Abstract
The practice of pathology is not generally addressed in the undergraduate medical school curriculum. It is desirable to develop practical pathology competencies in the fields of anatomic pathology and laboratory medicine for every graduating medical student to facilitate (1) instruction in effective utilization of these services for optimal patient care, (2) recognition of the role of pathologists and laboratory scientists as consultants, and (3) exposure to the field of pathology as a possible career choice. A national committee was formed, including experts in anatomic pathology and/or laboratory medicine and in medical education. Suggested practical pathology competencies were developed in 9 subspecialty domains based on literature review and committee deliberations. The competencies were distributed in the form of a survey in late 2012 through the first half of 2013 to the medical education community for feedback, which was subjected to quantitative and qualitative analysis. An approval rate of ≥80% constituted consensus for adoption of a competency, with additional inclusions/modifications considered following committee review of comments. The survey included 79 proposed competencies. There were 265 respondents, the majority being pathologists. Seventy-two percent (57 of 79) of the competencies were approved by ≥80% of respondents. Numerous comments (N = 503) provided a robust resource for qualitative analysis. Following committee review, 71 competencies (including 27 modified and 3 new competencies) were considered to be essential for undifferentiated graduating medical students. Guidelines for practical pathology competencies have been developed, with the hope that they will be implemented in undergraduate medical school curricula.
Introduction
In this article, we report the development and substance of consensus guidelines for competencies in anatomic pathology and laboratory medicine for
The teaching of pathology in medical education has traditionally been assigned to the preclinical years as a component of the basic science curriculum. The emphasis of preclinical pathology education has been on principles of pathogenesis and morphology, which are essential foundations for understanding the disease. Pathology is, however, a clinical discipline as well as a basic science discipline, with critical importance for patient care. Historically, students have had little formal experience in the medical school curriculum with the practice of pathology or its practical applications to patient care. 1 Electives in pathology have been generally available, but required experiences in pathology, specifically as related to patient care, have been rare. A recent survey of education leaders at American and Canadian medical schools revealed that fewer than half of the responding medical schools mandated some form of pathology experience in the clinical years. 2 The lack of undergraduate medical education in clinical applications of pathology was identified in a recent “white paper” sponsored by the College of American Pathologists and the Association of Pathology Chairs (APC). The article described the lack of formal pathology education as an important deficit that could lead to inappropriate use of anatomic pathology and laboratory services by future clinicians in the care of their patients. 3
Laboratory medicine, as a branch of the discipline of pathology, similarly lacks required and/or formal instruction. In a recent editorial, Laposata reported that only 9% of medical schools offer a separate course in laboratory medicine. 4 A recent national status report on laboratory medicine practice, sponsored by the Centers for Disease Control and Prevention (CDC), stated that “[p]hysician knowledge of laboratory tests and ability to order appropriately is complicated by … lack of formal education in laboratory testing”. 5 Wilson commented that “there are gaps in [medical school] education that defy common sense and reason, one of which is the lack of a requirement for formal education in laboratory medicine at all medical schools”. 6
There are several major purposes that would be served by required medical school experiences in the practice of pathology and laboratory medicine. First, medical students would develop knowledge and skills in appropriate ordering of laboratory tests and effective utilization of anatomic pathology for optimal patient care. Second, future physicians would develop applied knowledge of the role of pathologists as professional colleagues who can provide valuable consultation in diagnostic aspects of patient care. Finally, students would develop knowledge about the daily practice of pathology that would contribute to their consideration of pathology as a future career. Surveys of medical students’ attitudes have shown that the second-year pathology course “had little effect on medical students’ perceptions of pathology” as a career choice 7 and that, from students’ perspectives, pathology was “utterly invisible in clinical practice.” 1 In short, the lack of knowledge many students have about the daily practice of pathology hampers their consideration of pathology as a future career. 1,8 This issue is particularly important now, as pathology workforce analysis predicts a steady decline in number of pathologists beginning in 2015 and leading to a net deficit of more than 5700 full-time equivalent pathologists by 2030. 9 Enhanced recruitment of students into pathology is desirable to address this trend.
The pathology medical education community has been discussing these issues for some time, proposing enhanced elective offerings or required clerkships in pathology. In recent years, the concept of “competencies” in medical education has been introduced. Competencies were initially mandated for residency training across specialties by the Accreditation Council for Graduate Medical Education (ACGME) 10 and subsequently endorsed for medical school graduates by the Liaison Committee on Medical Education (LCME) in standards for medical school accreditation. Specifically, medical schools in the United States have been encouraged by the LCME (in ED-1-A) to state the “objectives of a medical education program …. in outcome-based terms that allow for assessment of student progress in developing the competencies that the profession and the public expect of a physician.” 11 In the 2009 report of the Association of American Medical Colleges-Howard Hughes Medical Institute (AAMC-HHMI) committee on the Scientific Foundations for Future Physicians, the authors recommended the concept of “competencies” (rather than courses) as the basis for preparing and assessing medical school graduates for the practice of medicine. 12 More recently, the AAMC identified 13 core “entrustable professional activities” that graduating medical students should be able to perform on the first day of residency, regardless of specialty choice. 13 The members of the AAMC panel adapted Frank and colleagues’ definition of competency as being “An observable ability of a health professional, integrating multiple components such as knowledge, skills, values, and attitudes. Since competencies are observable, they can be measured and assessed to ensure their acquisition.” 14
We believe that the concept of competencies is ideal for ameliorating the deficiency in practical pathology experiences in the medical school curriculum. Therefore, we have developed consensus recommendations for pathology competencies for graduating medical students, and in turn for the undergraduate medical school curriculum, which relate to direct patient management, that is, practical pathology competencies focused on utilization of pathology/laboratory medicine tests and interaction with pathologists/laboratory medicine physicians and scientists toward the ultimate goal of enhanced patient care. We recommend these competencies in both anatomic pathology and laboratory medicine for the “undifferentiated” graduating medical students, with particular emphasis on competencies for the future practicing clinician. In our consensus guidelines, we focus on the content of the competencies and not on the methods of instruction or assessment.
Materials and Methods
A national committee of experts was created, including anatomic pathology/laboratory medicine practitioners and experts in the discipline of medical education. Many of the participants were members of the Undergraduate Medical Educators Section (UMEDS) of the APC and/or the Group for Research in Pathology Education (GRIPE), both national organizations of pathology medical educators. All subspecialties of anatomic pathology and laboratory medicine, as well as curricular deans and education researchers, were represented on the committee. The common element linking all committee members was a keen interest in medical education.
The committee’s initial step was a literature review focused on potential recommendations for pathology and laboratory medicine competencies for the undifferentiated graduating medical students. Several publications over the last few years have proposed curricula and objectives for undergraduate medical education in pathology and related fields. Some of these publications expanded beyond the “basic science” pathological concepts to patient-related content and laboratory medicine. 15 -22 The competencies recommended by these authors provided a starting point for establishment of consensus guidelines.
The committee was organized in subcommittees, comprising individuals with expertise in the various subspecialties of practical pathology. Subcommittees met to formulate competencies in 9 domains, divided into 3 major general domains and their subcategories: (1) interactions with the departments of pathology and laboratory medicine; (2) anatomic pathology: surgical pathology/cytopathology, end-of-life issues (autopsy, death certificates, and forensic considerations); and (3) laboratory medicine: basic principles of laboratory testing, transfusion medicine, clinical chemistry and immunology, hematology, microbiology, and molecular diagnostics.
All competencies were formulated utilizing terminology recommended in standard education texts. 23,24 The draft competencies formulated by each subspecialty committee were reviewed by the entire committee for acceptance, rejection, or modification. The final list of proposed competencies was accepted by the entire committee, prior to submission to the broader medical education community for feedback, using a survey process. The committee’s final list included 79 proposed competencies, in the following domains: interactions with departments of pathology and laboratory medicine (5); anatomic pathology—surgical pathology and cytopathology (11) and end-of-life issues (8); laboratory medicine—basic principles of laboratory testing (18), transfusion medicine (7), clinical chemistry and immunology (12), hematology (6), microbiology (6), and molecular diagnostics (6).
A survey, including structured and open-ended questions, was created for other experts to review the proposed competencies. Respondents answered “yes,” “no,” or “uncertain” regarding concurrence/agreement with each competency. In addition, respondents were asked to comment about those competencies for which they had responded “uncertain” or “no” and to suggest additional competencies.
Members of the professional organizations that contain appropriate experts to review the competencies were targeted for survey distribution. These organizations consisted of pathology educators, including undergraduate medical educators (UMEDS and GRIPE), and residency program directors (the Pathology Residency Directors Section [PRODS] of the APC) as well as pathology department chairs (APC). We also planned to distribute surveys to members of organizations of nonpathology residency program directors in surgery, internal medicine, pediatrics, obstetrics and gynecology, anesthesiology, emergency medicine, family practice, and psychiatry. The reason for sending the survey to the nonpathology residency program directors was that these education leaders are stakeholders in the preparation of graduating medical students—with insight into competencies requisite for the clinician—in training.
Institutional review board approval was obtained at each committee member’s institution for distribution and analysis of the survey. Through contacts identified in each organization, a letter from the survey committee was distributed on 2 separate occasions through the organizations’ listservs soliciting anonymous participation in the survey (via a link to Survey Monkey) in late 2012 through the first half of 2013. The only demographic information collected on the respondents was professional organization affiliation. The residency program director organizations for internal medicine and pediatrics declined to distribute our letter on their listservs. Program directors in these specialties were solicited for their participation in our survey by individual committee members.
The collected survey responses were analyzed in an Excel spreadsheet. The results of the survey included quantitative data: the number of respondents and their organizational affiliations and the descriptive statistics (means and frequency distributions) for responses “yes”, “no”, and “uncertain” for each competency.
The survey responses also included narrative responses to open-ended questions, mostly explanations for responses of “no” and “uncertain” and suggestions for additional competencies. One member of our committee (IBH), an expert in qualitative methods, took the lead in qualitative analysis of these comments. 25 Using the constant comparative method associated with grounded theory, 26 she identified general themes across the 9 domains (eg, “better learned during residency training”) and categorized the comments by themes. Her initial qualitative analysis was independently reviewed by 2 other members of the committee (DTS and MSM) to confirm the validity and trustworthiness of the analysis and suggest modifications.
The overall committee reviewed the results and all comments. “No” and “uncertain” responses were batched as “nonagreement.” By committee decision, we determined that ≥80% agreement for a competency constituted consensus for adoption, although the committee would consider modification of the competency statement based upon review of comments. For any competency receiving less than 80% agreement, comments were reviewed to understand the rationale for the lower level of acceptance. Following committee discussion and review of comments, each competency was accepted, modified, or rejected. In a few cases, the committee decided to add a new competency following a review of comments, even when the new competency was suggested by only 1 respondent.
Results
Number of Respondents
There were 265 respondents. The vast majority (n = 224 [85%]) were pathologists (see Table 1). There were approximately 715 total pathologists approached in the different listservs, yielding an overall response rate of 31%. The response rates for the individual pathology organizations were GRIPE 57%, UMEDS 39%, PRODS 53%, and APC 28%. Only a small number of respondents (34 [13%]) were nonpathology residency program directors, and 10 of these respondents were also pathologists. This low response rate was disappointing although not surprising. Unfortunately, there were too few nonpathology participants to compare their responses as a separate cohort to the pathologists.
Affiliations of Survey Respondents.
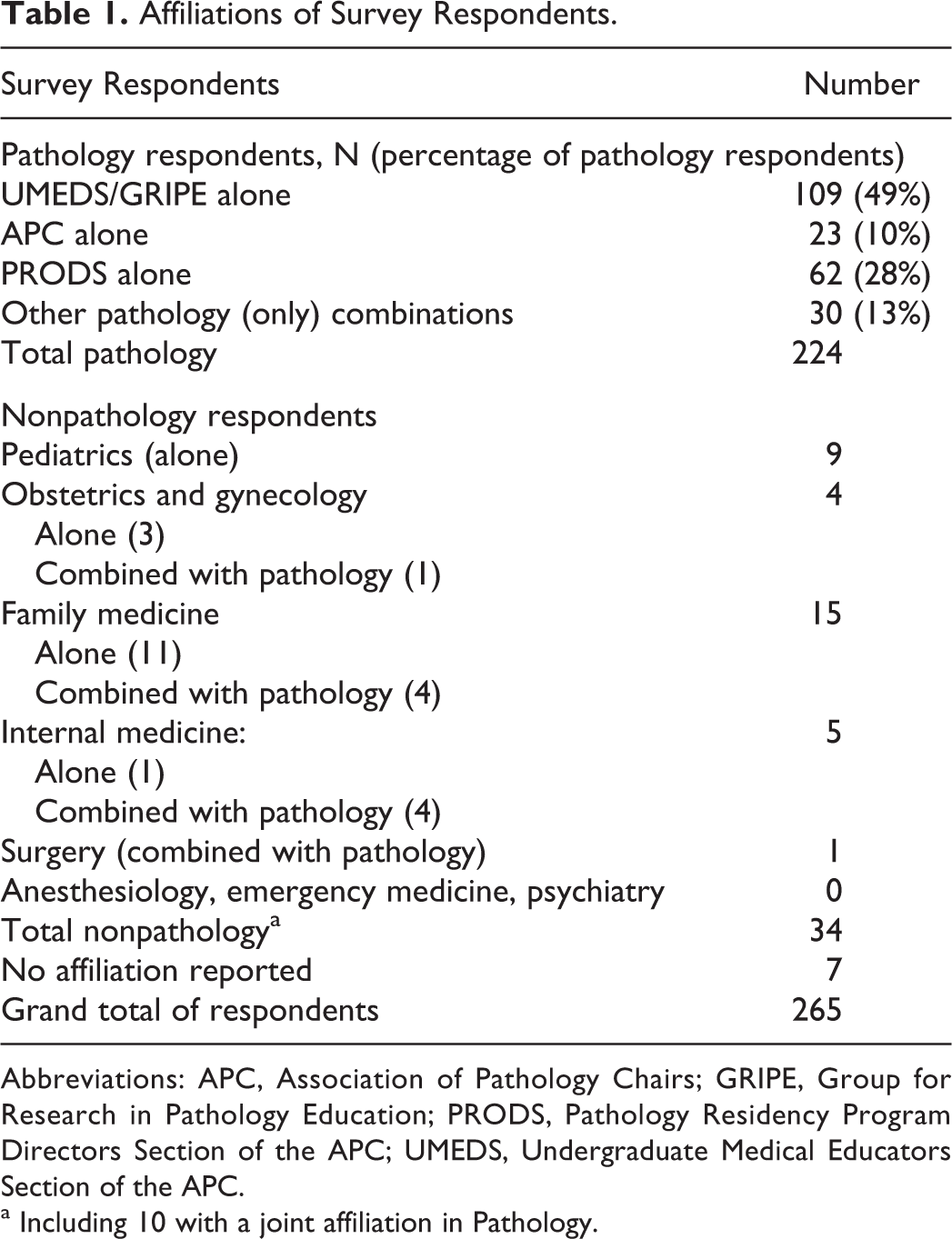
Abbreviations: APC, Association of Pathology Chairs; GRIPE, Group for Research in Pathology Education; PRODS, Pathology Residency Program Directors Section of the APC; UMEDS, Undergraduate Medical Educators Section of the APC.
a Including 10 with a joint affiliation in Pathology.
Level of Agreement With Competency Recommendations
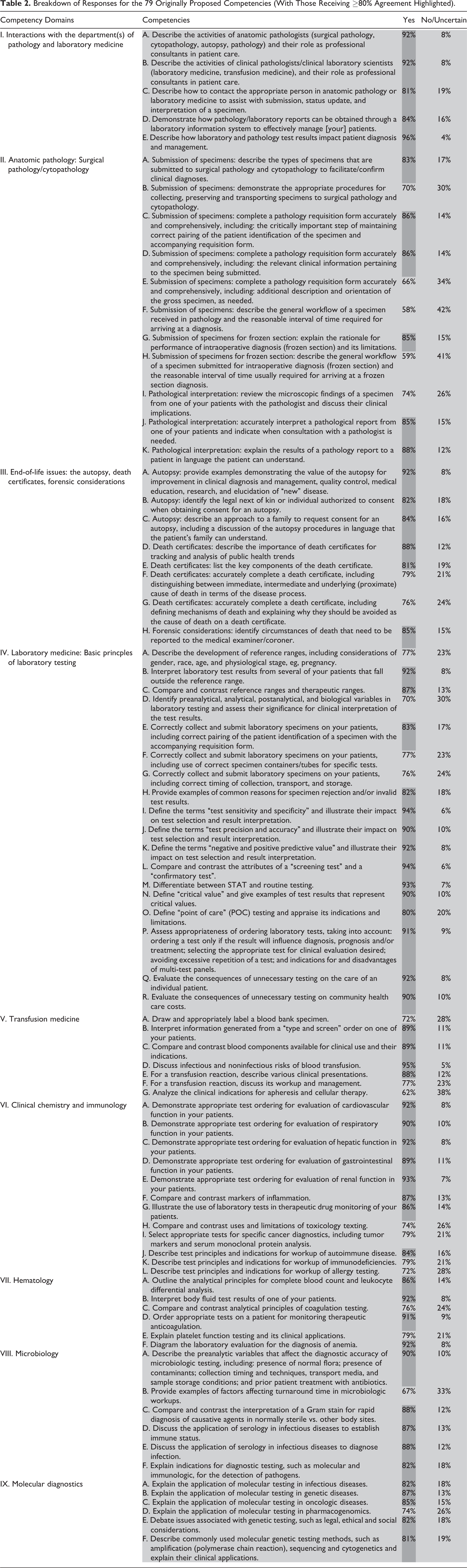
The breakdown of agreement categories across all competency domains is illustrated in Figure 1. Table 2 shows the details of responses for each of the 79 originally proposed competencies, grouped by domain, with those competencies achieving ≥80% agreement highlighted. All competencies were approved by a majority of respondents, and close to three-quarters (57 of 79; 72%) of the competencies reached the 80% agreement threshold for approval without requisite committee discussion. When looking separately at the 9 domains, we observed a range in the proportion of competencies that achieved the level of ≥80% agreement (Figure 2). For example, all suggested competencies were approved by ≥80% of respondents in interactions with the departments of pathology and laboratory medicine, compared with 55% of the competencies in anatomic pathology (surgical pathology/cytopathology). Explanations for the response rates were given in the comments provided by the respondents.
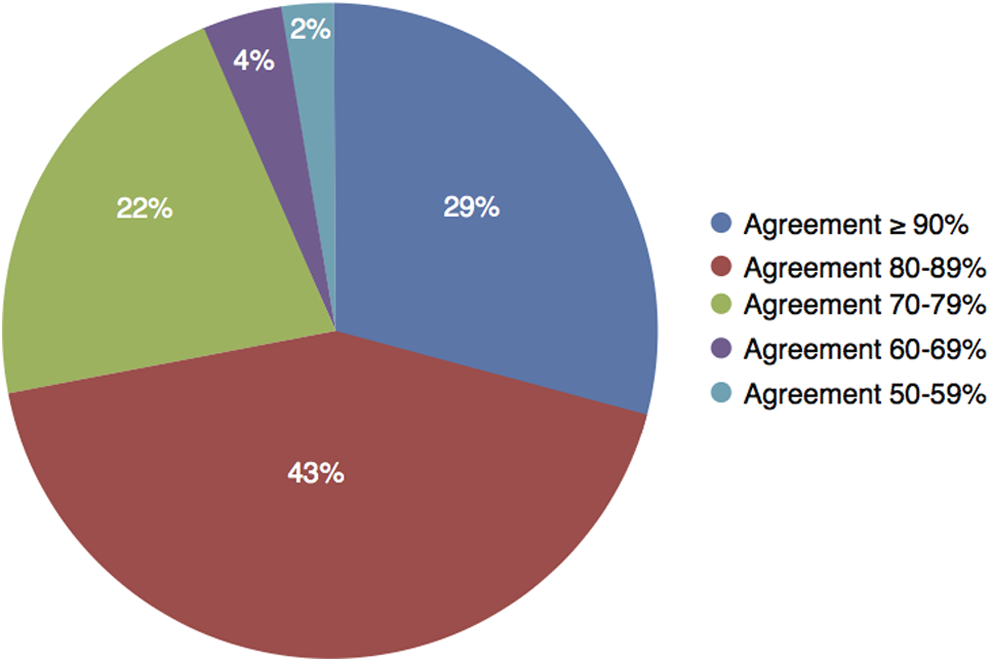
Breakdown of overall responses by percentage of agreement.
Breakdown of Responses for the 79 Originally Proposed Competencies (With Those Receiving ≥80% Agreement Highlighted).

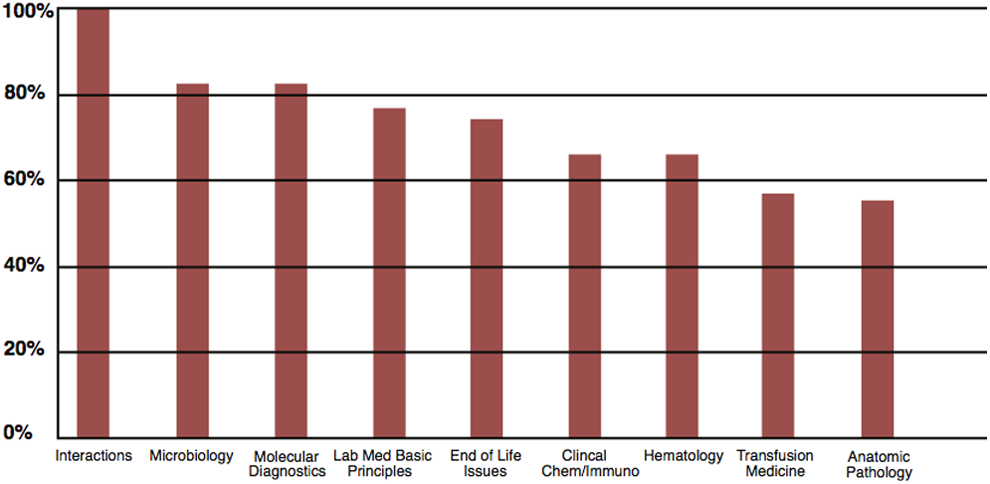
Percentage of the competencies in each category receiving ≥80% agreement.
Qualitative Analysis
There were 503 comments broken down by domains as interactions with the departments of pathology and laboratory medicine (65); anatomical pathology: surgical pathology/cytopathology (149); end-of-life issues (57); laboratory medicine: basic principles of laboratory testing (67); transfusion medicine (48); clinical chemistry/immunology (59); hematology (29); microbiology (15); and molecular diagnostics (14). The sheer number of comments and the thoughtfulness of the commentary testified to the respondents’ great level of interest in this competencies project. It was determined that analyzing responses in relationship with membership in pathology organizations was too complex and not helpful. Therefore, the responses were analyzed as a single group.
Most comments related to “uncertain” or “no” responses providing explanations for respondents’ lack of approval for a competency. The themes in the qualitative analysis that accounted for the most frequent comments were “better learned in residency,” “not essential/or necessarily expected for graduating medical students,” and “it is important to effectively communicate with pathologists.”
The committee had previously decided that with ≥80% agreement, a competency would be included in the consensus list of essential competencies but might, however, be subject to modification following review of comments. An example of a modified competency, which had received 82% agreement, was in the domain of interactions with the departments of pathology and laboratory medicine: “describe how to contact the appropriate person in anatomic pathology or laboratory medicine to assist with submission, status update, and the interpretation of a specimen.” In the qualitative analysis of comments, 19 of the 21 comments about this competency fit into the theme, “better learned during residency training in specific hospital contexts because systems vary among hospitals.” The committee determined that rewording of the competency was warranted. The wording of the competency was changed to “use one of your cases to demonstrate knowledge that pathologists and clinical laboratory scientists are available for consultation about interpretation of specimens.” In another case, in the domain of clinical chemistry/immunology, the competency, “demonstrate appropriate test
Qualitative analysis was critical for evaluation of those competencies receiving less than 80% approval. In some cases, the comments suggested approaches to enhance acceptability for inclusion. An example was in the domain of anatomical pathology: surgical pathology/cytopathology. There was 58% approval for the competency statement: “describe the general workflow of a specimen received in pathology and the reasonable interval of time required to arrive at a diagnosis.” The majority of comments about this competency fit into the theme of “not essential/or necessarily expected for graduating medical students” (eg, “knowing the turnaround time is important, but I don’t think it is necessary for a medical student to understand the inner workings of the pathology laboratory.”) Following review of the comments, the committee decided to reword this competency to “describe the reasonable interval of time required for arriving at a diagnosis of a specimen received in pathology.”
Several competencies receiving a low approval rating were deleted by the committee, following review and qualitative analysis of the comments, for example, in anatomic pathology, “complete a pathology requisition form accurately and comprehensively, including additional description and orientation of the specimen, as needed” (66% agreement) and in clinical chemistry and immunology “describe test principles and indications for workup of allergy testing” (72% agreement). In retrospect, the committee agreed with the significant number of respondents who commented, for the anatomic pathology competency, that medical students are rarely in the position of orienting a surgical specimen, and, for the clinical chemistry and immunology competency, that principles of allergy testing may be too specialized for the graduating medical student.
Rarely, the committee exercised its discretion to retain a competency without modification, despite its having received <80% approval, for example, “review the microscopic findings of a specimen from one of your patients with the pathologist and discuss their clinical implications” (74% agreement). In this case, the strong consensus of the committee was that this was an essential experience that could provide medical students with an appreciation of the role of anatomic pathology in the care of their patients.
A few times the committee agreed to include an additional competency in the consensus recommendations, even though it was suggested by only 1 respondent. An example is in the domain of interactions with the departments of pathology and laboratory medicine: “illustrate how clinical laboratory/pathology consultations may assist in devising the most efficient and cost effective path to diagnosis in specific patients or clinical situations.”
Overall, following committee review, 5 (6%) competencies were deleted, 27 (34%) competencies were modified, and 3 (4%) competencies were added. Additionally, in two instances several competencies were collapsed into a single comprehensive competency (test selection for different organ systems and applications of molecular testing). Therefore, from an original 79 suggested competencies, following review of survey results, including the descriptive statistics and qualitative analysis of comments, there was a final set of 71 competencies considered to be essential for undifferentiated graduating medical students. The list of these competencies is included in Table 3.
Final Consensus Recommendations for Practical Pathology Competencies for Undifferentiated Graduating Medical Students.

Discussion
The practice of pathology and its concrete application to patient care are not commonly addressed in American medical school curricula, a situation that provided the rationale for undertaking this competencies project.
Pathology is one of the major “diagnostics” disciplines, with essential contributions to patient management. Students must be educated in proper interactions with physicians/clinical laboratory scientists in anatomic pathology and laboratory medicine to understand practical implications for patient assessment and management, such as what potential information pathology services can provide, the intrinsic limitations of various clinical tests, optimal ways specimens should be prepared and delivered for evaluation, and reasonable expectations for turnaround time. Of particular importance today is the service that specialists in Laboratory Medicine can provide in recommending efficient and cost-effective strategies for laboratory diagnosis. A valuable lesson from experience with pathology services is the recognition that pathologists are professional colleagues and consultants who play an important role in health care teams. 27 A recent study of pathology residency training programs stresses the importance of preparing team-trained pathologists who collaborate with their interdisciplinary colleagues in providing medical care. 28 By extension, the education of medical students toward multidisciplinary team-based health care should include interactions with physicians in the diagnostic disciplines such as pathology. Exposure to pathology practice can counter negative stereotypes and demonstrate the pathologist’s ongoing contribution to patient care. Practical experience in pathology practice can also contribute to informed residency program choices.
Support for these purposes is provided by the LCME ED-17 standard: “educational opportunities must be available in a medical education program in multidisciplinary content areas (eg, emergency medicine, geriatrics) and in the disciplines that support general medical practice (eg, diagnostic imaging,
The purpose of this project was to develop consensus recommendations for practical pathology competencies—in both anatomic pathology and laboratory medicine—that
During the last few years and following the development of our project, a separate national effort to create competencies for pathology in undergraduate medical education was initiated under the auspices of the APC. 29 The proposed requisite pathology content was categorized into 3 broad competencies: disease mechanisms/processes, organ system pathology, and diagnostic medicine and therapeutic pathology. Academic pathologists in UMEDS were asked to submit learning objectives targeted to general learning goals within the competencies, which were edited by a select learning competencies editorial team and posted in an open-access online document. 30 Subsequent expansion of this “living document” is anticipated by continuing contributions by pathologists of more detailed subobjectives and specific examples for use in medical school curricula. Competency 3 (diagnostic medicine and therapeutic pathology) is analogous to the product coming out of our study and consists of 11 topics that cover similar categories to our domains. In its current form, it already provides considerable granularity within content objectives and promises to provide more detail with ongoing participation. This work is a valuable contribution to the development of pathology-related content in integrated medical school curricula. Our final proposals differ by being the result of a consensus of a large group of pathologists using rigorous methods to analyze data, with the goal being a broad competency-based curriculum designed for individualized implementation by each medical school.
Even more recently, exit competencies in pathology and laboratory medicine for graduating medical students were published by the Canadian Association of Pathologists. 31 Developed by the organization’s education group, the competencies were designed to be clinically focused and applicable to every medical graduate. The creation of this document demonstrates the recognition across the North American borders of the need for exit competencies in pathology. The final Canadian document includes 37 competencies: 11 “foundational” competencies (universally applicable to all areas of clinical practice), 4 competencies related to biopsy or cytology investigation, 3 for hematology practice, 5 for transfusion medicine practice, 5 for microbiology/infectious disease practice, 4 for biochemical testing of patients, 3 related to genetic testing, and 2 for the management of postmortem patients. Many of these competencies are similar in content to our competencies although there is a more general focus than our final list. The Canadian document places a valuable emphasis on communication—with pathologists, other members of the health team, and patients. This was a feature that was also commented on by many of the pathologists responding to our survey. Some of the differences in the 2 documents include the fact that our listing emphasizes that students obtain competencies covering a more global understanding of the role of pathologists and pathology as part of the clinical team (our section I). We have an expanded autopsy section that includes an understanding of death certificate, next of kin issues, and the role of the medical examiner (our section III). More practical aspects of specimen submission are included in many of our sections. The wording of some of the Canadian competencies requiring that the students “order” tests or procedures would not be feasible in the United States for developing measurable or observable behaviors, as discussed previously. While the procedures are not described by which the proposed competencies that were developed by the education group were endorsed by the Canadian Association of Pathologists, they do not appear to have gone through the broad survey with input from more than 200 pathologists and the extensive qualitative evaluation that yielded our final list of recommended competencies.
Other medical specialties and subspecialties have also addressed the issue of establishing a national core curriculum in their respective areas by attempting to define a minimum body of knowledge that should be required of all graduating medical students, regardless of their eventual specialty. 32,33 A curriculum designed by radiologists is most relevant to our efforts, since radiology is also a diagnostic discipline that supports general medical practice yet is infrequently incorporated into the medical school curriculum as a required clerkship. A recent article reported the results of a survey designed by academic radiologists and distributed to residency program directors in several clinical specialties. 33 The respondents were asked to determine which topics of the 28 proposed competencies should be considered essential core radiology knowledge and skills to be learned prior to graduation from medical school. Ten of the 28 skills were considered essential by 80% or more of all respondents. Not surprisingly, 6 of these 10 topics are analogous to our final pathology competencies in Table 3, including “communicate relevant clinical history when ordering a radiologic study” (our section II D), “ability to choose the most appropriate radiologic study for workup of common clinical situations in your field” (our section II A), “basic knowledge of the limitations of radiologic studies” (our section IV D, G-H), “ability to effectively communicate with patients about radiologic studies and procedures” (our section II J), “ability to interpret a radiologist’s report” (our section II I), and “ability to use radiologic findings to narrow a differential diagnosis” (our section I E). The common interests of pathology and radiology may facilitate introduction of our respective competencies into the medical school curriculum by collaborative effort.
Given the continuum that exists between the graduating medical student and the postgraduate year 1-level resident, we were interested in comparing our proposed list of final competencies with the ACGME level 1 (or equivalent) Milestones expected of incoming residents. We reviewed the milestones for several clinical specialties that are the major stakeholders in the adequate preparation of medical students for clinical practice; general surgery, 34 internal medicine, 35 obstetrics and gynecology, 36 pediatrics, 37 and emergency medicine. 38 We also looked at the pathology milestones, 39 although our proposed competency guidelines were not designed for the medical student planning to enter a pathology residency. Table 4 matches the specific Level 1 milestone of each discipline with the proposed pathology competencies (from Table 3) that address the topic. Not surprisingly, the number of pathology ACGME milestones (N = 16) that has corresponding pathology competencies in our consensus guideline is much higher than the number of milestones in the other clinical specialties that in some way relate to a corresponding pathology competency (general surgery = 4; internal medicine = 6; obstetrics and gynecology = 3; pediatrics = 2; emergency medicine = 3). The most frequent themes of the milestones in the nonpathology specialties that have some relation to pathology include test ordering in the clinical laboratory (test selection, understanding test performance characteristics, interpretation of test results, awareness of errors/variability, and emphasis on cost-effective care), recognition of interdepartmental teams in patient care, and communication of results to patients. There is no specific mention of pathology. Proper submission of specimens for anatomic pathology and the clinical laboratory is not addressed directly. The indications for STAT testing and the importance of critical values and their proper management are not described. None of the specialties address the autopsy or forensic considerations. The observation that some topics deemed important by pathologists are not always recognized by other specialties may introduce challenges for their introduction into the medical school curriculum. It also points out the need for ongoing discussions between pathology and other specialties to better understand why this discrepancy exists.
ACGME Level 1 Competencies in Selected Clinical Specialties Matched with Their Corresponding Practical Pathology Competencies.
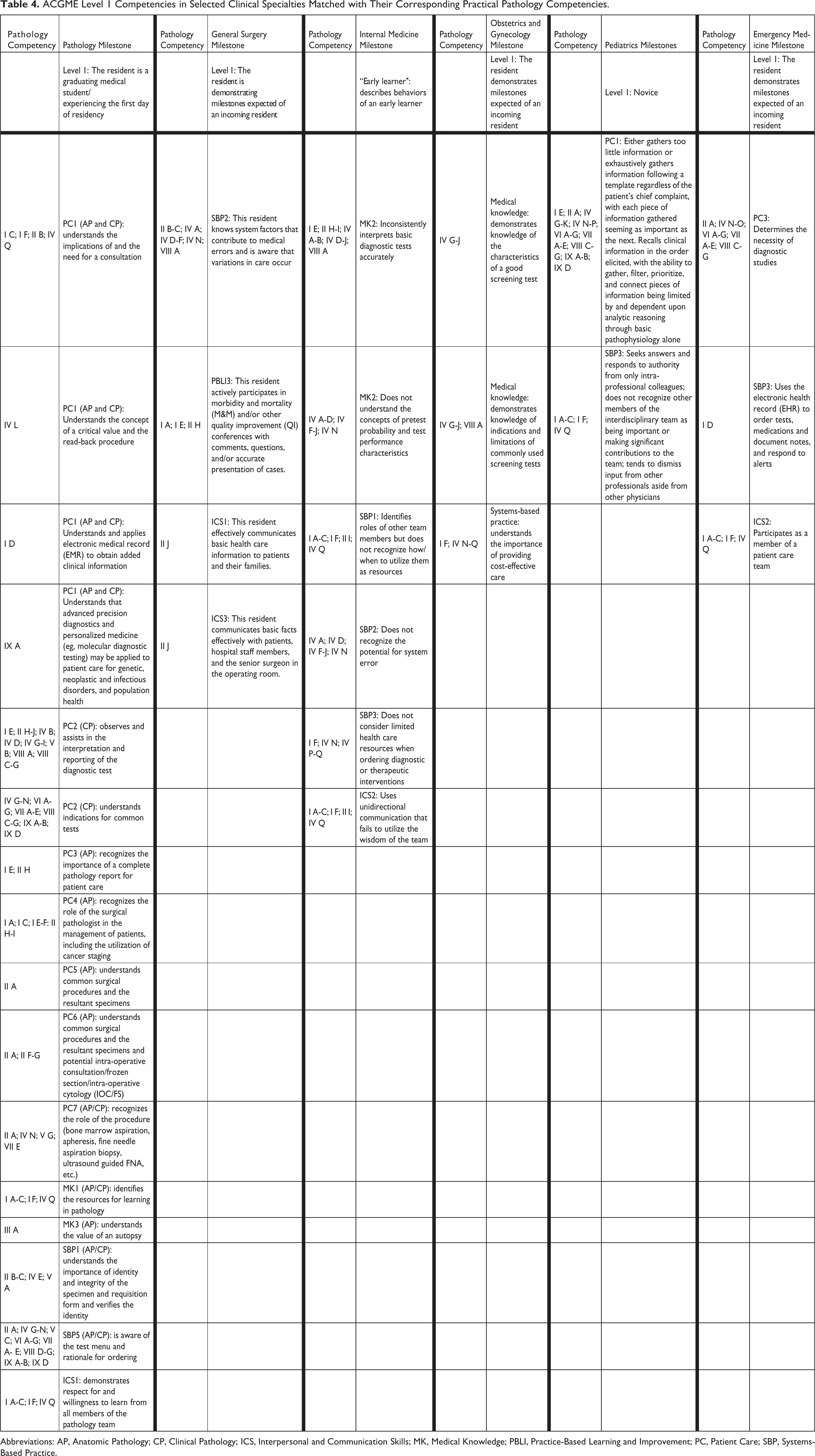
Abbreviations: AP, Anatomic Pathology; CP, Clinical Pathology; ICS, Interpersonal and Communication Skills; MK, Medical Knowledge; PBLI, Practice-Based Learning and Improvement; PC, Patient Care; SBP, Systems-Based Practice.
Finally, we considered how our proposed pathology competencies related to the AAMC core entrustable professional activities (EPA) framework. 13 We identified several of these broad medical school graduation requirements to which the pathology competencies are integral: EPA 3: recommend and interpret common diagnostic and screening tests; EPA 7: form clinical questions and retrieve evidence to advance patient care; and EPA 9: collaborate as a member of an interprofessional team.
The purpose of our project was to develop competencies considered to be essential for
We did not intend to prescribe the means for students to achieve these competencies but rather to encourage each medical school to develop instructional programs consistent with its curriculum and culture. However, several ideas that have been suggested for development of these competencies include required laboratory medicine courses in the clinical years; case-based small group discussions that incorporate questions about which laboratory tests to order and why; encouraging review of biopsies/surgical specimens on students’ patients in a longitudinal care module; incorporating instruction and assessment of the pathology competencies into requirements in surgery, obstetrics and gynecology, internal medicine, and pediatrics clerkships; and providing required clinical rotations in pathology where the student acts as a pathologist in a health care team. Methods of assessment, including standard setting, are beyond the scope of our study but are clearly an important agenda for future work. 24,40,41
Some respondents to the survey expressed concern that pathologists would not have the resources and time to help students develop these competencies. However, it is not expected that all of the competencies would be handled by pathologists—rather that they be addressed in the medical school curriculum by the most appropriate/available educators and in the most effective instructional formats. Most emphatically, these competencies are not designed for achievement only in the preclinical curriculum but are intended for instruction and assessment throughout medical school.
In summary, the consensus recommendations for practice-based pathology competencies presented here are based on expert review and consensus within the medical education community. The competencies were formulated to provide recognition of and knowledge about the essential role of pathology in medical practice, and in turn, for enhancement of patient care. We encourage review of these recommendations and adoption of the practical pathology competencies into medical school curricula, with the hope that instructional programs can be designed and implemented at the local level in each medical school to ensure student development of these competencies.
Footnotes
Acknowledgments
The authors wish to thank Regina Kreisle, MD, PhD, for participation in study design and providing expert advice about IRB submission, Deborah S. Shinn, PhD, for valuable administrative support, and all the respondents to the survey.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
