Abstract
Introduction
Clinical nursing education is an important component of the professional development of nursing students. Key informants such as nursing lecturers, nurse managers and clinical placement coordinators play an essential role in clinical education.
Purpose
The purpose of the study was to explore the perspectives of key informants on how the current state of clinical nursing education in Northern Ghana can be improved.
Methods
The study used an exploratory qualitative design. Sixteen participants were purposively selected and data were collected through face-to-face individual interviews. Data were analysed using framework analysis.
Findings
The study findings indicate that clinical nursing education can be improved by decreasing the overcrowding of students in the clinical setting, decreasing the theory-practice gap and providing relevant material resources in the clinical facilities. Also, nursing education institutions can improve clinical nursing education by equipping the skills laboratories, engaging an adequate number of lecturers, and carrying out clinical accompaniment.
Conclusion
There is a need to improve clinical education through collaboration between nursing education institutions and clinical facilities. Effective collaboration will ensure the planning of clinical placement to avoid overcrowding, provision of continuous professional development programmes for preceptors and improvement in clinical supervision. Also, the provision of material resources in skills laboratories and clinical facilities to enhance clinical teaching should be given priority.
Introduction
Clinical education is an essential component of nursing training. The training of nursing students to become competent professional encompasses theory-based approaches in the classroom as well as real-life practical learning in the clinical setting (Jeppesen et al., 2017). The nursing profession is practice-oriented hence the need to acquire practical competencies (Kpodo, 2015). The development of skills by students depends on factors existing in the clinical environment and nursing education institutions.
When the clinical environment is well resourced it supports the students in the acquisition of skills (Haraldseid et al., 2015; Mbakaya et al., 2020). In Ghana, students have reported that the equipment in the clinical placement area allows them to learn skills (Atakro et al., 2019). The clinical environment is said to be effective when there is adequate material and human resources to support the clinical learning activities of nursing students. Students consider the clinical learning environment positive if there is an adequate number of nurses in the clinical setting to support them with their skills learning (Kamphinda et al., 2019).
Bvumbwe and Mtshali (2018) in an integrative review revealed that despite the increased number of nursing training institutions across Sub-Saharan Africa, there are inadequate provisions to ensure effective clinical teaching of students. In Ghana, lack of material resources in the clinical placement area have been reported as a cause of theory-practice gap (Adjei et al., 2018; Salifu et al., 2019). In Malawi, students have reported the lack of material resources as a challenge in the clinical environment (Bvumbwe et al., 2015; Kamphinda et al., 2019). Similarly, nurse educators in Angola have indicated that nursing education is faced with challenges such as lack of human resources, material resources and infrastructure (Marchi-Alves et al., 2013).
The concept of preceptorship has been introduced in Ghana to ensure that students receive adequate support during clinical placement (Asirifi et al., 2017). Preceptors support students in their learning of clinical skills and report progress and challenges to nursing education institutions (Schuelke & Barnason, 2015). Despite the important roles of preceptors, there are inadequate training programmes for preceptors to improve their pedagogical skills in Ghana (Asirifi et al., 2017).
The number of nursing education institutions doing undergraduate nursing programmes in Ghana has increased in the past decade (Asirifi et al., 2019). In Ghana, clinical placement faces challenges such as lack of support by clinical nurses, ineffective clinical supervision and inadequate classroom preparation (Adjei et al., 2018; Atakro et al., 2019; Salifu et al., 2019). Adjei et al. (2018) found that longer travel hours which results in fatigue on students was a major challenge for clinical placements. Students arrive late for clinical placements due to poor arrangements to ensure the early departure of buses from the campuses, busy road traffic situations and the number of hospitals a particular bus may have to deliver students for clinical placement each day (Asirifi et al., 2017). Also, overcrowding of students during clinical placement has been reported in some instances (Asirifi et al., 2019).
The challenges are not limited to the clinical environment but the nursing education institutions as well. For instance, Bell et al. (2014) in a study in two Ghanaian Universities revealed that there is an inadequate number of lecture halls and equipment in the skills laboratories. They reported that the universities were faced with a lack of supplies such as basic nursing equipment, manikins, patient beds and simulation facilities.
The Nursing Education Stakeholders Group of South Africa upon recognising the impact of clinical nursing education on the professional development of student nurses developed a model to guide the effective clinical training of nursing students (Nurse Educators Stakeholder Group, 2012). The model essentially outlines the role of nursing education institutions, clinical facilities, nursing students and regulatory bodies in clinical nursing education. The present study aimed at exploring key informants’ perspectives of how clinical nursing education in Northern Ghana can be improved by clinical facilities, nursing education institutions and nursing students.
Methods
Research Setting
The study was done in a public university and three selected hospitals in Northern Ghana. The hospitals were a district, regional and tertiary level hospitals. The selected hospitals serve as clinical placement sites for nursing students from the selected public university.
Research Design
An exploratory qualitative design was used to explore the perspectives of key informants of the quality of clinical nursing education. The key informants were nursing lecturers and clinical nurses. The latter were clinical placement coordinators, unit managers and nurse managers. The design enabled the researcher to explore participants’ perspectives of the issue under investigation (Mayan, 2009).
Participants, Sample Size and Sampling Technique
The target population for this study was nursing lecturers, clinical placement coordinators, unit managers and nurse managers. The participants had a minimum of a bachelor's degree in nursing and five years of working experience. Sixteen participants were purposively recruited for the study and data saturation was reached within this group. Data saturation is said to occur when subsequent interviews do not yield new information (Bernard, 2000).
Data Collection Procedure
Having obtained permission from the authorities of the university and the selected hospitals, the primary researcher met the participants individually at their workplaces. The primary researcher explained the purpose of the study to each participant and a suitable date and time was scheduled for the interviews. The participants were allowed to ask questions or make clarifications before signing a consent form to participate in the study. The interviews were conducted face-to-face in the offices of the participants in the English Language only. Permission was obtained from the participants to audio-record the interviews.
Data Analysis
The data were analysed using the framework method of data analysis. The elements of the clinical education model developed by the South African Nursing Education Stakeholders Group served as a template for the analysis (Nursing Education Stakeholders Group, 2012). Framework analysis is a commonly used thematic analysis of transcripts emanating from semi-structured interviews (Pope et al., 2000). Gale et al. (2013) description of the steps of framework analysis was applied to analyse the data. The first step involved transcribing the audio-recorded interviews verbatim, checking for accuracy and becoming familiar with the transcripts. The transcripts were checked for accuracy by both researchers. The primary researcher (NGT) then read the transcripts line by line noting keywords, sentences and paragraphs and giving them codes. The coding was an inductive process with an overarching and deductive framework construction using the elements of the model for clinical nursing education as templates for defining the themes (Nursing Education Stakeholders Group, 2012). The codes were sorted into categories and subthemes under the main themes to form the analytical framework. The analytical framework was discussed by the researchers and a consensus was reached. The analytical framework was used as a guide to analyse the subsequent transcripts. Thus, the emerging codes from the subsequent transcripts were indexed using the existing pre-defined themes, subthemes and categories. An excel spreadsheet was used to create a matrix and the data was charted into it. The researchers interpreted the results by discussing the emerging interesting ideas, connections and characteristics.
Methodological Rigour
Trustworthiness or rigor is the extent to which the identified meanings accurately represent the perspectives of the study participants (Grove et al., 2015, p. 68). Lincoln and Guba (1985) criteria for ensuring the trustworthiness of a qualitative study was applied. Credibility was ensured by having a prolonged engagement with the participants and member checks of the research findings. Some of the participants were contacted to confirm if the findings were congruent with the views they expressed. The researchers gave a clear description of the procedure for the selection of participants, a detailed description of the setting and the processes involved in doing the entire study to ensure transferability. To ensure dependability the researchers documented the method used for data collection, analysis and interpretation. Confirmability was ensured by keeping an audit trail consisting of audio recordings, transcripts and analysis notes.
Findings
Background Information of Participants
Sixteen participants were recruited for the study. All the participants were nurses by profession occupying various positions. The participants consisted of eight unit managers, two nurse managers, three clinical placement coordinators and 3 lecturers. The age of the participants ranged from 27–59 years. The participants had a minimum of 5 years of working experience. Nine of the participants were males and the remaining 7 were females (Figure 1).
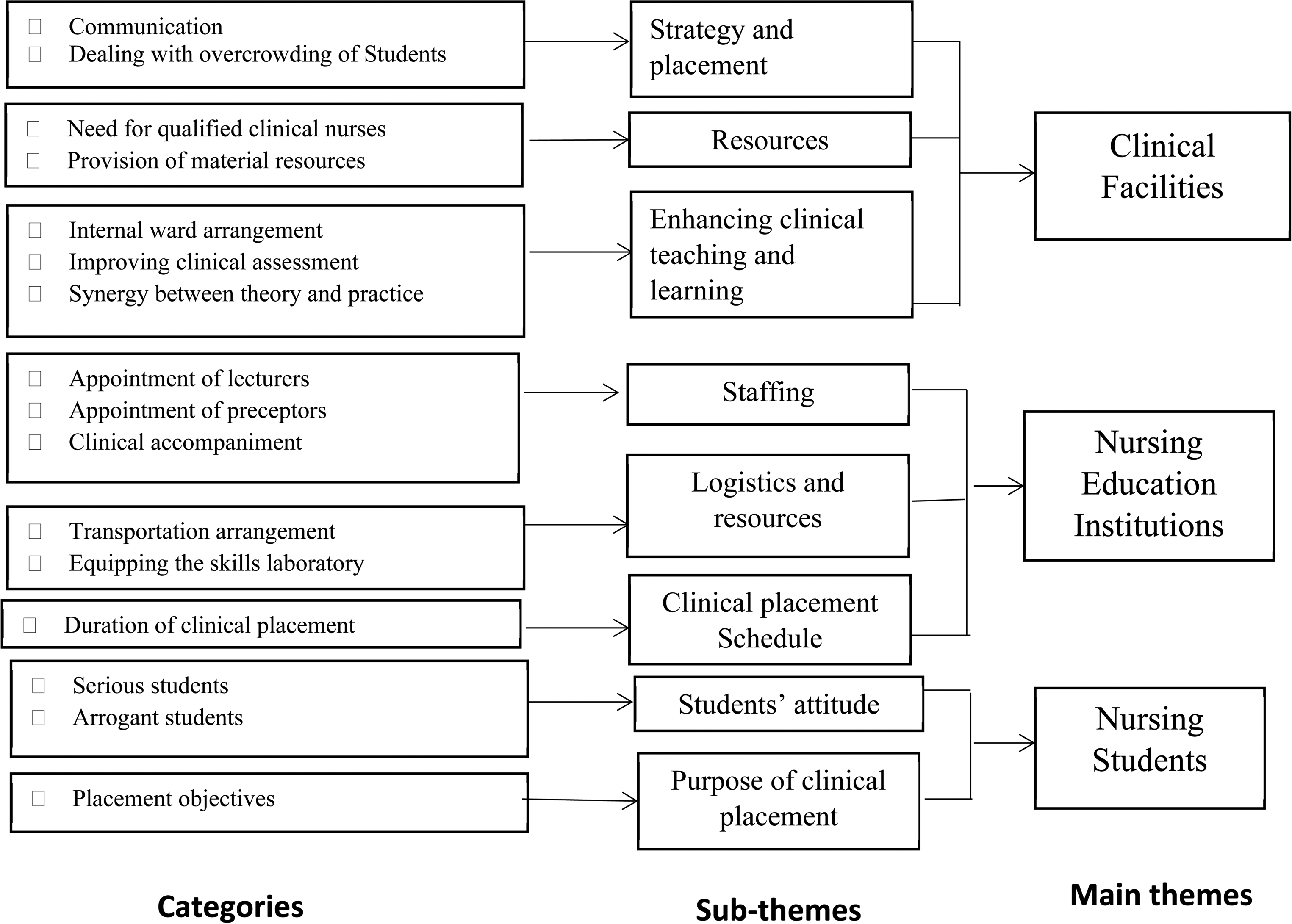
Thematic construction of findings.
Clinical Facilities
This theme revealed factors related to clinical facilities themselves that influence clinical nursing education. The participants indicated the clinical facilities provide important clinical learning opportunities for nursing students. The participants identified three main factors that influence clinical nursing education in the clinical facilities namely, strategy and placement, clinical teaching and learning, and resources.
Strategy and Placement
This subtheme consists of all the steps that were necessary to ensure that clinical placements were effective. The strategies that were deemed essential for effective clinical placement include communication and dealing with overcrowding.
Communication
The participants underscored the need for communication between academic institutions and clinical facilities. According to the participants, since the clinical facilities receive students from many nursing education institutions, effective communication will enable them to schedule to receive them in batches to ensure the effectiveness of clinical placement. A participant shared how communication is a necessary tool. “We have adapted a means where before a school sends us students, they need to communicate with us so that we will assess our capacity to be able to take on the students for clinical placement. If we assess and there are so many students or there are already several schools in the wards we will tell you to hold on until they depart and then you can send us the students” (Participant 9, Clinical placement Coordinator).
Participants stated that effective communication will inform the clinical nurses to know what is expected of the health facilities during the clinical placement so that they could prepare adequately to meet expectations. “I was thinking that even before the students come, the academic staff should come to the facility level, sit with the nurse manager and with the preceptors and say this is the competency areas that we are looking at and this what we expect you to do” (Participant 7, Unit Manager).
Dealing with Overcrowding of Students
The unit managers who participated in the study indicated that the clinical facilities receive nursing students from many academic institutions for clinical placement and this leads to overcrowding of the physical space within the wards. The participants indicated that the situation of overcrowding can be worse when NEIs are on a break during the same period. “There is no space and when the students come they are usually also a lot. Sometimes the students that come are more than the number of patients plus the staffs in the ward. You can have 15 students for one shift” (Participant 2, Unit Manager).
“You have the entire ward crowded with students constantly. During the Christmas break and towards the end of January so many students from different schools are on vacation and they come for clinical placement at the same time” (Participant 4, Unit Manager).
The participants expressed the view that the nursing education institutions should come together to draw a rotational plan for the clinical placement of their students. This will prevent many schools from sending their students to the clinical facilities at the same time “I think there should be some kind of consensus among the nursing training institutions. I know they have individual curricular but I think they should have some kind of consensus so that so many institutions do not send students for clinical practicum at the same period” (Participant 3, Unit Manager).
Resources
Human and material resources are required for clinical nursing education. Registered nurses were the main human resource involved in the teaching of students during clinical placement. The participants also pointed out that material resources were needed for nursing students to learn how to conduct procedures.
Need for Registered Nurses
The participants indicated that the clinical facilities are operating with an inadequate number of registered nurses. The inadequate numbers affect the patient care and clinical teaching of students. “We know the staffing norms in terms of numbers of nurse-patient especially in acute wards and normal general wards. However, we are nowhere near that number so the few nurses who are around are overburdened with work and this affects students teaching” (Participant 9, Clinical placement Coordinator).
There was an indication that some clinical facilities had a cadre of nurses referred to as enrolled nurses to make up the number of nurses required for patient care. However, some participants pointed out that the enrolled nurses may not be able to engage in clinical teaching. “As for the staffing, I wouldn’t say it is adequate because we have two categories of nurses within the facility. That is the enrolled nurses (EN) and that of the registered general nurses (RGN). So the number of RGNs is woefully inadequate and they are the staff that we think plays a key role in the training of the students” (Participant 4, Unit Manager).
Provision of material resources
The participants indicated that the material resources were below the required standard. Some of the participants decided to state the number of available resources on a scale or percentage. “Generally, on a scale of 0–100, I will put it at 60 in terms of having resources to adequately and properly carry out nursing procedures. So the other 40 percent that we don’t have that is what makes the nurses in the clinical field unable to teach students properly” (Participant 4, Unit Manager).
Enhancing Clinical teaching and Learning
This subtheme explained measures that could be taken to improve the teaching and learning of clinical skills during clinical placement. Some unit managers indicated that they try to improve clinical teaching and learning through internal ward arrangements. Other factors that were considered essential were improving clinical assessment and synergy between theory and practice.
Internal ward arrangements
At the ward level, the clinical nurses came out with ways of enhancing clinical teaching and learning. All the strategies that were implemented were planned by the nurses themselves without any directive from the authorities of the hospitals or academic institutions. Some of the wards selected some nurses to assist students in skills learning. Some of the nurses chosen by the unit managers to assist students with skills learning were nurses with an interest in clinical teaching. “Currently we have appointed one staff to handle students’ clinical teaching. That is something we have instilled in the paediatric unit, it rotates from nurse to nurse regarding the responsibility of guiding the students with their clinical practice” (Participant 1, Unit Manager).
“When students come we have nurses in the ward, they are usually two people. Those nurses like to teach so we call them “students’ incharges”. So usually when the students come they are those who handle them” (Participant 2, Unit Manager).
Peer learning was adopted where the students were of the same level of study are grouped because they will have the same placement objectives. “We put them in groups and let's say we are dealing with third year nursing students, so the group may contain students from other institutions. I usually ask them to set daily objectives as a group out of the competencies that they have.” (Participant 3, Unit Manager).
Improving Clinical Assessment
The participants suggested that the current method of clinical assessment of students should be modified. The clinical assessment was considered an essential strategy to determine what skills students have gained during clinical placement. Participants explained that the formative assessment of the students should be conducted instead of doing only summative assessments. “Apart from the exams time there should be an ongoing assessment but we don’t do that. In my ward, since the students have been coming there is no ongoing assessment” (Participant 11, Clinical placement Coordinator).
Some participants suggested that clinical assessment of students should be done in the clinical area since it presents a real-life situation. “Now I would have preferred we move clinical assessment from the skills laboratory to the actual clinical area for OSCEs. Because in the skills laboratory, the students are made to use dummies, mannequins and sometimes role-play, simulations and stories. However, in the clinical area the real clinical situation is facing them” (Participant 9, Clinical placement Coordinator).
For some participants, capacity building in the form of training for assessors and those acting as simulated patients in the clinical skills laboratory during practical examination is very important. The participants also pointed to the need to construct standard tools for the clinical assessment of students. “I think that we need to train the simulated patients and we need to also train ourselves and we should know what we are going to examine the student for. In addition to that, we can develop more tools. Currently, it is the same Nursing and Midwifery Council tools we use which are full of mistakes” (Participant 14, Lecturer 1)
Synergy between Theory and Practice
Students are taught theoretical aspects of nursing in the classroom and are expected to apply this theoretical knowledge in clinical learning. The participants indicated that there was a disconnection between theory and practice. One of the participants had this to say: “Practice seems to be hanging somewhere and theory is also hanging somewhere. It is very difficult integrating the two and it appears no very conscious effort has been made to bridge the two in Ghana unlike elsewhere” (Participant 9, Clinical placement Coordinator).
Some participants attributed the theory-practice gap to a lack of resources. They were of the view that students get confuse when there is lack of material resources for students to translate theory into practice. “We don’t have most of the resources so what is available we try to make use of them. But I think some of the students get confused because they learn the right thing in theory in the school and when they get to the ward it is a different thing because of no materials” (Participant 5, Unit Manager, Unit Manager).
The workload of clinical nurses was also seen as a major cause of the disconnection between theory and practice. Participants opined that when the number of nurses is inadequate they struggle to meet the competing needs of many patients hence they may not be able to follow standard steps in doing procedures. “Some of the nurses and midwives from whom the students learn when they come to the clinical area do not follow the standards sometimes because there is work overload on them. Some may not know actually what they are doing, others are there and they are simply overwhelmed among other things that may make them cut corners” (Participant 9, Clinical placement Coordinator).
Nursing Education Institutions
Clinical placement of students is planned by academic institutions based on their curricula. The amount of time spent on the clinical site is therefore determined by academic institutions. The effectiveness of clinical placement is largely determined by arrangements put in place by academic institutions. Academic institutions provide staffing, resources and logistics, and clinical placement schedules.
Staffing
Staffing is an important means of supporting the clinical learning of students. Clinical teaching of students depends on the availability of staff. Academic institutions are involved in recruiting lecturers, preceptors and planning clinical accompaniment.
Appointment of Lecturers
According to the participants, the academic institutions mandated to train nursing students are woefully understaffed and this affects clinical teaching. Two participants who were lecturers had this to say: “The lecturer who is the clinical placement coordinator is teaching many other courses, having a lot of workloads and then we are also not committed to some of these things. So I think that we have not done what we are supposed to do as a school and a department” (Participant 14, Lecturer 1).
The lack of lecturers puts too much burden on the available few and for that matter they are unable to engage in clinical accompaniment. “But we are also handicapped with staff. The department does not have enough staff. We are not always available or able to go for supervision and the monitoring” (Participant 16, Lecturer 3).
Appointment of preceptors
The engagement of preceptors was seen as a major factor that will help improve clinical nursing education. The appointment of a preceptor formally by the university meant that students will recognize that person and follow his instructions to achieve placement objectives. The preceptors will handle the clinical teaching of students and communicate feedback to academic institutions. The participants observed that there were no trained preceptors in the clinical facilities hence the need for academic institutions to recruit and train nurses for such roles. “When these students get to realize that a preceptor has been formally acknowledged by the university therefore this person is standing in as the clinical instructor on behalf of the institution, they also owe that preceptor some kind of duty to honour him and follow his instructions” (Participant 3, Unit Manager).
Participants saw preceptorship as an organised method of handling the clinical teaching of students. Participants indicated that preceptors know their roles and work within the guidelines from the curriculum. “With the preceptorship, it is a well-organized system that is put in place to ensure that students are well trained. A well-structured curriculum is given to these preceptors or they get training with regards to preceptorship. So when students come, they can ensure that all the objectives set within that timeframe are met” (Participant 4, Unit Manager).
Clinical Accompaniment
Clinical accompaniment was seen as an important step in enhancing the clinical experience of students. The participants expected lecturers to come to the clinical area for accompaniment.
However, participants observed that students were often sent for clinical placement without lecturers coming with them or following up. “I don’t remember seeing any supervisor from the university in my ward here.” (Participant 2, Unit Manager).
“There are certain times the students will come all through out and we wouldn’t see any lecturer following up from the school” (Participant 4, Unit Manager).
Some participants who were lecturers indicated that there was no well-planned strategy by the academic institutions for clinical accompaniment. This confirms what other participants working in the hospitals said about the lack of clinical accompaniment. “As a school, we don’t have any standard or structured way of even monitoring…………. there is poor supervision so you don’t know whether the students are going to the wards or not” (Participant 15, Lecturer 2).
Participant 14, Lecturer 1 added: “Somebody once made a statement that I was even shy. That the students have even complained that they see the tutors from other schools coming to monitor their students whiles they are on the wards and it is like they the from this university are orphans; we leave them there and nobody comes to monitor them” (Participant 14, Lecturer 1).
Logistics and Resources
The academic institutions have the responsibility of providing logistics and resources to ensure effective clinical teaching and learning. The participants identified the need for providing adequate skills laboratory equipment and arranging for transport of students for clinical placement.
Transportation Arrangement
The participants explained that the time of reporting and closing from the ward by the students is affected by the arrangements put in place by the nursing education institutions for the transport of students. The participants indicated that students report late and sometimes close earlier than they should because of the transportation issues. “So that challenge with the bus makes them come late and sometimes an hour before the actual closing, you see them either dodging or seeking permission to run away to wait for the bus to come and pick them back” (Participant 9, Clinical placement Coordinator)
“They go home early, mostly the reason is that there is a bus that has been conveying them to the campus and if they don’t catch up with the bus they will have to foot extra cost in getting to the campus. So; by 1:00 pm the students start leaving the wards when under normal circumstances they are supposed to leave around 2:00 pm” (Participant 3, Unit Manager).
Equipping the Skills Laboratory
The lecturers who participated in the study indicated that the lack of a well-equipped skills laboratory was a barrier to clinical skills training. According to lecturers who participated in the study, innovations such as dividing students into smaller groups and improvising for lack of equipment were all proving ineffective in enhancing skills teaching and learning. “For the second year group of students, they are about 28 in one group that I have to meet for skills at a particular time for 2hours. So assuming I even demonstrate something and I want a return demonstration, how many of them would be able to have hands-on within 2hours?” (Participant 14, Lecturer 1)
“The resources are woefully inadequate; you teach sometimes abstract practical because the things you need to demonstrate are not there so you are forced to improvise. Sometimes what you even use to improvise is not even close to real equipment so it makes it difficult for the students to get the understanding” (Participant 16, Lecturer 3).
Clinical Placement Schedule
Clinical placement planning is done by academic institutions. The academic institutions normally send students to the clinical area with the stipulated duration of the placement. The participants shared their views on the duration of clinical placement and how this could be improved.
Duration of Placement
The participants explained that a longer duration of clinical placement affords the student's a better opportunity for exposure to clinical learning. The participants indicated that clinical placement durations were short and did not contribute positively to students’ skills learning. “Nursing as a profession is more practical based but the students here have more instructional time than the clinical placement” (Participant 9, Clinical placement Coordinator).
“The time spent in the clinical area is absolutely or woefully inadequate; you can’t consider this as even coming close to the standard requirement” (Participant 4, Unit Manager).
Nursing Students
The nursing students are the recipients of clinical nursing education, hence factors related to them must be considered. The attitude of students and the purpose of clinical placement were identified as student-related factors that influenced their learning of clinical skills.
Students’ Attitude
The study revealed that some attitudes of students were good and enhanced skills learning. Other attitudes portrayed by students were negative and hindered skills learning. The attitudes that were identified include serious students and arrogant students
Serious students
Participants explained that some students are serious during clinical placement. Students regarded as serious students were those that show interest in learning clinical skills. Participants indicated that serious students were always willing to learn by participating in nursing care even when they were not invited. “When it comes to learning skills, some students are eager to learn. There are some students that naturally they will come and when they just see you getting up to do a procedure they are following; others too are adamant-sitting down” (Participant 2, Unit Manager).
Arrogant Students
Participants also noted a display of pride among some of the students. According to the participants, some of the clinical nurses from whom the nursing students are supposed to learn from are diploma or even certificate holders hence some university nursing students are being disrespectful towards them. Some participants explained that the university nursing students’ uniform is meant for senior nurses and this makes some of the students proud. “Some of the students too their attitude is very bad. They are wearing “white”(white colour is worn by senior staff) so when they come to the wards they feel “on top”. Some of them when they come you just see that they are already looking down upon those who are wearing the “green”(green colour is won by junior staff)”. (Participant 5, Unit Manager, Unit).
“You see because they know that when they complete they will be senior to the staff nurses, some of them are just proud.” (Participant 7, Unit Manager).
Purpose of Clinical Placement
Students are normally prepared for clinical placement based on the curriculum that is used for their training. Clinical placements are meant for students to achieve certain practical competences according to the schedule of training. However, the participants pointed out that students were not focused on achieving clinical placement objectives.
Placement Objectives
Students are normally given objectives prepared from the school for clinical placement. Achieving these objectives will help students become clinically competent. According to the participants, coming with placement objectives to the clinical area was seen as a formality. A participant indicated that students simply hand the objectives to the unit managers without making any reference to them when necessary. “What I have realized is that they come with objectives/competencies. In my observation, it is like just something they come with to give to the unit manager or staff receiving them but they don’t usually put their attention on the objectives/competencies. It is like it is just something formal that they have to fulfill” (Participant 11, Clinical placement Coordinator).
Discussion
The study revealed that factors that influence clinical nursing education are issues related to clinical facilities, academic institutions and nursing students. The study findings indicated that there are times when the wards are overcrowded with students. The overcrowding of students in the clinical area could be as a result of the increase in the number of nursing education institutions in Ghana (Asirifi et al., 2019). Overcrowding of students in the clinical area has also been found as a major challenge facing clinical nursing education in Malawi, Iran and Angola (Bvumbwe et al., 2015; Jamshidi et al., 2016; Marchi-Alves et al., 2013). In Malawi, Bvumbwe et al. (2015) found that there were times where 23 nursing students were placed in a ward that has 15 patients. It can be argued that when students are overcrowded in the ward it may be difficult for all of them to observe and effectively practice or learn nursing procedures. Scheduling students for clinical placement based on the clinical facility's capacity to accept them may be an important step to consider. The participants in the present study suggested that nursing education institutions could communicate among themselves to ensure that they do not send students to the clinical placement area at the same time. Also, communication of clinical placement dates and objectives with clinical facilities is a necessary step to ensure that students receive the expected support.
In the clinical placement area, registered nurses are directly involved in supporting students to learn clinical skills. In Ghana, there are two cadres of nurses which include professional nurses referred to as registered general nurses and nurse assistants. The nurse assistants are trained for two years and they assist the registered nurse in the discharge of their duties. The participants in this study particularly nurse managers and clinical coordinators were of the view that the number of registered nurses was inadequate. This study finding concurs with a Malawian study which revealed that the number of registered nurses was inadequate and this negatively affected clinical teaching and learning (Kamphinda et al., 2019). In Ghana, the inadequate number of clinical nurses is reportedly associated with the increased workload on the available few (Adjei et al., 2018). Increased workload on registered nurses may make them unable to assist students with skills learning because of the pressure associated with trying to meet patient care. The Ghana Health Service needs to consider posting more registered nurses to clinical facilities that act as clinical placement areas for nursing education institutions.
The participants in this study cited the lack of material resources as a major factor responsible for the gap that exists between theory and practice. In the classroom, students are taught standard steps in carrying out procedures and this requires the use of certain material resources or equipment. This finding agrees with other studies in Ghana which point to the lack of material resources as a key constraint in clinical nursing education (Adjei et al., 2018; Salifu et al., 2019). When the clinical environment is unable to support the translation of the theory learned into practice it affects the skills development of students. Clinical facilities serving as learning sites for students should therefore be supported by the authorities to acquire adequate material resources for nursing procedures.
The study participants indicated the need for the appointment of preceptors to provide a formal support system for students to learn clinical skills. Preceptorship is recognized as an effective means of improving clinical nursing education. The preceptors play an important role in supporting students with clinical learning by acting as role models, mentors, tutors, supervisors, and coaches (Girotto et al., 2019; Madhavanpraphakaran et al., 2014; Niederriter et al., 2017). Lecturers also rely on feedback from preceptors to monitor the progress of clinical skills development (Asirifi et al., 2017). In Ghana, the preceptors in most cases are clinical nurses with personal experience but no formal training. When preceptors are trained it will enhance their capacity to engage in clinical teaching.
The study findings indicated that the skills laboratory of the nursing education institution where this study was conducted was inadequately equipped and small in size. This finding agrees with an earlier study in two other universities in Ghana which also had inadequately equipped skills laboratories (Bell et al., 2014). Muthathi et al. (2017) suggested putting students in groups for skills laboratory training to improve participation. However, lecturers who participated in this study thought that considering class size, grouping the students inevitably result in larger group sizes which makes it difficult to have returned demonstrations. Providing an adequately equipped skills laboratory and ensuring the intake of students matches the available space will be an important step to be considered by academic institution authorities.
When students are serious about their clinical placement it positively affects their skills development. The study findings indicate that some of the students were not serious about gaining clinical competencies especially those in the second year and beyond. The findings disagree with a study in Jordan which indicated that students in higher classes had positive attitudes towards skills learning (Gharaibeh et al., 2017). The level of support students receive could be an important factor that influences their stance towards learning of clinical skills. There will be the need to have scheduled clinical conferences with nursing students during clinical placement. The conferences will allow the faculty to offer students the support they require.
Strengths and Limitations
The study was the first to assess the state of clinical nursing education in Northern Ghana from the perspective of key informants. The recruitment of key informants from the academic and clinical placement area gave a multidimensional view to the study that can inform decision making to improve the state of clinical education.
The recruitment of lecturers from one public university may not yield views that are representative of all the nursing education institutions in Ghana.
Implications for Nursing Practice
Effective communication between NEIs and clinical facilities was identified as one important strategy for improving clinical teaching. When there is effective communication between clinical facilities and nursing education institutions, a clinical placement schedule could be agreed upon to resolve overcrowding at the clinical placement area.
Preceptorship is necessary to enhance the teaching of clinical skills. However, currently in Ghana, most preceptors are not trained hence there is the need for collaboration between nursing education institutions and clinical facilities to provide training programmes for preceptors. Also, due to the increasing number of students requiring clinical placement, there may be the need to negotiate with clinical facilities to ensure that preceptors are given a protected time to support students.
Clinical accompaniment by lecturers is an important strategy for improving the supervision of students. In the present study, the participants reported lack of clinical accompaniment by lecturers because of the inadequate number of lecturers. That notwithstanding, adding clinical accompaniment to essential duties of nursing lecturers will result in effective clinical supervision.
The provision of adequately equipped skills laboratories by nursing education institutions was identified as an important strategy to improve clinical teaching and learning. A well-equipped skills laboratory will allow students to practice nursing procedures before going to the clinical area. Also, clinical facilities having the material resources required for nursing procedures will enable students to learn clinical skills. Clinical facilities that are used for clinical placement of students should endeavour to provide material resources to facilitate clinical teaching of students
The clinical assessment provides information on the progress of students in the development of clinical skills. Building the capacity of preceptors to ensure that they carry out effective formative assessments of students during clinical placement is essential in monitoring students’ progress. Also, to improve the assessment of clinical competency of students there is the need to implement a scheduled training of all preceptors and lecturers involved in clinical assessment.
Conclusion
The study findings indicate the need for nursing education institutions to work closely with clinical facilities to ensure that clinical placements are effective in improving the clinical skills development of students. Planning and implementing continuous professional development programmes for clinical nurses to build their capacity to assume the role of formal preceptors an important step in improving clinical education. The planning of clinical skills placement should ensure that students are not overcrowded during clinical placement. Also, nursing education institutions could improve clinical nursing education by equipping the skills laboratories, engaging an adequate number of lecturers, and carrying out clinical accompaniment.
Footnotes
Acknowledgments
The authors wish to thank Dr Hilary Thurling for co-supervising and supporting this study. We also wish to thank the participants of the study.
Availability of Materials
The original transcripts from which the paper emanated are available upon request from the corresponding author.
Ethical Considerations
Ethical Clearance was obtained from the Human Research Ethics Committee (Medical), University of the Witwatersrand (M190807) and Ghana Health Service Ethics Committee (GHS-ERC 007/09/19). A voluntary informed consent was signed by the participants before interviews and permission was obtained to allow for audio-recording, transcription, taking of field notes and reporting of their descriptions. Personal or identifying data were not collected and participants were assured of their confidentiality.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This paper is drawn from a broader study submitted to the University of the Witwatersrand, Johannesburg. South Africa for the award of PhD in nursing education. The candidate was awarded the Postgraduate Merit Award for the PhD studies by the University of the Witwatersrand, Johannesburg.
