Abstract
Pathologists and laboratory scientists provide valuable guidance on laboratory utilization, test ordering, interpretation, and quality control provided that clinical staff can easily access the laboratory team. To encourage consultation between clinicians with laboratory scientists and pathologists, we developed an easily accessible electronic tool termed “MyPathologist,” placed on the homepage of our electronic health record system. Over its 2-year pilot, utilization of this consultation tool climbed as we continued to publicize it and incorporated education into housestaff onboarding and electronic health record training. Physician satisfaction with the tool was high. Additionally, this became the primary source of consults to our residency call service. Evaluation of MyPathologist questions received during its pilot period showed that more than half the questions were of significant educational value to the residents, often focusing on results interpretation, appropriate test ordering, and quality control. MyPathologist is a novel electronic tool for pathology consultation within our electronic health record and also represents an avenue for educating residents, improving utilization of the laboratory, and improving patient care.
Keywords
Introduction
Clinical medicine is increasingly complex, with the regular implementation of new laboratory tests, diagnostic algorithms, and consensus guidelines. It is difficult for practicing clinicians to stay abreast of the rapid advances in laboratory medicine, even in the area of their expertise. One survey of laboratory utilization patterns revealed that primary care physicians were uncertain of up to 23% of tests utilized, with test ordering uncertainty in 14.7% and test interpretation uncertainty in 8.3%. 1 The 2015 Institute of Medicine report, “Improving Diagnosis in Healthcare,” recognizes diagnosis as a team effort that requires pathologist input and interaction with clinical colleagues. 2,3 Educating and providing consultation is a role that pathologists must embrace. 3
Pathologists can offer guidance on the utilization of the laboratory, a function that is becoming critical in this era of cost control and health-care reform. 4,5 A great opportunity exists for pathologists to advise clinical colleagues on appropriate test ordering, result interpretation, follow-up testing, and send-out tests. Increased consultation on correct ordering and interpretation of many laboratory tests can affect the speed, outcome, and cost of clinical management for many patients.
However, in this era of expanding, decentralized health systems and extensive use of the electronic health record (EHR), it is more difficult for physicians to access pathology and laboratory medicine staff for consultation and advice. A recent study noted that only 6% of primary care physicians consulted with laboratory professions in a given week. 1 The changing patterns of interphysician communication prompted by the EHR system, such as the electronic messaging system within the EHR, have also altered communication habits.
We have also noted shifting communication patterns in our clinical environment. Electronic communications have become the mainstay in our multihospital system, with many of our clinical colleagues practicing in ambulatory settings located at a distance from the hospital. Fewer of these physicians come to the pathology department to discuss laboratory findings, as the majority of inpatient care has shifted to hospital-based services and hospitalists; and thus, outpatient physicians may never be present in the hospital itself. The laboratory may be unknown territory for clinicians who may not understand which specific section of the laboratory a particular test is performed or may not know who to contact to obtain further information or interpretive assistance. Over time, we had noted the decreased frequency of traditional pager-based calls to our clinical pathologists and pathology residents. We postulated that in this era of electronic communication, we needed a new tool to enable clinicians in both the ambulatory and the inpatient settings to more readily query the pathology and laboratory medicine department.
To facilitate laboratory consultations, our goal was to build an easily accessible electronic communication function embedded in our EHR. We placed a laboratory icon on our EHR toolbar, linking it to several reference resources and an electronic consultation tool. This tool, named “MyPathologist,” transmits electronic messages to a shared pathology inbox and triggers an immediate text page to the pathology resident on call. This article reviews the design of and our initial experience with this consultation tool.
Methods
IT Build
Working with hospital IT, we placed a laboratory consultation icon, called “MyPathologist,” at the top of the main toolbar within our EHR. The MyPathologist icon remains accessible on the top toolbar throughout the EHR session for all physicians in both inpatient and outpatient settings. This includes approximately 2000 hospital- and community-based physicians. This tool was launched in late spring of 2015.
Workflow
Departmental guidelines for use and response to MyPathologist consultations were discussed and developed in a series of faculty and resident meetings. During this pilot period, operating hours were defined as Monday through Friday from 8
Incoming messages generate an immediate text page to the clinical pathology resident on call. Consultative questions are reviewed and answered via the EHR inbox with guidance from the attending clinical faculty or anatomic pathologist. Messages are retained in the group inbox available to all residents and pathology faculty for review and discussion. A monthly departmental conference is used to review important MyPathologist questions. Questions and responses are also copied into a shared spreadsheet available to Pathology faculty and residents that allows for quick reference and also provided data for this article.
During the pilot phase, MyPathologist access was open to physicians, hospitalists, and medical interns, residents and fellows, with the inclusion of nurse practitioners and physicians’ assistants planned after full implementation.
Publicity, Training, and Utilization
MyPathologist was initially publicized via instructional e-mails to all medical staff and housestaff as well as in-person presentations at multiple professional staff, medical group, and clinical division meetings during late 2015. Starting in 2017, it was included in housestaff orientation sessions and was formally added to the onboarding EMR training sessions for new physicians in late 2017.
In December 2017, a short survey was distributed to the professional staff via e-mail to gather data from users and nonusers to inform further revision of the tool.
Evaluation
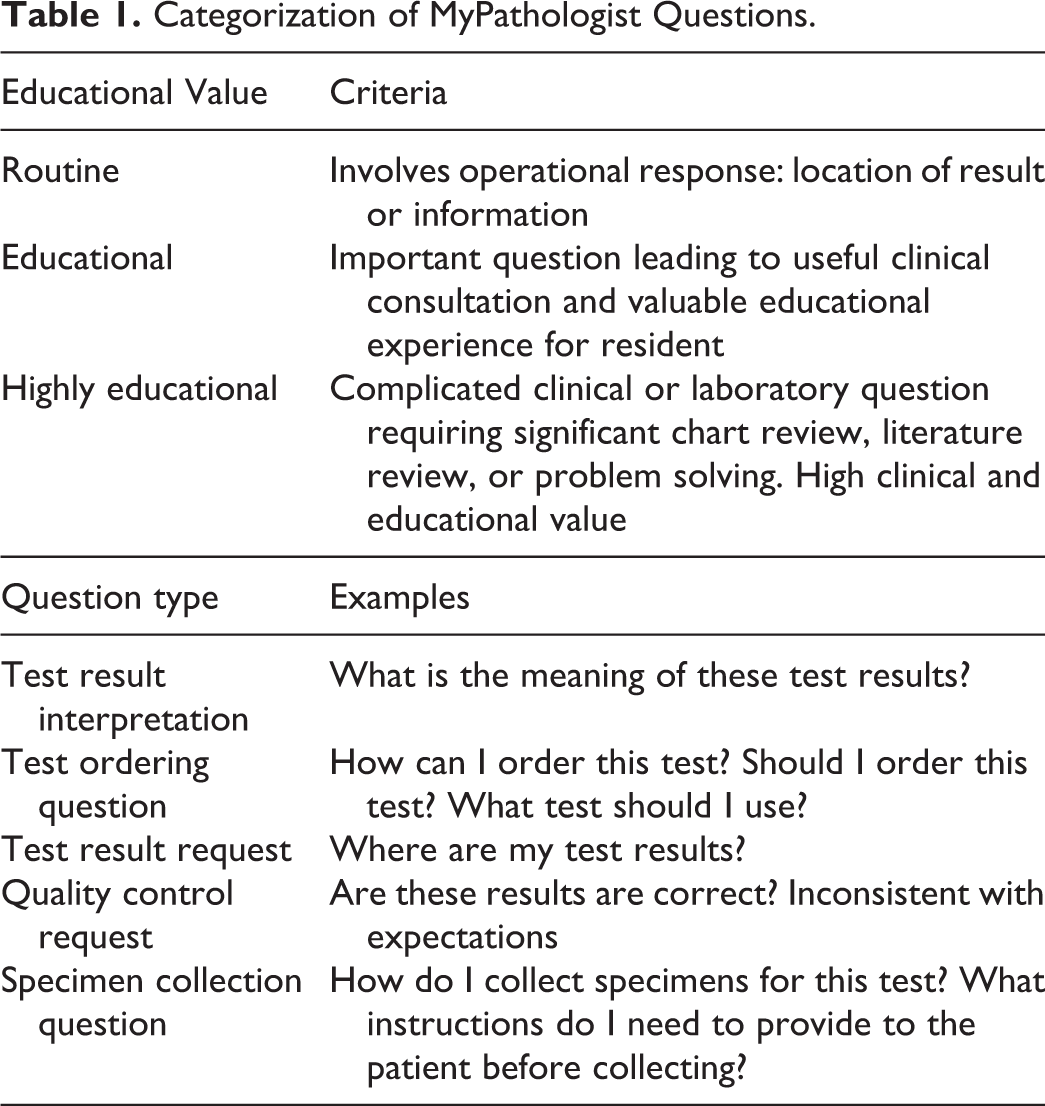
All MyPathologist questions and answers during a pilot period from May 2015 to May 2017 were evaluated for educational value by 2 pathology residents (E.S. and T.T.) and an attending pathologist (K.K.) using a 3-point scale (routine, educational, or highly educational). MyPathologist questions were also sorted by type into test result interpretation, test ordering question, result request, quality control review, specimen collection question, and miscellaneous (Table 1).
Categorization of MyPathologist Questions.
Frequency of physician use and time to response were also monitored.
Results
IT Build
The MyPathologist icon on the EHR home page is shown (Figure 1A). This icon is linked to a drop-down menu (shown) that contains key pathology resources for physicians, including our laboratory’s searchable test catalog, access to Department resources, links to Laboratory Tests Online, UpToDate, interpretative guidelines for test results, and at the top, a link to the MyPathologist consultation tool (Figure 1B). This tab links to a prepopulated electronic message window with the option of sending a general message or one linked to a particular patient. When sent or “accepted,” the in-basket message triggers a text page to the on-call clinical pathology resident indicating that an incoming query has been received in the MyPathologist inbox.
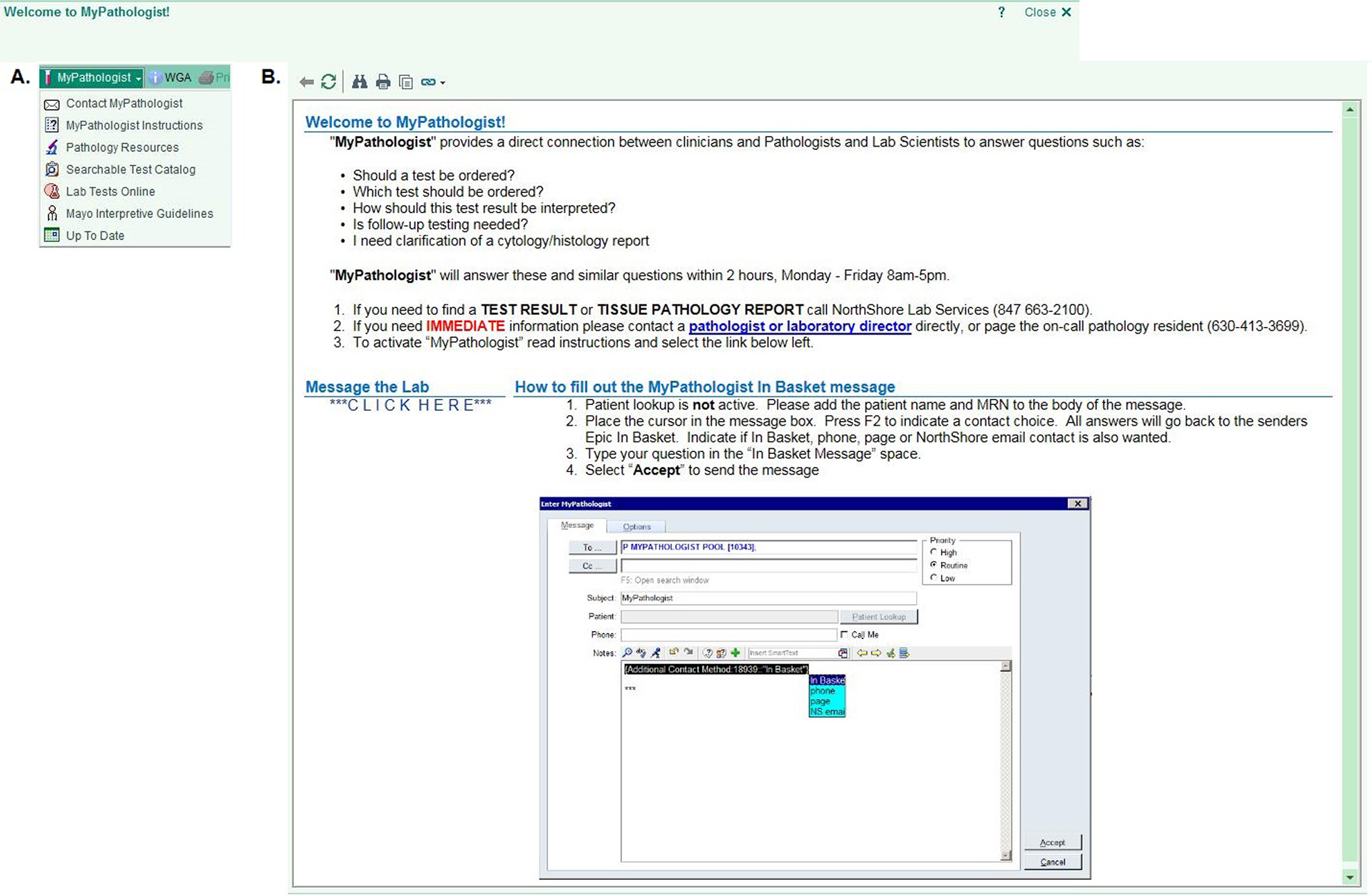
Screenshot images of the MyPathologist tool within our EMR. A, the MyPathologist icon in the EMR toolbar, along with the dropdown menu of additional tools and resources. B, The instructional display that appears when “contact MyPathologist” is selected, which includes the link to the electronic communication tool.
Frequency of Use
As shown in Figure 2, utilization of the MyPathologist tool increased gradually over time since its launch in May 2015. During the 2-year pilot period, an average of 18 queries per month was handled by residents fielding consultations via MyPathologist. Notable increases in the frequency of questions were observed following the addition of training to housestaff orientation in June 2017 and also after an e-mail distribution to the professional staff in December 2017 (which contained the link to the survey).
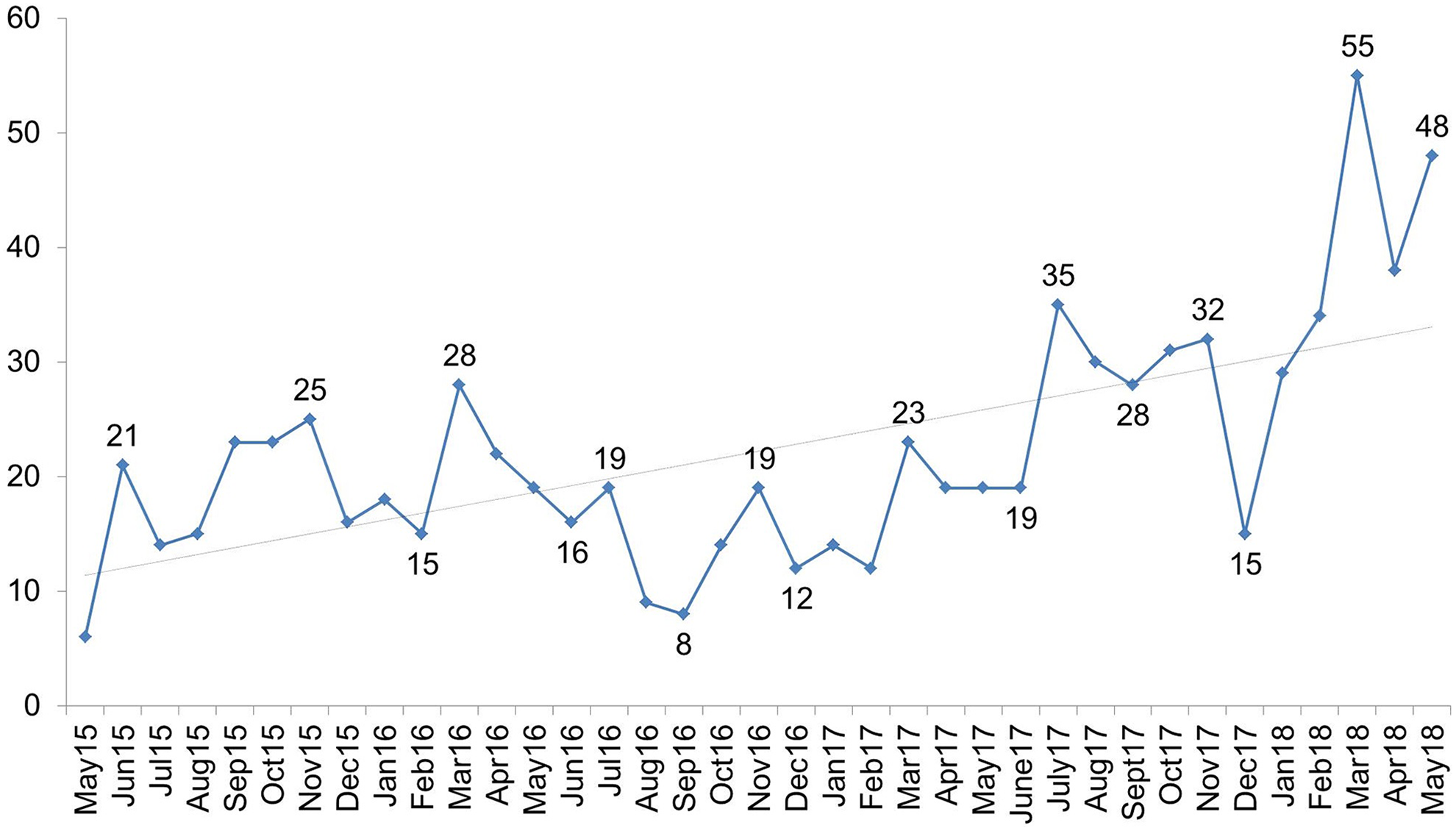
Frequency of consultations addressed via the MyPathologist tool. Notable increases occurred following presentation of the tool at housestaff orientation in 2017, and in early 2018 following inclusion of the tool in new physician training, and distribution of an e-mail to professional staff to remind them of the tool and request feedback.
Although response to the clinician survey was low, the results indicated that 40% of respondents who had not used the tool reported that they were not familiar with it. The uniqueness of this tool to our health-care system, and the need for additional publicity and training were underscored by these data, and the fact that usage increased following the distribution of the survey, which did promote the tool.
Surveyed users did report satisfaction with the ease of use within our EHR and with the speed and quality of responses and reported using it mostly for appropriate test selection and interpretive issues. Additional survey data will be collected.
Evaluation
A total of 433 MyPathologist questions were evaluated during the pilot period from May 2015 to May 2017. The clinical chemistry laboratory received the most questions followed closely by microbiology, surgical pathology, hematology, molecular, and blood bank (Figure 3A). The most commonly asked question types were quality control questions/requests followed by test ordering, test interpretation, test result requests, miscellaneous communications, and specimen collection questions (Figure 3B). Less than half of all questions were routine, with the remainder considered educational or highly educational (Figure 3C). Miscellaneous questions were mostly physician orders and communication to the laboratory. A sample of questions received in the MyPathologist consultation service is listed in Table 2.
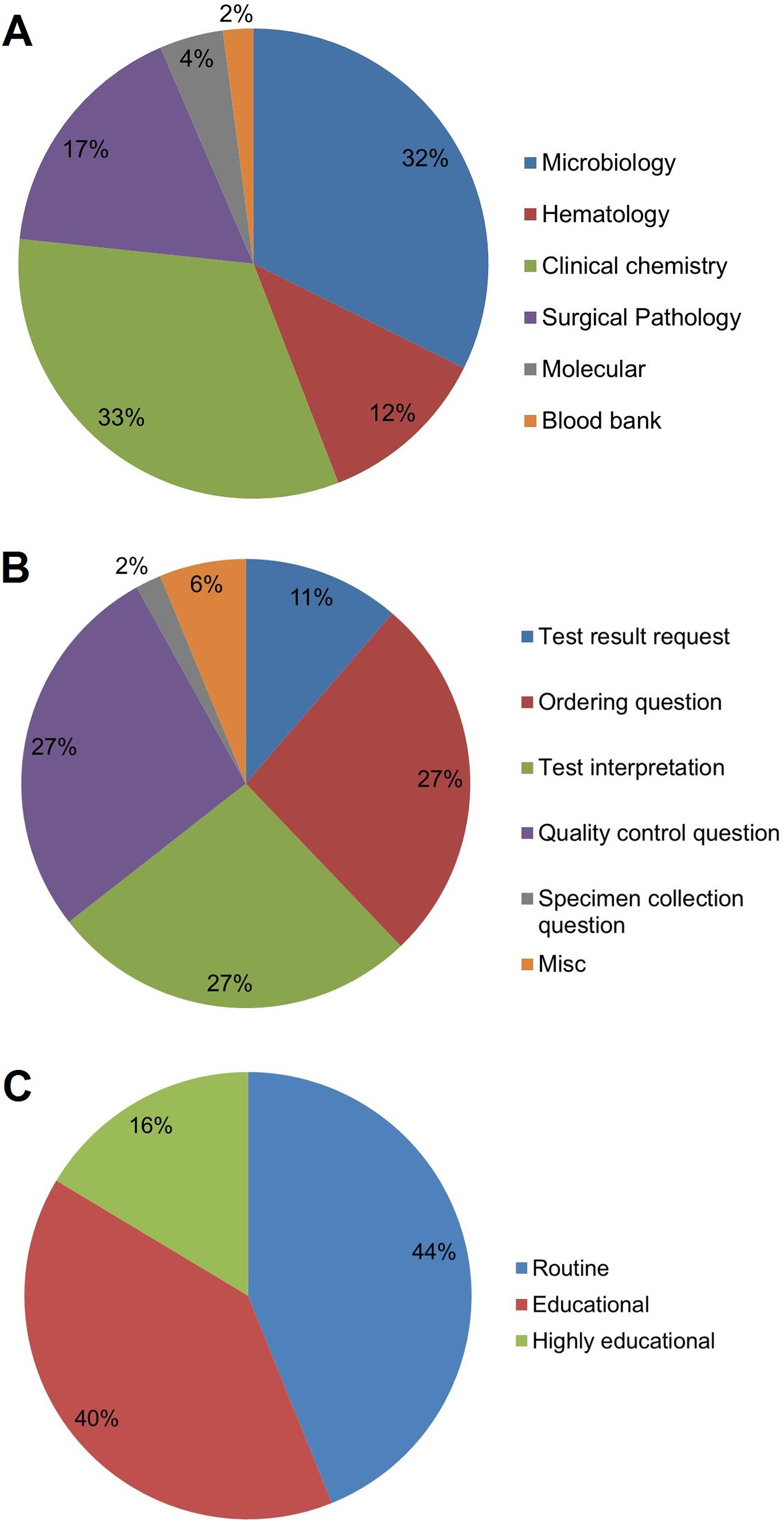
Types of consultative questions received via the MyPathologist tool, categorized by laboratory specialty (A), type of question (B), and assessed educational value (C).
Example MyPathologist Questions.
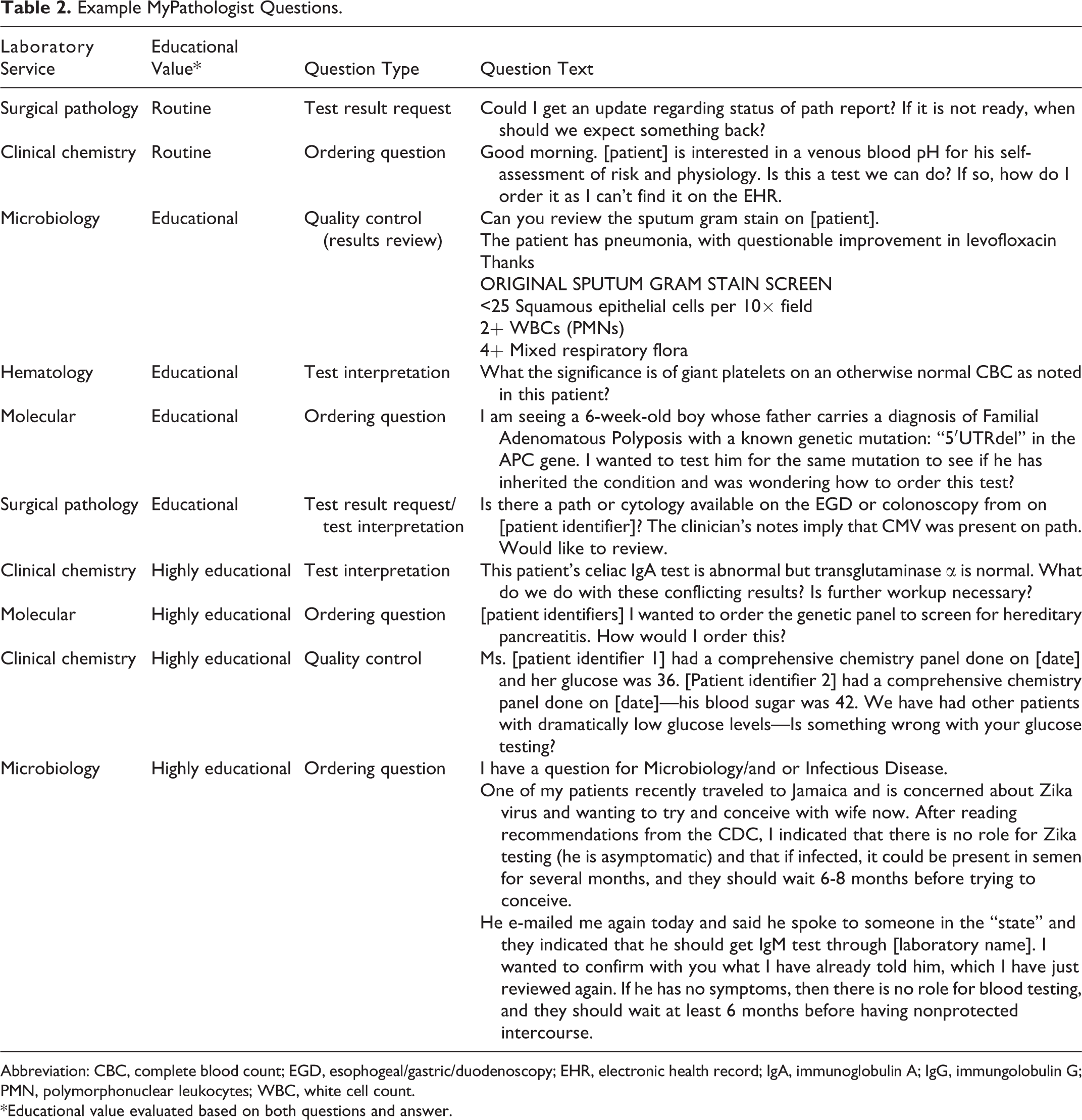
Abbreviation: CBC, complete blood count; EGD, esophogeal/gastric/duodenoscopy; EHR, electronic health record; IgA, immunoglobulin A; IgG, immungolobulin G; PMN, polymorphonuclear leukocytes; WBC, white cell count.
*Educational value evaluated based on both questions and answer.
Questions stratified by educational value, laboratory, and question type are presented in Figures 4 and 5. Approximately 72% of clinical chemistry, 56% of microbiology, 47% of hematology, and 68% of molecular questions were either of educational or of high educational value, with 28% of clinical chemistry questions receiving the designation of high educational value, as shown in Figure 4.
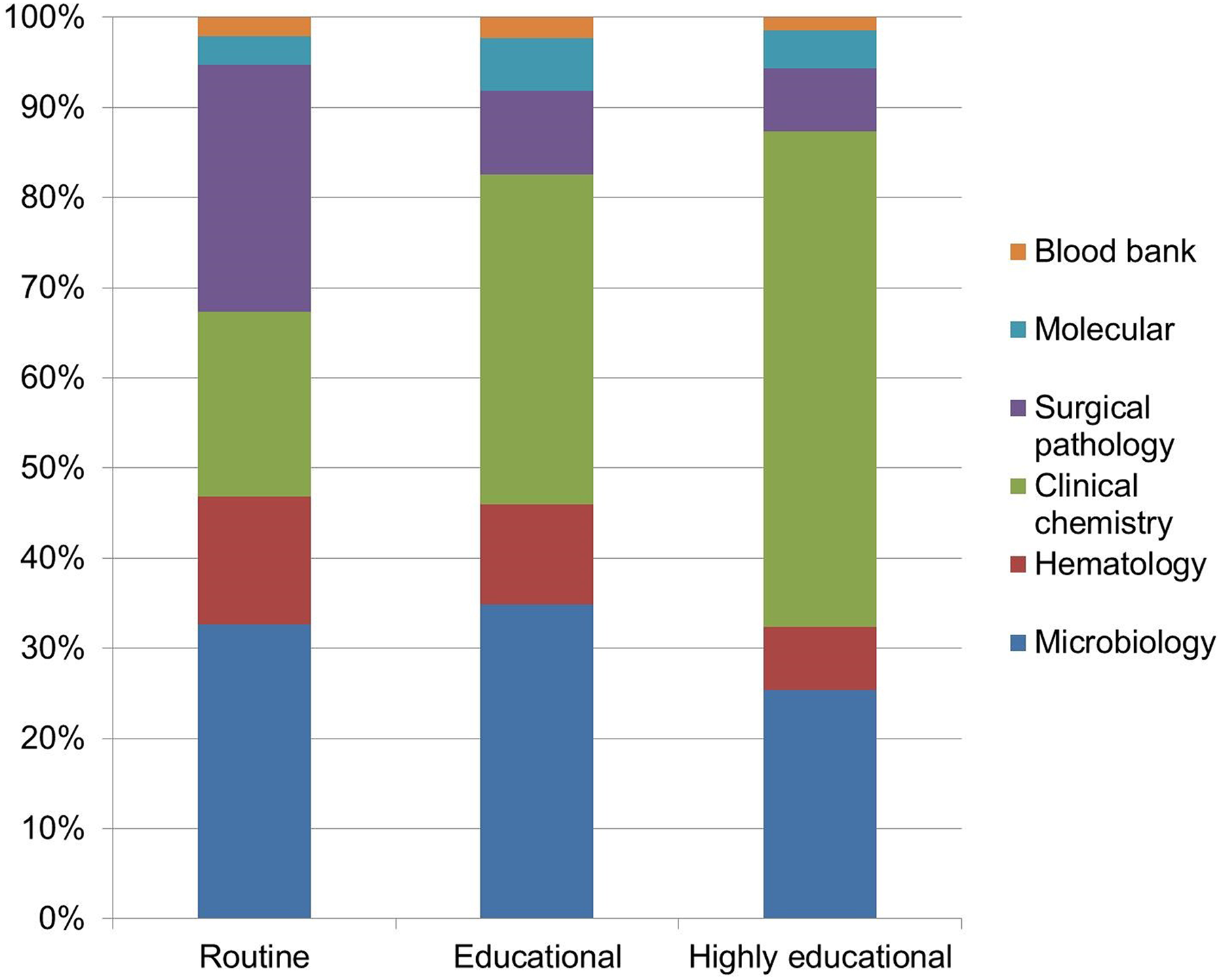
Relationship of the educational value of questions from the various laboratories.
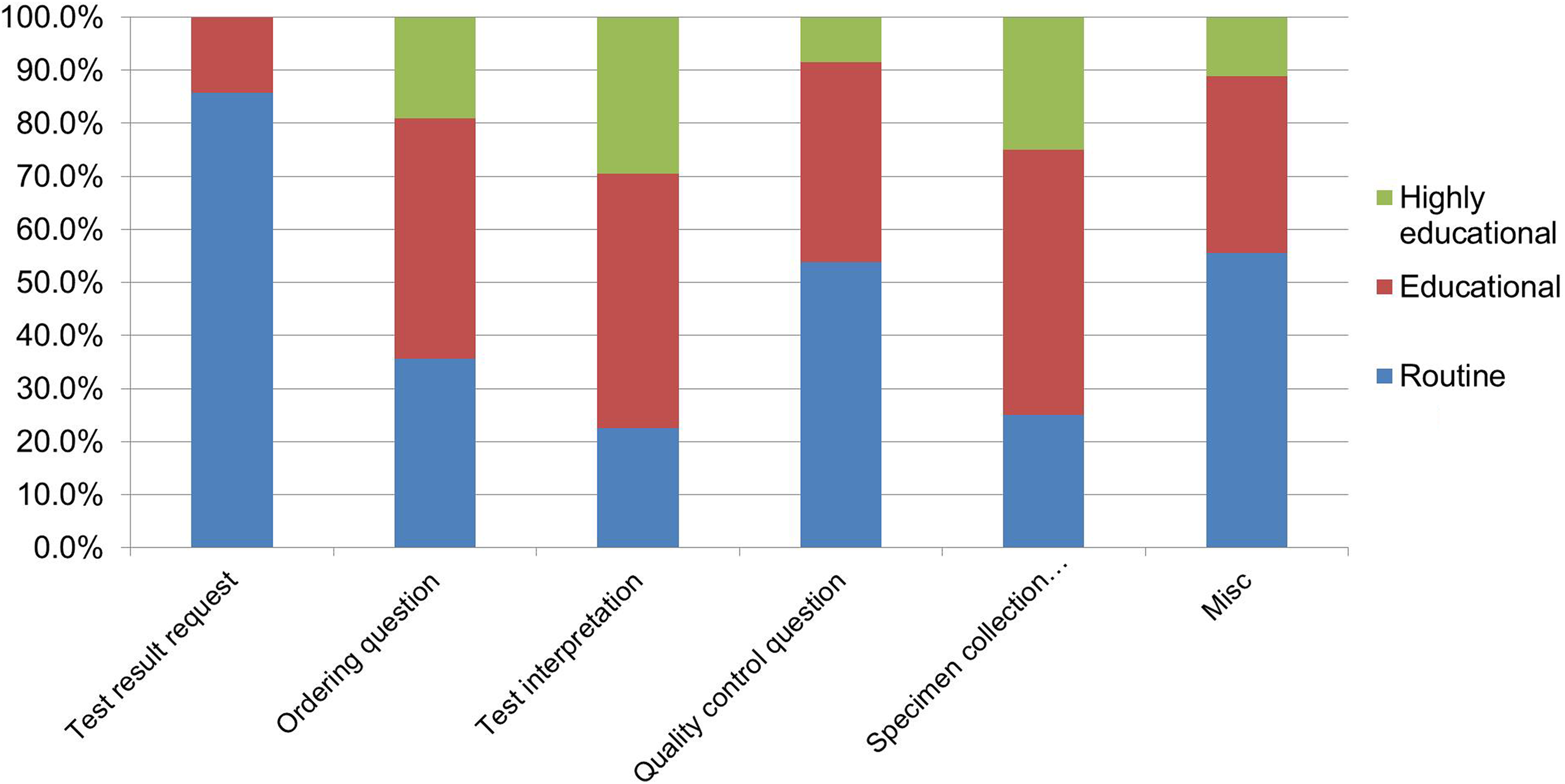
Relationship of the educational value of questions and the type of consultative question received.
The majority of questions with educational to high educational value were test interpretation or ordering questions (Figure 5). In particular, most molecular questions were ordering questions, where test utilization and interpretation is a key issue. Specimen collection questions also tended to have educational to highly educational value; however, the total number was relatively small. Test result requests, as expected, were mostly routine.
A significant proportion of quality control questions were slide review requests of Gram stains and peripheral blood smears, representing the majority of questions in microbiology (44%) and hematology (43%), respectively. These were often initiated because clinicians sought understanding of results that may not have been entirely consistent with expectations. Although the proportion of quality control questions with educational to highly educational value was less than that of ordering or interpretation questions, 46% of quality control questions proved to be of educational to highly educational value. Some questions in this category also required thorough investigation into laboratory management topics.
The majority (71%) of surgical pathology questions were classified as routine, consisting of simple requests for results. The majority of more challenging surgical pathology questions went directly to attending anatomic pathologists, leaving routine queries of “low” educational value to be directed to MyPathologist. Of note, surgical pathology results are readily available in our EHR. Additional user training and redirection of these results requests are planned to facilitate efficient access to results and reports.
Discussion
The implementation of MyPathologist has provided a valuable consultation tool for clinicians in our institution. This tool is utilized by physicians and housestaff across our inpatient and ambulatory operation, with plans to eventually expand to physician assistants and nursing staff. The gradually increasing utilization of this tool reflects the slowly growing familiarity within our health-care system. Although this tool was initially introduced via e-mail announcements to the professional staff and a series of live presentations (including our housestaff orientation), we have found that a surprising number of physicians remain unaware of MyPathologist. We have recently had the tool implemented into EMR training during physician onboarding and are renewing our promotional announcements.
The MyPathologist electronic consultation tool is intended as an additional method to consult with the laboratory, complementing phone calls, and our traditional on-call system. Although we did not quantify traditional calls to laboratory directors and the residents during this period, there was no perception of a decrease. We believe that the easily accessible MyPathologist tool served to increase communications with the laboratory.
In addition, MyPathologist proved to be useful tool for pathology resident training. The majority of questions with high educational value were test interpretation or ordering questions suggesting that in these areas where pathologist input is a valuable knowledge source for clinicians. These questions also provide an opportunity for clinician guidance regarding appropriate test utilization and cost considerations. Even routine questions have significant value in teaching pathology trainees to rise to the role of consultant and collaborator with clinicians. Clinical pathology consultation requires the exercise of good communication skills, critical thinking, and problem-solving. The MyPathologist call system simulates a clinical laboratory director’s role and helps fulfill ACGME pathology milestones. 6,7 Since clinical pathology call responsibilities are proportionally handled by more senior residents (PGY3 and 4), this also became an important part of graduated responsibility within our program. Additionally, the use of a common file and a regular conference also helps in documenting and teaching real-life, problem-solving skills to all residents. 8,9
A number of challenges and opportunities remain for our implementation of an EHR-based clinical pathology consultation system. Blood bank questions were comparatively low, since clinicians tend to consult directly with our transfusion medicine attendings. This contrasts with a prior study of clinical pathology resident on traditional pager-based call demonstrated that approximately 30% to 50% of calls at their institution were related to the blood bank. 6,10,11 This may reflect institutional cultural differences in the expectations of clinical physicians; in larger academic centers, there is an expectation of resident response to emergent calls such as are common in transfusion medicine, whereas in private hospitals and hybrid settings such as our institution, clinicians may be accustomed to direct communication with laboratory directors and anatomic pathologists. Additionally at our institution, senior clinical attendings, particularly specialists, have often continued established patterns of communication directly with laboratory directors.
Emphasizing the role and convenience of MyPathologist may help to increase usage. Additionally, modifying EHR training during orientation of new physicians, nurses, and physician assistants to include examples and references to MyPathologist may also promote use. In the 3 months prior to submission of this article, usage of this service approximately doubled compared to the pilot time period analyzed, suggesting that our ongoing efforts to promote MyPathologist continue to be effective.
If the MyPathologist system is expanded to include additional hours, weekends, or additional practitioners, resident and pathologist workload is expected to increase. In such a case, appropriate steps must be taken to ensure that resident education and general service duties are not compromised. Currently, the system serves as an educational adjunct, complementary but not conflicting with routine duties.
In conclusion, MyPathologist is a novel electronic tool for clinical pathology consultation and represents an avenue for educating residents for their future as clinical consultants. In the long term, it is hoped that this system will improve utilization of the laboratory, with resulting improvements in health-care cost and patient care.
Footnotes
Authors’ Note
T.T. and E.S. contributed equally to this work.
Acknowledgments
The authors appreciate the ongoing involvement of the residents and faculty of the NorthShore Department of Pathology in this project.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by the NorthShore University HealthSystem Department of Pathology.
