Abstract
Developing patient clinical assessments has evolved historically. It is an important skillset for all health care professionals to address the most appropriate treatment options for patients while collaborating with the interdisciplinary team. Implementing pharmacy and medical student collaborations can help pave the way in assessing patients in hospital and ambulatory care settings. Medical students’ proper diagnosis and pharmacy students’ medical recommendations can potentially reduce medical errors. Ultimately, interdisciplinary collaboration enhances clinical assessments, promotes evidence-based medicine, optimizes treatment regimens and monitoring, and improves overall health-related outcomes.
Actionable Insights
Historically, crucial developments over the past centuries have shaped physical and clinical diagnosis to adequately manage and treat patients. Similarly, interprofessionalism interactions among pharmacy and medical students has evolved patient care by offering various perspectives and promoting an exchange of expertise. 1 Hippocrates and his colleagues established medicine as a profession and confirmed that it has a rational basis. 2 After making appropriate diagnoses, primary literature and clinical guidelines are used to provide optimal treatment for patients. To ensure patients receive the most appropriate medical treatment, an assessment should be made collaboratively as it has been shown to improve patient outcomes and reduce hospitalizations.3,4 For example, throughout the patient's hospital course, both the medical and pharmacy student monitor the patient based on their scope. Once the patient is ready for discharge, pharmacy students can provide the patient with counseling regarding all medications and acknowledge the patient's understanding. This intervention can prevent rehospitalizations caused by nonadherence.
Patient clinical assessment in medicine is defined as an appraisal or evaluation of a patient's condition by a physician, nurse, or other healthcare provider, based on clinical and laboratory data, medical history, and the patient's presentation of symptoms. 5 It involves collecting, retrieving, evaluating, and interpreting data from multiple sources. 5 Advanced skills of assessment include an interpretation of findings within each clinical presentation. According to Gawlik et al, to effectively implement advanced assessment skills in clinical practice involves a complex series of steps; a foundation of knowledge; an ability to appreciate the information shared by an individual, patient, or family; and clinical interpretation of the assessments of health and well-being. 6 Particularly in medicine, this skill set is imperative to make decisions and treatment recommendations ultimately derived from these clinical assessments for each individual patient.
Practical Recommendations
Patient care treatment plans are developed by a collaborative healthcare team of expertise and can only be executed effectively with all disciplines involved. While incorporating a pharmacist within each interdisciplinary team is part of the Joint Commission Standards for improving safety and providing quality care in hospitals, this can also be implemented to students in training. Both medical and pharmacy students undergo rigorous didactic curriculums, medical students are primarily focused on identifying the body's structures, functions, and diseases while pharmacy students are focused on diseases and medications. For example during experiential rotations, first the medical students present to the team subjective and objective information as they interview and diagnose the patient. Second, pharmacy students can work with the medical students to evaluate the current pharmacotherapy regimens based on the medical student's assessment. Third, pharmacy students can contribute by dissecting each diagnosis and tailoring medications appropriately by addressing the patients’ needs and improving overall outcomes. 7 Lastly, together they can assist in documenting the patients’ progress of their current treatment regimens and provide the team with clinically valid recommendations after obtaining subjective and objective information from their clinical assessments.
It is essential to collaborate with clinical rotation students in each respected field to provide sound clinical assessments. Often, healthcare students-in-training may assume patients are on the most appropriate medications. Patient's diagnosis, pathology and physiology changes occur, new medications are FDA approved, and guidelines are constantly changing. Additionally, allergies, fluctuations in renal function, adverse drug related events, adherence to regimens, and lack of control of certain conditions can also contribute to changes in medications. Institutions have different policies or barriers for healthcare management that can dictate feasibility and cost for patients. All these potentially play a role in adjusting regimens/plans for patients that both medical and pharmacy students can implement collectively.
To prepare future clinicians, instilling curiosity and confidence will help them question and essentially assess each one of their patients to ensure they are on the more up-to-date regimens. This should address any issues with transitions of care, lost in follow-up, or any gaps in health care. To deliver the utmost quality of healthcare and ensure the best patient outcomes, evidence-based medicine has been introduced to healthcare professional students for years to debunk and decrease clinician culture at certain institutions, leading to sound, up-to-date clinical assessments that redirect our patients to the path of recovery. 6
Each healthcare professional program incorporates various methods to help students prepare valid assessments for their patients. In a systemic review by Elendu et al, found that simulation has a positive effect on the development of clinical decision making, clinical outcomes, increased patient safety, enhanced communication and teamwork abilities. 8 In addition to simulation, clinical rotations also provide students with more practice and opportunities to collaborate. For example, 4th-year pharmacy students at my internal medicine rotation can provide medical students with valuable input regarding medications such as side effects, contraindications, alternatives due to an allergy, and renal dosing. While more research is required to assess other techniques within each curriculum and their respected outcomes, it is not a surprise that practice makes perfect.
Patient clinical assessments require diligent attention and detail and may not always have a clear-cut outcome. It is up to each practitioner to use their clinical knowledge, area of expertise, and research literature to develop a final recommendation. For example, while medical students are interviewing patients to develop their diagnosis, pharmacy students can assess patients’ charts to ensure medications are ordered appropriately and administered in a timely manner. Risk versus benefit discussions may need to take place, and other specialties may also be involved, ultimately to ensure the patient receives the best care. In geriatrics specifically, anticoagulation is a common discussion regarding risk of falls and bleeding versus benefit of stroke prevention. Additionally, families and support systems are involved in these discussions to make appropriate, robust recommendations that satisfy the patient and their loved ones.
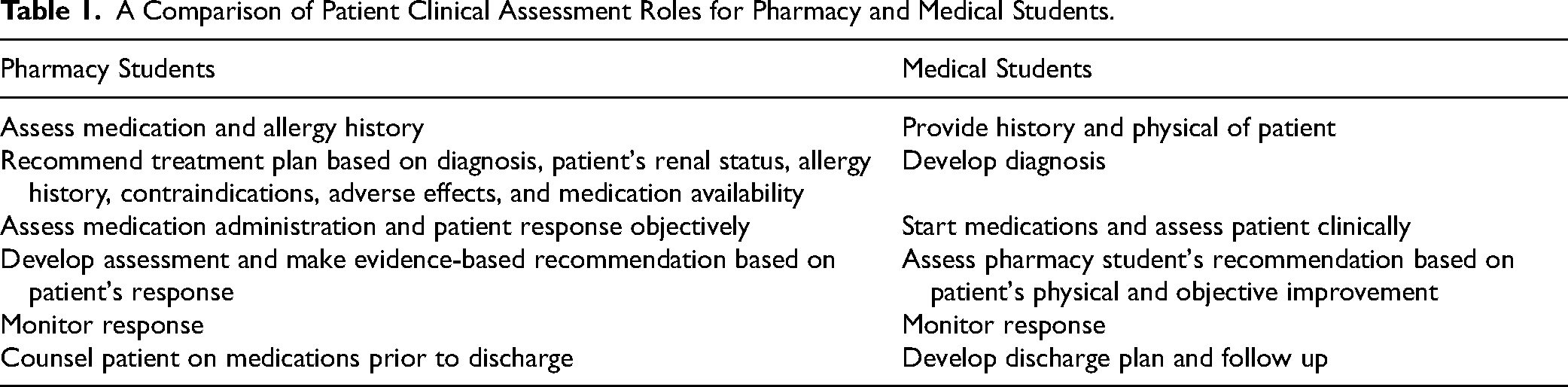
Finally, valid assessments lead to safe patient outcomes. According to Makary and Daniel, medical errors were the third leading cause of death in 2016. 9 While the cause of medical errors may be multifactorial, inappropriate assessments contribute to a portion of these medical errors. 9 Using the best evidence to make clinical assessments and patient care management has been identified as a significant factor in reducing the number of preventable medical errors and improving population health outcomes. 7 Practitioners can jointly implement individualized checklists while managing patients, giving healthcare students guidance to assess each detail appropriately Table 1.
A Comparison of Patient Clinical Assessment Roles for Pharmacy and Medical Students.
Conclusion
Advancements in developing collaborative clinical assessments are an essential part of patient care management. Key benefits of healthcare providers collaborating within clinical training can optimize treatment plans and provide opportunities for collective efforts, leading to advanced health-related outcomes in the future. Future research may evaluate measurable clinical outcomes that result from these collaborative efforts.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
