Abstract
Background
Alcohol use in early pregnancy increases the risk for Fetal Alcohol Spectrum Disorders. Women who engage in heavy drinking and become pregnant when they are not actively trying to conceive are at heightened risk for alcohol-exposed pregnancies. Identifying factors associated with greater risk for alcohol-exposed pregnancies is critical for prevention.
Objective
This study explored the odds of contraceptive nonuse and heavy drinking for women trying to conceive or ambivalent about pregnancy as compared to those trying to avoid pregnancy.
Methods
Logistic regression analysis was used to examine the role of pregnancy intentions, including ambivalence, on contraceptive nonuse and heavy drinking among a national sample of 583 sexually active heterosexual women of childbearing age conducted online in 2024.
Results
Results showed that women who are trying to conceive or are ambivalent about pregnancy have higher odds of contraceptive nonuse than women trying to avoid pregnancy (OR = 13.19, p < .01 and OR = 3.56, p < .001, respectively), but no significant differences in heavy alcohol use by pregnancy intention.
Conclusion
Pregnancy intentions are associated with contraceptive nonuse but not heavy alcohol use. Delayed pregnancy recognition among those not actively trying to conceive but also not consistently using an effective form of contraception might place women who are avoiding or ambivalent about pregnancy at heightened risk for an alcohol-exposed pregnancy.
Keywords
Introduction
Estimates of global prevalence of women's alcohol consumption vary greatly by region (WHO, 2018). Although men consume alcohol more frequently and in greater quantities compared to women, the “gender gap” in global alcohol consumption has narrowed over time due to sharp rises in women's alcohol use (Slade et al., 2016; White, 2020). In 2017, more than half (58.2%) of nonpregnant U.S. women aged 18–44 years old reported alcohol use in the past month (Hasin et al., 2019). Similar to global patterns, between 2002 and 2012, rates of heavy and binge drinking among U.S. women increased by more than 50% (Grant et al., 2017), with peak episodic alcohol consumption occurring during childbearing years (Dwyer-Lindgren et al., 2015). During the COVID-19 pandemic, U.S. women reported significantly higher increases in alcohol consumption than men (Barbosa et al., 2023). Whereas U.S. men's alcohol use declined during the pandemic, U.S. women's increased alcohol consumption in recent years has remained stable (Tucker et al., 2022).
About 10% of women worldwide consume alcohol during their pregnancies (Popova et al., 2017). Rates are similar in the United States; approximately 13.5% of pregnant adults reported current drinking during pregnancy between 2018 and 2020 (Gosdin et al., 2022). Although most women in the United States who consume alcohol stop drinking while pregnant, up to half fail to meet alcohol cessation guidelines prior to conception (DeJong et al., 2019). Alcohol use in early pregnancy increases the risk for Fetal Alcohol Spectrum Disorders (FASD). In particular, heavy alcohol use, defined as four or more drinks per day or eight or more drinks per week, is associated with a higher risk for FASD outcomes (Roozen et al., 2018). Up to 5% of U.S. children are affected by FASD, resulting in an estimated 187,500 affected infants in 2019 (May et al., 2018). The cost of FASDs globally in 2018 was estimated at $22,810 per child and $24,308 per adult, annually (Greenmyer et al., 2018).
Despite widespread knowledge about the potential impact of alcohol exposure in pregnancy, more than a third of childbearing-aged women in the United States do not use contraception (Daniels & Abma, 2020), and their alcohol consumption has increased in recent decades (McKetta et al., 2022). These trends suggest a substantial and growing public health concern for alcohol-exposed pregnancies (AEP) and their associated consequences. Identifying factors associated with heightened risk for AEP is critical for prevention. In this study, logistic regression was used to examine the role of pregnancy intentions, including ambivalence, in contraceptive and alcohol use behaviors among a national sample of 583 sexually active heterosexual women of childbearing age. The objective of the study was to better understand the salience of intentions, particularly ambivalence, to potentially identify a new target for the prevention of AEP.
Literature Review
Unintended Pregnancies and Delayed Pregnancy Recognition
Although modern forms of contraception are highly effective for preventing pregnancy, only about 65% of reproductive-aged women in the United States use contraception in a given month, and effectiveness varies by method and consistency of use (Daniels & Abma, 2020). The majority (87%) of women in the United States who consume alcohol stop drinking while pregnant, but up to half of all women fail to meet guidelines to stop prior to conception (DeJong et al., 2019). Moreover, pregnant women generally do not stop drinking until their pregnancy is confirmed (Cannon et al., 2015; DeJong et al., 2019). Prior studies indicate that during early pregnancy, even women who were trying to conceive consumed alcohol at virtually the same rate as those who did not intend pregnancy (55% and 56% of intended and unintended pregnancies, respectively) (Pryor et al., 2017). Nearly half (45%) of all pregnancies in the United States are unintended (Finer & Zolna, 2016). Unintended pregnancies are at greater risk for AEP because there is delayed pregnancy recognition (recognition at 7.2 weeks on average versus 5.2 weeks for intended pregnancies, respectively) (Ayoola, 2015). By the 7th week of gestation, the majority of embryonic development has already been completed (Floyd et al., 1999).
Pregnancy Ambivalence
Whereas prior investigations of the role of pregnancy intentions for AEP risk generally divide pregnancy intentions into dichotomous categories of intended versus unintended or planned versus unplanned/unwanted (e.g., Corrales-Gutierrez et al., 2020; Terplan et al., 2014), many pregnancies are neither planned nor unplanned. Nearly a quarter of U.S. women identify themselves as “okay either way” about becoming pregnant (McQuillan et al., 2011), which is generally referred to as “ambivalence” in the literature (e.g., Santelli et al., 2009; Shreffler et al., 2015). Women who are ambivalent about becoming pregnant reports low rates of contraceptive use (Miller et al., 2013; Shreffler et al., 2020), but their alcohol use behaviors have not been examined in prior research. Notably, pregnancy ambivalence has been associated with adverse birth outcomes including preterm delivery and low birthweight (Mohllajee et al., 2007; Rajendran et al., 2021). Ambivalence about pregnancy heightens concerns about AEP risk; although contraceptive use is low among those who are ambivalent, they might not be actively looking for signs of a pregnancy. The current study explored the role of pregnancy intentions in heavy alcohol use and contraceptive behaviors.
Methods
Study Design
This study used a cross-sectional, internet-based survey with age, sex, and race stratification to reflect the makeup of the general U.S. population, conducted in May 2024. The study examined contemporary reproductive attitudes and reproductive and health-related behaviors in 2,145 U.S. male and female adults of reproductive age (see Shreffler, 2024 for the survey instrument). The survey was programmed into Qualtrics and distributed to potential participants through Prolific, an established platform for academic survey research (Peer et al., 2017). The participants were paid $10/hr to complete the online survey (20 min average length).
The independent variable in the current study is pregnancy intendedness. To measure pregnancy intendedness, the following question from the National Survey of Fertility Barriers (McQuillan et al., 2011) was used that asked women about their current reproductive behaviors: “Currently, would you say you are trying to get pregnant, trying NOT to get pregnant, or okay either way?” Responses were coded as dummy variables for “Trying” (i.e., trying to get pregnant) and “Ambivalent” (i.e., okay either way), as compared to those who are “Avoiding” (i.e., trying NOT to get pregnant) as the reference group.
The outcomes of interest were contraceptive nonuse and heavy alcohol use. Contraceptive nonuse was coded as 1 if participants reported that they used contraception rarely or never when asked, “How often when you are sexually active do you use birth control,” or if the method they reported from a drop-down list when asked, “What type of birth control do you typically use?” is not considered to be highly effective (e.g., barrier methods, withdrawal, and fertility awareness-based methods; ACOG, 2021). Participants were coded as 0 if they reported consistent use (e.g., often or always) of a highly effective method (e.g., hormonal birth control pills, long-acting reversible contraception; ACOG, 2021). Heavy alcohol use was coded as a dichotomous variable where 1 indicated self-reported drinking at least four drinks per day or eight drinks per week and 0 as less than four drinks per day or eight drinks per week. Sociodemographic variables included in the analyses were age measured as a continuous variable ranging from 18 to 50, race/ethnicity coded as dummy variables for Black, Hispanic, or Asian as compared to non-Hispanic White as the reference category, union status coded as a dichotomous variable where 1 indicated married or cohabiting and 0 indicated single, college education coded as a dichotomous variable where 1 indicated at least a bachelor's degree and 0 indicated less education than a bachelor's degree, and parity measured as a continuous variable ranging from 0 to 6 children.
Research Question
How are pregnancy intentions, including ambivalence, associated with contraceptive nonuse and heavy alcohol use?
Sample
Participants were obtained through Prolific (www.prolific.co), an opt-in online survey platform designed for scientific research with human subjects. Prolific gathers participants’ demographic characteristics before screening for eligibility for research studies and is capable of producing nationally representative samples to reduce bias and promote the generalizability of findings. Prolific maintains a database of potential participants and distributes surveys using a survey panel approach to ensure stratification by age, race, and sex.
Inclusion/Exclusion Criteria
This study recruited participants aged 18–50 who were living in the United States and could speak and read English. The sample for the current study (n = 583) was restricted to participants from the larger sample who reported being biologically female and currently sexually active with a biologically male partner and were not currently pregnant at the time of the survey. The sample included participants who responded to all study questions; because only 1.7% of data were missing, missing data were handled with listwise deletion.
Institutional Review Board Approval
Potential participants were asked to review the informed consent information before clicking a link that they agreed to participate prior to the start of the survey. This study was approved by the authors’ university Institutional Review Board before data collection commenced (reference number 16032).
Statistical Analysis
A descriptive analysis of study variables was first conducted. Means and standard deviations of study variables were examined, and Tukey's post hoc tests were utilized to test for significant differences between pregnancy intentions groups on study variables. Logistic regression analysis was then used to examine the relationships between pregnancy intentions, contraceptive nonuse, and heavy alcohol use, controlling for age, race/ethnicity, whether the participant was living in a union, educational attainment, and parity. The first analysis examined the relationship between pregnancy intentions and contraceptive nonuse as the outcome variable, and the second analysis examined the relationship between pregnancy intentions and heavy alcohol use.
Results
Sample Characteristics
Similar to other recent national data reported by Daniels and Abma (2020), descriptive results indicate that contraceptive nonuse across the entire sample was high; two-thirds (66%) of participants reported that they were not consistently using a highly effective form of contraception. At 12%, participants’ heavy alcohol use statistics were similar to those reported in a recent CDC (2024) study on adult women's alcohol consumption.
In this sample, approximately 3.4% (n = 20) reported that they were trying to get pregnant, 18.5% (n = 108) reported that they were ambivalent, and 78% (n = 455) reported that they were trying to avoid becoming pregnant (see Table 1). Nearly all (95%) of the participants who reported that they were trying to get pregnant also reported they were not using contraception. However, 85% of those who were ambivalent about pregnancy and 61% of those trying to avoid pregnancy also reported that they were not regularly using an effective form of contraception. Tukey's post hoc tests for group differences found that the difference in contraceptive nonuse between those trying to conceive as well as those who were ambivalent about pregnancy had higher rates of contraceptive nonuse as compared to those who reported trying to avoid pregnancy. Group differences were not observed for heavy alcohol use; whereas 11% of those trying to conceive reported regular heavy alcohol consumption; 13% of those who were ambivalent and 12% of those interested in avoiding pregnancy reported heavy alcohol use. There were few group differences in sociodemographic characteristics by pregnancy intentions groups; Asian participants were more heavily represented in the “trying to conceive” group than the other groups, and those with a college degree were significantly less likely to report ambivalence about becoming pregnant than they were to be avoiding pregnancy.
Frequencies and Descriptive Statistics of Study Variables (N = 583).

Note: Frequencies are provided for dichotomous variables. Tukey's HSD post hoc test was used to determine significant differences between pregnancy intentions groups at the p < .05 level.
Logistic Regression Analysis of the Role of Pregnancy Intentions for the Odds of Contraceptive Nonuse and Heavy Alcohol Use (N = 583).
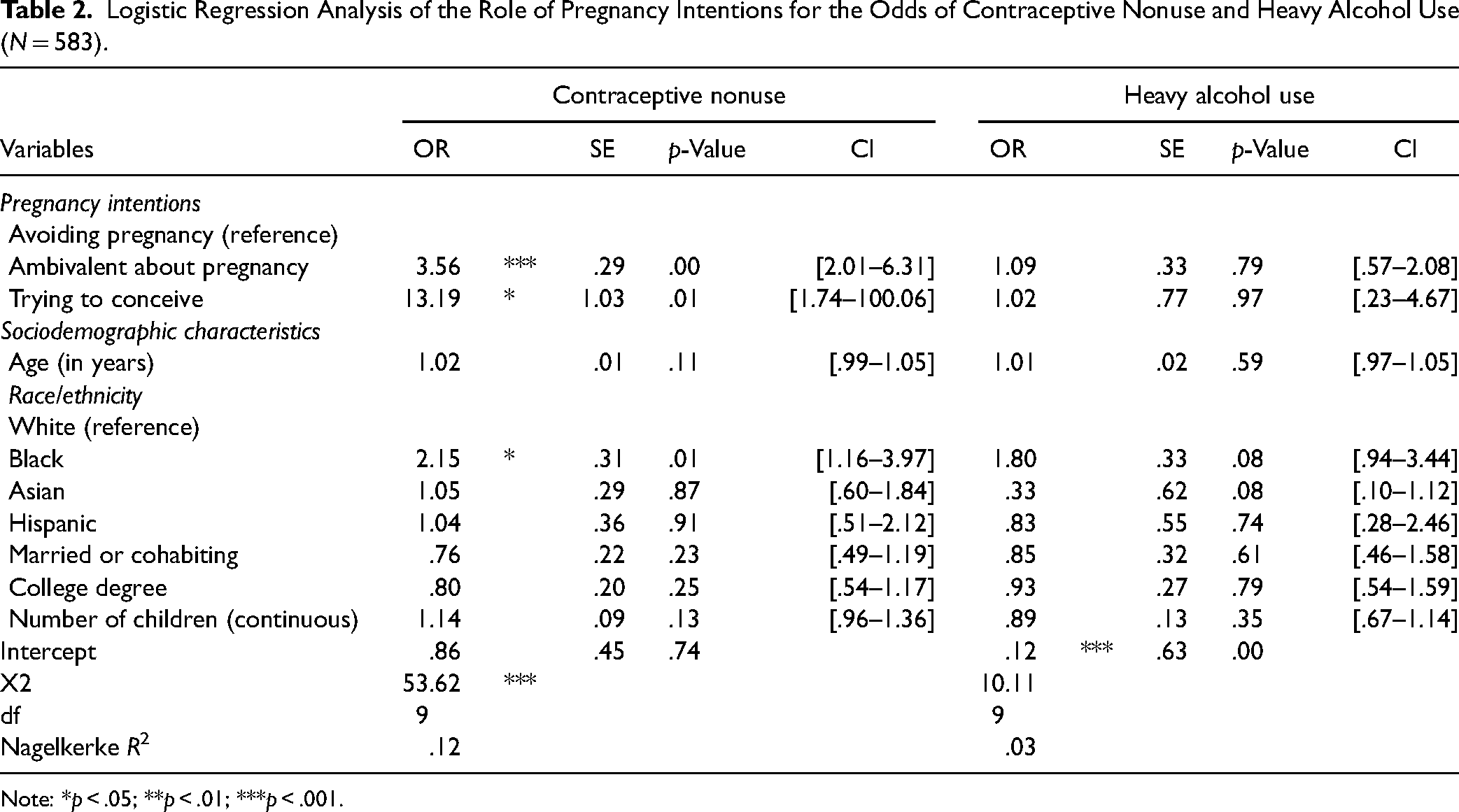
Note: *p < .05; **p < .01; ***p < .001.
Research Question Results
The logistic regression analysis found that compared to those who were avoiding pregnancy, participants who were ambivalent about pregnancy were more than 3.5 times more likely to report contraceptive nonuse (OR = 3.56, p < .001), and participants who were trying to conceive were more than 13 times as likely to report contraceptive nonuse (OR = 13.19, p < .05). The logistic regression analysis did not reveal any statistically significant differences in weekly alcohol use between the pregnancy intentions groups after controlling for sociodemographic characteristics (Table 2).
Discussion
The current study examined how pregnancy intentions are associated with contraceptive use and alcohol use in a national sample of heterosexual women of reproductive age who are sexually active. The results indicate that across all pregnancy intention groups, more than 10% of women reported heavy alcohol consumption (consuming at least four alcoholic drinks at one time per week or more than eight total drinks per week). Thus, some risk for AEP exists across all groups. The risk for AEP appears substantially greater among those trying to conceive and those who are ambivalent about pregnancy, however, due to differences in contraceptive nonuse patterns. Although the majority of women in this study reported that they were currently avoiding pregnancy, more than half of them (61%) were not consistently using effective forms of contraception, and 12% reported heavy alcohol use. Among those who reported being ambivalent about pregnancy, 85% were not consistently using effective forms of contraception, and 13% reported heavy alcohol use. Among those trying to become pregnant, nearly all (95%) reported not using contraception, but still 11% percent reported heavy alcohol use. In summary, the majority of women in the sample did not report using consistent, effective contraception, and a substantial minority of women in each intentions group heavy alcohol consumption on at least a weekly basis. It is unclear based upon available data whether participants across pregnancy intentions groups are regularly testing for pregnancy or being watchful for signs of early pregnancy, such as a missed menstrual cycle.
Strengths and Limitations
Strengths of this study include the use of a contemporary nationally representative sample, a pregnancy intentions measure that includes ambivalence as opposed to a more limited dichotomous measure, and measures on alcohol and contraceptive use patterns. There are also some limitations to the current study. The representativeness and diversity of the sample lend support to the validity of the findings, and the patterns of pregnancy intentions, contraceptive nonuse, and heavy alcohol use found in this study are similar to those noted in other nationally representative studies (e.g., McQuillan et al., 2011; Daniels & Abma, 2020; and CDC, 2024, respectively). Still, the lower rates of women who were trying to conceive or ambivalent about pregnancy in this study prevent subanalyses of these groups. Given the lack of knowledge about health behaviors such as alcohol use or delay of pregnancy recognition among those who are ambivalent about pregnancy, future studies should ensure the recruitment of a large sample of those who identify as ambivalent to ensure adequate power. Another limitation is that the measures used were intended to capture patterns of behaviors related to contraceptive use and heavy alcohol use, but this study does not have data on single episodes. This prevents the examination of the co-occurrence of heavy drinking and contraceptive nonuse. Although prior studies have found a strong relationship between alcohol consumption and contraceptive nonuse (e.g., Scott-Sheldon et al., 2010), this work has primarily focused on those who do not intend to become pregnant. Future studies should examine whether those trying to conceive use contraception during intercourse following a heavy drinking event or whether those trying to conceive are more likely to continuously monitor pregnancy status.
Implications for Practice
These results suggest three key findings for health promotion research and practice. First, intentions to avoid pregnancy cannot be assumed to indicate consistent contraceptive use. Nearly two-thirds of women reported inconsistent or no use of an effective form of contraception. This has important implications for research and practice because reproductive intentions have long been assumed to be the best, albeit imperfect, predictor of subsequent reproductive behaviors (Schoen et al., 1999; Rackin & Bachrach, 2016). This is particularly relevant for data sources such as the National Survey of Fertility Barriers, which includes the pregnancy intentions measure but not the contraceptive use measure. It is also highly relevant for providers, as a mismatch between stated intentions and behaviors is an important opportunity for intervention and contraceptive counseling. Health care providers and FASD prevention efforts can use tools such as the “One Key Question” (Allen et al., 2017) to identify women who are ambivalent. Providing contraceptive counseling to women who report being ambivalent about pregnancy increases contraceptive use (Shreffler et al., 2020); alternatively, counseling women who do not want to use contraception to avoid drinking during their fertile window and to test for pregnancy if appropriate would reduce alcohol exposure during pregnancy.
Second, results indicate that an alcohol-exposed pregnancy is a risk for women regardless of pregnancy intention status. Prior research has established that women who are trying to conceive tend to recognize pregnancy earlier than those who are not actively trying to conceive (Ayoola, 2015). With over 10% of women in the ambivalent and avoidant groups reporting heavy alcohol use, delayed recognition of alcohol-exposed pregnancies may put these women at enhanced risk of having a child with FASD.
Finally, these findings point to women who report ambivalence about pregnancy as a target for future prevention efforts. Women who reported being ambivalent about pregnancy have rates of contraceptive nonuse closer to those who are trying to conceive than those who are trying to avoid pregnancy. Because they might not be monitoring for signs of pregnancy as regularly as women who are trying to conceive, those who are ambivalent about becoming pregnant might be especially at risk for delayed pregnancy recognition and AEP.
Conclusion
This study confirms previous research indicating that many women actively trying to conceive continue to use alcohol on a regular basis. Notable to this work is the finding that women who are ambivalent about pregnancy have much greater odds of contraceptive nonuse than those trying to avoid pregnancy, but it is unknown whether they have similar rates of delayed pregnancy recognition. AEP and FASD prevention efforts that include a focus on this ambivalent group may be more likely to affect meaningful change.
Supplemental Material
sj-docx-1-son-10.1177_23779608241301858 - Supplemental material for The Role of Pregnancy Intentions in U.S. Women's Contraceptive and Alcohol Use Behaviors
Supplemental material, sj-docx-1-son-10.1177_23779608241301858 for The Role of Pregnancy Intentions in U.S. Women's Contraceptive and Alcohol Use Behaviors by Karina M. Shreffler, Alysa Roland, Christine N. Joachims and Julie M. Croff in SAGE Open Nursing
Footnotes
Author Contributions
Conceptualization: KS and JC developed the concept for the article. Methodology and Formal Analysis: KS acquired the data and performed the formal analysis. Investigation: KS, JC, and AR interpreted the findings. Writing-original draft: KS and CJ drafted the original manuscript. Writing-reviewing and editing: JC and AR reviewed and edited the manuscript. All authors approved the final version of the article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Ethical Approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the authors’ Institutional Review Board.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Funding
Financial support for data acquisition and open access publishing was provided by the Fran and Earl Ziegler Endowed Chair in Nursing Research, held by Karina Shreffler at the Fran and Earl Ziegler College of Nursing, University of Oklahoma Health Sciences Center.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
