Abstract
Introduction
The marked increase in the number of individuals with diabetes mellitus (DM) worldwide each year has resulted in the importance of the spouse's contribution to the promotion and support of patient self-management programs.
Objectives
This study aimed to systematically explore the role or involvement of spouses in collaborative management and glycemic behavior change in DM.
Methods
Five databases including Scopus, PubMed, Cumulative Index of Nursing and Allied Health Literature, SAGE, and Web of Science were reviewed for relevant articles retrieved from 2017 to 2022. Literature search used keywords, including “Spouse,” “Support,” “Self-management,” “Glycemic Control,” and “Diabetes mellitus.” The Joanna Briggs Institute guidelines were used for appraisal review of journals. The component of partner support in the self-management of patients with DM is associated with an increase in the patient's glycemic level.
Results
Twenty-five studies were identified that describe the different spousal roles and strategies in the promotion and support of DM management. Overall, spouses’ involvement positively impacted healthy diets, higher self-efficacy, improved quality of psychological well-being, increased perceived support, and changes in glycemic-influenced behavior. Adaptation in the spouse patient relationship including maintaining cohesiveness can result in positive coping is essential in normalizing and contextualizing the chronic condition of DM. Partner-based collaboration is important for diabetes management, overcoming management barriers, and generating communal coping.
Conclusion
This systematic review observed that the involvement of a spouse is important in improving collaborative management and results in better glycemic behavior in patients with DM. A better understanding of the relationship between spousal involvement, coping strategies, and adherence in daily management and the subsequent use of this information are highly useful for creating targeted and effective interventions.
Introduction
The global trend toward increasing cases of diabetes mellitus (DM) occurs in almost all countries. To date, approximately 425 million adults have DM, and this number is expected to continue to increase until 2045, with the number reaching 629 million, which is equivalent to a 48% increase (International Diabetes Federation, 2021). Spouses have a 26% increased risk of developing diabetes, highlighting the importance of collective effort to optimize healthy diet and physical activity (Gupta et al., 2019). Compared with age, urbanization level, and comorbidities (all P < .05), spouses contributed the highest (5.19%, P < .0001) to improving conditions in patients with diabetes (Wang et al., 2017).
Self-management behavior is critical and positively contributes to efforts for treating DM and preventing potentially fatal complications, particularly in type 2 DM (T2DM) (Rostampour et al., 2020). Management efficacy refers to consistent effective attitudes and efforts to improve the patient's quality of life, as well as elaborating medical management, psychological conditions, and behavioral compliance (Roberts et al., 2019). The long-term quality of life of patients with DM is markedly influenced by positive disease management, not only associated with physiological indicators but also minimal risk of complications (Hunt, 2015). One of the obstacles in the management behavior of patients with DM in studies conducted in developed countries such as Singapore, Canada, the United States, and the United Kingdom is low family support (Chithambo & Forbes, 2015; Compeán-Ortiz et al., 2018; Poole et al., 2020). Some research results have stated that interventions involving families particularly motivational support from spouses (Withidpanyawong et al., 2019) considerably improve management activities in DM. A powerful factor for the health of the couple that must be considered and utilized in disease management is the marital relationship (Liao et al., 2020). Patients with T2DM who receive spousal support have higher adherence to treatment (71%) than those who do not receive spousal support (52%) (P = .03, χ2) (Haines et al., 2018). Positive coping mechanisms influenced by a spouse emerge when the patient's chronic illness as a source of stressor can be viewed as a shared problem (Helgeson et al., 2017). Positive coping from the spouse can contribute to reducing the distress experienced by the patient, and joint efforts are made in managing the disease and improving the patient's self-efficacy (Helgeson et al., 2020; Liljeroos et al., 2021).
The limited support from the spouse that the patient receives will impact ineffective self-management (Soriano et al., 2021). As individuals who live in a family, all family members including the spouse have been shown to play a vital role in contributing to DM management (Tu et al., 2021). Moreover, partner relationship quality is associated with better glycemic control among individuals with diabetes (Helgeson et al., 2017). A spouse's contribution to self-care for T2DM affects the stability of glycemic levels in patients with T2DM (P = .041) (Soriano et al., 2021). Comanagement efforts with spouse participation are hypothesized to produce effective and sustainable outcomes in diabetes management (Seidel et al., 2012). Living with a spouse plays an important role in the positive implementation of DM management. This study aimed to systematically explore the role or involvement of partners in collaborative management and glycemic behavior change in patients with DM.
Methods
Design
This review describes the role or involvement of partners in collaborative management and glycemic behavior change in patients with DM. The type of research used was a systematic review through searching for articles in four databases, including Scopus, PubMed, Cumulative Index of Nursing and Allied Health Literature (CINAHL), SAGE, and Web of Science (WOS). A systematic review involves finding, reading, understanding, and forming conclusions about the published study and theory and presenting it in an organized manner (Brink et al., 2012). The Preferred Reporting Items for Systematic Reviews and Meta-Analyses checklist was used in developing this review (Supplementary) (Arya et al., 2021). This systematic review has been registered with PROSPERO (registration number CRD42023470510).
Eligibility Criteria
The search used four databases, including Scopus, PubMed, CINAHL, SAGE, and WOS, which were reviewed for relevant articles retrieved from 2017 to 2022. Literature search was performed using keywords that are adjusted to the Medical Subject Headings (MeSH), including “Spouse” OR “Couple” AND “Diabetes” OR “Diabetes mellitus” OR “Type 2 Diabetes mellitus” AND “collaboration” OR “support” AND “Self-management” OR “Self-care” AND “Glycemic Control” OR “Blood glucose.” The following were the inclusion criteria of the articles: (a) published in English, (b) original research, and (c) published in a peer-reviewed journal. We excluded studies that did not discuss the role or involvement of partners in collaborative management and glycemic behavior change in patients with DM.
Study Selection
Based on the results of a literature search on four databases using keywords that have been adapted to MeSH, the researchers identified 5,666 articles. Three reviewers (IN, NN, and IYW) independently screened the articles by applying the inclusion criteria, resulting in 797 articles, including Scopus (n = 123), PubMed (n = 74), CINAHL (n = 31), SAGE (n = 500), and WOS (n = 69). Next, the four databases were searched for duplicates (n = 128), followed by eligibility by excluding titles and abstracts whose study participants were not family members or patients with DM (n = 242), exposure/intervention were not related to partner collaboration/support (n = 222), outcomes were related to chronic disease (n = 64), and the study type was article review (n = 87); finally, 54 article titles and relevant abstracts were obtained. Subsequently, the availability of full-text articles was searched, and full-text articles wherein participants were not partners of patients with DM (n = 2), did not discuss the role of partners (spouse/couple) in diabetes self-management/self-care (n = 4), the outcome was chronic disease (n = 3), and the study type was article review (n = 3) was excluded (Figure 1) (Page et al., 2021). If any discrepancy or disagreement is noted between the reviewers during the screening process, it will be discussed until a consensus is reached.
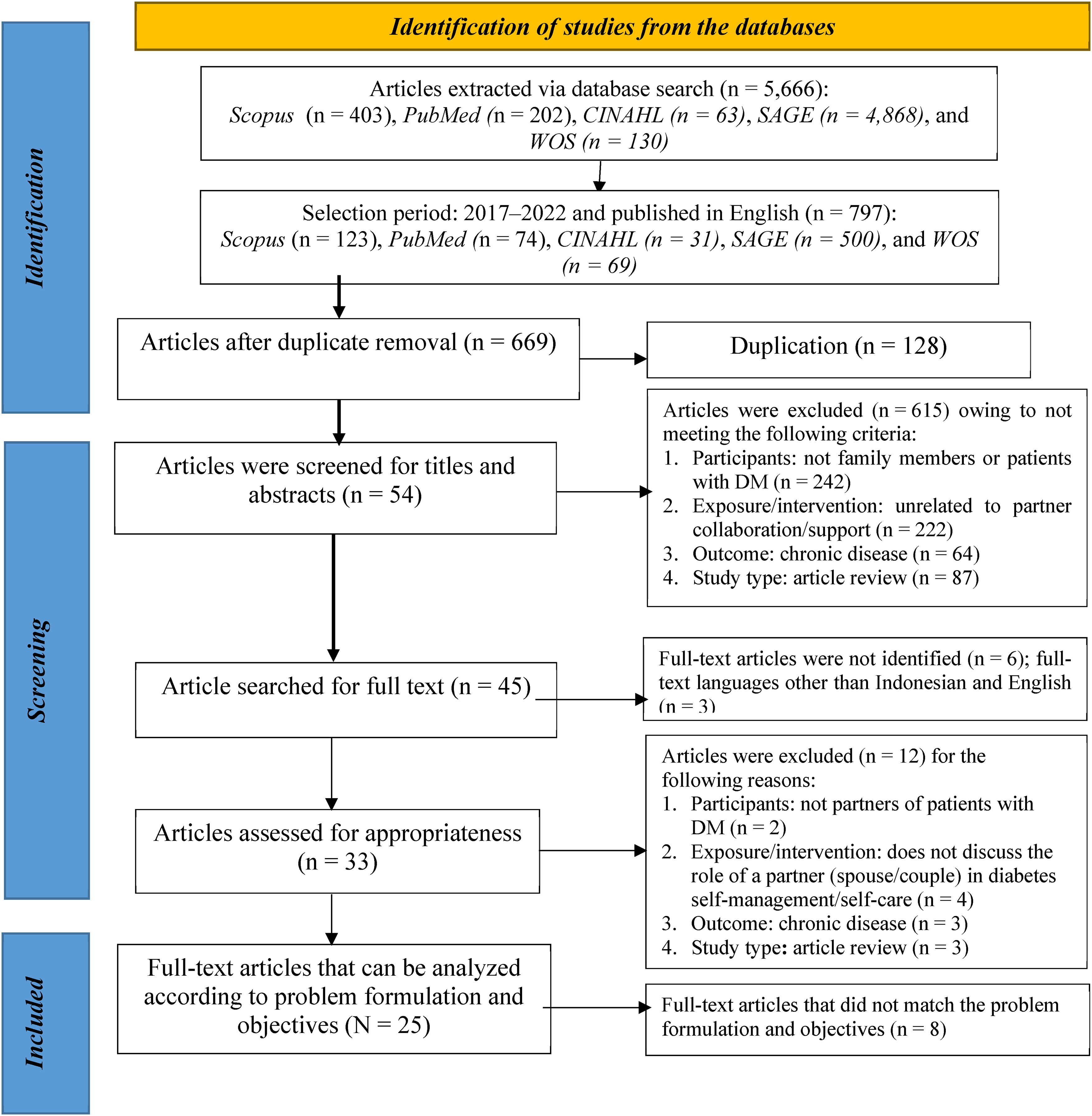
Preferred Reporting Items for Systematic Reviews and Meta-Analyses search article according to the criteria.
Methodological Quality Assessment
The authors identified research quality by considering the risk of bias by assessing the methodological quality of a study and determining the extent to which a study addressed possible biases in its design, implementation, and analysis. For this purpose, this systematic review uses the Joanna Briggs Institute (JBI) Critical Appraisal tool, which follows the research design used (The Joanna Briggs Institute, 2023). Three reviewers (IN, NN, and IYW) independently assessed the articles that met the inclusion criteria by assessing the validity of the methodology before being included as a review using the critical appraisal review assessment from the JBI for several types used, including cross-sectional studies (Moola et al., 2017), cohort studies (Joanna Briggs Institute, 2017), randomized controlled trials (RCTs) (Barker et al., 2023), and qualitative studies (Lockwood et al., 2015). The JBI-based checklist lists several questions to assess the quality of the study. The JBI for cross-sectional studies includes eight questions regarding inclusion criteria, study participants and settings described, exposures measured, standard criteria used for condition measurement, confounding factors and strategies for dealing with them, outcomes measured, and statistical analyses used (Moola et al., 2017).
The JBI for cohort studies includes 11 questions regarding similar characteristics in relation to exposure, how exposure was measured, confounding factors, outcomes measured, reported, adequate follow-up times, strategies to address incomplete follow-up, and statistical analyses used. The JBI for RCTs includes 13 questions regarding randomization used, allocation to a blinded group, treatment group, blinded participants, blinded outcome assessors, follow-up, outcomes measured, and statistical analyses used (Joanna Briggs Institute, 2017). The JBI for qualitative studies includes 10 questions regarding internal validity and risk of design bias, specifically confounding, selection, and information bias, as well as clear reporting (Lockwood et al., 2015).
The assessment criteria were provided a rating of “yes,” “no,” “unclear,” or “not applicable”; each “yes” rating was assigned one point, and the other ratings were assigned zero. Each rating was subsequently calculated and summed. If the research rating was at least 50%, it met the critical appraisal at the cutoff point. The risk of bias in this literature review used an assessment of the research methods of each study, including in the aspects of theory, design, samples, variables, instruments, and data analysis.
Results
Characteristics of the Selected Studies
Assessment of the results obtained by the included articles is shown in Table 1. Twelve articles with the checklist for analytical cross-sectional studies received a “yes” rating with a score of 8/8 (100%) with good quality, three articles received a “no” rating on the sixth and eighth questions with a score of 7/8 (87%) with good quality, and one article received a “no” rating on the sixth and eighth questions with a score of 6/8 (75%). Of the four qualitative studies with 1–10 question criteria, only one article received a “no” rating with a score of 9/10 (90%) but was still categorized as of good quality. Of the four RCTs with 1–13 question criteria, only two received two “no” ratings with a score of 11/13 (85%) but were still categorized as of good quality. One cohort study with 1–11 question criteria received two “no” ratings with a score of 9/11 (82%) but was still categorized as of good quality. Of the four RCTs with 1–13 question criteria, only two received two “no” ratings with a score of 11/13 (85%) but were still categorized as of good quality. The results of the review of the 25 articles achieved a score of >50%, fulfilling the critical appraisal, by which the data will subsequently be analyzed.
Assessment of the Study Results Criteria.

The results obtained by 25 articles published from 2017 to 2022 and published in English comprising 16 articles with cross-sectional studies, one article with cohort studies, four articles with RCTs, and four articles with qualitative studies are presented in Table 2. Of the articles, 17, 3, and 2 were conducted in the United States, China, and the United Kingdom, respectively. One article each was conducted in Ireland, Thailand, Portugal, and Canada.
Results of the Literature Search.

Role or Involvement of Partners in Collaborative Management and Glycemic Behavior Change in DM
Of the 25 articles that met the assessment criteria, all agreed that support in the form of collaboration and consistent spouse involvement in the daily management of patients with DM had an effect on patient compliance management and the ability to maintain good glycemic behavior. Spouse involvement is associated with assistance in the daily management of DM, including diet compliance, monitoring physical activity levels, monitoring blood glucose, monitoring medication or insulin therapy, and providing psychological support to patients (August et al., 2021; Berg et al., 2020; Berry et al., 2018, 2020; Fincham et al., 2018; Haines et al., 2018; Helgeson et al., 2017, 2020, 2021, 2022; Kelly et al., 2020; Lafontaine et al., 2020; Lee et al., 2019; Liu et al., 2021; Pereira et al., 2019; Reaney et al., 2018; Soriano et al., 2021; Trief et al., 2019; Tu et al., 2021; Van Vleet et al., 2019; Withidpanyawong et al., 2019; Wooldridge et al., 2019; Wooldridge & Ranby, 2019; Yue et al., 2019; Zajdel et al., 2018) (Table 2).
When DM is initially diagnosed, the patient's perception of the importance of positive support contributes to better blood glucose monitoring compliance later in life. However, it is also associated with the emergence of a spouse's perception in the form of positive support in communicating about treatment and chronic disease programs that are needed by patients openly and vice versa (Berry et al., 2018; Helgeson et al., 2022; Pereira et al., 2019; Van Vleet et al., 2019; Yue et al., 2019). Spouse involvement relates to daily diabetes outcomes, including influencing self-regulation, self-care, mean blood glucose, and perceived coping effectiveness (Berg et al., 2020; Fincham et al., 2018; Soriano et al., 2021; Yue et al., 2019). Important constructions in maintaining and strengthening self-efficacy in DM management are associated more with the role of the spouse in collaboration to achieve the expected intervention targets in patients with DM, achieving relationship satisfaction, and the support of health care providers (Berry et al., 2018; Fincham et al., 2018; Helgeson et al., 2017, 2020, 2022; Lafontaine et al., 2020; Lee et al., 2019; Trief et al., 2019; Wooldridge & Ranby, 2019).
Coping Strategies
Adaptation in the spouse–patient relationship including maintaining cohesiveness can result in positive coping, which is essential in normalizing and contextualizing the chronic condition of DM, especially for diabetes management and overcoming management barriers known as communal coping (Helgeson et al., 2022; Liu et al., 2021; Van Vleet et al., 2019; Zajdel et al., 2018). A communal coping environment was associated with lower feelings of depression, higher feelings of happiness, and lower periods of anger. Communal care between patients and partners was associated with better adherence to diet and medication management. By providing psychological support for illness and increasing adherence in disease management, daily communal care can help patients and spouses adapt positively to diabetes conditions (Helgeson et al., 2017; Van Vleet et al., 2019; Zajdel et al., 2018). Spouses’ more communal interaction and collaborative support represent disease management; such interactions are essential in a constructive strategy of overcoming perceived problems through more positive interactions. However, several studies have also reported that spouse communal coping is more consistently linked as a form of support only; however, long-term positive changes will occur if communal coping is also present in the patient (Van Vleet et al., 2019).
Discussion
This study identified 25 studies that described the different roles and strategies of partners in the promotion and support of DM management. All of the included studies agreed that support in the form of collaboration and consistent spouse involvement in the daily management of patients with DM had an effect on patient compliance management and the ability to maintain good glycemic behavior. Although existing literature supports the relationship between the effect of spousal support and subjective indicators of disease management (Craddock et al., 2015), whether there are significant clinical changes because of spousal support remains unclear. Several studies have examined the effect of spousal support in DM and hemoglobin A1c (HbA1c) management and have reported mixed results (Faizah et al., 2020; Fajriyah et al., 2020; Mayberry et al., 2019). The HbA1c is an indicator of DM glycemic control that reflects the portrait of blood glucose levels in the last 8–12 weeks in blood vessels. It is used as the main indicator for assessing the variability of body glucose levels. Variability is used for predicting the final complications of DM, both microvascular and macrovascular complications (Ganetsky et al., 2022; Vigersky et al., 2018).
Furthermore, this literature review noted that spousal perceptions of positive support play a role in medication and diabetes control adherence following DM diagnosis, whereas the increase in disease chronicity and negative perceptions of diabetes symptoms among spouses can reduce DM management adherence (Costeira et al., 2022; Morris & Sanders, 2018; Weitkamp et al., 2021). To maintain and strengthen self-efficacy in diabetes management, several studies associated relationship satisfaction factors with partner collaboration in contributing to target achievement and support from health care providers as a construct (Szabó-Bartha & Mirnics, 2021; Wooldridge et al., 2019; Wooldridge & Ranby, 2019). An understanding of related theory is important as a foundation for effectively collaborating with a spouse in a self-management intervention in a behavioral context (Pamungkas et al., 2017).
In this review, we observed partner-based collaboration for diabetes management, overcoming management barriers, and generating communal coping. Overall, spouse involvement resulted in consistent improvements in self-efficacy, dietary adherence, psychological well-being, glycemic control, and sources of support. To normalize and contextualize the chronic condition of DM, adaptation in a marital relationship including maintaining cohesion between partners is significant (Helgeson et al., 2022; Liu et al., 2021; Van Vleet et al., 2019; Zajdel et al., 2018). A communal coping environment was associated with lower feelings of depression, higher feelings of happiness, and lower periods of anger. Communal care between patients and partners was associated with better adherence to diet and medication management. By providing psychological support for illness and increasing adherence to disease management, daily communal care can help patients and spouses adapt positively (Helgeson et al., 2017; Van Vleet et al., 2019; Zajdel et al., 2018). Management behavior that refers to long-term management and compliance plays an important role in maintaining and supporting treatment efforts and maintaining the psychological well-being of patients. Adherence to self-management in patients with long-term DM will improve their quality of life and is not limited to controlling physiological indicators (Hunt, 2015; Pratiwi et al., 2018; Thojampa et al., 2020). Studies conducted in developed countries such as the United States, Canada, the United Kingdom, and Singapore have reported common barriers to management, one of which is the lack of family support (Chithambo & Forbes, 2015; Compeán-Ortiz et al., 2018; Poole et al., 2020). Some research results have stated that interventions involving families particularly motivational support from partners (Withidpanyawong et al., 2019) significantly improve management activities in DM. A powerful factor for the health of the couple that must be considered and used in disease management is the marital relationship (Liao et al., 2020).
A spouse's more communal interaction and collaborative support represent disease management; such interactions are essential in a constructive strategy of overcoming perceived problems through more positive interactions. However, several studies have reported that spouse communal coping is more consistently linked as a form of support only; however, long-term positive changes will occur if communal coping is also present in the patient (Van Vleet et al., 2019). Comanagement efforts with partner participation are hypothesized to produce effective and sustainable outcomes in diabetes management (Seidel et al., 2012). In addition to preventing microvascular and macrovascular complications in patients with T2DM, self-management also has challenges in terms of limited sources of support, particularly in efforts to maintain timely intervention (Indarwati et al., 2019; Pratiwi & Purwaningsih, 2019; Soriano et al., 2021). The spouse plays an important role in self-management because in the context of the nuclear family, the spouse is referred to as the unit closest to the patient (Luthfa et al., 2020; Sinawang et al., 2020; Tu et al., 2021; Wulandari et al., 2020). Furthermore, among patients with diabetes, partner relationship quality is associated with better glycemic control (Helgeson et al., 2017).
Strengths and Limitations
In general, the study highlighted that spousal perceptions of positive support play a role in medication adherence and diabetes adherence control following DM diagnosis. To maintain and strengthen self-efficacy in DM management, several studies have agreed that spouse collaboration in achieving the desired targets in interventions, relationship satisfaction, and support from health care providers are constructs influencing DM management. Notably, the findings obtained in this review are valuable information for health care workers, especially in providing education for spouses regarding the importance of collaboration and how to achieve positive coping in disease management interactions through positive perceptions that lead to solving the challenges experienced by patients with DM.
This review mostly included cross-sectional studies (16 studies), which may not establish a causal relationship between spousal support and the coping strategies used. More concrete relationship patterns must be elaborated with respect to spouse support and positive communal coping development strategies in the longitudinal study design. Some aspects of concern in the articles obtained for review include the possibility of publication bias arising from the dominance of research with proven hypotheses compared with unproven ones. Researchers do not have access to primary data owing to several reasons, one of which is the variability of the study design; therefore, a meta-analysis is not conducted and only a narrative description is performed. Therefore, we are unable to thoroughly explain the effect sizes of each study outcome.
Implications for Practice
The findings obtained in this systematic review can support the implementation of patient spousal empowerment intervention programs by nurses in self-management. The spouse empowerment program is expected to facilitate mutual support between partners in disease management, increase patient compliance and quality of life, maintain healthy lifestyle changes in the long term, and prevent complications and disease worsening for patients. The formation of positive perceptions that will result in positive coping from spousal support will result in positive collaboration strategies in daily DM management. Daily communal coping can help patients and spouses psychologically adjust to illness and improve patient self-care behaviors. The implementation of this intervention program can be performed in the hospital when the patient is an inpatient or outpatient.
Conclusions
This systematic review noted evidence that positive spouse collaboration is crucial in maintaining good management behavior and will impact controlled glycemic conditions in patients with DM. Adaptation in the spouse–patient relationship including maintaining cohesiveness can result in positive coping, which is essential in normalizing and contextualizing the chronic condition of DM, particularly for diabetes management and overcoming management barriers known as communal coping. A better understanding of the relationship between spousal involvement and adherence in daily management and the subsequent use of this information are highly useful for creating targeted and effective interventions.
Supplemental Material
sj-docx-1-son-10.1177_23779608241245196 - Supplemental material for Spousal Involvement in Collaborative Management and Glycemic Behavior Change among Patients with Diabetes Mellitus: A Systematic Review
Supplemental material, sj-docx-1-son-10.1177_23779608241245196 for Spousal Involvement in Collaborative Management and Glycemic Behavior Change among Patients with Diabetes Mellitus: A Systematic Review by Ika Nur Pratiwi, Nursalam Nursalam, Ika Yuni Widyawati and Vimala Ramoo in SAGE Open Nursing
Footnotes
Acknowledgment
The authors would like to acknowledge the authors of the sources used in this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
