Abstract
Background:
In 2014, Dudley Group of Hospitals (DGH) underwent an organizational change that necessitated closure of their Home Parenteral Nutrition (HPN) service. University Hospitals Birmingham NHS Foundation Trust (UHBFT) transitioned 50 patients from DGH into their HPN service. The transition model included communication with patients, communication between centers (development of an HPN Patient Passport), and rapid follow-up on transition ensuring clinical care continued uninterrupted.
Aim:
Evaluate patient experience and their level of satisfaction with our HPN transition model.
Method:
A 19-point, mixed mode paper-based questionnaire was developed. Questionnaires were posted to 42 surviving patients still receiving HPN.
Results:
Response rate: 67%. Communication with patients: The transition was discussed with them, and they had appropriate contact details during the process—94%. Patients informed of patient transition meetings—97%. Attendance at meetings: DGH 89%, UHBFT 55%. Ongoing care at UHBFT: 86% very satisfied and 11% satisfied. Overall rating of the transition process: 79% very satisfied and 14% satisfied. Friends and Family Test: 82% “extremely likely” and 18% “likely” to recommend our services.
Conclusion:
The transition model used was successful, with the majority of patients “very satisfied” with how the transition was managed and their ongoing care. Effective communication with patients and between the 2 centers was the key to success. To our knowledge, this is the first report of transition of care for HPN patients. It is proposed that this model may be used by other centers to plan for future HPN service transitions where necessary.
Keywords
Introduction
Parenteral nutrition (PN) refers to giving nutrition directly into the blood stream rather than via the digestive tract. In most cases, this will be achieved by inserting a central venous catheter into one of the large blood vessels in the chest.(1) There are significant risks associated with the use of PN including septicemia, hyperglycemia, blood electrolyte imbalances, and risks associated with inserting the central venous catheter itself.1 Thus, this type of nutrition is usually reserved for patients who have intestinal failure, where the digestive tract is either diseased or damaged to the extent that it cannot absorb nutrients and/or fluids adequately.(1) Parenteral nutrition is usually required short term and usually only during a hospital admission. However, for a small number of people where intestinal failure is likely to be prolonged, or indeed lifelong, PN is required to be given at home.
Home Parenteral Nutrition
Home parenteral nutrition (HPN) refers to the provision of parenteral nutrition in the patient’s home or primary care setting. Although HPN is still a relatively rare mode of nutritional support, the number of patients receiving HPN has increased significantly in Britain. The British Artificial Nutrition Survey (2) reports a prevalence of HPN of 1360 patients in 2015 compared to just 743 registered patients in 2011 (21.1 per million population). Short bowel syndrome remains the most common indication for establishing HPN (34% of new cases in 2015). Cancer and Crohn's disease were the leading diagnoses in adult HPN patients. Patients receiving HPN often report a reduced health-related quality of life compared to non-HPN patients with chronic conditions (3,4).
In 2008, the Home Intestinal Failure Network set out proposals for the management of this complex group of patients (5). In 2012, centers specializing in HPN in England underwent peer review followed by a tendering process in 2014; neither process reached culmination. Nevertheless, the tendering process helped to ensure that all HPN centers had the same organizational structure and ability to support the needs of this complex group of patients and to manage a high-risk therapy. This process is currently being repeated by NHS England.
On occasions there may be instances where existing specialized units are no longer able to continue to provide HPN services. In such cases, it is essential that the transfer of patient care is managed systematically and with due diligence. An efficient process ensures that the transition of this group of patients is carried out smoothly. This article describes our model of care and patients’ assessment of the transition process used when HPN services at a regional center were closed.
Background
The Dudley Group of Hospitals (DGH) NHS Foundation Trust had been delivering tertiary HPN services since 1987, supporting up to 65 patients annually at its peak in 2012 to 2013 with an increasing turnover. In 2014, DGH underwent an organizational change that led to the closure of their HPN service. This necessitated relocation of their HPN patients to another center. University Hospitals Birmingham NHS Foundation Trust (UHBFT) agreed to take over the care of these patients. The transition process began in the autumn of 2014, culminating in 50 patients being fully transitioned to UHBFT by February 2015.
Developing the Transition Model
There is published data on the transition of patient care from secondary to primary care (6) and important guidelines on the transition of care from child to adult services (7). However, to our knowledge, this is the only published data on transition of adult HPN services between 2 specialist centers.
Despite the lack of previously published data, there are common features related to the process of transitioning any level of care including planning, timely communication and information sharing, patient/carer education, and prompt follow-up (8,9). Our transition model was based on these 4 principles.
HPN Transition Model
Planning
The planning process between DGH and UHBFT began immediately following the decision to transfer care. The development of an “HPN Patient Passport” ensured timely and accurate transfer of essential patient information between the centers.
Timely Communication
A letter was sent to patients detailing the organizational changes, and where achievable with regard to care schedule, discussed in the patient’s next outpatient appointment. University Hospitals Birmingham NHS Foundation Trust developed a welcome pack for patients which included an introduction to the Nutrition Support Team (NST) and key contact details.
Patient education
Shortly following the letter to patients, structured patient information meetings were held at both centers to allow patients to discuss their concerns, ask questions, and ensure they had accurate information regarding the transition process. There was representation from a patient support group, Patients on Intravenous and Naso-gastric Nutrition Treatment (PINNT), at the initial DGH meetings to allow patients to seek independent advice. The UHBFT meetings included guided tours of the key outpatient areas and HPN ward.
Prompt follow-up
Patients were seen at UHBFT within 3 months of their last appointment at DGH. This ensured that their clinical care continued uninterrupted.
As the receiving center in the patients’ journey, it was essential for UHBFT to assess patient experience of the transition and their satisfaction with their ongoing care. Approximately a year after the transition process was complete, a questionnaire was developed to explore the process from the patients’ perspective. Approval was gained from the Trusts Clinical Governance and Audit department and registered as a service improvement initiative.
Aim
With this audit, we aimed to evaluate patient experience, their level of satisfaction with the transition model, and the subsequent provision of care at UHBFT.
Method
Pretransition: HPN Patient Passport
The HPN patient passport was developed by the NST at DGH to facilitate sharing of information. Having extensive experience of caring for HPN patients, the team identified information that they deemed immediately essential to allow ongoing HPN care and safe management. The passport summarized key details for each patient as follows:
HPN provider details
PN prescription
Current medication
Relevant medical history
Recent/relevant investigations
Recent/relevant microbiology history
Central venous access device history
Previous clinic letters had been transferred electronically to the UHBFT team, but it was the patient passport that was used as a key reference.
Posttransition: Questionnaire Development
In collaboration with the patient experience team at UHBFT, a 19-point, mixed mode paper-based questionnaire was developed, which included multiple-choice, scalar, and open-ended free text questions. Questions were devised to illicit patient knowledge and attitude toward elements of the transition process and their care. Broad elements for evaluation were identified from the transition model including effectiveness of communication with patients, continuity of care during the transition process, and satisfaction with their ongoing care arrangements. Demographic data were collected including age-group, gender, and ethnicity. In addition, the “Friends and Family Test” was included, as this is a broad measure of patient experience recommended for use across NHS organizations.(10)
Twelve multiple-choice questions were included, 3 of which related to demographic data. The remaining 9 questions related to patients’ knowledge and awareness of the need for the transition of their care, patient information meetings held across both centers, whether they felt they received adequate information, and had adequate opportunity to ask questions. These questions assessed the quality and impact of the information-sharing process that had been utilized during the transition.
In total, 3 scalar questions were included specifically to investigate participant attitude and feelings toward the transition process and their care. A scale of 1 to 10 was used with supporting “smiley face” graphical images to demonstrate that 1 on the scale indicated the least amount of satisfaction and 10 the highest satisfaction. The use of this graphic has been shown to assist participants with lower literacy skills in processing questions (11). In these questions, a score of 5 or above indicated at least an adequate level of satisfaction.
Four questions regarding what was done well or what could have been done better were asked, with blank boxes for free-text answers. Attention was paid to the amount of space provided within the boxes, as it has been suggested that a larger writing space is likely to illicit fuller answers from the participants (12). The questionnaire was not separately validated. It was developed with the patient experience team and was to be used with a specific group of patients only. It was felt that piloting the questionnaire in a different (control) group would not have been a reliable indicator of validity.
Questionnaire Distribution
In June 2016, the questionnaire was posted to 42 surviving patients who had transferred their HPN care from DGH to UHBFT in January/February 2015 and who remained on HPN.
A prepaid, addressed envelope was included to aid with response rates in addition to a covering letter from the consultant gastroenterologist explaining the rationale for the survey. Participants were assured that their responses would remain anonymous with no personal details required on the questionnaire. The aim was to encourage participants to be as honest as possible in their responses. A deadline of approximately 6 weeks was given to return the questionnaire. This time frame made allowances for overlapping holiday periods. Postal reminders were sent to all participants approximately 1 week prior to the deadline date, as it was not possible to identify which individuals had already sent their responses.
Participant Follow-Up
When patients attended for their normal outpatient clinic follow-up appointments in the 2 months after the deadline date, they were asked whether they had completed the questionnaire and encouraged to do so if they had not. Copies of the questionnaire and further prepaid envelopes were available in clinic where patients requested these.
Statistical Analysis
Descriptive analysis was only used in this study including percentages, means, and medians.
Results
Of the 42 patients who were sent questionnaires, 13 were male and 29 female. Indications for HPN included short bowel syndrome (n = 21), high stoma output (n = 4), scleroderma gut (n = 2), gut dysmotility (n = 10), enterocutaneous fistula (n = 2), and radiation enteritis (n = 6). Mean time on HPN was 6.3 years (median: 5 years, range: 2-30 years). Of these, a total of 28 completed questionnaires were received back—giving a response rate exceeding 67%.
Patient Demographic Data
Of the 28 responses, 26 patients completed the demographic data. Table 1 details the breakdown of demographic information including gender, age, and ethnic origin of the respondents.
Respondent Demographic Data.

Friends and Family Test
Of the 28 responses received, 23 (82%) reported they were “extremely likely” to recommend our nutrition services to their friends and family, and 5 (18%) patients reported they were “likely” to.
Organization of the Transition Process
Responses were collated into key themes related to the overall organization of the transition process and communication with patients. Table 2 details the patients’ perspective on team communication with them during the transition period. Almost all patients reported that the need to transfer their care to UHBFT was discussed with them (94%), and most patients attended at least 1 transition meeting, primarily the meetings held at DGH (89%).
Communication during the Transition Process.
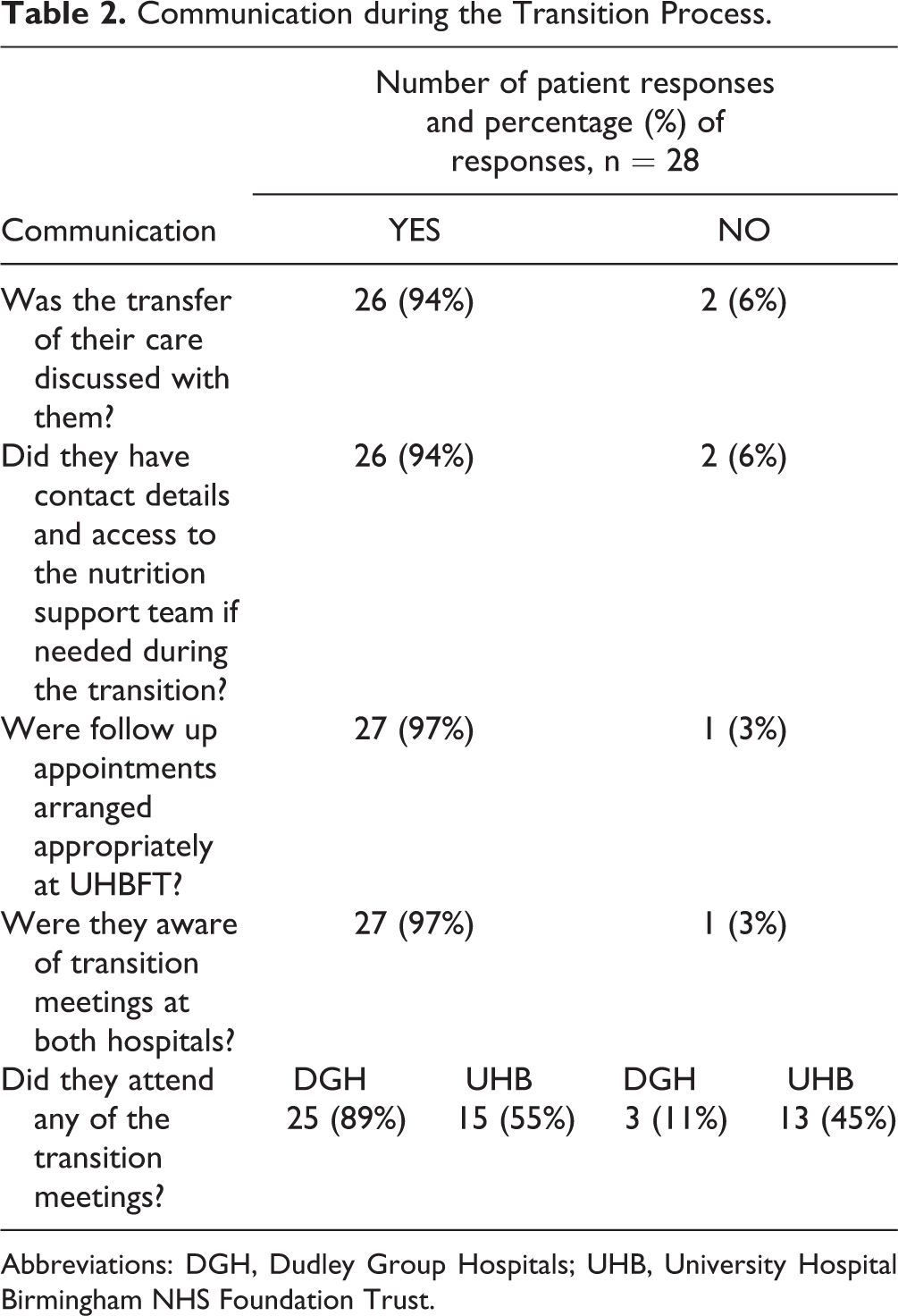
Abbreviations: DGH, Dudley Group Hospitals; UHB, University Hospital Birmingham NHS Foundation Trust.
Free-text responses—What went well?
A common theme was the success of communication with patients regarding the transition process. Free-text comments included: “I was well informed about the transition” “In general it was dealt with really well” “It was fully explained at DGH” “The notice period given before the move and the chance to ask questions”
A further common theme was the patient’s perception of a positive impact on their ongoing care since the transition. Free-text comments included: “For me everything went very smoothly” “Waiting times have improved since the move”
Free-text responses—What could have been done better?
Despite generally positive comments regarding communication with patients, it appears that some patients did not feel that communication had met all of their needs. Free-text comments included “Wider choice of dates and times to meet the team at UHBFT” “More information”
A less common theme appeared in the free-text comments related to the organizational decision-making process, which had led to their existing HPN service being closed. A key comment was:
“Consult with patients before the decision is made”
Effect on Nutritional Care
Responses related to the patients’ perspective regarding the effect of the transition to UHBFT on their nutritional care during the transition and their satisfaction with ongoing care at UHBFT were collated. Elements were grouped according to effect on their journey time, nutritional care during the transition, and their ongoing care.
Journey to UHB
A total of 16 (38%) patients reported that the journey to UHBFT for appointments and admission was easier; 5 (11%) patients reported that it was about the same, and 7 (16%) patients reported that the journey was more difficult.
Effect of transition on nutritional care
Table 3 details the responses to the scalar questions regarding patient satisfaction with their care and the overall transition process. A scale of 1 to 10 was used, with 1 indicating they were unsatisfied (their care had been badly affected) and 10 indicating they were very satisfied (their care was improved). Most patients were “very satisfied” with the 3 aspects detailed.
Patient Satisfaction With Their Nutritional Care.

Discussion
Overall, the experience reported by the patients who responded suggests that the transition model we employed was successful and ensured their care continued uninterrupted during the process. We would suggest that this would be an effective model to employ for future transitions of HPN care. This model is now embedded in our HPN service. However, some patients did express a wish to have more opportunities to visit UHBFT to orientate themselves and meet the team before transfer of care. This is important, as patients who attended the meeting at UHBFT felt reassured having had the opportunity to meet their new teams and familiarize themselves with their new care environment. Therefore, a key element we will change in future transitions of care will be to offer a range of dates for patient meetings.
In terms of service evaluation and patient satisfaction with their ongoing care at UHBFT, the aim was to ensure care was deemed to be at least the same or improved (a score 5-7 or 8-10, respectively). The majority of patients felt very satisfied and that their ongoing care had improved as a result of the transition. In the NHS friends and family test, 82% of respondents indicated that they were “extremely likely” to recommend our services with the other 18% being “likely” to. A key strength of the study was the anonymity of patients, affording confidence that respondents had felt able to be completely honest. However, a weakness of the study is that it was carried out a year after the transition of care when any initial concerns were likely to have resolved.
Communication with patients was key, and the success of the transition process was driven by the referring teams at DGH in ensuring excellent liaison with patients at the outset. Written information from DGH followed by a number of patient forum meetings were essential in ensuring patients were well informed and had opportunities to ask questions and raise any concerns. The presence of the patient support group, PINNT, at the DGH meetings provided an important independent source of reassurance for patients. Fewer patients were able to attend the patient meeting at UHBFT due to us offering only 1 meeting date.
Response to the Questionnaire
The response rate to the questionnaire was very good at 67%. Response rates to questionnaires are influenced by the method of delivery of the survey (13), for example, paper based versus web based. In our survey, questionnaires were sent in the post for self-administration by the participants. This method had disadvantages, as it placed several burdens on the participant: ability to read and comprehend the question, recall the information, and relate this to the question and finally to communicate this in their response (14). To reduce the burden of returning the completed questionnaire, a prepaid envelope was provided. In the planning phase, a web-based questionnaire was considered, given several advantages such as ease of data analysis and helpful features such as informative “pop ups” (13). Studies have revealed that response rates for web-based questionnaires are generally lower than postal questionnaires (13). This may be attributed to several factors, including a lack of computer literacy or Internet access among participants. Balancing the benefits and drawbacks of methods, postal delivery was chosen. Again we would suggest that paper-based/postal questionnaires continue to be considered according to patient needs, despite the current drive toward the use of digital media.
Information Sharing: HPN Patient Passport
The use of web-based patient portals is becoming popular in health care and allows computer-literate patients to have easy access to many of their medical records and to share these with other health-care professionals. The advantages of patient portals are that (1) the patient is in greater control of their health-care knowledge and (2) there is the potential for rapid sharing of information electronically allowing person-centered, coordinated care (15). However, there are a number of disadvantages to web-based information that restrict its usefulness in transitioning the care of a cohort of patients. First, some patients will not be computer literate and so will not be signed up to this form of information sharing. Second, not all centers have electronic records that can easily be uploaded to a web-based system. Third, with sharing of all previous medical notes, letters, and results, a receiving center would spend a considerable amount of time identifying the key clinical information that will allow the patients’ care to continue uninterrupted on transition. For this reason, an “HPN patient passport” was developed to ensure rapid sharing of the most important clinical details for each patient. The concept of the “patient passport” is well recognized in various health-care specialties, including asthma management (16), and dementia care (17), as an effective information-sharing method that ensures continuity of care between settings. To our knowledge, this is the first time it has been used for HPN patients. Although it was time consuming for the DGH team to create these for 50 patients, the patient passport ultimately provided an excellent source of information. Patients were reassured that the receiving team had rapid access to the most essential details regarding their history and ongoing needs. Once all patients had been fully transitioned, then the NST-held paper records were moved across to UHBFT to be amalgamated into the patients’ medical notes.
Future Developments
NHS England continues to review the provision of services, and the framework for ongoing care, for patients requiring HPN. In ensuring an optimal standard of care, one underpinning principle is that HPN is only provided by designated centers with an appropriate infrastructure to support complex needs (18). In the future, this principle may lead to the closure of existing HPN centers and the need to transition care in HPN patients to designated centers. Although national guidelines regarding transition of care from child to adult services are helpful in that setting, they do not inform the needs of an existing adult population (7) Information regarding secondary care to primary care transition is useful as a foundation (9) but is not specific to patients with challenging medical management needs such as those seen in intestinal failure. Thus, the results of this questionnaire are important in providing valuable feedback on the transition process of an adult HPN service to another specialist center.
Conclusion
The results from the patient experience data suggest that the transition process initiated, including the use of HPN patient passports, was successful. Although ensuring high standards of care for patients receiving HPN, the new NHS Framework may lead to a reduction in the number of HPN centers in England. If and where centers close and the care of complex HPN patients requires transition, a robust structure to the transition process is needed. Clear and consistent communication with patients and between centers is essential. We propose that our experience sets a clear transition model for use by other centers in the future. Auditing patient experience following transition of care is essential to monitor processes and ensure learning for future practice.
Footnotes
Authors’ Note
Jane Fletcher made substantial contributions to the article in the conception and design of the study, acquisition, and analysis of data and interpretation of data; drafting the article and revising it critically for important intellectual content. Saqib Mumtaz made substantial contributions in the conception and design of the study, acquisition, and analysis of data and interpretation of data. Merceline Dera made substantial contributions in acquisition and analysis of data and interpretation of data. Sheldon Cooper made substantial contributions in the conception and design of the study and revising the article critically for important intellectual content. All authors have approved the final version of the article to be submitted.
Acknowledgments
The Nutrition Support Team at The Dudley Group of Hospitals: Dr Barry Jones, Consultant Gastroenterologist (retired); Penny Deel-Smith, Jane Ratcliffe and Judith Jones, Nutrition Nurse Specialists and Alison Fairhurst, Dietitian. Caroline Wheatley, PINNT representative.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Jane Fletcher–CME McKinley Medical Expert Advisory Board 2016, honorarium received. Sheldon Cooper has received honoraria and participated in advisory boards for Eli Lilley, Honoria from Baxter, and educational sponsorship from Shire and Calea/Fresenius-Kabi.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
