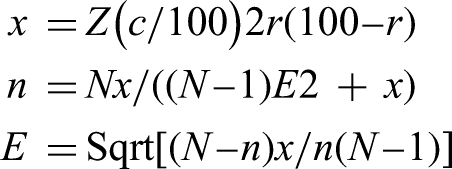Abstract
Introduction
Self-medication (SM) is a practice wherein an individual consumes medicines without consulting a physician. This growing practice can lead to serious consequences, such as adverse drug reactions or treatment failure. Evidence suggests that SM is particularly common among young adults.
Objective
To assess the patterns and knowledge of SM among undergraduate health sciences students.
Methods
The cross-sectional study was conducted on 571 undergraduate health sciences students from January to March 2023. Data on SM practices and associated factors were collected using a self-administered questionnaire. A convenient sampling method was employed to recruit the students. The collected data were analyzed using descriptive and inferential statistics with SPSS software.
Results
Self-medication was reported by 83.5% of participants. Knowledge of SM was satisfactory in 56% and unsatisfactory in 44%. Practice scores were unsatisfactory in 70% and satisfactory in 30%. Pharmacies (61.1%) and the Internet (53.5%) were the main information sources. Significant correlations were found between SM and chronic disease (χ2 = 10.846, p = .0009) and lack of medical insurance (χ2 = 84.175, p = .0001). Painkillers and antipyretics were the most commonly used SM drugs with 51.7% and 45.4%, respectively. Chronic diseases were reported by 8% of participants, of which 27.1%, 18.8%, 22.9%, and 31.2%, reported glucose-6-phosphate dehydrogenase deficiency, hypothyroidism, asthma, and anemia, respectively.
Conclusion
A significant proportion of the respondents practice SM. Although knowledge of SM was satisfactory, it is recommended to be aware risks of SM among students and enforce stricter supervision on the sale of over-the-counter drugs.
Keywords
Introduction
Self-medication (SM) is a practice where an individual takes medications without the advice or prescription of a physician. This phenomenon has been on the rise globally and is particularly prevalent among young adults including university students. SM can have serious consequences, such as adverse drug reactions, increased resistance to antibiotics, and the risk of misdiagnosing oneself, which may lead to inappropriate treatment and exacerbation of underlying conditions (Hamza, 2019). Medical students feel confident in their ability to self-diagnose and treatment regimen, hence SM practice is more prevalent among these students as suggested by the literature (Hiremath et al., 2021; Khatony et al., 2020). Despite this confidence, the knowledge base and decision-making processes of these students may still be insufficient to alleviate the risks associated with SM.
Review of Literature
Although many studies have been conducted on the prevalence of SM, comprehensive information on its global prevalence across all medications and health conditions remains limited (Daanish & Mushkani, 2022). SM is commonly used to address conditions, such as headache, common cold, fever, cough, and respiratory tract infections. Explanations for SM practices include previous experience with the illness, mildness of the disease, time constraints preventing professional consultation, and cost-effectiveness (Zeru et al., 2020). SM practice is influenced by sociodemographic factors such as gender, age, income, level of education, residence, religion, study year, field of study, and marital status (Behzadifar et al., 2020; Janatolmakan et al., 2022). Patients often obtain SM drugs from pharmacies, unused home medications, friends, and relatives, with these sources significantly contribute to SM prevalence. Information sources like healthcare professionals, pharmacists, reading materials, and social circles also influence SM practice; Helal & Abou-ElWafa, 2017; Zeru et al., 2020).
Study design, participants’ age, gender differences, and drug classifications (OTC or prescription) vary between countries, influencing SM prevalence among university students (Behzadifar et al., 2020; Orayj et al., 2021). In Saudi Arabia, studies have been conducted among medical and nursing students at various universities, but few have comprehensively addressed SM among health sciences students (Alshahrani et al., 2019; Essa et al., 2018; Faqihi & Sayed, 2020; Shatla et al., 2022). This stresses the need for understanding the practices of SM. Hence, the current study was undertaken to evaluate the prevalence, patterns, and knowledge of SM among undergraduate health sciences students. No such studies have focussed on health sciences students at the area of the authors. So, the objective of this study is to assess SM patterns and knowledge among undergraduate health sciences students.
Methods
Study Design and Setting
The cross-sectional study was conducted in the College of Applied Medical Sciences from January to March 2023. The college comprises four departments. Nursing, Public Health, Clinical Nutrition, and Health Informatics.
Study Sample
A convenience sampling technique was used to recruit the study participants from all four departments. The sample size of the study was calculated using Raosoft® Sample Size Calculator (Sample Size Calculator; Raosoft inc.) :
where Z(c/100) is the critical value of the confidence level c, N is the population size, E is the margin of error, r is a fraction of responses, and n is the sample size. Assuming 5% margin of error and non-response rate at 95% confidence interval (CI), the study sample size was estimated 571.
Inclusion and Exclusion Criteria
The study included undergraduate students who were enrolled in health sciences programs; who provided informed consent and were proficient in English and Arabic. It excluded students who did not provide or withdrew consent or those who submitted incomplete or inconsistent responses. The students who were on long-term prescription medications for chronic conditions were not considered in the study.
Data Collection Instrument and Procedure
After reviewing the relevant literature (Bhattarai & Karki, 2020; Esan et al., 2018; Subashini & Udayanga, 2020), a self-administered questionnaire was developed in English on SM practices as the data collection instrument. The English version of the questionnaire was also translated into Arabic by a language expert. Respondents were given the option to choose between the English and Arabic versions based on their comfort level of understanding between English and Arabic. The data were collected by sending the questionnaire to the targeted respondents through social media channels like WhatsApp, X (Twitter), Telegram, email, or through student representatives. Additionally, students were approached at the end of their scheduled classes for data collection.
At the end of the response, the Arabic version was translated back to English to maintain constancy. The questionnaire comprised four sections : (1) sociodemographic characteristics (e.g., age, marital status, gender, academic year, field of study); (2) 11 items on students’ knowledge of SM (e.g., safe usage, harmful consequences, side effects, and non-steroidal anti-inflammatory drugs [NSAIDs]); (3) nine items on SM practices (e.g., reading medication leaflet before self-medicating, following the dosage directions, the last time the participant self-medicated, who determined the SM dose, and side effects from SM); and (4) 28 items on other factors associated with SM. The latter addressed sources of SM information (seven items), sources for purchasing SM drugs (five items), types of medications used for SM (eight items), and reasons for self-medicating (eight items). The associated factors section included yes/no or multiple-choice questions.
For the first three sections, participants were scored on a 5-point Likert scale; positive items were scored at strongly agree = 5 points, agree = 4 points, neutral = 3 points, disagree = 2 points, and strongly disagree = 1 point, with reverse scoring for negative items. An overall score of 55, with a cutoff value of 33 (≥60.0%), was considered satisfactory, while scores below 60.0% were unsatisfactory.
Validity and Reliability
The questionnaire underwent testing in a pilot study involving 5% (n = 29) of study prospective participants, who were subsequently excluded from the final sample. To evaluate its clarity and applicability, Cronbach's α coefficient was employed to assess the questionnaire's reliability across its sections. Additionally, content validity was verified by six experts representing various fields: two professors each from Clinical Pharmacy, Medical-Surgical Nursing, and Nursing Administration. Their feedback informed modifications to the questionnaire. Results indicated Cronbach's α coefficients of .752 for knowledge, .891 for practice, and .752 for associated factors, demonstrating satisfactory internal consistency. Furthermore, the content validity/Kaiser–Meyer–Olkin (KMO) index values for these respective sections were .912, .889, and .765, affirming the questionnaire's reliability and suitability for achieving the study objectives.
Data Analysis and Management
The data were collected and anonymized to maintain the data confidentiality. Each data set was entered into Microsoft Excel 2021 version (Microsoft, Inc., USA) for further analysis. The data analysis was conducted in collaboration with a statistician using SPSS software version 24 (IBM Corp., Armonk, NY, USA). Descriptive statistics was carried out to present the data in percentages and frequencies. Pearson's correlation coefficient and the chi-square test were employed to ascertain associations between sociodemographic characteristics and SM usage. The strength of the associations was denoted by the adjusted odds ratio (OR) with a 95% CI. Regression analysis was carried out to find association between demographic variables and SM practice. A significance level of p ≤ .05 was considered statistical significance. The data were presented as M ± SD, wherever applicable.
Ethics Approval and Consent to Participate
Ethical approval was taken from the research ethics committee at local university. The confidentiality of the study participants was maintained throughout the study. All the participants were briefed about the study objectives and a written informed consent was obtained from all the respondents.
Results
Sociodemographic Characteristics of the Study Participants
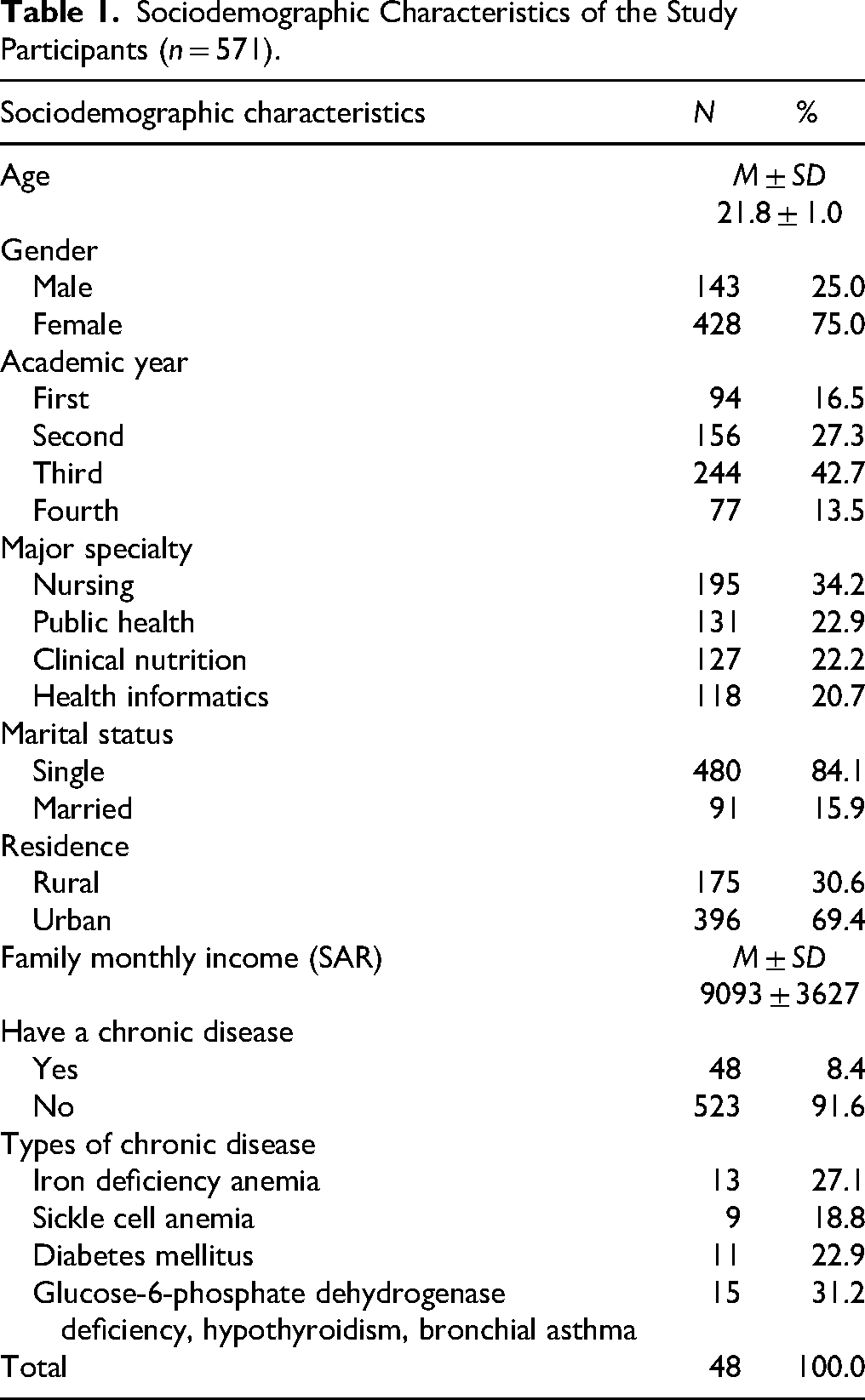
Seventy-five percent of the respondents were identified as female. The average age of participants was 21.8 years. The distribution of participants by academic year was as follows: 94 were in their first year, 156 in their second year, 244 in their third year, and 77 in their fourth year (Table 1). Regarding academic majors or specialties, 34.2% were in Nursing, 22.9% in Public Health, 22.2% in Clinical Nutrition, and 20.7% in Health Informatics. The majority of participants reported being single (84.1%) and residing in urban areas (69.4%). The mean monthly family income was 9093 Saudi Riyal. Eight percent of respondents reported having chronic diseases, with the most common being glucose-6-phosphate dehydrogenase deficiency, hypothyroidism, asthma, and anemia (27.1%, 18.8%, 22.9%, and 31.2%, respectively) (Table 1).
Sociodemographic Characteristics of the Study Participants (n = 571).

Use of Self-Medication Drugs Among the Study Participants
Approximately 83.5% of study participants reported engaging in SM (Figure 1).

Use of self-medication drugs among the study participants (n = 571).
Self-Medication Knowledge Scores Among Participants
The majority of respondents (56%) possessed satisfactory knowledge about SM, while 44% had unsatisfactory knowledge (Figure 2).

Total self-medication knowledge scores among participants (n = 571).
SM Practices Among Participants
However, 70% reported unsatisfactory SM practice scores, and only 30% reported satisfactory practice scores (Figure 3).

SM practices among participants (n = 571).
Knowledge Score and Frequency Distribution About Self-Medication Practice Among Respondents
The analysis of respondent's attitudes and knowledge toward SM practices revealed that a significant proportion expressed awareness of potential risks associated with OTC medication, with 67.45% disagreeing or strongly disagreeing that overusing OTC drugs is safe (Table 2). About 60.61% agreed or strongly agreed that using OTC drugs can hide the real disease behind the symptoms. Despite acknowledging the affordability and availability of OTC drugs in Saudi Arabia, with 57.79% disagreeing or strongly disagreeing that all people use them for this reason, respondents did not universally endorse their use based on these factors. Furthermore, while 52.5% agreed or strongly agreed that they follow dosage directions correctly, 52.25% also agreed or strongly agreed that they use OTC drugs during stress times, suggesting potential misuse (Table 2).
Knowledge Score and Frequency Distribution About Self-Medication Practice Among Respondents (n = 571).

Note. OTC, over the counter.
χ2 = 2.787; p = .097.
Associated Factors That Influence the Practice of Self-Medication Among the Study Participants
Pharmacies and the internet were the most common sources of SM information, cited by 61.1% and 53.5% of respondents, respectively (Table 3). These were followed by social media (32.6%) and previous prescriptions from doctors (32.5%). The least common source was textbooks, reported by only 6.5% of respondents. Regarding the sources of SM drugs, 77.6% of respondents obtained these from pharmacies or leftover medications from previous prescriptions (Table 3). Painkillers and antipyretics were the most commonly used SM drugs (51.7% and 45.4%, respectively), followed by eye drops (43.1%) and drugs for cough/runny nose (35.2%). Participants cited various reasons for self-medicating: relief of minor illness (45.2%), seeking quick relief (44.1%), having previous experience with a particular illness and self-treating with SM (35.4%), avoiding long waits at clinics (26.3%), urgency of illness (22.8%), a desire to enhance academic performance (19.6%), high cost of medical consultations (13.0%), and avoiding embarrassment (10.9%) (Table 3).
Associated Factors That Influence the Practice of Self-Medication Among the Study Participants (n = 477).

Note. The symbol # indicates the numbers do not add to 100% as participants might have more than one answer.
Bivariate Analysis of Sociodemographic Characteristics of Study Participants and Self-Medication
Following regression analysis, this study found no statistically significant correlations between SM and gender (χ2 = 0.410, p = .522), academic year (χ2 = 2.099, p = .552), specialty (χ2 = 3.670, p = .299), marital status (χ2 = 2.358, p = .125), residence (χ2 = 0.869, p = .351), or income (χ2 = 2.974, p = .226) (Table 4). In contrast, the study results indicated highly significant correlations between SM and chronic disease (χ2 = 10.846, p = .0009) as well as the absence of medical insurance (χ2 = 84.175, p = .0001) (Table 4).
Bivariate Analysis of Sociodemographic Characteristics of Study Participants and Self-Medication.

Note: **, statistically significant at p ≤0.01
Discussion
The integration of SM into many healthcare systems worldwide offers social and economic benefits but also poses several risks (Daanish & Mushkani, 2022; Olorunfemi et al., 2020). The present study aimed to determine the prevalence of SM among undergraduate health sciences students at the College of Applied Medical Sciences and to gather and analyze data on their SM practices. The study findings revealed an SM prevalence of 83%, consistent with similar studies in Riyadh, Saudi Arabia (80%), Iran (81%), and Pakistan (81.28%). This rate was higher than the King Saud University (50.9%) and Jazan University (43%), but lower than King Khalid University (98.7%) and Brazil (97.9%) (Alshahrani et al., 2019; Colares et al., 2019; Faqihi & Sayed, 2020).
Health sciences students often self-medicate due to the availability of OTC drugs and the accessibility of community pharmacies (Orayj et al., 2021). Painkillers, antipyretics, and eye drops were the most frequently used SM drugs, mainly for treating fever, chills, headache, common cold, throat inflammation, and gastric pain. These findings align with previous research indicating that headaches and fever are common reasons for SM (Aashi et al., 2016; Colares et al., 2019). Other reasons include allergies, digestive disturbances, and sleep problems (Aashi et al., 2016).
Health sciences students generally had satisfactory knowledge of SM, with studies from Pakistan, Iraq, and Saudi Arabia (Essa et al., 2018; Ramadan, 2022) confirming this. Their education includes drug-related courses that enhance their understanding of drug consumption, although personal attitudes toward symptoms, diagnosis, and treatment also play a role (Bekele et al., 2020).
Participants primarily self-medicated to relieve minor illnesses, seek quick relief, and due to prior experience with specific illnesses and treatments. This is similar to findings from studies by Misau et al. (2020), Helal and Abou-ElWafa (2017). Medical students at Umm Al-Qura University in Makkah also cited avoiding doctor visits for minor illnesses and using knowledge from previous experience (Shatla et al., 2022).
Despite their knowledge, respondents reported unsatisfactory SM practices, possibly due to pharmacies not adhering to regulations and the lax enforcement of restrictions (Alshahrani et al., 2019). This situation is common in many Arab and developing countries and may influence SM practices (Bekele et al., 2020; Mkola et al., 2022). Bhattarai and Karki (2020) noted that medical students’ perceived expertise could lead to poor practices with serious consequences, possibly due to their belief in their ability to self-diagnose and self-treat (Colares et al., 2019). Most participants had not experienced side effects from SM, consistent with Karimy et al. (2019), who reported that responsible SM can offer benefits like shorter waiting times and cost savings. However, these findings differ from a Saudi study reporting side effects such as drowsiness, loss of appetite, runny nose, itchy skin, and diarrhea (Mirdad et al., 2023).
Common sources of SM information included pharmacies, the internet, social media, and previous prescriptions. A study among Saudi undergraduate medical students found friends and relatives to be common sources, followed by physicians, pharmacists, parents, and the internet (Shatla et al., 2022). Similar findings were reported among Indian medical students (Mathewos et al., 2021). Access to information via the internet helps users understand disease symptoms and treatments, supporting findings by Karimy et al. (2019). Previous prescriptions also facilitate SM due to their availability and accessibility (Alshogran et al., 2018). Today's youth, exposed to pharmaceutical advertising online and through other media, may benefit from visiting medical websites and viewing educational advertisements (Alshogran et al., 2018; Alyahya et al., 2017; Naqvi et al., 2018).
There was a significant correlation between SM and having a chronic disease, consistent with Subashini and Udayanga (2020) who noted that chronic conditions are often associated with SM. Health personnel may self-medicate due to easy access to drugs and a positive view of SM, but risky practices can lead to prolonged illness, adverse reactions, and antimicrobial resistance.
No significant difference was found between gender and SM, potentially due to similar knowledge levels among educated participants. This contrasts with findings by Shawi et al. (2018), who reported higher SM rates among male students. Other studies have shown that men self-medicate more than women in South Karnakata, India, and Saudi Arabia (Mathewos et al., 2021). Misau et al. (2020) suggested that higher SM rates among females might be due to their greater vulnerability to stress and anxiety. Zeru et al. (2020) identified gender, income, year of study, and field of study as significant factors affecting SM. Socioeconomic status did not significantly impact SM usage, contrary to findings by Mathewos et al. (2021) and Behzadifar et al. (2020), which indicated higher SM prevalence in high-income countries. SM might be an option for individuals with lower Socioeconomic status who cannot afford medical care, given the increased accessibility of drugs today, which poses health risks if not managed properly. Most students reported knowing the risks of using non-prescription medications (NPMs) but continued to use them, possibly due to experimentation with drugs relevant to their future professions and the ease of access during training at health centers (Behzadifar et al., 2020).
Strengths and Limitations
Each study has its own strengths and limitations. This study has several limitations, such as the reliance on self-reported data for assessing self-medication practices, which may introduce bias. Without longitudinal data, it is difficult to assess changes in self-medication practices over time or the long-term impact of these practices on health outcomes. Participants might have provided responses they perceived as more socially acceptable or expected, leading to potential bias. The cross-sectional nature of the study limits the ability to establish causality between sociodemographic factors and self-medication practices. Additionally, although the electronic survey tool was online and anonymous, it still had some disadvantages, such as bias in reporting the types of drugs used for self-medication.
This study offers several unique strengths that enhance its contribution to understanding self-medication (SM) practices among health sciences students. Unlike other studies that provide a general overview, the current study includes a comprehensive demographic breakdown, which is often missing in similar studies that typically focus on SM rates and types of medications used. Additionally, this study uniquely identifies the prevalence of specific chronic conditions among participants, shedding light on the particular health challenges they face and their impact on SM practices. This study also provides a more refined breakdown of information sources, including social media and previous prescriptions from doctors, offering a broader perspective. Furthermore, this study assesses both knowledge and practices regarding SM, differentiating between satisfactory and unsatisfactory levels, an approach rarely seen in other studies. Finally, the current study details specific medications used and reasons for SM, adding depth to the understanding of SM practices compared to other studies.
Implications for Nursing Practice
Nursing practice can be significantly affected by self-medication. Here are some key points.
Patient safety: Nurses are responsible for educating patients on safe medication practices and recognizing the risks of self-medication, including adverse drug reactions, interactions, and incorrect dosing.
Assessment and monitoring: Regular monitoring by nurses can assist in identifying potential issues early by assessing patients’ medication use habits, which includes over the counter and herbal supplements.
Communication: To avoid drug interactions and make informed care decisions, nurses must encourage open dialogue about all the substances a patient is taking.
Consideration of legal and ethical issues: It is important for nurses to be aware of the legal and ethical consequences of self-medication, which involve ensuring that patients follow prescribed treatments and comprehend the risks of not doing so.
Conclusions
This study provides detailed understandings of SM practices among undergraduate health sciences students at the College of Applied Medical Sciences. With a high prevalence of 83%, the findings reveal a mixed understanding of SM behaviors. The practice was influenced by easy access to pharmacies and over-the-counter medications. The correlation between chronic diseases and SM, along with the lack of significant differences based on sociodemographic factors, underscores the complexity of SM behaviors. Although this study is limited by self-reported data, this research contributes to a deeper understanding of SM practices, promoting for greater regulatory measures and educational programs for safer SM practices among future healthcare professionals. Based on the study findings, the researchers recommend establishing behavioral programs to control irresponsible SM practices among students, developing policies and legislation to regulate the purchase of drugs from community pharmacies without a prescription, particularly those deemed safe for use by the general population, and conducting further studies to estimate the prevalence of SM among health sciences students in other cities and to investigate the various factors influencing its use in this population, including awareness and an understanding of its benefits and drawbacks.
Supplemental Material
sj-docx-1-son-10.1177_23779608251330865 - Supplemental material for Self-medication Patterns and Knowledge Among Undergraduate Health Sciences Students: A Cross-Sectional Study
Supplemental material, sj-docx-1-son-10.1177_23779608251330865 for Self-medication Patterns and Knowledge Among Undergraduate Health Sciences Students: A Cross-Sectional Study by Abeer Mohamed Abdelkader, Ghadeer Taher Alhassan and Wejdan Bader Albukhaytan, Esraa Ahmed Alnoubi, Wadha Nasser AlRasheedi, Eman Ali Alomran in SAGE Open Nursing
Footnotes
Ethics Approval and Consent to Participate
Ethical approval was obtained from the research ethics committee at KFU (Reference number: KFU-REC-2023-JAN-ETHICS477). The confidentiality of the study participants was maintained throughout the study. All the participants were briefed about the study objectives, and written informed consent was obtained from all the respondents.
Author Contributions/CRediT
Conceptualization: AMA, WNA, and GTA. Formal analysis: AMA, WNA, and GTA. Investigation: EAA, EAA, and WBA. Methodology: EAA, EAA, and WBA. Data curation: GTA, EAA, EAA, and WBA. Funding acquisition: AMA, EAA, and EAA. Supervision: WNA, GTA, and WBA. Writing—original draft preparation: AMA, WNA, EAA, and EAA. Writing—review and editing: AMA, GTA, and WBA. Each author has reviewed and accepted the published version of the article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Deanship of Scientific Research, Vice Presidency for Graduate Studies and Scientific Research, King Faisal University, Saudi Arabia [Grant No. A485].
Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
Data of this study are available from the first author upon request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.