Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.1
Keywords
Primary Objective
Objective UTK5.3: Immune-Mediated Renal Disease. Compare and contrast the mechanisms of immune complex and antibody-mediated glomerulonephritis.
Competency 2: Organ Systems Pathology; Topic UTK: Kidney; Learning Goal 5: Renal Syndromes.
Patient Presentation
A 28-year-old man presents to the clinic complaining of red urine over the past week. He denies any recent illnesses and has no chronic diseases. He was in the office 2 weeks ago for an annual physical examination, at which time no abnormalities were noted. On review of systems, he admits to coughing up blood once yesterday. He says he has not urinated as much as usual over the past week. He thinks he has passed blood in his urine on 2 separate occasions over the past week. This was not associated with pain, and he denies nocturia. He is on no medications. He smokes 1 pack of cigarettes daily and has done so for the past 8 years. He drinks a 6 pack of 12-ounce beers every weekend. He is not married and lives alone.
Diagnostic Findings, Part 1
On physical examination, his temperature is 98.9°F (37.2°C), pulse is 84/minute, blood pressure (supine) is 160/86 mm Hg, and respiratory rate is 14/minute. His height is 6′1″ (1.85 m), weight is 182 pounds (82.6 kg), and body mass index is 24.0 kg/m2. Physical examination reveals a well-appearing man in no significant distress. Examination of head, eyes, ears, nose, and throat is unremarkable, specifically with no oropharyngeal erythema or tonsillar exudates. Cardiac examination reveals a normal S1 and S2 with no murmurs, gallops, or rubs. Respiratory examination reveals slight crackles, with no wheezes, rhonchi, or evidence of consolidation. Abdominal examination reveals no organomegaly or fluid waves. Examination of the extremities finds mild pitting edema (1+) in bilateral lower extremities. No skin rashes are noted. Neurological examination reveals no significant findings.
Questions/Discussion Points, Part 1
What Is the Differential Diagnosis Based Upon History and Physical Findings?
This patient reports gross hematuria on 2 occasions in the past week, possibly with accompanying decreased urine output, as noted in review of systems. The reported hemoptysis may be related to his urinary symptoms. Physical examination is remarkable for hypertension and edema. The presence of slight crackles and mild lower extremity edema could suggest edema of cardiac origin with poor ventricular function. However, the presence of edema accompanied by hematuria suggests the possibility of a renal origin for the edema.
Broadly, edema can occur due to increased hydrostatic pressure, as in congestive heart failure or constrictive pericarditis. Impaired venous return due to deep venous thrombosis can also lead to increased hydrostatic pressure and edema in a local region. The absence of recent travel and the bilateral nature of this patient’s lower extremity edema make deep venous thrombosis less likely. Any etiology that lowers plasma albumin levels, for example, albuminuria in nephrotic syndrome, proteinuria in nephritic syndrome, or reduced albumin synthesis in decompensated chronic liver disease, can cause generalized edema due to decreased plasma oncotic pressure via hypoproteinemia.
The most important diseases to consider in the differential diagnosis in a previously healthy man with these findings include pulmonary renal syndrome, glomerulopathy, vasculitis (though no rash is noted), and renal or urinary tract tumor.
What Are the Best Next Steps in Diagnostic Evaluation of This Patient?
Review and comparison of any previous laboratory studies to current laboratory studies should confirm the presence of hematuria, determine the presence and extent of proteinuria, evaluate for renal functional impairment, and determine the presence of any specific renal syndromes.
A blood urea nitrogen (BUN) and serum creatinine are indicated, to see whether the patient’s historical and physical findings indicate impaired renal function or reduced glomerular filtration rate (GFR).
Serum electrolytes and a comprehensive metabolic profile will assist in determining the level of renal functional impairment, if present.
A complete urinalysis (including macroscopic, chemical, and microscopic evaluation) will confirm the reported presence of blood in the urine and inform the differential diagnosis, relative to the presence of proteinuria, and other pathologic urine features that might indicate glomerular dysfunction (presence of red blood cell casts, etc). In the absence of significant proteinuria or other indications of renal parenchymal impairment, causes for hematuria within the renal pelvis, ureters, urinary bladder, or urethra should be considered.
A complete blood count may be indicated to determine the extent of blood loss, although his history does not suggest significant renal or pulmonary blood losses.
A chest X-ray may assist in determining whether significant pathologic pulmonary findings are present and further evaluate the reported hemoptysis. It may also help to evaluate for the presence of cardiac abnormalities that could explain the presence of bilateral pitting edema.
If renal parenchymal impairment is suggested and findings point to a glomerular lesion, measurement of serum complement levels (C3 and C4), serum antistreptolysin O antibodies, serum antineutrophil cytoplasmic antibodies (ANCAs), serum antinuclear antibodies (ANAs), and antiglomerular basement membrane (anti-GBM) antibodies may be helpful.
Diagnostic Findings, Part 2
The patient’s laboratory findings from today, including a complete metabolic profile, complete blood count, and urinalysis, are shown in Table 1.
Review of his chart reveals that the patient’s BUN and serum creatinine were 23 mg/dL and 0.9 mg/dL 2 weeks ago at his annual physical examination.
A 24-hour urine collection reveals mild proteinuria: 530 g protein/24 hours (non-nephrotic range).
A chest X-ray reveals no significant acute pulmonary infiltrates and does not reveal cardiomegaly or mass lesions.
Laboratory Findings.
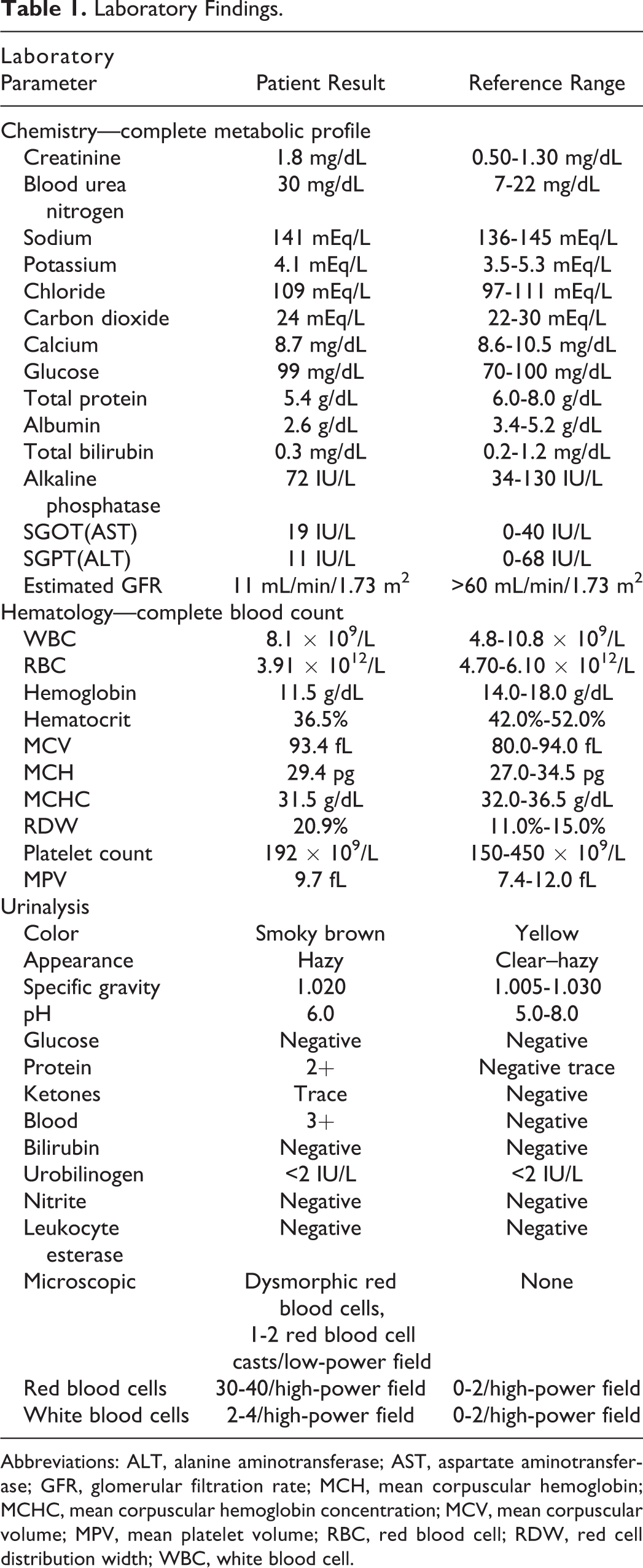

Abbreviations: ALT, alanine aminotransferase; AST, aspartate aminotransferase; GFR, glomerular filtration rate; MCH, mean corpuscular hemoglobin; MCHC, mean corpuscular hemoglobin concentration; MCV, mean corpuscular volume; MPV, mean platelet volume; RBC, red blood cell; RDW, red cell distribution width; WBC, white blood cell.
Questions/Discussion Points, Part 2
Do the Findings in This Patient Support the Presence of a Specific Syndrome?
This patient has impaired renal function that is acute (rise in serum creatinine from 0.9 up to 1.8 mg/dL within 2 weeks), as well as hypertension. On urinalysis, he has proteinuria, hematuria, dysmorphic red blood cells, and red blood cell casts. He reports a decrease in urine output (oliguria). These findings support the presence of nephritic syndrome, which is defined as the presence of a decline in GFR (often manifest as azotemia and oliguria), hematuria, often mild proteinuria, and hypertension. 2 Of note, the presence of dysmorphic red blood cells and red blood cell casts in the urine suggests active glomerular injury, and together, these findings are often referred to as “active urinary sediment.” These findings are typically seen in patients who present with nephritic syndrome. In contrast, patients with nephrotic syndrome usually present with a “bland urinary sediment” that contains lipid droplets, oval fat bodies, and lipid laden casts and is typically acellular. Since the decline in this patient’s renal function has happened over a relatively brief period, he could also be classified as having acute kidney injury.
What Is the Differential Diagnosis Now, Given the Initial Laboratory and Diagnostic Studies?
The differential diagnosis is now narrowed to focus on glomerular lesions that cause nephritic syndrome. In a young man with no significant past medical history (with the exception of smoking), entities such as postinfectious glomerulonephritis and IgA nephropathy should be considered as a cause for acute glomerular injury. Given his relatively acute course, diagnoses under the umbrella of rapidly progressive glomerulonephritis should also be entertained. These include anti-GBM antibody-mediated disease, immune complex disease (of many types), and pauci-immune glomerulonephritis. Notably, this patient’s normal chest X-ray does not completely exclude the possibility of a pulmonary renal syndrome. Therefore, since vasculitis can cause glomerular injury and pulmonary injury, vasculitis cannot be excluded in this patient at this time.
What Additional Studies Are Indicated to Arrive at the Diagnosis for This Patient?
Since the differential diagnosis is now narrowed to include disorders that cause glomerular lesions, a renal biopsy is indicated to include light microscopy, immunofluorescence microscopy, and electron microscopy.
For this patient, measurement of serum complement levels (C3 and C4), serum antistreptolysin O antibodies, serum ANCAs, serum ANAs, and serum anti-GBM antibodies would be helpful to arrive at the most likely diagnosis. At some institutions, these studies are ordered at the patient’s initial presentation, possibly in addition to other studies to identify potential etiologic agents that are known to be associated with glomerular injury (eg, hepatitis B infection and hepatitis C infection).
Diagnostic Findings, Part 3
A renal biopsy is obtained from the patient on an urgent basis. Ultrasound-guided biopsy with on-site gross evaluation is performed to assure that adequate tissue is obtained.
The histopathologic images, including light microscopic, immunofluorescence, and electron microscopic findings for this patient’s renal biopsy, are given in Figures 1 to 7.
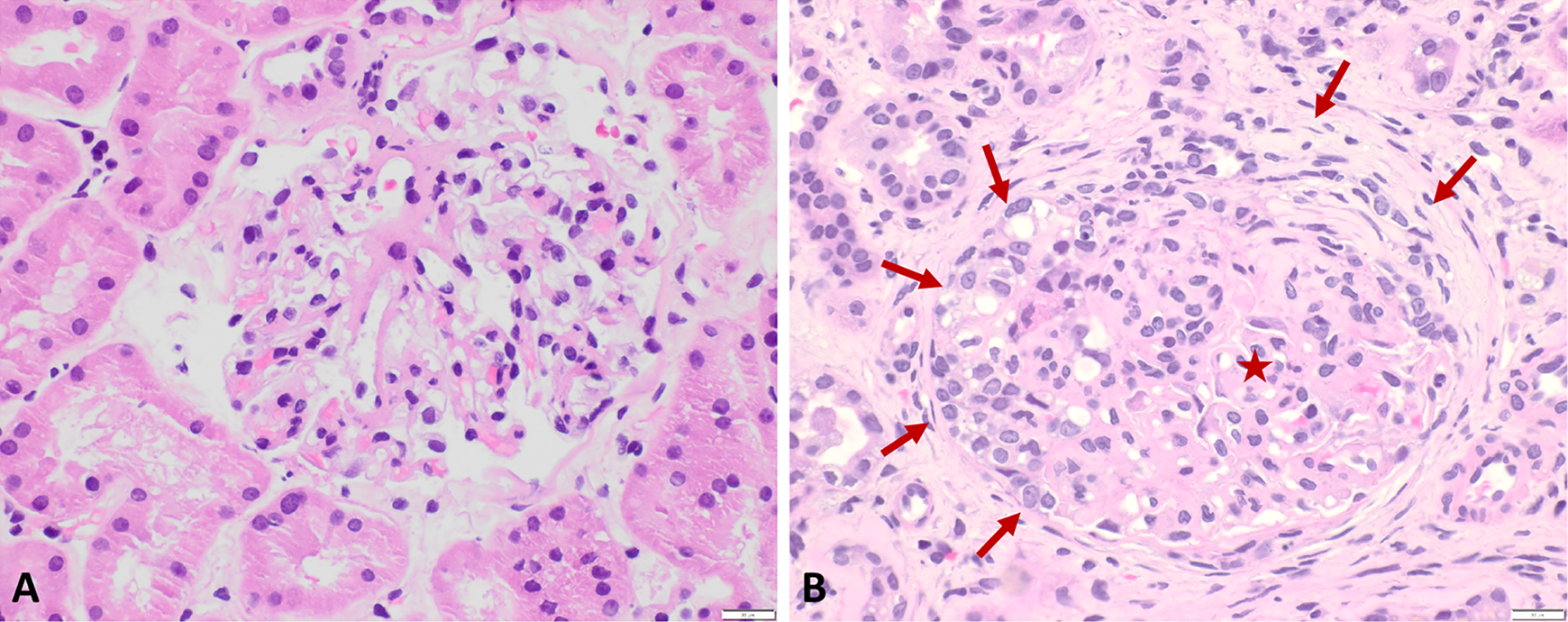
A, A normal glomerulus for comparison. B, An abnormal glomerulus from the patient’s biopsy. The glomerulus (indicated by a red star) shows proliferation and increased cellularity (endocapillary hypercellularity) causing obliteration of the capillary loops. A cellular crescent (indicated by solid red arrows) fills Bowman’s (urinary) space and is focally adherent to Bowman’s membrane (light microscopy, hematoxylin–eosin stain, original magnification ×400). Scale bar: 20 μm.
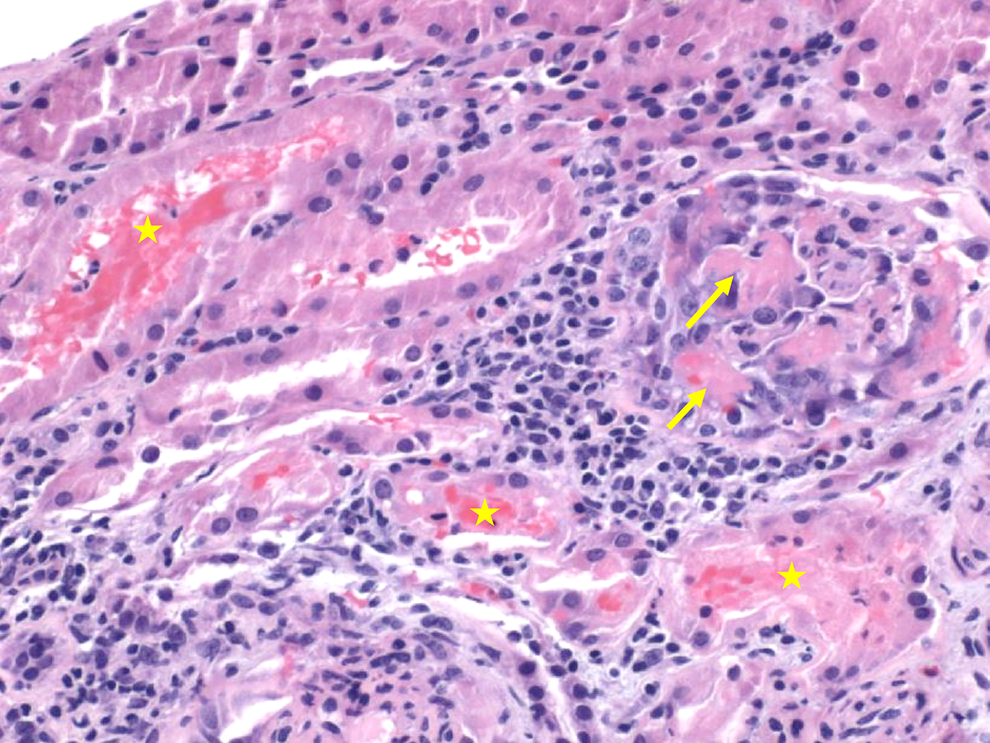
Glomerulus (on right-hand side) with obliteration of capillary loops and fibrin deposition (fibrin indicated by solid yellow arrows). Adjacent tubules contain red blood cell casts (indicated by yellow stars; light microscopy, hematoxylin–eosin stain, original magnification ×400).
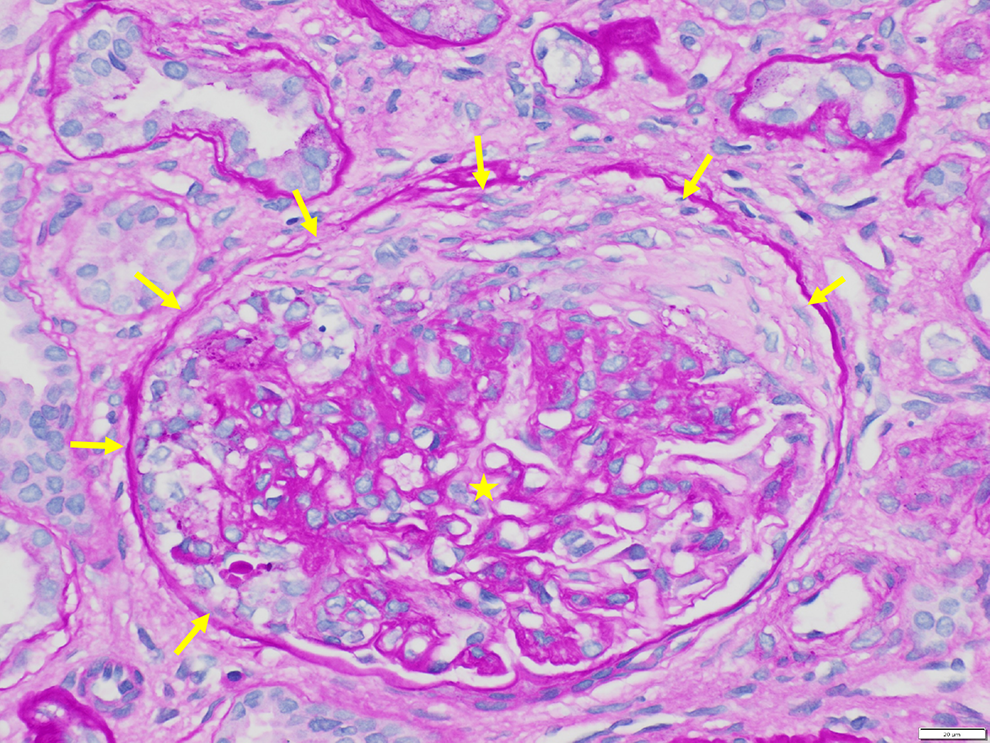
An affected glomerulus (indicated by yellow star) contains a cellular crescent (indicated by solid yellow arrows). Note that the periodic acid–schiff (PAS) stain highlights the distorted glomerular structure and also Bowman’s membrane (light microscopy, PAS stain, original magnification ×400). Scale bar: 20 μm.
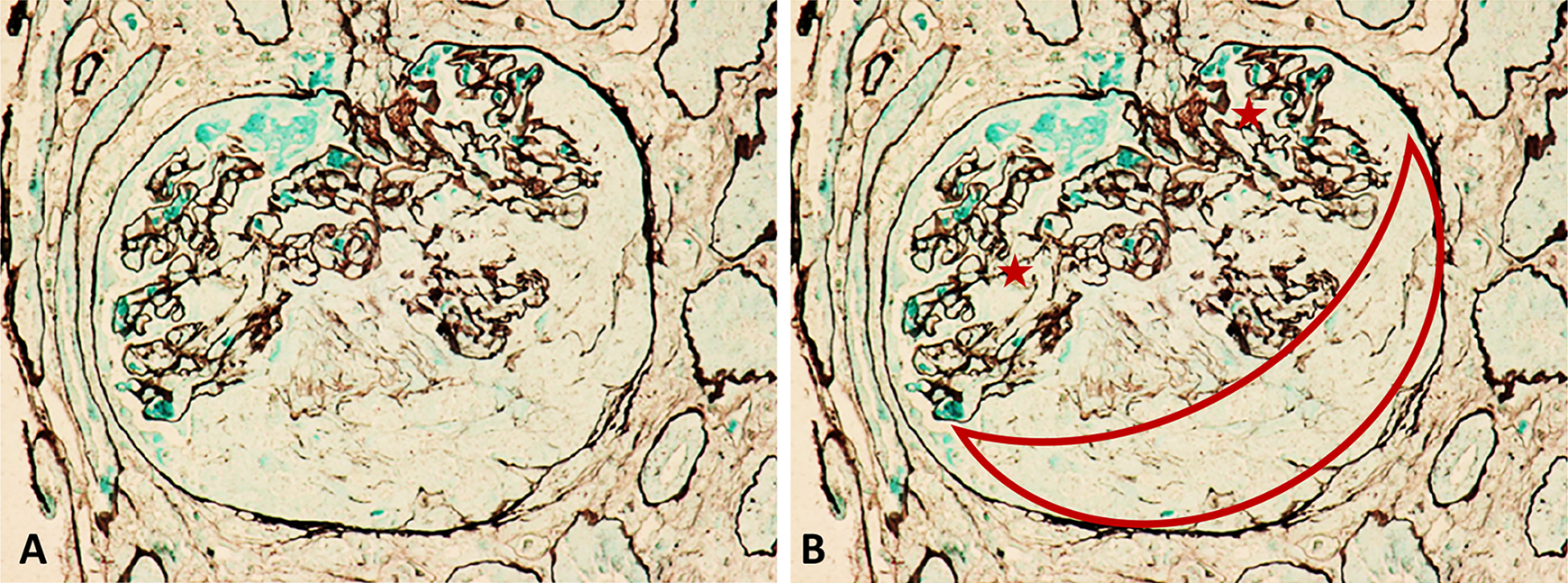
Glomerulus (unannotated) with cellular crescent occupying urinary space (A). In B (annotated), the crescent is outlined in red and the glomerulus is indicated by red stars. Note that the silver stain highlights the glomerular basement membranes and Bowman’s membrane (light microscopy, silver stain, original magnification ×400).
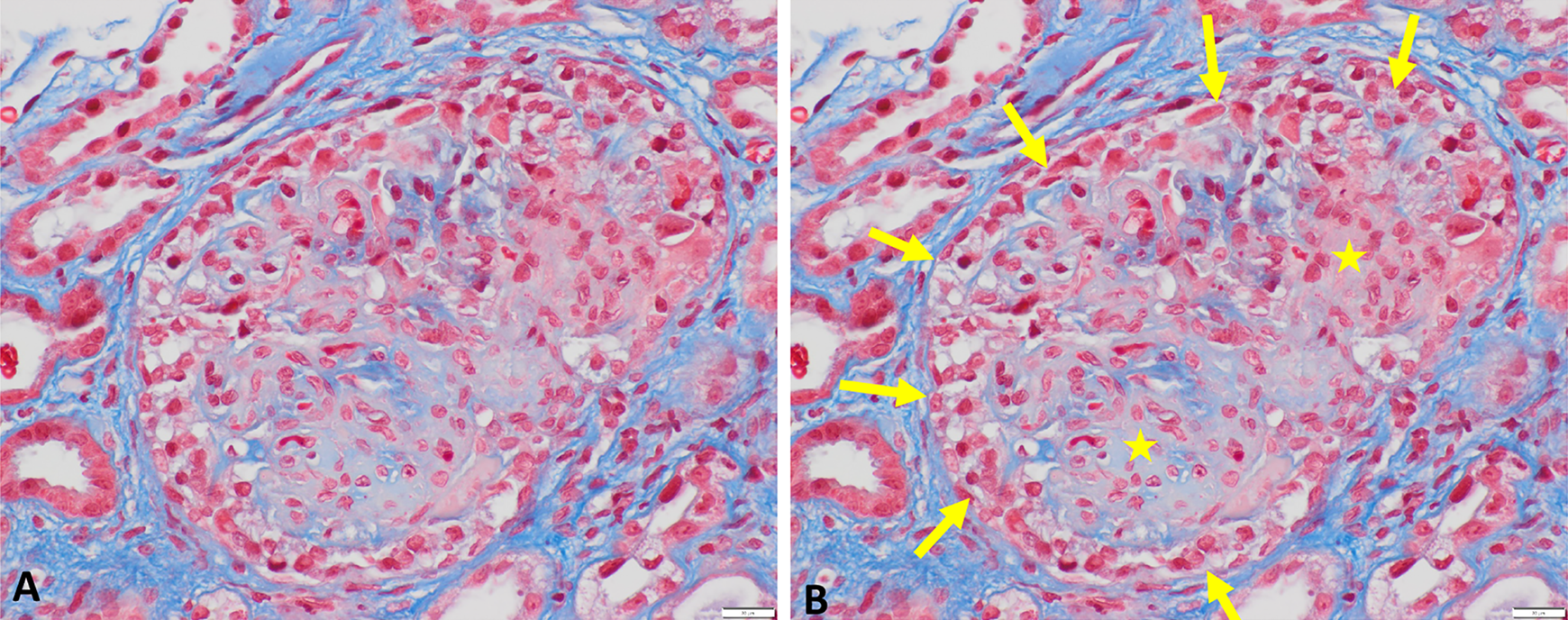
Glomerulus (A, unannotated) with endocapillary proliferation, obliteration of capillary lumina, and cellular crescent. Glomerulus (B, annotated) with endocapillary proliferation (indicated by yellow stars) and a cellular crescent (indicated by solid yellow arrows). Note the glomerular basement membranes and background interstitial fibrous tissue that stain blue (light microscopy, Masson’s trichrome stain, original magnification ×400). Scale bar: 20 μm.
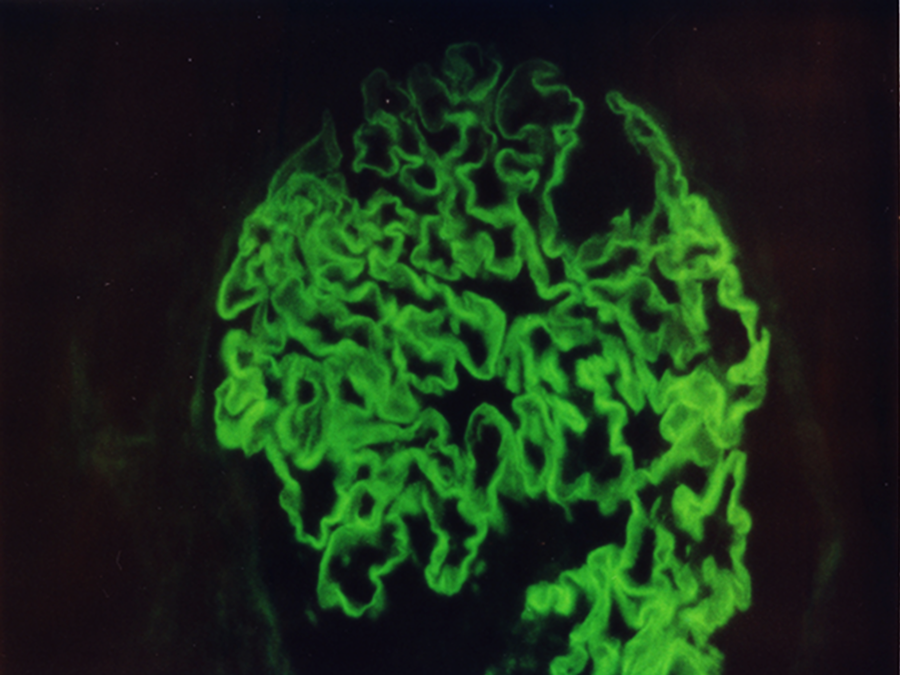
Glomerulus depicting linear staining along glomerular basement membranes on anti-IgG stain (immunofluorescence microscopy, anti-IgG, original magnification ×400). IgG indicates immunoglobulin G.
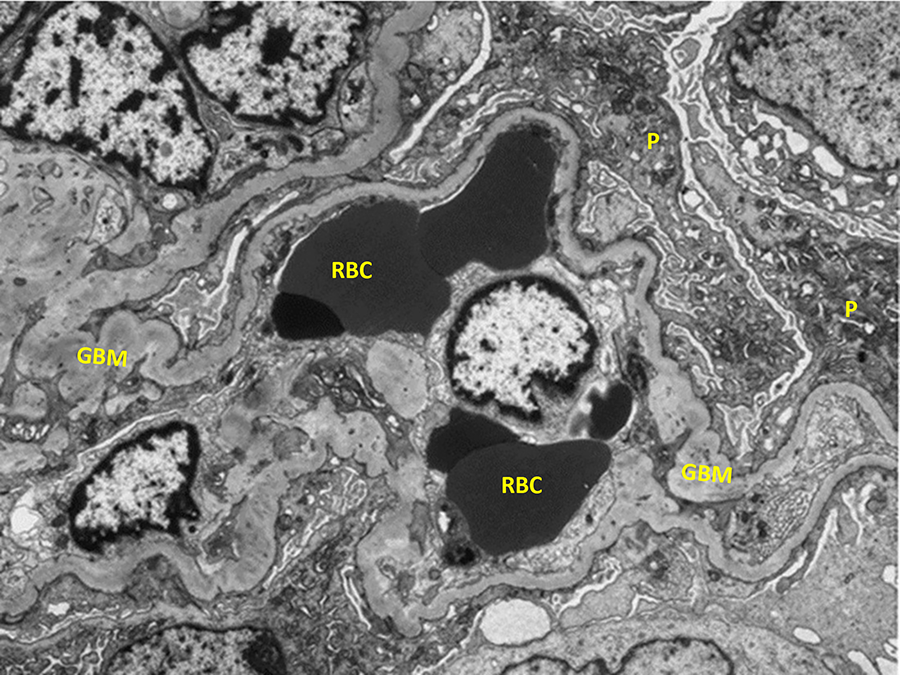
Glomerulus with capillary congestion and no electron-dense deposits along glomerular basement membranes (transmission electron microscopy, approximate original magnification ×3500). GBM indicates glomerular basement membrane; P, podocyte; RBC, red blood cell.
Questions/Discussion Points, Part 3
Describe the Histologic, Immunofluorescence, and Electron Microscopic Findings for This Patient’s Renal Biopsy, From Figures 1 to 7
A description of the findings in this patient’s renal biopsy follows. Note that some of the findings are not depicted in the figures, but are included, for completeness.
Light microscopy: Approximately 13 glomeruli are present, 2 of which appear normal. The remaining glomeruli show diffuse endocapillary hypercellularity with obliteration of the capillary loops, with 5 glomeruli demonstrating cellular crescents (Figure 1). In some glomeruli, fibrin deposition is seen, and red blood cells are present in the lumen of some tubules (Figure 2). Crescents are highlighted on periodic acid–schiff (PAS) and silver stains (Figures 3 and 4). The trichrome stain highlights GBMs and interstitial fibrosis around the tubules (Figure 5). No globally sclerosed glomeruli are noted. Some arteries show intimal edema and myxoid degeneration, consistent with acute hypertensive injury. Mild edema and mild chronic inflammation are noted in the interstitium.
Direct immunofluorescence microscopy: Eight glomeruli are present. Intense (3+) linear deposition of immunoglobulin G (IgG; Figure 6), κ, and λ are present along the GBMs. Weaker (1+) linear GBM deposition of C3 is present. Focal deposition of fibrin (1+) is present within some glomeruli. Staining with IgM, IgA, C1q, and C4 is negative.
Electron microscopy: Diffuse foot process effacement is present. Podocyte prominence is noted, as are mesangial and endocapillary hypercellularity. The basement membranes are irregularly thickened. No electron-dense deposits are identified (Figure 7). Focal fibrin deposition is present within glomerular capillary loops.
What Is the Diagnosis for This Patient Based Upon His History, Physical Examination Findings, Laboratory Results, and Renal Biopsy Findings?
Interpretation of this patient’s history (acute onset of hematuria, hemoptysis, and decreased urine output), physical examination findings (hypertension, slight crackles, edema), and laboratory results (elevated serum creatinine, hematuria, active urinary sediment) support the presence of nephritic syndrome. As is often the case, renal biopsy can elucidate the underlying cause for a nephritic clinical picture. By light microscopy, this patient has crescentic glomerulonephritis. On direct immunofluorescence microscopy, a linear staining pattern with IgG is seen, and there are no electron-dense deposits by electron microscopy. These findings, interpreted in the context of his overall presentation, support a diagnosis of anti-GBM antibody-mediated glomerulonephritis.
What Is the Underlying Pathophysiologic Mechanism for Antiglomerular Basement Membrane Antibody-Mediated Disease?
Injury in anti-GBM antibody-mediated glomerulonephritis is due to the formation of an autoantibody to native antigens that are present within the GBM. The trigger for development of the autoantibody is not known, but a high prevalence of a certain Human Leukocyte Antigen (HLA) subtypes (HLA-DRB1*1501) in affected patients suggests a genetic predisposition to develop autoimmunity in this population. 3 Environmental factors, in particular cigarette smoking, have been linked to development of this disorder, presumably by exposing pulmonary basement membrane antigens to the immune system. 4
The native antigen against which autoantibodies are formed is a component of the noncollagenous domain of the α3 chain of collagen type IV, which is present within the GBM. Once autoantibodies to this antigen have formed, they circulate and find their way to the glomerulus (recall the filtering mechanism of the kidney). When the autoantibodies encounter the antigen to which they are directed (present in the GBM), they bind to that antigen in situ (within the glomerulus). Once formed along the GBM, these antigen–antibody (Ag-Ab) complexes prompt production of various cytokines and recruitment of inflammatory mediators that promote proliferation of intraglomerular cells. 2,5 These cytokines also recruit inflammatory cells that further propagate glomerular injury by release of proteolytic enzymes. 6 This mechanism overall is typically described as a classic type II hypersensitivity reaction. 3 There is also evidence to support associated T-cell-mediated glomerular injury. 4,6
Since the inciting antigen is present in a relatively homogeneous fashion within the GBM, and the antibodies bind to all of the antigen they can find there, the immunofluorescence pattern is linear and uniform in this disorder, rather than granular (in the case of deposition of circulating, preformed Ag-Ab complexes).
In some instances, the anti-GBM antibodies have cross-reactivity with the basement membranes within the lung. If so, this may result in both renal and pulmonary injury, prompting a pulmonary renal syndrome known as Goodpasture disease. 4,5
Briefly Describe the Underlying Pathophysiologic Mechanism for Immune Complex–Mediated Glomerulonephritis. Compare and Contrast It to That of Antiglomerular Basement Membrane Antibody-Mediated Disease
Immune complex–mediated glomerulonephritis is typically characterized by the deposition of Ag-Ab complexes within the glomerulus that have previously formed within the plasma (circulating). The inciting antigens that prompt antibody formation may be native to the patient (endogenous) or derive from an external source (exogenous). Regardless of the antigen’s origin, the antibody that is formed binds to its corresponding antigen, forming circulating Ag-Ab complexes. These complexes then lodge within various parts of the glomerulus (mesangial, subendothelial, intramembranous, subepithelial). 2
As is common in many immune responses, the deposition of immune complexes in the glomerulus often prompts an inflammatory reaction. That inflammatory reaction is often complement mediated and promotes damage to the glomerulus through a variety of mechanisms and mediators. 2 The inflammatory reaction is often elicited through pathways similar to those that cause damage in the setting of anti-GBM-mediated glomerulonephritis.
As noted previously, anti-GBM antibody-mediated disease is caused by the formation of Ag-Ab complexes, but this occurs in situ within the kidney. The antigen is native to the GBM, and the antibody is typically an autoantibody. This is in contrast to immune complex–mediated glomerulonephritis, in which the Ag-Ab complexes form in the circulation and are then deposited or lodged within the glomerulus, as plasma courses through the glomeruli. In these cases, the antibody may be an antibody to foreign antigens (as in the case of postinfectious glomerulonephritis) or an autoantibody to self-antigens (as in the case of lupus glomerulonephritis).
Describe the Histopathologic Changes in Immune Complex–Mediated Glomerulonephritis (eg, in Lupus Glomerulonephritis). Briefly Contrast These to the Histopathologic Changes in Antiglomerular Basement Membrane Antibody-Mediated Disease
Lupus glomerulonephritis is a typical example of glomerular disease caused by the deposition of circulating, already-formed Ag-Ab complexes within the glomerulus. The self-antigens that prompt autoantibody formation are typically nuclear in origin. 7
Light microscopy: The location and extent of Ag-Ab complex deposition within the glomerulus will affect how a patient’s lupus glomerulonephritis is manifest microscopically. 8 As examples:
If the Ag-Ab complexes are primarily deposited in the mesangium, mesangial hypercellularity will be seen by light microscopy, with minimal accompanying glomerular inflammation. This is characteristic of class II lupus nephritis. 9
If the Ag-Ab complexes are primarily deposited in the subendothelial space of the glomerular capillaries, then typically more inflammation is elicited and endocapillary hypercellularity will be seen within most glomeruli. Accompanying glomerular neutrophilic infiltration with or without fibrinoid necrosis may be seen. Sometimes, cellular crescents may form in association with glomerular injury. These findings are typically seen in class III and class IV lupus nephritis, with more significant deposits and inflammatory changes typically seen in class IV. 10
If the Ag-Ab complexes are primarily deposited in the subepithelial space of the glomerular capillaries, then typically less inflammation is elicited, and the GBMs will appear thickened by light microscopy. In these cases, GBM spikes and holes may be seen with the aid of special stains (including silver stain). These features are characteristic of class V lupus nephritis. 9
The spectrum of glomerular histologic features seen in immune complex–mediated disease is generally variable, 11 whereas in anti-GBM antibody-mediated disease, the light microscopic features are typically less variable and relatively severe (glomerular endocapillary hypercellularity with cellular crescents).
Direct immunofluorescence microscopy: As with light microscopy, the location and extent of Ag-Ab complex deposition will affect the features present by immunofluorescence in immune complex–mediated disease. The immune deposits typically have a granular appearance, regardless of where they are deposited, since the complexes are aggregated together in small groups and clusters.
For most patients with lupus glomerulonephritis, deposition of antibody and complement components within glomeruli by immunofluorescence microscopy is typical. This is the so-called “full-house” staining pattern, wherein immunoglobulin components (IgG, IgM, IgA, κ, and λ) are deposited, as are complement components (C3, C4, and C1q). In contrast to the granular morphology observed on immunofluorescence in the setting of immune complex–mediated disease, anti-GBM disease demonstrates a linear morphology on immunofluorescence microscopy (see above).
Electron microscopy: For the various classes of lupus glomerulonephritis, the location and extent of Ag-Ab complex deposition noted on electron microscopy will mirror the findings present by immunofluorescence microscopy. In all cases, the Ag-Ab complexes are seen as electron-dense deposits within various glomerular locations. As examples:
For class II lupus nephritis, Ag-Ab complexes, as electron-dense deposits, will be seen primarily in the mesangium.
In class III or class IV lupus nephritis, the pathogenic Ag-Ab complexes (electron-dense deposits) will be present on the subendothelial side of the GBMs within glomerular capillary loops.
For class V lupus nephritis, the immune complexes (electron-dense deposits) will be present primarily on the subepithelial side of the GBMs. 9
In contrast, given the uniform distribution of the offending antigen in anti-GBM-mediated glomerulonephritis, and the in situ formation of the Ag-Ab complexes, no electron-dense deposits are observed in this disorder by electron microscopy.
A summary of the clinical presentation, as well as these light microscopic, direct immunofluorescence microscopic, and electron microscopic findings that are found in lupus nephritis, is presented in Table 2.
ISN/RPS 2003—Classification of Lupus Nephritis (LN).11
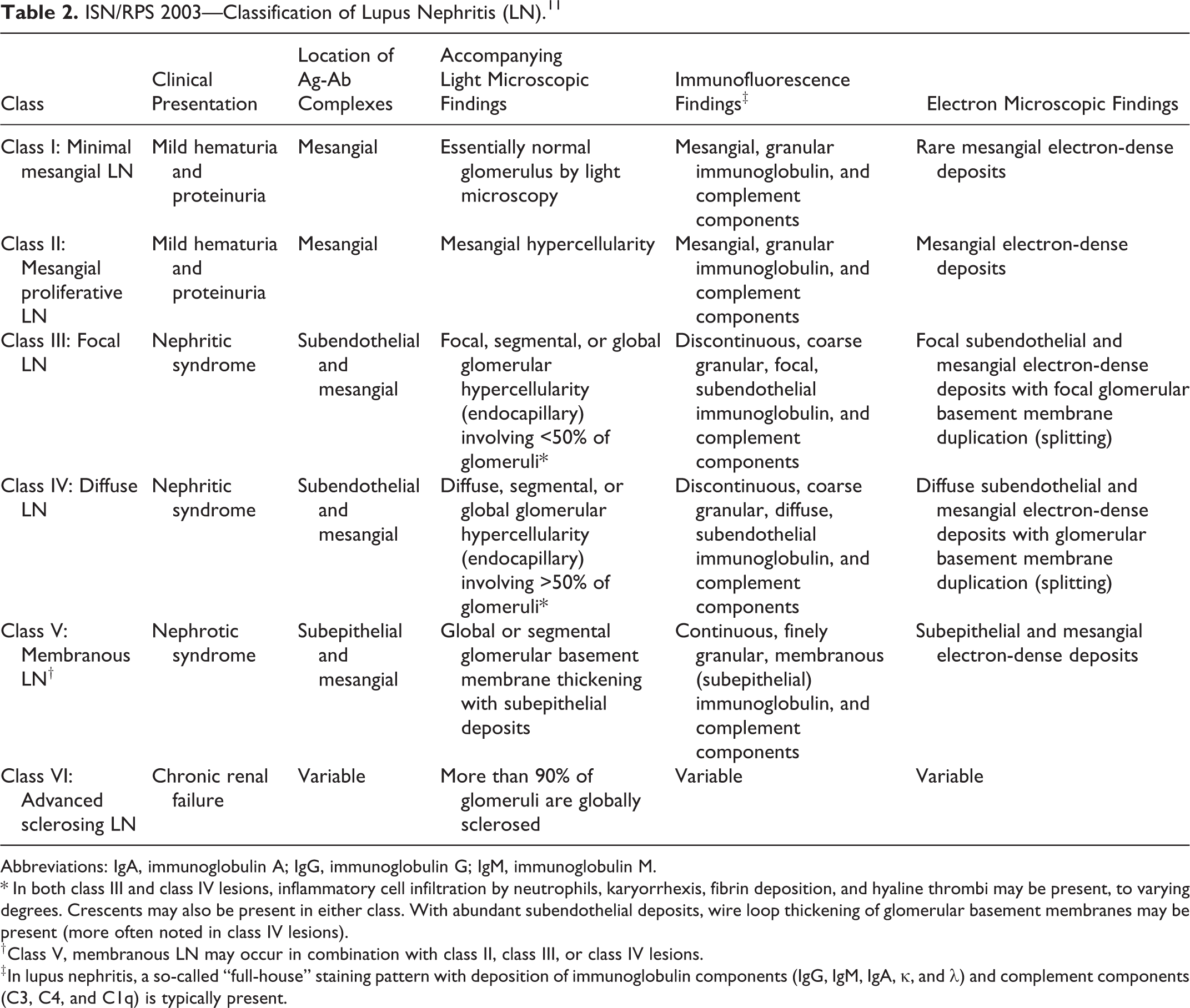
Abbreviations: IgA, immunoglobulin A; IgG, immunoglobulin G; IgM, immunoglobulin M.
* In both class III and class IV lesions, inflammatory cell infiltration by neutrophils, karyorrhexis, fibrin deposition, and hyaline thrombi may be present, to varying degrees. Crescents may also be present in either class. With abundant subendothelial deposits, wire loop thickening of glomerular basement membranes may be present (more often noted in class IV lesions).
† Class V, membranous LN may occur in combination with class II, class III, or class IV lesions.
‡ In lupus nephritis, a so-called “full-house” staining pattern with deposition of immunoglobulin components (IgG, IgM, IgA, κ, and λ) and complement components (C3, C4, and C1q) is typically present.
What Therapeutic Approaches Are Generally Successful in Treating Antiglomerular Basement Membrane Antibody-Mediated Disease? Why?
Once anti-GBM antibody-mediated disease is diagnosed, plasmapheresis is a mainstay of therapy. 3 Plasmapheresis (plasma exchange) serves to remove the offending antibody from circulation, replacing the patient’s removed plasma with plasma that does not contain the offending antibody. Immunosuppressive agents are also often used to help decrease overall immunoglobulin (autoantibody) production, thereby decreasing the number of pathogenic antibodies available to bind in the kidney and prompt organ damage. 3 Moreover, immunosuppressive and anti-inflammatory agents can help attenuate the immune response within glomeruli when antibodies bind glomerular antigens. 6
In Contrast, What Therapeutic Approaches Are Generally Successful in Treating Lupus Nephritis, as an Example of Immune Complex–Mediated Glomerulonephritis? Why?
In lupus nephritis, anti-inflammatory and immunosuppressive agents are used in combination, as a mainstay of therapy. Recall that in lupus nephritis, the deposition of circulating immune complexes can prompt an inflammatory reaction within the glomeruli. Therefore, it logically follows that the use of anti-inflammatory agents can attenuate the inflammatory reaction within glomeruli. Furthermore, use of immunosuppressive agents can decrease the patient’s autoimmune response overall, thereby reducing the number of circulating Ag-Ab complexes that form and are available to be deposited within the kidney and other organs. 7 More intense immunosuppression serves to quickly attenuate inflammation during a flare of lupus nephritis (induction), while lower dose immunosuppression over a longer term can help a patient maintain a flare-free state. 12,13 The classification, severity, and activity of lupus nephritis and the extent of chronic damage are typically determined by a renal biopsy, which then guides the therapeutic approach to an individual patient. 7,10
Teaching Points
Immune-mediated mechanisms underlie many cases of glomerular injury.
History and physical examination findings aid in formulating a relevant differential diagnosis in patients with renal syndromes.
Diagnostic laboratory studies, including serum electrolyte studies, serum BUN and creatinine, comprehensive metabolic profile, complete blood count, and urinalysis, are necessary to evaluate patients with renal syndromes. A rise in serum BUN and creatinine can indicate impaired renal function or reduced GFR, and abnormalities on a comprehensive metabolic profile can indicate the level of renal functional impairment. Urinalysis findings can help differentiate between a nephritic or nephrotic picture, which can then support formation of an appropriate differential diagnosis for a given patient.
Nephritic syndrome is defined by a decline in renal function (reduced GFR), hematuria, proteinuria, and hypertension.
An active urinary sediment, composed of dysmorphic red blood cells and red blood cell casts, is typically present in nephritic syndrome, in contrast to a bland urinary sediment (acellular), which is composed of lipid droplets, oval fat bodies, and lipid-laden casts and is often seen in nephrotic syndrome.
Nephritic syndrome is usually caused by damage to glomeruli via immune-mediated pathways. Examples include formation of Ag-Ab complexes in situ within the kidney, as in anti-GBM antibody-mediated glomerulonephritis, and deposition of circulating Ag-Ab complexes within various immune complex–mediated glomerulonephritides, such as lupus glomerulonephritis.
The Ag-Ab complex deposition and/or in situ formation within glomeruli often activate inflammatory pathways that cause glomerular injury.
In immune complex–mediated glomerulonephritis, Ag-Ab complexes may lodge in a variety of locations within glomeruli. The pattern and site of immune complex deposition influences how the disorder manifests clinically and pathologically.
In immune complex–mediated glomerulonephritis, the Ag-Ab complexes appear as granular glomerular deposits on immunofluorescence. However, in anti-GBM antibody-mediated glomerulonephritis, a linear membranous staining pattern is seen within glomeruli on immunofluorescence.
Due to the unique pathogenesis of anti-GBM antibody-mediated glomerulonephritis (autoantibody directed against native GBM antigen), plasmapheresis is indicated and helpful to remove the offending antibody from circulation.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
