Abstract
Introduction
During the practice of oral health care for the elderly, pigmentation of the oral mucosa is occasionally encountered, some of which has been overlooked for many years. In the elderly, oral mucosal pigmentation might be recognized as a physiologic effect of aging, oral mucosal melanoma, pigmentation due to systemic syndromes, drug-induced pigmentation, or as a melanotic macule (Rosebush et al., 2019). One of the conditions presenting with pigmentation of the oral mucosa is Laugier-Hunziker syndrome, which is a rare disease that is not well known, especially among dental professionals (Aboobacker & Gupta, 2022). Laugier-Hunziker syndrome is a benign pigmentary disorder characterized by the unique expression of pigmentation at mucosal, nail, and acral sites. It is not considered to be indicative of systemic abnormalities (Aboobacker & Gupta, 2022). Since the only clinical implications are esthetic, patients typically have a history of several years from pigmentation to consultation (Lalosevic et al., 2015; Paul et al., 2017). Although the etiology of Laugier-Hunziker syndrome is still unclear, some cases have shown an association with genetic disorders (Aboobacker & Gupta, 2022; Dupré & Viraben, 1990; Wei et al., 2018). Laugier-Hunziker syndrome occurs at a wide age range, affecting juveniles to adults, with a mean age of occurrence of 52 years (Aliagˇaogˇlu et al., 2008). The oral clinical manifestations include numerous light-brown to brown-black macules measuring 0.1 to 0.5 cm on the tongue, lips, buccal mucosa, hard palate, and posterior pharyngeal mucosa, with acral and cutaneous involvement also showing macules and patches similar to the oral mucosa, specifically on the surface of the fingers and toes (Aboobacker & Gupta, 2022). Fingernail and/or toenail pigmentation, sometimes in the form of longitudinal streaks, is seen in half to two-thirds of cases (Mignogna et al., 1999; Moore et al., 2004; Nikitakis & Koumaki, 2013).
In this report, we describe a rare case of an elderly woman with pigmentation of the oral mucosa that was diagnosed as Laugier-Hunziker syndrome.
Case Report
The patient was an 84-year-old female who resided at a facility for the elderly. She was a non-smoker and had a history of hypertension, chronic cardiac insufficiency, and mild dementia, but was not currently on any medication. She had no medical complaints and saw her internist regularly. During the first oral examination by the dental hygienist after her admission to the facility, since the patient expressed concern about her black lips, she was referred to the dentist for detailed examination.
Examination by the dentist revealed multiple, variously sized, brown-black patches of pigmentation on her upper and lower lips, buccal mucosa, and gingiva. Pigmentation, which seemed to be a physiological change, was also observed on her facial skin (Figure 1). She stated that the pigmentation of her lips had been there for over 5 years and had progressively become darker. Her medical records did not indicate any systemic disease likely to cause pigmentation of the oral mucosa, nor had she taken any medication that would have caused the pigmentation. The dentist definitively ruled out mucosal melanoma, although no definitive diagnosis could be made. A dermatologist was consulted at a later date, who suggested the possibility of Laugier-Hunziker syndrome and recommended close examination of the nails and skin. At the next dental examination, the patient’s fingers and toes were observed as not being pigmented, although longitudinal streaks were observed on her left first toenail (Figure 2). The patient’s final diagnosis was Laugier-Hunziker syndrome. Subsequently, the patient was given an explanation about her medical condition, and informed that no active treatment was required, only regular follow-up. Since then, regular observation by the responsible dental hygienist has been continued. A year later, no change in her condition has been observed at the dentist’s examination.

Facial and oral views of the patient: (A) physiological pigmentation was present on her face and (B–D) oral mucosal pigmentation was found on her lips, buccal mucosa and gingiva.
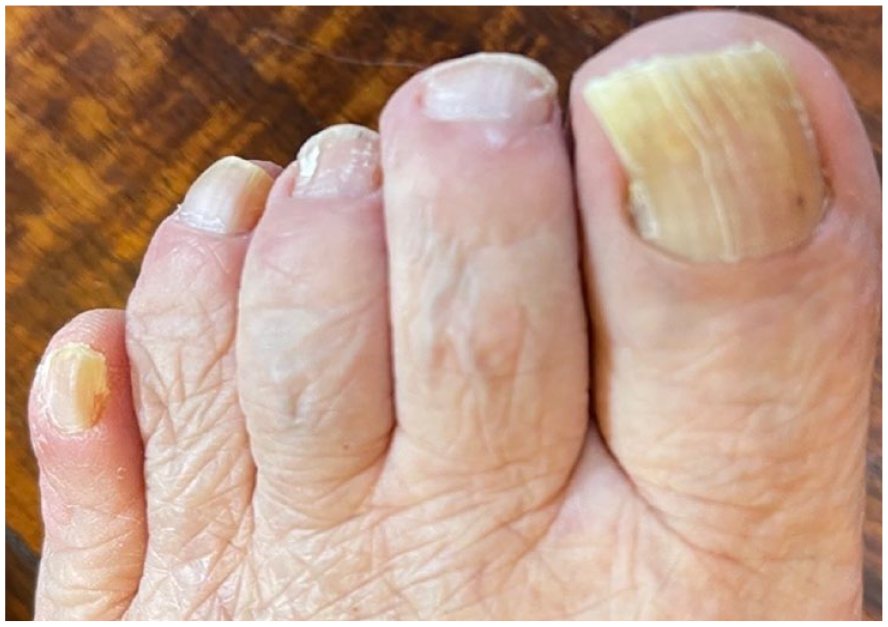
Longitudinal streaks were seen on the patient’s left big toe nail.
Discussion
This report describes a rare case of oral mucosal pigmentation caused by Laugier-Hunziker syndrome in a resident of an elderly care facility.
When providing medical care at various care facilities, including a facility for the elderly, it is necessary to first accurately assess the patient’s condition in-house, since taking the resident to an outside hospital is costly, including personnel expenses.
Knowledge about the various possible differential diagnoses is important because elderly people have a variety of possible causes of oral mucosal pigmentation. Since Laugier-Hunziker syndrome seems to be more of a diagnosis of exclusion, other conditions should be ruled out prior to making a diagnosis (Aboobacker & Gupta, 2022). The first condition that requires differentiation in cases of oral mucosal pigmentation is mucosal melanoma. Mucosal melanoma takes the form of a brown or black macule, patch or nodule, and most commonly occurs between the ages of 40 and 70, and has aggressive behavior. The most affected site is the hard palate or alveolar gingiva (Femiano et al., 2008; Lambertini et al., 2018). In addition, most oral mucosal melanomas appear as new lesions from apparently normal mucosa. However, about 30%–50% have persistent oral pigmentation for several to several months. A longer duration of oral pigmentation does not rule out oral mucosal melanomas (Femiano et al., 2008). Unlike melanoma, Laugier-Hunziker syndrome presents with multiple areas of pigmentation of the oral mucosa, accompanied by skin and nail symptoms.
Physiological pigmentation might have a similar clinical picture as Laugier-Hunziker syndrome, with macules of various sizes and shapes that increase with age (Rosebush et al., 2019). However, Laugier-Hunziker syndrome also presents pigmentation at other sites, such as the nails and skin. The commonly occurring melanotic macules, which usually present as solitary areas of pigmentation, should also be included in the differential diagnosis (Rosebush et al., 2019).
Systemic conditions of particular importance with similar mucosal pigmentation include Peutz-Jeghers syndrome, autosomal dominant genodermatosis and Addison’s disease, which is an endocrine disease due to adrenocortical insufficiency. However, these diseases have other signs and symptoms that are unique to the disease (Lalosevic et al., 2015). Additionally, in elderly patients with these conditions, it is likely that they are already known to have these systemic diseases. Of course, although there are other systemic diseases that cause pigmentation of the oral mucosa, they are rare.
Since various drugs can cause pigmentation of the oral mucosa, drug-induced pigmentation should also be considered in the differential diagnosis of Laugier-Hunziker syndrome (Lenane & Powell, 2000; Yuan & Woo, 2015). In such cases, a detailed medical and medication history is important. Among them, pigmentation due to cancer chemotherapy drugs is attracting attention. Anticancer drugs, such as alkylating agents, cyclophosphamide, carboplatin and gemcitabine, and antimetabolites, such as 5-fluorouracil and tegafur, might cause similar pigmentation of the oral mucosa, skin and nails (Deutsch et al., 2020). In general, drug-induced pigmentation occurs with administration of the drug for several months to several years, and disappears when the drug is discontinued (Lalosevic et al., 2015). However, pigmentation due to cancer chemotherapy drugs appears within a few weeks of administration of the drug and lasts for a long time.
Smoker’s melanosis is often seen in dental practice and is found on the lips and anterior gingiva. Since this type of pigmentation might persist even after quitting smoking, it is necessary to check the patient’s smoking history (Multani, 2013).
In this case, since physiological pigmentation was observed on the facial skin, physiological pigmentation of the oral mucosa was also considered in the differential diagnosis. However, because the mucous membrane was dark and conspicuous, some kind of disease was suspected. Although this condition was initially unknown to us, the diagnosis of Laugier-Hunziker syndrome was made based on the fact that the patient’s medical history and medication history were unremarkable and that she also had nail pigmentation.
The most presumed etiology of Laugier-Hunziker syndrome at present is that elevated activity of melanocytes leads to an increase in melanosome formation, resulting in the accumulation of melanin in the basal mucosal layer, with a normal number of melanocytes and a normal morphologic appearance (Aboobacker & Gupta, 2022; Moore et al., 2004; Yago et al., 2008).
In terms of the treatment for pigmentation, although cryotherapy and various laser treatments are performed, recurrence is common. Additionally, it is important to avoid exposure to sunlight (Ergun et al., 2013; Zuo et al., 2010).
Dental practitioners are relatively well aware of the white and red diseases of the oral mucosa, such as leukoplakia and lichen planus, but they seem to be less knowledgeable about black and brown diseases. Laugier-Hunziker syndrome, a disease that causes pigmentation of the oral mucosa, is less familiar in dentistry, and more familiar in dermatology (Lalosevic et al., 2015).
In conclusion, we reported a case of Laugier-Hunziker syndrome in an elderly institutional resident, which is not well known among dental professionals. Increasing dentists’ knowledge about diseases that cause pigmentation of the oral mucosa would be of great help in their clinical practice, especially at external facilities.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
