Abstract
Communication gaps within healthcare systems significantly compromise patient outcomes. This article explores systemic challenges through the dual lens of personal experience as a cancer survivor and professional insights as a human-centered design leader. Drawing on an IRB-approved study and literature review, it examines how ineffective communication creates barriers to patient understanding and safety, with disproportionate impacts on marginalized populations. The article introduces an innovative application of human-centered design methodology to transform healthcare communication by prioritizing patient needs and experiences. Seven evidence-based strategies provide actionable frameworks for healthcare stakeholders to enhance communication clarity, accessibility, and effectiveness, creating a more equitable, patient-centered healthcare system that serves all populations effectively.
Keywords
Introduction
My journey as a cancer patient illustrates critical issues in healthcare delivery. My abnormal biopsy results were initially overlooked due to poor communication, and I was misinformed that the biopsy was benign. Only through my insistence on an additional biopsy—a decision that saved my life—was the truth revealed: I had cancer. This diagnosis was delivered in an email filled with medical jargon that never explicitly mentioned “cancer.” When I sought clarity from my surgeon, I was dismissed. ‘You're smart enough to figure it out,’ he said, directing me to a breast cancer book.
This analysis explores the systemic nature of health communication failures and their cascading impacts on healthcare delivery. These gaps represent not just individual provider-patient challenges but fundamental system-level barriers that impact care quality, safety, and outcomes across populations. Understanding these challenges from a systems perspective allows us to address the structural and human factors perpetuating communication failures and health inequities. This article provides a framework for transforming health communication at individual and institutional levels, offering evidence-based strategies for driving systemic change.
This analysis's insights and case examples stem from an IRB-approved study at Emory School of Medicine and a systematic literature review demonstrating how communication failures occur in real-world healthcare.
The Cost of Miscommunication: Critical Gaps in Patient Care
Communication gaps in healthcare pose serious challenges in patient care, increasing the risk of medical errors and adverse events. 1 In the United States, 88% of adults have substandard health literacy, 2 and communication failures contribute to over 70% of sentinel events. 3 In operating rooms, communication breakdowns occur in 30% of team exchanges, jeopardizing patient safety. 4 These preventable issues, including medication errors, account for over 50% of global patient harm 5 and create substantial economic burden—linked to 15% of hospital expenditures and costing the US healthcare system over $17 billion annually. 6 Addressing communication gaps is critical to improving healthcare safety and outcomes.
As a principal investigator, I encountered multiple cases highlighting these communication breakdowns. A patient with multiple myeloma left her consultation unaware of her cancer diagnosis until reading a newspaper headline about the disease. This miscommunication delayed her treatment and impacted her life.
Another patient discontinued her cancer medication due to unclear instructions, resulting in rapid disease progression. Such communication failures impede treatment adherence, leading to poorer outcomes, increased hospitalizations, and chronic disease complications.
Health Literacy: A Systemic Responsibility
Health literacy—the ability to find, understand, and use information to make informed health-related decisions—plays a critical role in addressing these communication gaps. Improving health communication involves more than just sharing information; it requires ensuring patients and families can comprehend and act on that information. When healthcare providers fail to bridge this understanding gap, patients struggle to navigate their healthcare journeys, leading to worse health outcomes.
While the CDC's Healthy People 2030 initiative lays a strong foundation for improving health literacy, translating these guidelines into practice remains a challenge. To empower patients to understand their conditions and make informed decisions, we need solutions that bridge the gap between medical guidelines and real-world practice at the bedside.
By prioritizing clear, jargon-free, and empathetic communication, we can empower patients to take an active role in their healthcare. This shift in approach transforms health literacy from a patient's deficiency into a healthcare provider's responsibility. When providers communicate effectively and meet patients where they are, they foster understanding and engagement, leading to improved health literacy and better health outcomes. The financial impact of addressing literacy is substantial: low health literacy costs the US economy between $106 billion and $238 billion annually. 7
Actionable Insights
Human-Centered Design: A Methodology for Transforming Health Communication
My perspective on addressing health communication challenges is shaped by my background in human-centered design and my personal experience as a patient. The human-centered design methodology offers a systematic approach to understanding patient needs and creating evidence-based healthcare solutions through iterative testing and stakeholder engagement. Key strategies include fostering empathy, co-designing solutions with patients, and conducting iterative testing across diverse populations.
By combining my firsthand healthcare experience with the insights from patients interviewed in my IRB-approved study, I have identified critical barriers to effective communication between medical professionals and patients. My personal journey of experiencing delayed diagnosis, along with cases from my research, demonstrates how human-centered design principles could help prevent these harmful breakdowns. This multifaceted approach, which integrates design with a profoundly deep understanding of patient experiences, has enabled me to develop innovative solutions that bridge clinical expertise and real patient experiences at the bedside. Imagine a healthcare system where every interaction empowers patients, information integrates seamlessly, and enhanced understanding improves experiences and outcomes for all.
Communication as Health Equity: Beyond Access
As we work to improve health communication, it is crucial to acknowledge its close connection to health equity. Health communication initiatives must address the unique obstacles that marginalized communities encounter, going beyond merely offering interpretation services and multilingual materials. We must identify and confront the additional burdens these communities face, as they often experience the most significant consequences of ineffective health communication. 8
Effective health communication requires empathetic approaches that bridge cultural barriers. By genuinely understanding the experiences of diverse patients, we can address communication deficiencies that disproportionately affect marginalized populations. This transformative, empathetic approach is vital for bridging the gap in healthcare disparities and advancing health equity.
Through this lens of communication as health equity, we can create a healthcare system that ensures all patients—regardless of their background—have equal access to understanding and engaging with their healthcare. This human-centered approach empowers individuals to actively participate in their care, ultimately improving health outcomes.
Practical Recommendations
Seven Strategies to Transform Health Communication
This evidence-based framework integrates human-centered design principles with identified challenges in healthcare communication, as visually represented in Figure 1. Healthcare organizations can apply these strategies independently; however, the first strategy—fostering empathy—acts as the foundation for all the subsequent strategies, forming the core of our human-centered approach. Collectively, the seven proposed strategies strive to enhance interactions among patients, providers, and healthcare systems.
Cultivate empathy: Deepen understanding of patient perspectives through immersive learning, shadowing, and engaging with patient narratives. Enhance skills: Equip providers with empathetic communication and teach-back techniques. Emphasize plain language and ensure patient understanding through verification. Prioritize health equity: Design inclusive health communication to break systemic barriers and serve all cultural groups. Localize communication: Collaborate with communities to develop strategies that integrate cultural contexts beyond translation. Design for accessibility: Develop clear, user-centered materials through patient input and usability testing to ensure understandability and actionability. Prevent medical errors: Leverage human-centered design to improve communication and handoff protocols, ensuring safe and accurate care. Harness technology: Develop intuitive digital tools that simplify medical information and enhance patient interactions, ensuring clarity and ease of use.
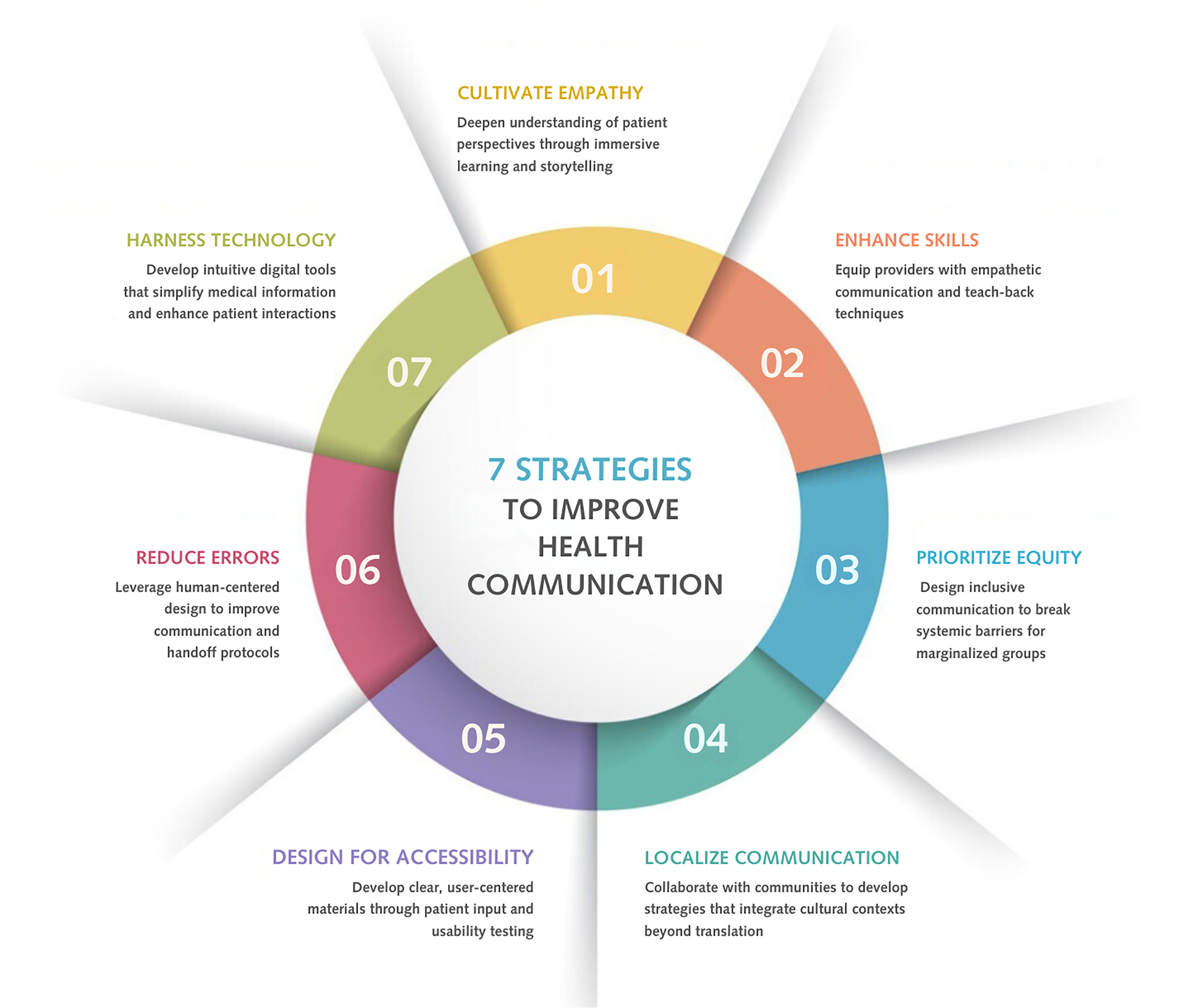
A human-centered framework for health communication.
Figure 1 visually demonstrates how these strategies interconnect to create a comprehensive approach to health communication transformation. The diagram emphasizes how empathy serves as the central foundation from which all other strategies extend.
Table 1 presents evidence from the literature demonstrating a significant return on investment from health communication interventions similar to those proposed in our framework. These findings highlight the potential impact when implementing improved communication approaches aligned with the strategies outlined in Figure 1.
Evidence-Based Outcomes of Health Communication Strategies.

From the patient's perspective, these strategies serve as crucial lifelines and vital opportunities to improve communication and prevent medical errors and misunderstandings. The urgency lies in creating a healthcare system that prioritizes understanding patient experiences and fosters effective communication. By doing so, we ensure meaningful improvements in patient outcomes. Transforming healthcare into a truly patient-centered, health-literate system is not just about improving metrics; it is about saving lives, reducing suffering, and empowering patients to actively participate in their care through shared decision-making.
Conclusion
To create a more informed healthcare system, various stakeholders can take immediate actions:
Healthcare providers: Use human-centered design methods, gather structured patient feedback, and conduct iterative testing of communication materials.
9
Healthcare organizations: Create systems that integrate patient input into educational resources and care processes. Patients and families: Advocate for clear communication during consultations by asking questions, requesting clarification, and sharing your concerns and needs. Policymakers: Establish health literacy and effective communication as fundamental standards of healthcare quality. Implement evidence-based policies that support these standards.
Through these collective actions, we can build a healthcare system where every patient understands and engages with their care. Effective healthcare communication not only saves lives but transforms the healthcare experience for patients, families, and providers alike. The time for transformation is now.
Footnotes
Acknowledgments
The author would like to express sincere gratitude to Dr Keerthi Gogineni of Emory University School of Medicine for her invaluable contributions to the IRB-approved study mentioned in this article. Her expertise and insights were essential to the successful execution of the research.
Consent to Participate
Informed consent was obtained from all participants prior to their involvement in the research.
Declaration of Conflicting Interest
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Considerations
The study mentioned in this article was conducted in accordance with ethical guidelines and received approval from the Institutional Review Board (IRB) at Emory University School of Medicine.
Funding
The author disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research was supported by a Genentech grant titled CGN 2020: Teaching Cultural Empathy to Reduce Bias in Cancer Care (Request ID: G-89093) in collaboration with Emory University School of Medicine.
