Abstract
Background
Clinical competence is a critical element in providing high-quality nursing care. A higher level of clinical competence positively influences patient health outcomes as well as nurses’ job performance and satisfaction. Nonetheless, there is limited data on nurses’ clinical competence in Ethiopia.
Objective
This study aimed to assess the level of clinical competency among nurses working in selected public hospitals.
Method
Institution-based cross-sectional study design was conducted from March 1 to 30, 2022. Two hundred five randomly selected nurses from three selected hospitals in the West Shoa Zone namely Ambo University Riferral Hospital, Ambo General Hospital, and Guder Primary Hospital participated in the study via a structured self-administered questionnaire. The collected data were checked for completeness and then entered Epi-data v.4.2.2 and analyzed by Stata software v.14.2. Independent t-test and analysis of variance were used to identify factors associated with nurses’ clinical competence. The level of statistical significance was declared at a p-value < .05.
Results
The overall clinical competence of participants was 2.501 (SD = 0.36), indicating a moderate level of clinical competence. Participants had higher competence scores on the professional development dimension and lower competence scores on the leadership dimension. The null hypothesis was rejected. Age, work experience, professional satisfaction, level of satisfaction, level of hospital, current position, shifting status, retrieval of newly published information, previous training, and frequency of training were the identified factors associated with nurses’ clinical competence.
Conclusion
Nearly five in 10 participants in the study setting had inadequate clinical competence. Professional satisfaction, level of satisfaction, previous training, and frequency of training were factors related to nurses’ clinical competence. It is recommended that responsible stakeholders like the Minister of Health and the Ethiopian Nursing Association should work to improve nurses’ clinical competence by focusing on the identified factors. Also, health policymakers should set strategies to assess nurses’ clinical competence frequently to ensure quality nursing care.
Introduction
Nursing clinical competency is the integrated knowledge, skills, judgment, and attributes required of a nurse to practice safely and ethically in a designated role (International Council of Nurses, 2021). It is the ability to provide safe care (Levett-Jones et al., 2011) using the skills, knowledge, attitudes, values, and abilities that bring about effective performance in professional positions (Meehan, 2018). Nursing competence is an essential component in providing safety and quality care (Flinkman et al., 2017).
Today, nurses’ clinical competence in healthcare settings is the focus and center of attention for managers and the healthcare system (Roberts & Lockhart, 2009). The World Health Organization identified crucial components for integrating and strengthening the nurse workforce. These include patient advocacy and education, effective communication, teamwork and leadership, people-centered care and clinical practice, continuous learning, and research (World Health Organization [WHO], 2015).
Review of Literature
The clinical competence of nurses is one of the key factors and essential requirements for safe and effective care provision based on professional performance standards (Cuyler, 2015). Nurses require high-level clinical knowledge and skill to effectively evaluate the patient's condition and deal with challenges that may occur during treatment (Fukada, 2018).
Factors such as effective communication, career interest, accountability, work experience, and personal factors such as ethical and professional principles, knowledge, and skills affect the competence of nurses (Memarian et al., 2007). A study conducted in Karma, Iran, revealed that work experience affects the clinical competence of nurses (Karami et al., 2017). Additionally, research conducted in Japan shows that the age of the patient affects nurses’ clinical competence (Yamamoto et al., 2021). Conversely, a study conducted in Mashhad, Iran, indicates that work experience does not affect the clinical competency of nurses (Abbaspour et al., 2021). Professional factors such as effective management, control, and monitoring, as well as external environmental factors such as an efficient education system and the provision of technology, are other factors affecting the competence of nurses. A review showed that there is a growing awareness about the competence of nurses, encouraging nursing managers to prioritize this concern and its associated factors (Yanhua & Watson, 2011).
The presence of skilled nurses is essential for maintaining the quality of healthcare services, as their professional competence plays a vital role in enhancing the level of nursing care provided to patients (Kemppainen et al., 2012; Manoochehri et al., 2015).
The competence of nurse professionals has a significant impact on the quality of care and is closely associated with job performance, satisfaction and absenteeism, and patient safety (Kuokkanen et al., 2016). It is approved that a higher level of clinical competence has a positive impact on patients’ health outcomes and nurses’ job satisfaction (Numminen et al., 2015; Park et al., 2015). Several studies have inconsistent findings on the clinical competence of nurses working in different health institutions in which the clinical competence of nurses was reported as high (Kim et al., 2015), moderate (Mirlashari et al., 2016), and moderate to low (Lee et al., 2015). Similarly, a study conducted in Finland revealed that nurse's clinical competence was moderate to high level (Lakanmaa et al., 2015). Consequently, healthcare administrators face challenges in getting competent and experienced nurses (Bifftu et al., 2016).
Studies on clinical competence and its associated factors among nurses were scarce in Ethiopia. In a current study setting, the level of clinical competence and its associated factors among nurses were not yet being investigated. Thus, the present study aimed to assess the level of clinical competence of nurses working in the selected public hospital of West Shoa Zone, Ethiopia.
Objectives of the Study
To determine the level of clinical competency among nurses working in selected public hospitals in West Shoa, Ethiopia.
To assess factors associated with clinical competency among nurses working in selected public hospitals in West Shoa, Ethiopia.
Hypothesis of the Study
Null hypothesis: There is no statistically significant difference in the level of clinical competence among nurses, considering a set of variables within the current study.
Alternative hypothesis: There is a statistically significant difference in the level of clinical competence among nurses, considering a set of variables within the current study.
Method
Study Design, Area, and Period
An institutional-based cross-sectional study design was conducted at selected public hospitals in the West Shoa Zone, Oromia, central Ethiopia from March 01 to 30, 2022. Ambo is the capital city of the West Shoa Zone located 114 km away from Addis Ababa. West Shoa Zone has a total of 2,869,314 populations, of which 1,433,704 are males, according to the West Shoa Zone population statistics report of 2021. In this zone, there are nine public hospitals. Both Ambo General Hospital and Ambo University Riferral Hospital are found in Ambo Town. Guder Primary Hospital is located 10 km from the town of Ambo. According to the hospital's human resource report, 362 nurses were working in selected public hospitals, and among these 219 were males.
Study Population
All nurses working in the public hospitals of the West Shoa Zone and all randomly selected nurses working in the selected public hospital of the West Shoa Zone were the source population and study population, respectively.
Inclusion and Exclusion Criteria
Nurses who had worked in the selected public hospitals of the West Shoa Zone during the study period and nurses who had less than 6 months were excluded from the study.
Sample Size Determination
The required sample size for this study was determined using a single population proportion formula with the following assumptions: 95% confidence interval CI), 5% margin of error, and 50% clinical competence of nurses (p = 50%). Therefore, the sample size was determined as follows: Thus,
Sampling Techniques
A list of nurses in each hospital was obtained from the hospital's human resources which serve as a sampling frame. Then proportional allocation of nurses to each selected hospital was performed. This proportional allocation was as follows, Ambo University Riferral Hospital 121 out of 213 total nurses, Ambo General Hospital 56 out of 99 total nurses, and Guder Primary Hospital 28 out of 28 total nurses. After that, individual participants were selected using simple random sampling to achieve the final sample size. The data collectors approached the respondents who met the inclusion criteria and agreed to participate. The self-administered written questionnaires were distributed to the individual nurses working in the selected hospital. The completed questionnaires were collected by the data collectors.
Variables
Dependent Variable
Nurses' clinical competence.
Independent Variables
Age, sex, marital status, education level, work experience, satisfaction with the nursing profession, average monthly income, employment position, information retrieval, type of health institution, previous training, frequency of training, and having guidelines/manuals.
Operational Definition and Definition of Terms
Data Collection Tool and Procedure
In this study, data were obtained by a self-administered structured questionnaire that was adapted from a questionnaire used in different studies (Lakanmaa et al., 2015; Mirlashari et al., 2016). Validity and reliability were established and reported by pretest. To measure nurses’ competency, the Competency Inventory for Registered Nurses (CIRN) was developed in China to assess the competence of nurses in various clinical positions in the form of self-evaluation (Liu et al., 2009). The tool consisted of 55 items under seven dimensions including clinical care with 10 items, leadership with eight items, interpersonal relationships with eight items, legal-ethical practice with eight items, professional development with seven items, teaching-coaching with six items, and research aptitude-critical thinking with eight items. The CIRN was scored using the 5-point Likert scale ranging from 0 to 4, with an incompetency score of zero), low competency (score 1), moderate competency (score 2), high or sufficient competency (score 3), and very high competency (score 4). Based on the study conducted at Ilu Aba Bor Zone, they were categorized based on the mean score of participants as mean scores below 2, 2-3, and above 3 were considered as low, moderate, and high competence respectively (Geleta et al., 2021). The data were collected over 1 month by trained 4th-year Bachelor of Science (BSc) nursing students and supervised by two MSc nurses. From the pretest result, the tools to measure the clinical competence of nurses were reliable with Cronbach's alpha at 0.89. After the pretest minor amendments were made like wording errors.
Data Quality Control
The quality of data was ensured through the provision of a 1-day training for data collectors and supervisors on objective, ethical issues, data collection instruments, and procedures. A regular review of each of the completed questionnaires was performed daily. A pretest of the questionnaire was conducted on 10% (21) of the sample size nurses working in Bako Primary Hospital 2 weeks before actual data collection to ensure clarity of the questionnaire.
Data Analysis
Data were entered into Epi Data version 4.2.2 and exported to the Stata software version 14.2 for analysis. Frequency, means, and standard deviations of independent variables and the level of clinical competence of nurses were analyzed using descriptive statistics. Independent t-test and one-way analysis of variance (ANOVA) were used to examine the mean difference between groups of independent variables. Data were tested for the assumption of normality and homogeneity. The assumption normality was tested by creating a histogram and values of skewness and kurtosis were confirmed by Kolmogorov–Smirnov tests at an alpha level of 0.05. The assumption of homogeneity of variance was examined by Levene's test of equality of variance. The results indicated that there were no significantly different variances among groups, thus the assumption of homogeneity of variance for all variables was tenable. The results indicated that there were no nonnormally distributed variables. An independent t-test is a parametric test that is used to compare the mean of two groups and ANOVA is also parametric that is used to compare the mean of three or more groups. Therefore, independent variables with two groups were analyzed by independent t-test, and variables with three or more groups were analyzed by one-way ANOVA. Finally, the statistically significant difference was set at p < .05.
Results
Sociodemographic Characteristics of Study Participants
Out of the total 205 distributed questionnaires, 194 completed data were returned, which made a response rate of 94.63%. The incomplete data were excluded from the analysis and counted as nonresponse rates. From this, 114 (55.6%) of participants were between the age group of 26 and 30 years old with a mean (SD) of 29.08 (±0.263), 114 (58.76%) were males, and 153 (78.87%) were having less than 5 years working experience. Regarding educational level, 167 (86.08%) had a BSc degree and 184 (94.85%) of them were staff nurses (those nurses who have no administrative position; Table 1).
Sociodemographic Characteristics of Study Participants Working in a Selected Public Hospital of West Shoa, Central Ethiopia, 2022.

Most of the respondents 113 (58.25%) were working in Ambo University Riferral Hospital and most of the respondents 184 (94.85%) were serving as staff nurses. The majority 158 (81.44%) of respondents wanted to retrieve newly published information related to nursing care and most of them 181 (93.3%) were satisfied with the nursing profession. Most of the respondents, 150 (77.32%), had at least one type of training in their professional careers. The majority 175 (90.2%) of them had taken the exit exam or certificate of competence (COC) upon graduation from their current education while almost all 174 (99.43%) of them passed the exam/COC. The majority of 152 (78.35%) respondents had at least one type of guideline/manual but 141 (92.8%) of them were using it (Table 2).
Frequency Distribution of Nursing Profession-Related Factors of Clinical Competency Working in Selected Public Hospitals of West Shoa, Central Ethiopia, 2022.

COC: certificate of competence.
Level of Clinical Competence of Nurses
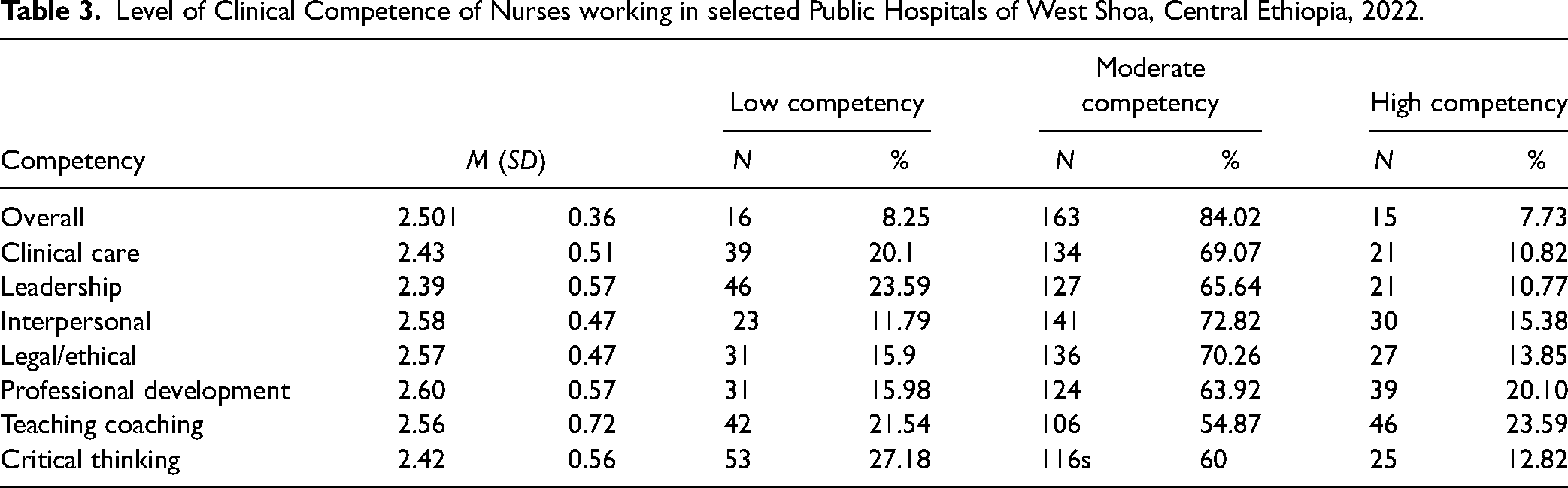
The overall clinical competence of participants was 2.501 (SD = 0.36) out of a total possible score ranging from 0 to 4, indicating a moderate level of clinical competency. It was also found that 16 (8.25%), 163 (84.02%), and 15 (7.73%) of participants were in low, moderate, and high clinical competency respectively. In comparison with other dimensions, participants scored a better mean of 2.6 (SD = 0.57) in the professional development dimension of clinical competence (Table 3).
Level of Clinical Competence of Nurses working in selected Public Hospitals of West Shoa, Central Ethiopia, 2022.
Factors Associated With Clinical Competence of Nurses
From factors associated with the clinical competence of nurses independent t-test found that there was no statistically significant difference between the mean scores of groups based on sex; t (192) = −0.52, p = .6, marital status; t (192) = −1.59, p = .11, taking an exit exam or COC upon graduation; t (192) = −2.78, p = .059, and having guideline/manual; t (192) = 2.58, p = .051. However, there were statistically significant mean differences were found among staff positions; t (192) = −2.95, p = .003, staff shift unit; t (192) = 3.3, p = .001, professional satisfaction; t (192) = 2.7, p = .007, newly published information on nursing care retrieval; t (192) = 3.38, p = .001, having professional training; t (192) = 2.87, p = .005, frequency of previous training; t (192) = −3.45, p = .001 and professional experience; t (192) = −3, p = .003 (Table 4).
Independent t-Test: Variables of Significant Mean Difference With Clinical Competence of Nurses Working in Selected Public Hospitals of West Shoa, Central Ethiopia, 2022 (n = 194).

Note. N = number of nurses; M = mean; SD = standard deviation; df = degree of freedom.
One-way ANOVA revealed that there was a statistically significant difference in mean scores among groups based on age; F (3,190) = 9.28, p = .001, level of the hospital; F (2,191) = 7.36, p = .001, and level of satisfaction; F (3,177) = 3.17, p = .025. However, there was not a statistically significant difference between the mean scores of groups based on level of education; F (2,191) = 0.43, p = .65 (Table 5).
Analysis of Variance: Variables of Significant Mean Difference With Clinical Competence of Nurses Working in Selected Public Hospitals of West Shoa, Central Ethiopia, 2022 (n = 194).

Note. N = numbers of nurses; M = mean; SD = standard deviation; df = degree of freedom; AURH = Ambo University Referral Hospital; AGH = Ambo General Hospital; GH = Guder Hospital; BSc = bachelor of science.
Discussion
In the current study, the level of clinical competency of nurses working in West Shoa 16(8.25%), 163(84.02%), and 15(7.73%) participants were low, moderate, and high respectively.
In contrast to the current study, several studies conducted in different countries reported better findings which indicated 20.5% of participants were high-level competent in Ilu AbaBor, Ethiopia (Geleta et al., 2021), 80% of participants were highly competent in Iran (Keykha et al., 2016) and 67.5% of participants were high-level competent in Finland (Lakanmaa et al., 2015). This difference might be due to differences in technological advancement, healthcare system, education facilities in nursing schools, accessibility and availability of teaching centers, and differences in the level of health facilities.
The current study also found that the mean score of participants was 2.501 ± 0.36 on a 5-point Likert scale (0–4). In addition, participants had higher competence scores on professional development and lower competence scores on the leadership dimension. In the current study, the participant's score was notably less than the score in the previous study which reported 2.70 ± 0.46 from 4 total scores. The mean score of participants in interpersonal communication, legal/ethics, clinical care, and professional development was higher than the mean score of participants in the current study (Tabriz et al., 2017). This difference from previous studies might be attributable to individual and organizational factors, higher levels of education, and longer periods of work experience in the prior study, which may have increased nurses’ confidence in their clinical competence. However, the current study result was slightly higher at 2.23 (SD = 0.6) compared to a study done in Ilu AbaBor, Ethiopia (Geleta et al., 2021). This difference may be due to differences in the study setting since the current study includes all levels of the hospital.
The present study found a significant mean difference in the score of clinical competence of nurses based on age groups in which older nurses scored higher than younger nurses. Studies in Iran (Keykha et al., 2016; Khodadadei & Salehi, 2016) and a study conducted in Japan reported similar findings that clinical competence was affected by a nurse's age (Abbaspour et al., 2021). The reason for this may be older nurses had more opportunities for exposure to different nursing care than younger nurses. This study also revealed that there is a significant association between years of nursing work experience and the clinical competence of nurses. From the current study, nurses having more experience scored higher mean than those less experienced nurses. Studies in Iran (Karami et al., 2017; Khodadadei & Salehi, 2016) and a study done in Japan revealed similar findings that the year of experience was among the factors that affect a nurse's competence (Abbaspour et al., 2021). A possible explanation for this may be their exposure to different patients for long periods might positively influence their clinical competence level. The present study revealed that the position of nurses was a statistically significant difference in the mean of the clinical competence of nurses, which indicated that working in a manager/leadership position had scored higher than staff nurses (those working with direct patient care). The previous study also supports this finding that the clinical competence of nurses was associated with the position of a nurse (Khodadadei & Salehi, 2016).
The present finding also revealed a statistically significant difference in mean scores of clinical competencies based on the level of nurses’ satisfaction. Similarly, a previous study showed that nurses who had higher levels of satisfaction with their profession had the highest mean scores of clinical competencies when compared with nurses who had less satisfaction (Geleta et al., 2021). Also, the current study indicates that the nurse's professional satisfaction was a statistically significant difference in the mean of competence, which showed nurses having satisfaction with their profession were a higher mean of competence scores than their counterparts.
Nurses who had more professional training were more clinically competent than those who had less professional training. This could be due to their updated knowledge positively influencing their clinical competence. Similarly, the current study finding shows that having professional training was a statistically significant difference in the means of nurses’ clinical competence. This shows nurses having professional training were more competent than their counterparts. This finding is supported by a study conducted in Ilu AbaBor, Ethiopia (Geleta et al., 2021).
The present study found that the level of the hospital was a statistically significant difference in the mean of clinical competence of nurses. Nurses working in the referral/teaching hospital scored a higher mean of clinical competency than nurses working in other levels of hospitals like general hospitals and primary hospitals. This might be because nurses who were working in referral/teaching hospitals have different opportunities like the opportunity to communicate with experts, attend academic meetings, meet with experienced nurses, and upgrade to the next level of education to become more competent.
Retrieval of newly published information related to nursing care was a statistically significant difference in the means of nursing clinical competence. This is also supported by a study done in Ilu AbaBor, Ethiopia which indicates nurses retrieving newly published information were more competent than their counterparts (Geleta et al., 2021). The possible reason might be having updated information enhances their knowledge which leads them to higher competence.
Participants working in a fixed unit scored higher clinical competence than those working in a rotation from one unit to another. This finding is consistent with a study conducted in Iran (Tabriz et al., 2017) which revealed nurses working in fixed shift schedules had higher clinical competence than those with rotating shift schedules.
Strengths and Limitations of the Study
This study, focusing on nursing professionals in institutional areas, is the first study for the area and provides foundational information for further research.
The results are generalizable for the public hospitals of West Shoa since they included all levels of hospitals (primary, general, and teaching or referral hospitals).
Findings might not be assumed to be generalizable to all nurses working in the West Shoa Zone, as other health facilities such as health centers, health posts, and private institutions were excluded.
A self-administered tool was used which may cause over or underestimate the result due to social desirability bias.
Implications for practice
Above all in the profession, clinical competence is one of the essential requirements for safe and effective care and the key elements in providing care based on standards of professional performance. The outcomes of this study provide current information regarding the level and factors associated with nurse's clinical competency. The result provides direction for concerned bodies to improve nurses’ clinical competence like hospital administration, policymakers, nursing associations, nongovernmental organizations, and researchers.
Conclusion
Even though the clinical competence of nursing is a matter of great concern as its direct impact on the quality of care provided, the current study setting revealed the mean score of clinical competence of nurses was moderate level this indicates inadequate since nursing care is expected to provide to the highest level. Participants had higher competence in professional development and lower competence scores on the leadership dimension. The null hypothesis of the study was rejected. Age, work experience, staff position, professional satisfaction, level of satisfaction, professional training, frequency of training, level of hospital, shift work, and retrieval of newly published information-related care were among the statistically significant mean differences that related to nursing clinical competence.
Health policymakers and stakeholders in healthcare systems need to design strategies for improving nurses’ clinical competence considering the identified factors. Healthcare managers should prepare and provide professional training for nurses. Future researchers have to consider including all levels of health institutions and observational tools.
Footnotes
Acknowledgments
We would like to thank Ambo University College of Medicine and Health Sciences, Department of Nursing for the opportunity, and the West Shoa health office and public hospitals for their information and cooperation during data collection. We also express our sincere gratitude to the staff of the West Shoa Zone public hospitals for their support and data collectors.
Authors’ Contributions
All authors made substantial contributions to this study by involving in conception and design, data acquisition, data analysis and interpretation, and manuscript preparation, and gave final approval for the version to be published and agreed to be accountable for all aspects of the work.
Data Availability Statement
The datasets used in the current study can be accessed from the corresponding author upon reasonable request; the summary of data is presented in the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Clearance
An ethical clearance was obtained from the Ambo University College of Medicine and Health Science Department of Nursing research committee (RREC ref. no: UGC/122/2022) to get permission and cooperation during the collection of the data. After the purpose and objective of the study were explained, consent was obtained from each selected study participant, and their agreement was verbal. Participants were also informed that participation is voluntary, and they can withdraw from the study at any time. The confidentiality of information provided by study subjects was also protected by making the data collection procedure anonymous and their names were not written on the questionnaire.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.


