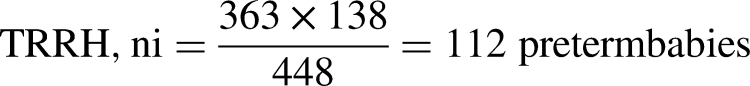Abstract
Introduction
Kangaroo mother care (KMC) has been proven to reduce preterm babies’ deaths by 40%. The study aimed at assessing the prevalence and predictors of knowledge about KMC among postnatal mothers of preterm babies in the Central zone, Tanzania.
Objective
To assess the level of knowledge about KMC and its associated factors.
Methods
It was an analytical cross-sectional study involving 363 mothers of preterm babies from the Central zone. All mothers admitted during data collection and who met the inclusion criteria were enrolled until the sample size was attained. A structured questionnaire was used for data collection. Data were analyzed using SPSS v23. Descriptive statistics were used to describe the study variable while inferential statistics (univariate and multivariate analyses) were used to determine the predictors of knowledge.
Results
Only 138(38%) postnatal mothers had adequate knowledge about KMC
Conclusion
Less than half of the interviewed postdelivery women had adequate knowledge of KMC. Postdelivery women who were more likely to have adequate knowledge about KMC were those aged more than 30 years, with a higher level of education, and living in extended families. We recommend a deliberate effort on improving postnatal mothers’ knowledge of KMC, one of the strategies being initiating care of preterm babies in the antenatal package to prepare these mothers.
Introduction
Prematurity is among the leading causes of newborn deaths, and it is considered the second cause of child death worldwide (Lawn et al., 2012). It is estimated that about 15 million newborns are born prematurely per annum (Mfuh et al., 2019). Complications of preterm births account for 35% of global neonatal deaths each year (Blencowe et al., 2013). Preterm births are defined by World Health Organization (WHO) as birth before 37 completed weeks of pregnancy gestation or <259 days on the first day of the last menstrual period (Blencowe et al., 2013). Sub-Saharan Africa and Asia experience the highest number of preterm deaths currently. There are more than 60% of the World's preterm births today. Also, over 80% of neonatal deaths every year are due to preterm-related complications (Wagura et al., 2018). The chances of preterm survival vary greatly depending on their place of birth (Lawn et al., 2012). However, the risk of death resulting from preterm complications is 12 times higher for African babies than the European baby (Berhe et al., 2019).
Tanzania like many other countries in Africa experiences high rates of newborn deaths (Dhingra et al., 2014). The country has neonatal mortality of 19 deaths per 1,000 live births and prematurity-related complications account for 24% of neonatal deaths (United Nations [UN], 2017). A study conducted in Mwanza Region-Tanzania revealed that 43.4% of neonatal deaths were due to preterm-related causes which occurred within the first 7 days of life. The report showed that about 39.4% and 32.3% of neonatal deaths were due to hypothermia and infections, respectively (Mbawala1 et al., 2014). According to the General Assembly resolution of September 25, 2015, all countries should focus on reducing neonatal mortality to at least as low as 12 per 1,000 live births by the end of 2030 (UN, 2015). Several studies have shown a significant reduction in mortality and morbidity with kangaroo mother care (KMC) practice (Lawn et al., 2010)
The implementation of KMC is an essential strategy for reducing preterm/premature deaths. KMC is a cost-effective method and if appropriately practiced, it reduces three-quarters of preterm/premature deaths (Vesel et al., 2015). The KMC is skin-to-skin contact between the mother/caregivers and child (Conde-Agudelo & Díaz-Rossello, 2016). It was discovered in 1978 purposively to assist the survival of neonates in the situation of scarcity of incubators (Bergh et al., 2012). KMC, apart from maintaining the baby's warmth, promotes exclusive breastfeeding which is appropriate for the weight gain of the baby. Research-based evidence indicates that KMC should be practiced in a continuum manner for more than 20 h a day(WHO, 2022). KMC has to be early, continuous, and prolonged skin-to-skin contact between the mother and the baby, and promotes exclusive breastfeeding, it is initiated in the hospital and can be continued at home; it is a gentle, effective method that avoids the tension routinely experienced in a busy ward with preterm infants (WHO, 2022)
According to WHO, KMC practice lowers the risks of hypothermia by 66%, reduces neonatal infections by 55%, and also lowers the risks of hospital-acquired infection by 61% if compared to conventional care (WHO, 2022). Additionally, KMC has been proven to reduce preterm baby deaths by 40%. Further, babies maintained on KMC were found to have increased body weight and promoted baby–mother attachment (Kampekete et al., 2018).
Review of Literature
A previous study done by Olawuyi et al. (2021) reported that there is a significant relationship between knowledge about KMC and postnatal mothers’ practice of KMC. Knowledge of postnatal mothers is crucial to KMC practice. Inadequate knowledge of KMC has been reported by several studies (Geetha & Hemavathy, 2015; Kinshellla et al., 2021Solomons & Rosant, 2012). It has shown an important role in the good outcome of the baby. Despite the reported significant relationship between knowledge and practice, inadequate knowledge of KMC among postnatal mothers is reported by several studies done in low resources countries. The study carried out by about knowledge of KMC among postnatal mothers in India revealed that more than half (53%) had poor knowledge regarding KMC. This reflected mothers’ negative attitudes toward the practice of KMC which resulted in the poor practice of KMC and hence poor neonatal health outcomes. Kassahun and Since (2019) in their study also revealed that nearly (52%) of postnatal mothers had inadequate knowledge of KMC. Moreover, the study conducted by Solomons et al. (2012) on KMC in Cape Town, South Africa, revealed that most of the postnatal mothers (83%) lacked knowledge of KMC although they were pleased with the weight progress of their preterm babies. The study is comparable to the two studies conducted elsewhere in India and Tanzania, Geetha and Hemavathy (2015) and Kinshellla et al. (2021), respectively.
Tanzania, as a country has established Neonatal Intensive Care Unit (NICU) services, though they are found only in Regional Referral Hospitals (RRHs). The services are also provided free of charge. The increased number of premature babies outnumbers the available incubators in most NICUs in Tanzania. KMC plays a potential role in alleviating the situation. Trained nurses in NICU play a substantial role in supporting postdelivery mothers in KMC. There are limited studies that explain postnatal mothers’ knowledge of KMC practice in the country as one of the barriers to KMC practice. Most previous studies have assessed the knowledge of KMC and its associated factors among healthcare employees (Prantamo et al., 2020; Mehjabeen et al., 2021)). Preterm babies are admitted, and the role of a competent healthcare worker in assisting postnatal mothers’ practice KMC is vital. Ideally, admission has to be extended until a neonate gain full maturity. With the limited space in most health facilities, the majority of these babies are discharged home before they gain full maturity and hence KMC has to be continued at home. The postnatal mothers are required to proceed with KMC to support the babies attain full maturity. Therefore, this study aimed to assess the level of knowledge and the predictors of knowledge on KMC among postnatal mothers of preterm babies in central zone of Tanzania.
Methods
Study Design
A hospital-based analytical cross-sectional study was conducted in the central zone of Tanzania (Figure 1) from April to July 2020. The zone is made up of three regions namely, Singida, Tabora, and Dodoma. Each region has one RRH where there is an NICU and the KMC unit for preterm care. According to National Census, population distribution is different among the three regions. Dodoma has a population of 2,083,588, Singida 1,370,637, and Tabora has 2,291,623 (Tanzania National Bureau of Statistics, 2013). Dodoma comprises seven districts and is among the fast-growing regions with a projected increase in the number of people due to its potential; it is the capital city of the country. Singida is made up of six districts while the Tabora region has seven districts. Each region has one RRH where there is an NICU and the KMC unit for preterm care.

Map showing the regions of central zone.
Data regarding knowledge of KMC among postnatal mothers were collected using a structured questionnaire. The questionnaire was adopted and modified from the Facilitators Guide for Training of Kangaroo Mother Care (Mbawala et al., 2014; UNICEF, 2018). Before filling out the questionnaire, the researchers created rapport and introduced themselves including the purpose of the research to the participants. The researcher identified a private place within the KMC unit where the interview was conducted to assure confidentiality and promote the freedom of respondents to answer questions. All study respondents answered the same questions about KMC. Mothers of premature babies were interviewed to obtain the sociodemographic characteristics and information of knowledge of KMC.
On assessing the level of knowledge of postnatal mothers, 10 multiple choice questions were asked to respondents. Each item had A, B, C, and D subitems. Each correct response scored 1 point, while the wrong response scored 0 points. There were 40 points in total in which those who scored 21 points were considered correct responses. The cut of points for the knowledge level of respondents was 10.5 mean scores. Those who fell below the mean score were considered to have inadequate knowledge and vice versa (Demissie et al., 2018). Knowledge was categorized into two main categories, adequate and inadequate knowledge. Adequate knowledge was the reference category which was given one (1) and inadequate knowledge was given zero (0) in the regression analysis.
Sample Size Estimation
A Kish Leslie (1965) formula was used to calculate the required sample size. The formula is provided below.
The proportional samples were computed by ni = (n/N)Ni; where minimum sample size per facility, n is the total sample size, N the total monthly number of preterm babies admitted from all facilities, and Ni the number of premature babies from each health facility.
The total monthly preterm birth at Dodoma RRH was 170, Singida RRH was 140, and Tabora RRH was 138. Therefore, the total monthly preterm birth in the study area were 448 babies.
The minimum sample size for each health facility
A convenient sampling technique was thereafter used to get participants from Tabora, Dodoma, and Singida regions’ RRHs. Each health facility was visited and all admitted mothers with premature babies were recruited until the sample size was reached.
Inclusion/Exclusion Criteria
All postnatal mothers with stable preterm babies within 4 weeks postdelivery and practicing KMC were included in the study. The study involved all postnatal mothers with stable preterm of 1 up to 4 months postdelivery who practiced KMC and attended preterm units/clinics from Singida, Tabora, and Dodoma RRHs. Those postnatal mothers with preterm babies who were severely ill, and those preterm babies identified to have severe congenital abnormalities were excluded from the study.
Statement Regarding Approval
The study was approved by the Institutional Review Board of the University of Dodoma with reference Ref:No.UDOM/RP/68/Vol.IV/14. Postnatal mothers were given detailed information about the aim of the study. Verbal and written consent was sought from the study participants before the interview. The respondents were ensured confidentiality and freedom of participation in the study.
Statistical Analysis
Data were checked for accurate filling before they were entered into the SPSS software v23. Data were then transformed and recorded in an analyzable manner. Descriptive statistics were done to analyze the social demographic characteristics of the study participants to determine the frequency and percentages of each variable. Means and standard deviations were also used to present continuous variables. All continuous variables were transformed into categorical variables for binary logistic regression analysis. To determine the association between the level of knowledge of postnatal mothers on KMC, and sociodemographic characteristics, chi-square values were presented at a 95% confidence interval (CI) with a P value <.05 was considered statistically significant. Both univariate and multivariate logistic regression analysis was used to determine the extent of association between knowledge and other significant variables.
Results
Sample Characteristics
Table 1 summarizes the sociodemographic characteristic of the participants. The majority of study respondents, 194 (53.4%), were aged between 20 and 29 years followed by ages above 30 years was 124(34.2%). Most of the participants, 159 (43.8%), were having secondary education and above, 252 (69.4%) were married, and 183 (50.4%) were employed. On the other hand, 207 (57%) respondents were from urban and 197 (54.3%) were from a nuclear type of family. The parity of most respondents was multipara 189 (52.1%) and Spontenous Vaginal Delivery (SVD) mode had a high proportion of 351 (96.7%) of postnatal mothers (Table 1).
Sociodemographic Characteristics of Study Participants (n = 363).

Research Question Results
Postnatal Mothers’ Level of Knowledge on KMC Practice
The research findings indicated that 225 (62%) of the participants had inadequate knowledge of KMC practice, while only 38 had adequate knowledge of KMC practice (Figure 2)
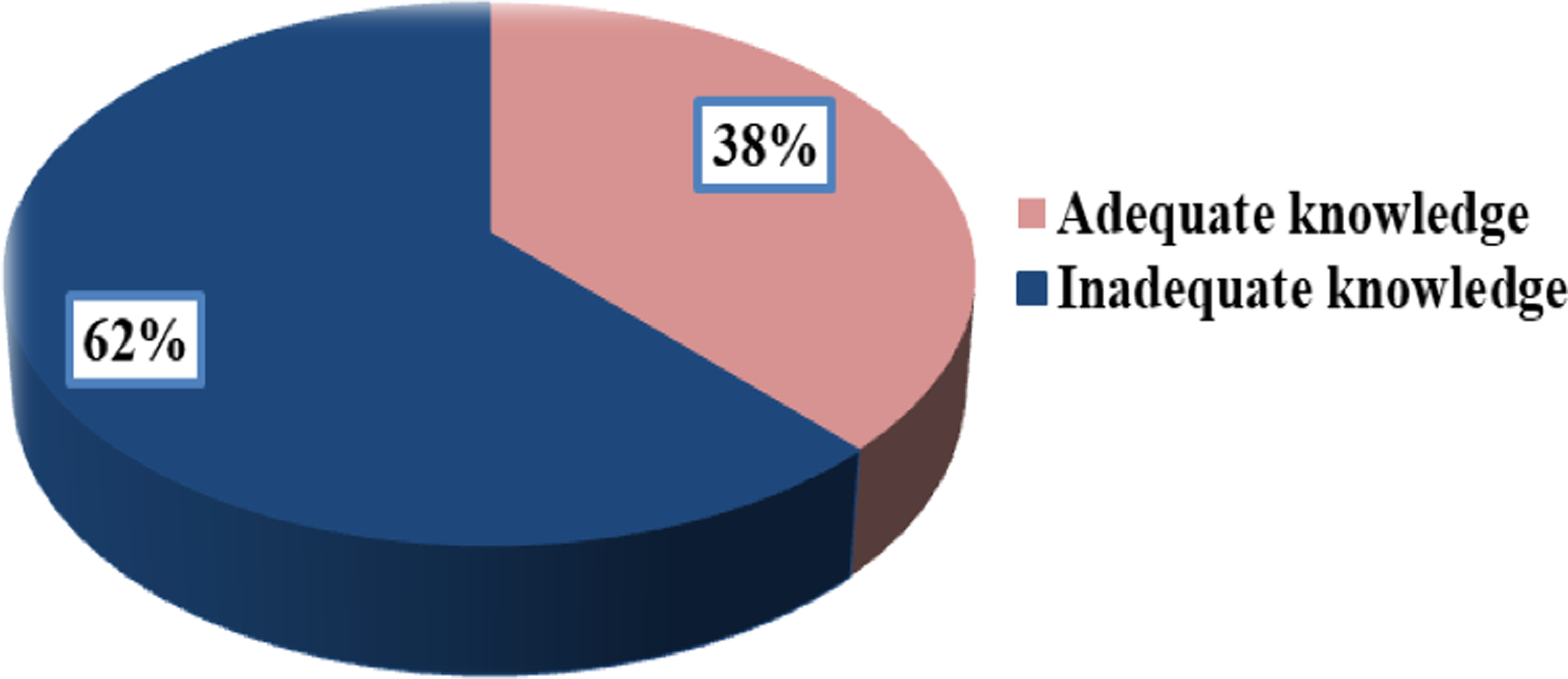
Postnatal mothers’ level of knowledge about kangaroo mother care practice.
Relationship Between Postnatal Mothers’ Characteristics and Knowledge of KMC
A chi-square analysis was done to determine the association between sociodemographic characteristics and knowledge. The results of chi-square for (region [X2 = 6.138; P = .046]), (age group [X2 = 18.919; P < .001]), (education level [X2 = 54.878; P < .001]), (occupation [X2 = 24.943; P < .001]) (residence [X2 = 17.780; P < .001]), (family type [X2 = 17.198; P < .001]), and (parity [X2 = 8.954; P < .011]) showed significant relationship with knowledge level on KMC (Table 2).
Relationship Between Postnatal Mothers’ Characteristics and Knowledge of Kangaroo Mother Care (n = 363).

Predictors of Knowledge of KMC Among Postnatal Mothers
Binary and multilogistic regression was done to determine the significant association between sociodemographic characteristics and knowledge. After controlling for confounders, the predictors of knowledge on KMC among postnatal mothers on KMC; those women who resided in Singida were almost two times more likely to have adequate knowledge compared to Tabora (adjusted odds ratio [AOR] = 1.990 at 95% CI = 1.058–3.741, P = .033), women aged ≥30 years were nearly four times more likely to have adequate knowledge than their counterparts (AOR = 3.913 at 95% CI = 1.038–14.75, P = .044). Other factors which showed statistical significance were education level, whereby all women who had secondary education and above were six times more likely to have adequate knowledge (AOR = 6.309 at 95% CI = 2.305–17.26, P < .001) and mothers from extended family were two times more likely to have adequate knowledge (AOR = 2.055 at 95% CI = 1.263–3.343, P = .004; Table 3).
Predictors of Knowledge of KMC Practice Among Postnatal Mothers (n = 363).

AOR=adjusted odds ratio; CI=confidence interval; KMC= kangaroo mother care; OR=odds ratio.
Discussion
In this study, it was revealed that more than half of postnatal mothers had inadequate knowledge of KMC practice. This is an alarming finding because premature neonates are discharged home before full maturity due to various reasons including the hospital space. Postnatal mothers are expected to continue with KMC until the babies are fully matured. The possible reason for inadequate knowledge could be an inadequate orientation on KMC practice during hospitalization. Our findings were nearly similar to the findings of the study done in India (Kassahun & Since, 2019; Ramaiah & Mokh, 2016; Urmila et al., 2018) which showed also inadequate knowledge of KMC among postnatal mothers. The results were inconsistent with two studies done in Ethiopia which assessed the same factor and showed nearly two-thirds of the study respondents were knowledgeable about KMC practice (Kassahun & Since, 2019). The observed differences might be due to variations in factors like the sociodemographic characteristics of participants.
The current study further indicated knowledge level differences between regional hospitals involved in the study area. Respondents who attended Singida regional hospital were nearly two times more likely to have adequate knowledge of KMC practice compared to the reference category. A multi-country study elsewhere in Africa found similar findings which showed that those health facilities with good supportive supervision, integrated KMC into their quality improvement, continuity of care, high-level buy-in and support for KMC implementation, and client-oriented care in KMC practice (Bergh et al., 2014). This might be the reason for the observed institutional differences in the current study.
We observed that three-quarters of the uneducated postnatal mothers were having inadequate knowledge of KMC practice. After doing adjusted for confounders, postnatal mothers with secondary education and above had six-fold as likely to have adequate knowledge of KMC practice. These findings were consistent with a study done in Ethiopia which found that postnatal mothers who completed grades 1 to 4 were over three-fold as likely to practice KMC (Kassahun & Since, 2019). The education level of a person has a positive and significant influence on healthcare utilization, including KMC practice (Agyemang & Asibey, 2018). A study done in India reported that the education level of postnatal mothers has a relationship with the knowledge of newborn care (Castalino et al., 2014).
We also found that mothers aged 30 years and above were almost four times more likely to have adequate knowledge of KMC compared to their counterparts. The study done in Mwanza, Tanzania cemented that there was significantly higher mortality in the preterm baby born to young mothers since they lacked the knowledge to practice KMC (Mathias et al., 2020). The reason for having inadequate knowledge among young mothers could be exposure to Antenatal Care (ANC) clinics. Older women could have benefited from the experience of ANC visits and childbirth.
Our study further showed parity of a postnatal mother significantly predicted the knowledge about KMC. Grand-multipara women had a reduced likelihood of having inadequate knowledge of KMC practice compared to their counterparts. Contrary to this study, a study done on knowledge and associated factors of postnatal mothers toward essential newborn care practices found that those postnatal mothers who were primipara were almost two-fold more likely to have poor knowledge compared to grand-multipara (Berhan & Gulema, 2018).
Furthermore, our study showed that the type of family the postnatal mother lives in predicted the knowledge of KMC. Those mothers from extended families were two times more likely to have adequate knowledge of KMC practice compared to the mothers from a nuclear family. Studies conducted elsewhere documented the importance of family support in KMC practice to the mother after home discharge (Chan et al., 2016; Liu et al., 2020), although did not indicate the knowledge differences between the type of families. In the extended family, the inhabitants are beyond the father, mother, and children; where possible, they might have learned from one another, should one among them ever experience a similar problem in the family, compared to the nuclear family where only the husband and wife live. The research evidence from elsewhere supports the premise that household responsibilities may be a barrier to KMC practice (Dawar et al., 2019) and this might be the cause for the increased folds of the extended family having adequate knowledge than a nuclear family where possible, the mother becomes the responsible individual to household chores.
Strength and Limitations
To the best of our knowledge this is the first study of its kind in central zone to assess the competence of postnatal mothers on KMC and associated health outcomes of preterm babies. It managed to document the level of knowledge on KMC among postnatal mothers and the factors associated with knowledge. The findings set the basis for a causal effect relationship study which could provide more conclusive relationship between the factors associated with knowledge on KMC.
Our research findings results should be interpreted in the following limitations. The study did not permit the evaluation of other factors that could influence the competence of postnatal mothers on KMC and its outcomes to preterm babies such as hospital staff competence and setting characteristics.
Implication for Practice
The study finding showed that majority of the respondents had inadequate knowledge on KMC among postnatal mothers of preterm babies. Therefore; the researchers recommend inclusion of KMC in antenatal education package. All pregnant women should be empowered on KMC during antenatal period. This will serve a vital purpose in case a pregnant woman delivers a premature baby. A supplement educational package will be offered in NICU. The current study outcome could be contributed with the current practice where a woman will be oriented to KMC only when she gave birth to premature neonate.
Conclusion
The majority of interviewed postnatal mothers had inadequate knowledge of KMC practice which threatens the health of preterm babies who are discharged home before full maturity and need continuation of KMC at home. Postnatal women who were more likely to have inadequate knowledge of KMC practice were those of young age of fewer than 30 years, those with a low level of education, and those living in nuclear families. The study recommends deliberate efforts on improving postnatal mothers’ knowledge of KMC practice, one of the strategies being initiating care of preterm babies in the antenatal package to prepare these mothers in case they have one.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.