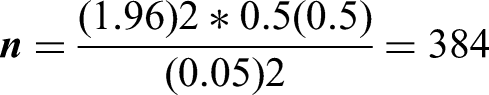Abstract
Background
The minor disorders of pregnancy are a series of commonly experienced disorders like nausea and vomiting, frequency of urination, heartburn, constipation, back pain, leg cramps, disturbance of sleep, and varicosities that mostly affect women during pregnancy. Across the world, due to a lack of self-management practice and less attention to minor disorders of pregnancy, pregnant women are exposed to major disorders of pregnancy, which have a negative impact on quality of life, and pregnancy outcomes. Most previous studies gave attention to the knowledge of minor pregnancy disorders and limited self-management practices of minor pregnancy disorders.
Objective
To assess the self-management practice of minor pregnancy disorders and associated factors among pregnant women attending the antenatal clinic at Tulu Bolo General Hospital, Southwest Shewa, Ethiopia, 2022.
Methods
An institutional-based cross-sectional study design was conducted from August 1 to September 30, 2022. Among 403, pregnant women were selected using a systematic random sampling technique. A structured and interviewer-administered questionnaire was used to collect the data. Data were entered in Epi Data version 3.1 and exported to SPSS window version 26 for analysis. Bivariate and multivariable analyses were done to identify variables associated with the self-management practice of minor pregnancy disorder in the binary logistic regression model. A statistical significance was declared at P-value < .05. Finally, tables, graphs, and narration were used to present the data.
Results
A 397 study participants were included with a response rate of 98.5%. This study revealed that 29.3% (95% confidence interval [CI]: 24%, 34%) of women had good self-management practices for minor pregnancy disorders. The age of the pregnant women (AOR = 4.4; 95% CI: 1.64, 11.60), household wealth status (AOR = 3.6; 95% CI: 1.68, 7.97), women's education status (AOR = 5.8; 95% CI: 2.16, 16.03) and (AOR = 4.11; 95% CI: 1.30, 12.97), women's occupation (AOR = 2.44; 95% CI: 1.09, 5.45), and knowledge on minor pregnancy disorders (AOR = 2.06; 95% CI: 1.12, 3.79) were identified as statistically significant factors.
Conclusions and recommendations
These findings showed that 70.7% of pregnant women were found to have had a lack of good self-management practices for minor pregnancy disorders. Hence, counseling and enhancing their knowledge of self-management should be provided to pregnant women to enhance their awareness regarding self-management practices of minor pregnancy disorders.
Introduction
Pregnancy is a crucial period of a woman's life that needs special consideration from the period of conception till the puerperium (Cunningham et al., 2022; Joo et al., 2024). Minor disorders of pregnancy (MDP) are the disorders that occur during pregnancy that are completely caused by the pregnancy or exacerbated by the pregnancy (Khalil & Hamad, 2019; Pinto et al., 2014b). They are caused by physiological, anatomical, biochemical, and immunological changes and adaptations that happen within the mother, which lead to many minor disorders (Dutta, 2016; Landon, 2024). In all trimesters of pregnancy, minor pregnancy disorders are common and threaten the well-being of the pregnant mother as well as the fetus (Landon, 2024; Latha & Indira, 2016).
Morning sickness, varicosities, backaches, constipation, heartburn, and leg cramps are among the minor disorders that worsen as the pregnancy progresses and negatively affect the pregnancy experience; their high prevalence has a significant impact on daily activities and a profound impact on the lives of the pregnant women and their families (Agampodi et al., 2013; Aziz & Maqsood, 2016; Sangeetha et al., 2015; WHO, 2016). Furthermore, minor pregnancy disorders would cause difficulties for both the health care provider and the pregnant woman due to misinterpretation as pathological, leading to unnecessary health facility visits (Australian Government Department of Health, 2018; Dutta, 2016).
During the prenatal period, self-management refers to the process by which women use knowledge and self-treatment skills that they may get from different sources to promote a positive outcome and restore a healthy lifestyle (Iyawa et al., 2021; Ryan & Sawin, 2013). Current healthcare practice is influenced by a variety of sociocultural determinants, and even the choice of self-management practices is learned primarily through prior experience, close relatives, and correct actions that are dependent on their monthly income and educational level (Nazik & Eryilmaz, 2014; Sangeetha et al., 2015).
The evidence revealed that for the management of common minor pregnancy disorders,World Health Organization (WHO), American College of Obstetric and Gynecology (ACOG) and pregnancy care clinical practice guidelines currently recommend non-pharmacological threapies and remedies such as ginger and vitamin B6 for morning sickness; lifestyle and diet modification for heartburn (such as avoiding heartburn triggers, overeating, and going to bed with a full stomach; maintaining upright posture until food digested; using foods like green beans, potatoes, and carrots); exercise regularly throughout pregnancy; use of a support belt with massage and acupuncture and acupressure for backaches; dietary modification for constipation (higher dietary fiber intake like fruits, legumes, vegetables and porridge, and adequate fluid intake); compression stockings, leg elevation, and water immersion for varicosities (ACOG, Guidelines, 2018; Australian Government Department of Health, 2018; Joo et al., 2024; WHO, 2016). An international study of 23 countries indicated that herbal remedies were utilized during pregnancy to manage pregnancy disorders (Kennedy et al., 2013).
In Africa, including Ethiopia, non-pharmacological therapies, including home remedies, are widely used to alleviate minor pregnancy disorders, particularly morning sickness, constipation, back pain, and leg cramps. Due to the accessibility of treatment and the availability of materials, many pregnant mothers choose to use home remedies to manage pregnancy-related problems (Belayneh et al., 2022; Laelago et al., 2016; Peprah et al., 2019; Shewamene et al., 2017; Tengia-Kessy & Msalale, 2021). Therefore, if appropriate, home remedies and non-pharmacological therapies can be used to alleviate minor disorders as a first option for self-care. However, medication may be required to ensure the well-being of the mother and prevent secondary adverse effects on the fetus (Dhanawade, 2017). Hence, if pregnant mothers are helped to manage their minor disorders, it effectively restores their health (Kaur & Gagandeep, 2017).
The pregnant woman who experiences minor disorders suffers from them, which is far from minor even though they are commonly referred to as “minor disorders” (Aziz & Maqsood, 2016; Joshi & Hamad, 2019). The high prevalence of these minor disorders and lack of self-management, however, have a significant influence on everyday activities and have a profound impact on the lives of pregnant women and their families (Sangeetha et al., 2015). Morning sickness (70%), varicosities (40%), back pain (50–70%), constipation (39%), heartburn (30–50%), and leg cramps (70–80%) are the minor disorders that worsen as the pregnancy progresses and negatively affect the pregnancy experience; among those, nausea and vomiting (NVP) account for 43.1% of hospital admissions (Agampodi et al., 2013; Aziz & Maqsood, 2016; Pinto et al., 2014a; Sangeetha et al., 2015; WHO, 2016). The study's findings in Iraq and India indicated that pregnant women's self-management regarding minor pregnancy disorders was very poor (Aziz & Maqsood, 2016; Peter, 2014; Rosy, 2014).
The majority of pregnant women did nothing to alleviate minor pregnancy symptoms, and many antenatal women were unsure how to manage their pregnancy condition, putting the fetus, family, and community at risk (Gouda Nasr et al., 2019; Nazik & Eryilmaz, 2014). According to the evidence, the consequences of a lack of self-management practice of common minor pregnancy disorders include increased risk of pain, disruption of sleep and daily activities (WHO, 2016), and a negative impact on quality of life, particularly physical and occupational function (Tan et al., 2018). Furthermore, some MDP, if left untreated, can lead to serious complications; even the severe form leads to an increased risk of severe anxiety, stress, preterm labor, and low birth weight, which might be the reason for hospitalization during pregnancy (Elena & Saborio, 2019; Gouda Nasr et al., 2019). Due to the cost-effectiveness of therapy and easy access to products, many pregnant women in Africa, including Ethiopia, use simple home remedies to manage pregnancy-related problems (Laelago et al., 2016; Peprah et al., 2019; Shewamene et al., 2017). Further, health education and counseling on self-management as a part of antenatal care during antenatal visits for pregnant women about how to handle pregnancy-related disorders and their home remedies (Kaiser & Allen, 2016; Nazik & Eryilmaz, 2014) help to continue the pregnancy without having any major effects, which leads to achieving the sustainable developmental goal (SDG) by 2030 (Gururani et al., 2018). Therefore, this study aimed to determine the self-management practice of minor pregnancy disorders and associated factors among pregnant women attending an antenatal care clinic at Tulu Bolo General Hospital, Ethiopia.
Objective of the Study
To assess the self-management practice of minor pregnancy disorders and associated factors among pregnant women attending an antenatal care clinic at Tulu Bolo General Hospital, Ethiopia, 2022.
Research Questions
What is the level of self-management practices of minor pregnancy disorders among pregnant women who attended the antenatal care clinic at Tulu Bolo General Hospital, Ethiopia?
What are the factors associated with self-management practices of minor pregnancy disorders among pregnant women who attended the antenatal care clinic at Tulu Bolo General Hospital, Ethiopia?
Methods and Materials
Study Setting and Period
This study was conducted at Tulu Bolo General Hospital, southwest Shewa, from August 1 to September 30, 2022. It is 80 km from Addis Ababa and 34 km from the zone capital, Waliso, on the way to Jimma. The Tulu Bollo General Hospital (TBGH) is located in Tulu Bolo Town. Tulu Bolo is a town in Oromia's Southwest Shewa Zone, with coordinates 8°40′N 38°13′E and an elevation of 2193 m above sea level (Lemma, 2020). Tulu Bolo Hospital provides antenatal care services for pregnant women. The hospital has surgical, medical, gynecological, and obstetric departments, as well as different OPD, emergency ward, and IPD departments with different health professionals. This research was carried out at an antenatal care clinic that provides antenatal care services with seven different healthcare providers.
Study Design and Population
Study Design
Institution-based cross-sectional study design was conducted from August 1 to September 30, 2022.
Population
All pregnant women.
Sample
All systematical selected pregnant women who attended the antenatal care clinic at Tulu Bolo General Hospital during the study period.
Eligibility Criteria
Inclusion Criteria
The study included pregnant women who attended the antenatal care clinic and were willing to participate in the study.
Exclusion Criteria
Antenatal women who come with emergency cases during data collection.
Sample Size Determination
The sample size was calculated using the single population proportion formula, with a 95% confidence interval (CI), a 5% margin of error, and considering population proportion of 50%.
With the following assumptions:
Where:
Therefore, by adding a 5% non-response rate, the actual sample size was
Sampling Techniques and Procedures
The study participants were selected using a systematic random sampling technique from the pregnant women who were attending antenatal care clinic during the study period. According to two months hospital reports, the estimated number of pregnant women who were attending antenatal care clinic was 968. The sampling interval (Kth value) was obtained by dividing the source population (968) by the total sample size (403), which yields an approximate result of 2. The first pregnant women were selected by the lottery method within the sampling interval. The interviewed pregnant women who were on follow-up, eligible, and not involved in the pre-test were included in daily base data collection. Then, at the exit, every second pregnant woman was interviewed face-to-face.
Study Variables
Dependent Variable
Self-management practice of minor pregnancy disorders.
Independent Variables
Socio-demographic variables: Age, Marital Status, Religion, Ethnicity, Women's educational status, Women's Occupation, Husband's educational level, Husband's Occupation, Household Wealth Status, Residence, and Family Size. Obstetrics-related variables:- Gravidity, Parity, A History of Previous Abortions, Previous Stillbirth, Gestational age (GA), and Type of Pregnancy. Previous history of minor disorders of pregnancy, previous history of hospitalization, Number of ANC visits, GA at 1st ANC visit, Counseling on minor pregnancy disorder (MPD). Knowledge of minor pregnancy Disorders.
Operational Definitions
Minor disorders during pregnancy refer to the common problems that occur during pregnancy, which include NVP, frequency of urination, heartburn, constipation, back pain, leg cramps, disturbance of sleep, and varicosities, which can affect the daily activities of the pregnant woman (El-Sharkawy et al., 2020; Ibrahim et al., 2020; Koonge et al., 2020; Sreeja, 2015).
In this study, “minor pregnancy disorder” refers to pregnant women who experience at least one common pregnancy disorder during pregnancy (Latha & Indira, 2016; Zielinski et al., 2015).
Self-management refers to the process by which women use knowledge and self-treatment skills that they may get from different sources to promote a positive outcome and restore a healthy lifestyle (Ryan & Sawin, 2013).
Good self-management practices: Pregnant women who scored the mean or above the mean on the self-management practice questions related to MDP were considered to have a good practice. However, contrarily, those who scored less than the mean score were considered to have poor self-management practices for minor pregnancy disorders.
Good knowledge: Pregnant women who scored 50% or higher on knowledge questions were considered to have good knowledge of the MDP. Those who scored less than 50%, on the other hand, were considered to have poor knowledge of minor pregnancy disorders (Khalil & Hamad, 2019; Sreeja, 2015).
Data Collection Tools
Data were collected using interviewer-administered, pre-tested questionnaires, which were from similar research done on the outcome of interest and used for collecting data. The questionnaire has four parts. First part: Socio-demographic Characteristics, which contains 11 items, in which age and family size were open-ended questions and the others were closed-ended questions with multiple choices, including multiple-choice questions for household wealth status. Second part: Questions related to obstetric factors, which contain 11 items in which GA, gravidity, and parity are open-ended questions and the rest are closed-ended yes/no responses. Third part: Questions related to knowledge of MPD, which are 18 questions. The overall knowledge score for each participant was calculated by summing the scores of 18 questions with a possible range of 0 to 18, which were divided into two categories: poor knowledge (score less than 9) and good knowledge (score greater than or equal to 9). The question items were given categorical responses (Yes, No), with 1 point given for each correct answer and 0 for each incorrect answer. Fourth part: Questions related to the self-management practice of minor pregnancy disorders, which consists of 32 self-management practice-related questions. The mean of the mean scores for the self-management practice questions was used to calculate the overall level of self-management practice among the participants after each participant's mean was computed for each experienced pregnancy disorder with a possible range of 0–32, which is the minimum and maximum score. The questionnaire responses were divided into yes-or-no categories of multiple choices, with 1 point given for each correct response and 0 for an incorrect one.
The questionnaires were prepared in English version after reviewing different literature, and translated into Amharic, then Afan Oromo the local language. Two Bsc Midwives and one Nurse as data collectors and one Msc Midwife supervisor were recruited for data collection. The content validity was checked by field experts and professionals for relevance, clarity, and completeness of the tool and the reliability of the questionnaires was checked using Cronbach's alpha value which was .75 and .84 for knowledge of minor pregnancy disorders and self-management practice of minor pregnancy disorders respectively.
Data Quality Control
To maintain the quality of data, the questionnaire was prepared first in English version and then translated into local language by an independent language expert to ensure its consistency. The training was given to both supervisor and data collectors before the actual data collection. A 5% pretest (21 pregnant women who fulfilled eligibility criteria) was conducted at Lemen hospital to check the questionnaire's clarity, length, consistency, and completeness. The quality of collected questionnaires was checked for completeness and consistency daily by the principal investigator and supervisor, and then timely corrections were made. Data were reviewed, coded, entered, and crosschecked during data entry into the computer software before analysis.
Statistical Analysis
The data were thoroughly coded, and carefully entered into Epidata version 3.1 and exported to SPSS window version 26. Principal component analysis (PCA) was computed to see the wealth status of households. From 15 items included in the analysis, three factors with ten items were created which could explain 72.3% total variance. Both descriptive statistics and analytical analyses were computed. A descriptive statistical analysis was computed to summarize and describe the characteristics of study participants, and the information was presented using text, frequency tables, and figures.
Inferential statistics were applied to reflect the association between outcome and covariates variables. In bivariate analysis, a crude odds ratio with a 95% CI was used to determine the relationship between each independent variable and the dependent variable using binary logistic regression. Initially, all variables were analyzed first by using a bivariate analysis to identify the candidate explanatory variables, and those candidate explanatory variables (P-value of <.25) were entered into a multivariable analysis by using the binary logistic regression model.
Multivariable analysis was done to control the effect of all possible confounders and to identify the factors associated with the self-management practice of minor pregnancy disorders. The strength of association was presented using an adjusted odds ratio (AOR) with a 95% CI. For all independent variables, the multicollinearity effect was checked by co-linearity diagnostic statistics via variance inflation factors (VIF) and tolerance test with a maximum value of 2.73 and minimum value of 36.6%, respectively. The regression model fitness was checked using Hosmer and Lemeshow goodness of fit and was well fitted (X2 = 6.708; df = 8; P = .568) and the full logistic regression model was a significant prediction performance [Omnibus test of model coefficient (X2 = 109.70; Df = 16; P < .001)]. Those variables with a P-value <.05 in multivariable analysis were considered significant associations. Finally, the results were presented in the form of tables, graphs, and figures.
Results
Among a total sample of 403 study participants, 397 were interviewed and gave a response rate of 98.5%, and the results were presented as follows under subheadings.
Socio-Demographic Characteristics of the Study Participants
More than half, 263 (66.2%), of the participants were in the age group 20–30 years. The mean ages of the respondents were 25.4 (±4.94) years. Two hundred and ten (52.9%) of the study participants were urban residents. The majority of participants, 295 (74.3%), were Orthodox religious followers. Among the study participants, 394 (99.2%) were married. More than two-fourths of women attended formal education: 228 (57.4%) and 152 (38.3%) of them reported that their husband's educational status was secondary and above. Two hundred and four (62.5%) of women were homemakers, and 48.9% of them reported that the occupational status of their husbands was a farmer. Regarding household wealth status, 134 (39.9%) and 125 (36.7%) of women were residing in a family with rich and poor quintiles, respectively (Table 1).
Socio-Demographic Characteristics of the Respondents at TBGH, Southwest Shewa, Ethiopia, 2022 (n = 397).

Note. a Catholic, Wakefeta, b Welayita, TBGH = Tulu Bollo General Hospital.
Obstetric-Related Characteristics of Study Participants
Of the total study participants, 223 (56.2%) and 113 (28.4%) women were in the second and third trimesters of pregnancy, respectively. Two hundred and twenty-five (64.2%) of the study participants were multigravida, and 281 (70.8%) were parous. Regarding pregnancy type, 365 (91.9%) had planned pregnancies. Among unplanned pregnancies,3 (9.4%) experienced unwanted pregnancies. Among the total study participants, 157 (37%) and 112 (28.2%) received second and third antenatal visits, respectively. Three hundred and forty (85.6%) women received care from midwives. Regarding the time to start ANC follow-up, 56 (14.1%) of respondents were late for ANC timing. Two hundred and ninety-one (75.3%) multigravida women had a previous history of minor pregnancy disorders, and among those women who previously experienced minor pregnancy disorders,10 (4.6%) had a history of hospitalization due to minor pregnancy disorders. Regarding counseling on minor pregnancy disorders, 139 (35%) study participants were not counseled on minor pregnancy disorders (Table 2).
Obstetric-Related Characteristics of the Respondents at TBGH, Southwest Shewa, 2022 (n = 397).

Note. a Health post, private clinic.
Knowledge Regarding Minor Pregnancy Disorders of Study Participants
More than half 175 (51.3%) of the study participants were not knowledgeable about minor pregnancy disorders, whereas 166 (48.7%) of the respondents were knowledgeable about minor pregnancy disorders (Table 3).
Knowledge About minor Pregnancy Disorders of Study Participants at TBGH, Southwest Shewa, Ethiopia, 2022.

In the current pregnancy, only 7.0% of respondents received counseling services for the self-management practice of MPD (Figure 1).

Type of services received during antenatal care follow-up at Tulu Bolo General Hospital, Southwest Shewa, Ethiopia, 2022 (n = 341).
Level of Self-Management Practices for Minor Pregnancy Disorders
Out of the total 397 participants, 341 had minor pregnancy disorders, and the self-management practice was computed based on 341 study participants who had minor pregnancy disorders. The overall self-management practice of MDP was found to be 29.3% (95% CI: 24.0%, 34.0%) (Figure 2).
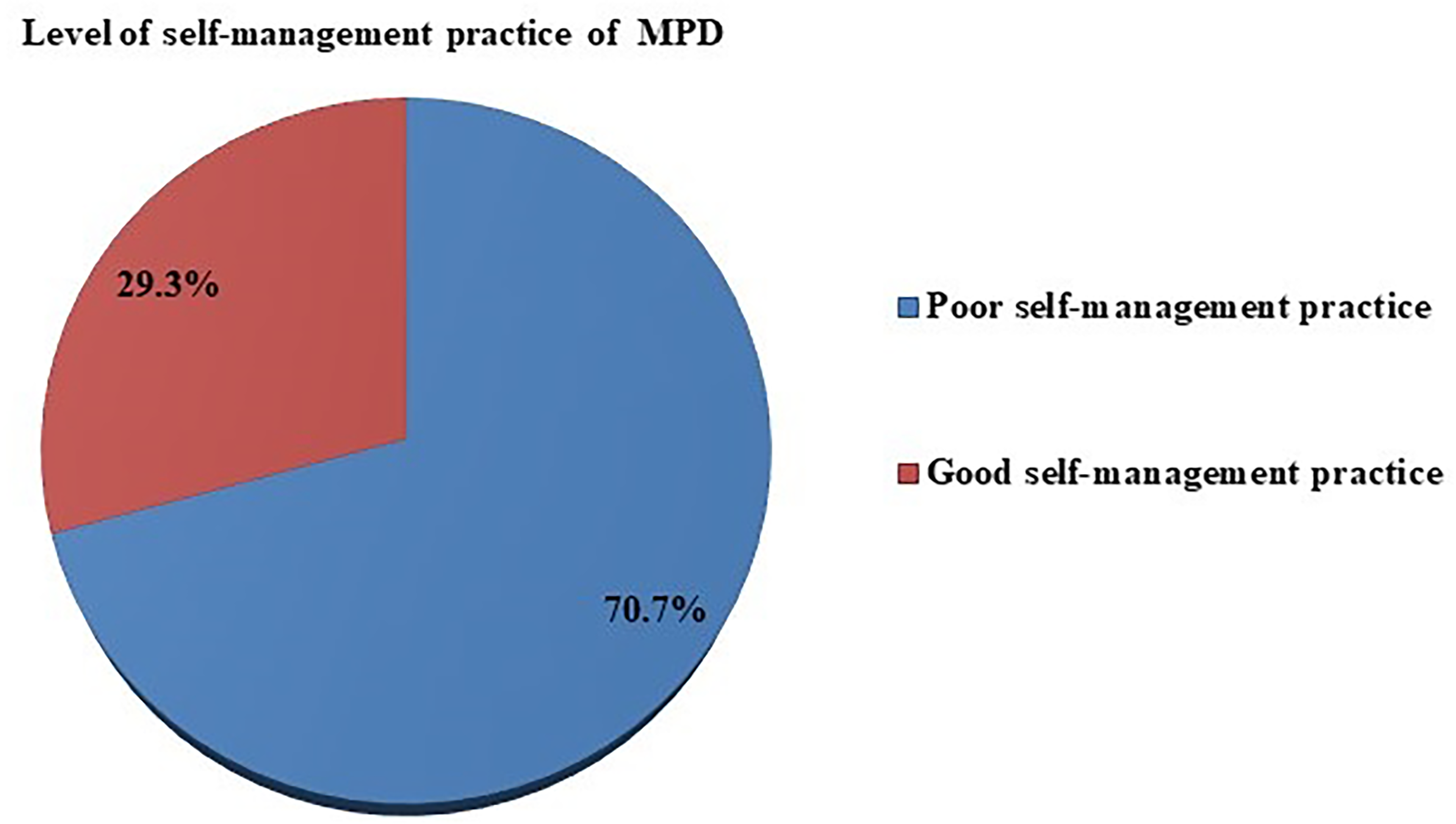
Level of self-management practice among pregnant women who had minor pregnancy disorders at Tulu Bolo General Hospital, Southwest Shewa, Ethiopia, 2022 (n = 341).
Among 341 study participants, 280 (82.1%) of the respondents experienced morning sickness; 140 (50%) and 154 (55%) of them were managed by using ginger and avoiding strong smells, respectively. One hundred and twenty (35.2%) experienced constipation; 66 (55%) of the respondents were managed by diet modification; 279 (81.8%) of the respondents experienced heartburn, and 179 (64.2%) were managed by diet modification.
Factors Associated with the Self-Management Practice of Minor Pregnancy Disorders
Binary logistic regression analysis was done to identify candidate variables for multivariable logistic regression at a P-value of.25, and variables from socio-demographics (age of pregnant women, residence, household wealth status, women's educational status, husband's educational status, women's occupation), from obstetrics-related factors (GA in a trimester and counseling on MPD), and knowledge about minor pregnancy disorders were taken to multivariable logistic regression. In multivariable analysis, five variables, including the age of the pregnant woman, the household's economic situation, the educational level of the women, their occupation, and their knowledge about MPD, were found to be statistically significantly associated with the self-management practice of minor pregnancy disorders after confounders were adjusted in the final model.
Women aged >30 years old were 4.4 times (AOR = 4.4; 95% CI: 1.64, 11.60) more likely to have had good self-management practices towards minor pregnancy disorders as compared to those women whose age <20 years. Pregnant women who attended secondary and above education and primary education were 4.1 and 5.8 times (AOR = 4.11; 95% CI, (1.30, 12.97) and (AOR = 5.88; 95% CI: 2.16, 16.03)) more likely to practice good self-management of minor pregnancy disorders than those who did not attend formal education. Women from rich household wealth quintiles were 3.6 times (AOR = 3.6; 95% CI: 1.68, 7.97) more likely to have had self-management practices towards minor pregnancy disorders than those who were from poor household wealth quintiles. The odds of having a good self-management practice for minor pregnancy discomforts were 2.4 times (AOR = 2.44; 95% CI: 1.09, 5.45) higher in pregnant women who were government employees as compared to homemakers. Women who were knowledgeable about minor pregnancy disorders were two times (AOR = 2.06; 95% CI: 1.12, 3.79) more likely to have had good self-management practices as compared to their counterparts (Table 4).
Factors Associated With the Self-Management Practice of Minor Pregnancy Disorders at Tulu Bollo General Hospital, Southwest Shewa, Ethiopia, 2022 (n = 341).

Note. COR = crude odds ratio; AOR = adjusted odds ratio; CI = confidence interval; 1 = reference; MPD = minor pregnancy disorders; GA = gestational age; SMP = self-management practice.
Statistically significant at P-value < .05.
Discussion
Self-management of minor pregnancy disorders is critical for pregnant women's health. Thus, poor MPD self-management practice is the root cause of major pregnancy complications, which are associated with maternal morbidity and mortality. This facility-based cross-sectional study identifies factors associated with MPD self-management in the study settings. The age of pregnant women, household wealth index, women's educational status, women's occupation, and knowledge of MPD were all associated with the self-management practice of minor pregnancy disorders in this study.
This study found that 70.7% of pregnant women with minor pregnancy disorders lacked good self-management of minor pregnancy disorders. This finding indicated that overall self-management of minor pregnancy disorders was considered poor. This might be due to a lower educational level, less MPD counseling, and a lack of knowledge about minor pregnancy disorders experienced by pregnant women. This finding is supported by a study conducted in Iraq on pregnant women's self-management practices for minor disorders (Aziz & Maqsood, 2016; Fahmy, 2024). The findings of this study were consistent with the findings of the multinational study, which were 28.9% (Kennedy et al., 2013), India, at 28% (Anthrayose, 2016), and Egypt, at 30.8% (El-Sharkawy et al., 2020). It was lower than a Saudi Arabian study's 47.0% (Aldossary et al., 2018). This inconsistency might be attributed to the study participants’ socioeconomic and demographic characteristics, the time interval between studies, and the difference in sample size (small sample size as compared to this study).
The results of this study were higher when compared to studies conducted in Kolar Hospital, India, which was 12% (Rosy, 2014), Hodeida City, Yemen, 5.5% (Youssef, 2019), and Egypt, 4.2% (AbdElhaliem & Mohamed, 2018). This disparity might be attributed to the time interval between studies, socio-demographic study populations, and some methodological features (sampling techniques of study participants, which were probabilistic vs. non-probability sampling techniques, inclusion and exclusion criteria). The self-management practice of minor pregnancy disorders found in this study could be attributed to the Ethiopian government's long-term commitment to maternal health, women's education, and the expansion of health services. The current study included women from both rural and urban areas. It is well known that urban women have a better education, a better economy, and greater access to information. Furthermore, this disparity could be due to a difference in sample size.
This study showed that the age of pregnant women was significantly associated with self-management practices for minor pregnancy disorders. As a result, pregnant women over the age of 30 were more likely to have had good self-management practices for minor pregnancy disorders than those under the age of 20. This might be because as age increases, their experience and exposure to the management of minor pregnancy disorders increase due to frequent contact with health care personnel providing health education that improved their knowledge and the experience to income generating activities rise as well, which in turn leads to an increase in self-care practices (Fahmy, 2024). Young women of reproductive age with low educational levels receive little or no care and are unaware of the importance of self-care during pregnancy(Sen et al., 2012). The study showed that, as age advanced, their knowledge also increased, which increased the experience of self-management (Aldossary et al., 2018; Atiyah & Oleiwi, 2024). In this study, household wealth status emerged as a statistically significant factor for women's self-management practice of minor pregnancy disorders. Women from richer household wealth quintiles had better self-management practices for pregnancy disorders than those who were from poor wealth index households. This finding was supported by studies conducted in Yemen (Youssef, 2019), Saudi Arabia (Aldossary et al., 2018), and India (Patel et al., 2016). The reason for this might be that as the household becomes wealthier, they are more likely to engage in self-management practices during pregnancy. Women with higher socioeconomic status practice better, which may be due to their ability to purchase or provide themselves with pregnancy necessities such as healthy foods, compression stockings, comfortable pillows, and hygiene materials(Aldossary et al., 2018; Patel et al., 2016). Furthermore, pregnant women with better financial circumstances are more likely to live healthy lifestyles (Patel et al., 2016; Youssef, 2019).
This finding showed that pregnant women who attended primary, secondary, or higher education were more likely to have good self-management practices for minor pregnancy disorders than those who did not attend formal education, respectively. This finding is consistent with studies conducted in Saudi Arabia (Aldossary et al., 2018), Iraq (Aziz & Maqsood, 2016), and Yemen (Youssef, 2019). This might be because the more a woman is educated, the more she is aware of the self-management of minor pregnancy disorders. The possible explanation is that educated women are more aware of self-care for pregnancy-related conditions (pregnancy disorders), and they can read pregnancy care books available on the market to learn about pregnancy and manage minor disorders (Atiyah & Oleiwi, 2024; Patil & Salunkhe, 2015).
In this study, a woman's occupation had a significant association with self-management of minor pregnancy disorders. Women who were government employees were more likely to have good self-management practices as compared to homemakers. This finding was supported by a study conducted in Yemen (Youssef, 2019). This might be because those women who are employed can have more information regarding their health and health-related conditions than those who are unemployed. Another explanation could be that being a homemaker is a culturally influenced occupation because women may not continue their education after marriage, which opens the door to becoming an employee (Aziz & Maqsood, 2016). Besides, working women were more knowledgeable than unemployed women (Patel et al., 2016), so they were exposed to a wider range of ideas and health roles, which may change their views about what they should be able to do regarding proper self-care practices.
Women who were knowledgeable about minor pregnancy disorders were more likely to have good self-management practices as compared to poorly knowledgeable women. This finding was in line with studies conducted in Egypt (AbdElhaliem & Mohamed, 2018; Sobhi Ahmed et al., 2022) and Saudi Arabia (Aldossary et al., 2018). Knowledgeable women had good self-management practices as compared to their counterparts. This study was supported by a study conducted in India (Awad et al., 2024; Patil & Salunkhe, 2015). This might be because those women who know minor pregnancy disorders could easily influence and convince their families about the significance of self-management practices related to pregnancy disorders.
The studies revealed that knowledgeable women can cope with, prepared to handle any discomforts and manage minor disorders successfully (Awad et al., 2024; Koonge et al., 2020; Patil & Salunkhe, 2015).
Strengths and Limitations of the Study
Strength of the Study
Measurements of the self-management practice of minor pregnancy disorders included both multigravida and primigravida women.
Up to the knowledge of the investigator, there has been no study conducted in Ethiopia, particularly in the study setting. In this study, potential biases were minimized by using clear objectives, research questions, pretested questionnaires, training provided for the supervisor, data collectors’ random sampling method and ideal sample size, and statistical adjustments (multivariable regression) to account for confounding variables. Finally, ethical guidelines were implemented to ensure unbiased participants.
Limitations of the Study
This study has the same limitations as other studies that are based on cross-sectional data.
There is a possibility of recall bias among study participants on the self-management practice of minor pregnancy disorders since the study was self-reported.
Since the cross-sectional study, the study does not show cause-and-effect relationships.
Implications for Practice
Even though minor pregnancy disorders cannot be avoided, good care can slow their progression and prevent further complications. The findings of this research have many implications for enhancing the self-management of minor pregnancy disorders. The study showed that 70.7% of pregnant women lacked good self-management of minor pregnancy disorders. Again, the study revealed that the factors associated with self-management of minor pregnancy disorders among pregnant women provide important information for Woredas, Zonal health offices, Hospitals, and Health Care Providers to improve the self-care status of women with minor pregnancy disorders. Nurses/Midwives are among the health workers who play an important role in enhancing awareness of pregnant women regarding knowledge of minor pregnancy disorders and their self-management practice.
This indicated the need for an ongoing plan for supportive self-management practice and effective Nurse/Midwife/education at the institutional and community levels (by Health extension workers) by developing a self-learning module or guidelines by the Ministry of health to counsel pregnant women about minor disorders and their management options. Finally, Nursing/midwifery researchers can use this study as input, explore other factors associated with self-management practice at a different level, and create an interventional project on modifiable factors affecting Minor pregnancy disorders self-management practices.
Conclusion and Recommendations
Conclusion
This study showed that 70.7% of pregnant women lacked good self-management practices for minor pregnancy disorders. Women's primary role in minor pregnancy disorders self-management is to improve their well-being and, indirectly, that of their fetuses and families. The ages of pregnant women, household wealth status, women's education, women's occupation, and being knowledgeable regarding minor pregnancy disorders were significantly associated with their self-management practices of minor pregnancy disorders. As a result, the study concludes that by intervening in the modifiable factors, pregnant women's awareness regarding self-management practices can be increased.
Recommendations
The following recommendations were given based on the above results to the concerned bodies:
To the Ministry of Education: Facilitate means to enhance pregnant women's education and knowledge level through strengthening public education that targets improving the level of self-management practice of minor pregnancy disorders.
To regional, zonal, and Woredas health offices: The health office should work to improve the self-management practice of MPD among women by enhancing health education and income levels through various programs such as having women's conferences at the health facility and delivering information via local media.
To encourage in-service training for pregnant women during ANC to update their knowledge, improve their ability to care for themselves, enhance self-management practices, and avoid unhealthy lifestyle practices.
At the community level: It is encouraged in the area to participate in improving women's self-management practices for minor pregnancy disorders by improving their educational status and thinking about proper home remedies for self-management as a culture.
To TBGH and health care providers: It is encouraged to extend health education and counseling to enhance pregnant women's self-management of minor pregnancy disorders.
To design a health education program on minor pregnancy disorders and their management strategies at both the facility and community levels.
For the researcher: A longitudinal study and qualitative study need to be done to identify important factors and a better understanding of women's self-management practices of minor pregnancy disorders with a large sample size. Besides, the current study recommends further research to investigate the unsafe practices related to minor discomforts during pregnancy and their effect on the mother and fetus.
Supplemental Material
sj-docx-1-son-10.1177_23779608251345324 - Supplemental material for Self-Management Practice of Minor Pregnancy Disorders and Associated Factors Among Pregnant Women Attending Antenatal Clinics at Tulu Bolo General Hospital, Ethiopia
Supplemental material, sj-docx-1-son-10.1177_23779608251345324 for Self-Management Practice of Minor Pregnancy Disorders and Associated Factors Among Pregnant Women Attending Antenatal Clinics at Tulu Bolo General Hospital, Ethiopia by Mangistu Abera, Aynalem Belay, Aberash Beyene Derribow, Girma Bacha and Sena Belina in SAGE Open Nursing
Supplemental Material
sj-pdf-2-son-10.1177_23779608251345324 - Supplemental material for Self-Management Practice of Minor Pregnancy Disorders and Associated Factors Among Pregnant Women Attending Antenatal Clinics at Tulu Bolo General Hospital, Ethiopia
Supplemental material, sj-pdf-2-son-10.1177_23779608251345324 for Self-Management Practice of Minor Pregnancy Disorders and Associated Factors Among Pregnant Women Attending Antenatal Clinics at Tulu Bolo General Hospital, Ethiopia by Mangistu Abera, Aynalem Belay, Aberash Beyene Derribow, Girma Bacha and Sena Belina in SAGE Open Nursing
Footnotes
Abbreviations
Acknowledgments
The authors would like to thank Jimma University for giving us the opportunity to conduct the research and for granting ethical approval. Authors also extend our gratitude to study participants, data collectors, and supervisor for their unreserved efforts and willingness to participate in this research study.
Ethical Approval and Consent to Participants
Ethical clearance was obtained from the Jimma University Institutional Review Board (JUIRB) Institute of Health, and Faculty of Health Science (Ref. No. JUIRB /92/2022). The study was conducted following the ethical standards of the Declaration of Helsinki. An ethical letter was written to Tulu Bollo General Hospital to obtain permission for data collection. The purpose of the study and participants’ right to refuse was explained to the study participants and informed written consent was obtained. Additionally, informed consent was gathered from parents or guardians of participants under 18 years old. Coding was implemented to remove respondents’ names and other personal identifiers throughout the study to ensure participant confidentiality. Furthermore, COVID-19 prevention measures were implemented.
Author Contributions
MA wrote the proposal, participated in data collection supervision, analyzed the data, and drafted the paper. MA, SB, AB, and GB approved the proposal with some revisions, participated in data analysis, and revised subsequent paper drafts. MA, ABD, and SB commented on the final paper and manuscript. All authors read and approved the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data that support the findings are available from the corresponding author upon a reasonable request.
Informed Consent
Written informed consent was obtained from all study participants.
Supplemental Material
Supplemental material for this paper is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.