Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.
Keywords
Primary Objective
Objective MS1.2: Bone-Forming Sarcomas in Children: Describe the most common benign and malignant bone-forming tumors in children and adolescents in terms of clinical presentation, radiologic findings, histologic features, treatment, and prognosis.
Competency 2: Organ System Pathology; Topic: Musculoskeletal System (MS); Learning Goal 1: Bone Neoplasia.
Secondary Objective
Objective SP1.4: Staging: Describe the information that the pathologist obtains from a resected tissue specimen, how this information is reported, how it is combined with clinical information to stage the tumor, and how staging information is used to guide treatment.
Competency 3: Diagnostic Medicine and Therapeutic Pathology; Topic: Surgical Pathology (SP); Learning Goal 1: Role in Diagnosis.
Patient Presentation
A 14-year-old male patient presents to the emergency department with severe pain in his right knee. The pain has been intermittent for the past 10 weeks, appearing and disappearing sporadically. The discomfort has grown more regular in the last week and is now compounded by marked swelling around the knee. Further interview reveals that the patient plays on a youth soccer team, and his knee feels especially painful during practice. His parents attributed the symptoms to “growing pains,” as the patient’s height and weight have been increasing appropriately for his age, and he has had no known skeletal diseases—nor any serious conditions—prior to onset of the pain.
Diagnostic Findings, Part I
Vital signs are evaluated and found to be normal. No systemic symptoms are noted. Physical examination reveals a large, palpable mass on the anterior aspect of the right proximal tibia. The mass is tender to palpation, but not warm to the touch.
Question/Discussion Points, Part I
Discuss the Differential Based on the Clinical Presentation
The patient’s large and painful tibial mass is nonspecific, and the differential diagnosis remains broad. At one level, we may consider whether this mass is neoplastic or non-neoplastic. If non-neoplastic, diagnoses might include Osgood-Schlatter disease, subacute osteomyelitis, or a reactive soft tissue lesion such as myositis ossificans. If the mass were neoplastic, one would first have to decide whether the neoplasm was benign or malignant and whether it involved the bone, soft tissue, or both.
For a patient of this age, the most likely malignancies of the bone are osteosarcoma and Ewing sarcoma. Chondrosarcoma may be considered alongside the two—though in its most common form, chondrosarcoma typically presents in the axial skeleton of persons above 40 years old. The mass may be a metastatic tumor, secondary to cancer elsewhere in the body, but the patient’s age and lack of prior disease make this unlikely as well.
Osteosarcoma is the most probable among these malignancies, comprising over 50% of malignant bone tumors for patients younger than 20 years. 1 Ewing sarcoma is the second most common primary bone malignancy in this age-group, representing over 30% of bone cancers for children and adolescents. 2 Children are the highest risk group for both sarcomas, though neither sarcoma accounts for more than 3% of overall childhood cancers. 2 Osteosarcoma most commonly occurs in children between 13 and 16 years of age, while peak incidence of Ewing sarcoma occurs between 10 and 15 years of age. 2,3 This age dependency may be related to the adolescent growth spurt, especially as osteosarcoma often manifests near the metaphyseal growth plate. 4 In both cases, males are at higher risk than females, though the reason for this is unknown. 4
Some benign bone tumors are capable of forming palpable masses similar to the one seen in the present patient. These include aneurysmal bone cysts (ABCs) and giant cell tumors. However, as we will see, giant cell tumors are exceedingly rare in children and adolescents.
Taking these considerations into account, the differential diagnosis includes Osgood-Schlatter, subacute osteomyelitis, myositis ossificans, osteosarcoma, Ewing sarcoma, chondrosarcoma, metastatic tumor, giant cell tumor, and ABC. At this stage, the differential is based solely on the clinical presentation. The patient’s age, his large tibial mass, and his male sex have been particularly informative. A simple radiograph of the area surrounding the palpable mass, in addition to histologic data, will be important for narrowing the differential diagnosis.
Diagnostic Findings, Part II
The Patient’s Radiograph Is Shown in Figure 1. Describe the Findings
Figure 1 shows a simple radiograph of the right distal femur, proximal tibia, and proximal fibula. There is an ill-defined mass in the tibial metaphyseal region expanding into the surrounding soft tissue, with “fluffy” calcification. The mass appears to be a neoplasm, as a Codman triangle—a small, triangle-shaped displacement of the periosteum which occurs as a tumor pushes through the bone cortex—can be seen in the medial cortex at the distal edge of the mass. 5 The Codman triangle is identified by a thin layer of ossification beneath a raised edge of periosteum and is indicative of bone tumors such as osteosarcoma and Ewing sarcoma. As such, non-neoplastic disorders can be eliminated from the differential. To further narrow the diagnosis, a deeper understanding of the possible neoplasms—including their radiology, histology, and epidemiology—may be of use.
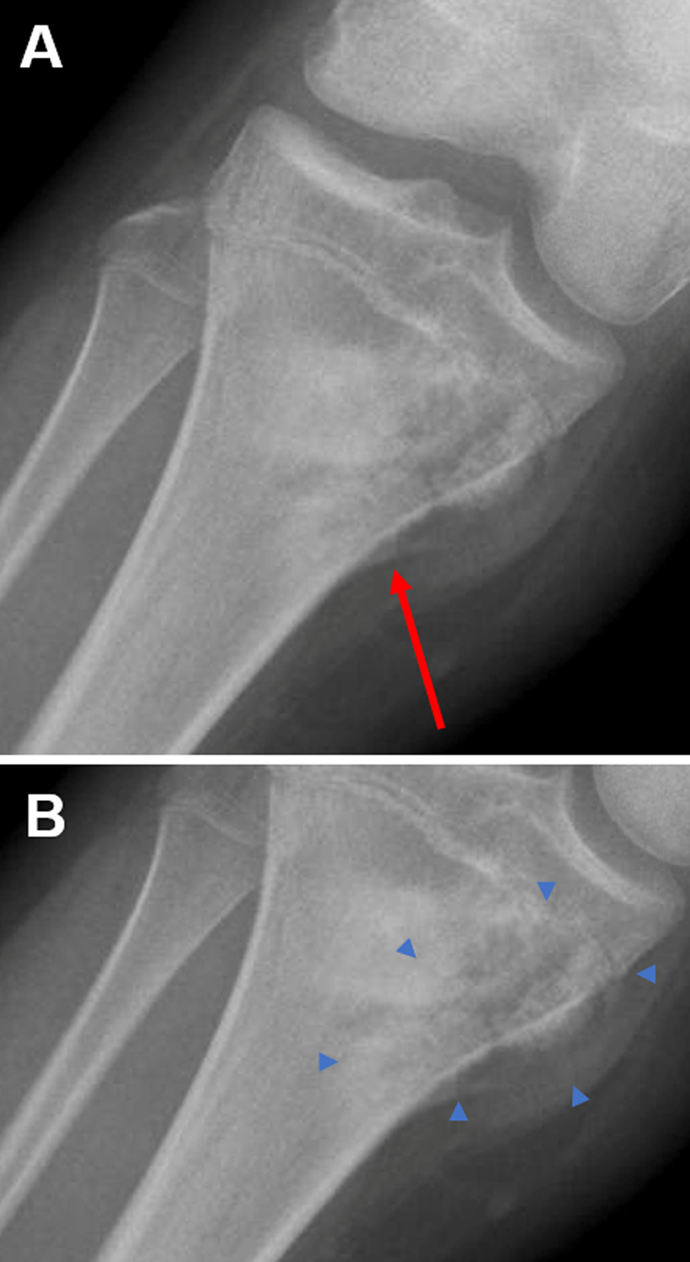
Simple radiograph of the right distal femur, proximal tibia, and proximal fibula. Note the large irregular mass obscuring the proximal tibial metaphysis. Red arrow denotes Codman triangle (A). Blue arrowheads delineate extension of tumor into the surrounding soft tissue (B). The mass is approximately 9 cm at its greatest dimension, according to imaging measurement of a subsequent computed tomography (CT) scan.
Question/Discussion Points, Part II
Describe the Pathological Features, Radiological Characteristics, and Clinical Courses for the Malignant Tumors Under Consideration
At the broadest level, we can delineate between primary and secondary bone tumors. Primary bone tumors originate within bone cells and do not arise from other cancers. Secondary bone tumors arise from cancers elsewhere in the body and typically arise through metastasis. (This is different from the classification for “secondary osteosarcoma,” referenced below.) Depending on the disease and stage, primary malignant bone tumors can have promising outcomes, while secondary bone tumors often carry poor prognoses.
Within the category of primary bone tumors, there exist several malignant and benign variants. Benign tumors are much more common, although malignant bone tumors represent the sixth most common childhood neoplasm and the third most common neoplasm in adolescents and young adults. 6 Approximately 2400 primary bone malignancies are diagnosed in the United States each year. 4
Osteosarcoma is the most common primary bone malignancy in children and adolescents, representing approximately 400 new cases each year in patients younger than 20 years. 2 The malignancy is a bone-forming tumor with several subtypes, most often producing “woven” osteoid tissue in the metaphyseal regions of the distal femur or proximal tibia. 4 Tumors typically present as painful masses, which may grow larger over time. Patients rarely present with systemic symptoms such as fever or weight loss. Radiographs of osteosarcoma may depict the Codman triangle, which forms as pleomorphic osteoid-producing cells expand through the periosteum. 4 The associated soft tissue mass includes regions of both lytic and sclerotic tissue. Histology shows large, pleomorphic tumor cells with hyperchromatic nuclei and haphazard, lacelike patterns of osteoid and mature bone. 4
Although osteosarcoma is technically a primary bone tumor, we can further delineate this malignancy into “primary” and “secondary” categories. Primary osteosarcoma is not directly related to prior diseases or treatments, while secondary osteosarcoma can develop from prior treatments (eg, irradiation, chemotherapy) or skeletal disorders (eg, Paget disease). 2 Regardless of origin, osteosarcomas are often assumed to have subclinically metastasized by the time a patient is diagnosed. 7 Therefore, treatment often progresses in 3 stages: neoadjuvant chemotherapy, surgical tumor resection, followed by additional chemotherapy and/or radiation. Given timely and proper therapy, two-thirds of patients with nonmetastatic primary osteosarcoma will survive long term. 2
Ewing sarcoma is the second most common bone neoplasm in children and adolescents, accounting for over 30% of primary malignant bone tumors in this age-group. 2 About four-fifths of Ewing patients are younger than 20 years, and males are slightly more affected than females. 5
Most often in Ewing sarcoma, primitive round cells develop into large lytic masses, producing tan-white tumors which are often palpable during the physical examination. Nearly 85% of cases involve a balanced translocation, where the EWSR1 gene of chromosome 22 is fused, in-frame, to the FLI1 gene of chromosome 11. 4 Under radiographic imaging, the resultant lytic masses appear as “moth-eaten” lesions of bone and may elicit the Codman triangle. An associated soft tissue mass may also be seen in radiographs of Ewing patients. 8 Periosteal layers may appear in an “onion peel” fashion, as the periosteum degrades into reactive layers. Histologic data typically reveal consistent groupings of small, round cells with low levels of cytoplasm. 4 In 10% to 20% of Ewing cases, patients may also have systemic symptoms such as fever, malaise, and weight loss. 5 Eighty to ninety percent of Ewing patients will relapse if treated solely with local therapy—suggesting, like osteosarcoma, that many have subclinical metastases at the time of diagnosis. 9 For clinically localized Ewing, treatment therefore involves a neoadjuvant chemotherapy, surgical resection, and adjuvant chemotherapy process similar to that osteosarcoma. When this course is followed, 5-year survival rates for Ewing can reach up to 75%. 4
Finally, chondrosarcomas are malignant, cartilage-producing tumors, which can also be delineated into smaller categories. The most common category is conventional chondrosarcoma, which accounts for nearly 90% of all chondrosarcomas. 4 The other 10% is divided between dedifferentiated, clear cell, and mesenchymal chondrosarcoma subtypes. Like Ewing and osteosarcoma, the cartilaginous tumors of conventional chondrosarcoma can permeate the medullary cavity, producing large and painful tumors. However, unlike Ewing and most osteosarcomas (which are bone-forming), the tumor is composed of hyaline cartilage. Upon radiographic imaging, such tumors may resemble bright regions of loosely-clumped, irregular calcification. And again in contrast to the other primary bone malignancies, these are typically diagnosed in persons between 40 and 60 years of age. 4 Furthermore, conventional chondrosarcoma is most often found in the axial skeleton, particularly in the pelvic and shoulder regions. 4
Chondrosarcomas are evaluated by a histologic grading system, which is highly relevant to their pathology and clinical course. This system is organized into 3 categories: grade 1, grade 2, and grade 3. Classifications are made based on the nuclear size, cellularity, mitotic activity, and staining patterns of histological specimens. 4 Grade 1 tumors have low to moderate cellularity; little mitotic activity; and small, round nuclei visible in the chondrocyte cells. 10 These tumors rarely metastasize, with 5-year survival rates near 80%. As a result, treatment may simply involve local resection of the tumor alongside local adjuvant treatment (such as phenolization, cryotherapy, or cementation). 10
On the other end of the spectrum, grade 3 chondrosarcomas are highly cellular, with extreme nuclear pleomorphism and remarkable mitotic activity. In contrast to grade 1 tumors—which contain abundant hyaline cartilage—grade 3 tumors have sparse levels of chondroid matrix. 4,10 The 5-year survival rate for patients with grade 3 chondrosarcoma is only 43%, and surgical resection is rarely sufficient to prevent relapse. 4 Regardless, chondrosarcoma is an unlikely diagnosis given the patient’s age and tumor localization.
Discuss the Benign Tumors Mentioned in the Differential
In theory, both giant cell tumor and ABC could produce a palpable mass like the one seen in this patient. And though the patient is not likely suffering from either form of tumor, the possibility merits consideration.
Giant cell tumors are aggressive collections of multinucleated, osteoclast-like cells. 4 Osteoclasts—which break down and reabsorb bone tissue—are normally quite active and multinucleated. But in giant cell tumors, these cells expand through and degrade the overlying bony cortex, producing a large mass of soft tissue. These osteoclast-like cells can contain over 100 nuclei each and are interwoven with groups of smaller, uniform mononuclear cells. 4 Their resultant tumors are soft and covered by a thin layer of reactive bone, with little bone tissue inside. In simple radiographs, they appear as expansive and lytic masses which are destructive to the bone cortex. These tumors are highly variable in their clinical behavior, though most are found in the distal femur or proximal tibia, and can be resected through curettage. Although the size and location of this patient’s tibial mass correspond to those of giant cell tumors, such tumors are exceedingly rare in children and adolescents. Therefore, the patient is not likely suffering from a giant cell tumor.
Aneurysmal bone cysts most often present in the metaphysis of the long bones in patients younger than 20 years. 4 These tumors are actually blood-filled cystic bodies, surrounded by fibrous walls which contain osteoblasts, osteoclasts, and woven bone tissue. The cysts are expansive and can rapidly degrade bone tissue, while also eliciting painful swelling. Radiographically, they appear as circumscribed “soap bubbles” or “egg shells,” with thin sclerotic rims surrounding the lesion, and fluid levels indicative of blood within the cystic space. Excision or curettage are the most effective treatments, though cysts can still recur afterward. Given this patient’s age, alongside his tumor location and size, one might be inclined toward a diagnosis of ABC. However, the typical ABC—with its “egg shell” appearance and high fluid levels under radiographic imaging—contrasts starkly with the mass seen in Figure 1. As such, the patient is not likely suffering from an ABC, reaffirming the likelihood of a malignant neoplasm.
Might This Patient Have a Secondary (Metastatic) Bone Tumor?
Secondary bone tumors carry very poor prognoses, yet are much more common than primary bone tumors. 4 However, the patient is not likely suffering from a secondary tumor. Firstly, because metastatic bone tumors rarely occur in the tibia—a majority occur in the axial skeleton, especially in the vertebral column. 4 (The patient has no indication of neoplasia in the axial skeleton, though a full-body positron emission tomography [PET] scan would be necessary to rule this out.) Secondly, most secondary bone tumors have metastasized from a few characteristic neoplasms. In adults, these are malignancies of the breast, lungs, thyroid, kidneys, and prostate; in children, they are neuroblastoma, Wilms tumor, and rhabdomyosarcoma. 4 Because the patient has not suffered from any malignancy prior to the clinical presentation, he is very unlikely to have a secondary bone tumor. (It is important to note the difference between secondary bone tumors and secondary osteosarcoma, mentioned above.) Nonetheless, a full-body PET scan could be used to identify possible primary cancers elsewhere in the body.
What Further Testing Is Indicated for This Patient?
Histological data are necessary to form an accurate diagnosis. These data could be acquired through either an open biopsy or a core needle biopsy. A full-body PET scan should also be ordered to rule out metastases and to confirm that the bone tumor is not secondary to another cancer elsewhere in the body.
Diagnostic Findings, Part III
The PET Scan Reveals No Clinical Metastases. A Core Needle Biopsy Is Performed, Yielding the Histological Specimen of Figure 2. Describe the Findings, and How They Influence Your Diagnosis
The histological image shows spindle-like, pleomorphic bone-forming cells, characteristic of a malignant neoplasm. Loosely woven pink osteoid tissue occupies most of the image, suggesting that these are osteoid-producing cells. (One can tell osteoid tissue from normal bone, by identifying the lighter, less-organized immature proteinaceous material.) In the bottom left-hand corner, darker, solid red tissue indicates more mature bone. This can be seen from the apparent mineralization (leading to darker appearance) and characteristic lamellae. Early ossification is occurring in the upper left-hand corner, shown by the moderately darkened and partially mineralized tissue. As a whole, the image shows haphazard arrangements of mature and immature bony material. Clearly, this is a malignant sarcoma which has been producing irregular osteoid tissue. In combination with the radiograph from Figure 1, this is likely an osteosarcoma. Given that this patient has no other clinically notable tumors, the osteosarcoma is a primary neoplasm.
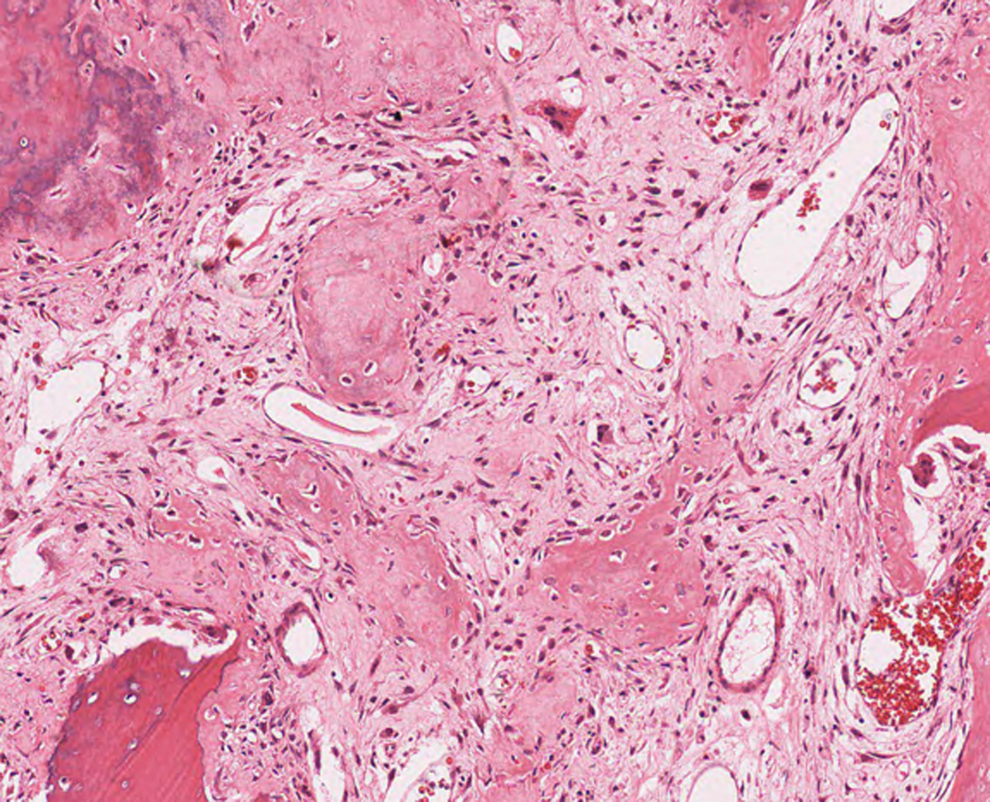
Histological slide from core needle biopsy of the right proximal tibia. Note the woven, haphazard arrangement of osteoid tissue and immature bone. Bottom left-hand corner shows region of darker, matured lamellar bone. Upper left-hand corner shows region of immature, ossifying tissue, more organized than surrounding light-pink osteoid material. Magnification = ×80.
Question/Discussion Points, Part III
What Would You Have Expected to See If This Were an Ewing Sarcoma?
If this patient had Ewing, one would not expect to see pleomorphic cells surrounded by irregular osteoid tissue. Instead, one would expect consistent groupings of small round cells, each about the size of a lymphocyte. 5 These cells would have a very high nucleus to cytoplasm ratio, with minimal sign of stroma, giving a characteristically dark stain to the resulting image. Figure 3 provides an example of this. Additionally, Ewing sarcoma cells are positive for CD99 by immunohistochemical staining, because their cell surfaces contain the CD99 antigen which is bound by the stain.
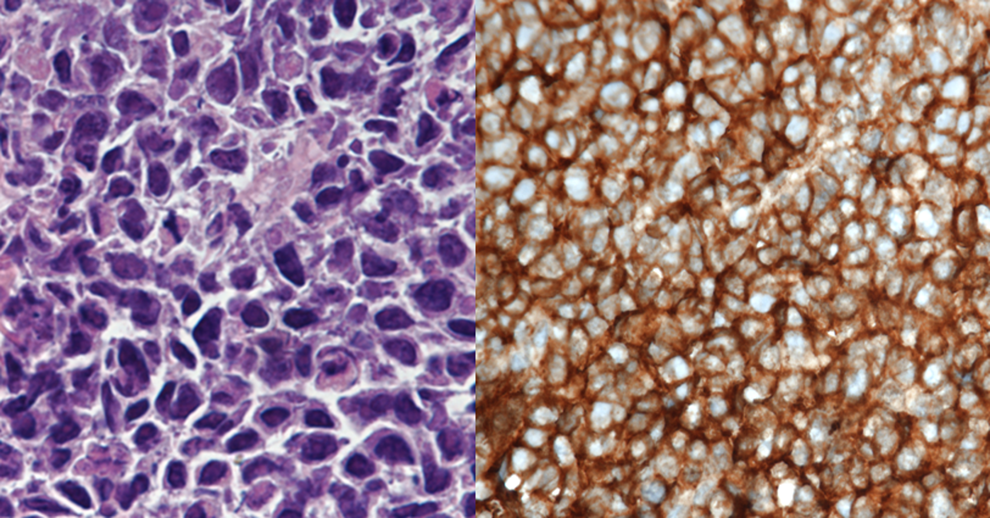
Histological slide typical of Ewing Sarcoma (left) and Ewing Sarcoma under CD99 immunohistochemical staining (right). Note the monotonous presence of immature small round cells, as well as the high nucleus to cytoplasm ratio. Magnifications = ×400.
Even Though Osteosarcoma Is the Most Common Childhood Malignant Bone Neoplasm, It Still Accounts for Just 3% of Childhood Cancers. What Risk Factors Might Have Predisposed This Patient to the Disease?
Before delving into specific risk factors, one might revisit the difference between primary and secondary osteosarcoma. Primary osteosarcoma, like other primary bone tumors, originates in bone cells and is not directly associated with another cancer or disease. Secondary osteosarcoma also originates in bone cells but is associated with either a skeletal disease or treatment from another condition (typically cancer). Perhaps confusingly, both forms are considered “primary bone tumors,” because both arise from bone cells themselves. Nonetheless, primary osteosarcoma is the predominant form in children and adolescents.
Genetic predisposition likely plays a role in childhood primary osteosarcoma. For example, approximately 70% of sporadic osteosarcoma tumors contain acquired mutations in RB, the negative cell cycle regulator. 4 Most commonly, these are loss-of-heterozygosity mutations, though point mutations also contribute. 11 Germline RB mutations also play a role, increasing osteosarcoma risk 1000-fold. 4
Inactivation of TP53, which codes for a protein critical to apoptosis and DNA repair, has also been linked to osteosarcoma. 2, 4, 12 For instance, patients with Li-Fraumeni syndrome (characterized by germ line inactivation of TP53) can suffer from osteosarcoma in addition to a multitude of other cancers. Inactivation of the CDKN2A gene—which codes for p14 and p16, 2 proteins involved in tumor suppression—also increases risk for osteosarcoma. This occurs through 2 respective pathways: those of p53 and Rb, respectively. 11 With the former, p14 functions to inhibit degradation of p53 (the product of TP53) by sequestering the E3 ubiquitin ligase to the nucleolus, thereby preventing ubiquitin tagging of p53. In the latter, p16 acts as negative regulator of CDK4, which typically phosphorylates Rb (the product of RB). When CDK4 does phosphorylate Rb, the cell cycle is allowed to progress from G1 to S phase; inactivation of p16, therefore, keeps this checkpoint constitutively open. 11,12 (It is important to note that loss-of-function mutations in RB, referenced above, can remove this checkpoint entirely.)
Unlike Ewing sarcoma, there is no characteristic translocation—or any canonical genetic mutation—associated with osteosarcoma. 4,11 However, the latter neoplasia has recently been linked to chromosomal instability (CIN), a heterogenous, genome-wide set of chromosomal alterations, which impacts the number of chromosomes or sections within chromosomes. 11 In turn, CIN itself arises from dysfunction in the cell cycle and DNA repair processes, partially explaining the importance of genes such as RB and TP53 in osteosarcoma.
As noted, a host of chromosomal alterations play a role in CIN-related osteosarcoma. For instance, chromosomes 3, 6, 9, 10, 13, 17, and 18 contain common locations for deletion events which impact copy number variation in osteosarcoma cells. 1 These regions are notable for encoding numerous tumor suppressors, explaining why such deletions may increase risk for osteosarcoma. 11,12 On the other hand, chromosomes 1, 6, 7, and 17 contain notable oncogenes and are the most common sites for amplification in osteosarcoma-related copy number alterations. 12 These complex rearrangements have potential for widespread genetic variations, even between osteosarcoma cells. As a result, the genetic etiology of osteosarcoma remains unknown, and the search for targeted molecular treatments remains unsuccessful. 11,12
Prior irradiation—from an earlier primary cancer, for instance—increases risk for secondary osteosarcoma and may be responsible for approximately 3% of osteosarcomas. 2 Exposure to chemotherapy heightens this effect. 2 The incidence of irradiation- and chemotherapy-related secondary osteosarcoma may only increase with time, as survival rates rise for certain childhood cancers.
Because 75% of osteosarcoma cases occur in persons younger than 20 years, much attention is paid to the risk factors for children and adolescents. 4 But in truth, osteosarcoma displays a bimodal age distribution, with older adults comprising a smaller, yet still significant proportion of cases. Interestingly, adult patients are more likely to develop osteosarcoma in the axial skeleton, and patients over 60 years old are at highest risk for metastatic tumors. In contrast to their younger cohorts, these patients often suffer from secondary osteosarcoma, typically associated with Paget disease. Paget, notable for its accelerated and disordered pattern of bone turnover, occurs in 1% of US adults older than 40 years. 4 Just fewer than 1% of Paget patients will undergo sarcomatous transformation of the disease, leading to secondary osteosarcoma. 2 In polyostotic cases of Paget (ie, cases involving multiple bones), this figure increases to 5% to 10%. 4
Now That You Have Diagnosed the Patient With Primary Osteosarcoma, How Do You Stage the Cancer?
Bone sarcoma staging guidelines, set by the American Joint Committee on Cancer (AJCC) and Union for International Cancer Control, operate using the TNM staging system. 2,13 In this system, tumors are evaluated for their size and extent (T), lymph node involvement (N), and metastases (M). There is also a category for histological grade (G). Each category contains a set of grades, depending on the type of tumor (eg, bone sarcomas). For instance, bone sarcomas in the appendicular skeleton have 5 grades for tumor extent: TX (primary tumor not assessable), T0 (no evidence of primary tumor), T1 (tumor ≤8 cm at greatest dimension), T2 (tumor ≤8 cm at greatest dimension), and T3 (discontinuous tumors in the primary bone site). Tumors are also evaluated for their absence (N0) or presence (N1) of regional lymph node metastases, alongside their absence (M0) or presence (M1) of distant metastases. If distant tumors have metastasized to the lung, they are classified at M1a, while metastases to the bone or other distant sites are classified as M1b. Finally, histological specimens are considered well differentiated and low grade (G1), moderately differentiated and high grade (G2), or poorly differentiated and high grade (G3). Finally, the AJCC provides a framework for assigning an overall “stage group” based on these collective classifications. 13
According to imaging analysis, the patient’s tumor is approximately 9 cm at its greatest dimension (Figure 1), making it a T2 bone sarcoma. The full-body PET scan revealed no metastases, qualifying as both N0 and M0. Finally, the histology appears to be moderately differentiated, indicating a G2 grade. Taken together, these classifications place the tumor in the II-A stage group. One should note that the tumor has been staged using “clinical staging” practices, which do not include surgical measurement. A “pathological stage” could be reached by incorporating data from surgical exploration or from removal of the tumor. These pathological data do, at times, alter the conclusions of clinical staging.
The Musculoskeletal Tumor Society (MSTS) provides separate staging guidelines for bone sarcomas. 14 The MSTS guidelines categorize malignant bone tumors by grade: stage I (low grade), stage II (high grade), and stage III (tumors with distant metastases). Within each stage, tumors are characterized as type A tumors (intracompartmental, contained within the bone cortex) and type B (extracompartmental, extending beyond the cortex). The final stage is used for surgical decision-making, with no impact on chemotherapeutic approach.
Given the lack of clinically notable metastases, this tumor is either stage I or stage II. The tumor is large, and histology shows a marked proliferation of osteoid cells, suggesting that this is a high-grade stage II tumor. Furthermore, the tumor has clearly lifted the periosteum (demonstrated by the Codman triangle) and expanded into the surrounding soft tissue. The patient can therefore be diagnosed with a stage II-B primary osteosarcoma when regarding the MSTS guidelines.
Briefly Describe the Therapeutic Approaches for This Patient
As noted, the treatment of primary osteosarcoma typically involves 3 stages: neoadjuvant chemotherapy, surgical resection of the tumor, and adjuvant chemotherapy. In the absence of clinically detected metastases, 5-year survival rates range between 60% and 70%. 2,4 When chemotherapy is excluded, however, up to 80% of patients will develop metastatic tumors (even if the original cancer is locally controlled). 2 This patient should, therefore, follow the standard 3-stage protocol.
There is no consensus on the ideal chemotherapy for bone sarcomas. Nonetheless, the American Osteosarcoma Study Group (AOST) has put forth the MAP regimen, which uses methotrexate, doxorubicin, and cisplatin for both neoadjuvant and adjuvant therapy. 15 In the AOST protocol, the neoadjuvant phase lasts for 10 weeks, surgery is performed in week 11, and adjuvant therapy resumes for weeks 12 through 29. A leucovorin rescue can be used alongside high-dose methotrexate.
Between the neoadjuvant and adjuvant chemotherapy, there are 2 main surgical approaches. The first is amputation of the affected region; the second is limb-sparing resection of the tumor. (With tumors of the metaphyseal region, resection is typically “osteoarticular,” removing the tumor, the tumor-bearing bony portion, and portions of the adjacent joint.) 16 Oncologic outcome is of primary concern when choosing a surgical approach, and functional outcomes are secondary. If complete excision of the tumor is anatomically impossible, or otherwise complicated, amputation remains the “gold standard” to avoid recurrence and metastasis. 16 Nonetheless, the use of limb-sparing resections has increased with the employment of effective chemotherapy. And regardless of approach, the level of chemotherapy-induced tumor necrosis found during surgery is highly relevant to long-term prognosis. 4,16
Given this patient’s age, activity level, and lack of clinical metastases, limb-sparing surgery is preferable to amputation. However, the patient will likely require reconstructive surgery. An allograft or expandable endoprosthesis may be suitable for his immature skeleton, allowing for equal development of his lower limbs.
If initial treatment is deemed successful, the National Comprehensive Cancer Network recommends follow-up surveillance every 3 months for years 1 to 2, every 4 months during year 3, every 6 months for years 4 to 5, and once annually from year 6 onwards. 15 While there is no established time line for the duration of follow-up, most bone sarcoma recurrences occur within 10 years of treatment. 15
Teaching Points
Radiographs of osteosarcoma typically depict a soft tissue mass, including lytic and sclerotic tissue, alongside the notable Codman triangle.
Bone tumors can be classified as primary (originating in the bone itself) or secondary (having metastasized from elsewhere in the body).
Osteosarcoma and Ewing sarcoma are the most common primary malignant bone tumors in children and adolescents.
Osteosarcomas are malignant bone-forming tumors which produce woven osteoid tissue and comprise 50% of all childhood bone neoplasms.
Histology of osteosarcoma shows haphazard arrangements of loosely woven osteoid tissue, surrounded by sections of mature lamellar bone.
While there is no established genetic etiology of osteosarcoma, CIN is common among osteosarcoma cells.
Giant cell tumors are soft, benign collections of multinucleated osteoclast-like cells, which appear near the epiphysis of the long bones.
Aneurysmal bone cysts are benign, blood-filled cystic bodies which typically appear as “egg shell” masses near the metaphysis of the long bones.
Malignant bone tumors are staged after diagnosis and before treatment. The specific stage of any given tumor will influence the prognosis and treatment of that cancer.
In the AJCC guidelines, bone sarcomas are evaluated for tumor extent (T), lymph node involvement (N), distant metastases (M), and histologic grade (G). They are then given an overall “stage group” (stages I-IV, subgroups A-B) based on these evaluations.
In the MSTS guidelines, bone sarcomas are staged by their grade (stages I-III) and whether they are intracompartmental (A) or extracompartmental (B).
Clinical staging of a tumor can be reached through imaging or other nonsurgical measurements, while pathological staging requires surgical exploration or removal of the tumor.
Treatment for osteosarcoma typically involves neoadjuvant chemotherapy, surgical removal of the tumor, and adjuvant chemotherapy.
Chemotherapy of osteosarcoma often follows the MAP regimen—methotrexate, doxorubicin, cisplatin—for both neoadjuvant and adjuvant phases.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
