Abstract
Introduction
Hypertension has remained a significant global health issue, with self-care being a critical yet underexplored area, particularly from an axiological perspective.
Aim
This study aimed to examine the axiological perspectives underlying self-care interventions and their impact on hypertension patient behaviors.
Methods
A systematic review was conducted using Scopus, ProQuest, Sage, and PubMed, adhering to PRISMA guidelines. Studies published between 2020 and 2024 were selected based on predefined PICOS criteria. Data analysis was performed thematically by two independent reviewers, with conflicts resolved by a third reviewer. The research protocol was registered in PROSPERO (CRD42024617855).
Results
Out of 2,925 retrieved articles, 10 met the inclusion criteria, involving 1,477 respondents from 11 countries. Three core themes were identified: (1) Personal values (beliefs, perceptions, emotional regulation, and intrapersonal characteristics), (2) Socio-cultural values (social support, family roles, cultural norms, and gender-related barriers), (3) Healthcare system values (accessibility, resource availability, and nurse-led education). Self-care interventions enhanced medication adherence and blood pressure monitoring.
Conclusion
The axiological perspective highlighted the critical role of personal, socio-cultural, and healthcare system factors in improving self-care behavior among hypertensive patients. Integrating these perspectives into nursing education and intervention strategies was essential for optimizing hypertension management.
Keywords
Introduction
Hypertension has been a major global health challenge, responsible for 10.8 million deaths in 2023, with nearly half of the 1.28 billion affected individuals unaware of their condition (World Health Organization, 2023b). In Southeast Asia, including Indonesia and Malaysia, hypertension has been the leading cause of cardiovascular disease, with prevalence rates continuing to rise each year (Nazeri et al., 2022; Sarfika et al., 2023). Moreover, fewer than one-third of individuals in low- and middle-income countries were aware of their hypertension status, and only about 8% effectively manage their blood pressure (Schutte et al., 2021). Self-care has been one of the most critical strategies for managing hypertension to reduce complications, morbidity, and premature death (Dickson et al., 2021; Jung & Moon, 2023). The World Health Organization (WHO) reported that only about one in five people with hypertension successfully control their disease (World Health Organization, 2023a). Improving patients’ knowledge of self-care can encourage them to take an active role in managing their health (Or et al., 2020). This situation underscores the need for more context-sensitive self-care approaches within broader hypertension management programs.
In line with the WHO, self-care in hypertension management referred to individuals’ ability to promote health, prevent complications, and manage blood pressure through an active and dynamic process that required self-efficacy, empowerment, discipline, knowledge, commitment, and self-regulation (Ademe et al., 2019; Konlan & Shin, 2023). It required adherence to medication, dietary control, physical activity, smoking cessation, stress management, and regular monitoring (Pahria et al., 2022; Riegel et al., 2021). Nevertheless, adoption of self-care remained limited due to perceptions, financial constraints, cultural influences, and inadequate social support (Riegel et al., 2021; Sarfika et al., 2023; Shin et al., 2018). Patients’ views about the causes of hypertension also played a significant role in their self-care and medication adherence. For example, patients in Western countries often attributed hypertension to internal factors such as stress, diet, and inactivity. In contrast, patients in Asian countries may have considered both internal factors and supernatural causes, such as taboos or moral violations (Yeom, 2021). These variations highlighted the importance of understanding the values influencing self-care behavior. According to the Health Belief Model, such beliefs and social influences reflected perceived susceptibility, perceived benefits and barriers, and cues to action that shaped health behaviors (Tan et al., 2022). These value-laden constructs provided a theoretical bridge between axiological perspectives and observable self-care practices.
Most research on hypertension has focused on clinical treatments, with limited exploration of the values shaping self-care behaviors, especially in low- and middle-income countries. The axiological perspective offers a valuable approach to understanding these underlying values, including personal values, healthcare system values, and socio-cultural values (Barus et al., 2023; Leonardo et al., 2023; Nguyen et al., 2024). Axiology focused on what is considered valuable, good, or right in decision-making. In self-care, this approach examined whose values guide decisions about treatment, dependence on family, and the acceptance of combining biomedical and traditional practices. An axiological (value-based) lens drew attention to the ethical, cultural, and philosophical dimensions of self-care and organization how patients decided what is “good,” “right,” or “worth doing” in managing their blood pressure and everyday lives. This perspective not only considered the outcomes of interventions but also examined how individual beliefs and cultural norms shaped patients’ understanding and adherence to self-care practices. For instance, patients from different cultural backgrounds may have had differing views on diet or the use of traditional medicine, which could have affected compliance (Barus et al., 2023; Siboni et al., 2021; Sringernyuang & Sottiyotin, 2022; Wahab et al., 2021). At the same time, differences in health services were organized; medications and the availability and affordability of medications, and the roles assigned to nurses in chronic disease management created distinct conditions for hypertension self-care in each country. Thus, understanding how values influence self-care behaviors was crucial in designing effective interventions.
Despite the growing body of research on self-care in hypertension management, no previous systematic review had specifically examined self-care interventions through an axiological perspective. Existing reviews focused largely on clinical effectiveness or behavioral determinants without explicitly analyzing the value-based dimensions embedded in interventions or patient responses. This study was the first to systematically explore how personal, socio-cultural, and healthcare system values influence self-care behaviors in hypertension management across diverse country contexts, highlighting how similar self-care interventions may be interpreted differently depending on each country's cultural norms and health-system arrangements. This systematic review identified key knowledge gaps and provided practical recommendations for developing evidence-based self-care programs that align with patients’ needs and values and can inform more comprehensive hypertension-related degenerative disease management strategies.
The purpose of this study was to investigate axiological perspectives (values, ethics, and cultural considerations) in self-care behavior among individuals with hypertension by answering the following questions:
What axiological principles, values, and cultural considerations were reflected in existing self-care interventions for hypertension? How did personal, healthcare, and socio-cultural values influence the effectiveness of hypertension self-management strategies reported in the literature? How did axiological attitudes and value-based considerations influence patients’ self-care behaviors and related health outcomes, especially in diverse cultural and healthcare contexts?
Methods
Study Design
This study was conducted as a systematic review following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 guidelines (Figure 1). Meta-analysis was not performed because the included studies were highly heterogeneous in terms of study design (cross-sectional surveys, qualitative studies, and randomized controlled trials [RCTs]), intervention content and delivery (educational, counselling, and multidomain self-care programs delivered in person or via digital/remote formats), and outcome measures (different scales and indicators for medication adherence, blood pressure monitoring, lifestyle behaviors, and quality of life). The research protocol was registered in PROSPERO (CRD42024617855).

PRISMA flow diagram.
Search Strategy
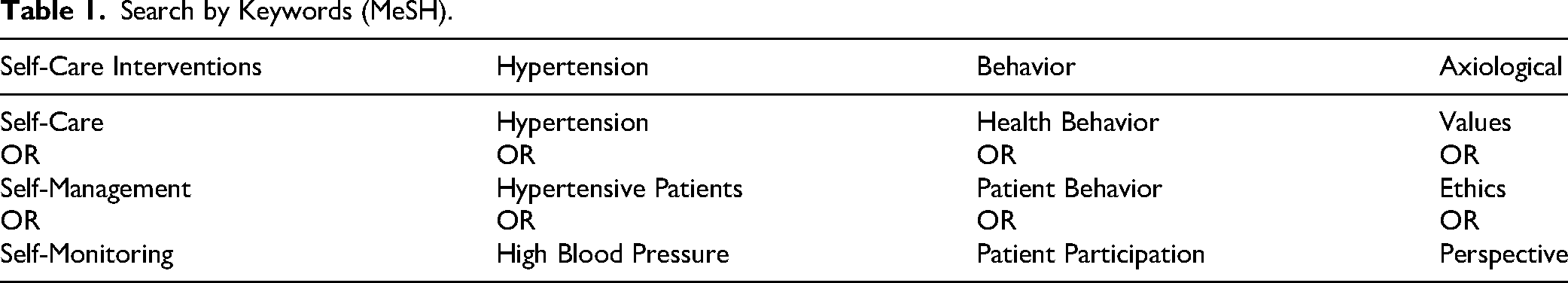
A comprehensive search was conducted of four international databases: Scopus, ProQuest, Sage Journals, and PubMed from October 1 to December 31, 2024. The search strategy combined Medical Subject Headings (MeSH) and free-text terms related to four concept blocks: (1) self-care interventions, (2) hypertension, (3) behavior, and (4) axiological or value-based perspectives (Table 1). Terms within each block were combined with “OR” (e.g., self-care OR self-management OR self-monitoring), and the four blocks were combined with “AND.” A publication-year filter of January 1, 2020 to December 31, 2024, language limits (English or Indonesian), and human-study filters were applied at the database level. The final search update was conducted on December 31, 2024. Full verbatim search strings (including field tags, truncation, adjacency operators, and limits) are provided in Supplementary 1.
Search by Keywords (MeSH).
Eligibility Criteria
The inclusion criteria encompassed studies describing axiological viewpoints on self-care and how these affected the behaviors of patients with hypertension. The inclusion criteria were defined using the PICOS framework as follows: Population: adults diagnosed with hypertension; Intervention: self-care interventions, programs, or behaviors examined from an axiological perspective, including values, ethics, or value-based perspectives (e.g., personal, socio-cultural, or healthcare-system values); Comparison: not applicable; Outcome: hypertension patient behaviors, including medication adherence, home blood pressure monitoring, physical activity, dietary habits, stress management, beliefs and attitudes related to self-care, and, where available, related outcomes such as quality of life or blood pressure control; Study Design: cross-sectional, qualitative, and RCTs published between 2020 and 2024. Exclusion criteria: studies on pregnancy-related hypertension, conference abstracts, non-journal articles, and studies without full-text availability.
Outcomes and Measurement
Across the included studies, self-care related outcomes were operationalized as self-care behaviors and practices, medication adherence, self-care agency, intentions or motivation, knowledge about hypertension, perceived social support, blood pressure control, and patient or clinician experiences of self-care. These outcomes were measured using hypertension-specific self-care instruments such as the Hypertension Self-Care Profile and the Hypertension Self-Care Activity Level Effects, as well as tools including the Hill-Bone Compliance to High Blood Pressure Therapy Scale, the Hypertension Knowledge-Level Scale, the Appraisal of Self-Care Agency Scale-Revised, the Multidimensional Scale of Perceived Social Support, and semi-structured or in-depth interviews. Detailed descriptions of these variables and instruments are presented in Supplementary 5.
Study Selection
After completing the literature search, all retrieved references were imported into Rayyan AI, which supported independent and blinded screening of studies for systematic reviews. Two reviewers (NP & KA) separately reviewed the titles and abstracts to remove papers that were irrelevant to the study. Potentially eligible full texts were then retrieved and assessed against the inclusion and exclusion criteria. Disagreements were resolved through discussion with a third reviewer. The selection process and numbers of included and excluded studies at each stage were summarized in the PRISMA flow diagram (Figure 1). The last screening of publications included in the systematic review yielded ten articles. Both reviewers performed the extraction process independently to ensure objectivity and minimize bias. Extracted information included author, year, country, aims and/or research questions, study design, number of participants, data collection, data analysis, and outcome (Supplementary 5).
Quality Appraisal
To assess the quality of the examined literature, the two researchers utilized the Joanna Briggs Institute critical appraisal tools for cross-sectional, RCTs, and qualitative studies (Aromataris et al., 2024). When reviewers reached differing conclusions, a third assessor was consulted to facilitate consensus. Of the ten studies reviewed, nine were rated as high quality and one was rated as moderate quality; no studies were rated as low quality. Full appraisal details are provided in Supplementary 2–4.
Data Synthesis
The heterogeneity of study designs, interventions, and outcome measures in this systematic review was summarized and interpreted using narrative synthesis (Kaewwanna et al., 2023). First, the extracted data were organized into descriptive tables by study design, population, setting, intervention or focus, self-care outcomes, and instruments used. A thematic synthesis of the findings was conducted, focusing on statements and results related to values, beliefs, and value-laden aspects of self-care. Two reviewers independently coded the results and discussion sections of each study, using both deductive codes informed by an axiological framework (personal, socio-cultural, and healthcare system values) and inductive codes to capture emerging concepts. Through iterative comparison and discussion, similar codes were grouped into categories and then consolidated into three overarching themes: personal values, socio-cultural values, and healthcare system values, which structure the Results section. Convergences, discrepancies, and patterns across countries were examined to highlight how similar self-care interventions were interpreted and experienced differently in different cultural and health-system contexts.
Results
Study and Participant Characteristics
Ten articles out of the 2,925 records retrieved met the inclusion criteria for this review. In total, the included studies involved 1,477 adults with hypertension (aged ≥18 years) and five healthcare professionals. Nine studies included both men and women, while one qualitative study focused exclusively on women in rural Bangladesh (Boitchi et al., 2021). The studies were conducted in diverse settings, including Indonesia, Malaysia, South Korea, Jordan, Alaska (USA), Nepal, Bangladesh, Ethiopia, Türkiye, Peru, Cameroon, and Malawi, representing both high-income and low- and middle-income countries. Study designs comprised six cross-sectional studies, three qualitative studies, and one RCT. Among the cross-sectional studies, four employed univariate and bivariate analyses, whereas one also used multivariate analysis. In the qualitative studies, two used focus group discussions (Al-Rousan et al., 2020; Schaefer et al., 2022), and one used in-depth interviews (Boitchi et al., 2021), with all three applying thematic analysis. The characteristics of the included studies and participants are summarized in Supplementary 5.
Behavioral Outcomes of Self-Care Interventions
Across the included studies, self-care interventions and value-informed self-care practices were associated with better medication adherence, blood pressure monitoring, and lifestyle behaviors, although overall performance remained suboptimal. Only around half of patients achieved good self-care (e.g., 54.1% in Ethiopia and over half in Nepal and Malaysia), and in the BPMONITOR multi-country study, only about 6–33% of participants reported home blood pressure monitoring (Al-Rousan et al., 2020; Gelaw et al., 2021; Nazeri et al., 2022; Shrestha et al., 2021). In Malaysia and Jordan, higher education and stable income clustered with better self-care scores, while in Ethiopia older age and urban residence were associated with good self-care, indicating that sociodemographic advantages tend to accumulate across behaviors (Gelaw et al., 2021; Hani et al., 2024; Nazeri et al., 2022). In the only randomized trial from Türkiye, a nurse-led self-management support program significantly improved treatment adherence and blood pressure control (decreased systolic and diastolic by 9.56 and 6.83 mmHg) compared with usual care (Kurt & Gurdogan, 2022).
Medication Adherence
Medication adherence was the most frequently reported behavioral outcome across the included studies. In the only RCT, a nurse-led self-management support program in Türkiye produced significantly higher adherence to antihypertensive therapy and better blood pressure control than usual care (Kurt & Gurdogan, 2022). Cross-sectional studies from Ethiopia, Malaysia, Indonesia, Jordan, and Nepal similarly showed that patients classified as having “good” or “adequate” self-care had higher adherence than those with “poor” self-care (Hani et al., 2024; Sarfika et al., 2023; Shrestha et al., 2021). From an axiological perspective, adherence was strongly shaped by patients’ values and beliefs: individuals who viewed hypertension as controllable, trusted the value of medication, and felt responsible for protecting their own or their family's health reported more regular medicine-taking, whereas fatalistic or external causal beliefs, as described in the Korean study, were associated with markedly lower adherence (Yeom, 2021).
Barriers to Self-Care
In Korea, patients who attributed hypertension to fate or other external causes had up to 79% lower odds of adhering to medication (Yeom, 2021). Qualitative studies from rural Alaska and multi-country low- and middle-income settings further showed that stigma, device costs, travel distance, and long clinic waiting times often led to missed appointments, interrupted medication use, and reliance on clinic-based rather than home blood pressure monitoring (Al-Rousan et al., 2020; Schaefer et al., 2022). Women in patriarchal communities faced greater obstacles in accessing care, as stigma and expectations about women's mobility frequently led to delayed clinic visits and interruptions in medication use (Boitchi et al., 2021).
Axiological Perspectives
Personal Values
Patients’ perceptions, beliefs, and motivation, assessed in the included studies using hypertension self-care, motivation, and self-efficacy scales and, in qualitative work, inferred from patients’ narratives, played a critical role in self-care (Gelaw et al., 2021; Hani et al., 2024; Sarfika et al., 2023; Shrestha et al., 2021). Older adults were up to 3.8 times more adherent than younger adults, with higher medication adherence and lifestyle self-care than younger adults (Boitchi et al., 2021; Gelaw et al., 2021; Yeom, 2021). These behaviors particularly home blood pressure monitoring, also reduced clinic visits and associated costs (Al-Rousan et al., 2020). However, misconceptions and fatalistic beliefs (e.g., attributing hypertension to transient emotions or fate) were associated with up to 79% lower adherence (Yeom, 2021). Generational differences were evident: younger adults often emphasized lifestyle as the main cause, whereas older adults described broader biological and contextual causes. Positive beliefs such as confidence in controllability through medication, diet, and exercise, and a sense of responsibility to protect personal and family health supported consistent adherence, while negative or ambivalent beliefs led to missed doses (Schaefer et al., 2022). Gender and socioeconomic position also shaped these value orientations: women frequently reported high stress and caregiving demands, whereas men tended to underestimate risk and delay monitoring; patients with adequate finances were better able to act on their intentions by purchasing medication and home BP devices (Boitchi et al., 2021; Gelaw et al., 2021; Nazeri et al., 2022).
Socio-Cultural Values
Based on several included studies, a well-established relationship between social support and self-care behavior among patients with hypertension was identified (Boitchi et al., 2021; Nazeri et al., 2022; Sarfika et al., 2023). In fact, those receiving adequate social support were 2.12 times more likely to have effective self-care practices than those with poor support (Gelaw et al., 2021). Across countries, family members and peers encouraged regular home blood pressure monitoring and lifestyle changes, which improved engagement with treatment plans (Al-Rousan et al., 2020; Schaefer et al., 2022). In Malaysia, self-care practice was significantly associated with religion and race, suggesting that ethnic and faith-based norms influenced how patients interpreted and acted on advice about diet, physical activity, and clinic attendance, and in this context spouses, peers, and religious practices also supported home blood pressure monitoring, lifestyle adjustments, and coping (Nazeri et al., 2022). Marital status and ethnicity also influenced adherence, as spousal involvement offered both emotional and material support that improved continuity of care (Nazeri et al., 2022; Sarfika et al., 2023). At the same time, cultural norms acted as barriers, particularly when traditional remedies were prioritized over biomedical treatment or when chronic illness was stigmatized (Sarfika et al., 2023; Schaefer et al., 2022). In rural Bangladesh, women described stigma, financial hardship, and reliance on husbands or other family members in decisions about clinic visits and medication use, illustrating how patriarchal gender norms and household power dynamics restricted their access to care and constrained hypertension self-management (Boitchi et al., 2021). In Alaska, preferences for behavioral change and traditional or community-based approaches over pharmacotherapy also reflected community norms and past experiences with the health system (Schaefer et al., 2022).
Healthcare System Values
System-level factors such as healthcare accessibility, availability of medicines and equipment, and the way services were organized had a marked influence on self-care behaviors. In rural Bangladesh, women described long travel distances, transport costs, crowded facilities, and shortages of antihypertensive drugs in government clinics as reasons for delaying care until symptoms became “unbearable,” missing routine appointments, or stopping treatment when medicines were unavailable or unaffordable (Boitchi et al., 2021). In the BPMONITOR study in Cameroon, Malawi, and Peru, only around one-third of participants reported monitoring blood pressure at home; most relied on clinic-based checks because they did not own devices, faced medication stock-outs, and perceived some drugs as expensive, especially when not covered by national health insurance, leading to rationing tablets or interrupting therapy (Al-Rousan et al., 2020). Conversely, in Turkey, the presence of a cardiovascular rehabilitation nursing unit and structured follow-up was associated with more systematic patient education and better adherence and blood pressure control (Kurt & Gurdogan, 2022). Across settings, nurse-led education and counselling, whether delivered through rehabilitation units, hypertension clinics, or primary care, were linked to improved knowledge, adherence, and blood pressure outcomes (Al-Rousan et al., 2020; Kurt & Gurdogan, 2022; Nazeri et al., 2022). Patients reported greater satisfaction when counselling was interactive and culturally sensitive rather than one-way information delivery, and participatory approaches that involved shared decision-making appeared to strengthen self-efficacy and sustained engagement with treatment (Schaefer et al., 2022).
Discussion
Interpreted through an axiological lens, the ten included studies showed that value-informed self-care interventions could improve hypertension management, although overall self-care performance remained suboptimal. Across settings, self-care was described as a cluster of behaviors with personal and cultural meaning, including diet, physical activity, stress management, blood pressure monitoring and adherence to treatment, and maintaining blood pressure within the target range remained the primary therapeutic goal in hypertension care (Kurt & Gurdogan, 2022). Several studies showed that only a minority of patients achieved “good” self-care, and home blood pressure monitoring was far from routine (Gelaw et al., 2021; Nazeri et al., 2022; Shrestha et al., 2021). Although self-care was still relatively “new” in many low- and middle-income countries (LMICs), most patients were willing to learn and take a more active role in controlling their condition, but adoption was constrained by cultural beliefs, health literacy, and health-system limitations (Al-Rousan et al., 2020; Mali et al., 2020).
Medication adherence, the most frequently reported behavioral outcome, remained suboptimal yet was a key pathway through which values and beliefs influenced health. Cross-sectional studies from multiple LMICs consistently showed that patients with “good” or “adequate” self-care had higher adherence than those with “poor” self-care (Hani et al., 2024; Sarfika et al., 2023; Shrestha et al., 2021). In the only randomized trial, a nurse-led self-management program in Türkiye improved adherence and blood pressure control compared with usual care (Kurt & Gurdogan, 2022). Conversely, the Korean study indicated that patients who attributed hypertension to fate or other external causes were far less likely to follow their medication regimen (Yeom, 2021). Taken together, these findings suggested that adherence improved when people believed hypertension was controllable, trusted the value of medicines, and felt responsible for protecting their own and their family's health, whereas fatalistic or external causal beliefs undermined adherence even when treatment was available.
Self-care practices were also shaped by broader socio-demographic and socio-cultural conditions. Healthcare systems, financial constraints, and cultural norms all influenced how patients interpreted and enacted self-care (Boitchi et al., 2021; Sarfika et al., 2023). Self-care scores were consistently higher among those with socio-demographic advantages (higher education, stable income, older age, and urban residence), indicating that structural resources accumulated across behaviors (Gelaw et al., 2021; Hani et al., 2024; Nazeri et al., 2022). Gender and family roles further influenced access to care and day-to-day self-management. Women in patriarchal communities reported stigma, restricted mobility, and dependence on husbands or relatives for decisions about clinic visits and medication purchases, leading to delayed care, treatment interruptions, and greater reliance on home-based or traditional remedies (Boitchi et al., 2021). Causal beliefs also played a key role: some patients attributed hypertension to fate or supernatural causes, viewing it as predetermined and beyond their control, which undermined their willingness to invest effort in self-care (Yeom, 2021).
System-level factors strongly conditioned what patients were able to do in their daily lives. Difficulties with transport, long travel distances, crowded facilities, and shortages of antihypertensive drugs in public clinics contributed to delaying care, missing appointments, rationing tablets, or stopping treatment when medicines were unavailable or unaffordable (Al-Rousan et al., 2020; Boitchi et al., 2021). By contrast, settings with structured nurse-led services and rehabilitation units reported more systematic education, closer follow-up, and better blood pressure control, underlining the potential impact of organized programs that support self-management (Kurt & Gurdogan, 2022). These findings showed that self-care was not simply a matter of individual motivation but also of how services, financing, and supplies were organized.
Social support also emerged as a critical socio-cultural value underpinning self-care adherence. Patients with strong social networks were more likely to engage in self-care (Gelaw et al., 2021). Spouses, peers, and religious communities encouraged home blood pressure monitoring and lifestyle changes in several countries, which improved engagement with treatment plans (Al-Rousan et al., 2020; Nazeri et al., 2022; Sarfika et al., 2023). At the same time, stigma surrounding hypertension led some patients to conceal their diagnosis to avoid being perceived as weak or burdensome, thereby reducing opportunities for emotional and practical support (Nazeri et al., 2022). Interventions that normalized hypertension as a chronic but controllable condition and actively involved family members in monitoring, medication management, and lifestyle modification could mitigate shame and increase adherence. Integrating patient–family management approaches could improve outcomes (Ekundayo et al., 2020).
Health professionals, especially nurses and physicians, were well placed to explore patients’ beliefs and values, correct misconceptions, build self-efficacy, and support autonomy (Nazeri et al., 2022; Sarfika et al., 2023; Schaefer et al., 2022). By co-creating individualized care plans that aligned medical recommendations with what mattered most to patients, clinicians helped reframe hypertension from a fatalistic condition to a manageable risk factor (Gelaw et al., 2021; Hani et al., 2024). Tailoring treatment strategies to patients’ preferences for treatment and monitoring, supported by nurse-led programs and structured follow-up where available, was associated with better blood pressure control in several studies (Kurt & Gurdogan, 2022).
Sustained self-care behaviors were crucial for long-term blood pressure control, and regular home blood pressure monitoring could both enhance treatment effectiveness and reinforce patients’ sense of agency in managing their condition (Kurt & Gurdogan, 2022; Shrestha et al., 2021). Nevertheless, maintaining long-term medication adherence remained challenging, particularly among patients with limited understanding of the consequences of uncontrolled hypertension or competing financial priorities (Ademe et al., 2019). Interventions that combined education, reminder systems, and social or family support appeared most promising for sustaining adherence over time.
Overall, the findings from this review suggested that effective hypertension self-care depended on the interaction between personal values, socio-cultural norms, and healthcare system structures. Interventions were more likely to succeed when they enhanced motivation and self-efficacy, resonated with local cultural and spiritual beliefs, and were supported by accessible, affordable health services. Because the included studies were conducted in diverse health systems across Asia, Africa, and the Americas, the patterns identified here offered a global picture but had to be adapted to the specific conditions of each country. Future research should therefore examine how axiological factors operate within particular national contexts and test country-specific self-care programs that align with local values, resources, and policy frameworks. Such work will enable governments and healthcare providers to design degenerative disease management programs for hypertension that are context-sensitive and capable of producing comprehensive, long-term impacts on population health.
Strengths and Limitations
This systematic review utilized the rigorous PRISMA guidelines to ensure transparency and reproducibility. It focused on the underexplored axiological dimension, addressing personal, socio-cultural, and healthcare system values in shaping self-care behaviors. By incorporating studies from multiple countries, the review provided a global perspective on hypertension management, and the use of established critical appraisal tools enhanced the quality and reliability of the included studies. However, the review had limitations. Only peer-reviewed articles in English were included, and the grey literature was not searched. Most studies were cross-sectional or qualitative single-country studies with small or non-probability samples, which may have introduced language bias and limited generalizability. Definitions and measurements of self-care and axiological constructs varied across studies, precluded meta-analysis, and reflected patterns rather than precise effect sizes. Finally, focusing on reported beliefs may have missed some relevant value-related dimensions due to selective reporting in the original articles.
Implication for Practice
These findings can guide the development of evidence-based self-care programs that integrate patient perceptions, cultural values, and health-system constraints. For nurses and other healthcare professionals, routinely exploring patients’ explanations of hypertension and preferred healing practices through brief cultural questions or patient-centered communication frameworks can align self-care plans with what matters to patients. Health systems and policymakers should embed cultural competency training in hypertension care, including skills to negotiate treatment plans that incorporate family roles and appropriate spiritual or traditional practices. At the community level, public health efforts should include community-based education, peer or family support groups, and collaboration with faith or community leaders; targeted media campaigns to reduce stigma, normalize hypertension as controllable, and encourage family engagement in monitoring, medication use, and lifestyle change.
Conclusion
Viewed through an axiological lens, this review showed that hypertension self-care was shaped by the interplay of personal values, socio-cultural norms, and healthcare system factors. Findings indicated that personal values (beliefs, motivation, and perceptions) directly influenced medication adherence, lifestyle changes, and blood pressure monitoring, highlighting the importance of integrating patient perspectives into nursing practice. Moreover, socio-cultural values, including family roles, cultural norms, and gender dynamics, significantly affected patient engagement in self-care, underscoring the need for culturally appropriate care and stigma-reducing public health campaigns. Healthcare system factors, such as access to services, nurse-led education, and infrastructure, required policy and organizational responses, including strengthened cultural competency training for healthcare professionals. Although patients across ten diverse settings generally expressed willingness to engage in self-care, adherence and home blood pressure monitoring remained suboptimal where cultural and structural barriers persisted. These findings suggested that self-care programs and hypertension policies should integrate cultural values, family involvement, and context-sensitive approaches rather than relying solely on biomedical prescriptions. Implications for practice include the need for tailored self-care interventions that consider local cultural and healthcare system contexts to improve hypertension management. Future research should examine these value-based determinants within specific country contexts and test tailored, axiologically informed self-care interventions so that hypertension, as a major degenerative disease, can be managed through country-specific programs with comprehensive, long-term impact.
Supplemental Material
sj-docx-1-son-10.1177_23779608261430127 - Supplemental material for Axiological Perspectives on Self-Care Interventions and Their Impact on Hypertension Patient Behaviors: A Systematic Review
Supplemental material, sj-docx-1-son-10.1177_23779608261430127 for Axiological Perspectives on Self-Care Interventions and Their Impact on Hypertension Patient Behaviors: A Systematic Review by Ni Putu Ayu Ratna Dewi, Nursalam , Komang Ardidhana Nugraha Putra, Suratmi and Titik Suhartini in SAGE Open Nursing
Supplemental Material
sj-docx-2-son-10.1177_23779608261430127 - Supplemental material for Axiological Perspectives on Self-Care Interventions and Their Impact on Hypertension Patient Behaviors: A Systematic Review
Supplemental material, sj-docx-2-son-10.1177_23779608261430127 for Axiological Perspectives on Self-Care Interventions and Their Impact on Hypertension Patient Behaviors: A Systematic Review by Ni Putu Ayu Ratna Dewi, Nursalam , Komang Ardidhana Nugraha Putra, Suratmi and Titik Suhartini in SAGE Open Nursing
Footnotes
Acknowledgments
The authors would like to thank colleagues and academic staff who provided valuable input and technical support during the preparation of this manuscript.
Ethical Approval
This article did not require ethical approval as it is a systematic review. The research protocol was registered in PROSPERO (CRD42024617855).
Author Contributions
All authors contributed significantly to the development of this manuscript.
All authors read and approved the final version of the manuscript and agreed to be accountable for all aspects of the work.
Funding
This work was supported by the Indonesian Education Scholarship (BPI), the Center for Higher Education Funding and Assessment (PPAPT Kemendiktisaintek), and the Indonesian Endowment Fund for Education (LPDP).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
