Abstract
Background
Artificial intelligence (AI) is rapidly transforming healthcare education and practice, making it essential for nursing and health sciences students to develop relevant competencies. However, their preparedness to engage meaningfully with AI in academic and clinical environments remains uncertain.
Objectives
This systematic review synthesizes global evidence on the knowledge, attitudes, practices, and barriers (KAPB) related to AI among students in nursing, medicine, pharmacy, and allied health disciplines.
Methods
Following PRISMA 2020 guidelines, a systematic search was conducted in PubMed, Scopus, CINAHL, and Google Scholar for peer-reviewed articles published between January 2020 and February 2025. Fourteen studies meeting inclusion criteria were analyzed using narrative synthesis. Both quantitative and qualitative studies were included. The review protocol was not registered.
Results
Students generally demonstrated high awareness of AI, but formal training was limited. Knowledge was often acquired informally through social media or peer networks. While attitudes toward AI were largely positive, students expressed ethical concerns and anxiety related to AI use. Practical engagement with AI was mostly restricted to academic writing tasks, with minimal clinical application. Major barriers included the absence of AI-focused curricula, limited faculty expertise, inadequate infrastructure, and concerns over data privacy, ethics, and job displacement.
Conclusion
Despite growing interest in AI, significant gaps remain in health sciences education. Comprehensive strategies such as curriculum integration, faculty development, and ethical training are urgently needed to foster responsible, confident, and clinically relevant AI adoption among future healthcare professionals.
Keywords
Introduction
Artificial Intelligence (AI) encompasses the design of computer systems capable of performing tasks that typically require human intelligence—such as learning, reasoning, and decision-making—through techniques including machine learning, natural language processing, and robotics (Salama et al., 2025). In healthcare, AI applications have revolutionized diagnostic accuracy, patient monitoring, and administrative processes, leading to improvements in clinical decision-making and operational efficiency (AlAli et al., 2025; Alruwail et al., 2025; Alowais et al., 2023). As AI becomes integral to modern healthcare, equipping nursing and health sciences students with foundational AI competencies is essential to ensure they can both harness its benefits and mitigate potential risks in clinical practice.
Although AI's potential to enhance evidence-based practice, personalized patient care, and workflow efficiency is widely recognized, educational institutions frequently lag in preparing future healthcare professionals for AI-driven environments. Studies in the Middle East highlight this gap: in Palestine, 84.5% of nursing students reported general awareness of AI, yet 69.9% had never received formal training on AI tools such as ChatGPT (Salama et al., 2025). Similarly, in Saudi Arabia, more than half of health sciences students indicated insufficient knowledge of AI's clinical applications (Alruwail et al., 2025), while in Jordan, students acknowledged AI's importance but expressed hesitation toward curricular integration due to uncertainty about its relevance in healthcare (Al-Qerem et al., 2023). Across these contexts, students often rely on self-directed learning—using platforms like social media, online tutorials, or peer discussions—to fill gaps in AI education (El-Maksoud et al., 2024; Han et al., 2025a), which may provide exposure but does not guarantee depth of understanding necessary for safe clinical deployment.
Attitudinally, nursing and health sciences students generally hold favorable views of AI's promise. In Saudi Arabia, 84.7% of students believed that ChatGPT could enhance their learning experience (Alharbi et al., 2024), and a multi-country survey reported that 91% of participants agreed AI would positively impact healthcare outcomes (Issa et al., 2024). In Egypt, 65% of students supported the use of AI in medical education (Amiri et al., 2024), and in Turkey, despite limited ability to explain AI's risks, 80% of students recognized its potential benefits (Civaner et al., 2022). Nonetheless, positive attitudes coexist with apprehensions: ethical concerns, data privacy issues, and fears of overreliance on automated systems are recurrent themes (Allam et al., 2024; Jussupow et al., 2025; Rajah et al., 2025). For instance, in Jordan, students voiced ethical reservations and anxiety about job displacement (Al-Qerem et al., 2023), while in Saudi Arabia, apprehensions centered on reduced human interaction and compromised empathetic care (Alruwail et al., 2025). These mixed perceptions underscore the complexity of student readiness for AI integration, shaped by both optimism and caution.
Practically, usage of AI tools among students remains inconsistent. In Palestine, only 33.9% of nursing students reported using ChatGPT in academic tasks (Salama et al., 2025), and 48.3% of pharmacy students and 53.8% of medical students used AI mainly for research-related writing (Issa et al., 2024). In Saudi Arabia, less than 10% of health sciences students had received formal AI training, which correlated with low confidence in utilization (Alruwail et al., 2025; Alghamdi & Alashban, 2024). In Jordan, AI use was largely confined to grammar checking and basic academic tasks (Al-Qerem et al., 2023), and only 34.6% of students expressed willingness to use AI in patient care with proper training (Naureen et al., 2025). Conversely, in the United States, 92% of nursing students reported using tools such as ChatGPT for learning, yet just 3.6% felt proficient (El-Maksoud et al., 2024; Han et al., 2025a, 2025b). These findings suggest that while access to AI tools is expanding, meaningful engagement requires structured training and institutional support.
Numerous barriers impede effective AI adoption in nursing and health sciences education. The most prevalent obstacle is the absence of formal AI curricula. In the Arab region, 92.4% of students reported no formal AI instruction (Allam et al., 2024), and globally, 76.3% of students had not encountered AI within their programs (Busch et al., 2024). Related institutional constraints—such as limited expert faculty, inadequate infrastructure, and lack of clear implementation policies—further exacerbate this educational gap (Alruwail et al., 2025; Rajah et al., 2025). Technical challenges, including poor internet connectivity and insufficient simulation technologies, restrict hands-on learning opportunities (Rajah et al., 2025). Psychological factors, such as moderate-to-high levels of AI-related anxiety, undermine students’ confidence in utilizing AI (Han et al., 2025a, 2025b; Migdadi et al., 2024), while ethical concerns—ranging from data security to depersonalization of care—deter students from embracing AI more fully (Civaner et al., 2022; Chen et al., 2023; Abd El-Maksoud, 2024).
Given the heterogeneity of findings across regions and disciplines, a systematic review is warranted to consolidate evidence on nursing and health sciences students’ knowledge, attitudes, practices, and barriers (KAPB) regarding AI integration in education. Such a synthesis will identify prevailing trends, contextual differences, and gaps in the literature, thereby informing educators, policymakers, and curriculum designers about effective strategies to promote AI literacy. By examining quantitative and qualitative studies from diverse global and regional settings, this review aims to: (1) assess the extent of students’ AI-related knowledge and identify factors influencing their conceptual understanding; (2) explore attitudes toward AI, including motivational drivers and ethical apprehensions; (3) evaluate practical engagement with AI tools and associated confidence levels; and (4) delineate barriers—educational, technical, psychological, and ethical—that hinder AI adoption.
Ultimately, understanding KAPB toward AI among nursing and health sciences students is critical for bridging the gap between emergent technology and healthcare education. As AI continues to reshape clinical practice, equipping future professionals with evidence-based training and support mechanisms will ensure that AI is leveraged ethically, effectively, and compassionately. The findings of this systematic review will provide a comprehensive foundation for developing targeted interventions—such as curriculum enhancements, faculty development programs, and resource allocation—that foster AI readiness and optimize educational outcomes in nursing and health sciences.
For conceptual clarity, this review defines AI literacy as the ability to understand fundamental AI concepts, applications, and implications within healthcare contexts. Proficiency refers to students’ self-reported ability to utilize AI tools effectively for academic or clinical tasks. Readiness encompasses both knowledge and confidence to engage with AI technologies responsibly in practice, considering ethical, technical, and psychological factors.
The term health sciences students, as used in this review, refers to individuals enrolled in programs such as nursing, medicine, pharmacy, and allied health disciplines, unless otherwise specified.
Literature Review
As AI gains prominence in healthcare systems worldwide, scholarly attention has turned toward how nursing and health sciences students perceive and interact with these technologies. A growing body of literature highlights significant variability in students’ experiences with AI across geographic regions, academic levels, and institutional contexts.
While baseline awareness of AI is widespread, deeper conceptual understanding and competence remain inconsistent. Multiple studies have shown that students often learn about AI through informal sources rather than formal education. For example, El-Maksoud et al. (2024) reported that nearly 39% of students in their study acquired AI knowledge independently, primarily through online platforms. Similarly, Han et al. (2025a, 2025b) observed that although 92% of students had used generative tools like ChatGPT, only a fraction could critically evaluate or apply AI outputs in clinical reasoning tasks.
These findings suggest a gap not only in AI familiarity but also in educational structure. The lack of standardization in AI curricula across health sciences programs contributes to fragmented learning experiences. For instance, while Maria et al. (2025) reported high AI knowledge scores among Saudi students, Issa et al. (2024) noted that 72.7% of UAE students had low levels of AI literacy, pointing to regional and institutional disparities.
Attitudes among nursing and health sciences students are broadly positive, particularly when students see AI as a tool to enhance learning and improve healthcare delivery. A survey by Moskovich and Rozani (2025) found that 86.2% of health profession students were familiar with ChatGPT, and the majority rated it positively in terms of usefulness. Importantly, prior exposure significantly affects attitudes; students who have used AI tools tend to exhibit higher enthusiasm and confidence (Al Omari et al., 2024).
However, attitudinal differences can also reflect psychological and demographic factors. Salem et al. (2024) demonstrated that students scoring high on traits such as openness had more favorable views of AI, while those high in neuroticism were more skeptical. Gender-based differences were also documented, with male students often reporting greater confidence in AI use than their female counterparts (Jebreen et al., 2024).
Despite the availability of AI tools, actual use in academic or clinical contexts remains limited. Alghamdi and Alashban (2024) found that fewer than 10% of Saudi students received formal AI training, while Al-Qerem et al. (2023) noted that students primarily used AI for superficial tasks such as grammar checking rather than clinical simulation or diagnostics. Tools like the MAIRS-MS scale have been developed to assess AI readiness among medical students, highlighting the importance of measuring not just exposure but also preparedness (Karaca et al., 2021).
Barriers to AI adoption are multifaceted. Technological limitations, lack of curriculum content, inadequate faculty training, and student anxiety are among the most cited. Migdadi et al. (2024) emphasized that ethical uncertainty and fear of AI replacing human roles contribute to resistance, particularly in patient-facing disciplines like nursing. Cultural concerns and institutional readiness also play critical roles, especially in under-resourced regions (Rajah et al., 2025; Doumat et al., 2022).
Aim of the Study
To examine and synthesize current evidence on the knowledge, attitudes, practices, and barriers related to the integration of AI in nursing and health sciences education.
This aim supports a comprehensive understanding of how prepared students are to engage with AI technologies in academic and clinical contexts, and what challenges must be addressed to enhance AI integration in health professions education.
Methods
This systematic review followed a structured methodology aligned with the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines to ensure transparency, reproducibility, and rigor in synthesizing evidence related to nursing and health sciences students’ knowledge, attitudes, practices, and barriers (KAPB) toward AI.
Study Design
A systematic review design was adopted to identify, evaluate, and synthesize quantitative and qualitative studies exploring the integration of AI in nursing and health sciences education. The review summarized trends, common findings, and variations in students’ experiences and perceptions globally, as illustrated in Figure 1.

PRISMA 2020 Flow Diagram Describing Study Selection for Systematic Review.
Search Strategy
A comprehensive literature search was conducted across the following databases:
PubMed; CINAHL; Scopus; Google Scholar
Search terms included combinations of:
“Artificial Intelligence” OR “AI” “Nursing students” OR “Health sciences students” “Knowledge” OR “Attitudes” OR “Practices” OR “Barriers” “Education” OR “Curriculum” OR “Training”
Boolean operators (AND, OR) and truncation symbols were applied to enhance search sensitivity.
Protocol Registration
This systematic review was not registered in PROSPERO.
Inclusion Criteria
Studies published between 2020 and 2025
Peer-reviewed articles and relevant grey literature
Studies focusing on nursing or health sciences students
Research examining at least one of the following: knowledge, attitudes, practices, or barriers toward AI.
Studies conducted in educational or clinical training contexts
Exclusion Criteria
Studies involving only faculty or professionals (excluding students)
Editorials, commentaries, or opinion papers without original data
Non-English language publications
Duplicate studies or articles with inaccessible full text
Study Selection
Two independent reviewers screened titles and abstracts for relevance. Full texts of potentially eligible studies were retrieved and assessed against the inclusion and exclusion criteria. Discrepancies were resolved through consensus or consultation with a third reviewer.
Data Extraction
A standardized data extraction form was used to collect information, including:
Author(s), year, and country Study design and sample characteristics AI-related knowledge findings Reported attitudes, practices, and barriers Instruments or scales used Key results and conclusions
Quality Appraisal
A formal quality assessment of the included studies was conducted using the appropriate Joanna Briggs Institute (JBI) critical appraisal tools, tailored to each study design (cross-sectional, qualitative, or mixed-method). Two independent reviewers assessed each study's methodological rigor, focusing on criteria such as clarity of objectives, sampling methods, validity and reliability of measurement tools, control of confounding variables, and ethical considerations.
Each study received a JBI quality score, with ratings categorized as high, moderate, or low quality based on the proportion of criteria met:
High quality: 75% or more criteria fulfilled Moderate quality: 50–74% criteria fulfilled Low quality: below 50% criteria fulfilled
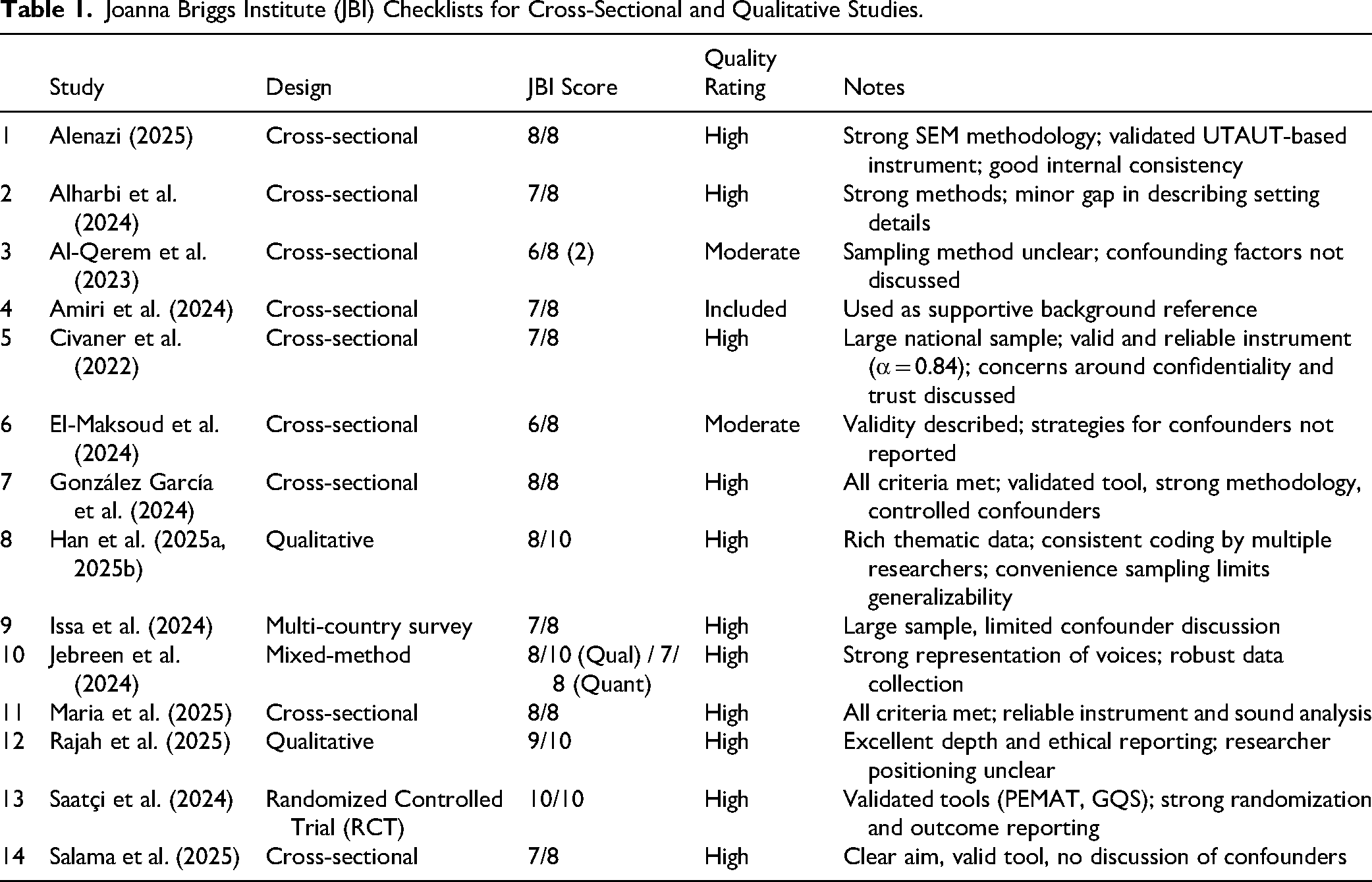
The included studies generally demonstrated high methodological quality, as reflected in strong Joanna Briggs Institute (JBI) appraisal scores. Most cross-sectional studies—such as those by Alenazi (2025), Civaner et al. (2022), and Maria et al. (2025)—used validated instruments, clearly stated objectives, and employed appropriate analytical methods. Qualitative studies, including Han et al. (2025a, 2025b) and Rajah et al. (2025), offered rich thematic insights supported by consistent coding procedures and transparent ethical reporting.
Despite these strengths, some limitations were observed. In several studies (Al-Qerem et al., 2023; El-Maksoud et al., 2024), sampling methods were not clearly described, and potential confounding variables were insufficiently addressed. A number of studies relied heavily on self-reported data, which may introduce recall and social desirability biases. Qualitative studies often employed convenience sampling, which limits generalizability beyond the studied population.
While these limitations do not undermine the overall value of the findings, they highlight the importance of interpreting results with caution. Future research should adopt more rigorous and standardized methodological approaches, such as probability sampling, longitudinal designs, and mixed-methods integration, to strengthen the evidence base on AI integration in health sciences education.
A summary of quality appraisal outcomes is presented in Table 1, providing transparency regarding study rigor and potential sources of bias.
Joanna Briggs Institute (JBI) Checklists for Cross-Sectional and Qualitative Studies.
Data Synthesis
A narrative synthesis approach was employed due to the heterogeneity of study designs, populations, and measurement tools. Both quantitative and qualitative findings were organized thematically under the four core domains: knowledge, attitudes, practices, and barriers. For qualitative data, an inductive thematic analysis was conducted. Two independent reviewers systematically coded the qualitative findings by carefully reading each included study and identifying recurrent concepts. Initial codes were discussed, compared, and refined collaboratively. These codes were then grouped into overarching themes, reflecting patterns across the studies. For quantitative studies, relevant descriptive statistics (e.g., frequencies, percentages) were summarized and mapped to the same thematic domains to enable integration of qualitative and quantitative results. Discrepancies in coding or theme development were resolved through consensus discussions. When disagreements persisted, a third reviewer was consulted to ensure methodological rigor and minimize potential bias. This iterative process ensured that the synthesis reflected the diversity of study contexts while maintaining consistency in theme interpretation as in table 2.
Study Characteristic and Details.

Results
This systematic review synthesized findings from 14 studies conducted between 2022 and 2025, examining the knowledge, attitudes, practices, and barriers (KAPB) associated with AI integration among nursing and health sciences students. The studies represented a range of geographical contexts, including Saudi Arabia, Jordan, Egypt, Turkey, the United States, Palestine, South Africa, Spain, and several multi-country surveys. Sample sizes varied, with a cumulative total of 9,693 participants in the studies that reported this information.
Knowledge of AI
Across studies, participants generally demonstrated a basic awareness of AI, though depth of understanding varied significantly. In Palestine, for instance, 84.5% of nursing students were aware of AI, yet 69.9% had never received formal training. Similarly, students in Saudi Arabia exhibited high AI knowledge scores in some contexts (Maria et al., 2025), whereas others, such as those in the United Arab Emirates, showed lower literacy levels (Issa et al., 2024). A consistent theme across the literature was that most students acquired knowledge about AI through informal channels, including social media, online platforms, and peer networks (El-Maksoud et al., 2024; Han et al., 2025a, 2025b), rather than structured curricular exposure.
Attitudes Toward AI
The majority of students held positive attitudes toward the potential of AI in health sciences education. In Saudi Arabia, 84.7% of students agreed that ChatGPT could enhance their academic performance (Alharbi et al., 2024), and in Egypt, 65% supported AI's inclusion in medical education (Amiri et al., 2024). However, these positive views were often tempered by ethical concerns and fears of job displacement. Some studies highlighted the role of psychological factors; for example, students scoring high in openness reported more favorable attitudes, while those high in neuroticism exhibited greater skepticism (Jebreen et al., 2024).
Practices and Engagement
Despite widespread access to AI tools, actual usage in educational and clinical contexts remained limited. In Palestine, only 33.9% of students reported using AI in academic tasks, and similar trends were observed in Jordan and Saudi Arabia (Al-Qerem et al., 2023; Salama et al., 2025). In contrast, a U.S.-based study reported that 92% of students used generative AI tools, though only 3.6% felt proficient (Han et al., 2025a, 2025b).
Barriers to Integration
Key barriers included the absence of formal AI education, lack of trained faculty, infrastructural limitations, and ethical concerns. In the Arab region, 92.4% of students reported no formal instruction in AI (Allam et al., 2024). Other barriers included internet limitations, AI-related anxiety, and concerns over data privacy and the depersonalization of care (Civaner et al., 2022; Rajah et al., 2025).
Discussion
This systematic review highlights growing global awareness and interest in AI among nursing and health sciences students. However, significant gaps persist in knowledge, practical application, and institutional readiness, revealing a misalignment between technological advancements in healthcare and current educational practices.
Although most students reported general AI awareness—often gained informally through social media and peer discussions—structured, curriculum-based AI education remains notably absent. Studies from Palestine, Saudi Arabia, and Jordan consistently show high awareness but low formal training rates (Alruwail et al., 2025; Al-Qerem et al., 2023; Salama et al., 2025), reflecting a global trend where familiarity with AI does not translate into clinical competence or confidence.
Despite positive attitudes toward AI, students also expressed ethical concerns and psychological reservations. Common fears included data privacy breaches, diminished human interaction, and potential job displacement—particularly noted in regions such as Jordan and South Africa (Al-Qerem et al., 2023; Rajah et al., 2025). These concerns highlight the importance of framing AI education within ethical and humanistic contexts.
Student interaction with AI tools remains largely superficial, with platforms like ChatGPT used mainly for academic writing rather than clinical decision-making. This trend underscores the need for structured, competency-based AI training in health sciences education. Without targeted interventions, student engagement is unlikely to evolve beyond basic, non-clinical use.
The methodological quality of the included studies was generally strong, with most employing validated tools and sound designs. However, limitations such as non-random sampling, inadequate control for confounders, and reliance on self-reported data should be acknowledged when considering the generalizability of the results.
Implications for Global Education and Policy
To bridge the readiness gap, there is an urgent need for global standardization of AI curricula. The wide variability in student exposure and competencies across countries underscores the absence of coordinated international benchmarks. Establishing standardized learning objectives, ethical guidelines, and assessment frameworks would reduce disparities and better prepare future healthcare professionals.
Faculty development is also crucial. Many institutions lack trained educators capable of delivering AI content, limiting the implementation of AI curricula. Investments in faculty training, interdisciplinary partnerships with computer science departments, and the integration of AI ethics are essential to building institutional capacity.
Moreover, addressing psychological and ethical concerns requires more than technical training. Educational programs should incorporate critical discussions on AI's limitations, ethical dilemmas, and its impact on patient care to foster responsible and reflective use of technology.
A recurring paradox in the studies is the coexistence of favorable attitudes toward AI with low preparedness and limited practical competence. This likely stems from structural and institutional barriers, including the absence of standardized AI curricula and overreliance on informal exposure (Alruwail et al., 2025; El-Maksoud et al., 2024). In Middle Eastern contexts, hierarchical educational structures and limited faculty expertise further constrain meaningful engagement with AI (Rajah et al., 2025). AI is often seen as an aspirational technology, fueling enthusiasm without equivalent investments in infrastructure or faculty development.
These findings mirror broader global trends in digital health, where technology adoption often outpaces institutional capacity, particularly in low-resource settings (Amiri et al., 2024; Liu et al., 2025). Bridging this gap requires integrated strategies that go beyond awareness, including the development of contextually appropriate curricula, faculty empowerment, and critical engagement with AI's ethical and clinical implications.
Methodological Rigor of Included Studies
The included studies generally demonstrated high methodological quality, supported by strong JBI appraisal scores. Most cross-sectional designs featured clear objectives, validated instruments, and appropriate analyses. Nonetheless, some studies suffered from unclear sampling methods, insufficient attention to confounding variables, and reliance on self-reporting, which may introduce bias. While qualitative studies offered valuable insights, many used convenience sampling, limiting the generalizability of findings. Future research should adopt more rigorous and standardized methodologies to strengthen the evidence base on AI integration in health sciences education.
Strengths and Limitations
This systematic review has several strengths. It synthesizes evidence from 14 recent studies across diverse geographical contexts, providing a comprehensive and up-to-date overview of nursing and health sciences students’ knowledge, attitudes, practices, and barriers toward AI integration. The inclusion of both quantitative and qualitative research allowed for richer insights and cross-validation of findings. Methodological rigor was generally high, with most studies employing validated instruments and robust analytical approaches. Additionally, the review followed PRISMA 2020 guidelines, ensuring transparency and reproducibility in study selection and synthesis.
However, certain limitations should be acknowledged. First, only studies published in English were included, which may have excluded relevant research conducted in other languages and introduced language bias. Second, although grey literature sources were screened, the inclusion was limited, raising the possibility of publication bias due to the greater likelihood of positive results being published in peer-reviewed journals. Third, there was notable variability in study quality, designs, and settings, which limits the comparability of results and precluded the use of meta-analytic techniques. Fourth, most included studies relied on self-reported data, which may be subject to recall inaccuracies and social desirability bias. Finally, the heterogeneity of measurement tools, outcome definitions, and participant characteristics made it challenging to draw uniform conclusions across contexts. These limitations underscore the need for more standardized, multilingual, and methodologically robust research to strengthen the evidence base for integrating AI into nursing and health sciences education.
Implications of the Study
This systematic review underscores critical implications for nursing and health sciences education in the context of AI integration. First, the evident lack of formal AI instruction highlights the need for comprehensive curriculum reform. Educational programs must embed foundational AI concepts, clinical applications, and ethical considerations to prepare students for technologically advanced healthcare environments. Second, faculty development is essential, as educators require sufficient knowledge and training to effectively guide students in AI use. Without this, student learning may remain superficial and reliant on informal sources. Third, institutional and governmental policies must support AI integration through infrastructure investments, access to AI tools, and clear implementation frameworks. The study also reveals ethical and psychological barriers, such as concerns over data privacy, job displacement, and AI-induced anxiety, which necessitate targeted educational interventions and support systems. Additionally, regional disparities in AI readiness suggest a need for international collaboration to standardize AI competencies and reduce educational inequalities. Finally, future research should explore the longitudinal impact of structured AI training on student performance and professional readiness. Collectively, these implications highlight the urgency for coordinated action among educators, policymakers, and health institutions to ensure ethical, effective, and equitable AI adoption in healthcare education.
Conclusion
There is a clear gap between the increasing relevance of AI in healthcare and the readiness of nursing and health sciences students to effectively and ethically use AI tools. While students generally show positive attitudes and high interest, their actual knowledge and application of AI remain limited due to a lack of formal education, insufficient faculty training, infrastructural constraints, and ethical or psychological concerns. To address this, institutions must adopt comprehensive strategies—such as integrating AI into curricula, enhancing faculty development, and providing ethical frameworks—to ensure future healthcare professionals are adequately prepared for AI-integrated practice.
Footnotes
Acknowledgement
We acknowledge the midwives who participated in the study.
Ethical Approval and Consent to Participate
Ethics approval was obtained from the Palestine Polytechnic University Ethics review committee (RCK-2/12/25). Informed consent was obtained from each participant with an assurance of anonymity and confidentiality.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data for this study will be available upon reasonable request from the principal investigator.
