Abstract
Objectives
Human Papillomavirus (HPV) is a leading cause of cervical cancer, yet existing social stigmas and unequal access to healthcare compromise its preventability through screening and vaccination. Understanding healthcare professionals’ knowledge and perceptions of HPV is pivotal in enhancing the quality and effectiveness of preventive healthcare strategies. This article aims to explore and understand the relationship between healthcare workers’ knowledge and stigma towards HPV.
Design and Methods
A questionnaire of 27 stigma and 24 knowledge questions was provided for healthcare personnel. Demographic questions were also included. Stigma levels were determined based on a total median score. Fully adjusted multinomial logistic regression models were used to find the correlation between knowledge regarding HPV and the stigma level.
Results
Five hundred fifty-two healthcare workers answered the questionnaire. The findings showed that while most participants had adequate to moderate knowledge about the prevention and complications of HPV, they lacked knowledge about symptoms and treatment. Stigma towards HPV disease was evident in some participants, with attitudes varying depending on demographic factors and knowledge level. The model indicated that age, gender, and specific knowledge questions were significantly associated with stigma levels. Interestingly, the presence of knowledge in some areas increased the stigma level.
Conclusions
In conclusion, the study sheds light on the stigmatization and knowledge gaps regarding HPV disease among healthcare personnel and, intriguingly, that increased knowledge does not necessarily correlate with decreased stigma. The findings highlight the need for targeted education and training programs to improve healthcare providers’ knowledge in these specific areas.
Introduction
Background
Cervical cancer remains a significant health concern for women worldwide, with high-risk Human Papillomavirus (HPV) being a leading cause. Several viable prevention strategies exist for HPV, including screening and vaccination, which can prevent up to 80% of cervical cancer cases. The World Health Organization (WHO) has launched a global strategy to accelerate the elimination of cervical cancer. It recognizes HPV-based screening as the most effective strategy for reducing its incidence. 1 However, disparities in the availability of screening, treatment, and vaccination access make it challenging to eliminate cervical cancer.
Stigma and Its Impact on HPV Prevention
Effective implementation of HPV prevention methods depends on personal risk perception, knowledge, and societal acceptance, all affected by the stigma surrounding HPV and cervical cancer. 2 Stigma refers to negative attitudes or beliefs directed towards individuals or groups based on specific defining characteristics perceived as undesirable, dangerous, or incurable, resulting in discrimination and loss of social status. Health-related stigmas act as significant barriers that impede an individual's engagement in care, adherence to treatment, and propensity to seek help. Stigma undermines social relationships and resource availability, exacerbates stress, and affects psychological and behavioral responses, ultimately impeding health outcomes. As such, it is crucial to have a clear, multi-level theoretical framework to guide effective intervention development, measurement, research, and policy to reduce health-related stigma.3,4
Knowledge and Stigma Among Healthcare Providers
Although studies have investigated the stigmatization surrounding HPV and its vaccination in more vulnerable populations, 5 there is still a lack of research on the relationship between stigma levels and knowledge of HPV among healthcare providers. It is acknowledged that knowledge about a disease can significantly diminish the associated stigma. However, it cannot be assumed that healthcare providers possess low levels of stigma toward HPV, particularly as some studies have shown that greater knowledge of HPV does not always indicate vaccine acceptance.6,7
Information Seeking and Online Resources
The lack of reliable and current information about HPV has left many women feeling uninformed about the condition, leading them to seek more knowledge from the Internet through social media, blogs, and various websites provided by labs and private professionals. Despite the abundance of online information, finding trustworthy sources for women with HPV can be challenging, with official websites being the preferred source for most individuals seeking accurate information. However, regular internet users have reported finding valuable information that has aided their understanding of the condition. 8
Study Aims and Hypotheses
This study primarily hypothesizes that healthcare personnel have a significant degree of stigma toward patients with HPV. We also propose that an increase in healthcare professionals’ knowledge about HPV does not necessarily lead to a reduction in stigma; in fact, it might even exacerbate it. The study aims to examine the relationship between healthcare workers’ knowledge and stigma toward HPV and its implications for HPV prevention and patient care.
Material and Methods
Participants
The present study is a quantitative, cross-sectional, and observational study conducted in 2022. Our target population comprised healthcare personnel from a hospital in Birjand, South Khorasan, Iran. The inclusion criteria encompass healthcare personnel from faculties such as Nursery, Practical Nursery/Behyar, Medicine, Immunology, Biochemistry, Genetics, Environmental Health, Radiology, Midwifery, Surgical Technologist, Hematologist, Laboratory Science, Biotechnology, Biotechnology Education, Psychology, Molecular Medicine, Occupational Health, Public Health, Dentistry, and Other Ministry of Sciences. Participants who were unwilling and those lacking access to the online questionnaire were excluded.
We employed an online questionnaire as the primary instrument for data collection. Participants were directed to the study through a specific website address, which guided them to an online platform dedicated to hosting the survey. Upon their arrival at the site, they were first presented with comprehensive information regarding the anonymity and confidentiality measures implemented to safeguard their responses and personal information. Upon completion of the questionnaire, their responses were automatically recorded by the online platform.
Questionnaire Structure and Scoring
The questionnaire featured 27 questions centered on stigma and 24 on knowledge [Appendix A], with the knowledge-based questions requiring a simple yes or no response. These knowledge questions were organized into Transmission, Symptoms, Complications, Prevention, and Treatment categories. For knowledge-based questions, each response was scored as either 1 or 0, denoting correct and incorrect answers, respectively. The total count of correct answers was tallied within each knowledge domain to assess participants’ understanding of that knowledge domain.
The stigma-related questions were designed with a five-point scale for responses, systematically encoded as follows: “completely agree” (1), “agree” (2), “no idea” (3), “disagree” (4), and “completely disagree” (5). Participants rated each stigma question within this framework. The overall median score from the responses to the stigma questions was then calculated for each participant. Based on this median score, cases were systematically categorized into one of five sigma levels, numbered 1 to 5, to accurately reflect the intensity of perceived stigma. The higher the stigma level assigned to a case, the greater the healthcare stigma toward people with HPV, indicating a more significant degree of negative perceptions and attitudes toward those affected by the virus.
Demographic Questions
The questionnaire also included demographic questions, such as gender, age, marital status, type of occupation, faculty, and level of education.
Questionnaire Reliability and Validity
The questionnaire's knowledge and stigma sections underwent rigorous evaluation for validity and reliability. The research team developed the knowledge-related questions and consulted with five infectious disease specialists to ensure the validity of these queries. Notably, one of the consulted experts is also a co-author of this paper. Similarly, the Stigma questions were adapted from a previous study, 9 which also underwent evaluation for validity and reliability. A test-retest methodology was employed to evaluate the reliability of the questionnaire. This entailed administering the questionnaire to a cohort of 20 individuals, comprising students and staff who were not part of the final study sample. The interval between the initial test and the subsequent retest was established at one week, after which the correlation coefficients for scores across various domains were calculated and compared. The analysis revealed a Pearson correlation coefficient of 0.98 (p < .001) for the test-retest of the knowledge scores and a coefficient of 0.99 (p < .001) for the test-retest of the stigma level, thereby indicating a high degree of reliability of the survey instrument.
Sample Size Estimation
The sample size was calculated using the formula
Data Analysis
To assess knowledge, each question was scored as either 1 for a correct answer or 0 for an incorrect answer. The total knowledge score and scores in specific areas were reported and categorized. For measuring stigma, we calculated the median score of responses to stigma-related questions for each case, scaled from 1 to 5. This led to the creation of a new variable termed “stigma level.” We employed multinomial logistic regression models, as they account for the interdependencies between different questions within the model. This model was used to identify significant contributing factors to stigma levels. The 24 knowledge assessment questions were factors in the analysis, while the demographic variables were included as covariates. In our models, “stigma level 3” was designated as the reference outcome since it was the most common answer.
Similarly, a correct answer in the knowledge evaluation questions was the reference factor. For stigma levels below 3, factors displaying an odds ratio higher than 1.0 and an incorrect knowledge answer indicated a higher likelihood of belonging to lower stigma categories. Conversely, for stigma levels exceeding 3, factors with an odds ratio greater than 1.0 and an incorrect knowledge answer suggested a greater propensity for falling into higher stigma brackets.
Similar multinominal fully adjusted tests were conducted to assess each knowledge domain (median of grouped questions) ‘s relation to stigma levels. For this goal, we took the median value of the answers to each domain question. We tested it against the stigma level while adjusting using occupation, education, age, marriage, gender, and faculty.
To address the challenge of multiple testing arising from the 24 knowledge questions and various potential stigma levels, we adopted the Benjamini-Yekutieli (BY) procedure for controlling the False Discovery Rate (FDR). This decision was informed by the BY method's capacity to handle the dependency structure between test statistics, making it particularly suited to our study's complex dataset. The BY method adjusts the significance thresholds for multiple comparisons, aiming to control the proportion of false positives among the detected significant results. We set the FDR at 0.1, indicating a tolerance for up to 10% of substantial findings being false discoveries. The BY correction is applied by ordering the p-values and then computing the critical value (CV) for each test using the formula:
Ethical Considerations
The Birjand University of Medical Sciences ethics committee approved the study according to the ethical code of IR.BUMS.REC.1398.078. Although explicit written or verbal informed consent was not collected, the study employed an implied consent procedure. Participants’ voluntary completion of the online questionnaire constituted consent to participate, and they were free to withdraw at any point during the survey. This approach to obtaining consent was reviewed and approved by the university's institutional research ethics committee prior to data collection.
Results
Data collection of 552 healthcare personnel participants was conducted to evaluate HPV disease knowledge and to identify the knowledge questions that significantly contributed to the stigma level.
Demographical Findings
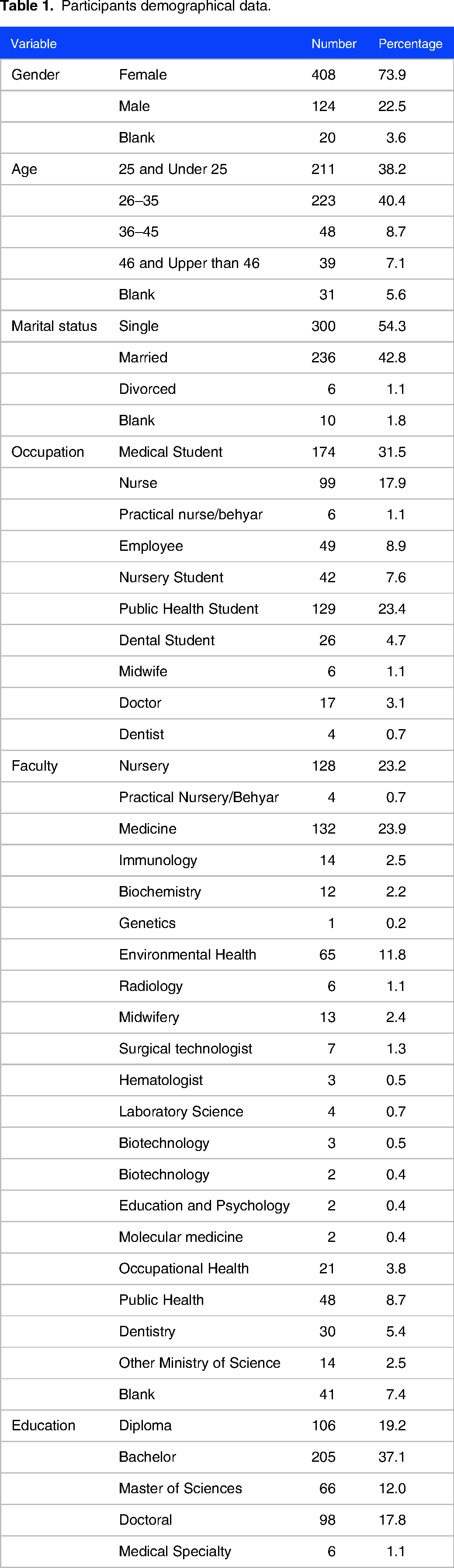
Table 1 presents the demographic data of 552 participants in the study; the data revealed that 73.9% of the respondents were female, while 22.5% were male, and 3.6% did not report their gender. Most participants were between 26–35 years old (40.4%), followed by those 25 years and below (38.2%). Regarding marital status, 54.3% were single, 42.8% were married, and 1.1% were divorced. Most respondents were medical students (31.5%) or public health students (23.4%), while nurses accounted for 17.9% of the participants. Regarding faculty, nursing (23.2%) and medicine (23.9%) were the most common areas. Furthermore, most participants had a bachelor's degree (37.1%), followed by doctoral degrees (17.8%), diplomas (19.2%), and master's degrees (12.0%). The data provide a diverse profile of participants concerning gender, age, occupation, education level, and specialty areas.
Participants demographical data.
Knowledge Evaluation Questions
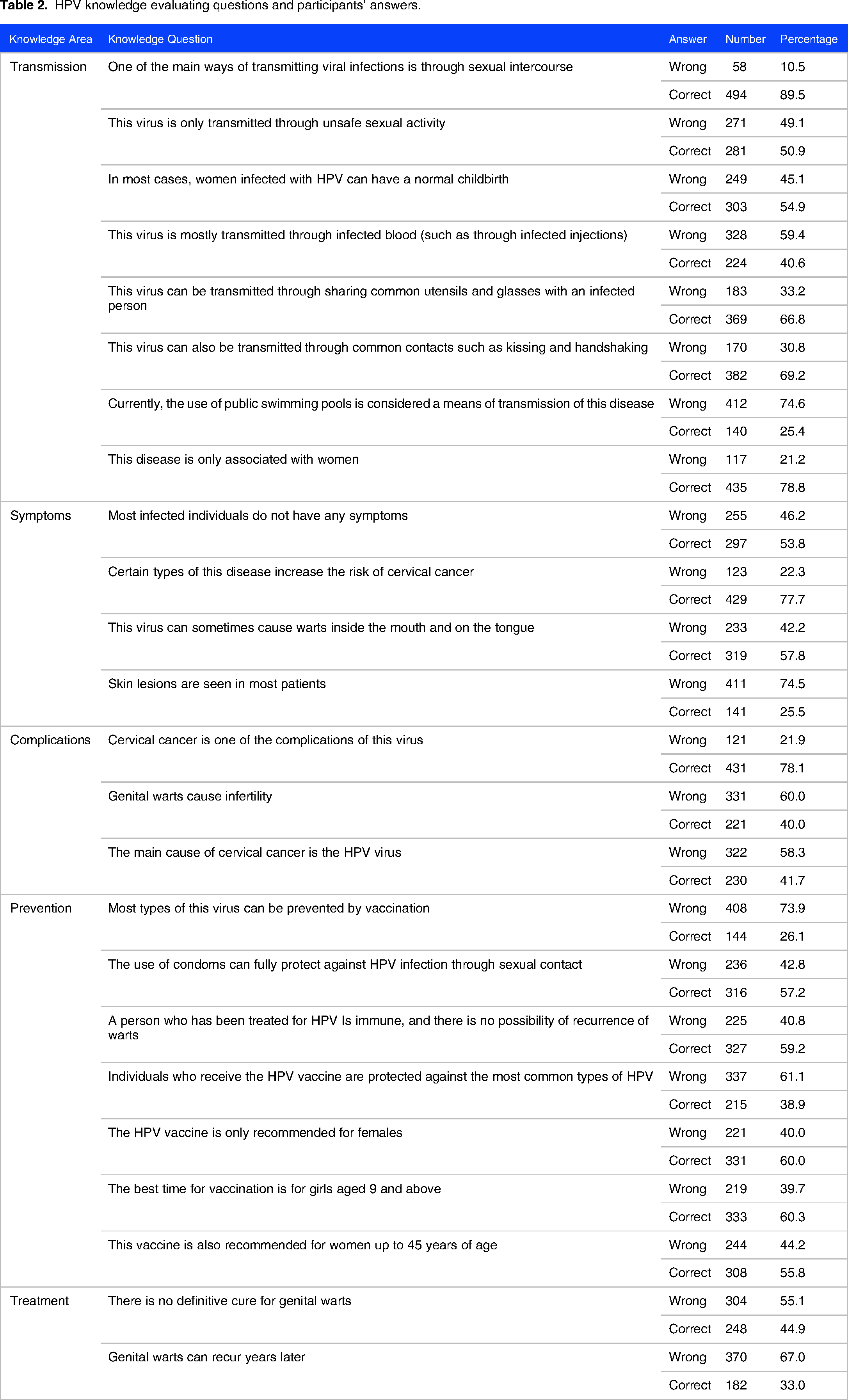
Table 2 summarizes participants’ knowledge regarding the transmission, symptoms, and prevention of the HPV virus through a questionnaire. Among the 552 participants, the majority (89.5%) correctly identified sexual intercourse as one of the main ways of transmitting the virus, and 74.5% were aware that skin lesions are seen in most patients. In contrast, only 26.1% knew that most types of the virus could be prevented by vaccination, and 77.7% correctly identified that certain types of the disease increase the risk of cervical cancer. Additionally, 67% of participants wrongly believed that genital warts could not recur later.
HPV knowledge evaluating questions and participants’ answers.
Analysis of healthcare personnel's knowledge of HPV disease in different knowledge areas reports that the mean total knowledge score was 12.8623 out of 24, with a standard deviation of relatively high at 5.18681 and a variance of 26.903, indicating relatively low to moderate knowledge. The knowledge in the treatment domain had the lowest score, with a mean score of 0.8333 out of 2. The knowledge of the Symptoms and the complications areas was also lacking, with mean scores of 2.1486 out of 4 and 1.5978 out of 3, respectively. The prevention knowledge score was relatively higher, with a mean of 3.5217 out of 7.
Stigma Evaluation Questions
Table 3 shows the responses to questions regarding stigma towards HPV disease. Participants were asked whether HPV is a punishment for bad behavior, and 63.8% disagreed with the statement. When asked if someone who contracts the disease through sexual intercourse or injection drug use has brought upon themselves what they deserved, 66.3% disagreed with the statement. Participants were also asked if those infected with HPV are immoral and reckless individuals, and 80.6% disagreed. Interestingly, 36.4% of participants had no idea whether people with HPV have many problems in their personal lives due to the disease. When asked if affected people should avoid kissing, shaking hands, and hugging, 61.9% disagreed. In comparison, 32.9% had no idea, and only A minority of participants (4.2%) believe that those infected with HPV are afraid of others finding out about their disease. However, some results indicate that stigma toward HPV infection exists among the healthcare population. For example, a significant portion of participants (36.1%) somewhat agree or completely agree that people with HPV blame themselves for their disease.
HPV stigma evaluation questions and participants’ answers.
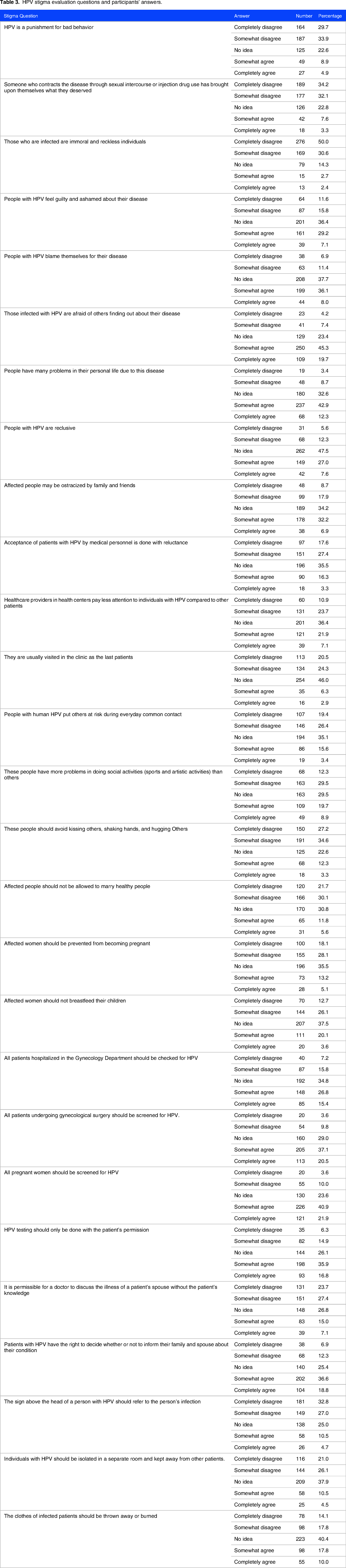
Additionally, a small percentage of participants (3.3%) believe that someone who contracts the disease through sexual intercourse or injection drug use has brought upon themselves what they deserve. A small percentage of participants (8.2%) believe that people with HPV are immoral and reckless individuals. Furthermore, some participants (19.4%) somewhat agree or completely agree that people with HPV put others at risk during common everyday contact. After analyzing the data from the stigma evolution survey, it was found that 27 participants fell into the category of stigma level 1. At the same time, 112 were categorized as stigma level 2, followed by 325 participants categorized as stigma level 3, 83 as stigma level 4, and a minority of only five individuals in stigma level 5.
Fully Adjusted Model
Individual Question Analysis
Our fully adjusted logistic regression model's overall fit was thoroughly assessed through model fitting information, goodness-of-fit statistics, and Pseudo R-squared values, alongside exploring alternative models. The significant improvement of the final model over the intercept-only model, as indicated by a chi-square value of 265.998 (df = 120, p < .000), and the goodness-of-fit statistics (Pearson chi-square and Deviance both showing p = 1.000) affirm a satisfactory model fit.
As shown in Table 4. the results of the fully adjusted model indicated that covariates such as age (p = .007, CV = 0.028, OR = 1.09) and, interestingly, the wrong response to “One of The Main Ways of Transmitting Viral Infections Is Through Sexual Intercourse (Question 1)” (p = .003, CV = 0.016, OR = 11.473) were significantly associated with stigma level 1 compared to stigma level 3. Other demographic variables and questionnaire item responses did not show significant associations.
Fully adjusted multinominal logistic regression model for stigma level based on the knowledge evaluation and demographical questions.

HPV: Human Papillomavirus; The questions are as follows: 1. one of the main ways of transmitting viral infections is through sexual intercourse 2. this virus is only transmitted through unsafe sexual activity 3. in most cases, women infected with the human papillomavirus (HPV) can have a normal childbirth. 4. this virus is mostly transmitted through infected blood (such as through infected injections). 5. this virus can be transmitted through sharing common utensils and glasses with an infected person. 6. this virus can also be transmitted through common contacts such as kissing and handshaking. 7. currently, the use of public swimming pools is considered a means of transmission of this disease. 8. this disease is only associated with women. 9. most infected individuals do not have any symptoms. 10. certain types of this disease increase the risk of cervical cancer. 11. this virus can sometimes cause warts inside the mouth and on the tongue. 12. skin lesions are seen in most patients. 13. cervical cancer is one of the complications of this virus. 14. genital warts cause infertility. 15. the main cause of cervical cancer is the HPV virus. 16. most types of this virus can be prevented by vaccination. 17. the use of condoms can fully protect against HPV infection through sexual contact. 18. a person who has been treated for HPV is immune, and there is no possibility of recurrence of warts. 19. individuals who receive the HPV vaccine are protected against the most common types of HPV. 20. the HPV vaccine is only recommended for females. 21. the best time for vaccination is for girls aged nine and above. 22. this vaccine is also recommended for women up to 45 years of age. 23. There is no definitive cure for genital warts. 24. genital warts can recur years later.
For stigma level 2, no covariates were statistically associated with being categorized as stigma level 2 compared to level 3. Unexpectedly, participants who reported a wrong answer to the question “This Virus Can Sometimes Cause Warts Inside the Mouth and On the Tongue (Question 11)” (p = .029, CV = 0.045, OR = 2.124) were more likely to be categorized as stigma level 2 compared to stigma level 3. Additionally, those who reported a wrong answer to the question “In Most Cases, Women Infected with The Human Papillomavirus (HPV) Can Have a Normal Childbirth (Question 3)” (p = .040, CV = 0.50, OR = 0.471) had lower chances of being categorized as stigma level 2 so correct answer to question 3 would more likely categorize the participant as stigma level 2 compared to level 3.
The model results analysis for stigma level 4 (compared to stigma level 3 as the reference) indicates that several demographic and question variables were significantly associated with stigma level 4. Specifically, covariates such as participants’ gender (p = .012, CV = 0.033, OR = 2.598) or not being married (p = .001, CV = 0.011, OR = 3.039) were more likely to report higher stigma levels; in contrast, a covariate education level (p = .045; CV = 0.056, OR = 0.713) was negatively associated with stigma level 4 compared to stigma level 3. Regarding the questions, participants who chose the wrong answer for “Currently, The Use of Public Swimming Pools Is Considered a Means of Transmission of This Disease (Question 7)” (p = .018; CV = 0.39, OR = 2.604) and “This Virus Can Be Transmitted Through Sharing Common Utensils and Glasses with An Infected Person (Question 5)” (p = .095; OR = 1.948) were more likely to be categorized as stigma level 4 compared to stigma level 3. In contrast and interestingly, those who correctly answered “The Best Time for Vaccination Is for Girls Aged 9 And above (Question 21)” (p < .001; CV = 0.005, OR = 0.233) were significantly more likely to be categorized as stigma level 4 compared to stigma level 3 meaning lack of knowledge in such areas reduce the stigma rather than increasing it.
Knowledge Domain (Grouped Question) Analysis
Knowledge domain (grouped question) adjusted multinominal logistic regression model for stigma level based on the knowledge domain (grouped question).

For stigma level 1 (compared to stigma level 3), only the age variable (B = 0.079, p = .003, CV = 0.037, OR = 1. 082) had a positive coefficient, suggesting that older individuals were more likely to experience lower stigma level 1 relative to average stigma level 3.
Several variables emerged as significant predictors of stigma level 2. The transmission knowledge domain (B = 1.165, p = .026, CV = 0.086, OR = 3.206) and the Treatment knowledge domain (B = 0.857, p = .036, CV = 0.099, OR = 2.355) had positive coefficients, indicating that higher levels of knowledge about transmission and treatment were associated with an increased likelihood of a lower stigma level.
For stigma level 4, multiple variables showed significant associations. Treatment knowledge domain (B = 0.953, p = .023, CV = 0.061, OR = 2. 594), Occupation (B = 0.125, p = .001, CV = 0.012, OR = 1. 134), Gender (B = 0.807, p = .016, CV = 0.049, OR = 2. 242), and Marriage (B = 1.057, p = .001, CV = 0.024, OR = 2. 877) had positive coefficients, indicating that higher levels of treatment knowledge, certain occupations, being male, and being married were associated with an increased likelihood of higher stigma level.
Discussion
Main Findings
Our main findings have revealed that educated healthcare workers experience a noticeable stigma, and a lack of knowledge regarding Human Papillomavirus (HPV) in certain areas is evident. Furthermore, our study identified that the presence of specific knowledge in certain areas of HPV disease could increase the level of stigma.
Our results indicate that the overall knowledge of healthcare personnel regarding HPV was at a low to moderate level, with notable gaps in understanding of treatment and symptoms. The participants scored the lowest in their knowledge of HPV treatment, and over 60% were unaware of the possibility of wart recurrence. However, in the multinomial models, treatment-related questions did not significantly impact the prediction of the stigma level. These findings underscore the necessity for educational initiatives to raise awareness about the HPV vaccine among healthcare professionals. By addressing these knowledge gaps, healthcare providers will be better equipped to educate and guide their patients in making informed decisions about HPV prevention and management. 11
Our second hypothesis was that expertise and in-depth knowledge do not necessarily equate to lower levels of stigma. 12 In fact, they may even contribute to an increase in the stigma level, as suggested by another study. After analyzing our model, we found that giving the wrong answer (due to lack of knowledge) to Question 1 (“One of the main ways of transmitting viral infections is through sexual intercourse”) and Question 11 (“This virus can sometimes cause warts inside the mouth and on the tongue”) can decrease stigma levels compared to level 3. Conversely, providing the correct answer (presence of knowledge) to Question 21 (“The best time for vaccination is for girls aged nine and above”) can significantly contribute to higher levels of stigma in comparison to level 3. Our two main findings suggest that the amount of expertise cannot solely indicate HPV knowledge or stigma, and considerable knowledge gaps and stigma exist, as demonstrated by us and other studies.13,14 Results suggest that accurately targeting knowledge gaps and providing education to healthcare personnel is crucial for reducing the level of stigma. It is essential to acknowledge that healthcare providers have a significant role in destigmatizing HPV. They can achieve this by accurately informing their patients about the virus, avoiding judgmental language, and regularly discussing sexual health to make it more normalized. 15
Our assessment using a stigma evaluation survey found that although stigma levels are generally moderate to low, there are still pockets of prejudicial attitudes toward individuals with HPV. These attitudes are evident in healthcare personnel who tend to agree, at least to some extent, with statements such as “individuals with HPV are responsible for their condition” or “those with HPV pose a risk to others in routine daily interactions.” Interestingly, the pockets of stigma observed align with broader research findings, indicating that stigmatizing attitudes exist within the general population. Prior studies have revealed that feelings of self-blame and shame can amplify the stigma associated with HPV. This suggests a new area of research interest that consists of exploring the possibility of high HPV prevalence among healthcare personnel.16,17 Furthermore, research shows that how a disease is publicly portrayed can significantly impact and even mitigate the level of associated stigma. This highlights the need for a more nuanced approach when discussing sexually transmitted diseases like HPV. This need for nuanced representation extends to the portrayal of mental illness in media, which plays a pivotal role in shaping public perceptions and either contributing to or alleviating stigma. When media outlets depict mental illness through negative, inaccurate, or violent lenses, such as in certain movies, it can foster increased prejudice toward individuals with mental health issues, underscoring the significant influence media representations have on public attitudes toward mental illness.18,19
The models showed that some demographical factors, such as gender and marriage, play essential roles in contributing to participants’ stigma levels. Studies have revealed that fear of being discovered by a partner and the risk of transmitting the disease through extramarital sexual conduct are key factors contributing to the social stigma surrounding HPV, 20 and reliable communication between partners is necessary for such instances regarding HPV diagnosis. 21 Some studies attributed the stigma specifically to the female gender with special needs. 22 Peterson, C. E. et al study found that Participants shared perceptions that members of their social networks blame women for their cervical cancer diagnosis and that there is a sense within their communities that HPV infection is viewed as shameful; the study also stated that men in the social circles of the participants were perceived to hold attitudes that created communication barriers or discomfort when discussing HPV and cervical cancer; therefore, gender play a crucial role in addressing patients attitudes towards HPV disease. 23 We could not obtain satisfactory results from our models concerning other demographic factors, such as occupation and faculty, possibly due to the too much diversity of the studied population.
Based on the model, the lack of understanding in some knowledge questions significantly contributed to higher stigma levels. We believe that such questions like “Currently, The Use of Public Swimming Pools Is Considered a Means of Transmission of This Disease (Question 7)” and “This Virus Can Be Transmitted Through Sharing Common Utensils and Glasses with An Infected Person (Question 5)” show gaps in areas of knowledge and awareness. These are misconceptions widely held by people. According to studies, healthcare providers are known as reliable and trustworthy sources of information, their recommendations are highly valued, and they can significantly influence the compliance of the central target populations towards vaccinating against HPV. 13 An essential factor in providing high-quality healthcare is ensuring that healthcare personnel receive accurate education. This education should be delivered using appropriate channels and effective options that cater to their learning needs. One of healthcare personnel's most successful learning options is online services and Lecture-based education. 24 These educational materials are designed to provide a comprehensive understanding of various healthcare topics. They are proven to be effective in increasing HPV knowledge scores, and these include the latest advancements in treatments, procedures, and medical technologies.25,26
One other aspect of knowledge questions that significantly contributed to stigma level was “In Most Cases, Women Infected with The Human Papillomavirus (HPV) Can Have a Normal Childbirth (Question 3)” based on our model participants who answered the question correctly were more likely to be categorized as lower stigma levels. This finding is specifically vital because based on another study regarding women's concerns about HPV infection and fertility mentioned that worrying about the adverse effects of pregnancy on their health was the main reason they decided not to get pregnant. In a mixed-method study conducted in the United States, 30 of 94 women who planned on getting pregnant indicated that their HPV test results would change their future pregnancy plans. 27
The results of the domain-based analysis exhibited similar patterns and significant factors. Interestingly, our hypothesis that specific knowledge questions can increase stigma levels, rather than the commonly held belief of lowering them, still holds true. The treatment knowledge question emerged as a significant factor contributing to both higher 4 and lower stigma levels 2 when compared to the average stigma level of 3. This finding underscores the importance of conducting studies with larger sample sizes and more robust power levels to accurately pinpoint the effect of similar knowledge domains on stigma levels.
Limitations
This study has several limitations that should be acknowledged, including relatively small sample size, particularly for participants falling into the highest level of stigma (level 5); the lack of questions regarding participants’ acceptance or previous reception of the HPV vaccine; limited diversity in terms of the healthcare personnel included; potential geographical constraints and specificity to certain types of healthcare facilities; and the inherent risk of self-reporting bias. A more extensive and more diverse sample, inclusion of questions about personal experiences with the HPV vaccine, consideration of geographical and facility-specific factors, and strategies to minimize self-reporting bias, such as using validated measurement tools and ensuring participant anonymity, could strengthen the reliability and generalizability of the findings in future research.
Conclusion
In conclusion, our study has identified that a noticeable stigma toward individuals with HPV exists among educated healthcare workers, and a lack of knowledge regarding HPV in certain areas is still prevalent. While the total knowledge score of healthcare personnel is, at best, moderate, the areas such as treatment and symptoms show a significant knowledge gap. The study interestingly found that knowledge in specific areas can increase the stigma level. Our findings highlight the need for proper education using appropriate and effective options catering to healthcare personnel's learning needs. Future research should focus on developing targeted educational interventions for healthcare personnel to address knowledge gaps and misconceptions about HPV, as well as exploring the nuanced effects such as knowledge increase on stigma levels and the impact of demographic factors like gender and marital status on these attitudes.
Supplemental Material
sj-docx-1-mde-10.1177_23821205241260596 - Supplemental material for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two
Supplemental material, sj-docx-1-mde-10.1177_23821205241260596 for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two by Arash Ziaee, Masood Ziaee, Arghavan Asghari, Samira Elhamirad and Ghodsiyeh Azarkar in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205241260596 - Supplemental material for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two
Supplemental material, sj-docx-2-mde-10.1177_23821205241260596 for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two by Arash Ziaee, Masood Ziaee, Arghavan Asghari, Samira Elhamirad and Ghodsiyeh Azarkar in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-3-mde-10.1177_23821205241260596 - Supplemental material for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two
Supplemental material, sj-docx-3-mde-10.1177_23821205241260596 for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two by Arash Ziaee, Masood Ziaee, Arghavan Asghari, Samira Elhamirad and Ghodsiyeh Azarkar in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-4-mde-10.1177_23821205241260596 - Supplemental material for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two
Supplemental material, sj-docx-4-mde-10.1177_23821205241260596 for Unpacking HPV Stigma: Assessing Healthcare Workers’ Knowledge and Stigma Towards HPV While Exploring the Connection Between the Two by Arash Ziaee, Masood Ziaee, Arghavan Asghari, Samira Elhamirad and Ghodsiyeh Azarkar in Journal of Medical Education and Curricular Development
Footnotes
Acknowledgements
We want to extend our gratitude to Prof. Mehdi Jabbari Nooghabi, whose guidance and insights have been instrumental in the development of this article's methodology and statistical analysis.
Authors Contributions
AS presented the study's main idea, AZ constructed the theory, evaluated needed data, developed article text, and contributed to the statistical analysis. MZ contributed to granting access to patient data and planning study procedures and study coherence; SE and AS contributed to data curation and manuscript drafting. GA contributed to conceptualization, supervision, and validation. All authors contributed to data evaluation and interpretation. The study's final approval and review procedure was done under the contribution of all authors. All authors read and approved the final manuscript.
Data Availability Statement
The data supporting this study's findings will be available upon request from the corresponding author. Requests for data access should be directed to Dr. Ghodsiyeh Azarkar at Gh.azarkar@yahoo.com.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
