Abstract
By listening to the “voice” of patients, Northwell Health, New York's largest healthcare organization, took an evidence-based approach to empowering physicians and advanced care providers. The Relationship Centered Communication course utilizes experiential learning to strengthen patient-centered communication and empathy skills to elicit provider–patient relationships grounded in partnership. This case study highlights (1) The pragmatic cultural journey requiring visionary leadership, strong collaborations, and an evolving educational strategy. (2) Over the course of 6 years, 3300+ providers were educated in this evidence-based communication course. (3) As a result, Northwell's Hospital Consumer Assessment of Healthcare Providers and Systems “Communication with Doctors” domain has increased by 22 percentile rank points, when compared nationally to peers, in addition to other notable patient experience metric improvements within ambulatory medical practice.
Introduction to the Issue
At the cornerstone of safety, quality and experience lies the provider–patient relationship. With communication at the core, establishing trust, personalizing interactions, and expressing empathy are factors that can affect patient satisfaction.
1
According to the Institute of Medicine's,
In 2006, the Centers for Medicare and Medicaid (CMS) launched the first national, standardized, publicly reported patient experience survey instrument, Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS). 4 Completed by patients following hospitalization, the 29-item survey aims to “produce data on patients’ perspectives of care that allow for objective and meaningful comparisons of hospitals on topics that are important to consumers”. 5 Through CMS's Value-Based Purchasing program, hospitals are rewarded and incentivized to provide quality care. Value-Based Purchasing calculations and Medicare's reimbursement modeling are comprised of weighted scores across Safety, Clinical Outcomes, Efficiency and Cost Reduction, and Person and Community Engagement measures. 6
There are 3 HCAHPS questions specific to physician–patient communication. Under the “Communication with Doctors” domain, patients rate the frequency of how often their doctor treated them with respect, listened carefully, and explained in a way they could understand. Numerous studies have shown a direct correlation between physician communication skills training and patient experience. 7–9 This case report describes the evidence-based, pragmatic approach a large healthcare organization has taken to infuse communication skills education and its impact on patient experience.
Description of the Intervention
Northwell Health is the largest healthcare system in New York State. Recognizing that resistance to change can occur due to lack of ownership, leadership, organizational complexity, and external influences, 10 a multifaceted framework and systems-based approach has been successfully implemented and sustained. In 2014, Northwell welcomed its inaugural Chief Experience Officer, which sparked the creation of the Office of Patient & Customer Experience (OPCE) team. Leveraging core concepts of Sagie's loose–tight theory of transformational leadership, OPCE interfaces with the organization promoting “a combination of central directive{s} and individual freedom”. 11
In 2015, the system-level HCAHPS “MD Communication” domain Top Box percentage was 78.6, equating to the 29th percentile when compared to peers within the Press Ganey national database. Northwell partnered with the Donald and Barbara Zucker School of Medicine at Hofstra/Northwell and the Academy of Communication in Healthcare (ACH). Aligned with Northwell's mission, these organizations worked collaboratively to create the Relationship-Centered Communication (RCC) curriculum. This immersive program focuses on communication skills, experiential learning, role play, and real-time mentoring.
Selected faculty represent physicians, advanced care providers (ACPs), and a patient experience leader who demonstrate strong communication skills, credibility, and ability to drive patient-centered culture. Diversity of role, specialty, geography, age, and experience was considered. To date, 46 faculty across 4 cohorts have completed ACH's train-the-trainer certification program. Relationship-Centered Communication faculty teach in addition to their leadership/clinical role and do not get compensated monetarily. They feel honored to have been selected and remain committed because they believe in the program and value their role as educator.
Relationship-Centered Communication classes comprise of small groups of interdisciplinary providers—attending physicians, residents, and ACPs. Curriculum is structured around communication and empathy microskills, utilizing the 3 Function Approach to the medical interview: (1) Build the Relationship, (2) Assess and Understand, and (3) Collaborative Management. 12 Faculty present evidence-based didactics, perform a live demonstration of a provider–patient scenario, and facilitate a group debrief. The curriculum was developed to strengthen communication skills that elicit dialogue and open conversation between providers and patients/family caregivers as opposed to closed-ended, monologue-type encounters. By extending this sentiment of communication “with” patients instead of “to,” the goal was to create a partnership relationship. A majority of the course is spent in breakout groups where skills-based practice and subsequent coaching from faculty and peers take place.
Large-scale implementation and cascade began by actively engaging and piloting the course with service line Chairs and Medical Directors so they can experience the course firsthand. The OPCE worked with the Northwell Office of Continuing Medical Education to designate RCC for Maintenance of Certification points, Continuing Education Units, and Continuing Medical Education. Participation in the course has always been voluntary and nonpunitive. Providers attend because they and their leaders view the RCC course as valued investment for professional development.
In March 2020, the COVID-19 pandemic brought to light the power of human connections, making the RCC teachings more prevalent. Considering social distancing restrictions the curriculum was revised for a virtual modality. Comprised virtually of 3-hours via Zoom, emphasis remained on skills and role-play opportunities while incorporating newly developed telehealth scenarios. A select group of existing faculty completed ACH training to prepare them to facilitate within the virtual learning environment. Virtual RCC courses were held regularly between September 2020 and December 2022. Beginning in January 2023, in-person RCC courses resumed due to impact and efficacy.
Evidence of Impact
Since launching in June 2017 to June 2023, 3300+ Northwell providers have taken the RCC course. Approximately 65% of participants attended an in-person course, while 35% attended a virtual session. Postcourse evaluations reflect 90% of attendees would recommend RCC to colleagues. Qualitative feedback remains positive. Provider attendee's agreement with the sentiment that learning the content will positively impact their professional life averages 95%. One participant remarked, “
Examining HCAHPS performance between June 2017 and June 2023, Northwell's overall system “Doctor Communication” domain has steadily improved from the 36th percentile to the 58th percentile, a 22-point increase in rank, as compared nationally to peers within the Press Ganey database. Individual domain questions also improved, with 21-percentile points for “Explain,” 24-percentile points for “Listen,” and 17-percentile points for “Courtesy/ Respect”; see Figure 1 for rank improvement details. Also, within this time frame, Northwell saw a 22-percentile rank point increase for the loyalty, overall inpatient measure “Likelihood to Recommend,” improving from the 42nd percentile to the 64th percentile.
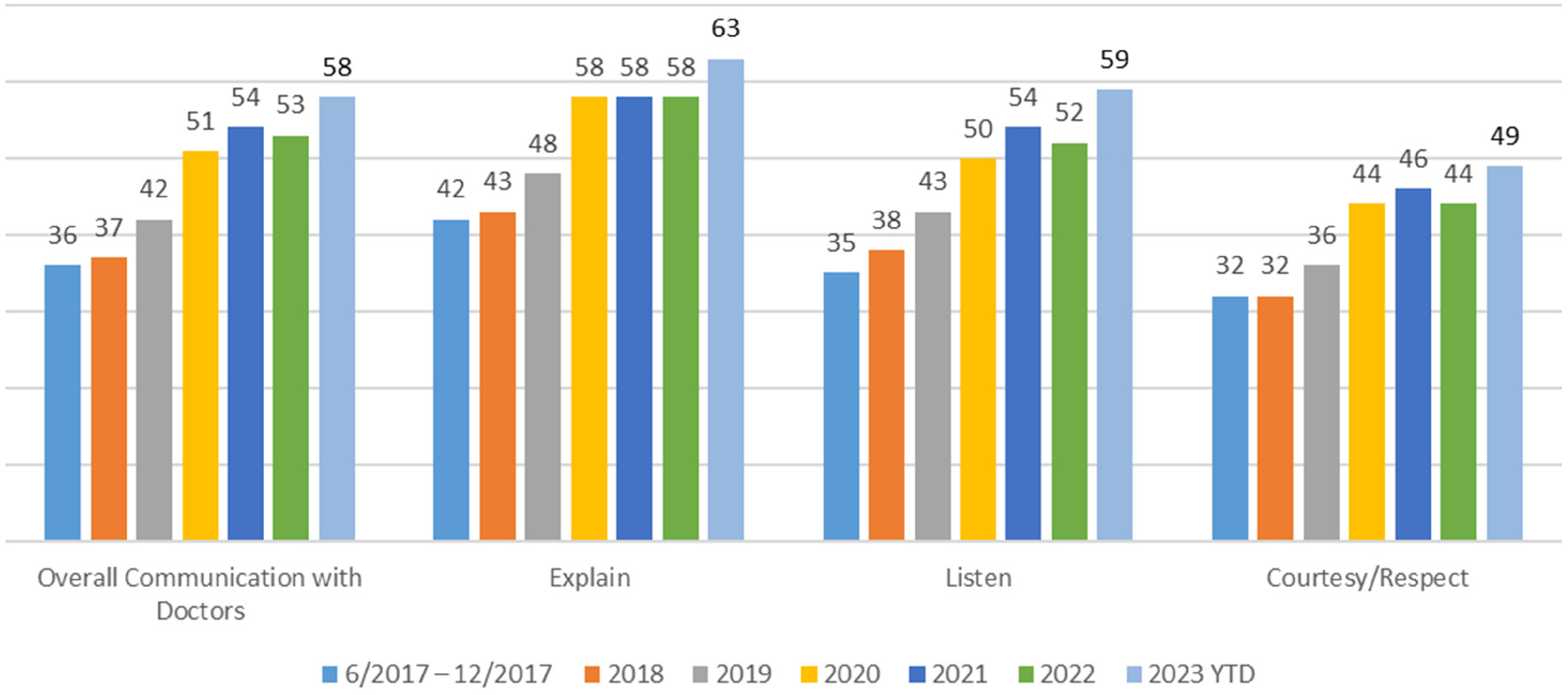
Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) Inpatient MD Communication Rank Improvement.
Further analysis at individual hospitals shows marked improvement. Prior to RCC implementation, 4 Northwell adult hospitals (26.6%) ranked at or above the 50th percentile for the HCAHPS “Communication with Doctors” domain. As of August 2023, that measure has increased to 8 hospitals (53%). On the Northwell Medical Practice patient experience survey, the “Likelihood to Recommend the Care Provider” domain increased 18-percentile rank points, placing the organization at the 84th percentile nationally. Specifically, there has been a 19-percentile point increase for “Address Concerns,” 23-percentile points for “Inclusion in Decision Making,” 17-percentile points for “Condition Explanation,” and “Clear Language” rose 23 percentile points; see Figure 2 for actual rank improvement details.
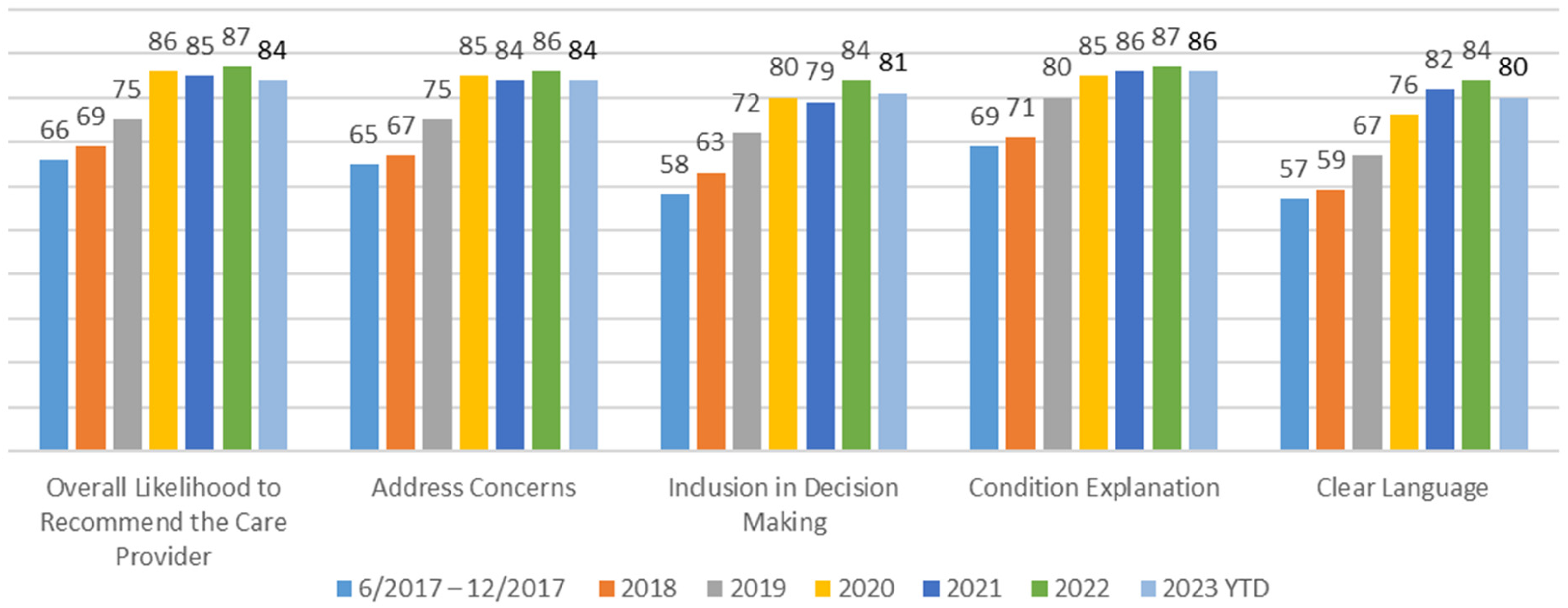
Medical Practice Communication Rank Improvement.
Conclusion
By focusing educational programming on communication and empathy skills, Northwell providers are given tools to enhance their relationships and rapport with patients. Operationalizing RCC required leadership who value the investment of professional development. Seeking partnerships that align to a core mission and vision helped create a curriculum that continues to feel authentic to Northwell,while introducing industry best practices. A pivotal component to the program's success is the selection and involvement of its faculty. They are role models and advocates of humanistic provider–patient relationships. The faculty's ability to connect the curriculum to real-life scenarios paired with a constructive approach to coaching has created positive and meaningful learning experiences. Investing time in developing faculty, has led to building a sense of community with shared purpose. One faculty member reflected, “
Northwell has been on a cultural transformation focused on elevating the patient and provider experience. Therefore, the OPCE recognizes that although the RCC course is an impactful hallmark program, it may not be the only factor influencing experience outcomes. The organization has made strides in access, care delivery model redesign, provider well-being programming and is currently updating its electronic medical record. The RCC course is a moment of time and skills-based learning requires ongoing attention. As a result, innovative sustainment methodologies have been implemented. One offering, Communities of Learning Practice, revolves around creating site-based communities of providers who regularly come together, review core RCC concepts and openly discuss techniques using relevant and timely patient scenarios.
Investing in communication and empathy underscores the interconnection between provider engagement and patient experience. When voluntary education programs are designed and deployed with leadership, intention, and efficacy, it can result in sustained outcomes. The RCC cultural journey from concept, implementation to sustainment has required dedicated faculty, synergistic and collaborative partnerships, and provider engagement. It necessitates patience as transformation often takes time, persistence, and agility. In reflecting on the past and as healthcare continues to evolve, the RCC program will remain a strategic priority for the organization.
Footnotes
Acknowledgements
The authors acknowledge Michael J. Dowling, Northwell Health's President and CEO for his visionary leadership and steadfast commitment to patient and provider experience. Thank you to the Academy of Communication in Healthcare and the Donald and Barbara Zucker School of Medicine at Hofstra/Northwell for their collaborative and synergistic partnerships. Sincere gratitude to Laura Cooley, Dr. R. Ellen Pearlman and Dr. Cathy Risdon for their unwavering support, guidance, and mentorship throughout this journey.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval is not applicable for this case report.
Statement of Human and Animal Rights
This case report does not contain any human or animal subjects.
Statement of Informed Consent
There are no human subjects in this article and informed consent is not applicable.
