Abstract
Background. Outcomes that should be measured during diabetic ketoacidosis management is crucial. However, data associated to this was limited in Ethiopia. Methods. A cross-sectional study was conducted among children with diabetic keto acidosis between 2016 and 2021.Data were stored in Epi-data version 4.6 and exported into STATA 14.0 software for analysis. The association between independent variables and length of hospital stay was assessed using binary logistic regression. Finally, variables with P-value <.05 were considered statistically significant. Result. Median length of hospital stay was 8 ± 6.2 days. Majority of patients (97.5%) improved and discharged. Factors that affected longer hospital stay were Residence(aOR = 4.31;95% CI = 1.25-14.80),family history of diabetes (aOR = 0.12; 95% CI = 0.02-0.64), glycemia at admission (aOR = 1.01; 95% CI = 1.00-1.02),insulin skipping (aOR = 0.08; 95% CI = 0.01-0.98), abdominal pain (aOR = 4.28; 95% CI = 1.11-15.52) and time in which the patient get out of diabetic ketoacidosis(aOR = 6.39; 95% CI = 1.09-37.50). Conclusion. Majority of patients showed improvement and discharged to homes after a long hospital stay. Majority of patients resolved from diabetic ketoacidosis between 24 and 48 hours.
Introduction
Diabetic ketoacidosis (DKA) is an expensive acute complication of T1DM that can occur when there is a comparative or complete decrease in circulating insulins.1-6 The magnitude of DKA among children with diabetes has increased over the past 3 decades. 7 DKA has become the most common sticky situation of T1DM in children with an incidence of 1% to 10% per year and 30 to 70% prevalence in both high and middle-income countries.7-9 It is the most common reason for hospitalization, morbidity and mortality in children with an admission rate of 16.5% to 78% in hospitals. 5 The pooled mortality for DKA is estimated to the range of 2%-5% in middle income countries and 6-24% in developing/low income countries.10-13
The prevalence of DKA was reported in 1% to 10% of known type 1 diabetic patient in industrialized countries; 35% to 40% in Africa. Whereas, among newly diagnosis it acounts15% to 70% in developed nation; 35.8% to 95% in less developed countries including Ethiopia.1,2,14,15 with the overall incidence rate of 2.27 per 100 children/month of observation. 16
Insulin deficiency, dehydration and hormone increments such as cortisol, adrenaline, glucagon, and growth hormone are some of the clinical features of children admitted with DKA. 17 The biochemical criteria for the diagnosis of DKA are hyperglycemia(blood glucose level > 200 mg/dL, venous pH less than 7.3 or serum bicarbonate level less than 15 mEq/L and ketonemia (blood b-hydroxybutyrate concentration++3 mmol/L) or moderate or sever ketonuria.6,18,19
Patients can be dramatically ill, and the severity of presentation can be graded based on the degree of acidosis and their clinical condition; Mild DKA: venous pH form 7.2 to 7.3 or serum bicarbonate<15 mmol/L, variability of effective serum osmolality, anion gap and oriented, alert mental status but fatigued with signs of no dehydration ; Moderate DKA: venous pH form 7.1 to 7.2 or serum bicarbonate<10 mmol/L, variability of effective serum osmolality, anion gap >12 and if the patient is with Kussmaul’s respiration, signs of dehydration and lethargic/sleepy/drowsy mental status; Severe DKA: venous pH < 7.1 or serum bicarbonate<5 mmol/L, variability of effective serum osmolality, anion gap >12 and if the patient is with Kussmaul’s or depressed respiration, signs of severe dehydration or shock and alteration of consciousness level/comma.3,19 As severity increases, the need for pediatrics intensive care as well as the the risk of morbidity and mortality increases. 20 However, with proper management, most patients recover rapidly. 7
It has been identified that, poor glycemic control, comorbidities, younger age, and low socio-economic status have been associated with an increased risk of developing DKA; but, it is unclear if this risk factor influences patient outcomes in pediatric management centers. 21
Higher mortality rates among children admitted with DKA were reported with an increased incidence of cerebral edema, sepsis, shock, cerebral injury, altered levels of consciousness, respiratory failure with hyposphotemia, renal failure, and delayed diagnosis both in developed and developing countries,10,13,22-26 DKA could be the principal source of death with an estimated mortality rate of 20% to 50%, with 15% to 35% of permanent neurologic deficits for survivors.11,27,28 This acute complication can also accompanied by malnutrition, parasitic infections, and microbial infections with tuberculosis and HIV. 28 Overlapping of these conditions contributes to the increment of morbidity and mortality rates. The inability of patients to afford insulin treatment leads to poor glycemic control. As a result, patients may seek alternative treatment from traditional healers or use herbal remedies further complicating the management process. 29
The most important issue that must be taken in consideration during treatment of DKA include correcting dehydration, acidosis and reversing ketosis, restoring blood glucose to near normal by replacement of insulin, fluid and electrolyte, watching for possible complications and other precipitating adverse event.4,5,17 Volume expansion with 10–20 mL/kg of 0.9% saline over 1 hour is compulsory immediately soon after diagnosis, daily maintenance fluid requirement and the estimated fluid deficit which is 85% is calculated to be administered over 48 hour. Deficit replacement should be by normal saline with consideration of 40 meq/L of potassium chloride administration; additional adjustment of fluid is based on serum random blood sugar (RBS);which means, normal saline 0.9% should be given until RBS is 250–300, and fluid will be changed to dextrose with normal saline (DNS) or ½ normal saline(NS) in 5% dextrose in water (DW) when the RBS bellow 250 to 300;whereas, 1/2 NS in 10% dextrose should be given when RBS <150 to 200 and 10% IV push if RBS <60.3,6,7
Regular Insulin administration with 0.5 U/kg half IV, half IM/SC is initiated 1 hours after the initiation of bolous fluid replacement therapy again, regular insulin of 0.5 U/kg subcutaneously 4 times per day can further established until the patient is free from ketone for possible standing dose initiation; continuous intravenous regular insulin/ CIRI at a rate of 0.05 to 0.1 IU/kg/hour until resolution of DKA can also be used.4,13 In situations where CIRI is not possible, 1 to 2 hourly subcutaneous (SC) or intramuscular (IM) administration of insulin can be as effective as intravenous (IV) regular insulin infusion with precaution of subcutaneous (SC) administration in patients with impaired peripheral circulation.5,6
In the study area, there is a standardized practice in the management of DKA, which is called DKA management protocol; This protocol was based on the recommendation from the international guideline like international society for pediatrics diabetes(ISPAD) and other recently revised pediatrics text books, articles, and opinion from senior experienced staffs.5,8 Applying the novel approach of early diagnosis and treatment by multidisciplinary diabetic care teams can also ensure good outcomes.24,30-32 Length of stay, complications associated with treatment, and overall mortality among children with DKA during inpatient management are the foremost outcomes that should be measured. This is because, it is highly trusted to improve DKA-management protocol. However, data associated with length of stay, complications following management, and rate of mortality due to DKA remain limited in Ethiopia.
Therefore, the current study aimed to determine treatment outcomes of children admitted with DKA at Felege Hiwot comprehensive referral hospital in Amhara region, Northwest, Ethiopia.
Method
Study Area and Period
The study was conducted in the Bahir Dar city; placed 565 km far from Addis Ababa, the capital city of Ethiopia, in Amhara region, Northwest Ethiopia., has 2 public referral hospitals, 1 primary hospital, 10 health centers, and 4 private hospitals. This study was conducted at Felege Hiwot’s comprehensive specialized referral hospital (FHCSH). This hospital is expected to serve more than 10 million people from the catchment area. This hospital currently has a total of 1431 manpower in each discipline with 500 formal beds, 11 wards, and 39 clinical and nonclinical departments/units/providing Diagnostic, curative, Rehabilitation, and preventive services both in outpatient &inpatient bases.
Apart from other services, the hospital provides diabetic treatment services by nurse practitioners, pediatric residents, and pediatricians. The study period addressed from 1st January, 2016 to February 30/2021.
Study Design
An institution-based retrospective cross-sectional study was employed.
Source and Study Population
Source population
All pediatricT1DM patients who were on follow-up at Felege Hiwot comprehensive referral hospital were the source of population in this study.
Study population
All pediatric T1DM patients who were admitted with DKA during the study period.
Sample Size and Sampling Technique
Randomly selected Pediatric cases (<15 years old) T1DM clients admitted with DKA in the period from Junuary1st 2016 to February 30, 2021 (5-years) were included. To determine the sample size, the following assumptions were considered: 80.95% of clients were discharged with an improvement in Jimma with a 95% confidence level and 5% marginal error. 12 The sample size was calculated using Raosoft software (http://www.raosoft.com/samplesize.html). Because the total population is <10 000, we used the correction formula. Yelds the final sample size 176.
Sampling Procedure
The study participants were selected from the registration book. The medical profiles of children admitted with DKA between January 1st, 2016, and February 30, 2021, were selected. Finally, cards that fulfilled the criteria were reviewed.
Inclusion criteria
Children aged less than 15 years and diagnosed with DKA from January 1/2016 to February 30/2021 were included
Exclusion criteria
Childre’s charts that had incomplete information and were lost during the study period.
Study Variables
Dependent variables
Length of stay, complication, and mortality of children admitted with DKA.
Independent variables
Socio-demographic (age, sex, residence, and educational status of the children including weight and height); diabetes-related variables/clinical and biochemical variables (family history of T1DM, type of T1DM, the severity of DKA, admission blood glucose readings, duration of chief complaint, sign and symptoms of client presentation, comorbidities, vital signs, DKA precipitating factors, frequency of DKA episode during the study period, electrolyte disturbance, ketone, and urine glucose level and treatment related
Operational definitions
Diabetic ketoacidosis (DKA): Is defined as an admission of blood glucose >200 mg/dL and the presence of ketonemia and/or ketonuria; arterial pH less than 7.30 and with other clinical presentation like depressed respiration, sign of dehydration and an altered level of consciousness.6,18,19
Hyperglycemia: Is defined as a random plasma glucose level>200 mg/dL and hypoglycemia is defined as a blood glucose level ≤70 mg/dL.20,33
A longer hospital stay: was defined as a hospital stay for >7 days and a short hospital stay was considered if the patient could stay in the hospital for ≤7 days. 34
Treatment outcome: the length of hospital stay, complications following treatment, and mortality of DKA were the measures of treatment outcome in the context of the present study.
Co-morbidity: Implies concomitant diseases that are not the complications of T1DM and/or DKA. 35
Co-medication: Co-medication are concurrent drugs prescribed for for the treatment of diseases, or deficiencies, other than antihyperglycemics.
Insulin defaulters: Are known type one diabetes patients who discontinued insulin treatment because of different reasons.
Data Collection Methods
Medical records of patients with DKA admitted to the hospital were drawn from patient logbooks and a card room. The selections of medical records for sampling were based on the physician’s confirmed diagnosis on patient logbooks. Participants included in the study were all T1DM patients with DKA admitted to Felege Hiwot comprehensive referral hospital with age <15 years old and whose medical records comprise complent client data.
Data Quality Control
The data were collected by trained data collectors using structured and pre-tested data extraction tools. Data were collected on patients demographics, presenting symptoms, precipitating causes of DKA, vital signs, biochemical profiles (admission blood glucose, admission urine ketone, urine glucose) at presentation to the inpatient department, time from presentation to the resolution of urine ketones, length of hospitalization and treatment outcomes.
Data Processing and Statistical Analysis
Data were entered into Epidata version 4.6 software for cleaning and exported to STATA version 14.0 for analysis. Tables and text were used to present the findings. Categorical variables were described using proportions, and continuous parametric variables with median and standard deviation. Categorical variables were compared using the Chi-square test and fisher’s exact test, whereas, continuous variables were compared using parametric (t-test). Binary logistic regression was done to determine the factors that affect length of hospital stay and mortality.
Result
Sociodemographic Characteristics
One hundred seventy-six (176) medical records were reviewed; of which, fourteen (7.95%) patient’s charts were not included in the study due to important variables being missing there. Accordingly, 162 patients medical record were investigated with 92.05% of response rate.
The median age of the study participants was 8 ± 4.7 with 2.4 years mean duration of diabetes. And greater than half of the patients were males (51.2%) and the majority of the patients (66.7%) were from rural areas (Table 1).
Sociodemographic Characteristics Among T1DM Children Admitted With DKA, Bahir Dar, Ethiopia, 2021 (n = 162).

Other—includes sisters, brothers, and another primary caregiver (guardian) in the home.
Clinical Characteristics
Out of the investigated patients, 129 (80.6%) were newly diagnosed cases and the remaining 31 (19.4%) were known T1DM patients. The majority (103[63.6%]) of the patients were on mixed insulin (regular and lent) treatment and the other patients were on either regular and NPH (30[18.6%]) or NPH alone (29[17.9%]) with an average insulin dose of 16.5 ± 10.7U/day. Greater than half of the patients had T1DM for more than 3 years (86[53.1%]). And many of the patients had a history of comorbid illness (108[66.7%]) (Table 2).
Clinical Characteristics among T1DM Children Admitted With DKA, Bahir Dar, 2021 (n = 162).

Frequency of DKA Episode Severity and Its Precipitating Factors
The rate of DKA reoccurrence was assessed and showed that, majority of the patients encountered on it at once (116[71.6%]), 31[19.1%] had 2 episodes, 12[7.4%] and 3[1.9%] of the patients had 3 and 4 episodes of DKA recurrence during their follow up period respectively. And 29(17.9%) of the patients were on severe DKA, whereas 61(37.7%) and 72(44.4%) of the patients had moderate and mild DKA during their presentation. The most common precipitating factor was found to be infection (91[56.2%]). Other precipitating factors are shown in (Figure 1 and Table 3).
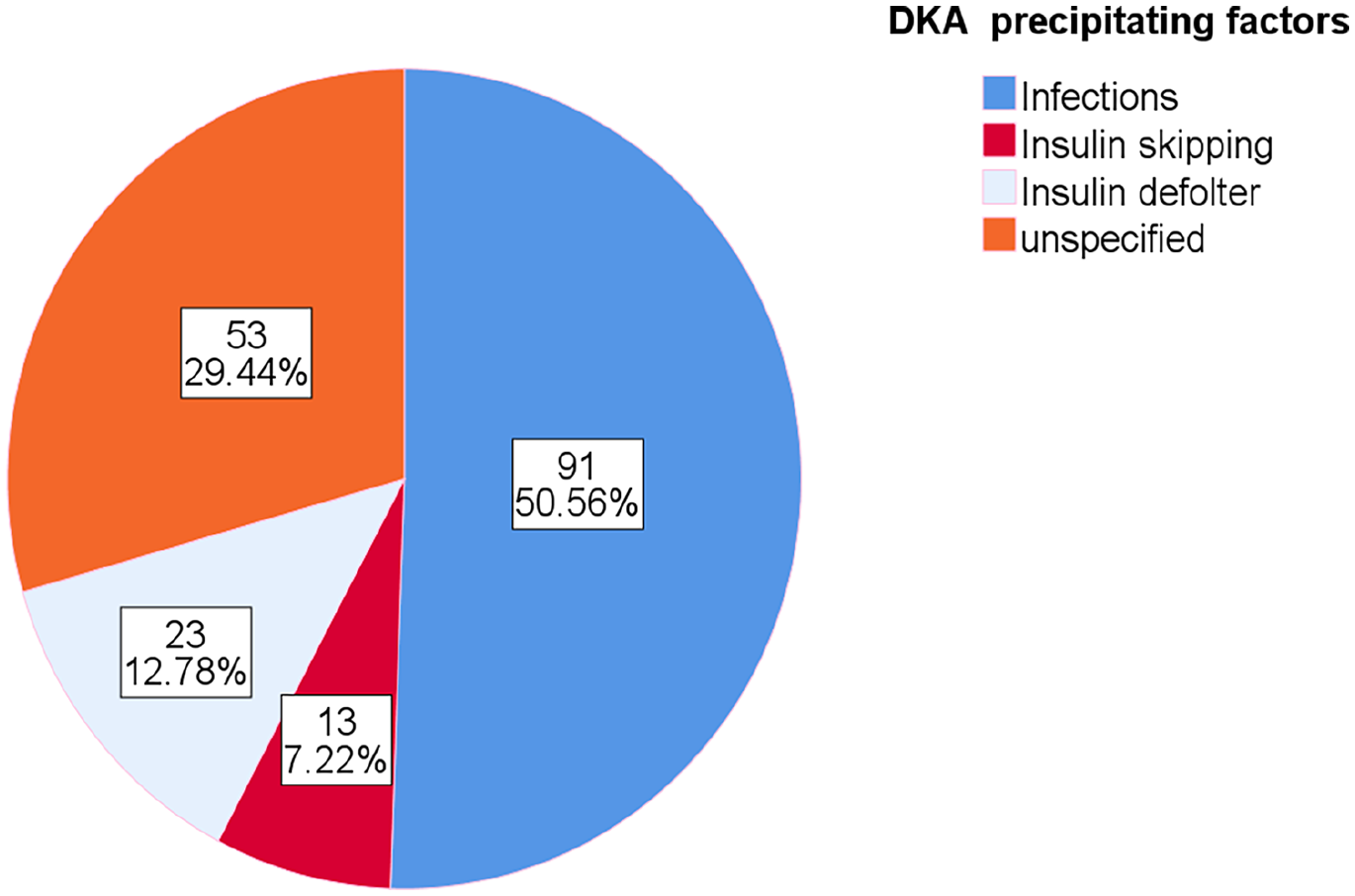
Precipitating factors of DKA among T1DM children admitted with DKA, Bahir Dar, Ethiopia 2021 (n = 162).
Frequency of DKA Episode, Severity, Precipitating Factors, Clinical Presentation and Laboratory Results Among T1DM Children Admitted With DKA, Bahir Dar, 2021 (n = 162).

Abbreviations: PR, pulse rate; RR, respiration rate; Others include diarrhea, headache, and dizziness; NB, the most common infection that precipitates DKA includes UTI, URTI, acute gastroenteritis, pneumonia. . .. See above in Table 2.
Clinical presentation and laboratory results of clients admitted with DKA
In this study, most of the patients were presented with polyuria (144[88.9%]) and polydipsia (137[84.6%]) as it was documented by physicians during history taking under patients clinical profile/chart. In addition to these, nausea/vomiting (63[38.9%]), polyphagia (61[37.7%]) and abdominal pain (51[31.5%]) were also reported. Regarding vital signs: 83(51.2%) of the patients were on tachycardic; where as, 56(34.6%)of the patients were on tachypenic with the mean value of pulse rate was 115 ± 22.1 beats/min, respiration rate was 31.1 ± 10.3 breath/min, and body temperature was 36.6 ± 0.9°C. (Table 3) shows the details regarding clinical presentation and some laboratory results.
Management Protocol, Comedication and Its Treatment Outcome
In this study, the most commonly used type of fluid bolus was found to be 0.9% normal saline/NS 0.9% normal saline (161[99.4%]) with an average volume of 362.2 ± 348.4 mL. Maintenance fluid was carried out mostly with normal saline (0.9%NS) and D5W (75[46.3%]). The average rate of fluids in the majority of the patient was 89 ± 14 mL/hour. Regular insulin was the only insulin drug administered to all DKA patients with an average rate of 9.6 ± 4.3 U every 2 to 4 hours and then every 6 hours, till the patients were free from ketone (start standing dose). However, only 56(34.6%) of the patients were repleted with potassium chloride with 68% of concomitant drug use, mainly antibiotics (73%; Table 4).
DKA Management Protocol, Comedications and Treatment Outcome Among T1DM Children Admitted With DKA, Bahir Dar, 2021 (n = 162).

Abbreviations: Where- Where-MF, maintenance fluid; SD, standard deviation; D5W, Dextros 5%; IV, intera venus; Other drugs include-antiviral & analgesics; LOS, length of stay; AKI, acute kidney injury; SD, standard deviation.
The majority of patients were free from/got out of DKA between 24 and 48 hours (58[35.8%]). More than three-quarters of the patients (139[85.8%]) did not develop any type of complication; However, hypokalemia (11[6.8%]) and hyponatremia (5[3.1%]) were found to be the most common complication followed by a neurologic sequel and hypernatremia both accounting 4 cases (4[2.5%]), 4[2.5%]).
The median time stayed in hospital was 8 ± 6.2 days; Where, majority of patients (96[59.3%]) stayed in the hospital for more than the expected duration (>7 days). Concerning the overall treatment outcome, only (4[2.5%]) patients died; where as the other patients (158[97.5%]) revealed improvement and discharged to their homes (Table 4).
Overall, treatment outcomes including length of stay, treatment associated-complications, and mortality in relation to other variables among T1DM children admitted with DKA, Bahir Dar, 2021(n = 162) showed in the perspectives figure and Table below (Figures 2-4 and Table 4).

Overall treatment outcome in relation to residence among T1DM children admitted with DKA, Bahir Dar, 2021 (n = 162).
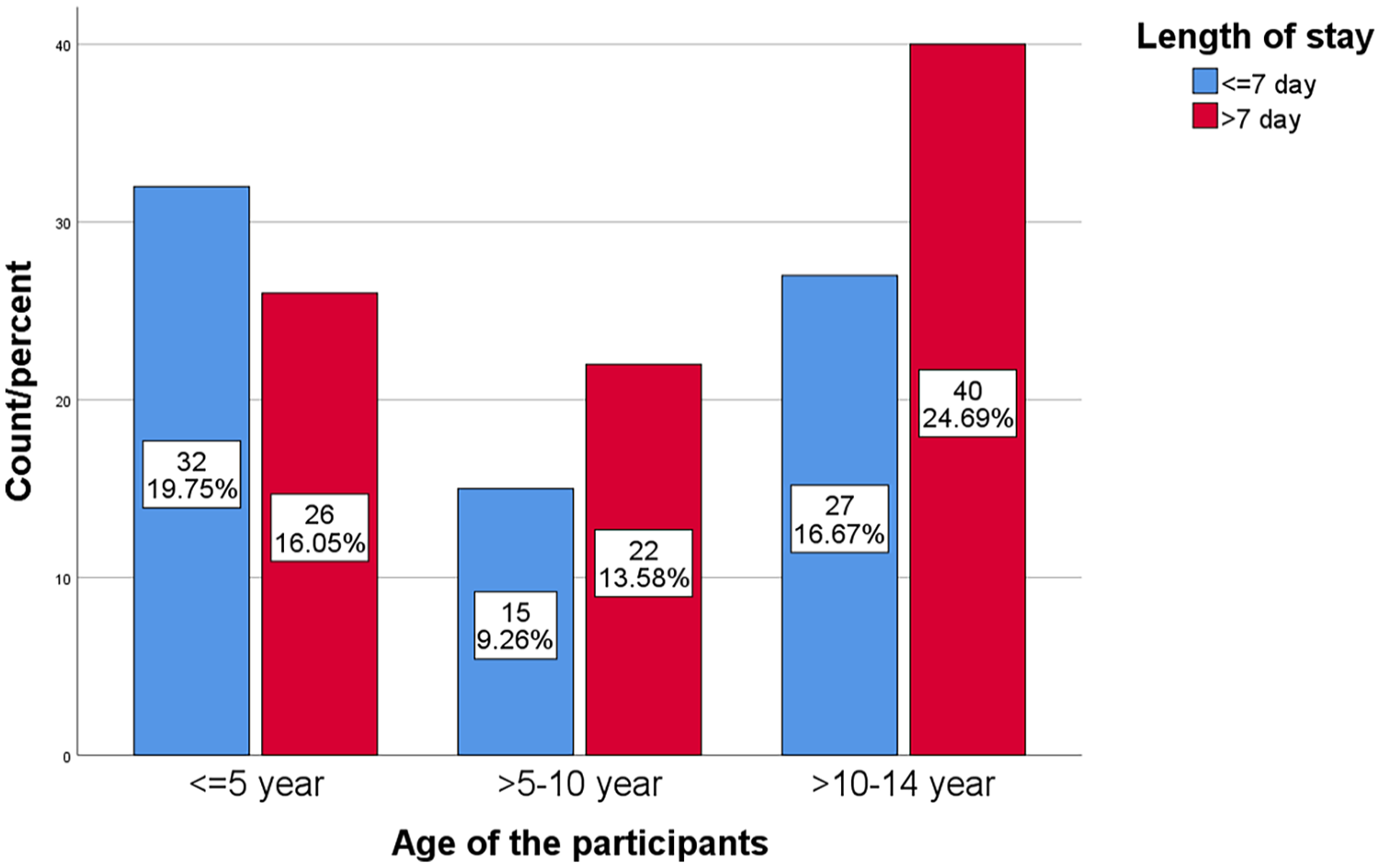
Proportion of patients stayed in the hospital in relation to age category among T1DM children admitted with DKA, Bahir Dar, 2021 (n = 162).

Proportion of patients who developed complication in relation to length of stay among T1DM children admitted with DKA, Bahir Dar, 2021 (n = 162).
Factors that Determine Long Hospital Stay Among Type 1 Diabetic Children Admitted With DKA
The independent variables such as age, residence, client educational status, BMI, duration of chief complaint, family history of T1DM, frequency of DKA episode during the study period, the severity of DKA, DKA precipitating factors, the clinical presentation of DKA like polydipsia, abdominal pain, cough and confusion, location of admission, glycemia at admission, body temperature, having a history of comorbidity such as UTI, URTI, fungal infection, Comedication, time in which the patient get out of DKA and management complication were significantly associated with long hospital stay at the point less than 0.25 level of significance from the bivariable analysis.
However, residence, family history of T1DM, glycemia at admission, DKA precipitating factors, DKA presentation with abdominal pain, location of admission, and time in which the patients could get out of DKA were found to be significantly associated with long hospital stay in the multivariable logistic regression model less than 5% level of significance.
The existence of interactions among independent factors was checked but there was no significant interaction.
Consequently, after adjusting other covariates, the odds of longer hospital stay among the rural resident patients were greater by 4.31times as compared with the urban resident group of the patients(aOR = 4.31,95% CI = 1.25-14.80, P-value = .020).
Likewise, DKA presentations with abdominal pain among patients were associated with longer hospital stay by 4.28 times compared to patients with no abdominal pain (aOR = 4.28, 95% CI = 1.11-15.52, P-value = .035). which means, the time of improvement/recovery time from DKA and to be discharged from hospital among patients with abdominal pain was significantly longer compared with patients with no abdominal pain during their presentation.
Furthermore, those patients who get out of DKA after 72 hours had more likely to be stayed in the hospital by 6.39 times as compared to patients who get out of DKA for less than 24 hours(aOR = 6.39, 95% CI = 1.09-37.50, P-value = .040)
However, patients with DKA precipitated by the omission of insulin for those with known diabetic patients had less likely to be stayed in the hospital by 92% as compared to DKA patients precipitated by infection (aOR = 0.08, 95% CI = 0.01-0.98, P-value = .048;) Table 5).
Factors That Determine Long Hospital Stay Among T1DM Children Admitted With DKA, Bahir Dar, 2021 (n = 162).

Where ®, Reference group.
Significantly associated variables at a point less than .05.
Discussion
The purpose of this study is to determine the treatment outcome of children <15 years old admitted with DKA in Bahir Dar city Felege Hiwot comprehensive referral hospital.
In this study, the majority (97.5%) of admitted DKA patients were showed improvement and discharged to their homes with 8- day median length of hospital stay. This finding is much higher than the study conducted at South Asia and Jimma University Hospital in Ethiopia, where only 80.5% and 84% showed improvement and were discharged to their home respectively.12,33
In this study, the magnitude of mortality rate is 2.5% which is higher than the study reported from developed nation (0.15%-0.31%) 11 and the mortality rate testified in Sudan which was 1.7% 36 the reason might be due to the high prevalence of infection (56.2%) and comorbidities (66.7%) as well as treatment complications (14.2%) in this study. However, lower than the study reported in India (8.75%-12.8%)10,27 and other developing countries like Kenya and Tigray region in Ethiopia (3.4%-13.4%).13,15,37
Concerning hospital stay, although no clear cut-off point is set about when to say, there is a long hospital stay for patients admitted with DKA, most clinical experts have a common conscience for a longer hospital stay, if and only if, the patient stayed/admitted for more than 7 days in the hospital with successful treatment by prompt correction of hyperglycemia, diabetic acidosis and electrolyte disturbances.34,35 Therefore, the findings of this study pointed out a longer hospital stay(8medians)days to be discharged from the hospital as compared to the study conducted in the united states (2.5) days, 32 Al-Azhar University in Gaza (5.88 ± 2.55) days, 35 and 3.7 to 3.4 days in another study; Even some clients can be discharged within 24 hours of hospital stay despite, the case is with sever DKA.7,38 However, the finding was found to be equivalent to the study reported in Kenya(8 medians) days. 22 This discrepancy in treatment outcome; inpatient recovery, mortality rate, and length of hospital stay can be due to differences in treatment protocol implemented by each health care institution and population characteristics, sample size, study design, and overall healthcare system including resource allocation.
Regarding determinant factors, residence of the participants was found to be significantly associated with length of hospital stay. The study showed that, patients from the rural area had 4.31 times more likely to stay in the hospital for a longer time as compared to those patients living in an urban area(aOR = 4.31,95% CI = 1.25-14.80). This can be due to the shortage of emergency service transportation to access immediate medical management,10,12 which again complicates the case 10 and the finding is supported by the study conducted in Turkey. 39
Those patients having a family history of diabetes mellitus had 88% less likely to stay in the hospital for a longer time as compared to patients with no family history of diabetes mellitus (aOR = 0.12, 95% CI = 0.02-0.64). The reason behind this is not inclusive yet.However,it is believed to be due to favorable knowledge and adherence they have in regard to diabetes mellitus.
The amount of serum glucose at admission was also significantly associated with longer hospital stays. Length of hospital stay increases by 1 day, as the serum glucose value increases by 1 unit (aOR = 1.01, 95% CI = 1.00-1.02). This could be due to severe hyperglycemia leading to severe acidosis/dehydration, electrolyte disturbances, and later altered sensorium at presentation.10,38,39 Which again overburdened the situation by increasing the number of patients to undergo further complications as was supported by the findings in this study.
In this study, precipitating factors of DKA by insulin skipping/omission were less likely associated with longer hospital stay by 92% as compared with that patient’s DKA precipitated by infection (aOR = 0.08, 95%CI = 0.01-0.98).
This is because, having concurrent infection influences T1DM disease progression with hurt of normal glucose metabolism which can lead worsening of optimal glycemic control. Infection can also reinforce hormones in triggering blood glucose level to be raised and can complicate the management process. 29 The finding is in line with the study conducted in Addis Abeba, Jimma, and Kenya.12,15,22
A patient with abdominal pain at the time of client presentation is 4.28 times more likely to be stayed in the health institution than patients with no abdominal pain (aOR = 4.28, 95% CI = 1.11-15.52). The finding is similar with study reported in Kenya 22 and Turkey. 39
Similarly, the time in which the patient free from/ got out of DKA was associated with a longer hospital stay in this study. Those patients who get out of DKA in greater than 72 hours were 6.39 times more likely to stay in hospital compared to those patients who get out of DKA for less than 24 hours (aOR = 6.39, 95% CI = 1.09-37.50). This might be due to differences in hyperglycemia state, clinical presentation, and delay in management.37,40
In general, this study can bring out positive implications for clinical care, health service management, and research in the area of diabetic specialization. Clinically, the health care worker can identify predictors associated with longer hospital stay among type one diabetic children admitted with DKA at clinical setup. Health care managers can access current evidence about overall treatment outcomes of DKA among T1DM children and take remedial action to strengthen service delivery by clinicians. Researchers can also be motivated to conduct further research in this area by taking this study as preliminary findings.
Conclusion
Management protocol was generally administered according to Ethiopian standard treatment guideline; However, poor practice of serum potassium assessment as well as potassium supplementation was noted .In this study, the majority (97.5%) of admitted DKA patients were showed improvement and discharged to their homes with in 8-day median length of hospital stay and with very low mortality rate and high management complications (14.2%). The study also suggests that, the times in which the majority of patients get out of DKA were between 24 and 48 hours.
Residence, family history of T1DM, glycemia at admission, DKA precipitating factors, and DKA presentation specifically, abdominal pain, and time in which the patients got out of DKA were significantly associated with a long hospital stay in the multivariable logistic regression model of less than 5% level of significance.
Thus, to achieve the intended treatment outcome early in time, clinicians and other stakeholders should focus on diabetic ketoacidosis presentation and precipitating factors with possible multicenter studies in this regard.
Limitation
Since the data were collected from medical records, the detailed treatment protocol and some of the important laboratory results were not addressed. Another limitation is that this study was conducted in one hospital only, which may be difficult to generalize the findings to another hospital in the region
Footnotes
List of Acronyms
ADA: American Diabetic Association; BGM: Blood Glucose Monitoring; BMI: Body Mass Index; CIRI: Continuous Intravenous Regular Insulin; DKA: Diabetic Keto Acidosis; FBS: Fasting Blood Glucose; HIV: Human Immunodeficiency Virus; IVF: Intravenous Fluid; ISPAD: International Society of pediatrics and Adolescent Diabetes; RBS: Random Blood Glucose; T1DM: Type one Diabetes Mellitus.
Author’s Contributions
Fentahun Meseret had a substantial contribution from conception to the acquisition of data. All authors had a great contribution to the study design, analysis and interpretation of the findings. FM drafted the manuscript and SM, TE and TG revised the drafted manuscript for important scholarly contents. Finally, all authors approved the final manuscript.
Data Sharing Statement
Data will be available upon request from the corresponding author.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval and Consent to Participate
In order to conduct this research, we tried to consider the declaration of Helsinki’s ethical principles for medical research. Ethical clearance and approval were obtained from the Institutional Review Board (IRB) of — university, college of medicine and health sciences, school of allied health sciences with ethical review board number (CMHS/IRB number01-008) decided on the date of February 26, 2021. Written supportive letters, as well as permission and/or informed consent, have been taken from the pediatrics department of the hospital and from the dataset owner to use the information in databases/repositories for this research on behalf of the patients. As this was a retrospective study, informed consent from individual patient was not requested because the authors and data collectors had no physical contact with them and the data were collected from their medical records after their discharge from the hospital. Informed consent from each study participant, for ethics approval, had been waived by the institutional Review Board of –university ethics committee. Information in the data extraction was anonymous. This study had no danger or negative consequences for the study participants. Medical record numbers were used for the data collections and personal identifiers of the patients were not used in this research report. Access to collected information was limited to the principal investigator and confidentiality had preserved throughout the time.
Consent for Publication
Not applicable.
