Abstract
US medical students, even before the COVID-19 pandemic, exhibited higher rates of mental health challenges than age-matched cohorts. The National Resident Matching Program (NRMP) match process, which places medical students into residency, is the culmination of medical school training and a well-recognized stressor that amplifies anxiety levels and the mental strain that accompanies medical school. Facing an unprecedented year with a decrease in 2021 NRMP placement percentages, Rocky Vista University College of Osteopathic Medicine (RVUCOM) introduced an innovative new program, the predoctoral internship (PDI), to support students who did not match into a residency program. At no extra expense to the student, this program offers a year-long opportunity to customize experiences in both clinical and academic settings, along with leadership training, aimed at bolstering their residency applications. Alternatively, students could participate in a Master's PDI (MPDI), which allowed students to concurrently pursue a master's degree of their choosing with an external program. RVUCOM achieved 100% placement for students completing the PDI or MPDI program, aligning with the institution's historical graduate trends. Perhaps equally important, students in the program reported feeling supported and less ashamed, fostering loyalty to RVUCOM. Transparency in communication and leaning into institutional values reinforced trust within community partners. The intentional balance of rigor and support, coupled with faculty investment, proved crucial for success. The experience held students accountable, allowing personal and professional growth and fostering the development of a deeper professional identity. RVUCOM's innovative approach to unplaced students not only addresses the challenges faced by RVUCOM students not achieving a residency placement, but also transforms an unforeseen circumstance into an opportunity for growth, resilience, and the development of more competitive and accountable medical graduates.
Keywords
Introduction
Each year graduating medical students, both MD and DO, enter the National Resident Matching Program (NRMP) seeking placement in residency programs designed to train physicians in specific medical specialties. The Match process consists of 4 primary phases: Match Monday, Supplemental Offer and Acceptance Program (SOAP), Match Friday, and The Scramble. Together, these 4 phases delineate the residency placement process, though it is noteworthy that a student can graduate with a medical degree without securing a residency position (see Figure 1). Failing to participate in any residency program carries substantial social and economic repercussions, leaving students not only unable to pursue clinical medical practice, but also consequently, potentially unable to meet their student loan obligations, resulting in daunting debt and an unescapable social stigma. Guided by the institutional values of compassion, excellence, innovation, and collegiality, Rocky Vista University College of Osteopathic Medicine (RVUCOM) endeavored to provide support for our unplaced students as they faced the challenges and biases inherent in the current placement process. The program described in this perspective report, the predoctoral internship (PDI), which includes elements of additional academic and clinical training as well as soft skills practice opportunities, was designed in response to a higher number of students in the Rocky Vista University College of Osteopathic Medicine (RVUCOM) Class of 2021 who did not place into a residency program; notably, this was the first Match season of the COVID-19 pandemic.
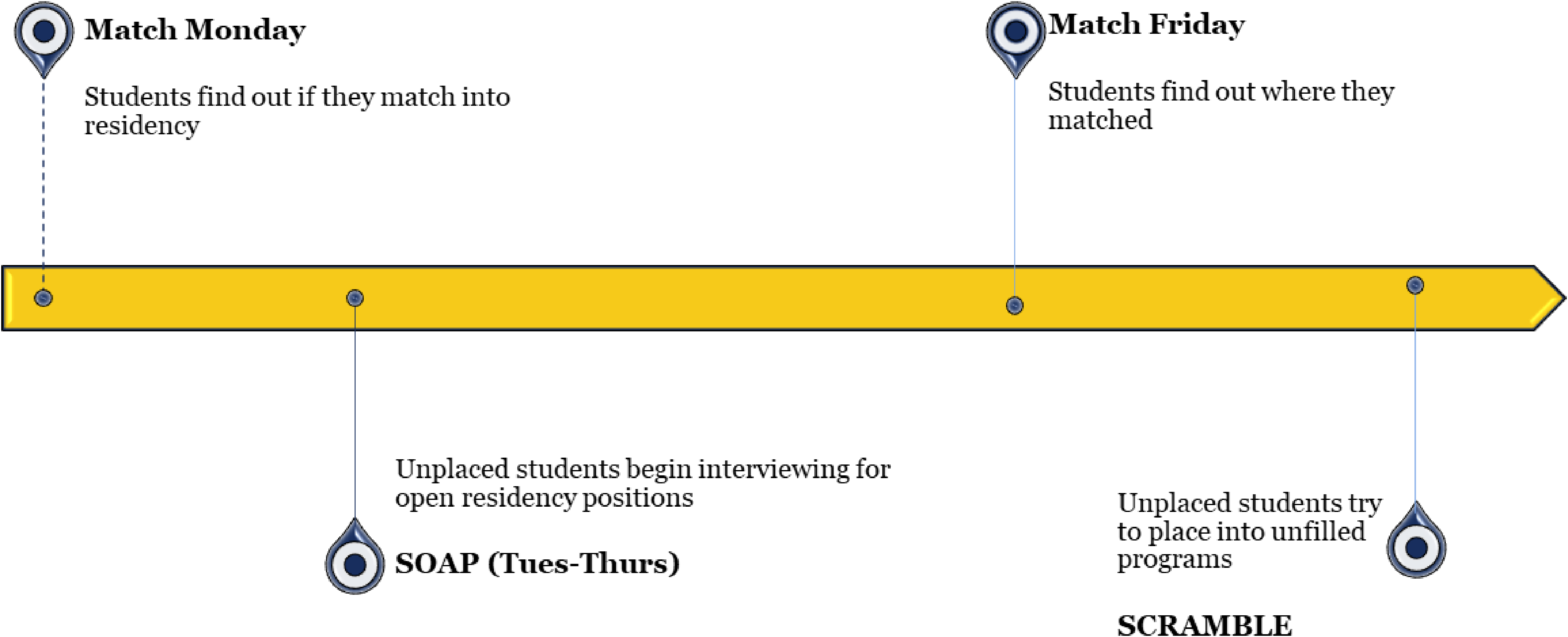
National Resident Matching Program (NRMP) Match activity timeline.
Body
Evaluation of RVUCOM students who have not placed over the last five years reveals some commonalities, including academic profiles not commensurate with the specialties to which they applied and, particularly to the interview and Match season since the COVID-19 pandemic, difficulty in connecting with interviewers through a virtual medium. Placement rates for students entering the Match process after failing to place into residency the first time are notably lower, a reflection of the unique set of prejudgments and assumptions faced by these students. Reasons that medical students do not place into a residency when entering the NRMP Match the second time are likely multifactorial and difficult to define; however, based on anecdotal evidence, potential reasons include misguided perceptions of applicant qualifications, along with a perceived lack of academic work and clinical exposure experienced between Match seasons. Additionally, those individuals re-applying for residency after an unsuccessful match often do not have the skills or language to be able to define their experience, which may give the impression that they are not capable of self-reflection.
In addition to examining student-specific factors that contribute to unsuccessful matches, characteristics of residency program selection behavior must also be considered. A common experience for Osteopathic graduates is the perception of bias that they are not as competitive in residency placement as their MD counterparts. While little research has been done to elucidate the characteristics of residency programs more apt to accept DO applicants, a recent study indicates that the most important factor in DO residency placement, especially in more competitive specialties, is whether that program has accepted DOs in the past. 1
Irrespective of individual student or residency factors, the impact of the current matching process on the mental health of students is undeniable. Mental health in the medical student population has been increasingly studied in recent years. Prior to the COVID-19 pandemic, US medical students showed significantly higher rates of depression, anxiety, and suicidal ideation than their age-matched peers. 2 In the summer of 2020, only months into the COVID-19 pandemic, 66% of undergraduate medical education students reported experiencing mild–severe anxiety, compared to prepandemic estimates of ∼20%. While there were stressors common to all students, including virtual residency interviews, rotation availability, and general pandemic exhaustion, students in each stage of training expressed themes distinct to their level of training. Fourth-year students, those entering the residency interview season, expressed high levels of anxiety compared to cohorts prior. As a result of instability in the traditional delivery of clinical education and national assessments, they also reported elevated concerns regarding their ability to take national board examinations and the fluidity of the residency selection process, including audition rotations and the NRMP process, amplifying an already acknowledged highly stressful time for medical students. 3
Residency placement and the NRMP match process are well-recognized sources of stress for medical students. In 2021, there were 42 508 total applicants for 35 194 postgraduate Year 1 positions. Nationally, 89.1% of 7101 US DO senior applicants matched, with 42.4% matching into their first-choice specialty and location, and 72.2% matching into 1 of their top 3 choices. Comparatively, US MD seniors saw a 92.8% match rate, with 46.4% attaining their first-choice placement, and 72.3% attaining 1 of their top 3 choices. This data tells us that ∼10% of US DO seniors did not match and needed to participate in the SOAP process or scramble for a residency spot.
Importantly, the NRMP data differentiates between first-time applicants, known as seniors, and graduates. A significant percentage of graduate applicants are those who were unsuccessful in their initial attempt to match as seniors. Both DO and MD graduates see a far reduced chance of placing into a residency. Match rates for DO graduates entering the 2021 Match after an unsuccessful match in 2020 decreased exponentially with a 44.3% placement rate, with a range of 38.4%–48.0% in a 5-year analysis. Comparatively, the US MD graduates saw a 48.2% placement rate, with a range of 43.8%–48.2%. 4 In addition to augmenting skills to assure the students’ future competitiveness, this phenomenon was a strong motivation for developing the PDI and Master's PDI (MPDI) programs.
In the Spring of 2021, RVUCOM experienced an anomalous year in terms of the NRMP Match with 95.8% of students placing on Match Monday, down from the consistent 99% seen in the previous 5 years. 5 While students placing during the SOAP was well above the national average noted above, and additional students placed in the scramble, RVUCOM still experienced an unprecedented 11 students unplaced by July 2021.
RVUCOM responded rapidly to this difficult situation. In tandem with the work being done to help students place, faculty and administrators developed the PDI within a 10-week time frame. The PDI is a yearlong, innovative program designed to tailor experiences to unplaced students’ individual needs and is offered to them tuition free. The students do not graduate with their matriculating cohort, instead extending their graduation by a year. Two variations of the program are available: the PDI or the MPDI. Critical steps in the process included creation of student learning outcomes consistent with program learning outcomes, building of syllabi, approvals through the program and institutional curriculum committees, and Rocky Vista University (RVU) Board approval. Both programs have successfully run each year since their inception, though with fewer students. The PDI is a 48-credit course split into 24 credits per semester. The MPDI is a 24-credit course split into 12 credits per semester with students concurrently enrolled in an accredited Master's program of their choice at a separate institution. The most common additional degree chosen by MPDI participants is a Master's in Public Health. MPDI students participate in all aspects of the program, with less emphasis on the teaching requirements described below. All work and financial obligations toward their chosen master's degree are handled through the host university (see Figure 2).

Predoctoral Internship (PDI) structure.
Participants in both programs specify 1 out of 4 focus areas in which they want to work: research, primary care, anatomy, or simulation medicine, each giving them a deeper understanding of how to operate within a team of educators (see Figure 3). Students work with faculty in their focus area to help deliver curricular content through lab or small group experiences. Students’ choices were heavily influenced by their future career desires. For example, a student interested in surgery has been more likely to choose to work with the anatomy team during their PDI/MPDI year. All students are also required to participate in research, either publishing or presenting their research at a conference; perform 2 audition rotations; and have regular meetings with their faculty mentors and career advisors. Successful completion of the PDI and MPDI programs entails demonstration of the AAMC's 13 Entrustable Professional Activities, 6 satisfactory progress during quarterly evaluations, and good academic standing in clinical rotations.

PDI Focus areas.
Resources required to execute the program are less than expected, with investment of faculty time being the most needed resource. One course director is identified for both programs, who works closely with the Senior Associate Dean of Clinical Education to assure that students are provided all resources needed for clinical rotations and Match support. Additional lead faculty are identified within each area of focus to assure a cohesive and comprehensive experience within the respective academic teaching teams. Scholarly projects were supervised through the Office of Research. On average, ∼2–4 h of faculty time per week is spent mentoring and training in interpersonal and interview skills. The financial impact of the program is absorbed by the university, as support for the students is considered paramount.
Interestingly, leadership learned through conversations with participants that faculty time investment was also the most impactful in terms of student success. Students reported that the personal interaction and attention they received helped them to feel less shame and anxiety, and the structure of the one-on-one time with faculty course directors allowed them space and time to reflect and grow personally as well as develop a deeper sense of professional identity. Evidence of this was seen as faculty compared residency interview preparation and personal interaction year to year.
Throughout the PDI year, faculty monitor student engagement and motivation through cultivating relationships with the students. In the first year of implementation, faculty discovered significant levels of shame involved in being unplaced. As a result, implementation of leadership training, combined with an intensive focus on addressing and reframing shame, was identified to be critical to students’ professional and personal growth. A series of leadership focused training based on Brene Brown's book,
In addition to student feedback, community feedback was sought through informal conversations with clinical faculty preceptors and residency program leadership. RVUCOM preceptors and residency program directors were asked to share the most important applicant qualities or challenges they were experiencing that would impact a student's ability to match. Interestingly, both groups reported that performance in core predoctoral curriculum and board performance, while important, would be considered secondarily in an applicant with issues in either professionalism or interpersonal skills. This information was taken into consideration as faculty were building a PDI curriculum centered around soft skills.
As noted above, traditional outcomes for unplaced applicants in subsequent rounds of the NRMP match rarely exceed 50% and decrease with each additional attempt. RVUCOM PDI and MPDI participants from the Class of 2021 experienced a 100% placement, a trend that has continued in each iteration of the program since.
A common assumption among medical educators is that applicants unsuccessful in their first attempt in the Match will not be able to place into more competitive specialties in subsequent attempts. Evaluation of the RVUCOM PDI/MPDI program data reveals otherwise. Evaluation of 5 years of placement data shows that nearly 50% of ∼150 annual RVUCOM graduates match into highly competitive specialties such as Dermatology, Orthopedics, Radiology, Anesthesia, and Obstetrician/Gynecology 5 (see Figure 4). RVUCOM PDI/MPDI participants placement has mirrored the RVUCOM graduate trends in all 3 years of implementation, with ∼50% matching into similar highly competitive specialties (see Figure 5).

Rocky Vista University College of Osteopathic Medicine (RVUCOM) Class of 2021 residency placement outcomes.

Inaugural RVUCOM PDI and MPDI participant residency placement outcomes.
Conclusion
Navigating challenging circumstances, confronting them directly, and devising creative solutions can present hurdles to success for institutions. In light of the considerable challenges faced by both students and the school during the Match process, the leadership at RVU and RVUCOM opted to embrace the institutional values, thereby reaffirming a reputation for excellence, compassion, innovation, and collegiality. Although placement rates have returned to near pre-COVID-19 pandemic levels, RVUCOM has chosen to maintain this program. Through this ongoing approach, valuable insight was gained while fortifying both internal and external relationships.
Perhaps the most impactful lesson learned is the importance of transparency in communication. Being clear with intentions, grounded in our values, our stakeholders, including students, preceptors, and program directors shared that they were better able to connect with the programs developed, and that they felt more trusting that RVUCOM cares for our internal and external communities. In course evaluations, students reported a sense of support and less anxiety throughout the program and felt as though RVU as an institution truly cared for their well-being and future. Many of the students who have graduated from the PDI/MPDI have processed this experience in such a way that the shame and embarrassment they felt at the beginning of the process, which initially made them reluctant to let anyone know, has been transformed into a willingness to reach out to future unplaced students to reassure and mentor them. Involving our network preceptors and residency program directors in the process provided them with a greater sense of confidence that the students engaged in the program received a genuine curriculum aimed at enhancing their skills as residents, thus making them more competitive candidates and effective physicians.
Another crucial aspect of this program, which significantly affected stakeholders, is its tuition-free availability. A large percentage of medical students graduate with some level of financial debt. RVUCOM leadership deemed it compassionate to refrain from adding to that debt load at a time when students are highly vulnerable, both personally and in their professional journey. This decision showed both students and external stakeholders that RVU chooses to operate in integrity with our institutional values, strengthening our reputation and our relationships.
Footnotes
Acknowledgments
The authors would like to acknowledge the support of the RVU Board of Trustees, Rocky Vista University leadership, and RVU College of Osteopathic Medicine faculty for supporting this endeavor and ensuring RVUCOM student success.
Author Contributions
Each author participated in the development of the PDI and contributed to the writing of this perspective report.
DECLARATION OF CONFLICTING INTERESTS
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Authors report no conflict of interest. Some elements of the program described in this perspective report have been included as part of a toolkit for unplaced medical students available to member organizations through the American Association of Colleges of Osteopathic Medicine (AACOM). It has also been presented in part at the AACOM Educating Leaders 2023 Conference in Baltimore, MD.
FUNDING
The authors received no financial support for the research, authorship, and/or publication of this article.
