Abstract
Background
Transfusion transmissible infections (TTIs) are among the greatest threats to blood safety for recipients and the economy of the developed and developing countries. Therefore, the study of the prevalence and trends of TTIs is important to assess for its prevention and control strategies.
Objectives
This study aimed to evaluate the prevalence and trend of transfusion transmissible infections among blood donors at the Bule Hora Blood Bank, West Guji, Ethiopia, from 2019 to 2021.
Method
A retrospective study was conducted on all blood donors at the Bule Hora Blood Bank from 2019-2021. The data of 4193 blood donors were collected from the databank (logbook) of the blood bank using a checklist. Data were analyzed by using SPSS software, and the chi-square test was used to assess the association between independent variables and transfusion transmission infection. Different types of graphs, charts and tables were used to present the data. P values less than .05 were considered statistically significant.
Result
The overall transfusion transmissible infection among blood donors was 4.6% (192). Out of the tested blood donors, 86 (2.1%) were found to be seropositive for hepatitis B virus. The trend analysis showed that the positivity rates of the screened tests were 28 (4.72%) in 2019, decreased to 77 (4.26%) in 2020 and increased to 87 (4.86%) in 2021. The sex of blood donors was significantly associated with TTIs (P value = .021), and the positivity rates were significantly higher among male than female blood donors. The study results showed that overall seropositivity rates increased along the age groups of the donors.
Conclusion
The study reported a moderate prevalence of transfusion transmissible infections among blood donors visiting the Bule hora blood bank. Health education about the transmission, prevention and create awareness of TTIs should be strengthened by the government and non-government organization.
Back Ground
Blood transfusions are transfusions of whole blood or its components. This is important to save millions of patients worldwide from death and morbidity each year. There were reports that a quarter of a million mothers died globally due to obstetric bleeding, particularly in developing countries where there was a high number of maternal mortality, motor accidents and populations non-immune to malaria. Furthermore, anemia causes 15% of child deaths in Africa.1,2 All the above mentioned cases required blood transfusions that correct the different conditions of patients, such as anemia, plasma clotting factor deficiency, thrombocytopenia, and hypoalbuminia.3,4
Blood transfusion is a therapeutic procedure, but contaminated blood transfusion can transmit infectious diseases and can be fatal instead of saving life. The discovery of transfusion transmissible infections (TTIs) has heralded a new era in blood transfusion practice worldwide with an emphasis on the fundamental objective, safety and protection of human life. Hepatitis B virus (HBV), hepatitis C virus (HCV), human immune virus (HIV) and syphilis are of great concern in transfusion medicine because of their prolonged viremia and carrier or latent state.5,6
TTIs cause serious mortality, morbidity and financial burden and are thus a major global health problem. The prevalence of TTIs antibodies among blood and plasma donors permits an assessment of the occurrence of infections in the blood donor population and consequently the safety of the collected donations. It also gives an idea of the epidemiology of these diseases in the community. Transfusion-associated infections continue to be a major threat. 7
Despite uncertainty in the exact rates of transmission, blood transfusion is still considered to be a contributing mode of virus and bacterial transmission in parts of Africa. The proportion of new HIV infections might range from 5% to 10%. 8 Similarly, 12.5% of patients are at risk of post-transfusion hepatitis infection. 9 HBV is a highly known potential infectious virus that is associated with complications such as cirrhosis, portal hypertension and hepatocellular carcinoma. 10
Several studies have been conducted to assess the prevalence and trends of TTIs among blood donors in different parts of the world. They found an increase or decrease in trends in TTIs. 11 Thus, the blood transfusion units of each health institution should have a major role in screening, monitoring and controlling TTIs. These practices also provide some clues about the magnitude of TTIs in healthy populations.1,11 Selection of blood donors with low TTIs risk was followed by effective laboratory screening in the majority of blood transfusion units.12,13
In Ethiopia, the main source of blood donation is voluntary donors, and most of them are students and teachers. Proper screening of blood and selection of donors is very important to ensure a safe blood supply. Conducting this study at Bule Hora blood bank, the only blood bank serving over million populations of the Pastoral community of South Ethiopia, can provide a better understanding of the epidemiology of these infections, particularly in pastoralist areas. This can support the development of strategies to reduce infectious disease transmission, in addition to the preventive and control measures that are needed to manage the burden of these infections in the community. Therefore, the study aims to assess the prevalence and trends of transfusion transmissible infections among blood donors at Bule Hora blood during the period 2019 to 2021.
Method
Study Area, Design and Period
The retrospective study was conducted at the Bule hora blood bank located in Bule hora town, which is located in the West Guji zone, Oromia region, South Ethiopia. The common name for this city was Hager Mariam. It is the capital city of the West Guji Zone. It is located approximately 470 kilometers south of Addis Ababa, the capital of Ethiopia. The blood bank was established in 2019 at the 02 Kebele of Bule hora town. The blood bank provides blood supply for 1.4 million people, including patients from Bule hora General Hospital and nearby health facilities in neighboring zones and districts. The data were collected between March 03 and June 20, 2022, from blood donors’ records covering the period from 2019 to 2021.
Study Population and Selection
The study populations were all blood donors who attended the Bule Hora blood bank during the 3-year period and those screened for hepatitis B, hepatitis C, HIV AIDS and syphilis antibodies. All blood donors who had complete data on the log book were included in the study. Blood donors with incomplete data were excluded from the study.
Sample Size and Sampling Technique
A total of 4193 blood donors who attended the Bule hora blood bank with complete data recorded on the log book from 2019 to 2021 were assessed in the present study.
Data Collection Procedures
At the Bule hora blood bank, the donors’ blood was screened for TTIs after donation. Blood samples were tested using kits following the manufacturer's instructions. Blood samples from donors were converted to serum or plasma samples before running for HBV, HIV, HCV and syphilis tests. The RPR test was used for screening for syphilis. Hepatitis B surface antigen (HBsAg) was detected using Murex HBsAg. Antibodies against HCV were detected using the Murex anti-HCV version. Antibodies against HIV types 1 and 2 were screened using Uni-Form II Ag/Ab. The results of tested blood were recorded on a registration logbook. Then, trained data collectors and supervisors checked the data for completeness and consistency. The complete, accurate and fulfilled all necessary requirements document were extracted for the study.
Data Quality Management
Before commencing data gathering, all 3-year data registration books were prepared. Then, trained data collectors and supervisors checked the data for completeness and consistency. The complete, accurate and fulfilled all necessary requirements document were extracted for the study using data extraction format. The data were double entered, and all completeness and appropriateness were checked before analysis.
Data Analysis
The data generated extracted from the laboratory data registration book were cleaned, edited and double entered using EpiData version 3.1 (EpiData Association, Odense, Denmark). The data were checked and exported to SPSS software version 25 for further analysis. Descriptive statistics such as percentage and frequency were computed, and the means with standards were used to summarize the continuous variables. Different types of graphs or charts and tables were used to present the data. A chi-square test was used to assess the association between sociodemographic and transfusion transmission infections. A P value less than .05 was considered statistically significant.
Ethical Consideration
The study was approved by the Bule Hora University, Institute of Health Review Committee (IHRC01/22) according to the Declaration of Helsinki. After ethical clearance, an official letter was written to Bule Hora blood bank. Then, data extraction commenced after the permission was obtained from the Bule hora blood bank. The information of blood donors was recorded in the anonymized registration book; therefore the confidentiality was kept strictly by the blood bank.
Result
Sociodemographic Characteristics
A total of 4193 blood donors were screened at the Bule hora blood bank, West Guji, South Ethiopia, from 2019 to 2021. The blood donor ages ranged from 17 to 58 years, with a mean (SD) age of 24 (±7.24) years. Of the blood donors, 2914 (69.5%) were males, and 1279 (30.5%) were females. The most common age group of donors was found to be 20 to 29 years (55.7%), while the least common age group was >50 (1.12%). The majority 1809(43.14%) of blood donors were seen in 2020. All of the blood donors were voluntary donors (Table 1).
Sociodemographic Characteristics of Blood Donors at the Bule Hora Blood Bank, South Ethiopia, from 2019 to 2021.

Sero-Prevalence of Transfusion Transmissible Infections
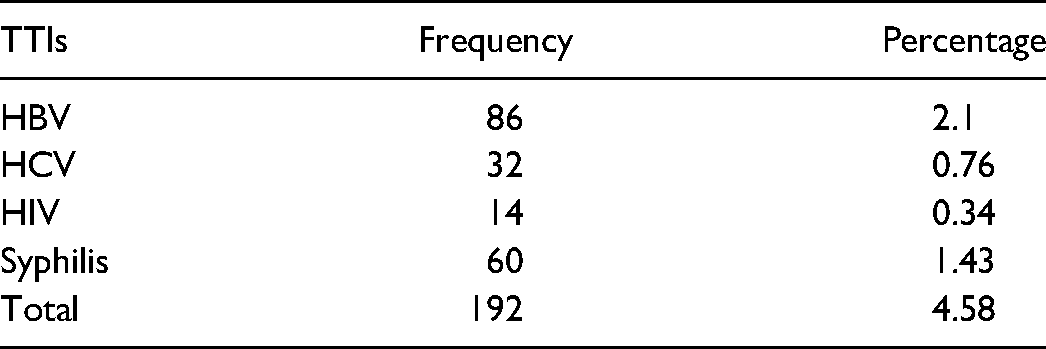
The overall prevalence of TTIs among blood donors who attended the Bule Hora blood bank was 192(4.6%). The seroconversion rates of HBV, HIV, HCV and syphilis in the blood donors were 2.1%, 0.34%, 0.8%, and 1.4%, respectively. There was no coinfection detected (Table 2).
Sero-Prevalence of Transfusion Transmissible Infections Among Blood Donors Attended at Bule Hora Blood Bank, South Ethiopia from 2019 to 2021.
Out of 192 sero-positive transfusion transmissible infections, the majority proportion 86(44.8%) was occupied by HBV, followed by syphilis 60(31.2%), HCV 32(16.7%) and HIV 14(7.3%) (Figure 1). From age groups of blood donors attended at the Bule Hora blood bank, the highest 7(14.9%) overall seropositivity was detected among those aged ≥50 years old. The study results showed that overall seropositivity rates increased along the age groups of the donors (Table 3).
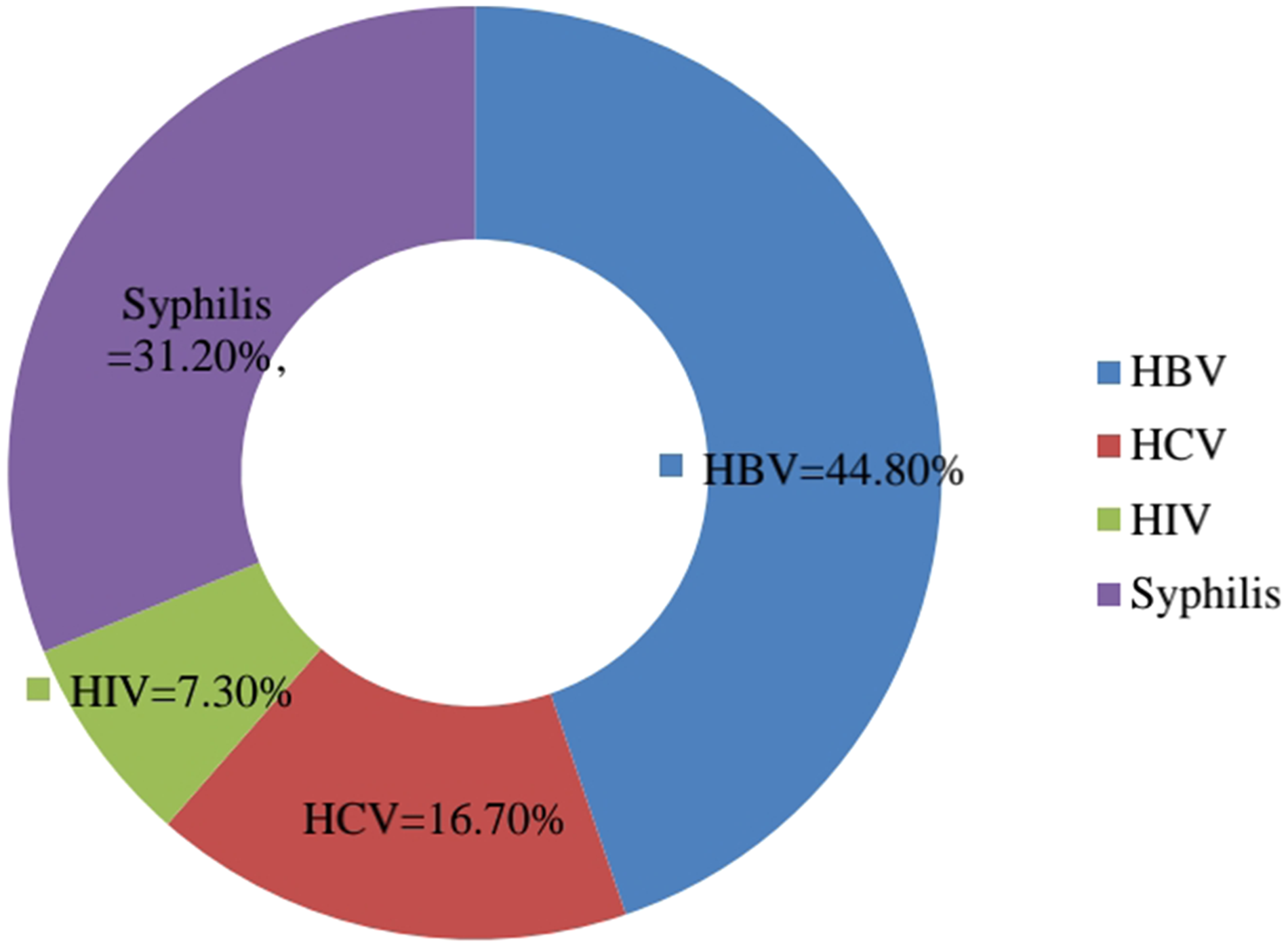
Proportion of transfusion-transmitted infections among seroprevalence.
Transfusion Transmissible Infections Distribution Among Age of Blood Donors at Bule Hora Blood Bank, South Ethiopia.

The overall prevalence of blood transfusion-transmitted infections was higher among male blood donors 135(4.63%) than among female blood donors 57(4.46%). The proportions of syphilis and HBV were higher among males, while HIV and HCV were higher among female blood donors (Figure 2).

Distribution of transfusion-transmitted infections among sexes of blood donors.
Factors Associated with Transfusion-Transmitted Infections
The sex of blood donors was significantly associated with TTIs (P value = .021). The TBT positivity rates were significantly higher among male than female blood donors. Similarly, syphilis, HIV and HCV were significantly associated with the sex of blood donors (P value = .009, P value = .001 and P value = .001). The age group of blood donors was significantly associated with syphilis (P value = .001) (Table 4).
Association Between Transfusion-Transmitted Infections and the Sociodemographic Characteristics of Blood Donors at Bule Hora Blood Bank, South Ethiopia, from 2019 to 2021.

Trends of Transfusion Transmissible Infection
The trend analysis showed that the positivity rates of the screening tests fluctuated over time. Blood transfusion transmissible infections were 28(4.72%) in 2019, then decreased to 77 (4.26%) in 2020 and increased to 87(4.86%) in 2021. From screened TTIs, HBV and HIV seropositivity decreased from 2019 to 2020 and increased again from 2020 to 2021. However, syphilis and HCV positivity rates gradually increased from 2019 to 2021 (Figure 3).

Trends of transfusion-transmitted infection among blood donors at the Bule Hora blood bank, South Ethiopia.
Discussion
In this study, the overall prevalence of TTIs among blood donors who attended the Bule hora blood bank over the past 3 years was 192 (4.57%). This finding was higher than that of studies conducted in neighboring Eritrea 3.8%, 14 Brunei Darussalam 1.49%, 15 Yemen 2.35%, 16 Kassala, eastern Sudan 3%. 13 However, this finding was lower than those of studies conducted in Guyana 6.2%, 17 Teaching Hospital of Islamabad 14.34%, 18 Nigeria 19.3%, 19 Northwest Ethiopia 43.2%, 20 Dire Dawa 7.1%, 21 Bahir Dar district 6.0%, 22 Hawassa 7.1% 23 and Harar 6.6% 24 regions of Ethiopia. The reason for the relatively lower rate of seroprevalence of TTIs in this study compared with other studies may be because of the existence of different magnitudes of risk factors for contracting transfusion-transmitted infections and may also be the sensitivity of the screening technique used. In addition, the present study only included voluntary blood donors with good health status, while other studies may have enrolled patients who required blood replacement.
In our study, the prevalence rate of HBs Ag was 2.1%. This finding is comparable with a study conducted among blood donors in India 2.15%. 25 This finding is higher than those of studies conducted among blood donors in Qatar (0.3%) 26 and Guyana (1.5%). 17 In contrast, the present finding is lower than those of studies conducted by Eritrea 4%, 14 Gondar University Teaching Hospital 4.7%, 27 Dire Dawa 4.67%, 21 and Bahir Dar district 3.9%. 22 However, the current finding is lower than those of studies performed on donors at Felege Hiwot Referral Hospital 25% 20 and Nigeria 18.6%. 28 The difference may be due to the applied diagnostic technique, sample size of participants and variation in prevalence among the community.
The prevalence of HCV among blood donors was 0.76%, which is in line with reports from Qatar (0.6%) 26 and Dire Dawa (0.96%) 21 ; however, this finding is lower than those of studies performed in Sudan (3.1%), 13 Egyptian donors (3.5%), 29 Guyana (1.3%), 17 and Bahir Dar district (0.5%). 22 The low prevalence of HCV when compared with HBV might be because HCV is less infective when compared with HBV and HCV is transmitted mainly through transfusion of blood or blood products, intravenous drug abuse and needle sharing, which may not be common in the Ethiopian Somali Region.
The prevalence of HIV in the current study was 0.33%, which is in line with a study performed in Bahir Dar district of 0.5%. 22 However, the findings of the current study are lower than those of studies from Guyana (0.8%) 17 and Dire Dawa (1.24%) 21 but higher than those of studies conducted in Qatar (0.18%) 26 and Egypt, in which no cases were reported. 29 The prevalence of syphilis in the present study was 1.43%, which is in line with reports of the Bahir Dar district of 1.2%. 22 In contrast, the current finding is higher than that of studies conducted in Qatar (0.43%), 26 Guyana (0.6%), 17 and Dire Dawa (0.44%). 21 The differences in prevalence among these studies may be due to discrepancies in government and nongovernmental interventions, socioeconomic status of the community, educational level and quality of blood bank laboratories.
In this study, the sex of blood donors was significantly associated with TTIs (P value = .021). The TBT positivity rates were significantly higher (4.6 times) in male blood donors than in female blood donors (4.5%). This finding agreed with studies conducted in Qatar, 26 Dire Dawa, 21 and Bahir Dar district, 22 which reported that the prevalence of transfusion transmissible infections was significantly higher among male blood donors than among female donors. The higher transfusion transmissible infection positivity rates among males may be due to more males being involved in blood donation and contact with risky activities than females.
The trends of transfusion-transmitted infections among the blood donors who attended the Bule hora blood bank fluctuated over time. Blood transfusion transmissible infections were 4.72% in 2019, then decreased to 4.26% in 2020 and increased to 4.86% in 2021. This finding was supported by a study conducted in Guyana. 17 This finding disagrees with studies reporting an increase in the overall prevalence of transfusion-transmissible infections from Qatar 26 and Bahir Dar district. 22 In contrast, a study conducted in Dire Dawa reported a significant decrease in TTIs among blood donors. 21 The study found that syphilis and HCV positivity rates gradually increased from 2019 to 2021, while HBV, which had the highest seroprevalence of TTIs among blood donors in the study area, decreased from 2019 to 2020 and again increased from 2020 to 2021, which resulted in a fluctuating overall trend.
In the current study, there was no coinfection detected among blood donors at the Bule hora blood bank. This result was lower than that of a study conducted in Bahir Dar district, 22 which reported that 0.14% of the study participants were coinfected with more than one infection. On the other hand, the study results showed that overall seropositivity rates increased along the age groups of the donors, with the lowest prevalence of 3.38% detected among the 15 to 19 age group and the highest prevalence of 14.9% detected among the above 50 age groups. This finding was supported by a study conducted in Dire Dawa 21 that reported that the prevalence of TTIs increased with age. The increase in TTIs with age might be due to an increase in risk contact and involvement in polygamous marriage among the old age group.
The Strengths and Limitations of the Study
The strengths of the study were large sample size data gathered from voluntarily blood donors hence, the findings could be generalized to determine the exact prevalence TTIs among the general population in the area. However, the current study was based on a retrospective review of monthly summary records at the Bule hora blood bank, which limits the independent variables to only sex and age. Since Bule Hora blood blanks were established a few years ago, the study assessed only three years of data with four blood transfusion transmissible infections, which restricted the study to seeing trends of long time and various infections. There was no confirmatory test performed in the Bule hora blood bank; hence, it was difficult to manage false positives.
Conclusion
The study revealed a moderate prevalence of TTIs among blood donors visiting the Bule hora blood bank. The trend analysis showed that the positivity rates of the screened tests fluctuated from 2019 to 2021. The TBT positivity rates were significantly higher among male than female blood donors. The study results showed that overall seropositivity rates increased along the age groups of the donors. The prevalence of HBV followed by syphilis is considerably higher than that of other TTIs among blood donors at the Bule hora blood bank. There was no coinfection detected among blood donors. Health education about the transmission, prevention and awareness of TTIs infections should be strengthened by the Bule hora Health Bureau. Inclusion of vaccination for hepatitis B virus in the expanded plan for immunization (EPI) is recommended by the Federal Ministry of Health.
Abbreviations
Antibody
Acquired Immune Deficiency Virus
Center of Diseases Control
Ag Hepatitis B core Antigen
Ag Hepatitis B surface Antigen
Hepatitis C Virus
Human Immune Virus
Rapid Protein Reagin
Transfusion Transmission Infection
World health organization
Footnotes
Acknowledgements
First, I would like to thank the almighty God who assisted me in performing this research smoothly and will successfully extend this acknowledgment to the Bule Hora University, Institute of Health and Department of Medical Laboratory for giving us a chance to conduct this research project. We extend our acknowledgment to our adviser Moti Shibru and Tekaligh Abebe for their unreserved data extraction and continuous assistance and their close cooperativeness with nice approach without saying we tired during our research writing, without their involvement, this work might have been worthless. Finally, we will acknowledge the Bule Hora blood bank and the staff given the chance to collect data from the data bank and their nice approach and assistance during the data collection.
Authors’ Contributions
AA: Conceptualization, developed proposal, resource, project administration, investigation, and supervision, performed data analysis and interpretation. GA: Data curation, formal analysis, software, investigation, and supervision; performed data analysis and interpretation; and wrote. SA: Data analysis and supervision; performed data analysis and interpretation; and wrote. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Consent for Publication
Not applicable.
Availability of Data and Materials
Data essential for the conclusion are included in this manuscript. Additional data can be obtained from the corresponding author upon reasonable request.
