Abstract
OBJECTIVES
High-quality research forms the basis of evidence-based practice and sets the foundation for trainees to develop critical thinking skills and approach clinical problems with an inquisitive mind. The attitudes to research however vary widely and there are significant barriers to conducting research relevant to each clinical discipline. Understanding both the attitudes of residents to research and the barriers to conducting research could allow for strategies to improve this core aspect of clinical development. This aim of this study was to characterise current attitudes and perceived barriers towards conducting research among residents in Obstetrics and Gynecology in Trinidad and Tobago.
METHODS
An online survey was sent to all residents in the four major public hospitals in Trinidad and Tobago. The 10-min previously piloted questionnaire contained questions related to demographics, career level, research experience, attitudes to research as well as perceived barriers to conducting research.
RESULTS
The response rate was 74% (48/65). Although most (77%) respondents were interested in performing research, lack of time (56%) and insufficient training in research (59%) were the main barriers. Lack of mentorship or supervision as well as departmental issues such as access to case notes, electronic databases and bureaucratic issues were also found to hamper a research-oriented environment.
CONCLUSION
For residents in Obstetrics and Gynecology, curricula revision is urgently required to include protected research time, training in research methodology, formal and dedicated research mentors in order to promote a research-oriented culture that ensures a greater understanding and output of research in this specialty.
Introduction
Advancement in any specialty is highly dependent on using high-quality evidence-based medicine which is facilitated by research. Exposure to research is essential for trainees and residents’ development of critical thinking and problem-solving in their approach to clinical scenarios.
The role of research in medical education remains an important topic as training programs continue to grow, evolve and undergo reform.1–3 Many postgraduate curricula mandate participation in scholarly research activity but this has not been a worldwide trend.4,5
In Trinidad and Tobago, a developing nation, many residents in obstetrics and gynecology are not equipped to effectively conduct research in this area and there is a paucity of clinical research generated from the trainees of this specialty. This is true for many other low-and middle-income countries.6,7
In our setting, once the undergraduate medical degree is awarded, there is a 12-month internship period during which there is exposure to the majority of specialties. This is usually followed by 1 to 2 years of clinical training in a major public hospitals in an area of their choosing before enrolling in a recognised postgraduate training program. All residents are encouraged to become involved in ongoing research projects and audits from the commencement of their specialty training. Although our postgraduate training program has a compulsory research requirement during years 3 to 5 of a 5-year program, this is usually viewed by residents as merely an obligatory exercise to fulfil but does not result in future participation in research or publication of work done.
In addition, there remains a lack of literature on residents’ opinions regarding research, its value, feasibility and barriers to conducting this in our setting. Therefore, it was our aim to characterise the current attitudes and perceived barriers towards research during the Obstetrics and Gynecology residency in Trinidad and Tobago.
Methods
A 30-item online-based survey (Google forms) was distributed to all residents in the Obstetrics and Gynecology Departments in the four major public hospitals in the country, Port-of-Spain General Hospital, San Fernando General Hospital and Mt Hope Women's Hospital and Scarborough General Hospital. The study period consisted of 8 weeks from January 3, 2022, to February 28, 2022.
Attitudes towards research and perceived research barriers were identified based on discussions and interviews with residents and university staff involved in research curricula, in addition to wide-ranging literature review. The survey was designed and edited by two university staff members involved in medical education and the current postgraduate curriculum for trainees in Obstetrics and Gynecology, and the questions were developed according to the protocol by Artino et al 8 A pilot study was completed by fifteen residents to assess response times, feasibility and question validity.
The final survey questions (30 items, 10-min response time) are shown in Supplementary Information 1 and contain an “in survey” consent mandate. The survey comprised 6 sections which were as follows: (a) demographic information, (b) previous research experience, (c) attitudes to research: nine data points using a 5-point Likert scale, (d) perceived research barriers: 10 data points using a score of 1 to 10, where 1 was the main barrier and 10 was the least barrier, (e) overcoming the barriers – free text and (f) additional comments – free text.
The study was approved by the Campus Research Ethics Committee of the University of the West Indies. Figure 1 shows the COREQ (COnsolidated criteria for REporting Qualitative research) flow diagram for screening, enrolment and questionnaire completion. Reminder emails were sent 2 and 4 weeks after the initial survey distribution. Responses were collected electronically for a period of 2 months. Saturation was reached at this time as we had an acceptable response rate with the same responses and themes.

COREQ (COnsolidated criteria for REporting Qualitative research) flow diagram for screening, enrolment and questionnaire completion.
Data analysis
Qualitative data was thematically analysed by two independent reviewers (SP and VH), blinded to each other's results to identify common themes in free-text responses, while quantitative data was analysed using Microsoft Excel.
Results
Residents from all 4 major public hospitals in Trinidad and Tobago responded to the questionnaire. The response rate was 74% (48/65). The respondents included trainees at all stages of Obstetrics and Gynecology training as determined by the postgraduate year. Demographic data and past research experience are shown in Table 1.
Demographic data and previous research experience of residents.
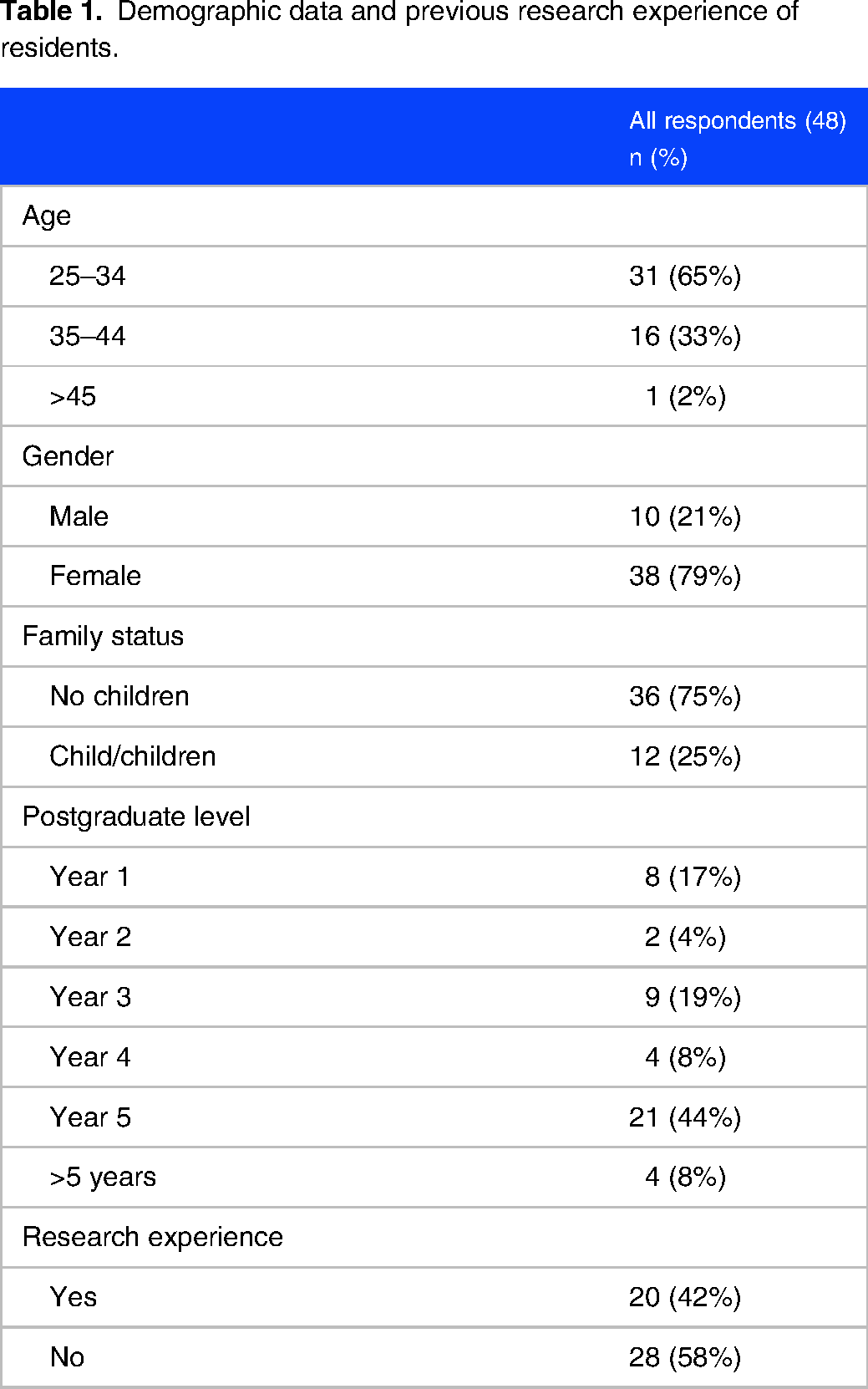
Although 21 out of 48 residents (44%) participated in some form of research in their training so far, only 12 (25%) had published in a peer-reviewed journal, with the majority reporting a single publication, and all of these respondents were year 3 to 5 residents who were fulfilling their mandatory research requirements.
Attitudes to research
Overall, the respondents had a positive attitude to performing research. Figure 2 shows the responses obtained from the survey on research attitudes using the 5-pont Likert scale for the 9 data points used.

Attitudes to research as reported by OBGYN residents in Trinidad and Tobago.
The majority of residents (77%) were interested in conducting some form of research and felt that research (66%) as well as training in research methodology (72%) should be a mandatory part of their program. Nevertheless, a large proportion of residents (68%) “strongly agreed” or “agreed” that undertaking research increased the burden on already overworked doctors, 33% and 35% respectively.
In addition, more than half of the residents, 56%, felt that they did not have enough time in their training to perform research while 91% felt that there should be protected time in the training program for undertaking research (56% – agreed and 35% – strongly agreed).
When considering help and support in conducting research, 40% both “disagreed” and “strongly disagreed” that they knew who to contact or speak to for help, while 37% were neutral (neither agreed nor disagreed).
Perceived barriers to research
Participants were asked to rank a list of 10 pre-specified barriers to conducting research, using a score of 1 to 10, where 1 is the main barrier and 10 is the least barrier. These results are shown in Table 2.
Ranking of perceived barriers to performing research.
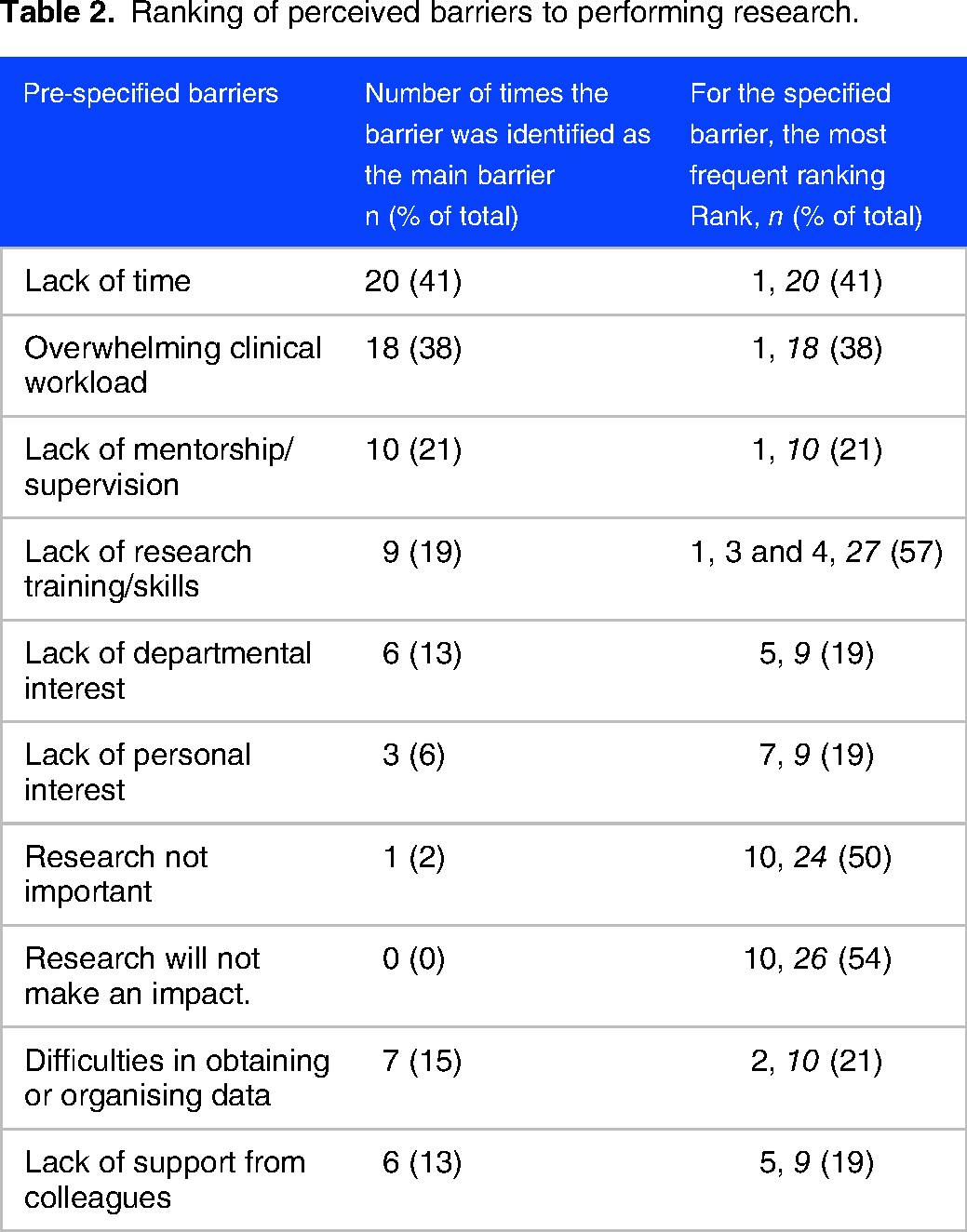
Lack of time was the main perceived barrier (n = 20, 41%), while an overwhelming clinical workload was ranked as the main barrier by 38% of residents. Lack of personal (6%) as well as departmental interest (13%) was less of a factor, although lack of mentorship and difficulties in obtaining data were seen as main barriers in 21% and 15% of residents, respectively. A minority of those who responded negatively viewed the importance or impact of research as a barrier.
Finally, regarding overcoming the barriers, 26 (54%) participants responded with free-text answers, and all agreed in the affirmative that barriers could be overcome. These free-text answers which included 42 suggestions to overcome these barriers were incorporated into four themes: time, education, supervision and departmental issues, as shown in Table 3.
Overcoming barriers – themes and subthemes.

Discussion
To our knowledge, this is the first study of its kind to characterise the current research attitudes and perceived barriers among residents in Obstetrics and Gynecology in a national setting of the four main public sector hospitals in Trinidad and Tobago. Despite the current research landscape including a mandatory requirement for those enrolled in postgraduate training, many do not continue conducting research once this requirement is fulfilled and do not go on to publish their findings in peer-reviewed journals. In addition, many trainees who are not enrolled in this program do not actively participate in research and are not always necessarily encouraged to do so.
The nature of this specialty as well as its unique and often high-risk patient population emphasises the need for research skills and the use of robust and up-to-date clinical evidence. It was therefore our aim to report on the attitudes and barriers that influence the ability to conduct research. Firstly, our response rate of 74% is reasonable and higher than many other similar studies, perhaps due to the use of reminders.9–11
The strongest identified factors preventing research were found to be time and training, seen in both the attitudes to research as well in perceived barriers, with 56% of trainees admitting to insufficient time to perform research and 59% stating that they have not had training in performing research and /or research methodology. In addition, those with publications were fulfilling mandatory requirements.
Time as a key barrier is consistent with other studies.11–13 Gill et al found that lack of time to be their most prevalent reported barrier (68%), although this was followed by lack of personal interest (31%) which was not a major factor in our study. Most suggestions for overcoming barriers therefore focused on dedicated research time, particularly in light of rigorous clinical commitments. In many specialties, including obstetrics and gynecology, 11 protected research time, as in the form of a rotation or additional training time has been shown to increase research productivity, also seen in anaesthesiology, 14 internal medicine 15 and general surgery. 16
The other key theme of lack of training, skills and research competence resulted in various suggestions of training workshops and sessions particularly on research methodology and statistics. Some studies feel that this should commence during undergraduate study, 17 as this interest may then continue into residency. Yarris et al stated that in addition to having a study question, it was crucial to teach study designs, choosing appropriate outcomes and the main core steps from research hypothesis to publication. These factors should all be considered when considering training in research, notwithstanding using collaborative groups which can also address other concerns such as statistical support. 18
The lack of research mentors and supervisors were also highlighted by our residents, again a common complaint in the literature. Appointment of a research director, 19 and structured research mentorship 20 have both been presented as possible strategies for overcoming this and have been shown to improve research output.
Departmental issues such as lack of staff and other resources, mainly due to financial reasons are often harder to address, as in our setting they require a national response to increase funding for research in general. Better access to case notes, electronic databases and less bureaucracy and “red tape” are problems reported by other similar studies and do require an overall enhanced research culture with more support from senior staff and collaboration with other departments of entities that have good research infrastructure. 11
Clearly, our overall findings suggest that there is considerable room for improvement in developing research curricula that can address these concerns and therefore better engage residents in our specialty. Our trainees did have positive attitudes to conducting research but require the support, training and time. The main strength of this study is that it represents a national sampling of residents in our four main centres, using a comprehensive survey with an acceptable response rate. In doing study we identified potential barriers that can now function as targets for program development. Limitations include potential responder bias due to the self-reported nature of the data, which cannot necessarily be independently verified.
Conclusion
Most residents in Obstetrics and Gynecology are interested in conducting research, but the main barriers are lack of time and limited research training. Our data suggests that strategies that aim to include dedicated research time, specific training and formal mentors are required. This will then allow for optimisation of the current research environment.
Supplemental Material
sj-docx-1-mde-10.1177_23821205231168221 - Supplemental material for Attitudes and Perceived Barriers to Research Among Residents in Obstetrics and Gynecology in Trinidad and Tobago: A National Multicenter Cross-sectional Study
Supplemental material, sj-docx-1-mde-10.1177_23821205231168221 for Attitudes and Perceived Barriers to Research Among Residents in Obstetrics and Gynecology in Trinidad and Tobago: A National Multicenter Cross-sectional Study by Sunil Persad, Saksham Mehra and Vanessa Harry in Journal of Medical Education and Curricular Development
Footnotes
DECLARATION OF CONFLICTING INTERESTS
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
FUNDING
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author contributions
All authors contributed to study design, questionnaire development and administration, data collection and analysis and in writing and revision of this study.
Ethical approval
This study was approved by the Campus Research Ethics Committee of the University of the West Indies in August 2021, Reference: CREC-SA.1127//08/2021.
Informed consent
Written informed consent was obtained from all participants via the online form, prior to the commencement of the study.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
