Abstract
Introduction
Simulation training has become an integral component of nursing education, offering students opportunities to develop and refine their clinical skills in a controlled and safe environment.
Objective
This study aimed to evaluate the clinical skill competence and professional behaviors of undergraduate nursing students following simulation training.
Design
A descriptive cross-sectional design was employed for this study.
Setting
The study was conducted in the simulation center at the University of Tabuk using the Clinical Competency Questionnaire (CCQ), with data collected between January 1, 2023 and February 28, 2023. Participants were enrolled using a convenience sampling method, including nursing students in the 3rd and 4th years who trained in the simulation center and agreed to participate.
Results
The study results indicate that a majority of students demonstrated strong theoretical knowledge and practical competence in performing sterile techniques and administering oral medications with minimal or no supervision, with percentages of 74.7% and 73.3%, respectively. A significant proportion of students reported uncertainty or lack of skill in performing shift reports using SBAR (38.4%) and assessing gastrostomy tube placement (32.9%). Students exhibited satisfactory knowledge and competence in maintaining appropriate appearance, attire, and conduct (71.2%), understanding, and supporting group goals (71.2%), and comprehending patients’ rights (69.9%).
Conclusion
The findings suggest that nursing students attain a relatively high level of clinical competence and self-confidence after simulation training. This study recommends incorporating simulation training in nursing education, which enhances professional behaviors like appearance, group goals, and patient rights, but requires improvement in constructive criticism, problem prevention, and cultural competence.
Introduction
Simulation, acknowledged as an instructional method for replicating real-world scenarios in educational settings, has become an integral component of nursing education, aimed at realizing educational objectives through experiential learning (Al-Elq, 2010). Simulation training, a form of experiential learning, employs life-size manikins with realistic physiological and pharmacological responses, providing a sophisticated interactive experience in lifelike situations (Adib-Hajbaghery & Sharifi, 2017). Recognized by Quality and Safety Education for Nurses and endorsed by Healthy Simulation, nursing simulation stands out as a top teaching strategy for nursing students. Simulation actively involves students in the learning process by facilitating knowledge construction, exploration of assumptions, and the development of psychomotor skills within a secure environment (Bailey & Emory, 2022). Furthermore, simulation training replicates various physiological responses and fosters the development of clinical reasoning skills more than the theoretical and clinical training (Tawalbeh, 2020).
Review of Literature
Simulations provide diverse opportunities for students to practice healthcare modalities, including safety, cultural competence, communication, teamwork, managing uncommon clinical situations, and handling bedside crises (Omer, 2016). The effectiveness of simulations as a teaching tool, improving students’ abilities and preparing them for their future profession (Adib-Hajbaghery & Sharifi, 2017; Eyikara & Baykara, 2018; Liaw et al., 2016). Despite these advantages and the fact that engaging nursing students in deliberate practice exercises within a simulation laboratory has demonstrated an enhancement in competence and confidence in safely applying techniques in patient care settings (Alharbi & Alharbi, 2022), the use of simulation training still faces some challenges as the risk of desensitization. Because of the controlled environment of the simulations, it potentially impacts their perception to real-world patients risks (Warren et al., 2016). Also, the lack of standardized frameworks and outcome measures may affect the simulation training.
The prevalence of simulation in nursing education is increasing, with Koukourikos et al. (2021) noting its adoption in both academic and clinical settings (Koukourikos et al., 2021). Also, in recent years, simulation training has been gaining attention in Saudi Arabian healthcare education (Arab et al., 2017). Because of the lack of knowledge about simulation training for nurses, a crucial element of healthcare system and the importance of training them to develop their skills to deliver the best possible patient care, the University of Tabuk's nursing department has developed a groundbreaking simulation program for the 3rd- and 4th-year students in 2022. The program offers a hands-on approach besides the professional communication skills where students honed crucial skills like assessment, communication, and teamwork, all under expert guidance.
Through a detailed examination of the specific nuances of the simulation programs implemented at the university, this study seeks to provide insights into the effectiveness of simulation as an educational strategy in the context of Saudi Arabian nursing education by evaluating their clinical skill competence and professional behaviors.
Method
Design
The descriptive cross-sectional study design was employed in this research to provide a comprehensive snapshot of the clinical skill competence and professional behaviors of 146 nursing students at the University of Tabuk over a defined period from January 1, 2023 to February 28, 2023
Sample
The enrollment of participants was facilitated through a convenience sampling method. Inclusion criteria comprised 3rd- and 4th-year undergraduate nursing students at the University of Tabuk who had undergone simulation training. Exclusion criteria included those who did not provide consent to participate in the study. The sample size was determined using Raosoft sample size calculator. This study assumed an expected proportion of 8% at a 95% CI and 5% margin of error, the minimum required number for this study was 114.
Procedure
In 2022, the nursing department started simulation training program for 3rd- and 4th year nursing students, signifying a transformative initiative. The curriculum was meticulously crafted, tailoring distinct courses to each academic level: Medical Surgical Nursing for 3rd-year students and Critical Care Nursing for 4th-year students. Over a comprehensive 4-week period, students actively engaged in immersive learning through 2 weekly simulation sessions. These sessions were strategically designed to expose students to scenarios mirroring the complexities of real-world nursing challenges.
The program aimed at fostering a broad array of critical nursing competencies, emphasizing the development of skills essential for competent and compassionate patient care. This encompassed proficiency in assessment skills, enabling students to conduct thorough health assessments with a focus on physical examinations and health history reviews. Additionally, there was a strong emphasis on honing clinical decision-making skills, instilling the ability to prioritize patient care interventions and make sound judgments in dynamic healthcare environments. Collaboration and communication skills were actively nurtured, promoting effective teamwork and interdisciplinary communication. Moreover, the program addressed patient education skills, ensuring students could adeptly convey medical information to patients and their families. The curriculum stressed the significance of ethical practice, encouraging students to uphold ethical standards, maintain patient confidentiality, and exhibit cultural sensitivity. Teamwork and collaboration were underscored throughout, cultivating a collaborative spirit among students in the face of challenging scenarios.
Furthermore, the training delved into technical procedures, covering a spectrum from intravenous (IV) catheter insertion to NG tube insertion and management, urinary catheterization, chest tube management, oxygen therapy administration, medication administration (including oral, intramuscular, and subcutaneous routes), wound care and dressing changes, blood glucose monitoring, and insulin administration. The critical care component extended to procedures such as ventilator management, hemodynamic monitoring, and the response to life-threatening emergencies, providing a holistic approach to nursing education. To ensure a seamless transition from theoretical knowledge to practical application, students underwent a comprehensive 2-week preparatory phase in the nursing college lab before engaging in the 4-week simulation training. In this preparatory phase, under the guidance of their instructors, students received hands-on training for the required procedures. The instructors provided demonstrations, and students had the opportunity for individual redemonstrations to ensure mastery. Facilitating effective training, students were organized into teams of three, with each session accommodating a total of 10 students. This small group structure aimed to ensure personalized attention and optimal participation. Notably, the simulation training program was strategically aligned with concurrent clinical training within hospital settings, fostering a seamless integration of theoretical knowledge with practical application. Upon completing the 4-week training, students were administered a self-report survey designed to assess their perceived skill, competencies, and their professional behaviors. Drawing inspiration from the Clinical Competency Questionnaire (CCQ), the survey covered a range of skills corresponding to the scenarios practiced during the training. This comprehensive approach aimed to provide valuable insights into students’ experiences and their perceived outcomes, contributing to the ongoing enhancement of the nursing education program at the University of Tabuk.
Data Collection and Instruments
Data for this study was collected through an online questionnaire comprising two parts: Part I, which gathered demographic information such as academic year, age, and gender; and Part II, which utilized CCQ. Developed by Liou and Cheng in 2013, the CCQ is a validated instrument designed to assess nursing students’ clinical competencies (Liou & Cheng, 2013). The adapted questionnaire consists of 37 items, each rated on a 5-point Likert scale ranging from 1 (“do not have a clue”) to 5 (“known in theory, competent in practice without supervision”). These items collectively measure students’ self-perceived competence across various clinical skills, competencies, and professional behaviors. The CCQ includes three subscales: skills, competency, and professional behavior. The skills subscale comprises 21 items, the competency subscale includes 16 items, and the professional behavior subscale assesses students’ self-perceived competence in professional conduct. It's important to note that the professional behavior subscale, as defined by Liou and Cheng, does not measure observed behavior but rather evaluates competencies related to professional expectations.
While Liou and Cheng initially proposed four subscales, the authors’ adaptation focused on the three mentioned above—skills, competency, and professional behavior. The researchers’ decision to exclude the “progression” subscale was made to align with the study's research objectives, focusing on evaluating nursing students’ self-perceived competence in practical skills, overall competency, and professional behavior. This adaptation maintains the integrity of the CCQ while ensuring its alignment with the study's goals and maintaining reliability.
Ethical Consideration
Ethical approval was obtained from the Institutional Review Board (IRB) of University of Tabuk (UT-227-70-2022) on 12th September 2022, Tabuk, Saudi Arabia. At the beginning of the survey, students were informed about their right to participate or withdraw from the study. The consent was taken at the beginning of the survey (by clicking on yes or no) before starting to answer the survey. To maintain privacy of the participant information, all the data were stored in the primary researcher's computer and only researchers related to this study had access to the data.
Statistical Analysis
The analysis was conducted using RStudio (R version 4.1.1). Descriptive statistics were employed for categorical data (frequencies and percentages) and numerical data (mean and standard deviation). Group-based differences in the scores of the CCQ scale and subscales were assessed using a Weltch t-test and Wilcoxon rank sum test for variables with two groups (sex and academic year) and an ANOVA test for variables with three groups. Spearman's test was used to explore the association between the scores of skill competency and professional behavior. Normality was checked using Shapiro–Wilk test and equality of variance was checked using Levene's test. A p-value of <.05 indicated statistical significance. The principal components analysis (PCA) analysis and reliability analysis conducted using the following packages: “corpcor,” “GPArotation,” and “psych.”
Validity and Reliability
Factor Analysis
PCA was conducted on the 37 items with orthogonal rotation (varimax) to identify the best factor structure of the CCQ. Mean Square Error of Approximation = 0.06 which is an acceptable range for a perfect fit. Fit based upon off diagonal values was 0.99 which is near to 1, so it indicates a perfect fit. An initial analysis was run to obtain eigenvalues for each component in the data. Two components had eigenvalues over Kaiser's criterion of 1 and in combination explained 59% of the variance. Two components were retained in the final analysis. Table 1 shows the factor loadings after rotation. The items that cluster on the same components suggest that Component 1 represents professional behaviors, and Component 2 skill competencies.
Factor Loadings After Rotation.

Cronbach's alpha internal consistency coefficient of the CCQ was found to be 0.98. Cronbach's alpha coefficients for the factors of professional behaviors, and skill competencies determined to be the same, 0.96, and 0.96 respectively. For the split-half coefficient, the scale split into two halves such that two halves would be as equivalent possible. The domains achieved appropriate mean interitem correlations: 0.51, and 0.6 for professional behaviors, and skill competencies respectively. The whole scale's mean item correlation value was found 0.52, which was in the acceptable range.
Results
Sample Characteristics
In the current study, the authors included data of 146 nursing students. Third-year students represented 56.2% of the sample, whereas 4th-year students represented 43.8%. More than half of the sample was females (57.7%). Participants aged 21 to 22 years represented 38.4% of the students (Table 2).
Demographic Characteristics of Students.

The variable has eight missing values.
The variable has four missing values.
Clinical Competency Questionnaire Scale and Subscales
As for skill competency, students were primarily knowledgeable in theory and competent in practice with minimal or no supervision for performing sterile techniques (74.7%) and administering oral medications (73.3%). In contrast, the proportions of students who do not have a clue or are unconfident at all in practice were high for performing shift reports using SBAR (38.4%) and assessing gastrotomy tube placement (32.9%; Table 3).
Students’ Responses to the Skill Competency Subscale.
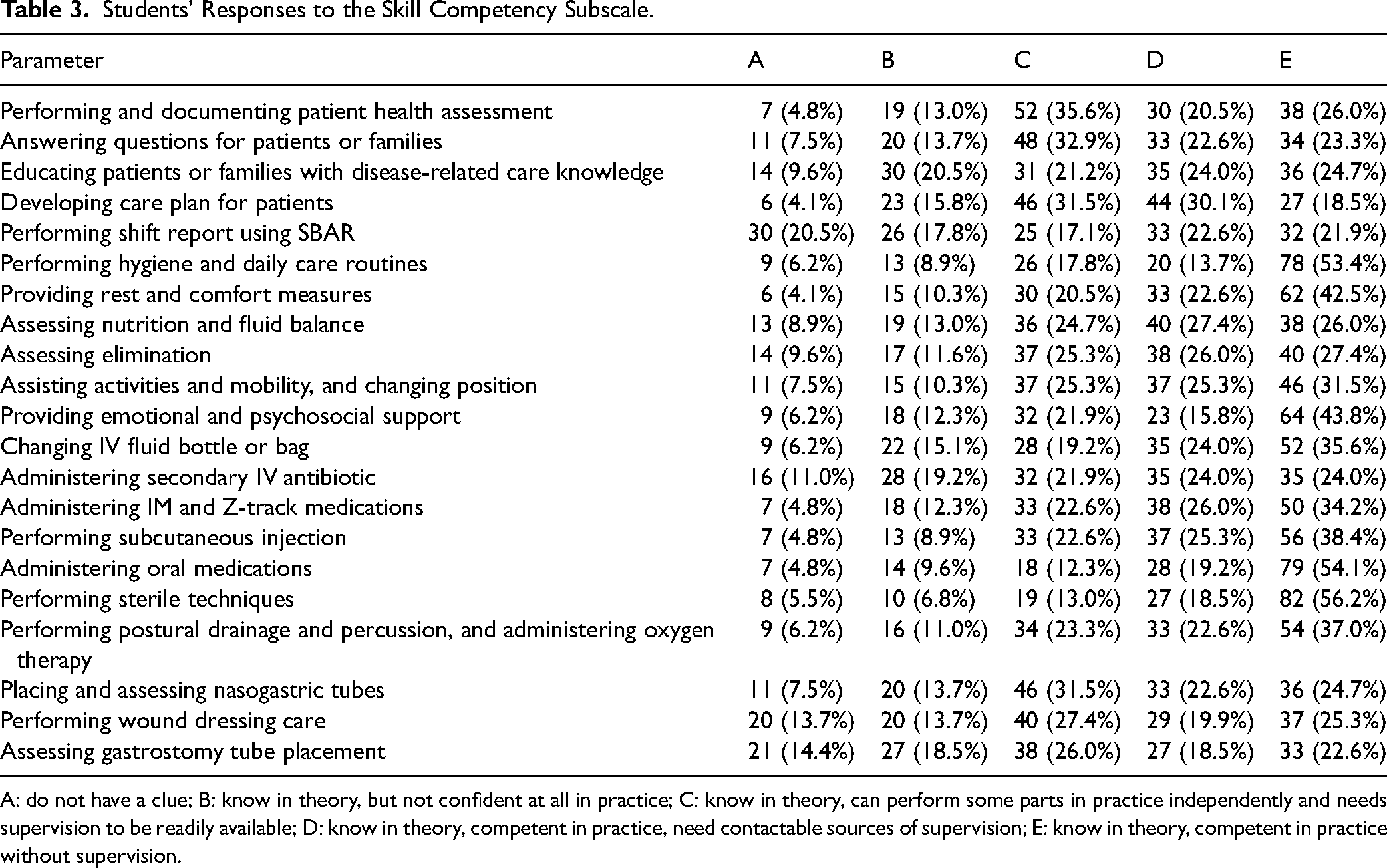
A: do not have a clue; B: know in theory, but not confident at all in practice; C: know in theory, can perform some parts in practice independently and needs supervision to be readily available; D: know in theory, competent in practice, need contactable sources of supervision; E: know in theory, competent in practice without supervision.
Concerning professional behavior, students had required knowledge and competence with no or minimal supervision for maintaining the appropriate appearance, attire, and conduct (71.2%), understanding, and supporting group goals (71.2%) and understanding patients’ rights (69.9%). Conversely, students had no clues or were unconfident in applying or accepting constructive criticism (24.7%), preventing patients from problem occurrence (22.8%) and demonstrating cultural competence (21.9%; Table 4).
Students’ Responses to Professional Behavior Subscale.

A: do not have a clue; B: know in theory, but not confident at all in practice; C: know in theory, can perform some parts in practice independently and needs supervision to be readily available; D: know in theory, competent in practice, need contactable sources of supervision; E: know in theory, competent in practice without supervision.
Factors Associated With the Scores of Perceived Clinical Competences
The average scores of the CCQ scale and subscales did not differ significantly according to the level of the academic year and students’ gender. However, the average CCQ score was insignificantly different among students who were ≥22 years (3.4 ± 0.8) compared with those aged 21 to 22 years (3.8 ± 0.9) and ≤20 years (3.7 ± 1.0, p = .376). Similarly, the oldest age category (≥22 years) had an insignificantly different professional behavior score (3.4 ± 0.9) compared to those aged 21 to 22 years (3.9 ± 1.0) and ≤20 years (3.9 ± 1.0, p = . 551). Nevertheless, the score of skill competency was not statistically different among different age categories (Table 5).
Factors Associated With the Scores of Perceived Clinical Competences.
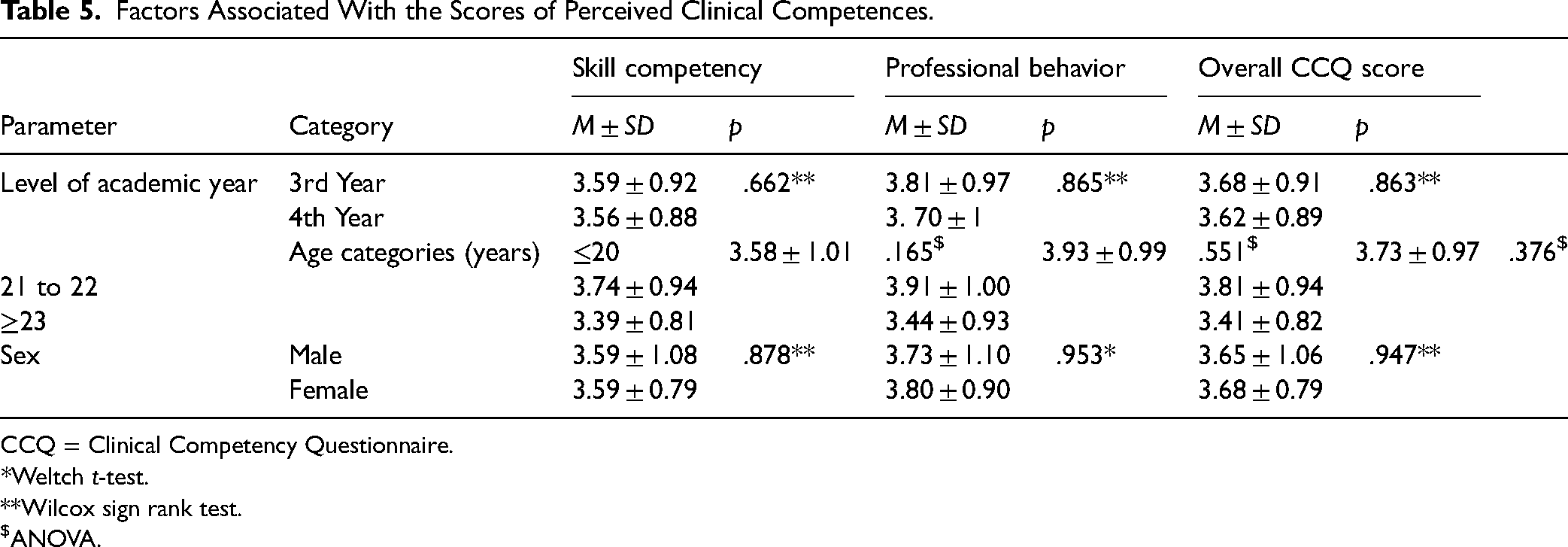
CCQ = Clinical Competency Questionnaire.
*Weltch t-test.
**Wilcox sign rank test.
ANOVA.
Correlation Between Skill Competency and Professional Behavior
The bivariate correlation analysis showed that the score of students’ skill competency was positively and significantly associated with the professional behavior score (R2 = 0.83, p < .0001; Figure 1).

A scatterplot depicting the correlation between students’ skill competency and professional behavior.
Discussion
This cross-sectional study evaluated the clinical skill competence and professional behaviors of undergraduate nursing students following simulation training by using an adapted CCQ which was previously validated and revealed good reliability (Cronbach's alpha > 0.9) for use in Saudi Arabian nursing students. The analysis revealed insights about clinical competency and professional behavior. In terms of skill competencies, the students showed a high level of competence in sterile techniques, oral medications administration, and carrying out hygiene and daily care routines. But students acknowledged weakness in shift reports using SBAR, assessing gastrotomy tube placement, and administering secondary IV antibiotics. In terms of professional behaviors, students have demonstrated strong self-perceived in maintaining the appropriate appearance, understanding group goals, and respecting patient rights. In contrast, accepting constructive criticism, preventing patient problems, and demonstrating cultural competence need further improvement.
The study did not find significant difference in overall or subscales on academic year and students’ gender. Despite the lack of statistically significant difference in the skill competency score among different age categories, the old age group has lower overall and professional scores compared to the younger group. Additionally, the current study results identified significant relationships between nursing students perceived clinical competence scores and their skill competency and professional behavior. Overall, these results highlight the significance of integrating high-fidelity simulation training into nursing education programs. They emphasize the need to address skill development, professional behavior, and self-efficacy to enhance students’ clinical competence. Additionally, the findings underscore the importance of considering individual factors and providing a supportive learning environment to optimize the effectiveness of simulation-based training.
In comparison with previously published studies, this study aligns with Pol Castañeda et al. (2022), demonstrating improvements in medication administration and addressing weaknesses in reporting and documentation among 179 2nd-year nursing students at a Spanish university using a mixed-method design. Students expressed satisfaction with the simulation's ability to bridge theory and practice, highlighting its utility as a teaching resource to enhance patient safety in medication administration. This alignment suggests consistency in the positive impact of simulation-based activities on nursing education, particularly in enhancing medication administration competence among students. Similarly, Arslan et al. (2018) conducted a quasi-experimental design among 3rd-year undergraduate nursing students in Turkey and found that simulation enhanced practical skills and self-efficacy in pediatric competencies. This suggests that simulation-based training has the potential to benefit students across various specialties within nursing education. Regarding self-confidence and quality of care, this study aligns with Bailey and Emory (2022, who conducted a study to examine the changes in confidence levels among nursing students following the introduction of a realistic obstetrics simulation. He found that enhancing student confidence through simulated learning environments can lead to enhanced patient care and clinical performance by fostering a sense of competence and preparedness among nursing professionals. Additionally, Guerrero et al. (2022) conducted a quasi-experimental study to explore the influence of high-fidelity simulation on critical thinking skills, satisfaction, and self-confidence among nursing students and staff nurses in Saudi Arabia. Results revealed significant improvements in critical thinking skills and reporting high levels of satisfaction and self-confidence postsimulation sessions. Overall, high-fidelity simulation emerged as an effective method for enhancing self-confidence and competencies in nursing education and practice.
Furthermore, the current study findings corroborated with a study conducted among 117 female nursing students in Saudi Arabia, reported that nursing students expressed high satisfaction with their clinical simulation experience, as well as, increased self-confidence, particularly in recognizing symptoms, performing necessary tasks, and engaging as effective team members, indicating the efficacy of simulation in enhancing both satisfaction and self-confidence (Omer, 2016). Another randomized controlled study involving 38 Jordanian nursing students in both experimental and control groups demonstrated the experimental group, which received simulation scenarios in addition to theoretical and clinical training, showed markedly superior enhancements in both knowledge and confidence in contrast to the control group, highlighting the efficacy of simulation in enhancing nursing students’ critical care skills (Tawalbeh, 2020). Furthermore, the need for further improvement in cultural competence highlighted in the current study aligns with the findings of integrative literature reviews by Marja and Suvi (2021) and Foronda et al. (2018). These reviews emphasize the instrumental role of simulation activities in nurturing students’ cultural sensitivity and competence, thereby refining communication skills and increasing confidence levels when engaging with patients from diverse backgrounds.
Strengths and Limitations
It is important to acknowledge the limitations of this study. The single-center nature of the research, conducted exclusively at the University of Tabuk, may restrict the generalizability of findings to other nursing programs with different contexts and resources. The utilization of convenience sampling introduces potential selection bias, as participants who volunteered may not fully represent the diverse population of nursing students. Relying on self-reported data for assessing competencies and behaviors may introduce response bias and social desirability. The cross-sectional design limits the ability to establish causations or observe changes over time, while the absence of a control group hinders the ability to make direct comparisons and draw causal inferences. Furthermore, the study predominantly relies on self-assessed competency scores, and the short duration of data collection might not capture long-term variations in competency development. To address these biases in future research, future studies should employ randomized sampling methods for more representative samples and use direct observations by trained evaluators for objective assessments. Longitudinal studies could provide stronger evidence on the long-term impact of simulation training on nursing students’ skills and professional behaviors. Despite these limitations, the study provides valuable insights into the perceived impact of simulation training on nursing students and identifies areas for future research and improvement in nursing education.
Implications for Practice
The current study findings underscore several critical implications for nursing practice. Firstly, targeted educational interventions should be implemented to address identified skill gaps among nursing students, thereby enhancing their clinical competencies, and ensuring a comprehensive education. Secondly, the integration of simulation training into nursing programs is essential for providing students with practical experience in a controlled environment, fostering the development of necessary skills and self-confidence. Thirdly, alongside clinical skills, the importance of professional behavior cannot be overstated. Incorporating scenarios that emphasize professional conduct will better prepare students for real-world clinical settings. These implications emphasize the importance of continuous improvement in nursing education to better prepare students for the challenges of clinical practice.
Conclusion
This study demonstrated the insignificant impact of simulation training on the skills, competencies, and professional behaviors of nursing students at the University of Tabuk. While students displayed high overall clinical competency, areas needing improvement were identified, emphasizing the need for targeted educational interventions. The findings revealed a strong positive correlation between simulation training and enhancing nursing students’ skills, competencies, and self-confidence. Additionally, the study revealed a significant association between skill competency and professional behavior. Although age influenced scores, no significant relationships were found with academic year or gender. Further investigating the influence of age on scores is important to understand its implication simulation training strategy. The results highlight the importance of integrating simulation training into nursing education, recognizing its role in fostering well-rounded clinical competence. This study recommended incorporating simulation training in nursing education, which enhances professional behaviors like appearance, group goals, and patient rights, but requires improvement in constructive criticism, problem prevention, and cultural competence. Also, this study recommends performing more studies with appropriate sampling method and exploring more diverse institutions and student years with developing the simulation program focusing on SBAR shift reports, assessing from gastrostomy tube, and administering IV medications, also, focusing on enhancing professional behaviors.
Supplemental Material
sj-docx-1-son-10.1177_23779608241274194 - Supplemental material for Evaluating Clinical Skill Competence and Professional Behaviors in Nursing Students Following Simulation Training at the University of Tabuk
Supplemental material, sj-docx-1-son-10.1177_23779608241274194 for Evaluating Clinical Skill Competence and Professional Behaviors in Nursing Students Following Simulation Training at the University of Tabuk by Muna Mutlag Albalawi and Khulud Ahmad Rezq in SAGE Open Nursing
Supplemental Material
sj-docx-2-son-10.1177_23779608241274194 - Supplemental material for Evaluating Clinical Skill Competence and Professional Behaviors in Nursing Students Following Simulation Training at the University of Tabuk
Supplemental material, sj-docx-2-son-10.1177_23779608241274194 for Evaluating Clinical Skill Competence and Professional Behaviors in Nursing Students Following Simulation Training at the University of Tabuk by Muna Mutlag Albalawi and Khulud Ahmad Rezq in SAGE Open Nursing
Footnotes
Acknowledgments
The authors would like to express their gratitude to all the participants who took part in this study. We sincerely appreciate their valuable time and active involvement, which contributed to the successful outcome of this research.
Author Contributions
Conceptualization: K.A.R. and M.M.A.; data curation: K.A.R. and M.M.A.; formal analysis: K.A.R. and M.M.A.; investigation: K.A.R. and M.M.A.; methodology: K.A.R. and M.M.A.; project administration: K.A.R. and M.M.A.; resources: K.A.R. and M.M.A.; software: K.A.R. and M.M.A.; supervision: K.A.R. and M.M.A.; validation: K.A.R. and M.M.A.; writing original draft: K.A.R. and M.M.A.; writing—review and editing: K.A.R. and M.M.A.
Data Availability Statement
All data are available upon contact with the corresponding author.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Consideration
Ethical approval was obtained from the IRB of University of Tabuk (UT-227-70-2022) on September 12th, 2022, Tabuk, Saudi Arabia. At the beginning of the survey, students were informed about their right to participate or withdraw from the study. The consent was taken at the beginning of the survey (by clicking on yes or no) before starting to answer the survey. To maintain privacy of the participant information, all the data were stored in the primary researcher's computer and only researchers related to this study had access to the data.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Prior to beginning the online questionnaire, participants were provided with a comprehensive information sheet to ensure informed consent.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
