Abstract
Introduction
Clinical supervision is a crucial aspect of developing nursing students' knowledge, skills, and professional attitudes. The characteristics of clinical instructors have a significant role in the progress and transition of students into their future professional roles.
Objective
The study aimed to examine the behaviors of effective clinical instructors as perceived by nursing students and faculty members in the UAE.
Methods
The study followed a cross-sectional quantitative research design to explore nursing students' and faculty members' perceptions of clinical instructors' effective behaviors that facilitate students' clinical practice. Data were collected from a convenience sample of 147 nursing students and 17 faculty members who completed an online version of the study survey at four nursing programs in the UAE.
Results
Students rated personality (M = 4.96, SD = 1.91) and teaching ability (M = 4.94, SD = 1.96) as the highest behaviors for effective clinical instructor. They perceived effective clinical instructor to be organized (M = 5.19, SD = 1.88), shows self-confidence (M = 5.16, SD = 1.84), able to answer questions (M = 5.16, SD = 1.90), emphasizes what is crucial to learn (M = 5.11, SD = 1.81), and takes responsibility for his/her actions (M = 5.11, SD = 1.90). While faculty members perceived effective clinical instructor to encourage a climate of mutual respect (M = 5.56, SD = 1.27), be approachable (M = 5.47, SD = 1.32), demonstrates clinical skill and judgment (M = 5.53, SD = 1.46), takes responsibility for his/her actions (M = 5.53, SD = 1.37), and be a good role model (M = 5.47, SD = 1.32).
Conclusion
Understanding clinical instructors' effective behaviors and supporting them during students' clinical experiences inspire a productive teaching-learning environment that is crucial to improve students' motivation, expand their learning opportunities and improve their hands-on skills.
Background
Nursing is a practice-based profession that requires quality clinical education for student nurses to develop the necessary clinical skills for safe practice in complex real-life situations (Madhavanprabhakaran et al., 2013). The goal of nursing education is to prepare student nurses who are able and committed to perform safe nursing care (Dimitriadou et al., 2015). To achieve this goal, students require clinical training experiences that promote the integration of the theoretical and practice components of the nursing curriculum and transform it into professional knowledge, skills, and attitudes (Papastavrou et al., 2016). Students' clinical training experiences are the training endeavors where undergraduate nursing students develop their competencies to practice confidently, independently and make quality practice decisions (Nehrir et al., 2016). The integration of adequate theoretical and practical clinical skills in well-structured clinical experiences prepare nursing students to assume their professional role and practice in real and complex healthcare settings (Kaihlanen et al., 2019). Students’ academic success depends on several influencing factors, such as implementing an effective model of clinical supervision (Henderson & Tyler, 2011), well-trained clinical instructors (Mackay et al., 2014) and the support of staff nurses (Kaphagawani & Useh, 2013). Any deficiency in one of these factors might result in undesirable effects on students' academic achievements (Arieli, 2013).
Clinical instructors have an essential role in shaping and facilitating students' learning in clinical areas. Educational and healthcare practice institutions facilitate students' learning by introducing quality experiences where students have supernumerary positions to practice under the supervision of competent nursing instructors to guide the students and promote their academic success (Hutchings et al., 2005; Pollard et al., 2007). Clinical instructors assist nursing students to integrate classroom teaching with clinical practice and to develop their clinical reasoning and decision-making skills (Oermann & Gaberson, 2016). Hence, instructors are considered the focal point in the student-staff-patient relationship, and to be able to do their job effectively, they need to own particular professional traits such as professional knowledge, clinical competence, effective communication, and role model skills (Barnett & Matthews, 2009).
Niederriter et al. (2017) identified four main characteristics for clinical instructors to assume their effective role. These characteristics were the ability to build trusting relationships, to have enough clinical knowledge and expertise, appropriate coaching abilities, and role-model characteristics. Gardner and Suplee (2010) stated that clinical instructors need to have adequate clinical expertise, problem-solving, clinical reasoning, and expert psychomotor skills. Additionally, clinical instructors need to have excellent leadership abilities, trusted by their colleagues, accountable for their actions, mature, open-minded, have non-judgmental behavior towards nursing students and self-confident.
Examining the perceptions of nursing students and faculty members toward clinical instructors' behaviors at the clinical setting is significant to maintain the quality of students’ clinical experiences and ensure adequate preparation of competent, safe and caring nursing graduates. Hence, this study aimed to examine the behaviors of effective clinical instructors as perceived by nursing students and faculty members in the UAE. Precisely, the study focused on the following objectives:
To identify the behaviors of effective clinical instructors as perceived by students and faculty members. To differentiate between the clinical teaching behaviors that students perceive as having the greatest and least influence on learning. To rank the frequencies of teaching categories as perceived by students and faculty members. To recognize any difference in the perceptions among participants towards the characteristics of a good clinical instructor.
Methods
Research Study Design, Setting, and Participants
A cross-sectional quantitative study was conducted to examine the behaviors of effective clinical teachers as perceived by nursing students and faculty members at Fatima College of Health Science (FCHS). FCHS is a governmental entity established in 2006 and is the primary allied health and nursing education provider in the UAE. The college has four campuses, three campuses in the Emirate of Abu Dhabi, and one campus in the Emirate of Ajman. The sample size was 147 students who completed at least one clinical training experience in the real clinical setting and 17 faculty members who have at least five years of experience in supervising nursing students’ clinical experiences. Participants were asked to complete an online version of the study survey at the four FCHS nursing programs in the UAE.
Instrument
The study used the Nursing Clinical Teacher Effectiveness Inventory (NCTEI) survey tool. Knox and Mogan (1985) developed the tool to assess effective clinical instructors' characteristics that affect nursing students' learning experience. The tool was not modified and kept in the English language form. The first part of the tool consists of participants' demographic information, which includes age, gender, occupation, level of study, and geographical location. The second section has 47 items describing clinical teacher behavior within five categories: Teaching ability, Nursing competence, Evaluation of students, Interpersonal relationship, and Personality of the clinical teacher. Participants were asked to describe the characteristics of a particular clinical instructor on a seven-point Likert scale (1 = not at all descriptive, 7 = Very descriptive). The third section asked participants to suggest ways to improve students' clinical preceptorship experience. Knox and Mogan reported that the tool was reliable and internally consistent (r = .79-.82) and was stable over time. Test-retest scores at 4 weeks were (r = .76-.93) indicating adequate reliability. Face and content validity were determined through a review of the literature and nursing experts (Mogan & Knox, 1987).
Data Analysis
The collected data were compiled and analyzed using Statistical Package for the Social Sciences (SPSS) version 21. Descriptive and inferential analysis was performed to summarize and present the demographic and participants' responses. The means and standard deviations were computed to identify clinical instructors' effective behaviors and describe the highest and lowest frequencies of behaviors influencing students' learning. A Mann-Whitney U test was used to determine the significant difference in perceptions of clinical instructor behaviors among nursing students and faculty members.
Ethical Considerations
The study received ethical approval from the FCHS Ethics Governance Committee before the commencement of the data collection (reference number: CHS/RECA/#019/2018-19). The aim and nature of the study and procedure were explained to all participants before data collection. Participants' anonymity and confidentiality were continuously guaranteed and protected throughout the study.
Results
Demographic Data
The demographic characteristics are summarized in Table 1. The majority of the respondents were between 20 and 25 years old (82.3%) and were mostly females (94.5%). 89.6% of the respondents were nursing students enrolled in the traditional BSN program (100%), and 10.4% were faculty members. Respondents were located at four different nursing programs in the United Arab Emirates; Abu Dhabi (15.8%), Ajman (24.4%), Al Ain (31.1%), and Al Dhafra (28.7%).
Demographic Characteristics.

Teaching Behaviors: Students' Perceptions
The results showed that the highest behaviors as perceived by students (see Table 2) were ‘appears organized' (M = 5.19, SD = 1.88) and self-confidence' (M = 5.16, SD = 1.84) from Personality teaching category, ‘answers carefully and precisely questions' (M = 5.16, SD = 1.90) and 'emphasizes what is important' (M = 5.11, SD = 1.81) from Teaching Ability category, and 'takes the responsibility of own actions' (M = 5.11, SD = 1.90) from Nursing Competence category.
Highest Rating Behaviors as Perceived by Students (n = 147).

The lowest behaviors perceived by students (see Table 3) were ‘communicates expectations of students' (M = 4.87, SD = 1.91) from the Evaluation teaching category and ‘promotes student independence' (M = 4.86, SD = 2.08), ‘remains accessible to students' (M = 4.85, SD = 1.98), ‘provides specific practice opportunity' (M = 4.85, SD = 2.01), and ‘enjoys teaching' (M = 4.85, SD = 2.08) from the Teaching category.
Lowest Rating Behaviors as Perceived by Students (n = 147).

Teaching Behaviors: Faculty Perceptions
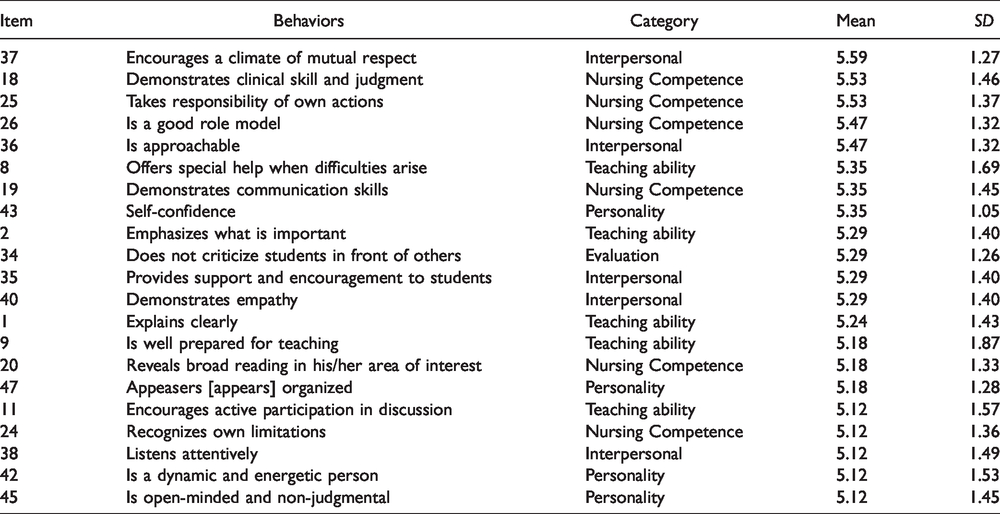
The results showed that the highest behaviors as perceived by faculty members (see Table 4) were ‘encourages a climate of mutual respect’ (M = 5.56, SD = 1.27) and ‘is approachable' (M = 5.47, SD = 1.32) from the Interpersonal Relations teaching category, and ‘demonstrates clinical skill and judgment' (M = 5.53, SD = 1.46), ‘takes the responsibility of own actions' (M = 5.53, SD = 1.37), ‘a good role model' (M = 5.47, SD = 1.32) from Nursing Competence category.
Highest Rating Behaviors as Perceived by the Faculty Members (n = 17).
The lowest behaviors perceived by faculty members (see Table 5) were ‘guides students' development of clinical skills' (M = 4.94, SD = 1.71), ‘quickly grasps what students are asking or telling' (M = 4.94, SD = 1.47), ‘gears instruction to students level of readiness' (M = 4.88, SD = 1.65) and ‘helps students organize their thoughts about the patient' (M = 4.88, SD = 1.61) from the Teaching Ability teaching category, and ‘is self-critical' (M = 4.94, SD = 1.34) from Personality teaching category.
Lowest Rating Behaviors as Perceived by the Faculty Members (n = 17).

The Rank of Teaching Categories
The frequencies of teaching categories, as perceived by students, are presented in Table 6. Respondents ranked the personality of the clinical instructors as the highest teaching category (M = 4.96, SD = 1.91), followed by teaching ability (M = 4.94, SD = 1.96) and interpersonal relations (M = 4.90, SD = 1.86). The lowest scored categories were nursing competence (M = 4.88, SD = 1.92) and evaluation (M = 4.85, SD = 1.98).
The Rank of Teaching Categories Among Students (n = 147).

The frequencies of teaching categories, as perceived by faculty members, are presented in Table 7. Respondents ranked the interpersonal relations of clinical instructors as the highest teaching category (M = 5.29, SD = 1.43), followed by nursing competence (M = 5.18, SD = 1.41) and personality (M = 5.10, SD = 1.36). Teaching ability (M = 5.02, SD = 1.57) and evaluation (M = 4.81, SD = 1.61) were the lowest scored teaching categories.
The Rank of Teaching Categories Among Faculty Members (n = 17).

In Table 8, a comparison of the mean scores of the five teaching categories between nursing students and faculty members was performed using the Mann-Whitney U test. The result showed no significant evidence to support any difference between the ratings of the two groups (p > 0.05).
The Difference in Perception Between Nursing Students and Faculty Members (N = 164).
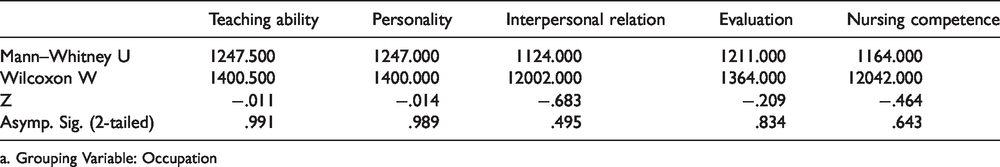
a. Grouping Variable: Occupation
Narrative Responses
This section had one open-ended question asking the participants to suggest ways to improve students' clinical supervision experiences. Participants' narratives were analyzed using content analysis (Polit & Beck, 2012). All narratives were read repeatedly and comprehensively to identify similar themes. Three themes emerged from the data: students' motivation, learning opportunity, the readiness of instructors.
Sixty-seven participants highlighted the need to improve students' motivation during clinical practice. To achieve this, participants cited that instructors have to treat students with more respect, be more flexible and supportive, deliver feedback frequently, answer students' queries and show a welcoming attitude. Fifty-one participants emphasized on improving students' learning opportunities during clinical experiences. Securing adequate learning opportunities by clinical instructors enhance students' involvement in comprehensive nursing care, facilitates the integration of theory to practice, and improves their overall clinical competence. Thirty participants indicated that clinical instructors should be well prepared to teach and oriented to students' learning needs. Nursing students are influenced by clinical instructors' attitudes and desire to teach. Instructors should have an adequate professional attitude that entitles them to act as role models for nursing students and be willing to perform this job. They must be open to students' questions, open-minded, and show enthusiasm and willingness towards working with students.
Discussion
The study aimed to examine the behaviors of effective clinical instructors as perceived by nursing students and faculty members. The findings suggest that participants have precise expectations of the behaviors of clinical instructors in facilitating students' clinical experiences. Nursing student rated the personality and teaching ability, as the highest categories for an effective clinical instructor. Students expected clinical instructor to be organized, able to answer precisely their questions, show self-confidence, emphasize what is crucial for them to learn, and take responsibility for his/her actions. The least rated category by the students was evaluation, and the least rated behaviors were the ability of the clinical instructor to give students positive reinforcement for good contributions, observations, or performance and identify students' strengths and limitations objectively. Alternatively, faculty members rated interpersonal relations and nursing competence as the highest categories for effective clinical instructors and rated evaluation as the lowest category. Faculty members expected an effective clinical instructor to encourage a climate of mutual respect, be responsible for his/her actions, demonstrate clinical judgment, and be a good role model.
The study findings were consistent with other studies such as Bifftu et al. study in Ethiopia, which found that the majority of students reported personality traits and teaching abilities as the most effective clinical instructors' behaviors. The majority of faculty members reported interpersonal relations and nursing competence as the most effective behaviors (Bifftu et al., 2018). In the Philippines, Soriano and Aquino found that the majority of the students selected personality traits and interpersonal relations as the most effective behaviors, and faculty members selected nursing competence and teaching abilities as the most effective ones (Soriano & Aquino, 2017). In Egypt, Ismail reported that students' most rated effective behaviors were teaching ability, nursing competence, and evaluation (Ismail et al., 2016). In Saudi Arabia, Gangadharan et al. (2016) found that the majority of the students reported personality traits, evaluation, and teaching ability as the most effective behaviors. The last two studies reported evaluation as one of the most effective behaviors, whereas participants in this study reported evaluation as the least effective behavior of clinical instructors. Clinical evaluation is the process used by clinical instructors to judge students' clinical performance and competencies in nursing practice (Oermann & Gaberson, 2016). Delivering students with constructive, prompt, timely, supportive, and encouraging feedback is a central responsibility to the clinical instructors (Clynes & Raftery, 2008; Ismail et al., 2016). To perform their job effectively, clinical instructors must have sound interpersonal skills that allow them to deliver effective teaching, provide constructive feedback and create positive relationships with students (Koy, 2015).
Recommendations for Nursing Education and Policy
The findings of this study provided recommendations that could be used by nursing education and administration to improve students' clinical supervision while on clinical practice. The study participants identified specific behaviors for clinical instructors such as flexibility, supportiveness, and ability to deliver frequent and prompt feedback. Nursing instructors need to be able to build trusting relationships based on mutual respect with the students. Also, clinical instructors should have an adequate professional attitude that entitles them to act as role models for the students, demonstrate maturity and self-confidence, and have non-judgmental behavior.
Faculty members need to have more collaboration with the nursing instructors to supervise the progress of students during clinical experiences. Faculty members have to be more available in clinical settings to provide students with more guidance and deliver better support for clinical instructors. Faculty members should be available to provide direction, clarification, and needed feedback for the clinical instructors throughout students' clinical practice.
The academic programs also have a responsibility to prepare and select clinical instructors who are willing to teach and have enough knowledge and skills to perform their roles. Nursing programs could deliver comprehensive orientation for clinical instructors on students' curriculum, teaching methods and students' learning objectives. Instructors' preparation program is necessary for clinical instructors to perform their role confidently and effectively. This program may include principles of adult learning, students' learning needs, evaluation of students' performance and clinical teaching methods. The program could also embrace elements of students' motivation, dealing with challenging students, and techniques of student coaching.
Limitations
Several limitations could be identified in the study despite the measures taken to assure its rigor. First, the perceptions of some of the participants might not be representative due to individual experiences during clinical practice. Second, personal commitments, work, or time-related factors could have affected participants’ amount of attention given to complete the survey. Third, there is a possibility that some participants may have given imprudent responses that do not reflect their real opinions to complete the survey quickly. Fourth, the sample of the study included nursing faculty members and students from one educational institution; hence, the findings might not be representative of all nursing education institutions in the UAE. It would be of importance to repeat the study and include other nursing programs in the UAE.
Conclusion
Overall, the findings of the study indicated that the behavior of clinical instructors has a significant influence on nursing students' clinical experiences. Nursing students and faculty members expect instructors to be supportive, interested, build trust relations with students and deliver effective feedback to prepare students for their future professional role. The most effective behaviors of clinical instructors as perceived by the students were personality, teaching ability, and nursing competence, whereas interpersonal relations and nursing competence were the most effective behaviors for faculty members. The least effective behaviors for both students and faculty members were evaluation, teaching ability and personality. The study did not show significant evidence to support any difference between the ratings of the two groups of participants. Understanding clinical instructors' effective behavior is significant to improve students' motivation, expand their learning opportunities, improve their hands-on skills and inspire a productive teaching-learning environment. Continuous support of clinical instructors by the nursing programs to perform their role facilitates the better and smoother transition of students into their future professional roles.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
