Abstract
Background
Postnatal periods are very sensitive periods for both the mother and the neonates where morbidity and mortality are high. Post natal care knowledge has significant role in reducing such complications. The research aimed to determine the educational guideline's effect on nurses’ performance regarding mothers and neonates’ postnatal care.
Design
A quasi-experimental design was decided to fulfil the aim of this study.
Setting
The study was conducted in the obstetric skill lab of faculty of nursing, Benha university.
Sample
A purposive sample was used to recruit 140 maternity nurses from Maternal and child health centres at kalioubia governorate. data collection: Two tools were used: Tool (I) Structured Questionnaire sheet. It is composed of these parts: Part I: Socio-demographic characteristics and Part II: nurses’ knowledge about postpartum care. Tool (II) postpartum care observation checklist.
Results
knowledge and practices about postpartum care showed highly statistically significant differences between pre and post- implementation phases, and total knowledge score regarding post-partum care were improved from 34.52% pre implementation to 45.65% after implementation with (t = 8.11 and p <0.01**) and total practice were improved from 38.52% pre implementation to 54.21% after implementation with highly significant difference (t = 12.75 and p < 0.01**).
Conclusion
Nurses’ knowledge and practice show a significant improvement post-implementation of health educational guideline regarding the care of postnatal mothers and neonates compared to pre-implementation.
Introduction
The postnatal period, starts about an hour after the delivery of the placenta and includes the following six weeks. Postnatal care should respond to the special needs of the mother and baby and should include: the prevention and early detection and treatment of complications and disease, and the provision of advice and services on breastfeeding, birth spacing, immunization and maternal nutrition (WHO, 2020).
A crucial stage in the lives of mothers and neonates is the postnatal era. During this time, important changes occur that affect the health and well-being of mothers and newborns. (Jilan & Al-Battawi, 2017). In addition, postnatal programmes should be regularly tailored to the physical and psychosocial needs of the mother, based on traditional cultural practices and beliefs, to optimize the use of postnatal health care services. (Abuidhail, 2018).
The goal of care is to promote the physical well-being of both mother and baby during the postnatal period and to support the growing relationship between the baby and his or her parents and relatives. In addition, it may also help the growth of infant feeding abilities and enhance the knowledge and trust of the mother in herself and the health and well-being of her baby. Therefore, awareness of postnatal care helps mothers to develop parenting skills to fulfil their function as mothers within their specific family. (Beraki et al., 2020). The goal of performance improvement studies is to enhance and improve the outcomes of care, to insure mothers’ safety, to increase the efficiency of mothers care and related processes, to reduce costs and to reduce risks and liability.
During the early (immediate) postpartum phase, nurses can provide appropriate knowledge and professional nursing care. During this vital time, nurses have to be vigilant and open-minded. This skill requires nurses to believe that there is a considerable concern about the first 2 h after delivery. Therefore, postpartum women and their families should be given professional care, recognizing their values, backgrounds, environment, and respecting their dignity. The role of the nurse in labour, delivery, and the immediate postpartum period is distinctive, as one of the most sensitive periods in women's lives is childbirth. Concentration is needed by nurses during this period on serving, protecting, advocating, and inspiring women. (Ricci et al., 2017).
Operational Definition
Educational guidelines: a process of enabling each individual to understand his abilities and interest to develop them as well as possible and to relate them to life goals and finally to reach a state of complete and matured self-guidance as a desirable human element of the social order. ( Imazeki and Reschorsky (2020).
Post natal care is the individualized care provided to meet the needs of a mother and her baby following childbirth. Although the postnatal period is uncomplicated for most women and babies, care during this period needs to address any variation from expected recovery. (Dol et al., 2019)
Nursing Performance: means that knowledge and practice for the nurses to improve care for mothers and neonates.
Significance of the Study
In developing countries, the Maternal Mortality Rate (MMR) estimate is 440/100,000 live births, with sixty four countries reporting an estimate above 500/100,000 live births. During childbirth, between 11 percent and 17 percent of such deaths occur and 50 percent to 71 percent in the postpartum period. Immediately after childbirth and within the postpartum period first week, most postpartum deaths occur. (Mridha & Koblinsky, 2018). Yet, most of these deaths could be avoided if preventive measures were taken and adequate care available. (El-Khawaga et al., 2019).
Around 830 women die per day from preventable pregnancy or complications associated with childbirth around the world. Maternal mortality remains a major public health issue, and the maternal mortality ratios between developing and developed countries are enormously disparate (Yenupini Joyce Adams (2019). In developing countries, ninety- nine percent of the global maternal mortality occurs. In developing nations, the maternal mortality ratio (MMR) is 19 times greater than in developed countries (WHO, 2020).
The impact of maternal mortality goes well beyond the death of a woman; it has lifelong consequences for her infant, her other children, her family, and the community at large. When mothers die, their babies can suffer from malnutrition due to lack of breastfeeding, and inadequate artificial feeding can kill the infant, or increase the risk of infection or stunting (Miller & Belizan, 2015). Lack of appropriate postnatal care sometimes may result in death or disability of the mother and/or newborn (Timilsina & Dhakal, 2015). Therefore this study conducted to improve nursing knowledge and practice regarding postnatal care of mothers and neonate.
Aim of the Study
This study aimed to:
Assess the effect of the educational guideline on nurse's knowledge regarding postnatal care of mothers and neonates. Assess the effect of the educational guideline on nurse's practice regarding postnatal care of mothers and neonates.
Research Hypothesis:
H1: Educational guideline
H2: Educational guideline
Subjects and Method
Research Design:
A quasi-experimental design (pre-posttest) was adopted for this study. This study was beginning from January (2020) to the end of September (2020)
Setting:
The study was conducted in obstetric skill lab of faculty of nursing, Benha University.
Subjects:
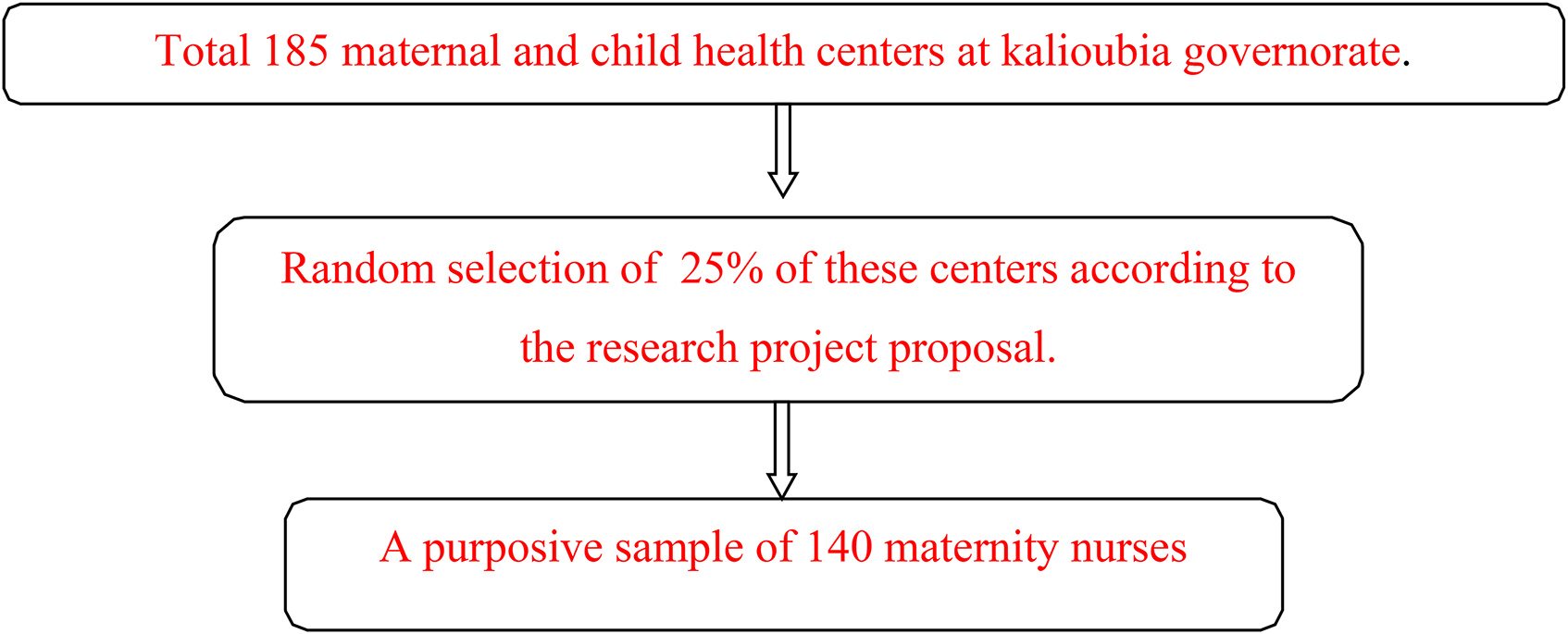
Data Collection Tools:
Tool (I): A-Self reported Questionnaire sheet. It was composed of the following parts: Part I: Nurses’ socio-demographic characteristics such as the workplace, age, level of education, experience years, and previous training programmes regarding the care of postnatal mother and neonates, the name of these training programmes (Hassanein et al., 2021).
As well As nurses total knowledge score was classified as the following: Adequate ≥ 60% of total knowledge score.
Inadequate < 60% of total knowledge score.
The total scores in the evaluation were graded as follows:
Incompetent when the total practice score was less than 60%. Competent when the total practice score was 60–100%.
Validity
The data collection tools were submitted to a board of three obstetrics and gynecology professional nurses to test the content validity. According to the board's comments on sentences’ clarity and the content's appropriateness, modifications were carried out.
Reliability
The test-retest was replicated on two occasions on the same sample of maternity nurses and then the findings were compared. Cronbach's Alpha of the knowledge tool was 0.75 and Cronbach's Alpha coefficient of the practice was 0.86.
Pilot Study
It was performed on ten percent of nurses (14 nurses). It was aimed at determining the tools’ usability and clarity. It also helped to predict the time required for the forms to be filled in. No modified changes occured for the tool.
Field Work
The following phases were adopted to fulfil this research aim: the preparatory phase, interviewing and assessment phase, planning phase, implementation, and evaluation phase. These phases were carried out from the beginning of January (2020) to the end of September (2020), covering nine months. On Sunday, Tuesday, Thursday (Three days a week), from 9.00 am to 2.00 pm, the researchers visited the previously mentioned setting.
A – preparatory phase:
A review of present, past, local, and international literature was performed using books, articles, journals, and magazines to identify the nursing care provided during the postpartum period. Also, An interviewing questionnaire was designed for nurses. An observational checklist was also developed to assess nursing care provided during the postpartum period to evaluate nurses’ clinical performance during the postpartum period.
Assessment Phase:
Before giving sessions, this stage was accomplished. After explaining the purpose of the study, nurses were asked to participate.
This sheet had filled through an interview which ranged from 10–20 min with each nurse utilizing proper communication channels and explaining the purpose of the study before beginning the questions.
The researcher observing nurses’ performance regarding postpartum care filled this sheet. The time taken to complete this sheet was 1–2 h.
Planning Phase:
Based on data from the assessment phase and literature review, the researchers established the educational guidelines in Arabic language. Goal priorities and predicted outcome criteria have been developed. The educational materials were prepared (posters, videos, pictures and PowerPoint presentation, real objects such as mother doula, baby doula, model of cord, measurement tape, cord clamp, and dressing ) to be used in the theoretical and partial session of the educational guideline. For compliance and as a guide, a coloured booklet was also produced and given to all participating nurses.
Implementation Phase:
The educational guideline involved a total of nine sessions (3 theoretical and 6 practical). Each session's duration ranged from one hour to two hours, including discussion periods according to nurses’ achievement, progress, and feedback. Implementation of educational guidelines took (14) weeks period and was implemented for a group of (10) nurses per week. The total number of groups were (14 groups). Each group received three sessions per day (one theoretical session followed by two practical sessions)
The researchers were available three days per week. At the beginning of each group's first day, an orientation to the educational guideline and its aims took place, Arabic language was used to suit the nurses’ level of understanding. The first theoretical session was started by the researchers, which included the postpartum period description, physiological (general, local) and psychological changes during this period, care given to a woman during the postpartum period followed by 30 min break, then this theoretical session followed by two practical sessions through demonstration and re- demonstration of procedures on the doula in the clinical obstetric skill lab in faculty of nursing, Benha university that included: assess vital signs, assess the uterine fundus and lochia.
On the second day of each group, the researchers began the second theoretical session, which included measures of infection control prior to, during, and after performing procedures. The measure included hand washing, wearing sterile gloves, discarding disposable equipment, and sterilization of the reusable equipment. This session also includes health education about (nutrition, exercise, episiotomy, family planning, warning signs of women, warning signs of baby) followed by break time for 30 min. This theoretical session was followed by two practical sessions in which the researchers explained, demonstrated, and re-demonstrated perineal care and episiotomy care. At the beginning of each session, feedback was given about the previous one.
On the third day of each group, the researchers began the third theoretical session, which included immediate baby care followed by 30 min break, then this theoretical session followed by two practical sessions in which the researchers demonstrated and re- demonstrated neonatal care, which included (cord care, eye care, weighing the baby, measure chest & head circumference, complete physical & neurological examination and breast care). At the beginning of each session, feedback was given about the previous one.
Different methods of teaching were used in theoretical sessions such as lecture, group discussion, instructional media included, handout prepared by the researcher and distributed to all nurses on the first day of the training, and other methods were used in practical sessions such as demonstration and re-demonstration, real objects such as mother doula, baby doula, model of cord, measurement tape, cord clamp, and dressing. Nurses were motivated and encouraged to cooperate and participate actively in the study throughout its different stages.
The post-test for the awareness and practice of nurses was carried out immediately after the implementation of the educational guideline by the same pre-implementation assessment format to assess the impact of the implemented educational guideline.
Evaluation Phase:
Evaluation was done by:
Before the theoretical sessions, assessment of nurse knowledge was carried out (two times) using the tool I part II to test nurse knowledge about postpartum caring and newborns and then immediately post sessions using the same methods. Before implementing nursing intervention, the performance of nurses was assessed (two times) using Before and after the introduction of educational guidelines, comparison was made regarding the knowledge and performance of nurses to determine the impact of the educational guideline on the nurses’ knowledge and performance about postpartum care and neonate.
Statistical Design
Data collected were organized, categorized, tabulated, and analysed using an electronic computer. Data were presented in tables using mean and standard deviation, number and Percentage, and other statistical tests such as the t-test.
Results
Table 1: reveals that nearly half (43.5%) of the studied nurses were in the age group of more than 35 years old with a mean age of (38.24 ± 7.84). More than half (51.4%) of them had a Bachelor's degree in education. Besides, about two-thirds (65.7%) of the studied nurses had more than ten years’ experience, and (85%) hadn’t training programmes
Distribution of Studied Nurses According to Demographic Characteristics (n = 140).

No.: Number %: Percentage.
Table 2: Shows a highly statistically significant difference in total postpartum care knowledge pre and post-implementation phases (p < 0.001).
Mean and SD of Participants’ Knowledge During pre and Post Intervention Phases (N = 140).

Figure 1: represents that total knowledge score regarding post partum care were improved after implementation than pre implementation.

Distribution of studied nurses regarding their total knowledge about post partum care pre and post implementation.
Table 3: Shows a highly statistically significant difference in total postpartum care practices pre and post-implementation phases (p < 0.001).
Mean and SD of Participants Practices Regarding Postpartum Care During pre and Post Intervention Phases (N = 140).

Figure 2: represents that total practice score regarding post partum care were improved after implementation than pre implementation.

Distribution of studied nurses regarding their total practices about post partum care pre and post implementation.
Table 4: Shows a highly statistically significant difference in total neonatal care practices pre and post-implementation phases (p < 0.001).
Mean and SD of Participants Practices Regarding Neonatal Care During pre and Post Intervention Phases (N = 140).

Figure 3: represents that total practice score regarding neonatal care were improved after implementation than pre implementation.

Distribution of studied nurses regarding their total practices about neonatal care pre and post implementation.
Discussion
In the life of a woman, the postnatal phase is critical. In order to demonstrate safe motherhood and healthy living, they need special care during pregnancy, at the time of childbirth, and after childbearing. Improper perception of postnatal health practices often leads the individual to shift towards unsafe motherhood. During the postnatal phase, mothers and newborns are vulnerable to illness and death. As significant and life- threatening complications in the postnatal period can occur, the postnatal period is a vital part of maternal health care. The health of the mother is considered the health predictor of society, so postnatal care is critical for the health of the mother and newborn. (Mridha & Koblinsky, 2018).
The current study aimed to determine the effect of education guidelines on nurses’ performance regarding mothers and neonates’ postnatal care. The present study results revealed improvements in nurses’ knowledge and practice after the implementation of the programme. So, the research hypotheses (The awareness and practice of nurses is expected to be strengthened after the adoption of health education guidelines on the care of postnatal mothers and neonates) is accepted and indicates that the health educational guideline regarding the care of postnatal mothers and neonates for nurses was effective.
Regarding the studied nurses’ demographic characteristics at table (1), the results showed that about half of the studied nurses aged above 35 years old with a mean age of (38.24 ± 7.84). These findings were different from (El-Khawaga et al., 2019), who stated that above one third of the nurses surveyed were aged 30 years or younger. Hassan et al. (2019) stated that above half of the surveyed nurses were aged 25 to 29 years. This may be linked to the various characteristics of the subjects in the sample.
Regarding education, the results revealed that more than half had a Bachelor's degree of education. These results agree with the study conducted by Hashem (2018) stated that fewer than two-thirds had a nursing bachelor's degree.
Also, about two-thirds of the studied nurses had more than ten years of experience, This finding agrees with El-Khawaga et al. (2019), who found that women who had 10 to 20 years of experience represented more than one-third. This may be due to nearly half of them had more than 35 years old, as a result, they have more years of experience. Moreover, No training courses on immediate postpartum nursing care were attended by three quarters of the studied nurses. the researcher thinks this may be better to avoid the influence of these previous courses in the results of the current research
Regarding mean and SD of participants’ knowledge during pre and post intervention phases at table (2), the study results revealed a highly statistically significant difference in postpartum care knowledge and neonatal care pre and post-implementation phases. This finding follows Aschalew (2016), who illustrated that approximately (55.3%) of the nurses in the sample had clear awareness of immediate neonatal care. This result is also consistent with Shinde (2018), who noticed that less than half of the nurses were aware of newborn care.
Regarding the studied nurses’ total knowledge about post partum care, the study revealed that total knowledge scores concerning postpartum care were improved after implementation than pre-implementation. This lack of postpartum care knowledge pre- implementation may be because that studied nurses didn’t receive the needed courses and workshops about postpartum care and also the immediate impact of the educational programme sessions assisted by the given postpartum care booklet may probably be attributed to it.
Also, the lack of nurses’ knowledge was because the hospital administration did not provide them with any refreshment and training programmes on quality of nursing performance during the postpartum period nor provide them with care standards for the postpartum period. With nursing procedures manuals which help in guiding their action. This lack of knowledge, of course, result in poor quality nursing performance.
The findings were also supported by Beraki et al. (2020), who indicated the poor quality of care given. The major requirement for quality service is having effective service personnel in place. Sikorski et al. (2018), who mentioned that the nurse must know about physical changes in the mother and psychosocial and emotional changes in the entire family to provide quality care for postpartum women. In the researcher point of view, when nurses had a full understanding of postpartum woman physical, psychosocial and emotional changes, they can tolerate any responses from women and can respond to woman's needs effectively and efficiently
Regarding mean and SD of participants practices regarding postpartum care and neonatal care during pre and post intervention phases at table 3 and 4, a highly statistically significant difference was present between pre and post-implementation. The meaning of that post programme best practice in the current study may be linked to the nurses’ capability and interest to update their knowledge and upgrade their practice. The study revealed that after implementation, total practices score regarding postpartum care were improved compared to pre-implementation. These inadequate practices in the pre-implementation phase regarding postpartum care maybe because studied nurses did not receive the needed training regarding postpartum care. This finding agrees with Berhe et al. (2017), who concluded that (76%) healthcare providers performed it on a regular basis. In the meantime, conflicting with Chaudhary et al. (2018), who reported that most staff nurses had strong overall immediate newborn care experience
It was found that most of the studied care items were clearly and substantially improved after implementing the educational programme. This may be due to a lack of information, nurse shortage, deficiency in equipment and supplies available, and a weak documentation system. The result, on the other hand, is different from Simbar et al. (2017), who found that the standard of care in many areas of postpartum care was poor in 12.95% of nurses.
It is important to note that the privilege of continuing education services has not been offered to working nurses, which will dramatically increase their awareness and enhance their abilities. Absence of continuous monitoring and regular performance review, lack of motivation, not clear job specifications, and shortage of personnel all contribute to overlap when certain care items are given and others are ignored. Moreover, the time required to provide the requisite information and advice for parturient women is minimized by early discharge after delivery. Finally, in addition to their roles as health care professionals, it should not be forgotten that working nurses are overwhelmed with administrative duties.
Implications for Nursing
The findings of this study have several implications that can affect the practice of nurses. It may also help in better inform the job of professionals who take care of women in the hospital during postnatal period. This research evidence overwhelmingly suggests that a healthy post partum period depends on the ability of nurses to effectively employ her own skills to ensure that postnatal women needs and the needs of child are met and help women build their individual skills to successfully meet those needs.
Conclusion
Based on the current study's findings, the study concluded that the research hypothesis is supported, and nurses’ performance shows a significant improvement post- implementation of educational guidelines regarding postnatal care of mothers and neonates compared to pre-implementation.
Recommendations
Offering scheduled in-service training programmes for all postpartum nurses on the value of postpartum and neonatal care to improve expertise and efficiency and eventually improve health care quality.
In order to achieve more generalization of findings, it is suggested to replicate the current research with a greater representative sample size at different institutions.
Footnotes
Acknowledgments
This research was supported by Benha University, Egypt, and the scientific Research Account Fund, and a grateful thanks to all nurses who trust & participate in our study. All authors agree and accountable for all aspects and in ensuring questions were related to accuracy or integrity of any part of work are appropriately investigated and resolved and no competing interests.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics
Ethical approval was taken from Faculty of Nursing's Ethical Committee, Benha University, this research was conducted. Written and verbal informed consent was taken from the participants before collecting data and participants’ privacy and confidentiality were maintained during data collection and publication
Supplemental Material
Supplemental material for this article is available online.
