Abstract
Introduction
The implementation of nursing clinical learning in Indonesia has several challenges that require innovation in the learning method strategy. The method that has been used so far focuses on the hierarchical relationship between lecturers/preceptors and students, so that there are many shortcomings in learning outcomes. The application of the method of active learning with Peer Learning (PL) and Problem Based Learning (PBL) techniques has proven effective in classroom learning, but its rarely found in clinical learning.
Objective
The purpose of this study was to determine the effectiveness of the PL and PBL towards the achievement of clinical learning in nursing students.
Methods
The research method used a true experiment with a posttest only control group design, the sampling technique was taken by randomize control trial. An instrument for clinical learning achievement using AssCE.
Results
The analysis was carried out as descriptive and bivariate. The results showed the mean in the experimental group was 7.059 and the control group was 6.325. Further statistical test results were obtained p-value = 0.001 (p < 0.05) which showed that the average score there were differences in clinical learning achievement development scores.
Conclusion
Clinical learning using peer learning and PBL methods can directly improve various aspects of student competency achievement.
Background
Clinical education is an essential part of nursing education. In clinical education, nursing students learn to apply or practice the theories taught in a clinical environment. Students also learn about the nursing profession and how to become safe and effective practitioners in the future (Henderson & Newton, 2010). Furthermore, students learn to face the reality of their roles and work in clinical practice, knowing all aspects of patient care. It is essential to prepare students to face professional practice challenges and ensure their readiness to obtain a professional practice permit (Bridges et al., 2012; Lekalakala-Mokgele & Caka, 2015).
Clinical education plays a vital role in improving students' clinical skills, building soft skills, and attaining the profession's competencies. Morrell et al. (2020) explain the soft skills that professional nurses must have, including self-confidence, critical thinking, teamwork, and communication. This competence can be achieved by applying the clinical practice in the field. A lack of clinical competence will result in nurses’ unpreparedness to enter the workforce and meet healthcare providers’ demands (Bulman & Schutz, 2013). Indeed, learning support has focused on various professional studies in recent times (Christiansen & Bell, 2010).
Several studies show some of the obstacles faced by students in clinical field practice. Nahariani et al.’s (2013) research evaluated students’ clinical learning and revealed that 57% of students lacked preparation for mastery of the material to be studied, 65% did not have clear objectives in learning, and lacked analysis skills in evaluation. In addition, 54% of students still lacked motivation, as indicated by the lack of preparation to master the topic to be delivered in learning. Wilson’s (2012) research reported that nursing students generally lack communication competencies and skills. Many students feel stress during their clinical practice. For example, studies have investigated nursing of stress in clinical education practice (Liu et al., 2015; Nelwati et al., 2012; Sun et al., 2016; Rahmi et al., 2019). A Qualitative Study by Sun et al. (2016) found that almost students showed anxiety responses, including tension, insomnia, restlessness, stomach pain, and lack of confidence during clinical practice. Christiansen and Bell (2010) revealed that students' new environment caused them to feel inadequate, anxious about staff situations, and worried about the perceived lack of knowledge and skills. The obstacles students face above are influenced by learning environment factors, and this should be the teacher's attention to modifying these factors. The optimal clinical learning environment has a positive impact on students' professional development (Jamshidi et al., 2016).
The clinical environment includes everything around students, including clinical practice settings or methods, equipment, staff, patients, nurse mentors, and lecturers. The learning environment and learning support are not only obtained from the lecturer-student hierarchical relationship but also a network of peer relationships (Jamshidi et al., 2016). On the other hand, the clinical environment is challenging to control, and many stimuli are making it difficult for students to take what is essential (Changiz et al., 2012). The learning method is a modifiable factor in optimizing the student learning environment.
Learning methods that focus on students (Student-Centred Learning = SCL) are currently seen as a solution to improve students' understanding of competency attainment. One suitable SCL method used in nursing practice is Problem-Based Learning (PBL) (Baeten et al., 2010). PBL emphasizes learners' role, including active and interactive learning that is designed in collaborative and cooperative learning. Such learning activities encourage students to explore the fields of science that they are interested in and build their knowledge responsibly and ultimately achieve the competencies set out in the curriculum. This method has been used in various programs in the last decade, but in clinical nursing education, only a few studies have reported its use (W. Zhang, 2014). PBL encourages independent, individualized learning and responsibilities for learning, problem-solving and critical analysis, increasing integration between theory and practice (Dreier-Wolfgramm et al., 2018a).
Problem-Based Learning (PBL) is a learning method in which students are confronted from the beginning with a problem, followed by student-centered information seeking(Dreier-Wolfgramm et al., 2018b). Both the content and the learning process are emphasizing in PBL. Over the past 30 years, many PBL variants have appeared; however, the main elements of PBL have not changed. Students will have certain positive skills and attitudes, including collaboration in groups, teamwork between students outside group discussions, leading groups, listening to peer opinions, noting things discussed, respecting friends' opinions/views, being critical of the literature, learning independently, being able to use learning resources effectively, and having presentation skills (Ehrenberg & Häggblom, 2007; Hartling et al., 2010). Overall, these skills and attitudes are the main assets in forming lifelong learners.
Other factors that can impact clinical learning experience include the quality of guidance and peer support available (Baeten et al., 2010). The role of peer support in learning is known as peer learning. Peer learning does not eliminate the role of the clinical supervisor. In fact, the clinical supervisor's role is crucial in providing feedback to improve student performance and provide guidance to students. The peer learning method is advantageous in learning because students are able to appreciate, think for themselves, work in a team and solve problems (Nygren & Carlson, 2017). Peer learning provides a conducive environment for the development of student abilities. Several previous studies have explained that peer learning students increase students' sense of safety and comfort in learning and clinical practice. (Hamzah et al., 2019; Pålsson et al., 2017). In general, students learn from each other in a mutually beneficial way by sharing ideas, knowledge, and experiences.
The peer learning concept has reappeared as a strategy to reduce obstacles in universities and institutions, where the number of preceptors and the quality of guidance are still lacking; in addition, supervisors are not always present in the clinical practice (Z. Zhang & Bayley, 2019). Nursing academic preceptors and lecturers are central to this method, facilitating students to study together, providing ongoing support and constructive feedback for students. A tripartite relationship between the mentor and the student supports the implementation of a learning contract and clarifies the roles and limitations listed in the clinical learning program plan (Christiansen & Bell, 2010). The method is widely used in medical education with the concept of “foster brothers and sisters,” where higher-level students become friends and assist their juniors (Stenberg & Carlson, 2015).
Research by Stenberg and Carlson (2015) describes that feeling of safety appeared to be related to learning, including increased learning motivation and independence, but competition seemed to have a negative effect. Learning method showing active support from fellow students, who have empathic understanding, seems to have a positive impact on students' sense of social isolation, and students can deal more effectively with challenges faced through the creation of safe and non-threatening learning (Christiansen & Bell, 2010). In Indonesia, a study about peer learning is not widely found. Arjanggi and Suprihatin (2010) research indicated an influence of peer tutoring method on student self-regulation.
A preliminary study by interviews with four clinical supervisors revealed that some students unable to make the right decision in nursing care and could not improve their critical thinking skills in practice. Two supervisors mentioned the less-than optimal quality of nursing care, possibly due to the lecturers and supervisors` inability to always be present in the practice rooms. Interviews with six students indicated a lack of supervision in nursing care and stress during practice were clinical learning constraints. Peer learning and PBL methods are intended to overcome the lack of clinical instructor quantity and quality, reduce environmental stressors, and the lack of student understanding to solving nursing problems quickly.
In recent years, peer learning and PBL have been increasingly implementing in various nursing education institutions in Indonesia. However, little is known about their implementation in clinical education. So, it is important to know how effective the implementation of peer learning and PBL is in clinical education on learning outcomes.
Method
The study was a true experiment, with the post-test-only-control-group design. The participants were 31 students who took Medical-Surgical Nursing Clinical Practice in the Three-Year Diploma Nursing Study Program at the Faculty of Sports and Health Education, Universitas Pendidikan Indonesia.
The sample was taken by randomized subject-post-test-control-group sampling design. The supervisors randomly assigned study partners by pairing each of the participants. The treatment group and control group consisted of 16 and 15 students, respectively.
Data collection was carried out directly by researchers by asking respondents to fill out questionnaires on students’ and mentors’ perceptions and clinical learning outcomes. The intervention variable was the integrated peer-learning and problem-based learning method, whereas the control group was taught the conventional method.
The dependent variables in this study use AssCE (Assessment of Clinical Education) developed by Löfmark and Thorell-Ekstrand (2014). This instrument was developed to guide the assessment of learning outcomes internationally; this instrument has been used for more than 15 years in several countries. The instrument consists of 4 assessment components: communication and teaching, nursing care, examination and treatment, and professional approach (Engström et al., 2017). Once translated into Indonesian, the researchers conducted a validity test, and the results indicated that overall, the instrument's questions were valid with an r count of 0.387–0.913 and a reliability value of 0.961.
Research Procedure
The study was carried out with the following steps. First, the researchers prepared all instruments and modules to be used in the study. Secondly, the researchers explained to all respondents and the clinical instructors at the hospital about the research mechanisms, procedures, and assessments. The researchers explained the implementation of the PBL and peer learning methods to the intervention group. While in the control group, the explanation was in the form of a conventional method. The researchers sought for their consent to become respondents to this research. All student respondents were randomly divided into two groups and put in pairs.
The data were processed according to the principles of statistical analysis. To test the research hypothesis, namely whether there is an influence of peer learning and PBL learning methods on clinical learning outcomes, the gain scores between the treatment and control groups were compared using the statistical tests of descriptive analysis and independent t-test.
Results
The sample included 31 nursing students, mean age 18.45 years, ranging from 17 to 20 years. The majority were female (84%), and male were (16%). There were no differences between participants at baseline regarding any of the study variables confounding (the type of curriculum, learning process of academic) or demographic characteristics.
The study shows that there are differences in clinical learning outcomes after an intervention. Based on Table 1, the experimental group's mean score was 7.05, and a standard deviation of 0.33. The mean score of the control group was 6.32, and a standard deviation of 0.98. Further statistical tests obtained P-value = 0.001 (P < 0.05), which shows that there was a difference in the average scores of clinical learning outcomes after treatment.
Differences in Clinical Learning Outcomes After Treatment.

Distribution of Mean Scores for Each Component of Clinical Education After Treatment
Clinical learning outcomes for each component can be seen in Table 2. It can be seen that the mean score for the Communication and Teaching component of the experimental group was 7.08, and a standard deviation of 1.291. Further statistical test results obtained p-value = 0.001 (p < 0.05), which shows that there was a difference in the mean scores of clinical learning outcomes in the component of communication and teaching after the treatment. For the component of nursing care, the mean score obtained by the experimental group was 7.050, and a standard deviation of 0.346. The mean score in the control group was 6.253, and a standard deviation of 0.972. Further statistical test results yielded p-value = 0.005 (p < 0.05), which shows that there was a difference in the mean scores of the clinical learning outcomes in the component of nursing care after treatment.
Distribution of Mean Scores of Clinical Learning Outcomes for Each Component After Treatment.
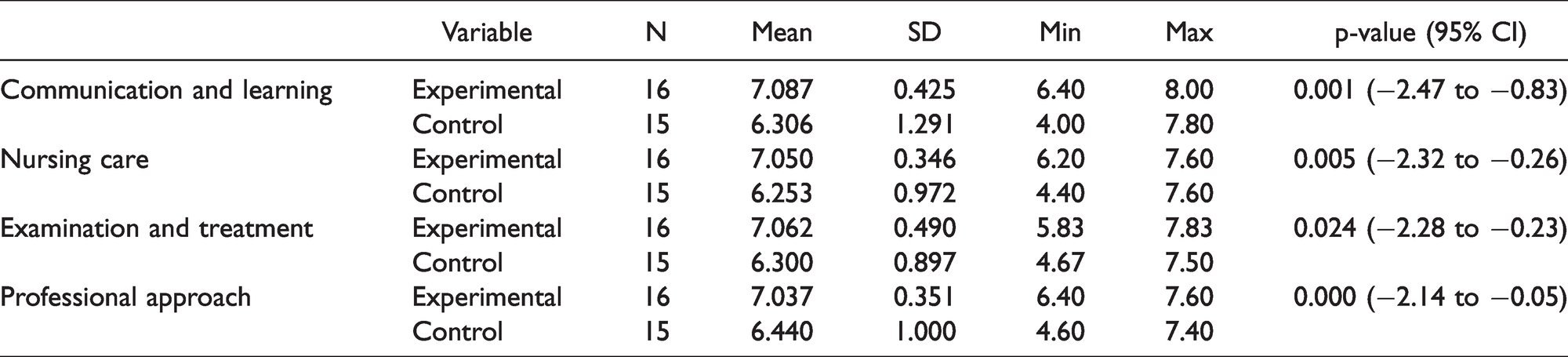
With regard to the examination and treatment component, the experimental group's mean score was 7.06, and a standard deviation of 0.49. The mean score in the control group was 6.30, and a standard deviation of 0.89. Further statistical test results obtained p-value = 0.024 (p < 0.05), which shows that there was a difference in the mean scores of clinical learning outcomes in the component of examination and treatment. For the professional approach component, the experimental group's mean score was 7.037, and a standard deviation of 0.351. The mean score of the control group was 6.44, and a standard deviation of 1.000. Further statistical test results obtained p-value = 0.000 (P < 0.05), which shows a difference in the mean scores of clinical learning outcomes in the professional approach component.
Discussion
This study supported the peer learning method and problem-based learning as an approach in the clinical learning process. Peer learning and PBL can affect clinical learning outcomes in the aspects of communication and teaching, nursing care, examination and treatment, and professional approaches. Peer learning and PBL learning methods' main role is to improve clinical reasoning skills through problem-solving and students' critical thinking (Hartling et al., 2010). No previous study has shown the integration of Peer Learning and PBL in the clinical field, but implementation separately recorded quite a different result.
The current study provides findings concerning the effectiveness of PBL to the conventional method. Besides strengthening the material mastery segment, the PBL method encourages efforts to improve students' abilities in mapping, analyzing, and working together to solve existing problems (Khatiban & Sangestani, 2014; Li et al., 2020). Besides, the implementation of PBL in clinical education is proven to strengthen students' character and personality (Khatiban & Sangestani, 2014). However, (Hartling et al., 2010), in a systematic review study, concluded the PBL does not affect knowledge acquisition and learning improvement. This can be found, wherein its implementation the PBL method seeks to prioritize the spirit of mutual respect, to strengthen the value of independence and responsibility (integrity), which must be done recently to produce students who are not strong only in the mastery of knowledge, but also strong in character and personality.
Peer learning is a conceptual approach to learning in which students are grouped or paired, both in formal and informal ways, where knowledge and skills are acquired through active assistance and support among each other (Pålsson et al., 2017). Feedback from learning partners gives students a certain internal motivation to strive to improve and enhance their learning. Some research explains that support and guidance will make it easier for students to integrate all the knowledge that has been obtained at the academic stage in clinical learning and providing care to clients in the clinic (Tai et al., 2017; Tursina et al., 2016). Qualitative research in Indonesia regarding student experiences in peer learning enabled students to practice leadership and cooperation, besides that students expressed feelings of self-confidence and foster self-esteem (Hamzah et al., 2019).
Communication and Learning
One factor that influences the relationship between nurses and patients is communication. Therapeutic communication becomes a reference in a nurse-patient relationship to improve the patient's health status (Reinke, 2018)(Stenberg & Carlson, 2015). Therapeutic communication is based on interpersonal communication, where the communication process occurs without any medium, so it has the following characteristics: 1) messages from the communicator are not limited to verbal messages but also nonverbal messages such as facial expressions, limb movements so that the message has a variety of meanings that can also lead to a variety of responses. The most prominent stimulus received by the communicatee is likely facial expression (nonverbal) without being realized by the communicator so that the response received by the communicator does not match the desired content; 2) communicatees can change roles as communicators at the same time (during the communication process), causing interruptions. Changing roles simultaneously is a feedback mechanism that may cause communication barriers to be not immediately known by both parties (Ferreira et al., 2016).
This study shows peer learning and PBL have high scores than conventional methods in communication and learning outcomes. The statistical test showed that P-value = 0.001 (P < 0.05), meaning there was a difference in the mean scores of the component's clinical learning outcomes. This result is in line with Chojecki et al. (2010) and Hellström-Hyson et al. (2012), reporting that students had a comprehensive increase in problem-solving, discussion, teamwork, and communication skills. In the implementation of clinical nursing practice, students and patients build therapeutic relationships using therapeutic and interpersonal communication. Students learn to communicate by modeling the clinical nurses and peers when dealing with patients. With the peer learning model, students learn and share communication outcomes with patients. Nurses and team members can directly evaluate communication with patients (Putu et al., 2017).
Nursing Care
Nursing care is the core part of clinical nursing education. Students learn to do a series of processes in providing nursing services to patients. The nursing care process begins with conducting a comprehensive assessment, determining diagnoses, making intervention plans, and carrying out interventions and evaluations. Critical thinking is needed in nursing care to analyze patient problems and determine interventions to be carried out.
For the component of nursing care, the mean score obtained by the experimental group was 7.050, with a minimum score of 6.20 and a maximum score of 7.60, and a standard deviation of 0.346. The control group's mean score was 6.253 with a minimum score of 4.40 and a maximum score of 7.60, and a standard deviation of 0.972. Further statistical test obtained p-value = 0.005 (P < 0.05), which shows a difference in the mean scores of clinical learning outcomes in the component of nursing care after treatment.
Ehrenberg and Häggblom (2007), Hamzah et al. (2019), and Khatiban and Sangestani (2014) all believed that peer learning had improved cognitive development on process nursing care analysis. However, several other studies disprove it (Hartling et al., 2010). By practicing nursing care together with friends and using problem-based learning, students learn to analyze any problems found together, discuss and determine the goals and action plans to be achieved. In this case, students learn to act collaboratively, influence learning and development, share comfort with nursing care providers, increase self-efficacy and psychological empowerment (Pålsson et al., 2017).
Examination and Treatment
Students may face unexpected situations in the real clinical setting, such as unexpected patient responses, patient conditions that suddenly change, and the gap between theory and practice (Stone et al., 2013; Rahmi et al., 2019). These unexpected occurrences require speed and accuracy of clinical decision making. The management of medical procedures includes very dynamic examinations and treatments, which require a good attitude from the nurse.
Observation and follow-up on nursing care related to intervention and treatment are a series of activities done by undergraduate students. Students are expected to be responsible for planning the examination and treatment chosen, demonstrating knowledge about patients' procedures and treatment (Löfmark & Mårtensson, 2017). Student readiness in implementing intervention plans and awareness of the safety of interventions taken is important to achieve. Peer learning and PBL lead students to discuss cases with a partner before taking action, conducting in-depth analysis, and discussing with friends so that there is very little chance of mistakes.
In the examination and treatment component, the experimental group's mean score was 7.062, with a minimum score of 5.83 and a maximum score of 7.83, and a standard deviation of 0.49. The control group's mean score was 6.30, with a minimum score of 4.67 and a maximum score of 7.50, and a standard deviation of 0.89. Further statistical test results yielded p-value = 0.024 (P < 0.05), which shows a difference in the average score of the clinical learning outcomes in the examination and treatment component. These findings support work conducted on Z. Zhang and Bayley (2019) study, which reported that peers who teach and learn from one another in clinical practice settings positively impact student clinical skills development.
Professional Approach
Professional approaches include reflective and analytical skills, seeking and developing new knowledge, conducting intervention with ethical awareness, demonstrating the ability to identify needs according to knowledge, and showing strong thinking in the decision and work strengths (Löfmark & Mårtensson, 2017).
For the professional approach component, the experimental group's mean score was 7.03, with a minimum score of 6.40, a maximum score of 7.60, and a standard deviation of 0.35. The control group's mean score was 6.44, with a minimum score of 4.60, a maximum score of 7.60, and a standard deviation of 1.000. Further statistical test results obtained p-value = 0.00 (p < 0.05), which shows a difference in the average scores of clinical learning outcomes in the professional approach component after treatment. Dreier-Wolfgramm et al. (2018b) research reported on the application of PBL in interprofessional education shows that their ability with regard to both interprofessional communication and collaboration had improved. However, Hartling et al. (2010) conducted a systematic review and meta-analysis of the effectiveness of PBL, resulted that no significant differences in clinical practice.
Implications
The choice of the clinical education model is significant to learning. Using peer learning models and PBL, educators create spaces for students to take responsibility for their learning processes and experience empowerment. Peer learning is likely to create an integrated learning environment for clinical and academic skills (Mamhidir et al., 2014). The result suggests peer learning and PBL methods indirectly enhance students' ability to think critically; consequently, students can appear more professional in their nursing practice. PBL is built on the idea of reflection, mainly focused on cognitive knowledge (Stenberg & Carlson, 2015). The combination of peer learning and PBL can facilitate affective, cognitive, and psychomotor learning during clinical education. This is supported by several previous studies (Stone et al., 2013).
Instructors act in line with the idea of peer learning, in which fellow students interact and learn together while the implementation of nursing care. It is essential to provide clinical strategy training to clinical lecturers and instructors to ensure this implementation is appropriate to the curriculum goal. Furthermore, this methods can help overcome the lack of the number of clinical instructors in the hospital.
Conclusion
Peer Learning and PBL methods work by improving students' ability to learn actively by discussing with partners who then determine nursing care actions to be performed. This study proves that Peer Learning and PBL in clinical practice can provide improvement the four aspects of student learning outcomes and improve students' critical thinking skills. As a result, students can appear more professional in their nursing practice.
Further studies with large sample sizes that evaluate PBL and peer learning in context from students' and clinical instructors' perspectives are needed to strengthen this study's findings. Further studies should explore a broad range of clinical practice fields to support PBL and Peer Learning methods.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by LPPM Universitas Pendidikan Indonesia (Grant Year 2019).
