Abstract


Introduction:
Diastasis recti (DR) is defined by the European Hernia Society (EHS) as an abnormal separation between the rectus abdominis muscles >2 cm caused by thinning and widening of the linea alba. 1 Common in postpartum women and middle-aged men, it causes abdominal pain and cosmetic concerns, impacting quality of life. Conservative treatments include physiotherapy and abdominal binders. Surgical management is indicated for persistent symptoms, concomitant hernias, or cosmetic reasons. Traditionally, DR was surgically managed by plastic surgeons as part of abdominoplasty. However, with the advent and increasing expertise in minimal invasive techniques, other procedures, such as SCOLA (Laparoscopic Subcutaneous Onlay Aponeuroplasty), eTEP (enhanced Total Extra Peritoneal), ELAR (Endoscopic Linea Alba Reconstruction), and REPA (Pre-Aponeurotic Endoscopic Repair), have been attempted in specific cases. SCOLA is technically easy to perform and feasible. The current EHS and Swedish guidelines suggest plication +/− mesh repair either through open or minimally invasive approach, to be a recommended option for repair, in patients with postpartum status, presence of symptoms, a large defect size (>5 cm), completion of core strengthening exercises for a minimum period of 6 months, and completed family.1,2
Methodology:
We report the case of a 32-year-old postpartum female presenting with a complaint of abdominal bulge for 2 years, which was more pronounced on straining, standing, coughing, and resolved on lying down. It was associated with recurrent dull aching pain, with acute severe episodes since the last 6 months. No history of nausea, vomiting, abdominal distension or fecal/urinary incontinence. She had two normal vaginal deliveries, the last was 4 years ago. She had been doing abdominal strengthening exercises for over a year. Clinical examination revealed a 10 × 8 cm bulge predominantly in the lower abdomen tapering in the supraumbilical region, with a positive cough impulse. A computed tomography scan demonstrated an inter-rectus distance of 6 cm, with a small umbilical hernia of leading to a diagnosis of DR. The condition was classified using the EHS classification system as T1 (postpartum), D3 (>5 cm inter-rectus distance), and H1 (with umbilical hernia). 1 Per EHS guidelines, this patient was deemed a suitable candidate for repair of DR, as she was symptomatic for divarication with umbilical hernia, completed family, last child 4 years ago, and no resolution despite core strengthening exercises. She was planned for SCOLA with mesh repair.
Results:
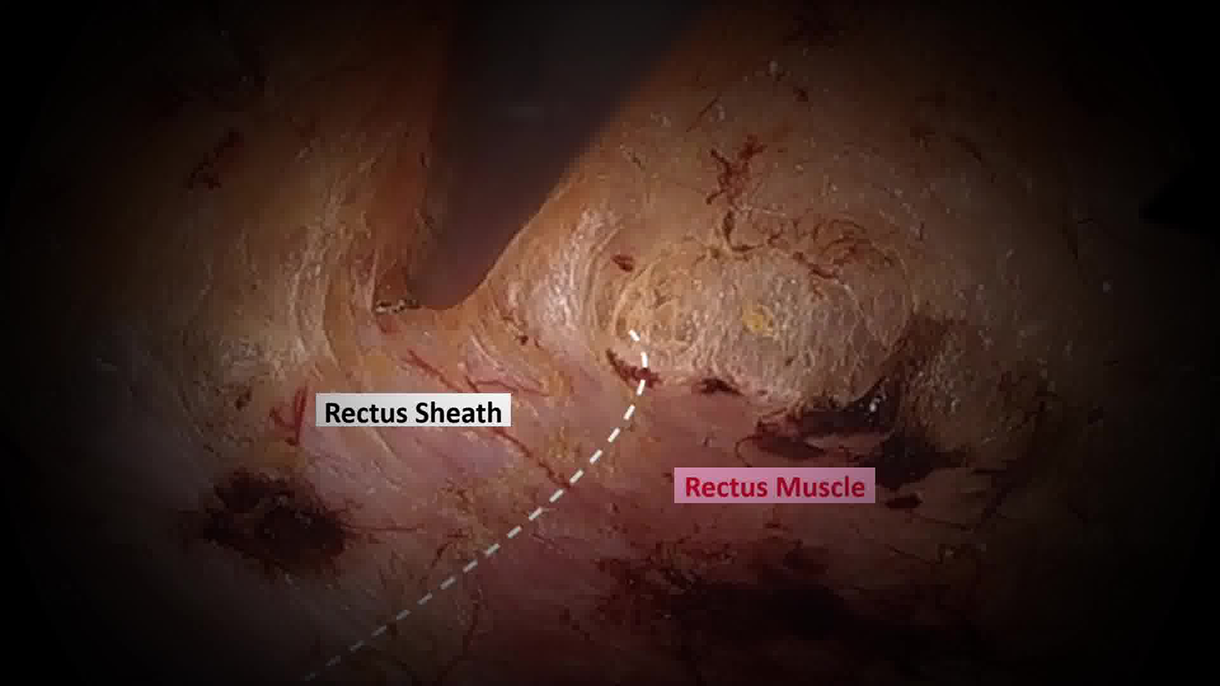
This video demonstrates the Laparoscopic Subcutaneous Onlay Aponeuroplasty (SCOLA) technique for repairing DR. Key steps include creating a subcutaneous pocket anterior to the anterior rectus sheath, closing the hernial defect, followed by plication of the diastasis using non-absorbable braided sutures, mesh reinforcement (mid-weight polypropylene of 20*10 cm2), and umbilicus fixation. Each step is thoroughly illustrated, highlighting key anatomical landmarks, technical nuances, and critical points to optimize outcomes. The patient recovered well; her drain was removed on postoperative day 2, and she was discharged on the same day. At 21 months of follow-up, she is doing well without any recurrence.
Conclusion:
The SCOLA technique offers a safe and feasible minimally invasive option for treating DR, providing both functional and aesthetic benefits over traditional methods.
All India Institute of Medical Sciences, New Delhi.
The authors declare that there have been no commercial associations, financial relationships, or other conflicts of interest over the past 2 years that could be perceived as influencing or creating a conflict in connection with the content of this video.
The authors have received and archived patient consent for video recording and publication in advance of video recording of the procedure.
Runtime of video: 9 min 38 secs
