Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.1
Keywords
Primary Objective
Objective MS1.1: Categories of Bone Tumors. Describe examples of bone forming, cartilage forming, and other common bone tumors including the clinicopathologic features, radiological features, treatment, and prognosis of each.
Competency 2: Organ System Pathology; Topic Musculoskeletal System (MS); Learning Goal 1: Bone neoplasia.
Patient Presentation
A 28-year-old female presents to the Department of Otolaryngology with a 2-month history of a rapidly expanding left mandibular mass. In addition, the patient notices that she is not able to feel anything on the left side of her mandible along with loose dentition in the same area. She does not report pain or bleeding in the affected area. She is then referred for an imaging study.
Diagnostic Findings, Part 1
On physical examination, the patient’s vital signs were reported as normal. The mandibular mass measured at least 3 cm in diameter and was associated with prominent selling of the surrounding soft tissue. It was found to be originating from the body of the left mandible and extending anteriorly. There appeared to be mucosal involvement of the mandible. A dentition examination revealed the roots of tooth 17 were loose. A fiberoptic examination was notable for prominent adenoid and lingual tonsillar tissues. The true vocal folds and larynx appeared normal. The rest of the head and neck examination was unremarkable with cranial nerves II through XII intact besides the mental nerve anesthesia. A computed tomography (CT) scan was ordered for further analysis of the mass.
Question and Discussion Points, Part 1
What Is the Differential Diagnosis Based on the History and Physical Examination?
A number of nonneoplastic and neoplastic conditions may present as a mandibular mass. Nonneoplastic conditions, such as a cyst or abscess, tend to be fairly well-defined and usually are associated with a history of tooth cavity invasion or tooth extraction. 2 Benign neoplastic lesions are typically lucent, well-defined, and cystic. The malignant lesions are more often solid, poorly defined, and with infiltrative borders. The additional history of mental nerve anesthesia, as present in this case, strongly suggest a possibility of malignancy since this symptom has been found to be predictive of malignancy. 3 The differential diagnosis of the mandibular mass includes a variety of lesions of odontogenic and nonodontogenic origin. Table 1 displays the possible tumors for a differential diagnosis based on the World Health Organization 2017 classification. 4 -7 In addition, the patient had a history of Goltz-Gorlin syndrome a skeletal deformity disease known to be associated with bone tumors. 8 This is discussed further below.
World Health Organization (WHO) Classification of Odontogenic and Nonodontogenic Tumors.

Diagnostic Findings, Part 2
A CT scan was completed and shown in Figure 1.
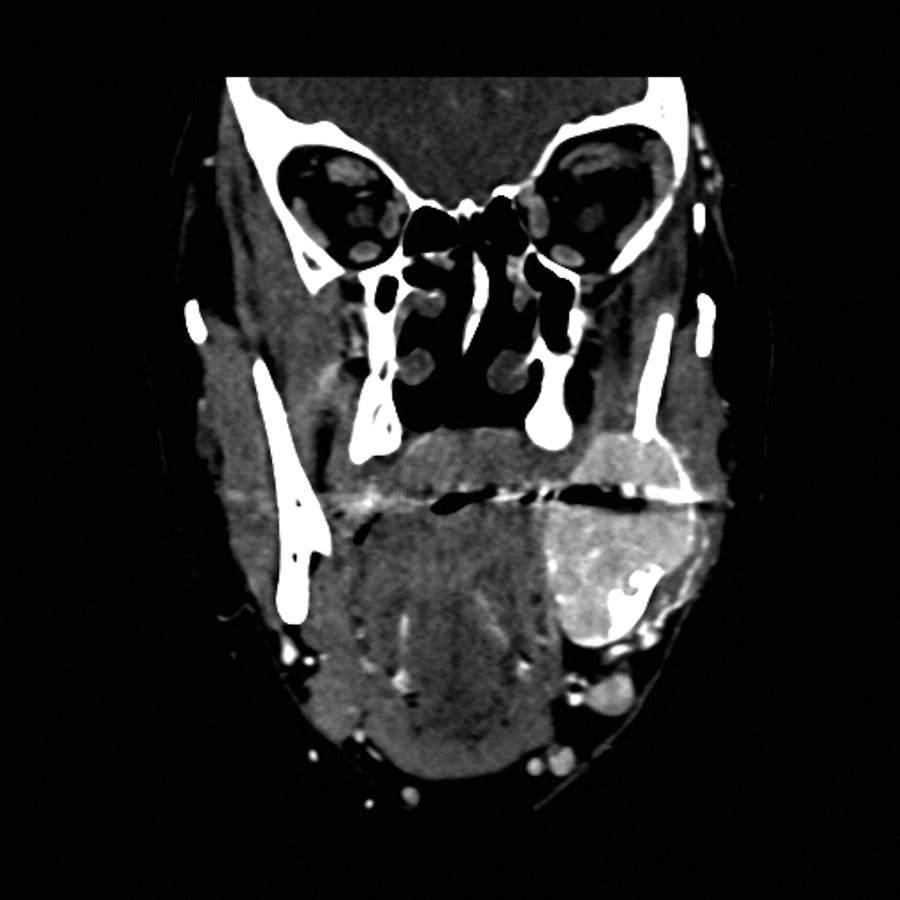
Coronal contrast enhanced computed tomography (CT) image of the face showing solid, enhancing soft tissue mass destroying bone, centered at the angle of the left mandible.
Question and Discussion Points, Part 2
What Are the Findings in the Computed Tomography Scan?
The CT scan showed an aggressive solid, expansile lytic mass at the left mandible involving both the posterior body and ascending ramus and was measured at 4 × 2.9 × 2.4 cm. The lesion involved the inferior alveolar nerve as well as the roots of tooth 17 or 18. The mass also invaded the soft tissues as it involves the left pterygoid muscles medially and the masseter muscle laterally. Several enhancing lymph nodes in the left level 1B measuring 9.5 mm were also noted. This suggested a lymph node pathology that could be benign or indicative of metastases. Both the submandibular and parotid glands were found to be unremarkable. A leftward nasal septal deviation was also found. A CT scan of the pelvis was performed to rule out the presence of other bone lesions. The CT scan showed a lucent lesion in the right iliac.
What Entities Are in the Differential Diagnosis Based on the Above—Radiologic Studies?
Based on the CT results, the differential diagnoses can be narrowed to primary solid tumors with an aggressive, fast paced pattern of growth. 4 -7 A diagnostic biopsy should be performed in order to determine the origin of the tumor.
What Are the Major Categories of Bone Tumors?
The primary bone tumors are classified based on the normal cell types recapitulated or matrix produced. There are 4 major categories of bone tumors: cartilage forming, bone forming, tumors of unknown origin, and notochordal tumors (summarized in Table 2). 7 Cartilage forming tumors are the most prevalent type accounting for approximately 40% of all benign and malignant bone tumors. These tumors are characterized by formation of various types of cartilage; the examples are osteochondroma, the most common benign bone tumor, and its malignant counterpart: chondrosarcoma. Second most common bone tumors are bone-forming (32%). These tumors may produce unmineralized osteoid (osteosarcoma) or mineralized woven bone (osteoid osteoma and osteoblastoma). Other less common types include tumors of unknown origin (19%; eg, giant cell tumor, Ewing sarcoma) and notochordal tumors (5%; chordoma). Overall, benign tumors are more prevalent than malignant tumors and typically occur earlier in a patient’s lifetime, between 1 and 30 years of age. Malignant bone tumors are rare in the United States and account for less than 1% of all bone diseases; however, 50% of cases are lethal. The most common primary malignant bone tumors, osteosarcoma and Ewing sarcoma, occur in childhood. Chondrosarcoma occurs more frequently in older adults. 7
Major Primary Bone Tumors.*
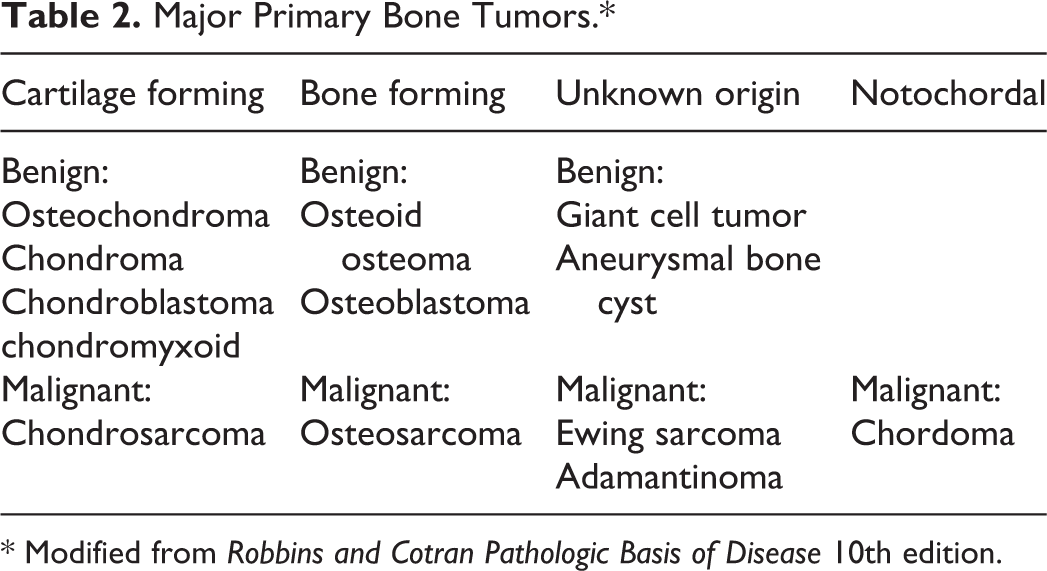
* Modified from Robbins and Cotran Pathologic Basis of Disease 10th edition.
Diagnostic Findings, Part 3
The left mandibular mass was biopsied, and a left molar tooth extracted. The biopsy is shown in Figure 2.
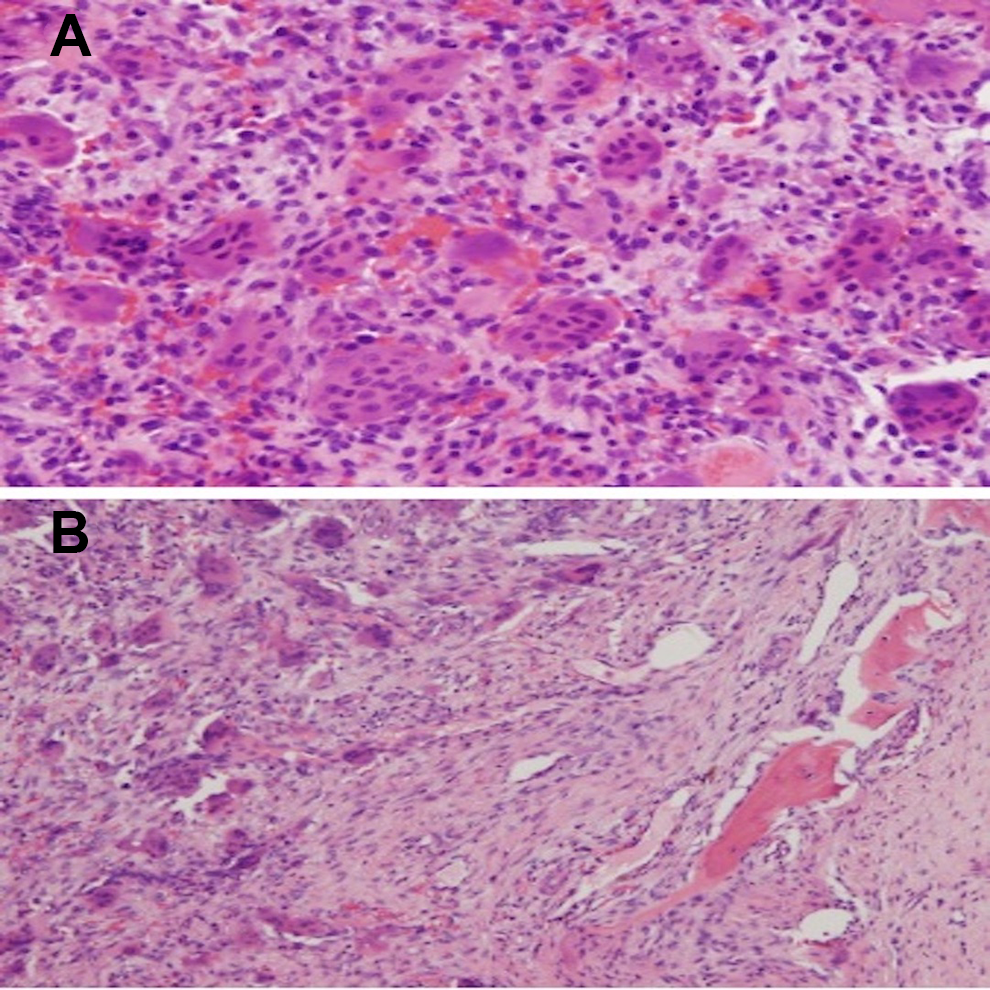
A, Tumor composed of numerous giant cells in a background of mononuclear stromal cells. B, Lower magnification showing fragmented bone adjacent to the tumor. (Hematoxylin and eosin, magnification A: ×200, B: ×100).
Questions and Discussion Points, Part 3
What Are the Histological Findings in Figure 2?
Histologic evaluation of the mass revealed a bone-destroying tumor comprised of multinucleated giant cells that are uniformly distributed among stromal cells (Figure 2). Both populations of cells have similar appearing uniform nuclei. There was no evidence of necrosis or atypia. Mitotic figures were very rare (less than 1/10 high power field). The biopsy of the right iliac bone was performed as well and showed a similar lesion.
Based on histologic findings of multinucleated giant cells, the differential diagnoses can be narrowed to central giant cell granuloma, cherubism, giant cell tumor of bone, brown tumor of hyperparathyroidism, and giant cell reparative granuloma.
What Is the Diagnosis Based on the Clinical and Histopathologic Findings?
The diagnosis of giant cell tumor of bone was supported by the morphologic findings in the biopsies of both the mandible and right iliac bone and were considered to be a manifestation of multifocal disease. Giant cell tumor of the bone is characterized by sheets of uniform oval mononuclear cells interspersed with multinucleated osteoclast-like giant cells in which the nuclei of both populations are similar in appearance. 7
What Are the Usual Differential Diagnoses for Giant Cell Tumor of Bone?
The differential diagnosis of a bone tumor containing giant cells include, both benign and malignant lesions. Benign processes include brown tumor of bone, reparative granuloma, central giant cell granuloma, and Cherubism. Malignant tumors include chondrosarcomas and osteosarcomas as can be seen in Table 2. As this patient did not have a history of hyperparathyroidism, brown tumor of hyperparathyroidism was unlikely. 7 Reparative granulomas have a distinct histological presence with bland fibroblast cells that usually surround hemorrhagic foci, 9 whereas central giant cell granulomas have multinucleated giant cells dispersed throughout the tumor, but concentrate around a hemorrhage area. Cherubism presents with fewer giant cells and has perivascular cuffing by tumor cells, both distinct features from giant cell tumor of bone. 10
Describe the Histological and Radiographical Appearance of Giant Cell Tumors of Bone
The tumor presents on radiographs as lytic lesions that are typically well-defined. They are eccentrically located and usually extend into the subchondral bone. Histologically, giant cell tumor of bone is comprised of multinucleated osteoclast-like giant cells intermixed with mononuclear stromal cells. 7,11
What Is the Epidemiology of Giant Cell Tumors of Bone United States?
Giant cell tumors of the bone (GCTB) compose 3% to 5% of all the primary bone tumors in the United States and account for 15% to 20% of benign bone tumors, although they can have metastatic properties. 12 These tumors are most common in individuals between the ages of 20 and 50 and also appear to have an increased prevalence in women. 7,11
What Is Giant Cell Tumor of the Bone and How Does It Typically Present?
Giant cell tumors of the bone are usually benign, locally aggressive tumors with 75% to 90% of cases occurring in the long bones of individuals. The 3 most common locations for these tumors include the distal femur, proximal tibia, and distal radius. Although these tumors most commonly occur in the appendicular skeleton, up to 15% of cases affect flat bones including the ribs, spine, pelvis, and facial bones. 11,13 In the majority of patients, pain is the most common symptom. 14,15 These tumors are rarely palpable in the appendicular skeleton. 11,13,14,16
These tumors are mostly composed of non-neoplastic osteoclasts and their precursors. The neoblastic cells are suggested to be osteoblastic precursors that express high levels of RANKL. This promotes the proliferation of osteoclasts. Overall, the bone remodeling communication between the osteoblasts and osteoclasts is disrupted in this disease, causing a localized and highly destructive bone matrix resorption through reactive osteoclasts. 7
Resnick et al (2010) has reported on the differences between maxillofacial tumors and axial/appendicular GCTB. The most common place for maxillofacial tumors was found to be the mandible with approximately 77% of tumors presenting there. Patients with maxillofacial tumors tended to be younger upon presentation and were asymptomatic or had painless swelling, whereas the axial/appendicular patients were more likely to present with pain. Also, aggressive maxillofacial tumors were more likely to present in younger individuals. 17
Giant cell tumors of the bone used to be defined through a specific grading scale defined by Campanacci et al (1987). Now, it has been shown that this classification scale has limited clinical value and is no longer used. 14
There is a local benign recurrence rate in approximately 25% of all patients. 13 Approximately 1% to 6% of patients can also experience lung metastases with GCTB although these lesions are benign. Histologically, these metastatic lesions have a similar appearance to that of the primary bone tumor and usually present bilaterally in the peripheral lung. These metastases have a slow progression and are believed to be associated with recurrence rates. Although GCTB tends to be more common in females, lung metastasis does not have a sex-related distribution. Rarely, malignancy occurs with GCTB. 11,13
What Is the Prevalence of Malignant Giant Cell Tumors of Bone and How Are They Categorized?
Malignancy in GCTB occurs in 1.1% to 11.3% of patients. When malignancy does occur with GCTB, it is categorized into primary or secondary malignant GCTB. Primary malignancy is evident upon the diagnosis of GCTB. This type of malignancy is rare, occurring in approximately 1.6% of patients. Histologically, malignancy is characterized by an area of sarcomatous growth with pleomorphic mononuclear cells along with typical appearing GCTB. 13
Secondary malignancy is more common, with an incidence of approximately 2.4% and presents as sarcomatous growth at a previously treated site of GCTB. Approximately 75% of these cases occur several years after radiotherapy. Secondary malignancies can also occur after a surgical treatment without radiotherapy in approximately 25% of cases. 13
Overall, primary malignant GCTB has a better prognosis than secondary malignant GCTB with a 5-year survival rate of 87% in primary malignancy and 32% in secondary malignant GCTB. 13
How Are Giant Cell Tumors of the Bone Treated?
The standard treatment for any GCTB is surgical resection, especially with aggressive tumors, when possible; however, this should be evaluated depending on the location of the tumor to avoid long-term deficits. The treatment of GCTB has evolved over the last several years. Originally, GCTB was treated with surgery and curettage with cement placing; however, the addition of burr drilling and cryoablation with liquid nitrogen has significantly lowered the recurrence rate to 7.9%. Most recently, denosumab, a chemotherapeutic drug has also been used in the treatment of GCTB. Denosumab inhibits osteoclastic activity and causes necrosis of the tumor. It should be noted that this drug is still under investigation. Follow-up imaging is necessary to observe for recurrent tumors. 11,15
If pulmonary metastases occur, they typically have a histologically “benign” appearance. If the lung function is compromised, the metastatic lesions may require surgery. Rarely, the metastatic foci may develop a malignant histology called sarcomatous pulmonary metastases; which is often associated with poor clinical outcome. 11,13
What Is Goltz-Gorlin Syndrome and Does It Play a Role in Giant Cell Tumor of the Bone?
Goltz-Gorlin Syndrome, also known as focal dermal hypoplasia, is suspected to be an X-linked genetic disorder with a dominant inheritance pattern with lethality in males. This is a rare syndrome that has a range of organ involvement and can vary in severity. The organ systems usually affected include the skin lesions, skeletal, and teeth deformities, although ocular anomalies, including a coloboma, can be present in approximately 20% of patients. The majority of skeletal deformities involve the hands and feet. This can include absence or hypoplasia of digits, absence of part of the extremity, ectrodactyly, and many more. Scoliosis can also present in a portion of this population. Facial features can include thin, low set, and protruding ears, a narrow bridge of the nose and a broad nasal tip, as well as asymmetry of the face. Rarely is mental retardation present. 8
Although rare, there have been documented cases of patients with Goltz-Gorlin syndrome developing GCTB. In one previous case study, a patient developed a GCTB tumor in the distal phalanx, a traditionally rare area for these tumors to form. Some investigators suggest that there is a connection between GCTB and this syndrome and that GCTB is part of this disease. 18
What Other Risk Factors Exist?
Patients with Paget disease can also develop GCTB. These tumors differ in presentation compared to those who do not have Paget disease. A recent study, conducted by Divisato et al (2017) reported 75% of all Paget disease GCTB occurred in the axial skeleton such as the mandible, skull, and pelvis. This greatly differs from typical GCTB presence with 15% of tumors occurring in the axial skeleton. Patients with Paget disease also differed in traditional presentation as it typically presents in individuals 40 years of age or older and with a 5-year survival rate less than 50%. This supports a different genetic background of GCTB specifically for Paget disease as the tumor presents in such a distinct manner. 19
Teaching Points
Benign primary bone tumors are more prevalent than malignant tumors.
Malignant tumors are rare, but lethal in 50% of cases.
The most common primary malignant bone tumors, osteosarcoma and Ewing sarcoma, occur in childhood.
Cartilage tumors make up the majority of primary bone tumors.
Giant cell tumors of the bone (GCTB) make up approximately 20% of all benign bone tumors most often in the appendicular skeleton.
Giant cell tumors of the bone occurs most often in women between the ages of 20 and 50 years old.
The diagnosis of GCTB needs to be confirmed through a biopsy as many bone tumors are not able to be distinguished from each other through imaging studies.
The recurrence rate of GCTB is approximately 25%.
Primary malignant GCTB is diagnosed upon initial presentation with GCTB.
Secondary malignant GCTB occurs in an area that has already been treated for GCTB, most likely with radiotherapy. This is associated with a poorer prognosis.
Imaging should be continued after treatment for GCTB to monitor for the presence of a reoccurring tumor.
There is a potential association between Goltz-Gorlin syndrome and GCTB.
Paget disease has a distinct clinical presentation of GCTB with most cases occurring in the axial skeleton.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
