Abstract
Bronchopulmonary dysplasia (BPD) is a complication of preterm and low birth weight infants. The incidence of BPD has not decreased over the past 20 years. Complications of BPD include rehospitalization, chronic lung disease, cardiovascular disease, and impaired growth and development which will affect the patient's quality of life. There are unfortunately limited data available regarding BPD in Indonesia. This study is expected to be a reference in taking preventive measures to reduce mortality and morbidity in preterm and low birth infants. This study aims to determine predictors of BPD in infants with birth weight less than 1500 g. We conducted a retrospective cohort study that included 116 infants with birth weight <1500 g. Twenty-two (19%) infants had BPD with the highest proportion (63.6%) in the 28 to 31 weeks of gestational age. Multivariate analysis showed mechanical ventilation in more than first 2 days of life (
Introduction
Bronchopulmonary dysplasia (BPD) is a clinical diagnosis based on persistent oxygen dependence for a period after birth. 1 The consensus held by the National Institute of Child Health and Human Development (NICHD) in 2001 divided BPD into 2 groups, that is, infants with gestational age <32 weeks and those with ≥32 weeks. The time to determine the diagnosis is at 36 weeks postmenstrual age (PMA) in infants with gestational age of <32 weeks. Meanwhile, it is at a chronological age of 28 to 56 days in infants with gestational age ≥32 weeks.
The global incidence of BPD in extremely preterm infants (<28 weeks of gestational age) is 10% to 89% (10%-73% in Europe, 18%-89% in North America, 18%-82% in Asia, and 30%-62% in Oceania). 2 Forty percent of extremely low birth weight infants (<1000 g) will develop BPD. 3 Studies about BPD in Indonesia are still rare. According to a study conducted in Bandung, Indonesia, 14.8% of preterm infants (28-34 gestation weeks) with respiratory distress syndrome (RDS) experienced BPD. 4 Unlike other complications of preterm birth, the incidence of BPD has not decreased over the past 20 years as reported by the NICHD Neonatal Research Network.
BPD remains a problem as the more very low birth weight neonates survive; the higher their survival rate, and the more likely the incidence of BPD to increase. 5 It is essential to identify predictors of BPD development, and preventative interventions should therefore be targeted at high-risk infants. Several studies indicated that the duration of mechanical ventilation,6-8 RDS,9,10 early onset sepsis,10,11 small for gestational age,12,13 patent ductus arteriosus,7,9,14 neutrophil lymphocyte ratio (NLR), 10 thrombocytopenia, 15 and anemia 8 were associated with the incidence of BPD. However, those studies showed inconsistent results. We would like to estimate the incidence of BPD among infants born with birth weight of less than 1500 g at our Neonatal Unit and to identify associated predictive factors.
Methods
Study Design and Population
We conducted a retrospective cohort study at the level II and III of Neonatal Unit of Dr. Sardjito Hospital Yogyakarta Indonesia, in the period between January 1st, 2017 and November 31st, 2021. All survived infants beyond 28 days after birth with birth weight <1500 g who were admitted to Neonatal Unit for the first 24 hours were recruited. The infants with major congenital malformations (congenital pulmonary airway malformation, congenital lobar emphysema, and critical congenital heart disease), post-surgery that affected the respiratory system such as diaphragmatic hernia, infants born to mothers with hemolysis, elevated liver enzymes, low platelets (HELLP), immune thrombocytopenic purpura (ITP), or systemic lupus erythematosus (SLE), and infants with incomplete medical records were excluded.
Data Collection
Data were obtained from a secondary database. The recorded predictors were mechanical ventilation, RDS, early onset sepsis, hsPDA, SGA, hematocrit level, platelet count, and NLR. Duration of mechanical ventilation was determined as either with intubation or nasal intermittent positive pressure ventilation (NIPPV) for more than first 48 hours of life. RDS was defined as respiratory distress with radiographic findings showing a uniform reticulogranular pattern, referred to as a ground-glass appearance, and was accompanied by peripheral air bronchograms. Hemodynamically significant patent ductus arteriosus (hsPDA) was defined as the ductus arteriosus which remains to open with a systemic-to-pulmonary shunt resulting in pulmonary hyperperfusion and systemic hypoperfusion. Diagnostic parameters for the hsPDA includes (1) precordial pulsation, (2) systolic murmur, (3) tachycardia (heart rate >160 beats per minute), (4) respiratory arrest or use of mechanical ventilation, (5) pulse bounding of femoral conditions, (6) hepatomegaly, (7) metabolic acidosis (pH <7.30) and base excess <−5, and (8) worsening respiratory function. HsPDA was confirmed if the score was ≥2 and/or confirmed by echocardiography performed by a pediatric cardiologist. Small for gestational age (SGA) was a birth weight below the 10th percentile; while percentile between the 10th and 90th was categorized into appropriate for gestational age (AGA) and >90th percentile was considered large for gestational age (LGA) based on the Yogyakarta Indonesian Newborn Curves. 16 Neutrophil lymphocyte ratio (NLR) was defined as the absolute neutrophil count divided by the absolute lymphocyte count measured for the first time within 24 hours postnatally. The NLR cut-off was 0.64. 17 Neonatal early onset of sepsis was defined as bacteremia occurring at ≤ 72 hours, which met 4 out of the following criteria, that is, temperature instability, central nervous system dysfunction, respiratory distress, cardiovascular disturbance, gastrointestinal symptom, renal insufficiency, and hematologic disorder. Platelet count was determined within the first 2 weeks of life, with cut-off less than 150 000/mm3. 15 Hematocrit was confirmed within the first 2 weeks of life, with cut-off less than 39%. 8
Statistical Analysis
Baseline characteristic predictors and outcome variables were compared between infants with birth weight <1500 g and those ≥1500 g. We performed a Kaplan-Meier curve to determine the mean time of BPD occurrence in each independent variable. Multicollinearity test was conducted on the independent variables that had similarities in regression model, namely early onset sepsis, platelet count, and NLR. Cox regression analysis was used to ascertain the magnitude risk of the variable on the incidence of BPD. To identify the most influential factor on the incidence of BPD; multivariate Cox regression was applied to the independent variables with
Ethical Approval
The study was approved by the Medical and Health Research Ethics Committee of the Faculty of Medicine, Universitas Gadjah Mada/Dr. Sardjito Hospital Yogyakarta, Indonesia with number KE/FK/0108/EC/2022.
Results
We enrolled 116 neonates with the proportion of male and female 1:1.3. The highest proportion in the gestational age group was 28 to 31 weeks (Table 1). Out of all subjects, the incidence of BPD was 19%, for which the highest proportion was found in the <28 weeks of gestational age and <1000 g group.
Baseline Characteristics of the Subjects.

Abbreviations: CPAP, continuous positive airway pressure; HsPDA, hemodynamically significant patent ductus arteriosus; PDA, patent ductus arteriosus.
The mean time to diagnose BPD in infants <1500 g was 65.6 days (Figure 1). In total, 22 out of the 116 infants whose birth weight was <1500 g developed BPD, with the incidence rate of 4.7 cases per 1000 person-days, or 1.7 cases per person-year. The mean BPD survival time of mechanical ventilation more than first 2 days, hsPDA, SGA, and hematocrit levels showed a statistical significant difference (Table 2).

Kaplan-Meier curve of BPD in infants with birth weight <1500 g.
BPD Survival Analysis on Predictors.
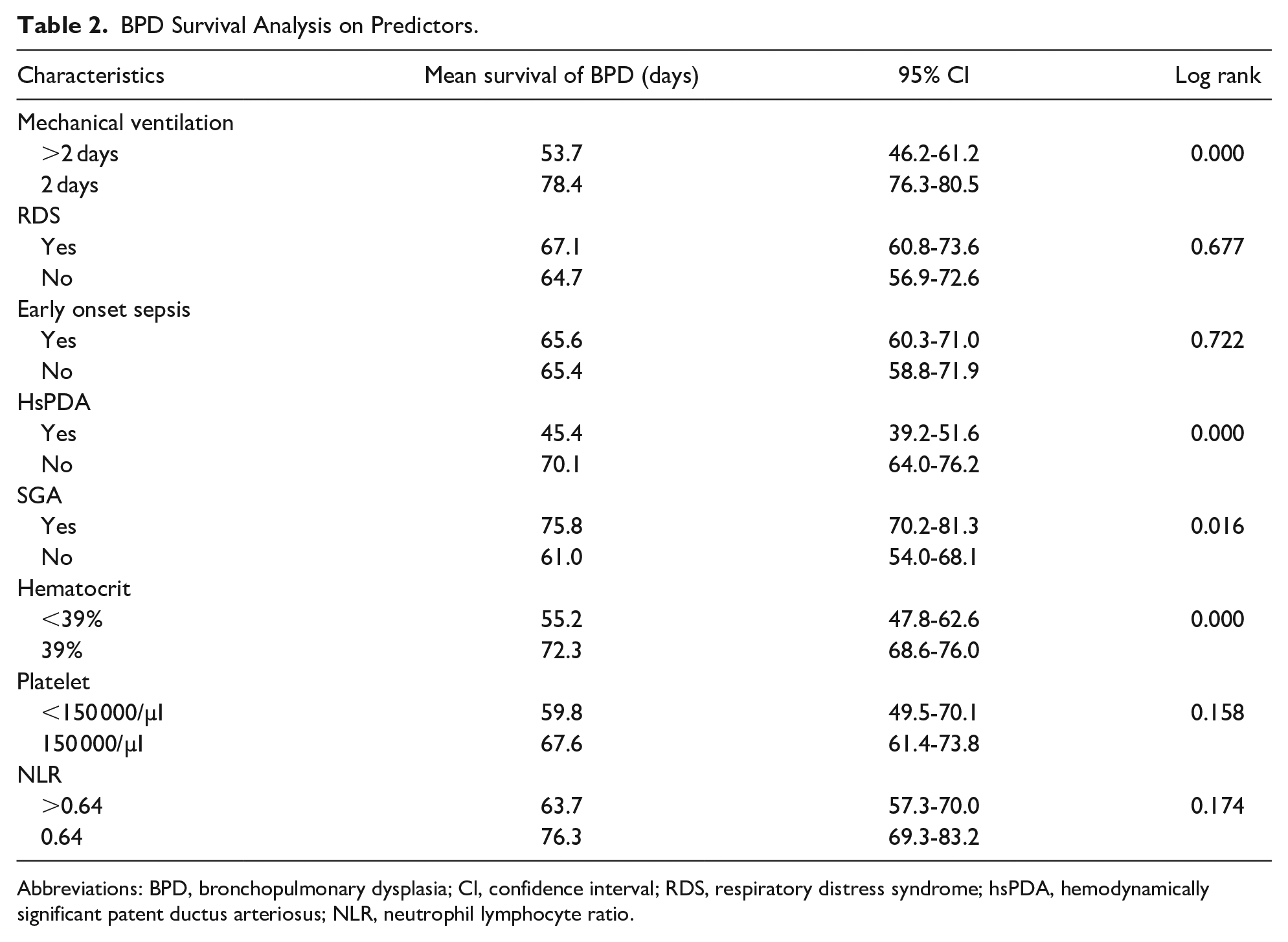
Abbreviations: BPD, bronchopulmonary dysplasia; Cl, confidence interval; RDS, respiratory distress syndrome; hsPDA, hemodynamically significant patent ductus arteriosus; NLR, neutrophil lymphocyte ratio.
Cox regression analysis was used to determine the magnitude of risk from each independent variable on the incidence of BPD. Bivariate analysis (Table 3) revealed that the use of mechanical ventilation for more than first 2 days of life significantly affected the incidence of BPD (
Prediction of BPD.
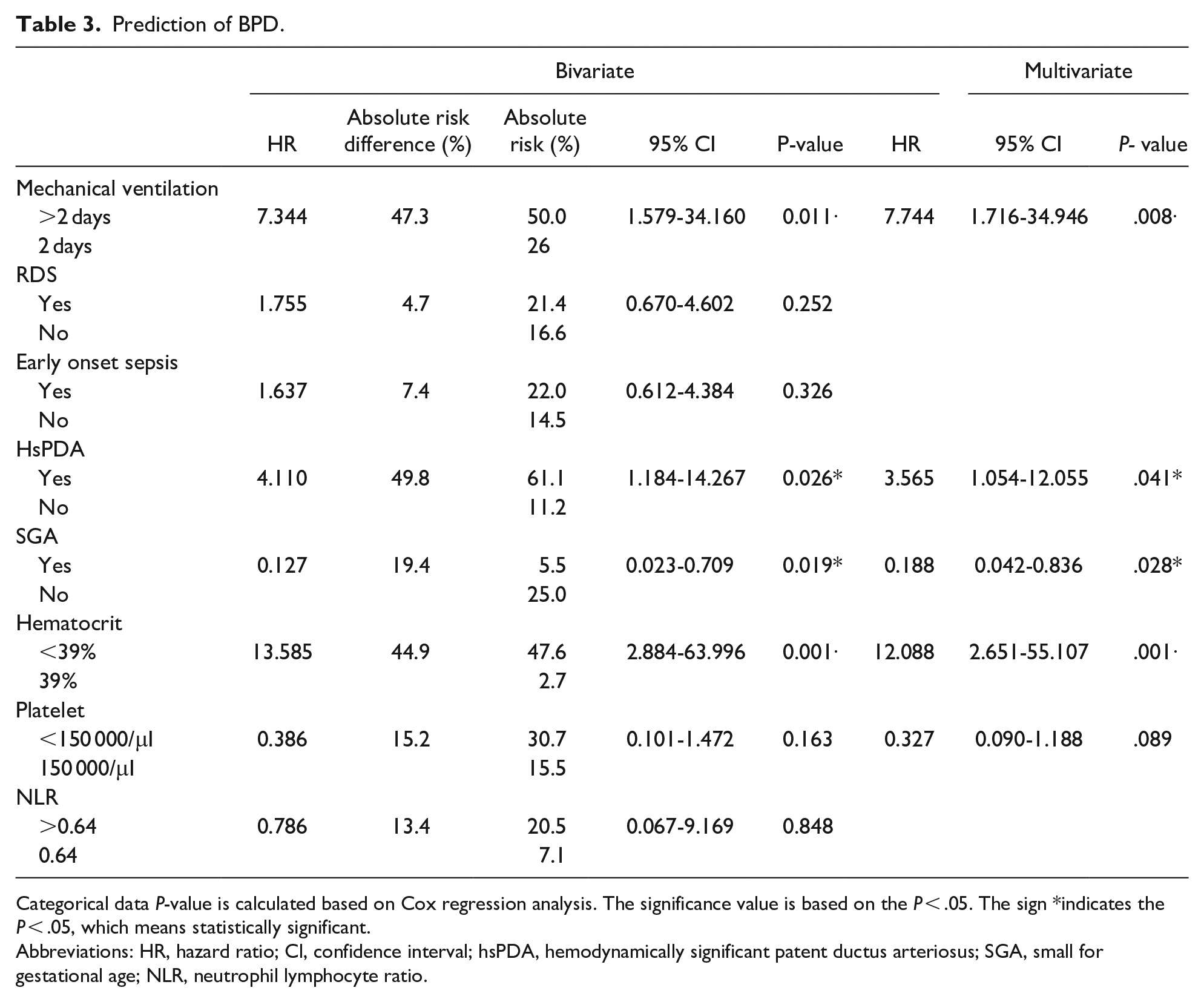
Categorical data
Abbreviations: HR, hazard ratio; Cl, confidence interval; hsPDA, hemodynamically significant patent ductus arteriosus; SGA, small for gestational age; NLR, neutrophil lymphocyte ratio.
Multivariate analysis included 5 variables out of 8 variables with
Discussion
The incidence of BPD in infants with birth weight <1500 g in our Neonatal Unit was 19%. It was lower than that of the South American Neocosur Neonatal Network study (25%) and Brener Dik et al 18 (29.7%). Another study reported the incidence of BPD in VLBW infants was 28.9%; 37.3% for moderate BPD and 62.7% for severe BPD. 19 We found BPD among infants aged ≤31 gestational weeks. The highest BPD proportion (61.5%) was found in <28 weeks of gestational age infants. A similar result was reported by Zhang et al 20 that BPD occurred in <28 weeks of gestational age infants. According to the birth weight, our study showed that BPD was found in 11 out of 21 (52.3%) <1000 g infants. Cunha et al 21 also described similar result. Our data showed that the incidence of BPD was proportional to the gestational age and birth weight. The younger the gestational age and the lower birth weight, the more likely BPD to increase.
The use of mechanical ventilation during first 2 days of life was the most significant predictor of BPD (
The proportion of BPD in infants with RDS was 48.3%. The absolute risk of RDS infants was greater than that in the control group (21.4% vs 16.6%). However, there was no significant difference between the RDS group and non-RDS (
The absolute risk of BPD was higher in the early onset of sepsis than in non-sepsis group (22% vs 14.5%). However, we observed no significant difference between the sepsis and non-sepsis group (
Thrombocytopenia was identified to be high in BPD. The absolute risk of BPD in the thrombocytopenia group was greater than that in the control (30.7% vs 15.5%); however, it was not a significant predictor of BPD in this study (
The absolute risk of BPD in the NLR >0.64 group was higher than in the control group (30.7% vs 15.5%). The multivariate analysis showed that it was not a significant predictor of BPD in infants with birth weight <1500 g (
HsPDA was a significant predictor of BPD in infants with birthweight <1500 g (
Anemia with hematocrit level <39% was a significant predictor for the incidence of BPD. The anemia group had higher absolute risk of BPD than the control group (47.6% vs 2.7%). Studies by Duan et al
8
and Lee et al
32
had similar results, which showed that anemia was associated with increased risk of BPD. Different result was reported by Ming et al
33
that anemia was not a significant predictor for the incidence of BPD (
The risk of BPD between SGA and AGA group was statistically significant (
It was the first study regarding the predictors of the incidence of BPD in infants with birth weight <1500 g in Indonesia. The limitation of this study was the retrospective study design, for which the use of secondary data from medical records could lead to measurement bias compared with prospective study. This study did not differentiate the outcome of BPD based on severity. A research of the effect of early CPAP administration and management of PDA closure (medication or ligation) on the incidence of BPD needs to be conducted.
Conclusion
Mechanical ventilation use for more than the first 2 days of life, hematocrit <39%, and hsPDA were the significant predictors for the incidence of BPD in infants with birth weight <1500 g.
Footnotes
Author Contributions
GM Maytasari: Contributed to conception and design; Contributed to analysis and interpretation; Drafted the manuscript; Gave final approval; Agrees to be accountable for all aspects of work ensuring integrity and accuracy. EL Haksari: Contributed to conception and design; Contributed to analysis and interpretation; critically revised the manuscript; Gave final approval; Agrees to be accountable for all aspects of work ensuring integrity and accuracy. EP Prawirohartono: Contributed to conception and design; Contributed to analysis and interpretation; critically revised the manuscript; Gave final approval; Agrees to be accountable for all aspects of work ensuring integrity and accuracy.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
