Abstract
Purpose
This study assessed the association between holding an additional graduate degree beyond a Doctor of Medicine (MD) or Doctor of Osteopathic Medicine (DO) and residency match outcomes. Specifically, the authors examined graduate degree attainment trends among residency applicants and evaluated whether graduate degree holders experience lower match rates than non-holders.
Methods
A retrospective, observational analysis was conducted using publicly available data from the National Resident Matching Program's Charting Outcomes in the Match reports (2016-2024). The 10 specialties with the highest applicant volumes were analyzed, encompassing 80 136 matched and 6820 unmatched U.S. MD and DO senior applicants. Trends in graduate degree attainment were evaluated using linear regression models. Match rates were stratified by graduate degree status and compared using two-proportion z-tests based on aggregated matched and unmatched counts for each specialty and overall.
Results
From 2016 to 2024, the proportion of graduate degree holders entering the match increased significantly for MD (15.77% to 18.29%, P = .0008) and DO (19.93% to 23.31%, P = .0151) applicants. Across all 10 specialties, graduate degree holders matched at lower rates than non-holders. Among MD applicants, graduate degree holders matched at 92.57% compared with 94.12% for non-graduates (P < .0001), with specialty-specific differences ranging from 0.22% in Psychiatry to 4.61% in Anesthesiology; five specialties demonstrated statistically significant disparities. Among DO applicants, graduate degree holders matched at 84.54% compared with 88.64% for non-graduates (P < .0001), with specialty-specific differences ranging from 1.44% in Family Medicine to 10.48% in Obstetrics and Gynecology; five specialties also reached statistical significance.
Conclusions
The proportion of graduate degree holders in the residency match is increasing, and these applicants experience lower match rates than non-holders. These findings challenge the assumption that additional graduate education provides a competitive advantage and underscore the need for further research into the applicant-level factors contributing to these disparities.
Keywords
Introduction
Medical students increasingly seek additional graduate degrees alongside their Doctor of Medicine (MD) or Doctor of Osteopathic Medicine (DO) to enhance their preparedness for residency applications. Although many perceive these degrees as beneficial, their impact on match outcomes remains uncertain. The National Resident Matching Program (NRMP), colloquially known as The Match, facilitates the placement of allopathic and osteopathic medical students into postgraduate training programs. Residency positions are competitive, and securing a match in a desired specialty can be career-defining. The recent shift of the United States Medical Licensing Exam (USMLE) Step 1 to pass/fail scoring has increased emphasis on other selection criteria, including Step 2 scores, academic performance, clinical evaluations, and research activity. 1 While some educators and program directors anticipate potential benefits for DO and underrepresented-in-medicine applicants, the long-term impact of this change on residency selection remains unclear. Consequently, NRMP data shows an increase in the mean number of research experiences among the Step 1 pass/fail cohort.2,3
With Step 1 no longer being numerically scored, residency selection committees place greater emphasis on other factors. Prior studies have shown that key application metrics, such as the proportion of applicants with non-doctoral graduate degrees, number of ranked programs, and research experiences, have steadily increased from 2007 to 2020. 2 Despite these trends, MD match rates have remained stable between 92% and 95% since 1982, according to the American Medical Association. 4 This phenomenon, often called an admissions arms race, reflects rising expectations for applicants even as match rates remain constant.
To gain an edge in this competitive environment, medical schools increasingly offer multidisciplinary graduate programs, such as master's degrees, which, along with graduate degrees earned before or independently of medical training, are perceived by many to provide a competitive advantage in The Match. Enrollment trends reflect this: between 2010 and 2018, MD/ Master of Public Health (MPH) enrollment rose 434%. 5 Medical schools may be incentivized to encourage students to pursue ancillary graduate degrees, as these programs generate additional revenue. However, prior data from the Texas Seeking Transparency in Application to Residency database shows limited or no advantage for graduate degree holders in matching. 6
In this study, we provide the first national, data-driven analysis of match outcomes for applicants with additional graduate degrees, utilizing NRMP's Charting Outcomes in the Match data from 2016 to 2024 for the 10 most applied-to specialties. Specifically, we tested the following hypotheses:
Hypothesis: The proportion of residency applicants with graduate degrees is increasing, and these applicants have a statistically significantly lower match rate than non-holders. Null Hypothesis: The proportion of residency applicants with graduate degrees is not increasing, and there is no statistically significant difference in match rates between graduate degree holders and non-holders.
To address this literature gap, we conducted this analysis of match outcomes for applicants with additional graduate degrees using NRMP Charting Outcomes in the Match data from 2016 to 2024. Our study examines trends in graduate degree attainment and assesses whether these degrees are associated with differential match success among U.S. medical school seniors (MDs and DOs). Understanding these trends is crucial for medical students considering additional education and residency programs, as well as for evaluating applicants with graduate degrees.
Methods
Study Design
We conducted a retrospective, observational study using publicly available U.S. NRMP Charting Outcomes in the Match data from 2016, 2018, 2020, 2022, and 2024, representing U.S. MD and DO applicants and released on a biennial schedule during this interval. We analyzed MD and DO data separately to account for differences in training pathways and match outcomes. Our analysis focused on the 10 specialties with the highest applicant volume: Anesthesiology (Anes), Diagnostic Radiology (DR), Emergency Medicine (EM), Family Medicine (FM), General Surgery (GS), Internal Medicine (IM), Neurology (Neuro), Obstetrics and Gynecology (OBGYN), Pediatrics (Peds), and Psychiatry (Psych). We selected these specialties to ensure robust datasets, as smaller fields often lacked complete data. Our study aggregates data from 10 specialties, so overall results may differ from those of broader NRMP reports. We analyzed deidentified, publicly available data, so our study is exempt from Institutional Review Board approval. The NRMP approved the use of the data and reviewed this analysis.
Study Setting and Population
We obtained study data from NRMP Charting Outcomes reports, which include self-reported information from U.S. allopathic and osteopathic applicants via the NRMP Applicant Registration Form. Applicants provided consent for the use of their academic and demographic information, ensuring compliance with ethical research standards. Our study population comprises 58 962 matched and 3864 unmatched MD applicants and 21 174 matched and 2956 unmatched DO applicants, totaling 80 136 matched and 6820 unmatched applicants across the 10 analyzed specialties, for a combined total of 86 956 applicants. This study focuses exclusively on U.S. MD and DO seniors, as defined by the NRMP
Study Protocol
We identified the number of matched and unmatched applicants with and without graduate degrees for each year and specialty through direct data extraction. Our primary outcomes were (1) trends in the proportion of graduate degree holders entering the match and (2) match rates by graduate degree status. Specialty-specific values were calculated directly from the raw yearly counts. Overall match rates were calculated by summing matched and unmatched applicants with and without graduate degrees across all 10 specialties. We sourced the dataset from finalized NRMP reports, which required no additional preprocessing, as all data was pre-verified. Because the dataset is observational and aggregated, all analyses are descriptive and comparative in nature and are not intended to infer causality.
Measurements and key Outcome Measures
We defined the key study variables as match status (matched vs unmatched) and graduate degree status (graduate degree holder vs non-graduate). For each specialty and for MD and DO applicants, we calculated yearly trends in the proportion of applicants holding graduate degrees. We calculated specialty-specific match rates for graduate and non-graduate degree holders using the aggregated matched and unmatched counts. These metrics were used to assess differences in match outcomes between graduate and non-graduate applicants.
Data Analysis
Proportion of Graduate Degree Holders Over Time
We analyzed trends in the proportion of graduate degree holders for MD and DO applicants between 2016 and 2024. For each specialty, we calculated the percentage of applicants with graduate degrees using the combined raw counts of matched and unmatched applicants reported in each Charting Outcomes year. We also calculated overall yearly proportions for MD and DO applicants by summing the total number of graduate degree and non-graduate degree applicants across all 10 specialties for each year.
The independent variable was the year, and the dependent variable was the proportion of applicants with graduate degrees. Linear regression was performed for each specialty and for the overall MD and DO applicant pools to assess temporal trends. Statistical significance was evaluated using P-values, and R2 values were used to describe the strength of the linear fit.
Match Rates for Graduate Versus Non-Graduate Degree Holders
We analyzed match rates separately for MD and DO applicants by specialty and in aggregate between 2016 and 2024. Overall match rates were calculated by summing matched and unmatched applicants with and without graduate degrees across all 10 specialties. To assess whether match rates differed between graduate degree holders and non-holders, we compared proportions using two-proportion z-tests based on aggregated matched and unmatched counts. All analyses were performed independently for MD and DO applicants.
Statistical Approach
We summarized applicant characteristics and residency match outcomes using descriptive statistics. Then, we analyzed yearly trends in graduate degree holders using linear regression, assessing statistical significance and model fit with P-values and R-squared values. To compare match rates between graduate and non-graduate applicants, we used two-proportion z-tests based on aggregated matched and unmatched counts for each specialty and for overall MD and DO cohorts. We aggregated data across specialties by summing matched and unmatched counts, without applying weighting, to ensure accurate representation of the full applicant pool. This approach was selected because aggregation increases analytic stability, reduces noise inherent in smaller specialties, and reflects applicant-level totals more accurately than analyzing each specialty independently. We applied a significance threshold of P < .05 to all analyses. Data were organized and tabulated using Microsoft Excel (Microsoft Corporation, Redmond, Washington). All statistical analyses were performed using RStudio 2023.06.1 + 524 (Posit, PBC, Boston, Massachusetts), performing computations with base R functions and regression and hypothesis testing packages.
Results
Proportion of Graduate Degree Holders Entering the Residency Match
Overall Trends in Graduate Degree Holders
We found that between 2016 and 2024, the percentage of graduate degree holders entering the residency match increased significantly for both MD and DO senior applicants, highlighting a growing trend in graduate degree attainment among U.S. medical students. Figure 1 illustrates these trends, highlighting the steady rise in graduate degree holders. Among MD applicants, the proportion of graduate degree holders increased at an average rate of +0.317 percentage points per year (P = .0008, R2 = 0.9853), rising from 15.77% in 2016 to 18.29% in 2024. For DO applicants, the proportion increased at a higher average rate of +0.462 percentage points per year (P = .0151, R2 = 0.8941), rising from 19.93% in 2016 to 23.31% in 2024.
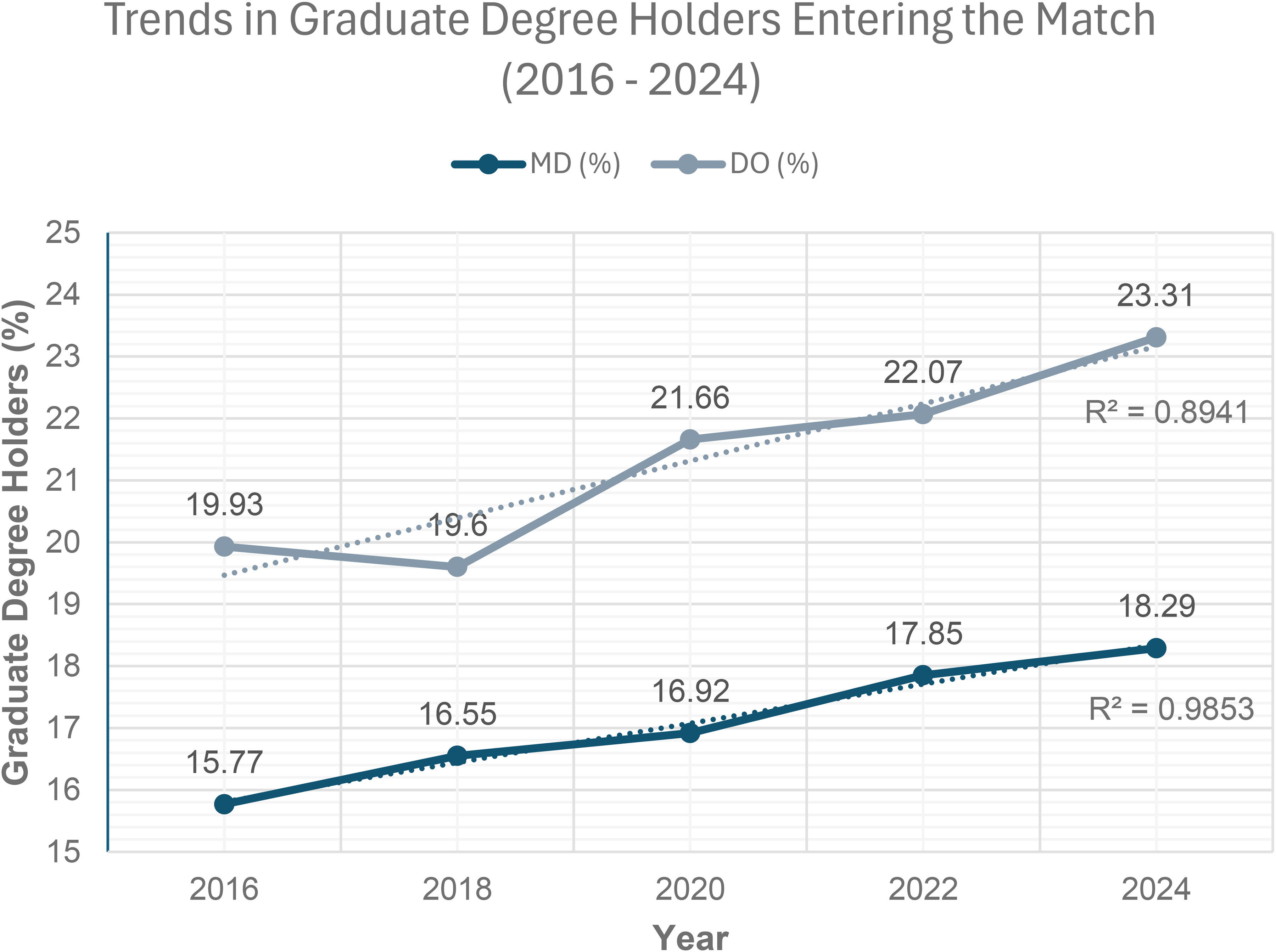
Trends in the percentage of allopathic (MD) and osteopathic (DO) residency applicants with graduate degrees entering the National Resident Matching Program, 2016-2024. The graph illustrates the increasing proportion of graduate degree holders among MD and DO candidates over time, with separate trend lines and R2 values for each group.
Specialty-by-Specialty Trends in Graduate Degree Holders
Specialty-by-specialty trends in graduate degree holders are presented in Table 1. Across the 10 specialties analyzed, most demonstrated descriptive increases in the proportion of applicants with graduate degrees between 2016 and 2024. Family Medicine among MD applicants and Pediatrics among DO applicants were the only specialties showing a descriptive decline over this period.
Trends in the Percentage of U.S. MD and DO Residency Applicants with Graduate Degrees by Specialty, 2 016-2024 (NRMP Charting Outcomes in the Match).

Abbreviations: ANES, anesthesiology; DR, diagnostic radiology; EM, emergency medicine; FM, family medicine; GS, general surgery; IM, internal medicine; NEUR, neurology; OBGYN, obstetrics and gynecology; PEDS, pediatrics; PSY, psychiatry; NRMP, National Resident Matching Program.
For MD applicants, R2 values ranged widely across specialties (0.03-0.96), reflecting substantial variability in linearity. However, this broad range was driven largely by Neurology (R2 = 0.0278); excluding this outlier, the remaining specialties demonstrated a much tighter spread (R2 = 0.40-0.96), indicating generally consistent upward trends over time. Only IM, OBGYN, and Peds showed statistically significant linear increases (P < .05), while the other specialties demonstrated modest, non-significant upward changes. The largest descriptive increase occurred in OBGYN, which rose from 15.02% in 2016 to 21.32% in 2024 (P = .0196). FM was the only MD specialty to show a descriptive decline, decreasing from 17.52% in 2016 to 16.24% in 2024; however, this trend was not statistically significant (P = .2557, R2 = 0.3956).
For DO applicants, R2 values also varied substantially across specialties (0.01-0.88), indicating heterogeneous linearity over time. Only EM and Psych demonstrated statistically significant linear increases (P < .05), while most other specialties showed modest, non-significant upward trends. EM experienced the largest increase, rising from 17.42% in 2016 to 25.43% in 2024. Peds was the only specialty to show a descriptive decline, decreasing from 21.28% in 2016 to 19.69% in 2024; however, this change was not statistically significant (P = .3430, R2 = 0.2962).
When viewed alongside the aggregate trends in Figure 1, the specialty-level findings demonstrate that the overall increase in graduate degree prevalence among MD and DO applicants is not uniformly reflected across all specialties. While the aggregate data support the first part of our hypothesis, showing a significant rise in graduate degree holders over time, the specialty-specific results reveal considerable variability in linearity, magnitude of change, and statistical significance. Some specialties show clear upward patterns, while others display flat or fluctuating trajectories, indicating that the overall increase in graduate degree attainment is driven by contributions from multiple specialties rather than a consistent rise across all fields. Taken together, these findings support the first component of our hypothesis, demonstrating a statistically significant increase in the proportion of graduate degree holders entering the residency match over time.
Match Rates by Graduate Degree Status
Overall Match Rate Comparison
Graduate degree holders exhibit statistically significantly lower match rates than non-graduate applicants for both MD and DO candidates. In all analyses, odds ratios (ORs) reflect the relative odds of
Specialty-Specific Match Rate Comparison
MD applicants with graduate degrees demonstrated lower match rates across all 10 specialties than their non-graduate counterparts. The absolute differences in match rates ranged from 0.22% in Psych to 4.61% in Anes, and in every specialty, the graduate degree group matched at a lower rate. However, only five specialties showed statistically significant differences: Anes, EM, FM, IM, and Peds (all P < .05). The most pronounced difference occurred in Anes, where graduate degree holders matched at 87.78% versus 92.39% for non-graduates (P < .0001; OR for not matching = 1.69). EM, FM, IM, and Peds also demonstrated statistically significantly lower match rates among graduate degree holders, though with smaller absolute differences; in these specialties, the ORs for not matching ranged from 1.30 in EM to 1.71 in Peds. In contrast, DR, GS, Neuro, OBGYN, and Psych exhibited descriptively lower match rates among graduate degree applicants, but these differences did not reach statistical significance.
DO applicants with graduate degrees demonstrated lower match rates across all 10 specialties than their non-graduate counterparts. The absolute differences in match rates ranged from 1.44% in FM to 10.48% in OBGYN, and in every specialty, the graduate degree group matched at a lower rate. Five specialties showed statistically significant differences: DR, EM, IM, OBGYN, and Peds (all P < .05). The most pronounced difference occurred in OBGYN, where graduate degree holders matched at 60.67% versus 71.15% for non-graduates (P = .0004; OR for not matching = 1.60). DR, EM, IM, and Peds also demonstrated statistically significantly lower match rates among graduate degree holders, though with smaller absolute differences; in these specialties, the ORs for not matching ranged from 1.37 in EM to 1.66 in Peds. In contrast, Anes, FM, GS, Neuro, and Psych exhibited descriptively lower match rates among graduate degree applicants, but these differences did not reach statistical significance.
Across all 10 specialties, the specialty-specific results presented in Table 2 show applicants with graduate degrees, both MD and DO, match at lower rates than their non-graduate counterparts. However, the magnitude and statistical significance of these differences vary greatly by specialty. Among MD applicants, statistically significant differences were observed in five specialties (Anes, EM, FM, IM, and Peds), while the remaining specialties exhibited smaller, non-significant gaps. Among DO applicants, five specialties likewise demonstrated statistically significant differences (DR, EM, IM, OBGYN, and Peds). The magnitude of these disparities was generally larger in the DO cohort than the MD cohort, particularly in OBGYN and DR. Overall, these results suggest that the disadvantage associated with holding a graduate degree is more pronounced among DO applicants, both in terms of effect size and statistical significance. While the specialty-level findings do not indicate a uniform effect across all fields, the overall pattern supports the conclusion that graduate degree holders experience comparatively lower match success, with the degree of disadvantage varying by specialty and applicant type.
Residency Match Rates of U.S. MD and DO Candidates With and Without Additional Graduate Degrees by Specialty, 2016–2024 (NRMP Charting Outcomes in the Match)
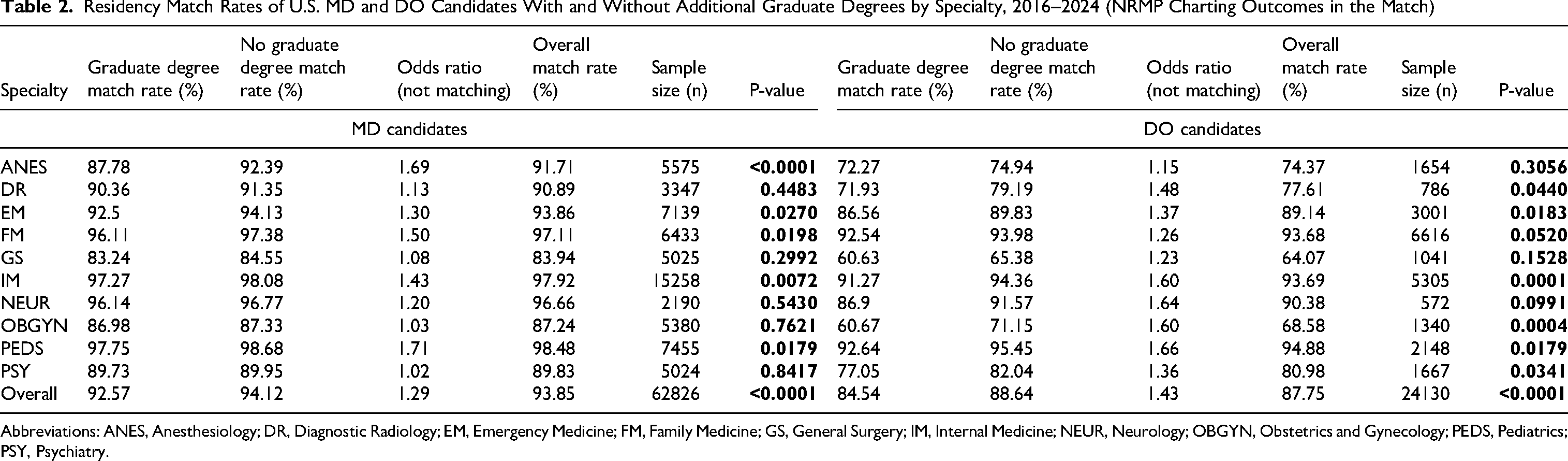
Abbreviations: ANES, Anesthesiology; DR, Diagnostic Radiology; EM, Emergency Medicine; FM, Family Medicine; GS, General Surgery; IM, Internal Medicine; NEUR, Neurology; OBGYN, Obstetrics and Gynecology; PEDS, Pediatrics; PSY, Psychiatry.
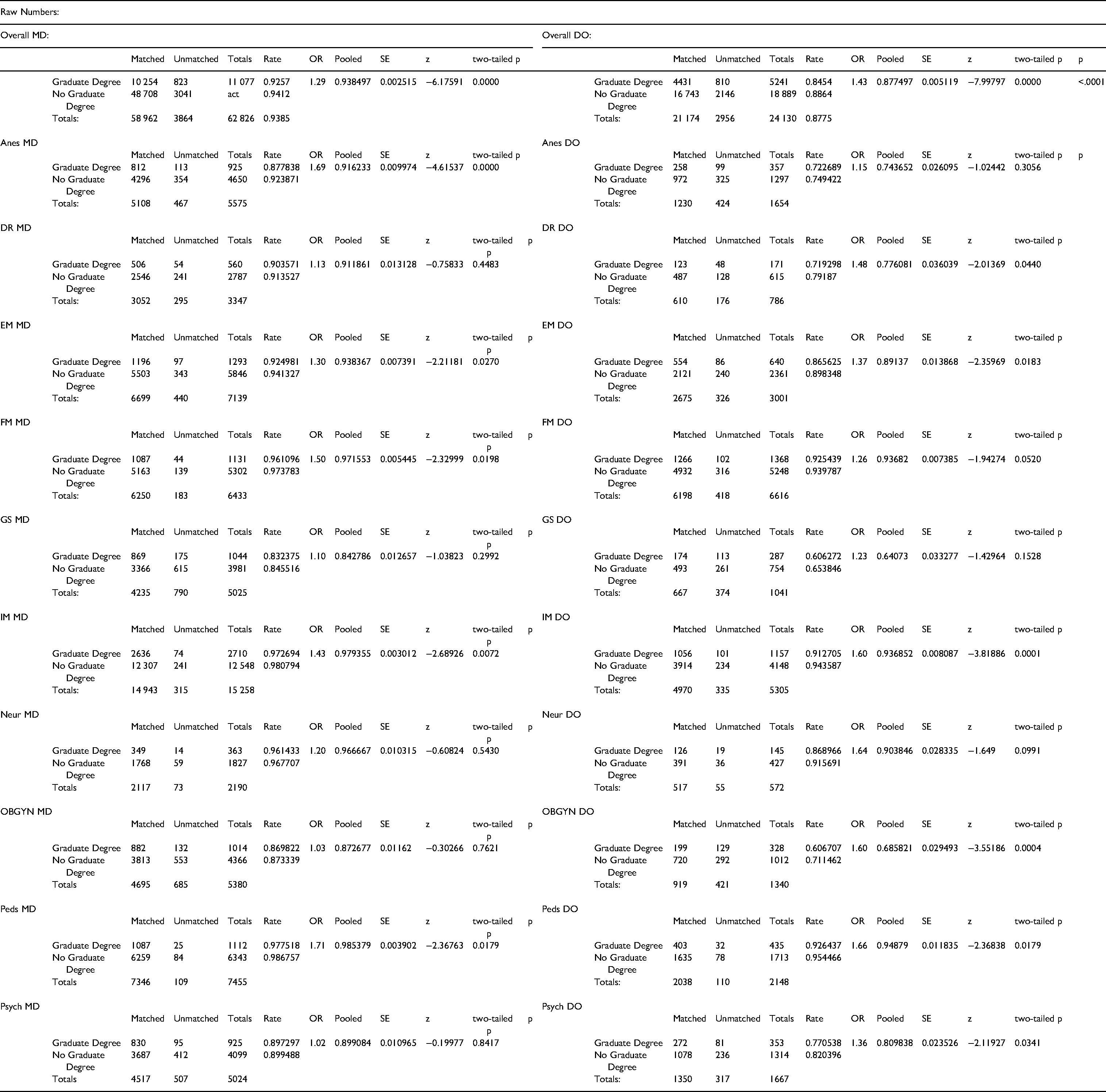
When taken together as aggregate data, these findings show that while graduate degree attainment has increased significantly over time among both MD and DO applicants, the effect of graduate degree status on match outcomes is more variable at the specialty level. Specialty-specific analyses demonstrate that graduate degree applicants consistently match at lower rates than their non-graduate peers, but the magnitude and statistical significance of these differences differ across specialties and between MD and DO cohorts. The aggregate match rate comparisons indicate a measurable, statistically significant overall disadvantage for graduate degree applicants, particularly among DO seniors. The specialty-specific results highlight heterogeneity in how this pattern manifests across individual fields. These results collectively demonstrate that the observed increase in graduate degree holders entering the match coincides with comparatively lower match success for this group. These findings confirm the second component of our hypothesis, showing that graduate degree holders consistently experience lower match rates than their non-graduate peers, with statistically significant disadvantages at both the aggregate and specialty levels. However, the strength of this relationship depends on applicant type and specialty context.
Discussion
Research productivity is highly valued in residency selection, with dedicated research years in medical school seen as strong predictors of academic output, particularly in competitive fields.7,8 Research experience and output have become even more emphasized by program directors following Step 1 of the USMLE transition to a pass/fail scoring format.9–13 Although graduate degrees are often viewed as markers of research competence, our analysis suggests that this perceived advantage may not translate into a competitive benefit in the residency match. The consistently lower match rates among graduate degree applicants indicate that whatever research value programs may attribute to these degrees is not outwardly reflected in improved match outcomes. Rather than indicating a direct disadvantage from holding a graduate degree, these findings may instead reflect underlying applicant-level characteristics that are not captured in the NRMP dataset. Despite this, the number of medical students pursuing graduate degrees continues to rise, a trend confirmed in our analysis and consistent with the first component of our hypothesis.
The reasons graduate degree holders have a lower match rate remain unclear and require further investigation. One key limitation of our study is the inability to differentiate between degree types, timing of attainment, and applicant motivations, introducing potential confounders. For instance, those earning graduate degrees before medical school may be non-traditional or career-changing applicants, facing distinct challenges in the match process. Older applicants may also encounter systemic biases, as studies suggest an inverse relationship between age and performance indicators such as MCAT scores, USMLE Step 2 scores, and clinical evaluations. 14 These factors may contribute to lower match rates among graduate degree holders, but further research is needed to clarify their impact.
Prior literature on specialized master's programs (SMPs) in biomedical sciences, often affiliated with medical schools, aim to improve applicant's academic performance, particularly USMLE scores, regardless of prior MCAT performance, thus “leveling the playing field.” 15 While SMPs have shown success in enhancing Step 1 outcomes, it remains unclear whether these benefits extend to mentorship, networking, research output, or residency match success. 15 Moreover, holding a graduate degree may not significantly strengthen other key application metrics, such as research productivity, clinical performance, or standardized exam scores, potentially blunting a perceived competitive edge from their degree.
In some cases, pursuing a graduate degree during medical school requires prolonged leaves of absence or deceleration from the core curriculum, which may disrupt longitudinal learning and contribute to weaker performance on USMLE exams, clerkships, or other academic milestones. Additionally, some institutions may encourage students to enroll in master's programs to provide additional time before high-stakes assessments, or to remediate academic gaps, meaning that graduate degrees can occur alongside pre-existing challenges unrelated to the degree itself. Graduate programs may also be pursued during periods of personal hardship or increased family or caregiving responsibilities. Taken together, these scenarios highlight that graduate degrees should not be viewed in isolation but understood within the broader context of an applicant's academic and personal trajectory.
Our analysis does not differentiate between graduate degree types, such as Doctor of Philosophy (PhD), Juris Doctor (JD), Master of Business Administration (MBA), or Master of Public Health (MPH), each of which may uniquely impact residency matching and shape career trajectories. Non-clinical degrees, such as an MBA, may lead residency program directors to question an applicant's commitment to clinical practice, potentially contributing to lower match rates as programs may favor candidates who align more closely with clinical practice. Additionally, individuals pursuing specialized dual-degree programs may forgo the residency match entirely, opting for post-doctoral research, law, or healthcare administration careers. These shifts indicate a more targeted professional focus compared to the broader goals of traditional medical graduates. 6 Further research is needed to understand how specific degrees influence match outcomes and applicant motivations.
Future analyses should examine key limitations, including graduate degree type and timing of attainment, and applicant characteristics such as age, undergraduate background, MCAT scores, USMLE performance, medical school academic metrics (including clerkship evaluations), and records of remediations, leaves of absence, professionalism concerns, or prior exam failures. Additionally, studies should assess whether research productivity and clinical evaluations influence match outcomes more than degree status alone. Elucidating these relationships would provide valuable insights for applicants considering graduate education and residency programs evaluating candidates. Further investigation into whether graduate degrees enhance scholarly output could clarify their role in residency selection and inform decision-making for medical students and residency programs.
Limitations
Our study has inherent limitations due to its retrospective observational design. Leveraging self-reported NRMP Charting Outcomes data introduces potential reporting variability and selection bias. The absence of detailed demographic and academic data limits control for confounding factors such as age, MCAT scores, grade point average, Step scores, and motivations for pursuing graduate degrees, including SMP participation, as well as important determinants of residency competitiveness such as clerkship grades, clinical evaluations, number of applications submitted, interview yield, and research productivity. Due to the publicly available, aggregated nature of the NRMP Charting Outcomes dataset, we were unable to access applicant-level data required to adjust for these variables. Additionally, we were unable to differentiate between types of graduate degrees (eg, MPH, MBA) or the timing of degree completion (before, during, or after medical school), which likely introduces substantial heterogeneity in the group of graduate degree holders. While regression analyses identify statistically significant associations, they do not establish causality or fully elucidate the interplay of confounding variables. Additionally, factors such as personal statements, letters of recommendation, and program-specific selection criteria may influence residency selection, but we did not analyze them in our study.
Despite these limitations, our findings offer meaningful insight into aggregate trends in graduate education and match outcomes. Although the diversity of the graduate degree holder population limits the ability to draw conclusions for individual applicants, the results suggest that additional degrees do not universally confer a competitive advantage. This raises important questions about how residency programs value graduate education and may reflect a disconnect between the incentives of medical school admissions (which often encourage dual-degree enrollment) and residency selection practices. Future studies should incorporate more granular academic and demographic data to identify competitiveness markers, clarify the impact of specific degree types and timing, and explore program-specific perceptions of graduate degree holders. Such research could inform medical education policies, better guide students considering dual-degree programs, and help align expectations across the medical training continuum.
Conclusion
Our analysis demonstrates that while the proportion of graduate degree holders entering the residency match has increased significantly from 2016 to 2024, these applicants consistently match at lower rates than their non-graduate counterparts. This pattern was evident in both MD and DO cohorts and across all 10 analyzed specialties, with statistically significant disadvantages observed in five specialties for each group. The magnitude of these differences was generally larger for DO applicants, suggesting a more pronounced disparity in this cohort. These findings collectively support both components of our hypothesis and challenge the assumption that additional graduate degrees confer a competitive advantage in the Match.
However, considerable heterogeneity across specialties and applicant types indicates that the effect of graduate degree status is not uniform and likely reflects applicant-level characteristics not captured in the NRMP dataset. Given these limitations, further research incorporating granular demographic, academic, and degree-specific data is needed to clarify the mechanisms underlying these disparities. Such work will be essential for informing medical students considering graduate education and for guiding residency programs as they evaluate applicants with additional degrees.
Footnotes
Acknowledgements
None.
Ethical Approval
Given the retrospective nature of this study and the use of publicly available, deidentified data from the NRMP, this study was deemed exempt by our institutional review board.
Author Contributions
Conceptualization, methodology, formal analysis, investigation, writing (draft), writing (review & editing), and visualization was done by all authors; data curation was done by DWB, HY, RSP; supervision was done by DER and BMB.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
Data were obtained from publicly available NRMP
Other Disclosures
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Disclaimers
None.
Previous Presentations
None.
