Abstract
Objective. To assess the impact of chronic illnesses on risk behaviors and psychosocial adjustments among adolescents during the COVID-19 pandemic in Thailand. Methods. A cross-sectional study was conducted between June 2021 and September 2022, including adolescents aged 10 to 18 years. Participants completed the Thai Youth Risk Behavior Survey and the Strengths and Difficulties Questionnaire (SDQ). Data were analyzed using descriptive statistics, Student’s t-test, Chi-square test, and logistic regression. Results. Adolescents with chronic illnesses (n = 120) were more likely to exhibit risk behaviors related to violence (38.3%) and mental health issues (18.3%). They also scored higher on total difficulties (mean = 12.23, SD = 5.14) and emotional symptoms (mean = 3.08, SD = 2.45) than the healthy group (n = 120). Conclusion. During the COVID-19 pandemic, adolescents with chronic illnesses in Thailand demonstrated increased risk behaviors related to violence and mental health issues, highlighting the need for tailored interventions.
What We Already Know
Over the years, there’s been a notable evolution in the risk-taking behaviors exhibited by adolescents.
Prior to the COVID-19 pandemic, adolescents diagnosed with chronic medical conditions were observed to engage in risk-taking behaviors at a frequency either equivalent to or greater than their peers without such conditions.
The COVID-19 pandemic, with its associated lockdowns and public health mandates, has further transformed adolescent behaviors, exacerbating certain risk-taking behaviors.
What This Article Adds
This study provides a direct comparison between adolescents with chronic diseases and their healthy counterparts in the context of the COVID-19 pandemic in Thailand.
Despite the expected negative implications of the pandemic, adolescents with chronic conditions demonstrated a stronger prosocial behavior and healthier lifestyle choices, suggesting a resilience possibly developed from managing their chronic conditions.
The research identifies specific areas, such as the prevalence of violence and mental health challenges, where tailored interventions can be targeted for adolescents with chronic conditions during global crises.
Introduction
The COVID-19 pandemic has brought significant disruptions to the lives of adolescents worldwide, particularly affecting their health behaviors and psychosocial adjustments. 1 In Thailand, the government’s strict lockdown measures, school closures, and social distancing policies have impacted adolescents’ daily routines, social interactions, and access to healthcare services. 2
Previous research indicates that during the pandemic, many adolescents reported heightened depressive symptoms, anxiety, fear, and negative emotions. 3 These feelings were further amplified by increased loneliness, burnout, and reduced school bonding and engagement. 1 Recent study found that the current rates of anxiety and depression symptoms were 28.3% and 30.8%, respectively, among adolescents during the COVID-19 pandemic. 4 The severity of the disease, high mortality rates, and applied preventive measures exacerbated adolescents’ fears and affected their learning processes. 5
Adolescents with chronic conditions might experience more severe impacts from the pandemic and lockdown compared to their healthier counterparts. Already burdened with their health challenges, adolescents with chronic diseases were further subjected to the psychosocial stressors introduced by the pandemic. Prior to the COVID-19 pandemic, research indicated that adolescents with chronic diseases participated in risk-taking behaviors either equally or more frequently than their healthy counterparts.6,7 The COVID-19 lockdown led to marked reductions in physical activity8,9 and study time for adolescents. 10 Additionally, numerous studies highlight a surge in screen time compared to the periods before lockdown.9-12
Alterations in their behavior, particularly the uptick in risk-taking, may have profound implications on their health and how they manage their conditions. Studying these behaviors during the pandemic offers a window into the adaptability and resilience of these adolescents. Insights gleaned help in formulating targeted interventions to aid them during such challenging times. As global threats from emerging health crises grow, learning from the present pandemic is crucial for shaping preparedness and response for future events.
This study examines risk-taking behaviors among Thai adolescents with chronic diseases during the COVID-19 pandemic. Our goal is to provide insights that assist health practitioners, educators, and policymakers in developing interventions to address the complex challenges these adolescents face.
Methods
Participants
We conducted a cross-sectional study from June 2021 to September 2022. The inclusion criteria for the chronic illness group were adolescents aged between 10 and 18 years with chronic medical conditions requiring long-term medication for more than 3 months, who have independent daily-living skills and attend school. Patients were enrolled from the specialty pediatric outpatient clinic at Chiang Mai University Hospital, the largest tertiary care hospital in northern Thailand. For the healthy group, the inclusion criteria were adolescents aged between 10 and 18 years who visited the outpatient department with no chronic medical condition, cognitive impairment, or severe mental health problem. In both groups, participants and their legally acceptable representatives provided written informed consent for study participation. The exclusion criteria for both groups were a language barrier preventing reading or understanding the Thai language and failure to complete the questionnaire. Following eligibility verification and acquiring parental written consent, eligible adolescents assented and completed questionnaires through a mobile-accessible electronic form using a QR code. The electronic form was hosted on a secure server with access restricted to the research team. Each participant was provided with a unique, single-use QR code to prevent repeated answers. The study was approved by the Ethics Research Committee of the Faculty of Medicine, Chiang Mai University (Approval No. 193/2021).
Data Collection
The questionnaire captured demographic details such as age, sex, body weight, height, educational status, parents’ marital and educational status, and family income. All participants completed the self-reported, computer-based Thai Youth Risk Behavior Survey (Thai-YRBS) and the Strength and Difficulties Questionnaires (SDQ) to gage risk-taking behaviors and psychosocial challenges.
The Thai-YRBS used in this study was translated from the 2021 version of the U.S. CDC’s Youth Risk Behavior Survey, which is updated biennially. 13 The YRBS has been widely used in the United States to assess adolescent risk behaviors for many years . 14 For use in this study, the 2021 YRBS was translated into Thai and back-translated into English to check for accuracy and equivalence. Although a new validation study was not conducted, the YRBS has previously undergone rigorous adaptation and translation for use with Thai adolescents, demonstrating good cultural validity and conceptual equivalence. 15 It has been used in several previous studies of Thai adolescent risk behaviors.16,17 The survey focuses on 6 categories of health risk behaviors in adolescents, including:
Unintentional injuries: at least 1 episode of riding in a car/other vehicle when drinking alcohol or at least 1 episode of texting or using electronic devices while driving a car/other vehicle.
Violent acts: at least 1 episode of physical fight, carrying a weapon, being in an unsafe environment, or dating violence.
Mental health problems: at least 1 episode of depressed mood and suicide-related behaviors in the past 12 months.
Current tobacco and alcohol use: at least one episode of smoking or drinking an alcohol-containing beverage in the past 30 days.
Sexual behavior problems: at least 1 episode of having sexual intercourse, unprotected at last sexual intercourse.
Unhealthy dietary behaviors: missing breakfast more than 1 day per week or eating fruit and vegetables less than once per day; physical inactivity: exercise <3 days per week; excessive screen time: screen time use greater than 2 hours per day; inadequate sleep time: sleep <8 hours per night.
The Strengths and Difficulties Questionnaire (SDQ-Thai version) is a brief self-reported tool designed for children and young people to assess prosocial and other behavioral problems. 18 The questionnaire comprises 25 items, each scored from 0 to 2 (not true/somewhat true/certainly true), and is classified into 5 subscales: emotional symptoms, conduct problems, hyperactivity/inattention, peer relationship problems, and prosocial behavior. 19 The “total difficulties” scale is derived from the sum of the scores from the 4 difficulty subscales. Except for the prosocial behavior subscale, higher scores indicate more behavioral problems. The SDQ has demonstrated a sensitivity of 84.8% and a specificity of 80.1%. 20
Statistical Analysis
We used the SPSS 22.0 software for data analysis. Descriptive statistics, including mean, standard deviation (SD), and percentages, characterized the demographic and clinical attributes. The Student t-test and the Chi-square test were used to compare continuous and categorical variables, respectively, as appropriate. Odds ratios (OR) and adjusted odds (aOR) with a 95% confidence interval (CI) were calculated. A P-value of <.05 was considered statistically significant.
Results
The study enrolled 240 adolescents. In the chronic disease group (n = 120), there were 17 (14.17%) adolescents with attention-deficit/hyperactivity disorder (ADHD), 11 (9.17%) with asthma, 17 (14.77%) diabetes mellitus, 31 (25.53%) systemic lupus erythematosus (SLE), 28 (23.33%) thalassemia, and 16 (13.33%) congenital heart disease. The baseline characteristics of both the chronic disease group and the healthy group can be found in Table 1. Adolescents with chronic diseases and healthy adolescents showed similarities in gender, mean age, BMI, and parental status.
Baseline Characteristics Between Chronic Diseases and Healthy Adolescents.
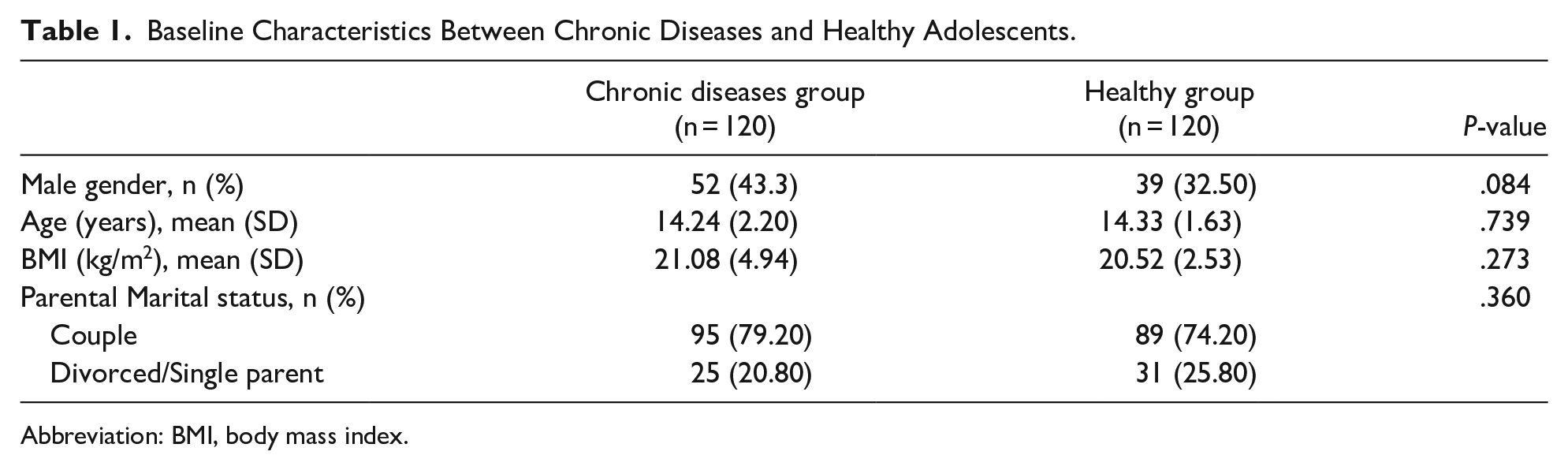
Abbreviation: BMI, body mass index.
The chronic diseases group exhibited the following prevalence of risk-taking behaviors: excessive screen time 74.2%, inadequate exercise 65.8%, interpersonal violence 38.3%, inadequate sleep time 37.5%, unintentional injuries 20.8%, alcohol exposure 20.0%, mental health problems 18.3%, sexual behavior problems 5.0%, tobacco use 3.3%, and substance use 0.8%.
When adjusted for age, gender, BMI, and parental status, adolescents with chronic illnesses were at a significantly higher risk for mental health problems (aOR 27.78, 95% CI 3.59-215.10) compared to healthy adolescents, but a similar risk in unintentional injury, interpersonal violence, substance use, and sexual behavior as shown in Figure 1A. However, healthy adolescents were at higher risk for physical inactivity (aOR 0.21, 95% CI 0.10-0.43), excessive screen time (aOR 0.07, 95% CI 0.02-0.24), and inadequate sleep time (aOR 0.26, 95%CI 015-0.47) than the chronic illness group.

Risk behaviors among adolescents in Northern Thailand. (A) Bar graph comparing the prevalence of risk behaviors between healthy controls and those with chronic illnesses. (B) Heatmap representation of the prevalence of risk behaviors across specific chronic diseases. *P < .01. **P < .001 indicates statistical significance compared to the Healthy Control Group.
Within the chronic group, individuals with SLE reported the highest incidence of mental health problems (35.5%). The prevalence of risk behaviors for other specific chronic diseases is depicted in Figure 1B.
Table 2 displays the SDQ scores. Compared to their counterparts, the chronic disease group scored higher on the total difficulty, emotional problems score, and peer problems score than their counterparts. Conversely, they exhibited a better prosocial behavior score.
Psychosocial Adjustment in Adolescents With Chronic Illness Compared to Healthy Controls.

Discussion
The COVID-19 pandemic has significantly challenged adolescents, especially those with chronic conditions, highlighting crucial disparities compared to their healthier peers and changes from pre-pandemic behavior patterns. Our study confirms that these adolescents faced heightened mental health challenges during the pandemic, echoing findings from previous studies have shown that during the pandemic, adolescents with chronic diseases and other vulnerable groups experienced persistently high levels of fear, anxiety, and hopelessness,3,21 emphasizing the urgent need for effective early interventions.
Our study noted a lower prevalence of mental health issues (18.3%) among adolescents with chronic conditions during the pandemic compared to pre-pandemic data, which reported a significantly higher rate (38.5%). 22 This decrease, despite the global health crisis, prompts further investigation. Potential factors include enhanced external support systems, improved coping mechanisms, or a normalization of shared pandemic-related struggles.
Violence emerged as a significant risk among adolescents with chronic illnesses, increasing from a pre-pandemic rate of 9.3%. 22 The restrictive conditions of home isolation, compounded by familial and financial stresses, likely worsened these behaviors. This observation aligns with trends seen in other vulnerable youth groups during the pandemic,23-25 underscoring the critical need for targeted and timely interventions.
Despite global trends toward increased sedentary behaviors due to shifts to home-based learning and digital interactions,8-12,26 adolescents with chronic conditions demonstrated notable resilience. This resilience might stem from their previous experiences with activity restrictions related to their health conditions. However, the long-term effects of increased sedentary behaviors pose a significant risk to their overall health, 27 suggesting the benefit of tailored online fitness programs and digital health awareness campaigns .
The pandemic has also fostered a shift toward digital platforms, 28 enhancing social interactions among these adolescents. This shift likely deepened their sense of empathy and solidarity within online communities of peers facing similar challenges. Enhanced prosocial behaviors, rooted in shared experiences and mutual support, are vital for building resilience.
As the pandemic wanes, its long-term impact on behavioral patterns could persist, evolving into entrenched habits that necessitate proactive policy responses. Adolescents with chronic diseases face unique challenges that require comprehensive strategies addressing their physical, psychological, and socio-emotional needs.
While our study offers valuable insights, its scope is limited to a single tertiary hospital in Northern Thailand, potentially affecting its broader applicability. The cross-sectional design provides an immediate perspective but lacks the continuity insights of a longitudinal study. The reliance on self-reported data might introduce biases, and the limited sample size for each chronic ailment remains a constraint. Upcoming research, especially with expansive participant pools, should encompass diverse variables, including disease severity, socio-economic contexts, and the depth of participants’ health education.
Conclusion
The COVID-19 pandemic has unveiled the vulnerabilities and resilience of adolescents with chronic diseases, highlighting the need for tailored interventions and robust support systems. To ensure their well-being and prepare them for future adversities, continuous research, monitoring, and adaptive strategies are crucial. Policymakers must prioritize the unique needs of this susceptible group to develop holistic support structures that encompass their comprehensive health needs.
Supplemental Material
sj-pdf-1-gph-10.1177_2333794X241274732 – Supplemental material for Chronic Conditions and Resilience: Adolescent Health Behaviors in the Midst of the COVID-19 Pandemic in Thailand
Supplemental material, sj-pdf-1-gph-10.1177_2333794X241274732 for Chronic Conditions and Resilience: Adolescent Health Behaviors in the Midst of the COVID-19 Pandemic in Thailand by Phatchara Thitamethee, Narueporn Likhitweerawong, Orawan Louthrenoo and Nonglak Boonchooduang in Global Pediatric Health
Footnotes
Acknowledgements
The authors would like to thank the adolescents for their valuable participation in this research study.
Author Contributions
All authors contributed to the study’s concept and design. PT and NB handled data collection, data analysis, interpretation, and the initial drafting of the manuscript. NL and OL offered critical revisions and finalized the manuscript. All authors have reviewed and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Faculty of Medicine, Chiang Mai University under Grant number 143/2564.
Ethic Approval
The study was approved by the Ethics Research Committee of the Faculty of Medicine, Chiang Mai University. (Approval No. 193/2021).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
