Abstract
Background. Neonatal sepsis is the cause of substantial morbidity and mortality, mostly affecting the developing countries including Ethiopia. Previously conducted studies also highlighted the high prevalence of neonatal sepsis in Ethiopia. Therefore, this study was aimed at assessing the determinants of neonatal sepsis in the central Ethiopia. Method. Institution based un-matched case control study was conducted among 192 cases (neonates with sepsis) and 384 controls (without sepsis) in public hospitals in Central Ethiopia. The data were collected through face-to-face interview using structured questionnaire and extraction from maternal and neonatal charts. Binary logistic regression (bi-variable and multi-variable) model was fitted. Adjusted odds ratio with respect to 95% confidence interval was employed for the strength and directions of the association. Results. Younger maternal-age; 30 to 34 years (AOR = 0.41, 95%CI: 0.19-0.85) and 25 to 29 years (AOR = 0.38, 95%CI: 0.17-0.84), not having antenatal care (ANC) follow-ups (AOR = 1.89, 95%CI: 1.02-3.49), place of delivery; home (AOR = 12.6, 95%CI: 5.32-29.82) and health center (AOR = 2.74, 95%CI: 1.7, 4.41), prolonged duration of labor (AOR = 1.90, 95%CI: 1.22, 2.96), prolonged rupture of membrane 12 to 17 hours (AOR = 3.26, 95%CI: 1.46, 7.26) and ≥18 hours (AOR = 5.18, 95%CI: 1.98, 13.55) were maternal related determinants of neonatal sepsis. Whereas, prematurity (AOR = 2.74, 95%CI: 1.73, 4.36), being resuscitated (AOR = 1.93, 95%CI: 1.22, 3.06) and not having meconium aspiration syndrome (AOR = 2.55, 95%CI: 1.34, 4.83) were identified as neonatal related determinants of neonatal sepsis. Conclusion. Younger maternal age, not having antenatal care follow-up, home, and health center delivery, prolonged duration of labor, prolonged duration of rupture of membrane, prematurity, had resuscitation, and neonates without meconium aspiration syndrome were found to be determinants of neonatal sepsis. Therefore, the concerned stakeholders should consider those identified determinants during an intervention for improvement of neonatal health.
Background
Globally, neonatal death accounted for 41.6% of under 5 deaths by the year 2013, the majority of it in developing countries. 1 Data from Ethiopian demographic and health survey 2019 indicated, the neonatal mortality rate was 30 deaths per 1000 live births. 2 From study done in southwest Ethiopia 2014, birth asphyxia (47.5%), neonatal infections (34.3%), and prematurity (11.1%) were the leading causes of death in neonates. 3
Neonatal sepsis contributes significantly to morbidity and mortality, contributing about 26% to annual neonatal deaths. In which about 99% of deaths occur in low and middle-income countries.4,5 Bacterial, fungal or viral, group B streptococcus and Escherichia coli are the most commonly involved organisms, especially in early-onset neonatal sepsis.4,6 The prevalence of neonatal sepsis in Ethiopia varies from 17% to 78%. 7
Home delivery, premature rupture of membranes (PROM), prolonged labor, primiparity, bleeding disorders, not crying immediately at birth, and have received resuscitation were factors associated with neonatal sepsis.8-15 Additionally, preterm delivery (gestational age <37 weeks), low birth weight.9,13,14,17-20 intrapartum fever, APGAR score at fifth minute14,15,20 and a history of maternal urinary tract infection or sexually transmitted infection,12,13 birth asphyxia,13,19 neonates aged <7 days and receiving oxygen via face mask21,22 were also risk factors for neonatal sepsis. Furthermore, older maternal age, multiple per digital vaginal examination, delayed breastfeeding after an hour of birth 22 and ANC follow up 15 are reported by different studies to be determinants for neonatal sepsis globally.
Clean delivery service, hygienic intrapartum, tetanus toxoid vaccination, detection, and treatment of syphilis, asymptomatic bacteriuria, pre-eclampsia, malaria (intermittent presumptive treatment), skilled maternal emergency obstetric care and immediate, emergency neonatal care for sick neonates with emphasis to low birth and preterm newborns could decrease the neonatal mortality attributed by neonatal infection by 20% to 50%. 23
Ethiopia is among the countries aiming to reduce neonatal mortality to at least 12 per 1000 live births by the year 2030. 24 Despite of the tremendous efforts to scale up maternal and neonatal care, the neonatal mortality rate in Ethiopia remains high, increasing from 29% in 2016 to 30% in 2019 Ethiopian demographic and health survey 2 and the prevalence of neonatal sepsis and its contribution to neonatal mortality and morbidity remains high. 7 Although there are few studies previously conducted on neonatal sepsis in Ethiopia, most of them were cross sectional, which are weak to actually identify the real risk factors. Studies on determinants of neonatal sepsis were limited in Ethiopia and no study was conducted in the study area. Additionally, most of those previously conducted studies were only limited to a single study setting or institution, but the current study addressed larger study setting, including all level of health facilities from primary hospital to tertiary level. Hence, there is a need to carry out a research to wholly understand what factors determine the neonatal sepsis, and as a result to improve the health of neonates. Therefore, this study aimed to assess the determinants of neonatal sepsis in hospitals of West Shewa Zone, Central Ethiopia.
Materials and Methods
Study Design, Area, and Period
An institutional based unmatched case-control study was conducted among neonates admitted to hospitals with their index mothers in the west Shewa zone, central Ethiopia from February 2nd to July 30th, 2020. The west Shewa zone is located in the Oromia Regional State to the west of Addis Ababa the capital city of Ethiopia. Ambo the capital of the west Shewa zone is located 114 km from Addis Ababa. The total population of the west Shewa zone is 2 661 188 of which 1 317 288 are male and 1 343 900 are females. The zone has 8 hospitals and 90 health centers providing maternal and child health care services. Eight hospitals namely Ambo general hospital, Ambo University referral hospital, Gedo Hospital, Guder Hospital, Gindeberet Hospital, Inchinni Hospital, Bako Hospital, and Jeldu Hospital were currently providing Neonatal Intensive Care Units (NICUs) services in the west Shewa zone (West Shewa zonal Health Office).
Source and Study Population
All neonates who were admitted to hospitals with their mothers in a west Shewa zone were the source population. All neonates who were admitted to hospital in the west Shewa zone along with their mothers, and who were selected randomly were the study population. Cases (Neonatal with sepsis) were all neonates who were diagnosed as having neonatal sepsis by physician and admitted to hospitals in the west Shewa zone. Controls were all neonates who were admitted to hospitals in the west Shewa zone with other non-sepsis clinical diagnosis (without neonatal sepsis). Neonates with whom their mothers were deceased or abandoned neonates were excluded from the study.
Sample Size and Sampling Technique
Sample size was calculated by using Epi info version 7.2.4.0 software by using double population proportion formula for unmatched case control study with the assumptions of: 95% 2-sided confidence level (CI), Power of 80%, 2:1 ratio of controls to cases, and 35.4% of low birth weight neonates among the controls exposed and odds ratio of 1.68 from the case-control study conducted at Jinka General hospital southern Ethiopia. 13 The final calculated sample size was 576 (192 cases and 384 controls).
The study participants were proportionally allocated to all hospitals providing NICUs services in the west Shewa zone considering their last 3 months neonatal admission. All cases (neonates with neonatal sepsis) admitted to hospitals during data collection period were included in the study. Every 2 controls (neonates without sepsis) admitted to hospitals after each case were included as controls.
Measurements
Data Collection Tools, Procedure, and Quality Control
The English version questionnaire was initially prepared by reviewing different related literatures conducted previously9,12 and then translated to Afan Oromo and back to English by language experts to check consistency. The questionnaire had contained socio-demographic characteristics, past medical, and obstetric history, current obstetric history (prenatal, intrapartum, and immediate post-partum) and neonatal related factors. Data was collected through face-to-face interview by using a structured pre-tested Afan Oromo version questionnaire from mothers and using a data extraction checklist for the different clinical observations from both mothers and neonatal medical records. Data was collected by 8 trained BSc Nurses and supervised by 4 MSc graduated supervisors.
Data quality was assured during collection, coding, entry, and analysis. Two-day training was given for the data collectors and supervisors before actual data collection. The collected data were reviewed and checked for consistency, clarity; completeness, and accuracy throughout the data collection process by data collectors and supervisors. Furthermore, the pretest was done among 5% of the sample at Wolliso Hospital and the result was used to modify the tool.
Data Processing and Analysis
Both bivariate and multivariable logistic regressions were performed to identify significant predictors. The case and control groups were compared based on socio-economic and demographic characteristics, obstetrics, and neonatal characteristics. Those variables with P < .2 in bivariate analysis were considered for multivariable logistic regression analysis. Hosmer and Lemeshow goodness of fit test was used to check model fitness before running the final model which is 0.82. Finally, screened variables were fitted to the multivariable logistic regression model through a backward stepwise method to reduce the effects of the cofounders and to identify the independent effects of each variable on the outcome variable. Finally, adjusted odds ratios with 95% confidence interval were employed to declare strength, directions of the association of the predictors of the neonatal sepsis and P-value of <.05 was used to declare statistical significance.
Ethical Approval and Informed Consent
The study was conducted in accordance with the World Medical Association Declaration of Helsinki. Ethical clearance was obtained from an Institutional Review Board (IRB) of the College of Medicine and Health Sciences, Ambo University with reference number of AU-CMHS/RCS/018/2012. A support letter was submitted to each hospital.
Results
Sociodemographic Characteristics
In this study a total of 544 mothers with their index child had completely responded, making the response rate of 94.4% (188 cases and 356 controls). The mean age of respondents was 26.5 years with a standard deviation of 5 years. More than one-third 76 (40.4%) of cases were in the age group of 18 to 24 years and 137 (38.5%) of controls were in the age group of 25 to 29 years. The majority of cases 113 (60.1%) were from rural and 185 (52.0%) of controls were from urban residence. One-third 62 (33.0%) of cases and 115 (32.3%) of controls had no formal education. About 84 (44.7%) of cases and 127 (35.7%) of controls were farmers
Socio-Demographic Characteristics of Parents of Neonates Admitted to Hospitals in West Shewa Zone, Central Ethiopia, 2020 (Ncontrols = 356, Ncases = 188).
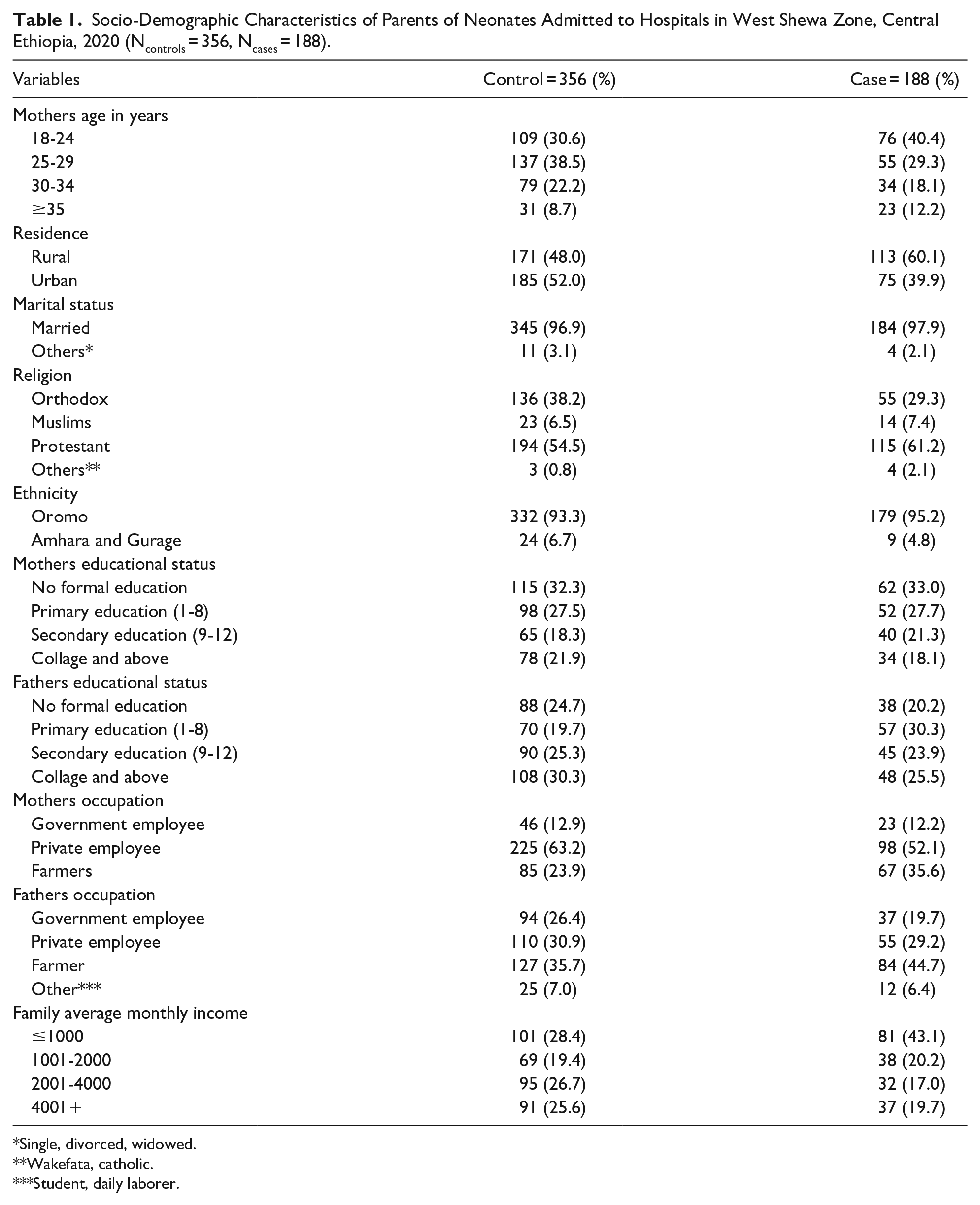
Single, divorced, widowed.
Wakefata, catholic.
Student, daily laborer.
Obstetric Related Factors
The mean and median number of parity among mothers was 2 with standard deviations of 2.12. More than one third 74 (39.4%) of cases and 178 (50.0%) of controls had gave birth to 2 to 4 children. More than four-fifth of mothers, 155 (82.4%) cases and 318 (89.3%) controls had ANC follow-ups for the index child. Only few mothers, 17 (9.0%) of cases and 33 (9.3%) controls had experienced obstetric complications during the pregnancy of the index child. More than half 104 (55.3%) of cases and 283 (79.5%) of controls were born in hospital. Nearly four-fifth 149 (79.3) of the case and 239 (67.1) of control index children were born spontaneously. More than four-fifth of cases 160 (85.1%) and 324 (91.0%) of controls were singleton birth (Table 2).
Obstetric Related Factors of Cases and Controls Admitted to Hospitals in West Shewa Zone, Central Ethiopia, 2020 (Ncontrols = 356, Ncases = 188).

Neonatal Related Factors
More than four-fifth 161 (85.6%) of cases and nearly all 338 (94.9%) of controls were admitted within 7 days of age. More than one third 72 (38.3%) of cases and nearly one-fifth 61 (17.1%) of controls were preterm. More than a third 67 (35.6%) of cases and 97 (27.2%) of controls were resuscitated after birth. One-fourth 56 (29.8%) of cases and 94 (26.4%) of controls had normal 1st minute APGAR score. More than one-fifth 55 (29.3%) of cases and nearly one-sixth 60 (16.9%) of controls had hypothermia during admission (Table 3).
Neonatal Related Factors of Cases and Controls Admitted to Hospitals in West Shewa Zone, Central Ethiopia, 2020, (Ncontrols = 356, Ncases = 188).

Determinants of Neonatal Sepsis among Neonates Admitted to Hospitals
In multi variable logistic regression analysis, maternal age, antenatal care follow-up, place of delivery, duration of labor, duration of rupture of membrane, prematurity, resuscitation, and neonates with meconium aspiration syndrome were found to be determinants of neonatal sepsis among neonates admitted to hospitals in the study area.
Mothers age was found to be a determinant of the neonatal sepsis in which those neonates whose mothers were 30 to 34 and 25 to 29 years of age were 62% and 59% less likely to develop sepsis than who were older (AOR = 0.41, 95%CI: 0.19, 0.85) and (AOR = 0.38, 95%CI: 0.17, 0.84), respectively.
Having antenatal care follow-up and places of delivery were found to be a determinant of neonatal sepsis in the study area. The odds of having neonates with sepsis were almost twice among those mothers who had no ANC follow-up compared with their counterparts (AOR = 1.89, 95%CI: 1.02, 3.49). The odds of having neonatal sepsis were 12 and almost 3 times more likely among those mothers who delivered at home and health center compared with those who gave birth at hospitals (AOR = 12.6, 95%CI: 5.32, 29.82) and (AOR = 2.74, 95%CI: 1.7, 4.41), respectively.
Neonates who were born after 12 hours or more on labor were almost twice more likely to have neonatal sepsis than those with shorter duration (AOR = 1.90, 95%CI: 1.22, 2.96). The odds of having neonatal sepsis were 3 and 5 times higher among neonates who were born after 12 to 17 hours and greater than or equal to 18 hours of rupture of membrane compared to those who were born within 12 hours of rupture of membrane (AOR = 3.26, 95%CI: 1.46, 7.26) and (AOR = 5.18, 95%CI: 1.98, 13.55), respectively.
Neonates with prematurity were 2.7 times more likely to develop neonatal sepsis than those who were not (AOR = 2.74, 95%CI: 1.73, 4.36). The odds of having neonatal sepsis was almost twice among those neonates who had been resuscitated than their counterparts (AOR = 1.93, 95%CI: 1.22, 3.06). The odds of having neonatal sepsis was lower among neonates who were admitted with meconium aspiration syndrome than those who were not (AOR = 2.55, 95%CI: 1.34, 4.83) (Table 4).
Determinants of Neonatal Sepsis among Neonates Admitted to Hospitals in West Shewa Zone, Central Ethiopia, 2020, (Ncontrols = 356, Ncases = 188).
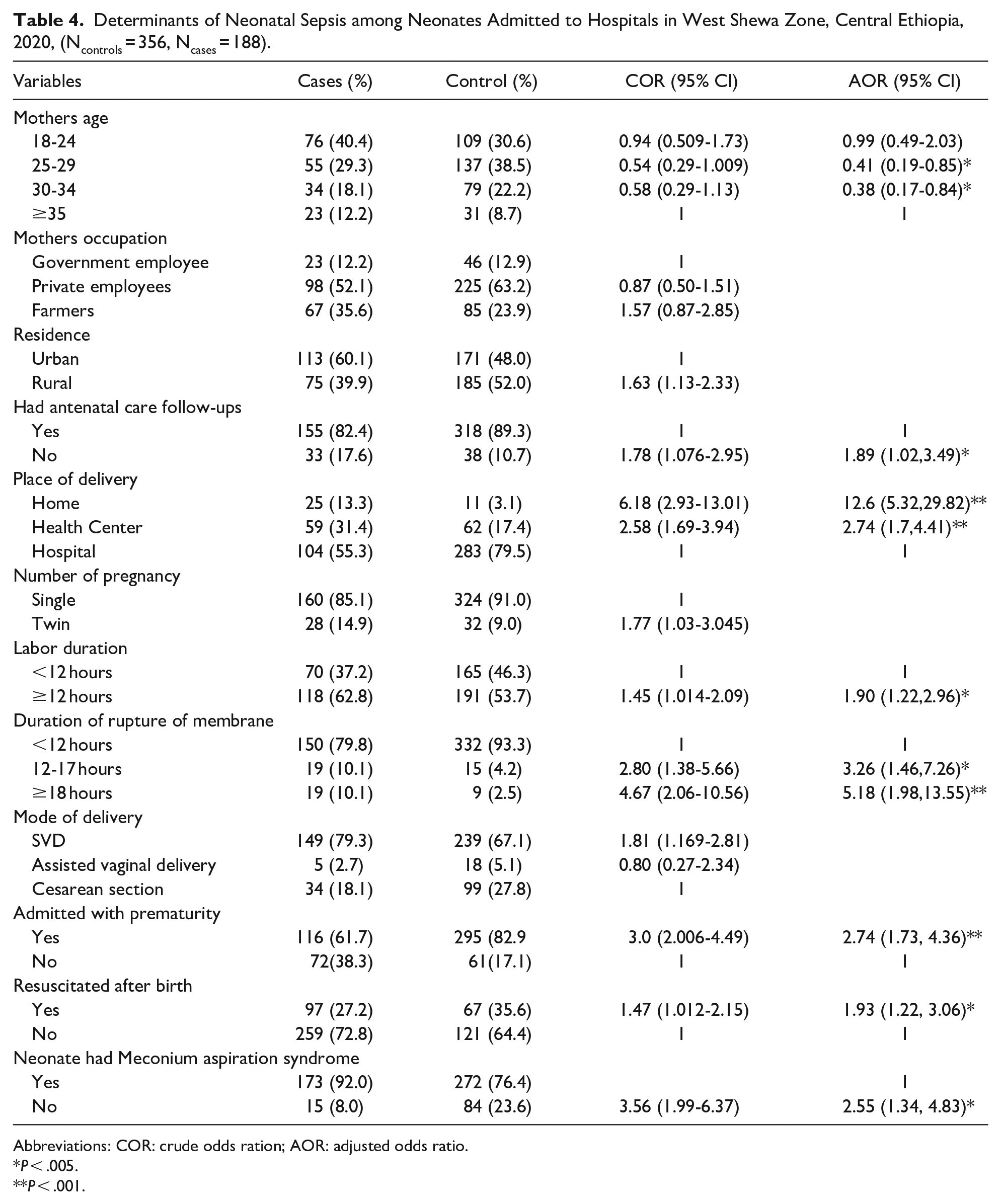
Abbreviations: COR: crude odds ration; AOR: adjusted odds ratio.
P < .005.
P < .001.
Discussion
Neonatal sepsis is the cause of substantial morbidity and mortality, especially in developing countries. Therefore, to improve neonatal health and survival it is of paramount importance to assess the predictors of this problem. This study assessed the determinants of neonatal sepsis.
According to the current study, neonates born to 30 to 34 and 25 to 29 years of age mothers were 62% and 59% less likely to develop sepsis than those who were born to older mothers. This is consistent with study done in Wolaita Sodo Town, Southern Ethiopia. 22 This might be due to the likely exposure to infectious diseases, bacterial colonization from their obstetric and gynecologic history, which tend to increase in older women that might expose neonates to sepsis. 4
This study also reported the odds of neonatal sepsis to be almost twice among those mothers who had no ANC follow-up compared with their counterparts. This is in line with the study done in Northwest Ethiopia. 15 This might be due to those mothers who had ANC follow up had a chance to be screened for infections, early detection and treatment of maternal health problems and getting vaccinated for preventable diseases during pregnancy which eventually help to decrease the neonatal infection. 23
According to the present study the odds of having neonatal sepsis were 12 times higher among mothers who delivered at home when compared with those who gave birth at hospitals. This is in agreement with the study done in Ghana 10 and systematic review done in East Africa. 8 This might be due to clean delivery practices, hand washing, and postnatal care practices are effective in reducing its prevalence and neonatal mortality from sepsis and tetanus, which is essentially lacking in home birth without the presence of a skilled birth attendant.25,26 Similarly, the odds of neonatal sepsis were almost 3 times higher among mothers who delivered at health center when compared with those who gave birth at hospitals. This is consistent with the study done in Mekelle City, Northern Ethiopia. 12 This could be because health care workers in government hospitals were likely to adhere to infection prevention practices 27 which in turn decrease the possibility of neonatal infection.
Furthermore, neonates who were born after 12 hours or more of labor had the odds of neonatal sepsis almost twice higher than those with shorter duration of labor. This is consistent with systematic review done in East Africa, 8 and study done in Southern Ethiopia. 14 This could be explained by the fact the longer labor allows the colonization and the ascension of the infection causing microorganisms to the uterine cavity exposing the fetus to sepsis. 28
The odds of having neonatal sepsis were 3 and 5 times higher among neonates who were born after 12 to 17 hours and greater than or equal to 18 hours of rupture of membrane compared to those who were born within 12 hours of rupture of membrane, respectively. This is in accordance with the studies done in Karachi, Pakistan, 11 East Africa, 8 Ghana, 10 Northwest Ethiopia,9,15 Mekelle City, North Ethiopia 12 Jinka, Southern Ethiopia, 13 and Arbaminch, southern Ethiopia. 14 Protecting the fetus from infection is one function of the membranes, ruptured membranes means the protection is gone and infection causing microorganisms are allowed to ascend from the vaginal tract. 26 Additionally, infectious, inflammatory, maternal uterine, and vascular disease and immunological diseases have been proposed to contribute to premature rupture of membrane which in turn reflect the risk of infection on the neonates. 11
According to the present study neonates with prematurity had the odds of developing neonatal sepsis 2.7 times higher than those who were not. This is consistent with studies done in India, 18 Ghana 20 Northwest, Ethiopia, 9 Southern Ethiopia, 14 and systematic review and meta-analysis in Ethiopia. 17 Immune dysfunction and an absence of trans-placentally acquired maternal immunoglobulin-G antibodies in premature infants might increase risk of infection. 4 Additionally, preterm infants often require prolonged intravenous access, endotracheal intubation, or other invasive procedures that provide a portal of entry or impair barrier and clearance mechanisms, placing them at increased risk for hospital-acquired infections. 4
Moreover, the odds of having neonatal sepsis was almost twice among those neonates who had been resuscitated than their counterparts. This is in line with the studies done in the northwest part of Ethiopia 9 and Dar Es Salaam, Tanzania. 16 This might be due to the infection prevention practices during the procedure, introducing microbes to the respiratory system of the neonates. 25 Furthermore, the physical bruises during the resuscitation might help as an entry point for microbes. 4
The odds of having neonatal sepsis was lower among neonates who were admitted with meconium aspiration syndrome than those who were not. This might be explained by the fact that those neonates with meconium aspiration syndrome (MAS) were most of the time admitted in the neonatal intensive care units receiving closer care and follow-up which helps improve neonates health and survival. 29 Additionally, the ministry of health protocol here in Ethiopia recommends empirically treatment of all neonates with MAS with antibiotics, which might prevent the risk of developing sepsis from those neonates. 30
Limitation and Strengths of the Study
As a limitation this study is lacking generalizability for the entire population, since the data for the current study were collected from those neonates admitted to hospitals. Addressing a larger number of different level hospitals is one of the strengths of this study.
Conclusions
In the current study older maternal age, not having antenatal care follow-up, home and health center delivery, prolonged duration of labor, prolonged duration of rupture of membrane, prematurity, had resuscitation and neonates with no meconium aspiration syndrome were found to be determinants of neonatal sepsis among neonates admitted to hospitals in the study area.
Therefore, the concerned stakeholders should work on increasing ANC follow for all mothers, make all births attended by skilled care providers, maintaining the intrapartum infection prevention practices at health centers and during resuscitation, and consider antibiotic prophylaxis for those neonates born to mothers with prolonged labor and rupture of membrane as an intervention for reduction of neonatal morbidities and mortalities.
Footnotes
Acknowledgements
The authors are grateful to the study participants who shared their time to give us their genuine responses, data collectors and supervisors of the study.
Authors’ Contributions
GAB, DBF, BSG, and BTD were involved in conception, design of the study, training and supervision of data collectors and supervisors, analysis, interpretations and preparation of subsequent drafts of the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data Availability
All the datasets used and/or analyzed during the current study are available from the corresponding author reasonable request.
