Abstract
Introduction
The COVID-19-related restrictions imposed to reduce viral transmission have highlighted the need to support the importance of maternal breastfeeding. Clear guidelines for consistent practices across settings have been drawn up on the basis of the best available data. Emerging recommendations call to increase nurses’ and midwives’ awareness of these guidelines.
Objective
This study aimed to explore nurses’ and midwives’ awareness of the recommended breastfeeding practices and associated factors in Jordan during the COVID-19 pandemic.
Methods
An online descriptive cross-sectional design was adopted. This study was conducted in clinical settings representing Jordan's North, Middle, and Southern regions. One hundred seventy nurses and midwives were selected through a convenient sampling technique.
Results
The mean total score of the awareness was 7.78 (SD = 1.60); 62.9% of participants were highly aware of the recommended breastfeeding practices. Nurses and midwives who were aware of the recommended breastfeeding practices during the pandemic of COVID-19 (90.7%) were more likely to perceive COVID-19 preventive measures as effective than those who were not aware of breastfeeding practices (74.6%) (χ2 = 7.886, p = .005), while work experience in years (χ2 = 8.966, p < .01) was significantly associated with awareness of the breastfeeding recommended practices.
Conclusion
Most Jordanain nurses and midwives were highly aware of the recommended breastfeeding practices during COVID-19 pandemic. This awareness was positively associated with working experience and perceiving that the preventive measures of COVID-19 are effective. Educational programs for nurses and midwives about breastfeeding practice recommendations are necessary to help mothers obtain appropriate care and education.
Introduction
The COVID-19-related restrictions imposed to reduce viral transmission have highlighted the need to support the importance of maternal breastfeeding and keeping mothers and babies together (Walker et al., 2022). However, years of pandemic, have been seen as one of the most challenging debates in health care services in understanding their impacts on mothers and their newborns (Walker et al., 2022).
Recent reviews showed no evidence of COVID-19 transmission from the mother to the fetus (Chambers et al., 2020; Diriba et al., 2020; Yang et al., 2020). Yet, there is a risk for mothers to spread infectious airborne droplets to the neonate (Abuidhail et al., 2022; Centers for Disease Control and Prevention [CDC], 2020). The latest World Health Organization (WHO) guidelines recommended that it is unnecessary to isolate the mother with an actual COVID-19 or suspected COVID-19 infection from their newborns (WHO, 20–21).
Despite the possibility of spreading the COVID-19 virus, the advantages of breastfeeding and the importance of bonding and attachment between the mother and her newborn insist on adopting an essential practice guideline to prevent the transmission of infection and promote the growth and development of the newborn (Semaan et al., 2020). Initiation of exclusive breastfeeding within the early postpartum period with the proper application of preventive measures is an essential element of care for the breastfeeding process during the COVID-19 pandemic (Kebede et al., 2021). WHO recommends that the best element for newborn nutrition is breast milk, regardless of the mother's status of COVID-19 (WHO, 2020). Recent evidence showed that even newborns of COVID-19-positive mothers will get protection from breastfeeding against COVID-19 infection (Dong et al., 2020).
Recently, the possibility of transmission of COVID-19 has been questionable (Kimberlin & Stagno, 2020). Hence, mothers should be aware of the importance of the initiation and duration of breastfeeding and should be encouraged to continue breastfeeding even if they are confirmed or suspected of having a COVID-19 infection. In addition, they should be aware that the benefits of breastfeeding outweigh the risks of COVID-19 transmission and that the COVID-19 virus cannot spread through breastfeeding (American Academy of Pediatrics [AAP], 2020).
Maternity healthcare services are sectors that are highly affected by the COVID-19 pandemic (Green et al., 2021). Therefore, one of the key components of maternity care is the requirement for clear guidelines to promote and maintain safe breastfeeding practices across settings, and these guidelines should be prepared based on recent evidence-based resources (Green et al., 2021).
Literature Review
To date, there is little empirical evidence that reflects the level of awareness of breastfeeding practices among healthcare workers during the COVID-19 pandemic (Kebede et al., 2021). In India, the cross-sectional descriptive study showed that 54% of the participants were familiar with breastfeeding practices according to WHO recommendations during the pandemic, while 15% of the participants were completely unaware (Malik et al., 2021). Another survey reported that 80% of nursing and 58% of medical healthcare providers were aware that mothers with positive or suspected COVID-19 can provide expressed breast milk to their newborns (Rajan & Vishal, 2020). Another study was conducted in Ethiopia, and it showed that two in five healthcare workers were found to be aware of the recommended breastfeeding practices during the pandemic of COVID-19 (Kebede et al., 2021).
In Jordan, little is known about mothers and their concerns about breastfeeding during this COVID-19 pandemic. (Abuidhail et al., 2022; Hamadneh et al., 2022; Masa’deh et al., 2023). One study assessed the breastfeeding knowledge and practices of mothers during the COVID-19 pandemic. The participants were breastfeeding mothers (n = 170) who completed the online survey (Abuidhail et al., 2022). The percentage of participating mothers who are familiar with some basics of COVID-19 correct “preventive measures” was high, but they had misconceptions regarding COVID-19 transmission through breast milk (Abuidhail et al., 2022). In addition, little evidence is available regarding nurses’ and midwives’ awareness of the recommended breastfeeding practices during the pandemic of COVID-19 in Jordan. Thus, an investigation of this issue could be helpful to identify gaps in knowledge and to start effective action plans for the actual and continuous implementation of the recommendations to enhance and maintain newborn health. Therefore, our study aimed to explore nurses’ and midwives’ awareness of the recommended breastfeeding practices and associated factors in Jordan during the COVID-19 pandemic.
Methods
Design
An online cross-sectional descriptive survey was conducted.
Population
The target population was all nurses and midwives in Jordan.
Setting
The study was conducted to represent three geographical areas, including the north, middle, and south of Jordan. Data collection was performed between January 2023 and May 2023. All maternal health settings in governmental, private, educational, and maternity health centers were included.
Inclusion Criteria
The inclusion criteria were nurses and midwives being employed the selected hospitals as well as maternal and child healthcare centers and having at least 1 year of working experience.
Sample
The sample size was calculated using the OpenEpi sample size calculator (Sullivan et al., 2003). This study had an estimated sample size of 384. The link of the online survey were shared with 391nurses and midives in the selected settings, among them, 170 participents were completed the online survey, with a response rate of 43.4%.
Data Collection Instruments
A structured questionnaire was used consisting of social and demographical data, information related to working experience, and items to assess nurses’ and midwives’ awareness of the recommended breastfeeding practices during the COVID-19 pandemic.
Ethical Considerations
The study proposal was submitted for review and approval by the Research and Ethics Committee of Balq Applied University. A written or online consent form includes a description of the study's purpose and procedure. Upon conducting the study, anonymity was maintained through the following: first, only the researchers would have access to the collected data. Second, each participant was assigned a digital code number to protect their identity. Third, the online-completed questionnaires were stored on a secured computer accessible only to the principal researcher. Participation in the study was voluntary, and participants were allowed to withdraw from the study at any time.
Data Collection
Once approval had been given to conduct our study, an online questionnaire was used to collect data. The link to the instrument, including an invitation letter and consent form, was sent to the head nurses in all wards in each hospital, and maternal healthcare centers. Each head nurse in each ward was responsible for sharing the link with the nurses and midwives who only met the inclusion criteria to participate in the study. The instrument access was restricted to being submitted by each participant for only one time.
Data Analysis
Analysis of the data was performed using IBM SPSS (SPSS) version 28. We used frequency tables to describe the sample characteristics. Logistic regression was used to predict the associated factors that affect nurses’ and midwives’ awareness related to breastfeeding recommendations.
Results
Study Sample Characteristics
The total number of included nurses and midwives was (n = 170). Approximately, 42% of participants were aged 30 years or less; most of them were married (62.4%) and had an income level of 650 JD or less (73.5%). Less than half of participants had a baccalaureate degree in nursing (33.5%), (4.7%) held a baccalaureate degree in midwifery, while (67.1%) had at least 4 years of clinical experience. Most participants (54.7%) worked in governmental hospitals, and (48.2%) worked in maternity and neonate wards (Table 1).
Characteristics of Participants (N = 170).

NICU=neonatal intensive care unit.
Nurses’ and Midwives’ Awareness of the Recommended Breastfeeding Practices
Most of the participants (90.6%) agreed that COVID-19 is dangerous, yet the preventive measures for COVID-19 are effective (84.7%) (Table 2). At least 60% of participants received online training programs about COVID-19 and had training on essential newborn care. While 91.8% of participants reported that they used the Internet as a source of information on COVID-19, 84.7% followed the updated guidelines of the WHO/CDC COVID-19 regarding the practices of breastfeeding during the pandemic.
COVID-19-Related Clinical Characteristics of Participants (N = 170).
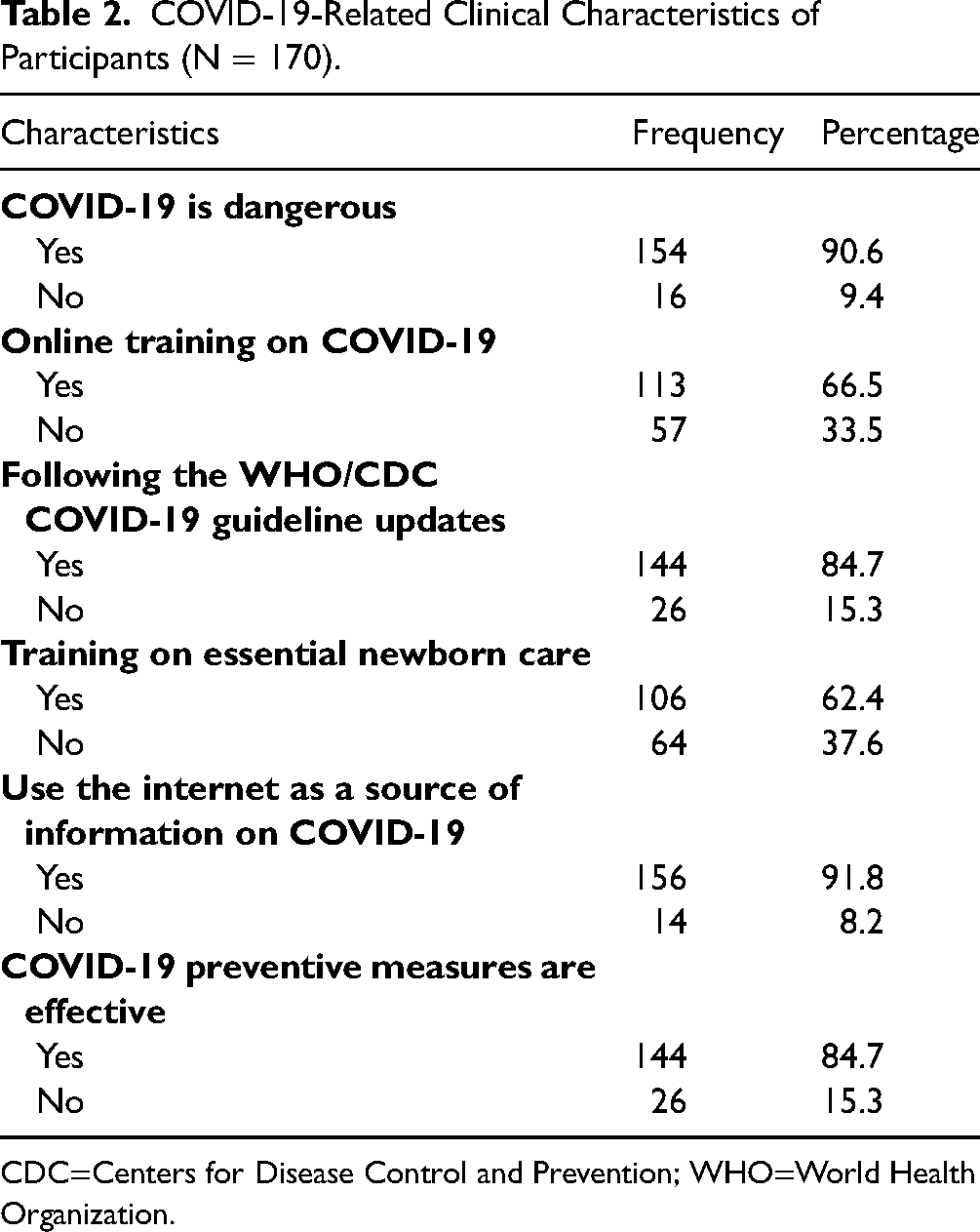
CDC=Centers for Disease Control and Prevention; WHO=World Health Organization.
Table 3 shows the responses regarding the awareness of recommended breastfeeding practices. The mean of the total score was 7.78 (SD = 1.60); 62.9% of participants had a score above the mean, indicating being highly aware of the recommened breastfeeding practices. The most frequent responses (> 80%) were about: “the mother should be told that the benefit of breastfeeding outweighs the potential risks of COVID-19 transmission” (84.1%); “umbilical cord should be clamped as usual” (88.8%); “breastfeeding should be initiated within one hour after delivery” (90.0%); “direct breastfeeding is recommended” (88.8%); “a COVID-19 suspected or confirmed mother should take routine precaution measures” (90.0%); and “Rooming-in is recommended” (82.9%).
The WHO Breastfeeding Practice Recommendations During COVID-19 Pandemic in Suspected or Confirmed Cases (N = 170).

WHO=World Health Organization.
The least frequent responses were for two items: “Mother with COVID-19 can give expressed breast milk if she is too unwell to directly breastfeed” (71.2%) and “Donor human milk can be used if a woman is severely infected with COVID-19” (60.9%).
Factors Associated With Nurses’ and Midwives’ Awareness of the Recommended Breastfeeding Practices
Among sociodemographic and clinical characteristics, only work experience in years (χ2 = 8.966, p < .01) was significantly associated with the awareness of breastfeeding recommended practices (Table 4). In addition, those who were aware of the recommended breastfeeding practices (90.7%) were more likely to perceive that the preventive measures of COVID-19 are effective than those who were not aware of the recommended breastfeeding practices (74.6%) (χ2 = 7.886, p = .005).
Factors Associated With Nurses’ and Midwives’ Awareness of the Practice Recommendation for Breastfeeding During the COVID-19 Pandemic.

CDC=Centers for Disease Control and Prevention; NICU=neonatal intensive care unit; WHO=World Health Organization.
Predictors of Nurses’ and Midwives’ Awareness of the Recommended Breastfeeding Practices
Through multivariable logistic regression analysis, we found that nurses and midwives with less experience were less likely to be aware of breastfeeding practices compared to those with a high level of experience (adujusted odds ratio [AOR]: .140; 95% confidence interval [CI]: .028–.697, p = .006). Finally, nurses and midwives who reported that COVID-19 preventive measures are effective had five times the odds of the awareness of breastfeeding practices compared to those who did not report that COVID-19 measures are as effective (AOR: 5.452; 95% CI: 1.755–16.931, p = .003) (Table 5).
Logistic Regression Modeling the Predictors of Nurses’ and Midwives’ Awareness of the Practice Recommendation for Breastfeeding During the COVID-19 Pandemic.

AOR=adjusted odds ratio; CDC=Centers for Disease Control and Prevention; NICU=neonatal intensive care unit; WHO=World Health Organization.
Discussion
The COVID-19 pandemic presents the largest public health threat in healthcare settings (Amro et al., 2022). In this context, nurses and midwives must be aware of the national and international guidelines, in addition to the most recent evidence, to be able to provide qualified maternal care (Ng et al., 2020). Regarding this, this cross-sectional study aimed to explore nurses’ and midwives’ awareness of the recommended breastfeeding practices during the COVID-19 pandemic and the associated factors in Jordan. Accordingly, two-thirds of participants were aware of the recommended breastfeeding practices during the COVID-19 pandemic. Work experience years and perceiving that COVID-19 preventive measures are effective were significantly associated with awareness of the recommended breastfeeding practices during the COVID-19 pandemic.
In this study, 62.9% of the participants were aware of the breastfeeding practice recommendations during the pandemic in Jordan, which is higher than similar studies conducted in India (54.1%) (Malik et al., 2021) and Ethiopia (40.7%) (Kebede et al., 2021). This may suggest that Jordanian nurses and midwives had access to updated information reported by WHO during COVID-19 pandemic. Congruently, Ng et al. (2020) in their significant discussion paper reported that nurses and midwives are aware of recommended guidelines by international organizations, especially WHO recommendations. Regardless, this finding is inconsistent with a study conducted in the United Arab Emirates (Bhagavathula et al., 2020). Researchers found that there was insufficient information about the transmission of COVID-19, and important signs were found among healthcare workers including nurses. Hence, future studies are required to address how health systems across countries shaped the access to information pertaining the transmission of COVID-19 and how such access might affect breastfeeding practices among mothers with COVID-19.
The majority of the participants (90.0%) in this study were aware of the recommendations regarding direct breastfeeding and rooming-in. This result is higher than the result found in previous literature, Kebede et al. (2021) found a third (33.6%) and one-fifth (21%) of health care providers (HCPs) know rooming-in as essential for routine protection for mothers supposed or confirmed COVID-19. Besides, about (89%) of the participants were aware that the initiation of breastfeeding should be within the first-hour postdelivery and that the mother with a suspected or confirmed infection of COVID-19 should be aware of the routine precautionary measures. Similarly, about (73.1%) of HCPs know that breastfeeding should be initiated within 1h after delivery. A mother can breastfeed her newborn, breastfeeding should be initiated within hours after birth, regardless if she has a positive or negative COVID-19 test (Kebede et al., 2021). Researchers suggested that this concern frames health policy-makers to regularly provide updated information and organize training opportunities for HCPs regarding breastfeeding practices during the COVID-19 pandemic (Kebede et al., 2021). Interestingly, more than three-quarters (84%) of the participants in our study agree that they should be informed that the benefits of breastfeeding during the pandemic outweigh the potential risks.
This study revealed that nurses and midwives who were more experts were more likely to be aware of the recommended breastfeeding practice guidelines compared with nurses and midwives with fewer experience years. This result is consistent with a study conducted in a university hospital in Egypt (Abdelglil et al., 2022). The results of that study showed that nurses and midwives who have higher years of experience were more likely to have higher levels of knowledge than nurses and midwives who have lower years of experience. Moreover, nurses and midwives who have more than 10 years of experience had higher odds of awareness of the recommended breastfeeding practices even after adjusting for other factors. This was expected because most of the expert nurses are likely to be the leaders and the charge nurses in their unit, and they are required to always be updated with the latest recommendations and guidelines. In addition, this is consistent with a study conducted by Wen et al. (2021) in China, which reported that nurses who have more than 20 years of experience reported higher scores of knowledge, attitude, and practice of COVID-19 than nurses with <10 years of experience.
Likewise, reporting that the preventive measures of COVID-19 are effective was significantly affecting the nurses’ and midwives’ awareness of the recommended breastfeeding practices during COVID-19. Thus, nurses and midwives who reported that the preventive measures of COVID-19 are effective had five times the odds of awareness compared to those who did not agree with the effectiveness of the COVID-19 measures. This may reflect one assumption of the Health Belief Model that assumes that the perceived benefits of health action—which is reflected here by the effectiveness of preventive measures for COVID-19—will lead the person to take the action to avoid transmission of COVID-19 (Maiman & Becker, 1974).
Therefore, the nurses and midwives who perceived that the preventive measures were effective in preventing the transmission of COVID-19 would take action and have the stimuli to be aware of these guidelines. While there is limited number of studies addressing factors associated with the awareness of WHO breastfeeding recommendations during COVID-19, previous studies showed that perceived benefits of preventive measures for COVID-19 were significantly associated with increased awareness of health-related practices (Elgzar et al., 2020; Shi Y et al., 2020; Stirling et al., 2015; Alsulaiman & Rentner, 2018). For example, a study assessed the awareness of Saudi nursing students regarding COVID-19 including the preventive measures showed that students who received the education program have a significantly higher awareness of COVID-19 than students who did not receive the educational program (Elgzar et al., 2020). Hence, the current study contributes to our understanding of factors related to the awareness of midwives and nurses of recommended breastfeeding practices during COVID-19 pandemic.
Strength and Limitation
The strengths of the study include its novelty in the Jordanian context and using a standardized instrument to assess nurses’ and midwives’ awareness. In addition, this study was multisite targetting nurses and midwives in many areas in Jordan. However, there are some limitations in this study. First, a cross-sectional design was used, and thus it could be hard to discern the cause-and-effect relationship between the dependent and independent variables. Second, the sampling technique was convenience and the response rate was only 43.4%, suggesting a potential selection bias. Third, since the questionnaire was self-administered, recall and social desirability biases could affect the validity of the responses. Finally, this study only examined awareness of recommended breastfeeding practices among nurses and midwives without addressing the aspects of implementation of these practices and perceived barriers to such implementation.
Implications for Practice
This study provides evidence and data that helped in identifying the level of awareness and factors associated with breastfeeding practice recommendations among nurses and midwives in Jordan. The majority of Jordanian nurses and midwives were aware of these recommendatios; significant predictors included the level of clinical experience and perceiving that the preventive measures are effective in preventing the spreading of COVID-19. Therefore, these findings could guide managers in developing continuous education and training programs in each healthcare setting to promote and maintain the application of breastfeeding practices among healthcare providers. In addition, an orientation program for new staff with less clinical experience needs to address these recommendations. While insisting on the vital role that nurses and midwives could play in achieving the continuity of the recommended breastfeeding guidelines during their practices
Conclusion
This study is one of the first to explore awareness of the recommended breastfeeding practice among nurses and midwives during the COVID-19 pandemic in Jordan. Thus, follow up is essential through the conduct of educational programs for nurses and midwives, especially those with a lower level of awareness about breastfeeding practice recommendations. Also, further studies are needed to identify barriers and facilitators to implementing breastfeeding practice recommendations during the pandemic by nurses and midwives.
Footnotes
Acknowledgements
The authors acknowledge all the participants of the study. In addition to Noor Abueid, RN, Islamic Hospital, we appreciated her efforts in data collection procedure.
Author Contributions
SJ and TS were involved in conceptualization; SJ, TAT, and EHM in data curation; TS in formal analysis; SJ, TS, TAT, and AR in methodology; SJ and SAJ in project administration; and SJ, TS, AR, TAT, YAS, and FS in writing—review and editing of the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Statement
Ethical approval was obtained from the Institutional Ethical Review Board (IRB) of the University of Balqa Applied University.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
