at the initial, 6-month, and 12-month time points. Data pertained to faculty gender, number of years working as an inpatient faculty member, and faculty perceptions of the journal club (including EBM adherence, recertification stress, and peer connectedness). Faculty perceptions were also explored observationally in relation to gender and number of years working as an inpatient faculty member; however, significance testing was not possible given that the small sample size reduced statistical power. As a final step of analysis, we made descriptive observations of the 3 aforementioned faculty perception parameters in concert with any other identified themes from the free-text survey responses and semi-structured interviews until data saturation was reached. Again, due to small sample size and the primarily qualitative aim of this study and data collection, significance tests were not performed.
Ethics approval and informed consent
This project was reviewed by the University of Michigan Medical School Institutional Review Board (IRBMED) and received a Not Regulated as Human Subjects Research designation, study ID: HUM00218771. The act of filling out the anonymous surveys constituted implied agreement to participate in this element of the project, and all interviewed subjects willingly agreed to participate in interviews prior to these sessions being conducted.
We used the SQUIRE checklist when writing our report. 29
Results
A total of 11 monthly journal club sessions were held between July 2022 and June 2023; a session was not held in April 2023 due to illness of the person who had planned to present at the journal club that month. While we did not maintain a strict attendance record, in-person attendance ranged from 2 to 12 faculty members at a given journal club session. Of 13 eligible inpatient faculty members in this study, 10 completed the initial survey (response rate 77%), 8 completed the 6-month survey (response rate 62%), and 6 completed the 12-month survey (response rate 46%). Figure 1 shows the breakdown of respondents by gender and number of years working on the inpatient unit; slightly higher proportions of women and faculty working on the unit for 1 to 5 years were observed.

Breakdown of respondents by gender and number of years working on inpatient unit. (a) Breakdown of respondents by gender. (b) Breakdown of respondents by number of years working on inpatient unit.
Most faculty reported feeling equally confident that their practice was evidence informed after participating in the journal club, while a minority reported a modest increase in such confidence. Most faculty also reported feeling less stressed about board recertification after 6 months, and, by 12 months, all reported feeling less stressed. In addition, most faculty felt more connected with peers after the first 6 months and equally connected at 12 months. See Figures 2 to 4 for raw data on survey responses regarding self-perception of EBM adherence, recertification stress, and peer connectedness, respectively.

Level of confidence in evidence-informed practice at baseline, 6 months, and 12 months.

Level of stress related to board recertification at baseline, 6 months, and 12 months.

Level of perceived connectedness to peers at baseline, 6 months, and 12 months.
In terms of demographic variables (Tables 2 to 4, available in online supplement), prior to the commencement of the journal club, men and women appeared equally confident in practicing EBM, and, at 12 months, equal proportions of each group (1/3 each) were somewhat more confident that their practice was evidence informed. Although more women than men reported feeling stressed about board recertification prior to starting the journal club, at the 12-month mark, all respondents reported feeling less stressed. Equal proportions of women and men noted some level of connectedness prior to journal club commencement, and feeling more connected with their peers at 12 months compared to before the journal club started.
Results of baseline survey of hospital psychiatry faculty.
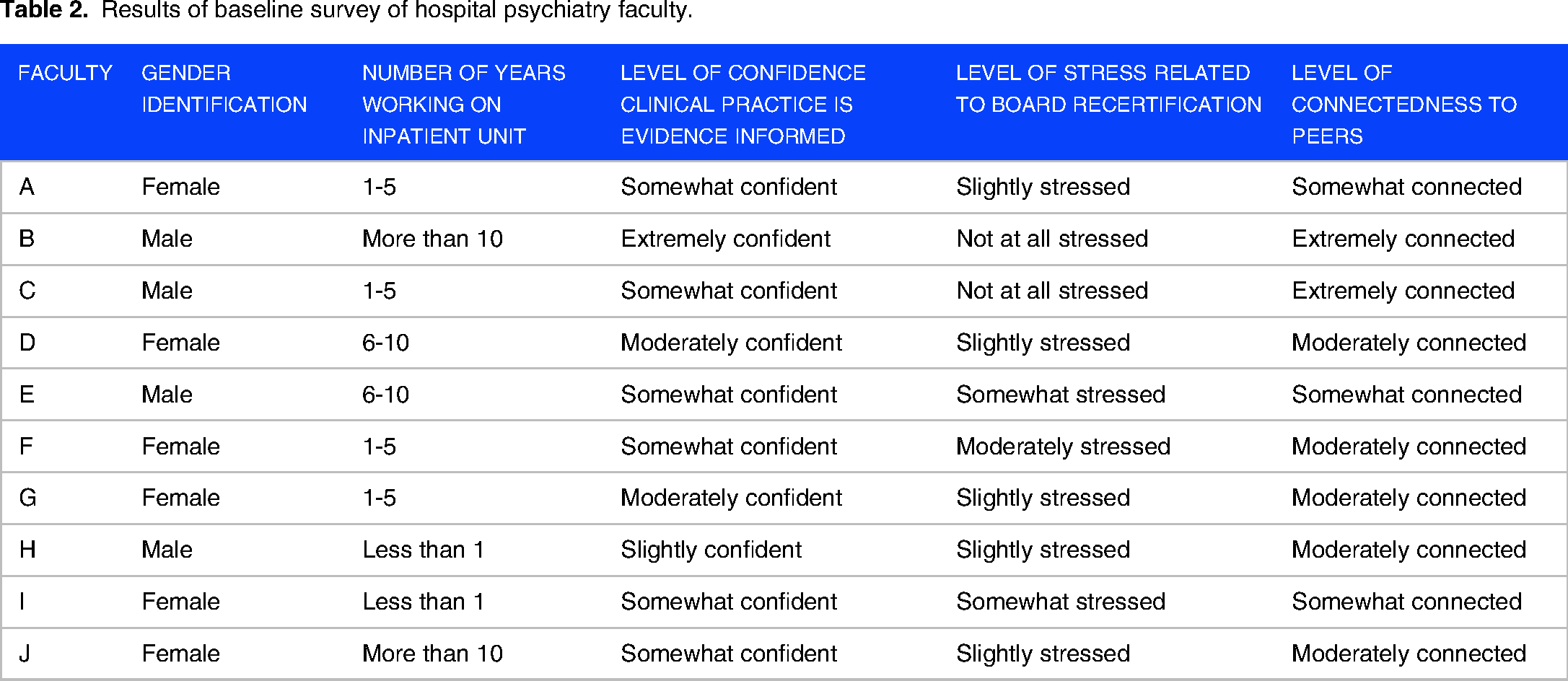
Results of 6-month survey of hospital psychiatry faculty.
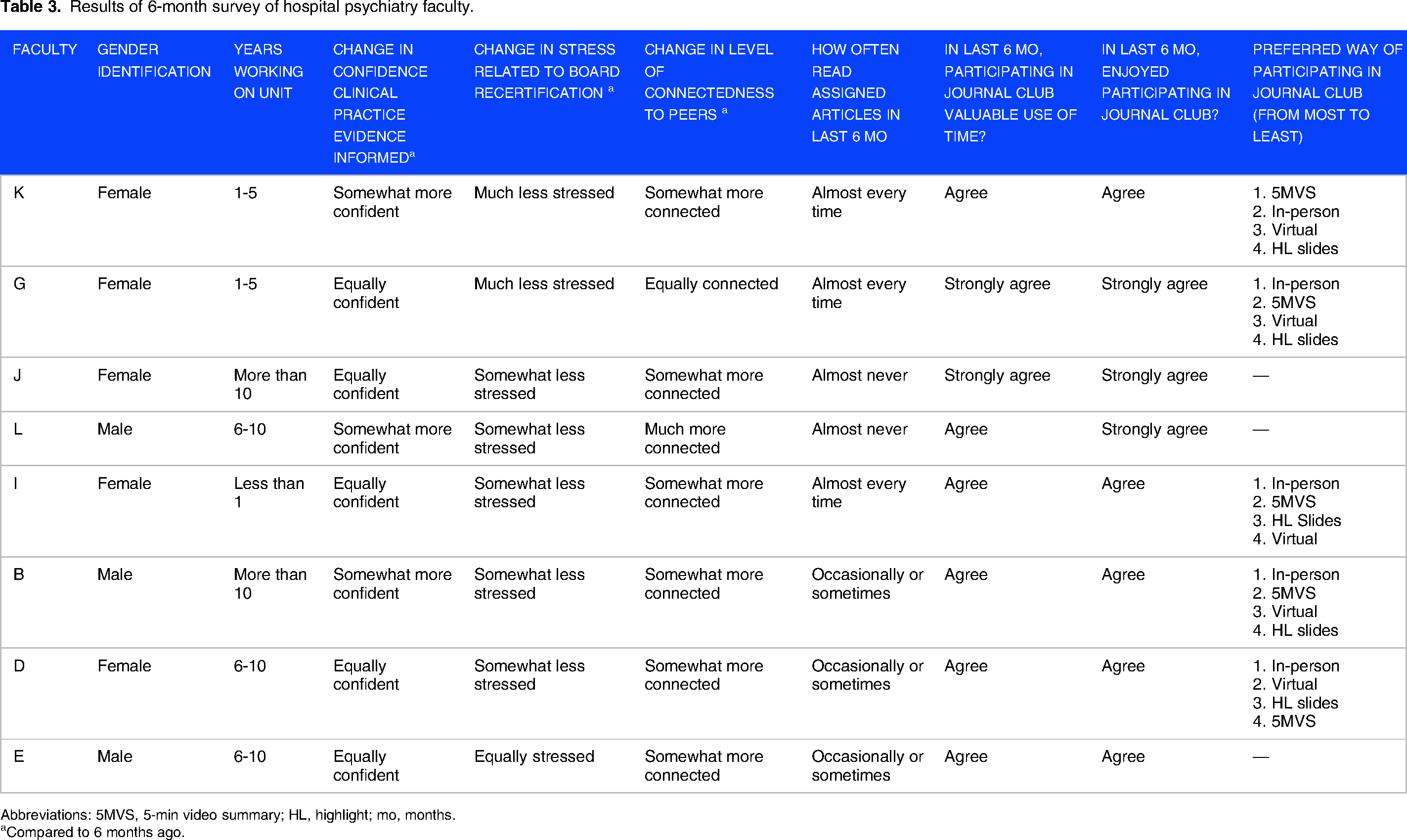
Abbreviations: 5MVS, 5-min video summary; HL, highlight; mo, months.
Compared to 6 months ago.
Results of 12-month survey of hospital psychiatry faculty.

Abbreviations: #, number; 5MVS, 5-min video summary; ABPN, American Board of Psychiatry and Neurology; HL, highlight; mo, months.
Compared to 6 months ago.
In the initial/baseline brief survey questions, confidence that one's clinical practice was evidence informed was higher in more senior faculty compared with more junior faculty; however, at 6 and 12 months, we observed no such pattern. Junior faculty (those with less than 5 years working on the unit) reported feeling “much less stressed” over completing board recertification requirements at 12 months compared to baseline or 6 months; otherwise level of stress did not appear observationally to vary across years of experience working on the unit. Similarly, level of peer connectedness did not appear observationally to vary across number of years working on the unit.
Figure 5 displays survey responses to items addressing the inherent quality of the journal club experience, elicited at 6 and 12 months (also shown in Tables 3 and 4). For example, most respondents read the articles presented at least occasionally and all respondents endorsed feeling that the journal club was enjoyable and a valuable use of their time.

Survey responses to items addressing inherent quality of journal club experience. (a) In the last 6 months, I read the assigned articles for journal club. (b) In the last 6 months, participating in the journal club was a valuable use of my time. (c) In the last 6 months, I enjoyed participating in the journal club.
Figure 6 displays faculty members’ preferred method of participating in the journal club (also shown in Tables 3 and 4), ranked from most to least preferred (total of 5 faculty responses for this item at the 6-month time point and 3 faculty responses for this item at the 12-month time point). In-person discussion was the most preferred (ranked first by 4 of 5 respondents at the 6-month time point and 2 of 3 respondents at the 12-month time point), followed by watching the 5MVS (ranked first by1 of 5 respondents at the 6-month time point and 1 of 3 respondents at the 12-month time point), virtual (Zoom© 22 ) participation, and reviewing the “highlight” slides. Results (as shown in Tables 3 and 4) suggested that non-in-person participants experienced similar benefits from the journal club as in-person participants, although the small number of respondents in each category precluded statistical analysis for significant differences between these groups. Of note, 6 faculty respondents (3 at the 6-month time point and 3 at the 12-month time point) did not respond to the survey item asking about the preferred mode of participation, making it difficult to ascertain if additional faculty members participated via non-in-person forums and if so, experienced similar benefits.

Respondents’ preferred method of participating in journal club. (a) Q11: Considering the last 6 months, please rank the different ways of participating in the journal club in order from your most preferred to your least preferred (6-month time point). (b) Q12: Considering the last 6 months, please rank the different ways of participating in the journal club in order from your most preferred to your least preferred (12-month time point).
Table 4 displays faculty responses to the statements (presented at 12 months), “I took ___ of the ABPN/ABCC article quizzes corresponding to the 11 articles presented in Journal Club this past year,” and “I passed ___ of the ABPN/ABCC article quizzes corresponding to the 11 articles presented in Journal Club this past year.” Although the 6 faculty who responded to this item took varying numbers of quizzes, in almost all cases (12/13), respondents successfully passed the quizzes they chose to take. Of note, the relatively small number of faculty who reported taking the quizzes at the 12-month survey (3 of 6) is partly due to one respondent having just passed her initial board certification examination as the journal club started, and another faculty member having completed her ABPN article quizzes prior to journal club commencement.
Table 5 presents the qualitative themes identified from (1) semi-structured interviews of 8 faculty respondents and (2) faculty free-text responses to the brief survey items, “If you would prefer another forum or approach to enhancing evidence-informed care or reducing stress related to recertification, please describe…” and “Please enter any other comments about your journal club experience, or other ways of supporting connections with your peers.” The themes identified from these free-text survey responses and interviews, for which data saturation was reached, were as follows:
Many faculty appreciated the various methods for participating in the journal club, which allowed them to partake in some capacity, even if they were unable to do so in person: My schedule is pretty busy/hectic, so it's not easy to make these, but I appreciate the video summaries and the highlight slides. (Faculty A, female, 1-5 years on unit) Themes identified from faculty interview and free-text survey responses regarding journal club experience. I have not been able to successfully attend an in-person session due to scheduling limitations, but learn from and thoroughly enjoy the slides and recap provided! (Faculty G, female, 1-5 years on unit) Faculty valued the inclusion of residents in the journal club, as well as the opportunity to connect with peers: I think that this was a great opportunity to meet with colleagues and learn from others including our own residents. (Faculty M, male, 6-10 years on unit) Residents seeing attendings learning was a positive. (Faculty D, female, 6-10 years on unit) It was good to see some of the younger residents; put us on the same playing field… raised my opinion of some of the residents who helped [by presenting articles] or really spoke up; made me feel more connected. [As a] byproduct, allows faculty to evaluate residents for their own evaluations. (Faculty J, female, more than 10 years on unit) Attendance/participation in the journal club sessions was limited by logistical constraints, including insufficient time, conflicting obligations, location, technical difficulties, and shift-based conflicts: Busy service, one time [I] wanted to do it virtually, but [the] Zoom link didn’t work. (Faculty A, female, 1-5 years on unit) Struggled to attend… purely logistics, too many other competing things going. (Faculty E, male, 6-10 years on unit) Faculty generally preferred to participate in the journal club in-person, and this forum seemed to be linked to a sense of connectedness: Good to come together in an educational environment with peers…. (Faculty B, male, more than 10 years on unit) Physical presence, interpersonal interaction is important. (Faculty D, female, 6-10 years on unit) It was much more collegial in person, and I think I can pay attention more in person than over Zoom. Over Zoom, I’m more likely to multitask. (Faculty I, female, less than 1 year on unit) Faculty appreciated lunch being made available at the journal club sessions: Lunch always helps. It does make a difference, especially if it's a busy day. I figure I can make it to journal club for at least 45 minutes. If there wasn’t lunch there, I’d probably choose to go to the cafeteria first. (Faculty I, female, less than 1 year on unit) Free lunch was a bonus! (Faculty C, male, 1-5 years on unit) Faculty generally found the journal club to feature clinically relevant articles, be a helpful and more engaging way to prepare to take the ABPN/ABCC maintenance of certification quizzes, and demystify and normalize the recertification process: Appreciated the clinical connection between a recent journal article and practice. (Faculty H, male, less than 1 year on unit) Worthwhile approach? Yes, definitely! I have to do 50 articles every 3 years; really grateful they did this. (Faculty J, female, over 10 years on unit) 100% helped with the quizzes; it made it very easy to pass… anything we can do to help recertification. Better than doing this by yourself. (Faculty M, male, 6-10 years on unit) From a faculty development standpoint, this helped to “educate and normalize” this recertification process (some people were unaware this was an option to take these quizzes as a recertification every 3 years). (Faculty I, female, less than 1 year on unit)

Discussion
Study findings that a third of participants reported perceiving improved confidence in evidence-based practice and that articles were perceived as clinically relevant are consistent with literature to date on the benefit of journal clubs in facilitating knowledge acquisition and confidence in applying this information to clinical practice.14,18,22 Our observation that most faculty did not perceive improvement in EBM adherence could reflect sample selection effects, as faculty offered academic medicine positions likely demonstrate reasonable clinical skills and adherence to EBM at the time of hire, making it less likely that they would report low confidence at baseline.
Many faculty expressed that participating in the journal club helped decrease their recertification stress, liked efforts that reduced barriers to participation (eg, delivering content in multiple formats and providing lunch at live presentations), and found the journal club a more engaging way to prepare for recertification that demystified the process. With fewer logistical barriers, enhanced participation, and greater engagement, faculty may have felt less stressed as they experienced the reading of recertification articles as less laborious than initially imagined. Our observations are supported by other authors who, while not directly measuring board recertification stress, have noted the earning of continuing medical education credits and maintenance of certification as important benefits of journal clubs in academic settings.14,22
Additionally, many faculty expressed that journal club participation increased their sense of connectedness with peers; moreover, we heard faculty comment on appreciating opportunities to connect with residents. The beneficial effects of face-to-face journal club interactions on participant connectedness 30 and of promoting social connection between residents and faculty in academic settings 31 have been published. This literature reinforces our study findings and points toward the implication that journal clubs have important potential to be beneficial for faculty.
An interesting finding from our study to note is that faculty rated the 5MVS as the second most preferred method of participating in the journal club. This tool was created to provide an easily accessible, time-efficient, and multisensory (visual and auditory) means of helping faculty learn the key concepts from relevant articles, taking into account busy faculty schedules and differences in faculty learning styles (eg, visual vs auditory learners). The proposed use of this innovative educational tool in medical learners with attention deficit hyperactivity disorder has been published. 32 Frequent external interruptions in the day of an inpatient psychiatrist limit opportunities to have undivided attention for extended periods of time. Our results suggest that the 5MVS could be useful in keeping hospital psychiatry faculty (and potentially faculty and learners in other medical disciplines) current on evidence-based practice when full reading of scientific articles (or on-site attendance at journal clubs) is difficult to achieve.
Although the results of this study are preliminarily encouraging, some limitations should be noted. First, this was a primarily qualitative, longitudinal, non-controlled study design, thereby limiting our ability to draw any conclusions about the causal influences of the journal club on the parameters of interest. Second, the sample size of this study was small, limiting its power and our ability to detect significant differences between faculty groups based on factors such as gender or number of years working on the unit, the suitability of the study to statistical analysis, and the generalizability of the findings. As such, no sample size/power analysis was performed. However, the small sample size also accurately reflects the relatively small numbers of inpatient psychiatrists comprising the faculty at many academic facilities. Third, although we attempted to assess the impact of the journal club on faculty learning by inquiring whether respondents felt the journal club was helpful to their clinical practice and how many of the 11 ABPN/ABCC article quizzes they had taken and successfully passed over the study period, these measures of learning outcomes were subjective and recall dependent, respectively. Fourth, although faculty schedules served as one nidus for the development of the journal club (to make learning content of relevant scientific articles easily accessible and engaging), schedule and availability also impacted faculty attendance at the journal club sessions, with some sessions having only 2 or 3 faculty members present (in-person and virtually). This limited the number of sessions that participants were engaged with to ascertain the impact of the journal club on a sense of connectedness among hospital faculty. That stated, even having 2 or 3 faculty present at a session created opportunities for connection, sharing, and support. Finally, given that presentations were rotated among 3 of this study's authors, it is possible that variability in presenting styles may have influenced levels of faculty engagement and learning during a particular presentation. However, regular meetings between the 3 presenting authors (as outlined in the Methods section) hopefully provided for some uniformity in the article presentation.
Future research should expand on our efforts to facilitate effective, engaging continuing professional development of health professionals while reducing recertification stress and improving sense of connectedness among these individuals. Broadening the scope of such initiatives to include other health care disciplines such as nurses, social workers, psychologists, activity therapists, and pharmacists would also be worth exploring, to improve interprofessional connectedness and ultimately patient care by cultivating better-informed, less stressed, and more cohesive multidisciplinary inpatient hospital teams. Preliminary efforts at such initiatives have been published, with encouraging results. 33
Conclusion
The many demands of hospital psychiatry faculty inside and outside of work behoove the development and implementation of approaches to effectively improve confidence in evidence-informed clinical practice, reduce stress related to board recertification, and improve connectedness with peers.
Our study provides potential support for the use of a monthly journal club to achieve these objectives. Academic medical centers and other organizations should consider investing time and resources for dedicated medical staff to organize and execute such programs, including the use of innovative educational tools to enhance learning as a supplement to such programs. If continued benefits are demonstrated moving forward, future research should expand these efforts and consider broadening their scope to include other health care disciplines to ultimately create better-informed, less stressed, and more connected multidisciplinary hospital teams providing improved patient care.
Footnotes
Author Contributions
DI substantially contributed to the conception and design of this study, the acquisition, analysis, and interpretation of the data, and the drafting and revising of the work. AB and CR substantially and equally contributed to the acquisition of the data and the revising of the work. LS and AL substantially contributed to the design of the study and the acquisition and analysis of the data. AH substantially contributed to the analysis of the data and the revising of the work. LB substantially contributed to the qualitative analysis and dissemination of the study, in addition to contributions in writing and editing the revised manuscript. All authors read and approved the final manuscript and have agreed both to be personally accountable for the author's own contributions and to ensure that questions related to the accuracy or integrity of any part of the work, even ones in which the author was not personally involved, are appropriately investigated, resolved, and the resolution documented in the literature.
DECLARATION OF CONFLICTING INTERESTS
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
FUNDING
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for lunches and creative participation incentives was provided by an educational initiative unit fund supplied to each inpatient unit by our institution.
Consent to Participate
This project was reviewed by the University of Michigan Medical School Institutional Review Board (IRBMED) and received a Not Regulated as Human Subjects Research designation, study ID: HUM00218771. The act of filling out the anonymous surveys constituted implied agreement to participate in this element of the project, and all interviewed subjects willingly agreed to participate in interviews prior to these sessions being conducted.
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Ethical Considerations
All study protocols were approved by our institutional review board at Michigan Medicine, IRBMED, study ID: HUM00218771.
